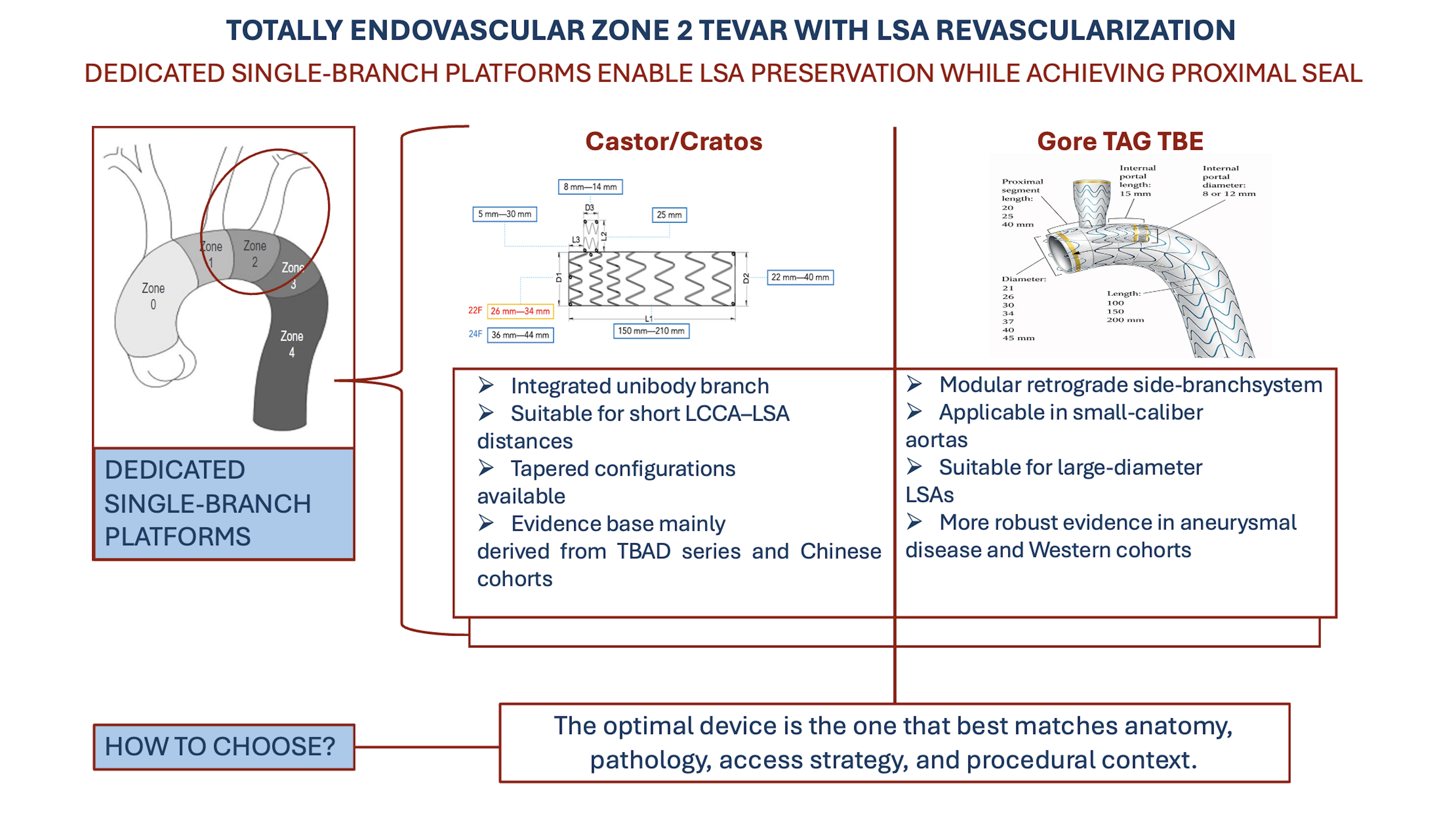
Zone 2 thoracic endovascular aortic repair (TEVAR) frequently requires left subclavian artery (LSA) preservation to maintain vertebrobasilar and upper-extremity perfusion while obtaining a durable proximal seal. Dedicated single-branch endografts were de-veloped to standardize this step and to convert a traditionally hybrid scenario into a reproducible fully endovascular strategy. Two different concepts currently dominate this field: integrated unibody branch platforms, represented by Castor and the sec-ond-generation Cratos, and modular retrograde-branch systems, represented by the Gore TAG Thoracic Branch Endoprosthesis (TBE). The Castor/Cratos evidence base is broader, older, and much more heavily weighted toward type B aortic dissection, including long-term prospective multicenter data and several large real-world cohorts with fa-vorable branch patency and aortic remodeling. By contrast, TBE evidence is expanding rapidly and is supported by prospective midterm data in arch aneurysms as well as by increasingly large post-commercial series and comparative analyses across zones 0–2. Beyond outcomes, the two platforms differ substantially in branch directionality, con-tribution to proximal fixation, modularity, branch diameter range, proximal landing requirements, access profile, and regulatory/off-the-shelf availability, all of which have direct consequences for anatomical suitability in dissection, aneurysm disease, and trauma. This narrative review synthesizes current evidence and proposes an anato-my-first, pathology-aware framework for selecting between Castor/Cratos and TBE in totally endovascular zone 2 TEVAR with LSA revascularization.