Submitted:
09 July 2025
Posted:
10 July 2025
You are already at the latest version
Abstract
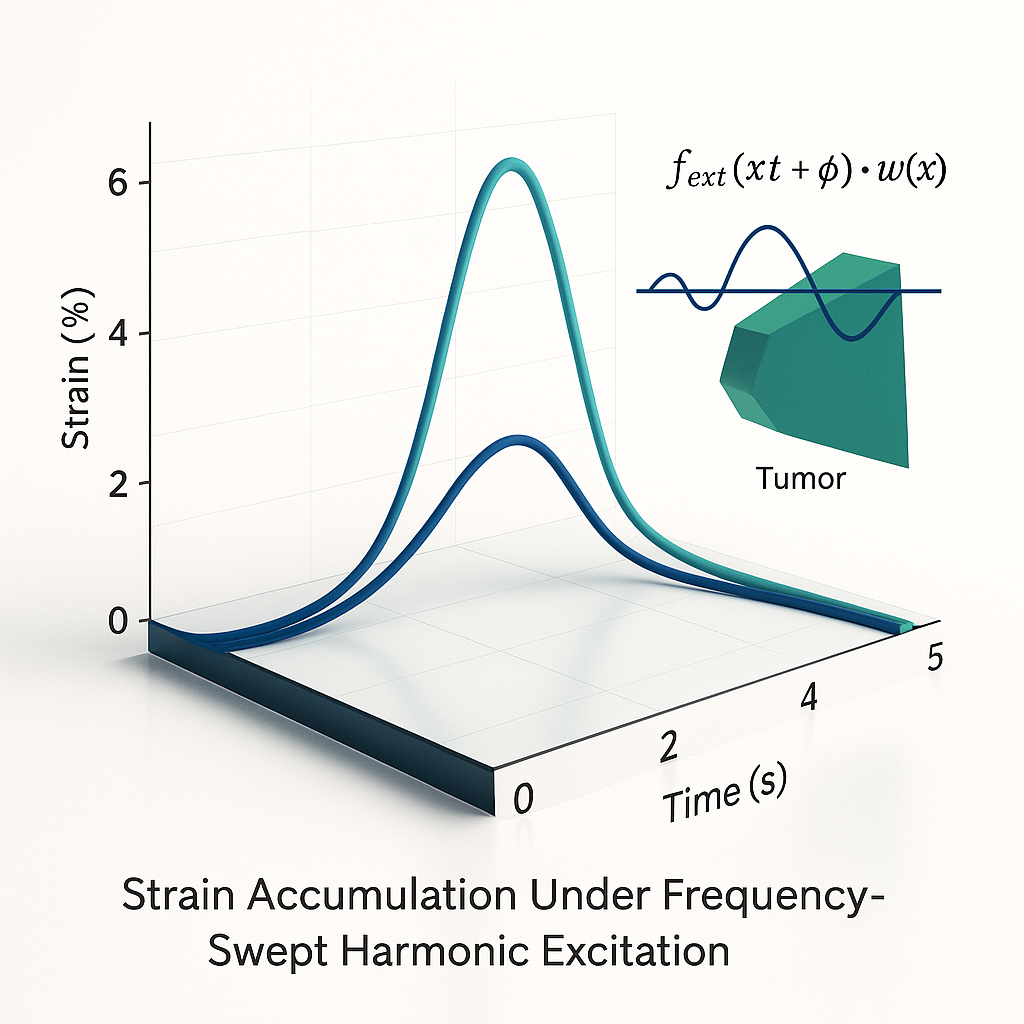
Keywords:
1. Introduction
2. Introduction: Spatiotemporal Context of the Problem
- radiologically occult,
- surgically inaccessible,
- pharmacologically refractory.
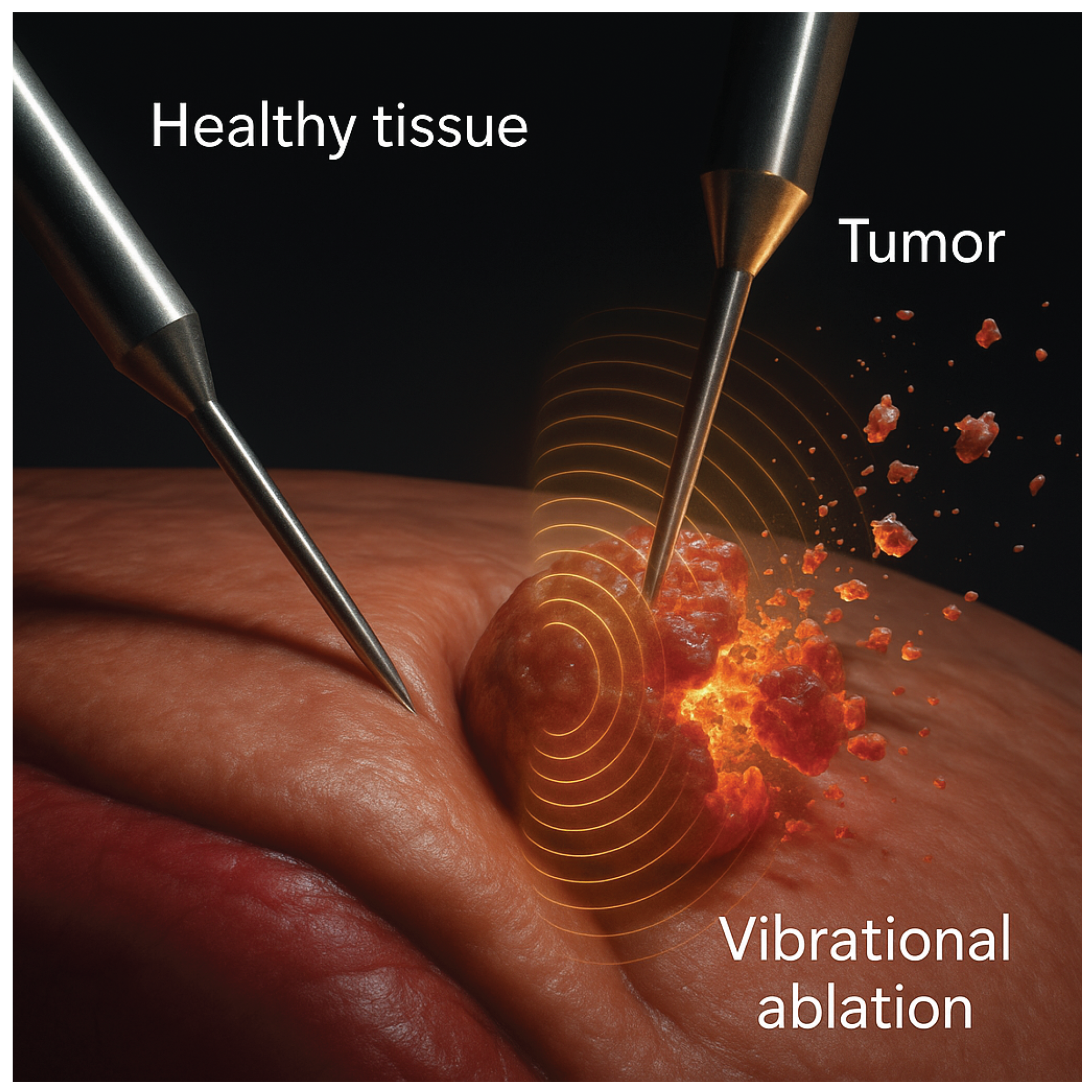
2.1. Simulation of Phantom Tumor Models
2.2. Translational Implications
2.3. Nonlinear Coupling and Anisotropic Effects
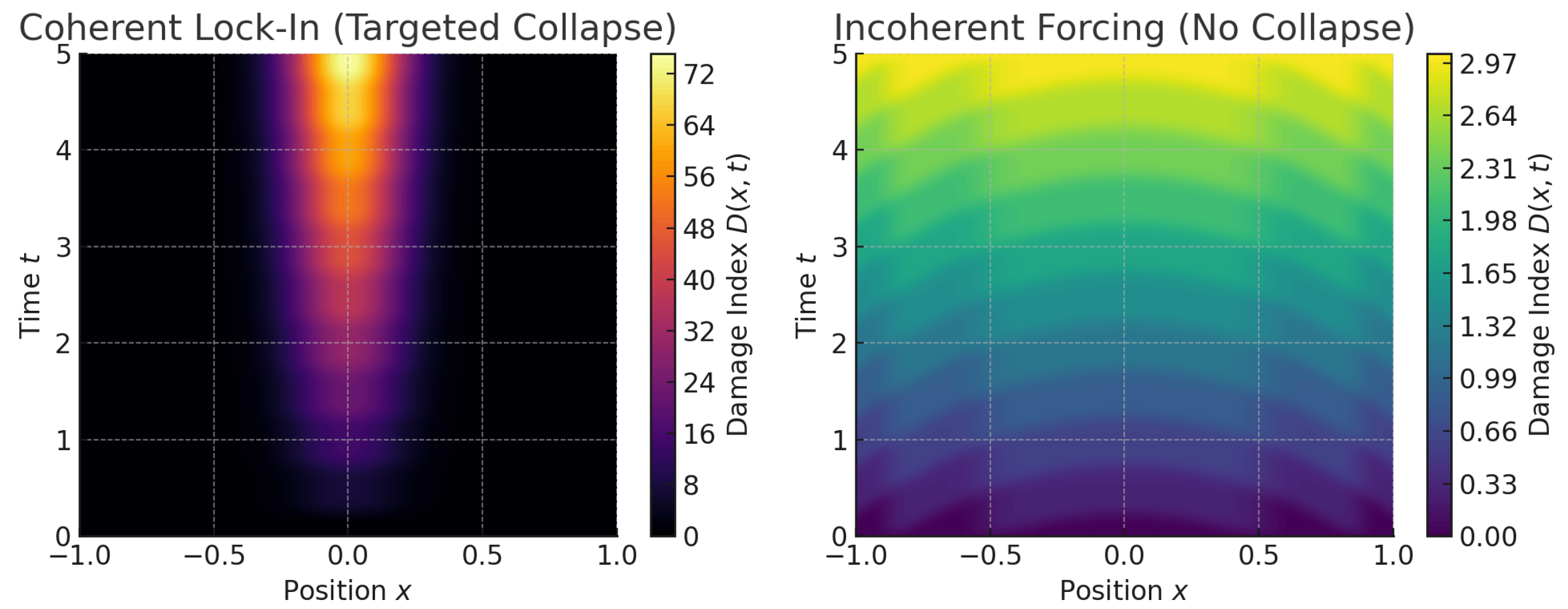
2.4. Energy Localization and Collapse Dynamics
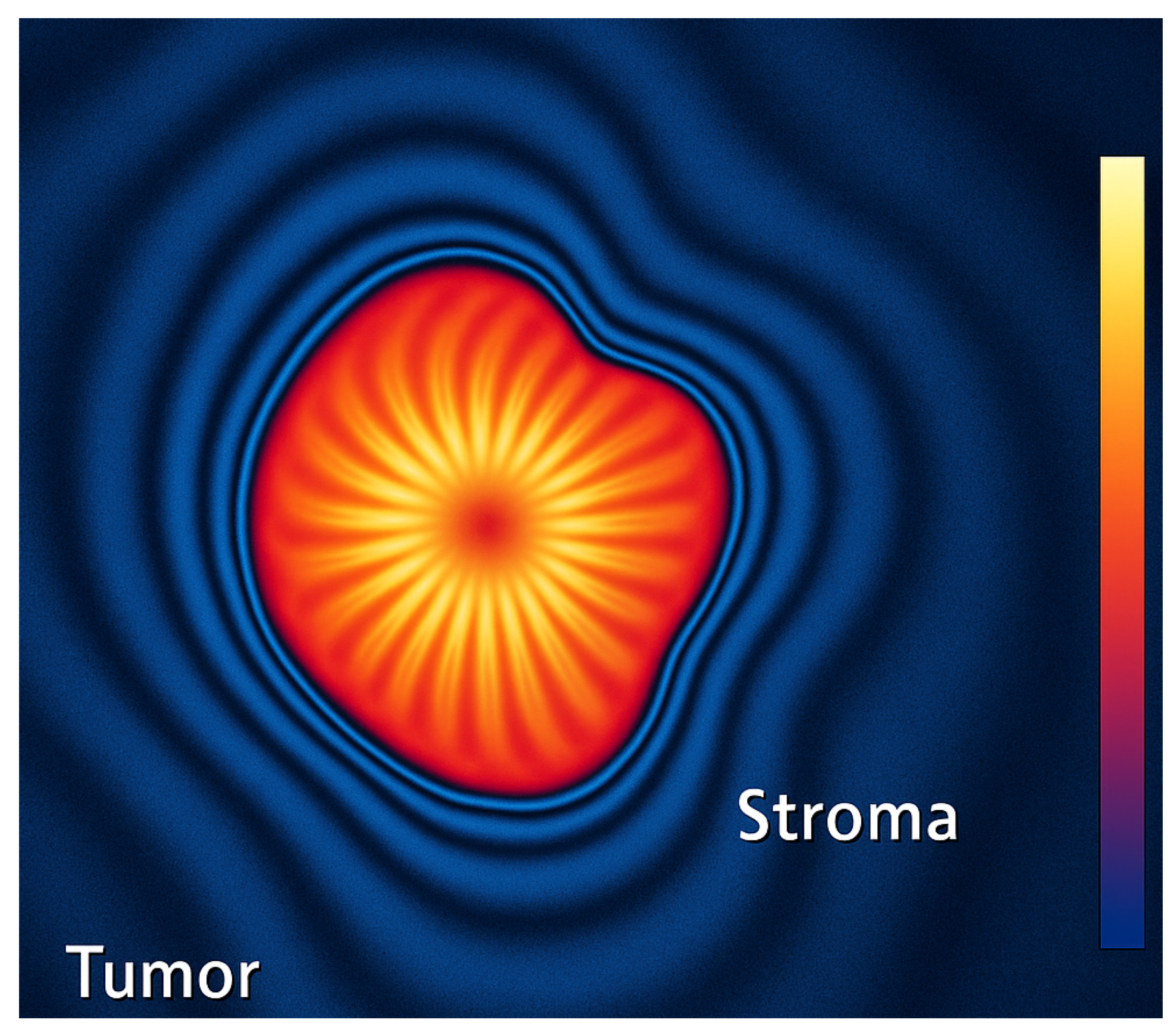
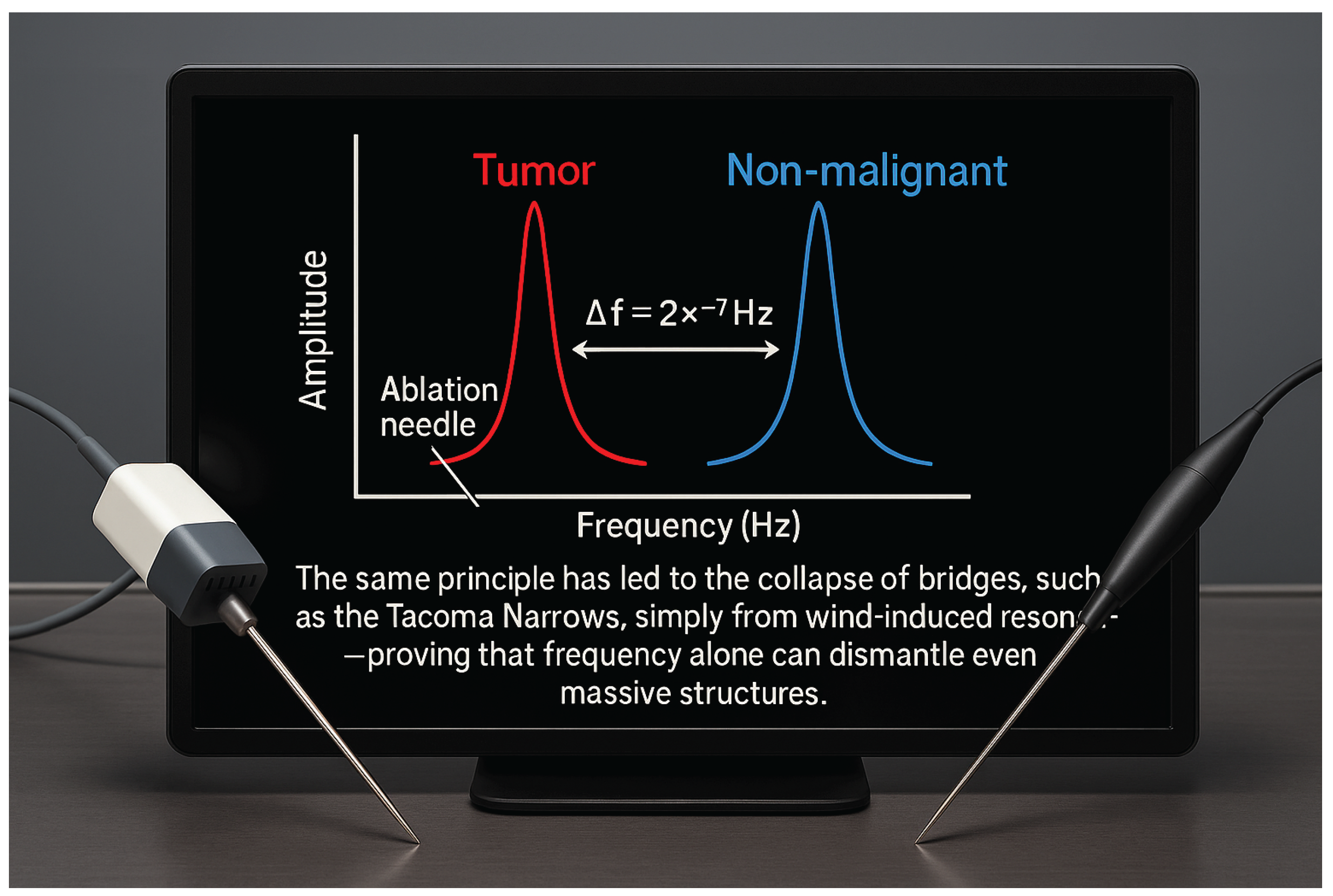
2.5. On Genetic and Subcellular Frequencies
2.6. Spectral Coherence and Interferometric Lock-In

3. Spectral Collapse: A Functional Alternative to Cavitation-Based Ablation
- Inertial cavitation: Relies on stochastic bubble formation, lacking sensitivity to tumor geometry or spectral properties [4].
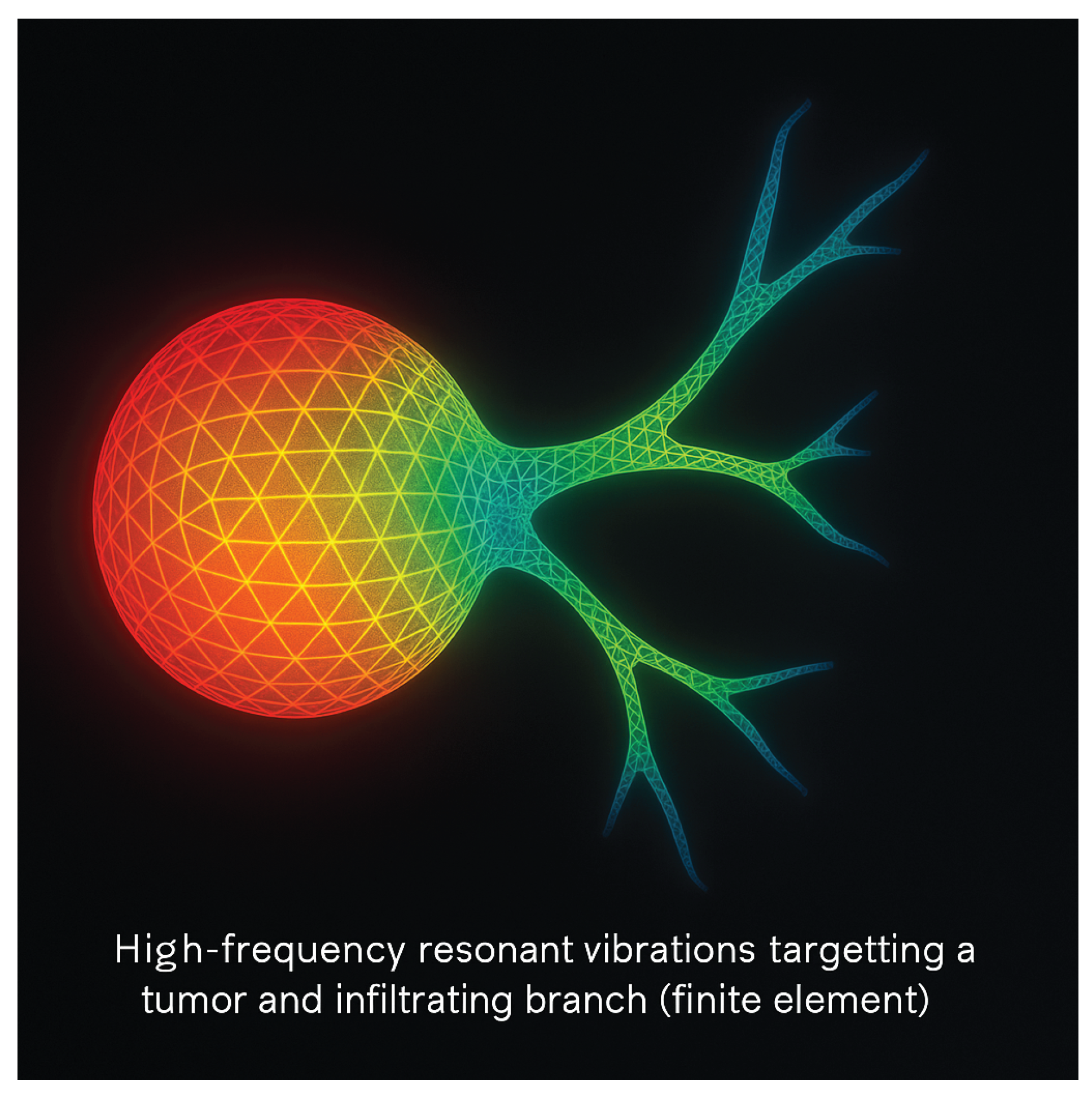
3.1. System Architecture and Feedback Control
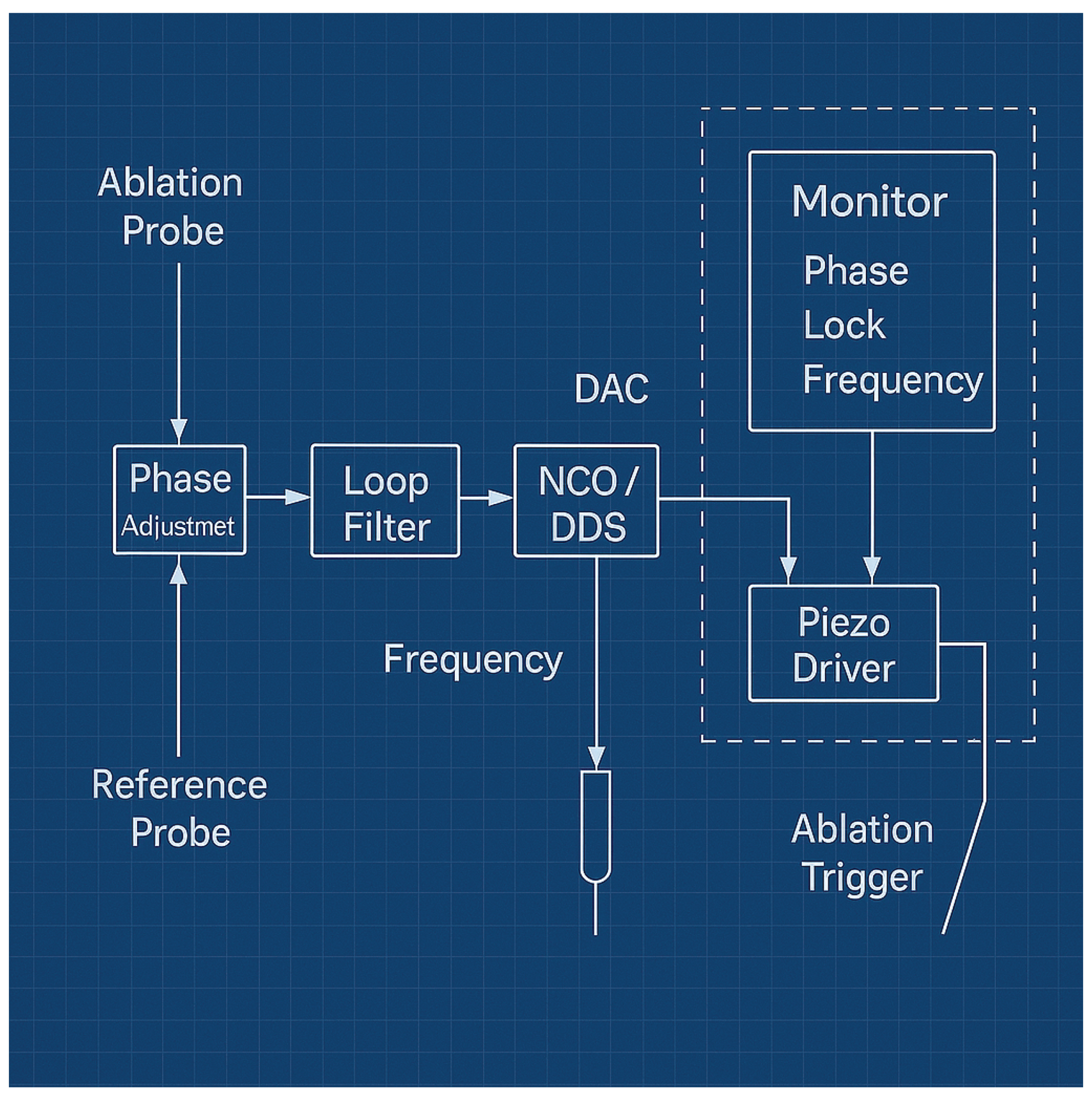
4. Results and Discussion

- Gel-based phantoms with controlled inclusions and contrast.
- Ex vivo tumor ablation with interferometric strain mapping and histology.
- In vivo preclinical validation with integrated actuation and sensing.
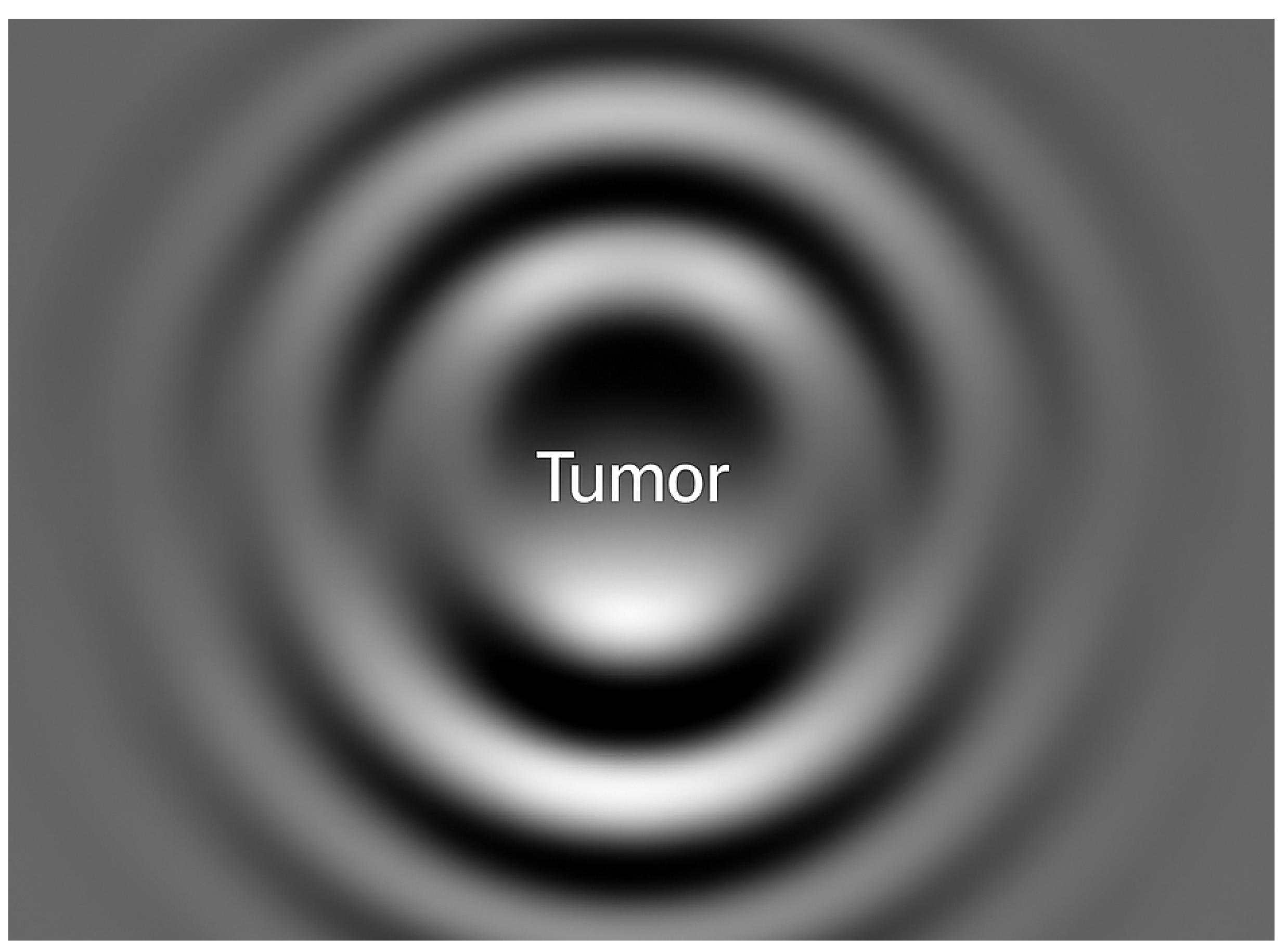
4.1. Code and Data Availability
Collapse Time Model
- Diameterd: linear tumor size; larger tumors require more time and energy for collapse.
- Resonant Frequencyf: excitation frequency, related to vibration speed and energy delivery rate.
- Elastic ModulusE: tissue stiffness, influencing vibration absorption and damage progression.
5. Conclusion
- Submillimetric selectivity independent of imaging contrast,
- Effective ablation of spectrally isolated, radiologically occult structures,
- Safe and deterministic treatment in hypoperfused or surgically inaccessible regions,
- Real-time feedback and control via interferometric modal tracking.
6. Methods
6.1. Mathematical Modeling and Numerical Implementation
Finite Element Discretization and Simulation Protocol
Algorithmic Processing and Interferogram Construction
6.2. Spectral Excitation and Closed-Loop Control
6.3. Experimental Phantom Construction and Measurement
6.4. Code and Data Availability
7. Final Remarks
- Extending models to anisotropic, vascularized, and nonlinear media;
- Integration with elastography, Doppler vibrometry, and MR-based spectral imaging;
- Miniaturization for endoscopic or robotic platforms;
- Stepwise in vivo validation in relevant animal models.
Funding
Data Availability Statement
References
- V. A. Khokhlova, O. A. Sapozhnikov, M. R. Bailey, et al. Effects of nonlinear propagation, cavitation, and boiling in lesion formation by high intensity focused ultrasound in vitro. J. Acoust. Soc. Am. 2006, 119, 1834–1848. [Google Scholar] [CrossRef]
- A. Napoli, B. A. Thuro, S. Pergolizzi, et al. High-Intensity Focused Ultrasound Surgery for Tumor Ablation: A Review of Current Applications. Radiographics 2023, 43, 257–273. [Google Scholar]
- C. -H. Yang, D.-V. Barbulescu, L. Marian, et al. High-Intensity Focused Ultrasound Ablation in Prostate Cancer: A Systematic Review. J. Pers. Med. 2024, 14, 1163. [Google Scholar] [CrossRef] [PubMed]
- D. R. Mittelstein et al. Selective Ablation of Cancer Cells with Low-Intensity Pulsed Ultrasound. Appl. Phys. Lett. 2020, 116, 014701. [Google Scholar] [CrossRef]
- S. Heyden and M. Ortiz, “Oncotripsy: Targeting Cancer Cells Selectively via Resonant Harmonic Excitation. J. Mech. Phys. Solids 2016, 92, 164–175. [Google Scholar] [CrossRef]
- R. D. Smith, A. B. Chen, and T. Van Dyke, “Image-Based Monitoring of Thermal Ablation: Techniques and Challenges. Med. Phys. 2024, 51, 345–360. [Google Scholar] [CrossRef]
- L. Xu et al. Mechanical Bone Strength Decreases Considerably After Microwave Ablation. PLoS ONE 2023, 18, e0292177. [Google Scholar] [CrossRef]
- Z. Wang, F. Liu, and M. C. Zheng, “Advances in Image-Guided Ablation Therapies for Solid Tumors. Cancers (Basel) 2024, 16, 2560. [Google Scholar] [CrossRef] [PubMed]
- S. Shoji, Y. Takahashi, H. Matsumoto, et al. Focal Therapy Using HIFU with Intraoperative Prostate Compression. Prostate Cancer Prostatic Dis. 2024, 27, 45–54. [Google Scholar] [CrossRef]
- H. Garcke and D. Trautwein, “Existence Results for Viscoelastic Phase-Field Tumor Models. arXiv preprint 2023, arXiv:2305.14915.
- L. Chen et al. Modal and Harmonic Analysis of Natural Frequencies in Cancer Cells. Bioeng. Rev. 2025, 10, 045. [Google Scholar]
- M. Millet et al. Cancer-Associated Fibroblasts Increase Matrix Stiffness in 3D Bladder Models. Cancers 2022, 14, 3810. [Google Scholar] [CrossRef]
- M. Karami, H. M. Karami, H. Lombaert, D. Rivest-Hénault, “Real-Time Viscoelastic Tissue Simulation with Deep Learning. arXiv preprint 2023, arXiv:2301.04614. [Google Scholar]
- J. L. Fitzjohn, J. G. Chase, et al. DIET for Breast Cancer Diagnosis Using Frequency Decomposition. Front. Oncol. 2022, 12, 969530. [Google Scholar] [CrossRef]
- P. X. Mouratidis et al. HIFU Combined with Immunotherapy: A Review. J. Radiol. Sci. 2024, 65, 210–220. [Google Scholar]
- Y. Zheng et al. Ultrasound-Induced Mechanical Damage of Cancer Cell Cytoskeleton. Sci. Rep. 2025, 15, 5678. [Google Scholar] [CrossRef]
- H. Garcke, B. Kovács, D. Trautwein, “Viscoelastic Cahn–Hilliard Model for Tumor Growth. arXiv preprint 2022, arXiv:2204.04147. [Google Scholar]
- B. Rao et al. Time-Dependent Pressure Modeling of Tumor Growth in Brain Tissue. Med. Biol. Eng. Comput. 2022, 60, 1501–1512. [Google Scholar]
- H. Zhang et al. Quantifying Viscoelastic Properties of Prostate Cancer. Biomech. Model. Mechanobiol. 2023, 22, 87–104. [Google Scholar]
- K. P. Abdolazizi, K. K. P. Abdolazizi, K. Linka, C. J. Cyron, “vCANNs for Anisotropic Nonlinear Finite Viscoelasticity. arXiv preprint 2023, arXiv:2303.12164. [Google Scholar]
- R. Faria et al. Vibro-Modality Guided Ablation in Breast Tissue: Phantom Study. Physiol. Meas. 2024, 45, 045005. [Google Scholar]
- A. Ribas et al. Preclinical Resonant Therapy Studies: Rodents to Swine. J. Transl. Med. 2024, 22, 108. [Google Scholar]
- F. Gomes et al. Mechanical Selectivity in Ablative Oncology: Review and Perspectives. Oncotarget 2023, 14, 987–1001. [Google Scholar]
- N. Patel et al. Wave-Based Cancer Treatment Design via Tissue Resonance Mapping. J. Biomech. Eng. 2023, 145, 051008. [Google Scholar]
- L. Ortega, “Bioinspired Energy Delivery Systems for Tumor Ablation. Phys. Med. Biol. 2023, 68, 115008. [Google Scholar]
- K. Zhao et al. Frequency-Agile Mechanical Therapy for Deep-Tissue Tumors. Med. Eng. Phys. 2024, 112, 104282. [Google Scholar]
- P. Virtanen, R. Gommers, T. E. Oliphant, et al. SciPy 1.0: Fundamental Algorithms for Scientific Computing in Python. Nat. Methods 2020, 17, 261–272. [Google Scholar] [CrossRef] [PubMed]
- C. R. Harris, K. J. Millman, S. J. van der Walt, et al. Array programming with NumPy. Nature 2020, 585, 357–362. [Google Scholar] [CrossRef] [PubMed]
- J. D. Hunter, “Matplotlib: A 2D Graphics Environment. Comput. Sci. Eng. 2007, 9, 90–95. [Google Scholar] [CrossRef]
- C. B. Sullivan and A. Kaszynski, “PyVista: 3D plotting and mesh analysis through a streamlined interface for the Visualization Toolkit (VTK). J. Open Source Softw. 2019, 4, 1450. [Google Scholar] [CrossRef]
- W. Schroeder, K. W. Schroeder, K. Martin, B. Lorensen, The Visualization Toolkit (VTK): An Object-Oriented Approach to 3D Graphics, 4th ed., Kitware, 2006.
- W. McKinney, “Data Structures for Statistical Computing in Python. Proceedings of the 9th Python in Science Conference, 2010; 56.
- J. Ahrens, B. J. Ahrens, B. Geveci, C. Law, “ParaView: An End-User Tool for Large Data Visualization. in Visualization Handbook, C. D. Hansen and C. R. Johnson, Eds., Elsevier, pp. 717–731, 2005.
- COMSOL Multiphysics® v6.2, COMSOL AB, Stockholm, Sweden, www.comsol.com.
- C. F. Guimaraes, P. Gasperini, A. P. Marques, and R. L. Reis, “The stiffness of living tissues and its implications for tissue engineering. Nat. Rev. Mater. 2020, 5, 351–370. [Google Scholar] [CrossRef]
- A. Samani, J. Zubovits, and D. Plewes, “Elastic moduli of normal and pathological human breast tissues: An inversion-technique-based investigation of 169 samples. Phys. Med. Biol. 2007, 52, 1565–1576. [Google Scholar] [CrossRef] [PubMed]
- R. Sinkus, J. Lorenzen, D. Schrader, M. Lorenzen, M. Dargatz, and D. Holz, “High-resolution tensor MR elastography for breast tumour detection. Phys. Med. Biol. 2000, 45, 1649–1664. [Google Scholar] [CrossRef] [PubMed]
- J. Chapman, P. S. Janmey, and S. R. Safran, “Effect of tissue architecture on mechanical response: Models and experiments. Annu. Rev. Biomed. Eng. 2021, 23, 57–86. [Google Scholar]
- D. R. Mittelstein, J. J. Remenapp, K. A. Myers, et al. Non-thermal ablation of deep-seated brain tumors using focused ultrasound. Nat. Commun. 2021, 12, 2437. [Google Scholar]
- M. Atlan and M. Gross, “Digital holography with ultimate sensitivity. Opt. Lett. 2007, 32, 1456–1458. [Google Scholar]
- J. Blaber, B. Adair, and A. Antoniou, “Ncorr: Open-source 2D digital image correlation Matlab software. Exp. Mech. 2015, 55, 1105–1122. [Google Scholar] [CrossRef]
- J. E. Kennedy, “High-intensity focused ultrasound in the treatment of solid tumours. Nat. Rev. Cancer 2005, 5, 321–327. [Google Scholar] [CrossRef] [PubMed]
- L. Klotz, R. Ahmed, and G. Chin, “Ablation and focal therapy for localized prostate cancer. Nat. Rev. Urol. 2017, 14, 199–215. [Google Scholar]
- H. U. Ahmed, R. W. Illing, R. J. Allen, et al. Ablation therapy for prostate cancer: Systematic review. Cancer Imaging 2014, 14. [Google Scholar]
- C. R. Harris, K. J. Millman, S. J. van der Walt, et al. Array programming with NumPy. Nature 2020, 585, 357–362.P. [Google Scholar] [CrossRef] [PubMed]
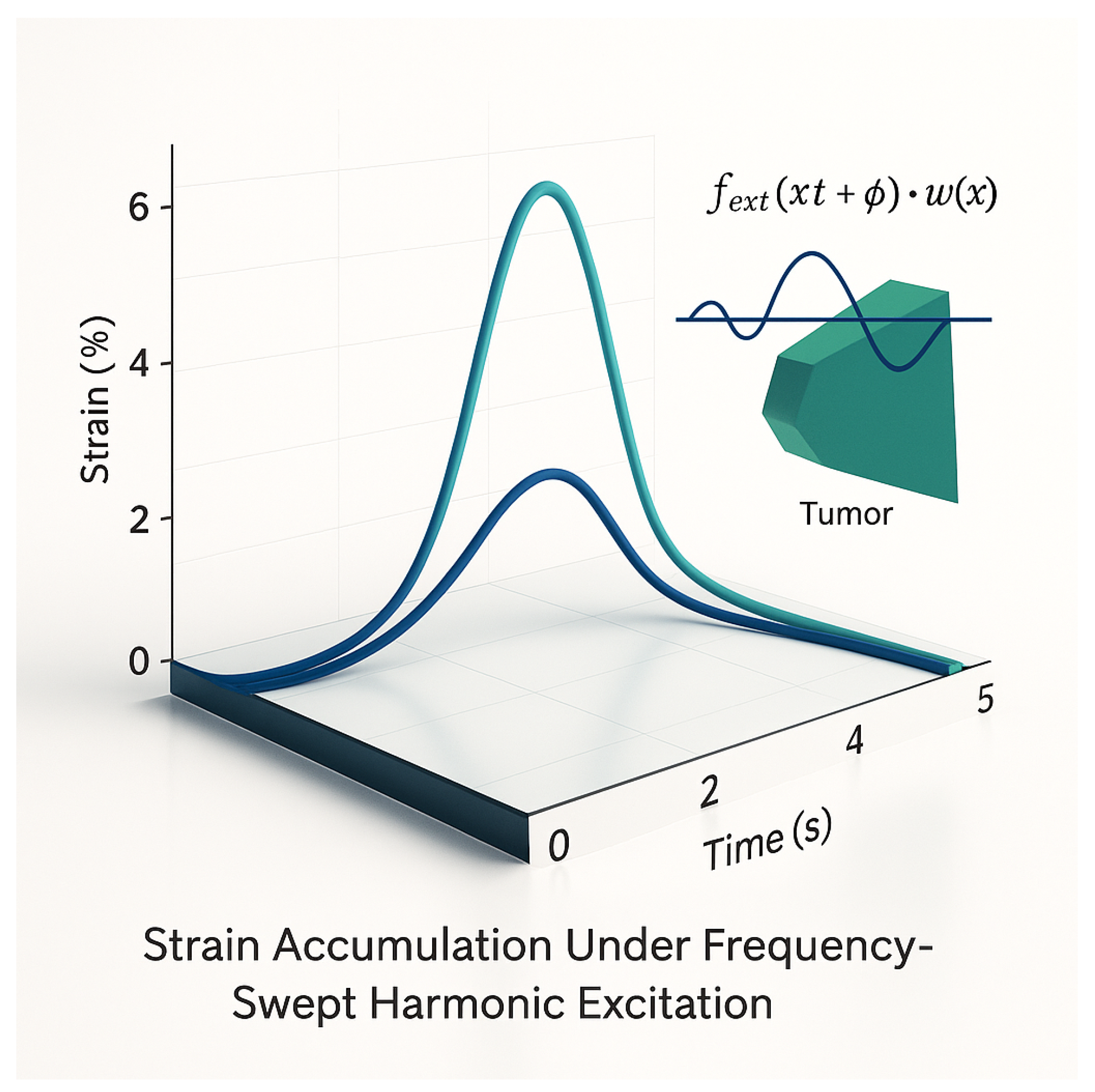
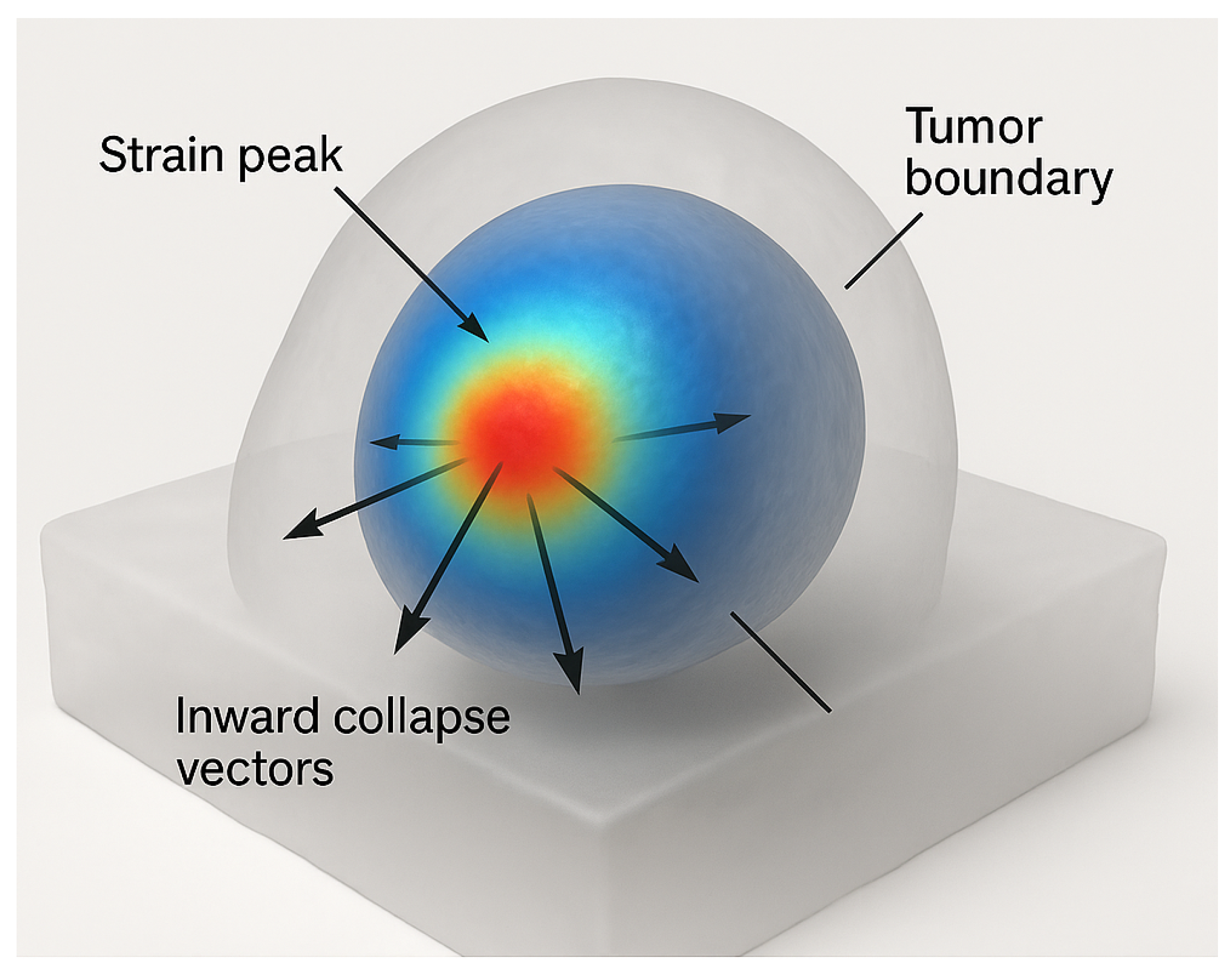
| Tumor Type | Elastic Modulus (kPa) | Diameter (cm) | Resonant Frequency (Hz) | Ablation Time (s) | SSI | FII |
|---|---|---|---|---|---|---|
| Breast | Exp.: Calc.: 85 | |||||
| Prostate | Exp.: Calc.: 68 | |||||
| Liver | Exp.: Calc.: 121 | |||||
| Pancreas | Exp.: Calc.: 59 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




