3. Results
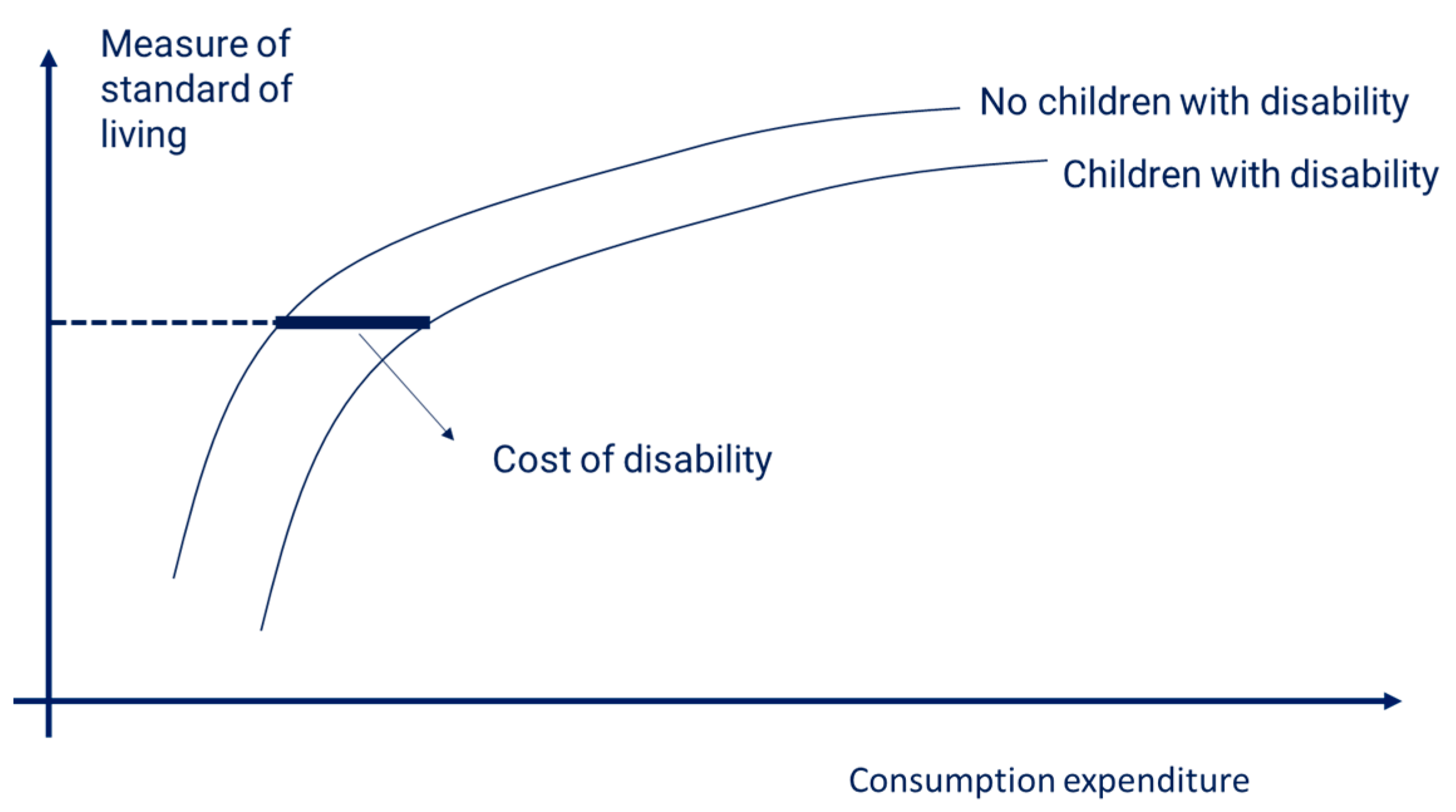
The survey estimated that there are 325,000 children with a disability ID card in the Philippines, but also that there are many other children with functional difficulties without a disability ID card. In summary, findings show families with children with disabilities experience systematic disadvantage in comparison to families with children without disabilities. Highest rates of disadvantage were found among children with disabilities who did not have a disability ID card. The highest additional costs were on health expenditure with families of children with disabilities spending three times more than other families. Depending on the severity of disability, a child with disabilities in the Philippines requires 40% to 80% higher expenditure to reach the same standard of living as a child without disabilities. Recognizing the extra costs of disability implies that poverty rates among households with children with disabilities are at least 25% higher than what ignoring these extra costs would reveal. After taking the extra costs into account households with children with disabilities have poverty rates (percentage of poor) that are 50% higher than those of other households with children.
3.1. Quantitative findings
Table 1 reports the distribution of household types separating households with at least one child with functioning difficulties and households with children without disabilities. The table also shows the average number of children with functional difficulties in households with at least one child with functional difficulties. Nuclear families, or households composed exclusively of parents and children, represent almost two thirds of all households with children. Other households are three generation households, with grandparents, and complex household types, for example where the parents’ siblings are present or parents of at least one of the children are not in the household. There are not large differences between household types with or without children with disabilities; however, within nuclear family households with children with disabilities there tend to be more children. The average number of children with disabilities in the household is 1.16.
Table 2 shows basic descriptive statistics for households with and without children with disabilities and separates nuclear families from other types of households. All main variables used in the analysis are included: consumption expenditure in logarithm terms, the age of the household head, the household size, the location of the household and then the three variables chosen to capture the living standards. These are the asset index, the number of deprivations, and self-reported poverty position.
3.2. Regression results
Several regressions were estimated restricting the sample to certain household types, using different measures of disability (ownership of disability card and functional difficulty) and different measures of living standards. The results that prove more consistent and where it is easier to derive the extra cost for a child with disabilities comes from the sample of nuclear families (two thirds of our sample) and use of functional difficulties, including the advantage of being able to distinguish the severity of disability by reported difficulty.
Results of the regressions are reported in
Table 3 together with the estimated implications of proportional extra expenditure required by the household with a child with disability to reach the same living standards of other households.
In all three models, consumption expenditure is positively correlated with the living standard measure and highly significant. Also, as predicted, the measure of disability has negative coefficients, which are consistently highly significant in the case of moderate/severe functional difficulties and smaller and with lower degree of accuracy in the case of milder functional difficulties. In terms of other explanatory variables, significant variables are similar across the asset index model and the number of deprivations model but differ in terms of the self-reported position in society model. This latter model also has a very low explanatory power suggesting a significant level of inaccuracy in the values reported for this question.
Estimates of the proportional higher expenditure incurred by families with a child with disability are different when we compare the results using the asset index coefficients and the other two models. Across all models, moderate/severe functional difficulties involve twice as much extra expenditure compared to milder functional difficulties. Much higher differences in expenditure are obtained from the models using deprivations and position in society compared to the asset index.
The proportional extra expenditure reported in
Table 3 is at the household level, and estimating this at the level of the child requires making some further assumptions. In the Philippines when computing poverty estimates, income and consumption measures are simply divided by the household size. Therefore, in the case of the model using the asset index as the indicator of living standards, transforming the household level extra cost of 19% when there are children with moderate/severe functional difficulties means that the extra expenditure per child with functional difficulties can be estimated dividing by the ratio of the average number of such children and the average household size. This results in an estimate of approximately 80% extra expenditure.
Based on the estimate of extra expenditures above, we can assume that the equivalence scales for a child with moderate/severe functional difficulties is 1.8, and that for those with milder functional difficulties is 1.4. Using these equivalence scales in computing an adjusted measure of consumption results in significantly increasing poverty measures for such households. In our sample, poverty estimates for households with children who have functional difficulties increase by more than 25% relative to estimates that do not take into account the extra costs faced by children with disabilities, so that when comparing poverty rates of households with children with disabilities and other households with children their poverty rate is about 50% higher.
Analysis of consumption patterns across families with and without children with disabilities clearly showed the main sources of extra costs. The share of household budget spent on health by households with a child with disabilities is three times higher than for households with children without disabilities. Moreover, even though one third of children with disabilities are not enrolled in school, the share of education expenditure is higher among families with children with disabilities compared to other households with children. Other costs frequently cited to be higher for people with disabilities are transportation costs. This was clearly identified in qualitative interviews, but significant differences were not found in the quantitative survey. Alongside what may be prohibitive transportation costs for some, the timing of the fieldwork may have been a contributing factor as movements were restricted because of lockdowns and school closures.
3.3. Health expenditure
As shown from household survey data, highest costs related to health. Reported cost items from qualitative interviews included routine and specialist consultations, surgery, maintenance medicines, nutitional supplements, and the sourcing, fitting and maintenance of assistive devices. These were additional to the routine health costs experienced by children with and without disabilities. Highest reported costs were for specialist diagnoses and surgery at tertiary facilities, with costs in the tens of thousands of (US) dollars reported. Routine check ups were a significant source of expenditure with frequent visits (up to three times a week) to multiple specialists.
Medications were noted as the highest cost for households of children with chronic health conditions. A few respondents could source cheaper medicines, including directly from manufacturers or through contacts with medical professionals or local politicians. Vitamin supplements were commonly prescribed and expensive. Further costs included purchase of blenders, and electricity, and time and expense of individually prepared food. While an example of the use of feeding tubes was reported, simple assistive products were rarely used. For example, feeding chairs to support a child while eating.
Overall, knowledge of assistive products and devices was low. Parents often became aware of assistive products through informal sources or by chance. For example, through seeing another person using a product, including on Tik Tok. Families reported being unable to, or assumed they were unable to, afford assistive products. A family described paying significant optometrist fees and then being unable to afford the recommended glasses. Use of one assistive product did not preclude unmet needs for other products. The appropriateness and safety of existing assistive products was questioned, and costs of maintenance and replacement noted. Information was also scarce. For example, parents of a child who had outgrown her prosthetic leg did not know how to contact the charity that provided it. Buying assistive products from online market places was noted as was the use of second hand products. The use of homemade assistive products, such as canes and handrails from wood or bamboo was reported.
3.4. Adaptations to home
Adaptations to homes reduce physical barriers and promote independent use of the home by the child. Few families had adapted their homes. Adaptations were difficult in rented accomodation as they required landowner’s consent and making adaptations was often not prioritised in the face of competing demands for financial resources and time.
Reported adaptations included installing a new toilet, installing a concrete floor to aid mobility, and constructing a sleeping platform. A family reported they were rebuilding their home to provide additional space and privacy for their child. Another example was a family who wanted to install child-safe electrical sockets for their child but had not yet been able to do so. Other adjustments included purchase of mattress toppers and installation of air conditioning. Another family explained how they kept lights in their house on to assist their child with low vision. Costs of electrical bills for the air conditioner and lighting examples were considered very high.
3.5. Costs of education and learning
Not all children were enrolled in school. Among children aged 5 to 17 with a disability ID card and at least some functional difficulties enrollment was 66%, whereas enrolment among children without functional difficulties and without disability ID card was 96%. Additional costs of attending school for children with disabilities included higher fees for some special education (SPED) schools, noting the Philippines does not yet have a comprehensive system of inclusive education, and the need for a shadow, or support, teacher. Examples of the costs of a shadow teacher needing to be shared between families were reported.
Costs of travel were cited as a frequent concern across all domains, but particularly for daily school attendance. This included having to travel further to access a school with a SPED programme or, simply, to a school that would accept their child. Accompanying a child to and from school increased expenditure on public transport as well as opportunity costs of forgone work with some parents staying at the school throughout the day to support their child. A lack of reasonable accomodation was reported with simple adjustments not implemented, such children with visual impairments being seated at the back of a class. Administrative barriers to annual reenrollment each year, such as being asked to provide medical certificates, were noted.
Social costs included bullying by pupils and parents without disabilities. For example, bulling by a parent who could not accept a child with disabilities could perfom better than their child without disabilities. Also, an incident of physical assault by a teacher on a child with disabilities that led to the parents’ withdrawing their child from school. Limited social interaction and opportunities for play were reported, including parents not allowing their child outside for fear they may become sick. Overall, there was limited expenditure on play items, but the use of downloaded or online games for mobile devices was noted.
During COVID-19, remote learning was not provided by all schools. Families accessing remote learning paid extra for modules and tests. It was noted that the modules could leave a child under stimulated and bored. The example of a child with psychosocial disability attending a private SPED school was noted ads the household’s ‘heaviest expense’. The school reduced fees under COVID-19, but any savings were offset by having to buy a laptop and accessories for online learning.
3.6. Costs of care
Costs of care included financial and non-financial costs, including forgone social or economic opportunities. Care was predominantly, but not exclusively, provided by women. Primary and secondary carers included siblings, grandparents, and other family members. Care could be provided to more than one child with disabilities in a household. Among households with children with moderate/severe functional difficulties, in 24% of cases there was more than one child with functional difficulties. Qualitative interview responses shed further light on care. For example, two households had hired an outside carer at one point. In one case the cost had been paid by a relative and in the other the household could not afford to continue paying the carer. Absent parents with no further contact with the child or family were reported. Carers emphasised their role was not ‘baby sitting’ and was a full-time support role. Older carers were concerned over the future of the child with disabilities that would survive them.
No carers reported receiving emotional support for themselves or respite care. The need for additional support, such as moving a heavier or older, was noted; however, one respondent noted it was hard to trust others to provide this help. Opportunity costs included having to give up work; lost income, such as from selling goods outside of the busiest hours; and moving to lower paid jobs for more flexible work hours. One mother reported having to pay extra for ice to keep her fish fresh for sale while she accompanied her child to school. Work could be missed for extended periods when a child needed health care, particularly for travel to tertiary healthcare facilities. Two people may be needed to assist moving a child adding to travel costs and accompanying siblings miss school. Not having relatives in urban areas could result in additional costs for accomodation and food.
3.7. Allied health costs
Three composite stories were developed to illustrate potental additional health expenditure from birth to 18 years old. These were based on scenarios of ‘full intervention’, including consultations, including with multiple specialists; check-ups; medications; and assistive devices with fitting, maintenance, and replacement. Scenarios were based on services available in the Philippines; however, this does not mean all services were accessible or available in all areas. While households often underestimated these potential costs, allied professionals could overestimate, including overprescribing frequency of consultations, in their calculations. As such, the following are high end cost scenarios.
For a child with spina bifida, total health cost estimates to a family before adulthood could be in the region of USD 39,000. We also considered mulitple impairments. For a child with intellectual disability, autism, and hearing impairment the estimates reached USD 46,500. The scenario for a child with cerebral palsy and epilepsy resulted in an estmate of USD 90,000. Costs vary over time and may increase or decrease with the age of the child. These estimates are costs to the household and assume no health insurance, deductions, or other financial support. Calculations based on actual health expenditure from the household survey are assumed lower and to be based on access to a limited suite of health services.