1. Introduction
Hypernatremia is an electrolyte disorder characterized by an elevation of serum sodium concentration above 145 mmol/L, reflecting a state of relative water deficit. Although relatively uncommon in the general population, hypernatremia is disproportionately observed among older adults and is consistently associated with adverse clinical outcomes, including prolonged hospitalization, functional decline, and increased mortality. In geriatric patients, hypernatremia often develops in the context of frailty, cognitive impairment, functional dependency, and a reduced ability to maintain adequate oral fluid intake [
1,
2].
Previous studies have shown that hypernatremia in older adults is frequently not an isolated biochemical abnormality but rather a clinical marker of severe vulnerability. Factors such as impaired thirst perception, dysphagia, dependency for basic activities of daily living, and polypharmacy contribute to its development and persistence. Several hospital-based cohorts have reported markedly increased short- and medium-term mortality among elderly patients with hypernatremia, suggesting that this condition may reflect advanced physiological reserve depletion rather than a reversible electrolyte imbalance alone [
3,
4,
5].
Hospital-at-Home (HaH) programs have expanded substantially in recent years as an alternative to conventional hospitalization, particularly for older patients with complex chronic conditions. These programs aim to provide hospital-level care in the patient’s usual environment, either at home or in long-term care facilities, while reducing hospital-related complications. However, patients managed through HaH are often highly dependent, cognitively impaired, and clinically fragile, placing them at increased risk of hydration-related disorders. Despite this, data on the epidemiology and clinical impact of hypernatremia in HaH settings remain scarce [
6].
Moreover, important differences may exist between patients receiving HaH care in their own homes and those institutionalized in nursing homes or long-term care facilities. Institutionalized patients frequently present with more advanced functional and cognitive impairment, higher levels of dependency, and limited autonomy in fluid intake, which may further increase the risk of hypernatremia and associated mortality. Understanding these differences is essential to tailor preventive strategies and optimize care models in both settings [
7].
Therefore, the aim of this study was to evaluate the prevalence, clinical characteristics, and short- and medium-term mortality associated with hypernatremia in a large cohort of patients managed through a Hospital-at-Home unit. We specifically compared patients treated at home with those treated in institutional settings, hypothesizing that hypernatremia would be more prevalent and associated with worse outcomes among institutionalized patients, reflecting a higher degree of underlying frailty [
8].
2. Materials and Methods
2.1. Study Design
We conducted a retrospective observational cohort study including all patients admitted to the Hospital-at-Home (HaH) unit of Hospital Universitario Infanta Cristina between January 2019 and December 2024. The study was designed to evaluate the prevalence and clinical impact of hypernatremia in older adults receiving hospital-level care in non-conventional settings.
2.2. Setting and Participants
The Hospital-at-Home unit provides acute and subacute hospital care to patients either in their private homes or in long-term care facilities, including nursing homes and residential institutions. Eligible patients were classified into two cohorts according to the care setting:
All consecutive patients admitted during the study period were included. No additional exclusion criteria were applied, ensuring a real-world representation of HaH activity.
2.3. Variables and Definitions
Sociodemographic variables included age and sex. Functional status was assessed using the Barthel Index, with lower scores indicating greater functional dependency. Cognitive status was evaluated using the Global Deterioration Scale (GDS). Polypharmacy was defined as the regular use of five or more medications.
Hypernatremia was defined as a serum sodium concentration >145.00 mmol/L at any point during HaH admission and was further classified as mild, severe, or extreme according to established thresholds. Clinical complications frequently associated with frailty were recorded, including dysphagia, aspiration events, and pressure ulcers [
9,
10].
2.4. Outcomes
The primary outcome was all-cause mortality during HaH admission and at 30, 60, and 90 days after the diagnosis of hypernatremia. Secondary outcomes included the prevalence of hypernatremia in each care setting and the association between hypernatremia and functional, cognitive, and clinical characteristics.
2.5. Statistical Analysis
Continuous variables are presented as mean ± standard deviation or median and interquartile range, as appropriate. Categorical variables are expressed as absolute numbers and percentages. Comparisons between groups were performed using Student’s t-test or Mann–Whitney U test for continuous variables and test for categorical variables.
Survival analysis was performed using Kaplan–Meier curves, with differences assessed by the log-rank test. Multivariable Cox proportional hazards regression models were constructed to evaluate the association between hypernatremia and mortality, adjusting for age, sex, functional status (Barthel Index), cognitive impairment (GDS), and care setting (home vs institutional). Results are presented as hazard ratios (HRs) with 95% confidence intervals (95% CI). A two-sided p value < 0.05 was considered statistically significant. Statistical analyzes were performed using standard statistical software [
11].
2.6. Ethical Considerations
The study was approved by the local Research Ethics Committee (Code: PI 05/24 of 8, January 2024) of Hospital Puerta de Hierro - Majadahonda and conducted in accordance with the Declaration of Helsinki. Due to the retrospective nature of the study, informed consent was waived.
3. Results
3.1. Study Population
A total of 4.501 patients were admitted to the Hospital-at-Home unit during the study period. Of these, 2.701 (60.0%) were treated in their own homes (HaH-home), while 1.800 (40.0%) received care in institutional settings (HaH-institution). Baseline characteristics by care setting are shown in
Table 1.
Institutionalized patients were significantly older than home-dwelling patients (90.10 ± 8.00 vs. 69.50 ± 18.0 years) and presented with markedly higher levels of functional dependency and cognitive impairment, as reflected by lower Barthel Index scores and higher Global Deterioration Scale stages.
3.2. Prevalence of Hypernatremia
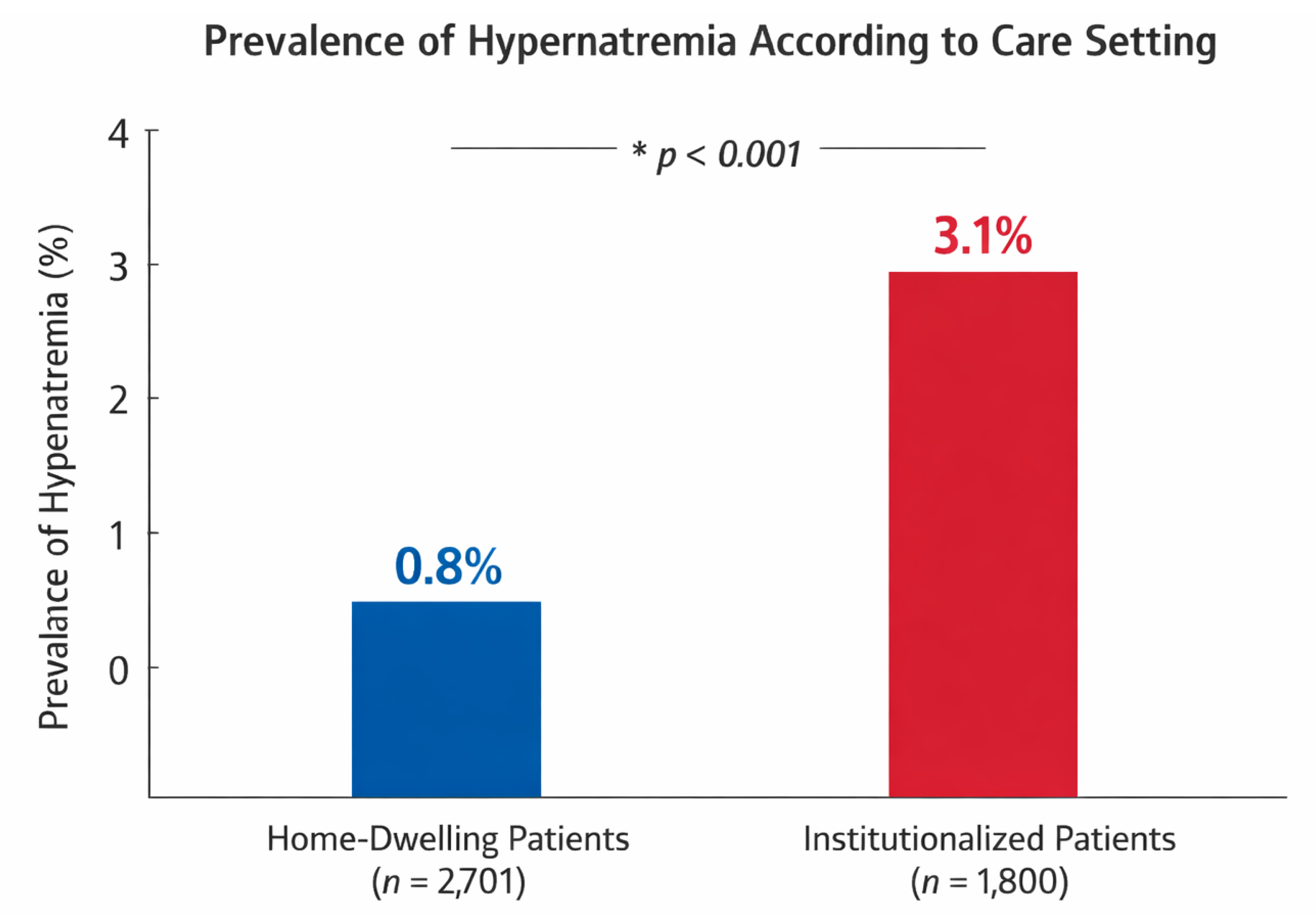
The overall prevalence of hypernatremia differed significantly between care settings. Hypernatremia was identified in 0.80% of patients treated at home and in 3.10% of institutionalized patients (p < 0.001).
Among home-dwelling patients, those who developed hypernatremia were older and significantly more functionally dependent than non-hypernatremic patients (82 ± 14 vs. 69 ± 18 years; Barthel Index 39 ± 37 vs. 83 ± 27; both p < 0.001).
Figure 1.
Prevalence of hypernatremia according to care setting in the Hospital-at-Home cohort. Hypernatremia was significantly more prevalent among institutionalized patients (3.1%) than home-dwelling patients (0.8%; p < 0.001; HaH-home: n = 2701; HaH-institution: n = 1800).
Figure 1.
Prevalence of hypernatremia according to care setting in the Hospital-at-Home cohort. Hypernatremia was significantly more prevalent among institutionalized patients (3.1%) than home-dwelling patients (0.8%; p < 0.001; HaH-home: n = 2701; HaH-institution: n = 1800).
In contrast, among institutionalized patients, age did not significantly differ between those with and without hypernatremia (88.4 ± 8.2 vs. 90.4 ± 7.9 years). However, hypernatremic institutionalized patients showed significantly greater functional dependency, more advanced cognitive impairment, and a higher proportion of women compared to their non-hypernatremic counterparts (
Table 1).
3.3. Clinical Characteristics of Institutionalized Patients with Hypernatremia
A total of 84 institutionalized patients with hypernatremia were identified. Mean serum sodium concentration was 160.00 mmol/L (range: 146.00–189.00), and 32.00% of patients presented with extreme hypernatremia (>165 mmol/L).
This subgroup exhibited severe frailty, with a mean Barthel Index of 11.6 and advanced cognitive impairment (mean GDS 5.8). Polypharmacy was common, with a median of six medications per patient. Frequent clinical complications included dysphagia (43.5%), aspiration events (32.9%), and pressure ulcers (30.6%) (
Table 2).
Table 2.
Characteristics of institutionalized Hospital-at-Home patients according to hypernatremia status.
Table 2.
Characteristics of institutionalized Hospital-at-Home patients according to hypernatremia status.
| Variable |
No hypernatremia (n = 1743) |
Hypernatremia (n = 57) |
p value |
| Age, years, mean ± SD |
90 ± 8 |
88 ± 8 |
NS |
| Male sex, % |
25 |
21 |
NS |
| Barthel Index, mean |
15 |
11 |
0.041 |
| GDS stage, mean |
5.5 |
6.0 |
0.033 |
Table 3.
Clinical characteristics and mortality according to severity of hypernatremia in institutionalized patients.
Table 3.
Clinical characteristics and mortality according to severity of hypernatremia in institutionalized patients.
| Variable |
Mild (146–155) |
Severe (156–165) |
Extreme (>165) |
p value |
| |
n = 35
|
n = 22
|
n = 27
|
|
| Age, years, mean |
88 |
89 |
88 |
NS |
| Barthel Index, mean |
12 |
13 |
10 |
NS |
| GDS stage, mean |
6 |
6 |
6 |
NS |
| In-hospital mortality, % |
37 |
27 |
33 |
NS |
| 30-day mortality, % |
74 |
41 |
63 |
0.041 |
3.4. Mortality and Survival Analysis
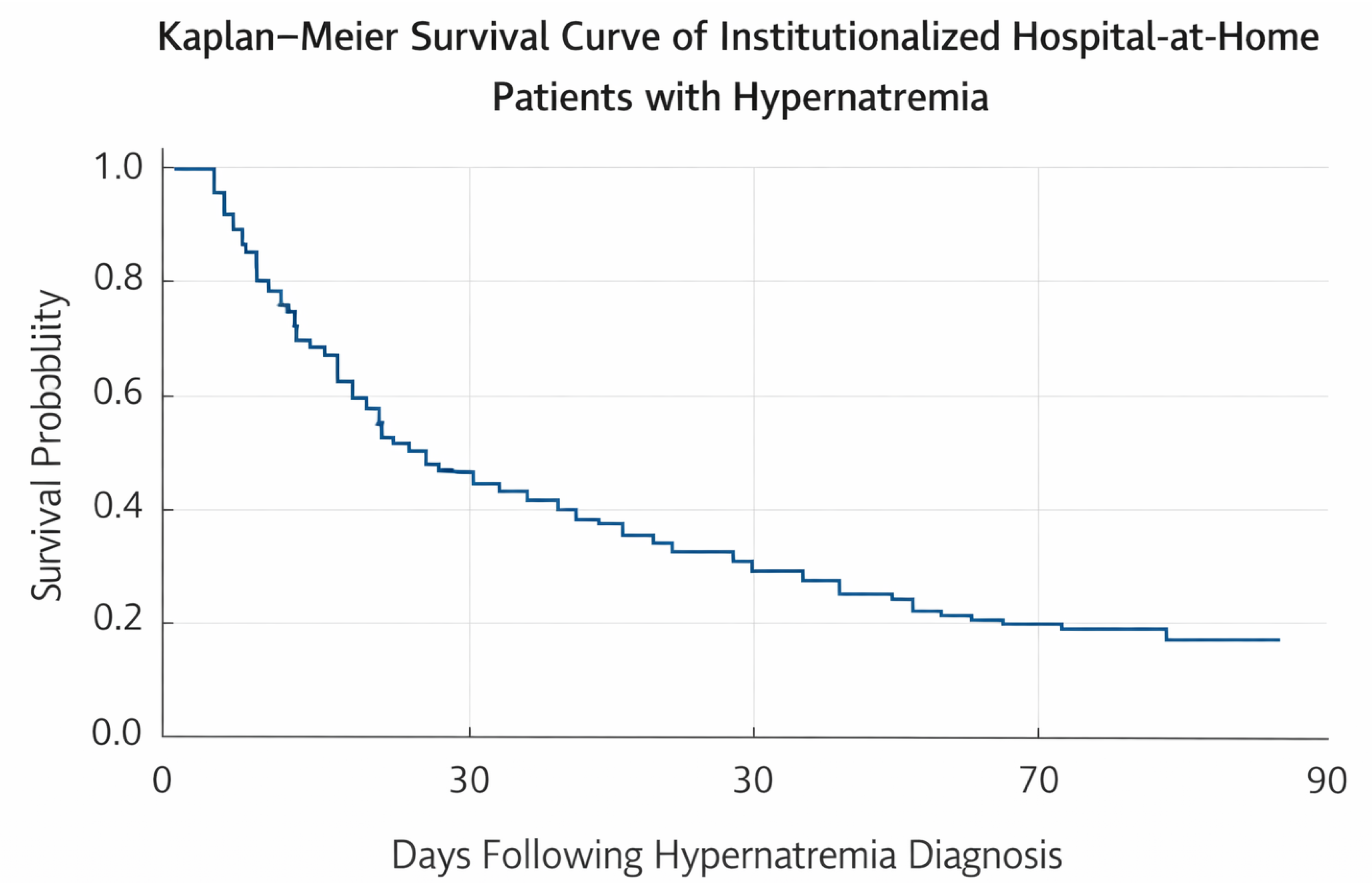
Mortality among institutionalized patients with hypernatremia was high. In-hospital mortality during HaH admission was 32.90%. Cumulative mortality increased to 61.20% at 30 days, 70.60% at 60 days, and approximately 79% at 90 days.
Kaplan–Meier survival analysis demonstrated a rapid decline in survival during the first month following hypernatremia diagnosis, with a trend toward poorer outcomes among patients with higher sodium levels (
Figure 2).
In multivariable Cox regression analysis adjusted for age, sex, functional dependency, cognitive impairment, and care setting, hypernatremia remained strongly associated with increased mortality (
Table 4).
4. Discussion
In this large real-world cohort of patients managed through a Hospital-at-Home (HaH) program, hypernatremia was an infrequent but clinically significant finding, particularly among institutionalized older adults. Our results demonstrate that hypernatremia was significantly more prevalent in institutional settings than among patients treated at home (3.1% vs. 0.8%) and was associated with profound functional dependency, advanced cognitive impairment, and extremely high short- and medium-term mortality. These prevalence figures align with prior reports from hospital settings, where hypernatremia affects 1–3% of older patients, rising to 10–12% among those admitted from nursing homes [
12,
13,
14,
15].
These findings are consistent with previous hospital-based studies reporting hypernatremia as a strong predictor of adverse outcomes in older adults. For instance, large cohorts have documented mortality rates of 30–45% in hypernatremic elderly patients during hospitalization, escalating to over 70% in ICU or sepsis contexts, comparable to our 79% 90-day rate in institutionalized HaH patients. However, our study extends existing knowledge by specifically focusing on the HaH setting, an increasingly important model of care for frail elderly patients. In this context, hypernatremia appears less as an isolated electrolyte disturbance and more as a clinical marker of advanced vulnerability and physiological reserve depletion [
3,
8,
11,
12,
14].
The comparison between home-dwelling and institutionalized patients provides important insights. While age and dependency were both associated with hypernatremia in home-dwelling patients, age alone did not discriminate risk among institutionalized patients. Instead, functional dependency and cognitive impairment emerged as the main distinguishing factors. This pattern mirrors data from care home cohorts, where nursing home residents showed a 10-fold higher hypernatremia risk (12% vs. 1.3% in own-home patients), largely attributable to dementia and dependency, even after multivariable adjustment. This observation supports the concept that biological frailty and neurocognitive dysfunction, rather than chronological age, are key determinants of hydration-related disorders in older adults [
11,
12,
13,
16].
Mortality among institutionalized patients with hypernatremia was strikingly high, approaching 80% at three months. The Kaplan–Meier survival analysis revealed a rapid decline in survival during the first month following diagnosis, highlighting the particularly poor short-term prognosis. Importantly, mortality did not differ significantly according to the degree of hypernatremia severity, suggesting that even moderate elevations in serum sodium may reflect a critical underlying clinical state. This is consistent with geriatric literature viewing hypernatremia not as a direct cause of death but as an indicator of inadequate care, severe frailty, or depleted physiological reserves in institutionalized settings. This reinforces the interpretation of hypernatremia as a marker of advanced frailty rather than a direct causal factor of death [
3,
7,
11,
12,
14].
From a clinical and organizational perspective, these findings have relevant implications for HaH programs and long-term care facilities. Institutionalized patients often depend entirely on caregivers for fluid intake and basic needs, and subtle reductions in hydration may go unnoticed until severe biochemical disturbances develop. Studies in care homes link hypernatremia to preventable dehydration, with population-attributable fractions up to 36% for hospital admissions and 85% for in-hospital deaths. Early identification of patients at risk, systematic monitoring of fluid intake, and proactive hydration strategies may help prevent the development of hypernatremia or allow earlier intervention. Furthermore, prompt correction protocols are essential, as delayed or overly rapid management exacerbates outcomes. Furthermore, in patients with advanced dependency and cognitive impairment, the detection of hypernatremia should prompt a comprehensive reassessment of goals of care, including the timely integration of palliative approaches when appropriate [
12,
13,
15,
16,
17].
5. Limitations
Several limitations of this study should be acknowledged. First, its retrospective observational design precludes the establishment of causal relationships between hypernatremia and mortality. Second, the study was conducted in a single HaH unit, which may limit generalizability to other healthcare systems with different organizational structures or patient profiles. Third, detailed data on fluid intake, thirst perception, and caregiver-related factors were not available, preventing a more granular analysis of the mechanisms leading to hypernatremia. Finally, although functional and cognitive status were systematically assessed, other potential confounders such as comorbidity burden or inflammatory markers were not included in multivariable analyzes.
Despite these limitations, the large sample size, real-world setting, and consistent assessment of functional and cognitive variables strengthen the validity of our findings.
6. Future Directions
Future research should focus on prospective studies aimed at identifying early predictors of hypernatremia in HaH and institutionalized populations. The development and evaluation of structured hydration monitoring protocols, combined with caregiver education, may help reduce the incidence of this complication. Additionally, integrating hypernatremia into frailty assessment frameworks could improve risk stratification and decision-making in advanced care planning. Multicenter studies are also warranted to confirm our findings and explore potential differences across healthcare systems and models of HaH delivery.
7. Conclusions
Hypernatremia was significantly more prevalent among institutionalized patients receiving Hospital-at-Home care than among those treated in their own homes. In institutional settings, hypernatremia was closely associated with severe functional dependency, advanced cognitive impairment, and extremely high short- and medium-term mortality. These findings suggest that hypernatremia should be regarded as a marker of advanced frailty rather than an isolated electrolyte abnormality. Strengthening preventive strategies and hydration monitoring in HaH programs and long-term care facilities may help improve care quality and support timely, patient-centered decision-making in this vulnerable population.
Author Contributions
Conceptualization, J.A. and A.E.; methodology, M.C and P.C-R.; software, J.A and S.N-P.; validation, P.C-R., S.N-P. and P.C-R.; formal analysis, J.A.; investigation, P.G-T and Y-M-C; resources, P.C.; data curation, J.A.; writing—original draft preparation, M.C.; writing—review and editing, S.N-P and F.G.; visualization, F.G.; supervision, P.C. and P.G.; project administration, M.C.; funding acquisition, F.G. All authors have read and agreed to the published version of the manuscript.
Funding
The APC was funded through the funds of the IDIPHISA Foundation (Research Institute of the Puerta de Hierro University Hospital), with which the Infanta Cristina University Hospital in Madrid was
Institutional Review Board Statement
The study was approved by the local Research Ethics Committee (Code: PI 05/24 of 8, January 2024) of Hospital Puerta de Hierro - Majadahonda and conducted in accordance with the Declaration of Helsinki.
Informed Consent Statement
Patient consent was waived due to the retrospective nature of the study, informed consent was waived.
Data Availability Statement
The original contributions presented in this study are included in the article. Further inquiries can be directed to the corresponding author.
Acknowledgments
During the preparation of this manuscript, the authors used Perplexity AI for improving the English language editing, academic redaction, and translation from Spanish drafts. The authors have reviewed and edited the output and take full responsibility for the content of this publication.
Conflicts of Interest
The authors declare no conflicts of interest.
Abbreviations
The following abbreviations are used in this manuscript:
| HaH |
Hospital at Home |
| DOAJ |
Directory of open access journals |
| TLA |
Three letter acronym |
| LD |
Linear dichroism |
References
- Palevsky, P.M.; Bhagrath, R.; Greenberg, A. Hypernatremia in hospitalized patients. Annals of Internal Medicine 1996, 124, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Adrogué, H.J.; Madias, N.E. Hypernatremia. New England Journal of Medicine 2000, 342, 1493–1499. [Google Scholar] [CrossRef] [PubMed]
- Chassagne, P.; Druesne, L.; Capet, C.; Ménard, J.F.; Bercoff, E. Clinical presentation of hypernatremia in elderly patients: a case control study. Journal of the American Geriatrics Society 2006, 54, 1225–1230. [Google Scholar] [CrossRef] [PubMed]
- Tolea, M.I.; Morris, J.C.; Galvin, J.E. Dysnatremia in relation to frailty and age in community-dwelling adults in the National Health and Nutrition Examination Survey. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences 2017, 72, 376–382. [Google Scholar] [CrossRef]
- Corona, G.; Giuliani, C.; Parenti, G. Moderate hyponatremia is associated with increased risk of mortality: a systematic review and meta-analysis. European Journal of Endocrinology 2014, 170, 745–752. [Google Scholar] [CrossRef]
- Liamis, G.; Filippatos, T.D.; Elisaf, M.S. Evaluation and treatment of hypernatremia: a practical guide for physicians. Postgraduate Medicine 2016, 128, 299–306. [Google Scholar] [CrossRef] [PubMed]
- Wolff, A.; Stuck, A.E.; et al. Are patients admitted to hospitals from care homes dehydrated? A retrospective cohort study to develop a predictive model. Journal of the Royal Society of Medicine 2015, 108, 259–261. [Google Scholar] [CrossRef] [PubMed]
- Torrens, M.; et al. Hypernatremia in hospitalized patients: a large population-based study. Kidney360 2022, 3, 649–659. [Google Scholar] [CrossRef] [PubMed]
- Spasovski, G.; Vanholder, R.; Allolio, B. Clinical practice guidelines on diagnosis and treatment of hyponatraemia. Nephrology Dialysis Transplantation 2014, 29, i1–i39. [Google Scholar] [CrossRef] [PubMed]
- Burst, V. Hyponatremia and hypernatremia: A practical approach to disorders of sodium and water balance. Deutsches Ärzteblatt International 2015, 112, 745–752. [Google Scholar] [CrossRef]
- Wald, R.; Jaber, B.L.; Price, L.L.; Upadhyay, A.; Madias, N.E. Impact of hospital-associated hyponatremia and hypernatremia on mortality. Archives of Internal Medicine 2010, 170, 294–302. [Google Scholar] [CrossRef] [PubMed]
- Snyder, N.A.; Feigal, D.W.; Arieff, A.I. Hypernatremia in elderly patients. A heterogeneous, morbid, and iatrogenic entity. Annals of Internal Medicine 1987, 107, 309–319. [Google Scholar] [CrossRef] [PubMed]
- Assadi, F. Hypernatremia in the geriatric population. Clinical Interventions in Aging 2014, 9, 1987–1992. [Google Scholar] [CrossRef] [PubMed]
- Arampatzis, S.; Frauchiger, B.; Fiedler, G.M.; Leichtle, A.B.; Otto, T.; Ramineni, S.; Benz, C.; Schwarz, C. Characteristics, symptoms and outcome of severe dysnatremias present on hospital admission. The American Journal of Medicine 2012, 125, 1125.e1–1125.e7. [Google Scholar] [CrossRef] [PubMed]
- Lindner, G.; Funk, G.C. Hypernatremia in critically ill patients. Journal of Critical Care 2013, 28, 216.e11–216.e20. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Xu, X.; Fan, H.; et al. Hypernatremia is associated with mortality in severe elderly sepsis patients: a retrospective cohort study. PLoS ONE 2024, 19, e0310245. [Google Scholar] [CrossRef]
- El-Sharkawy, A.M.; Sahota, O.; Lobo, D.N. Acute and chronic effects of hydration status on health. Nutrition Reviews 2015, 73, 97–109. [Google Scholar] [CrossRef] [PubMed]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).