Submitted:
04 March 2026
Posted:
04 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Ethical Approval, Study Settings, and Participants
2.2. Inclusion and Exclusion Criteria
- Normal patients (NP): individuals suspected of having thyroid complications and having no kidney complications or other confirmed diagnosed diseases.
- Non-dialysis kidney patients (NDKP): individuals with kidney or renal complications confirmed by a creatinine level > the reference range (0.6-1.3 mg/dL) who are suspected of having thyroid complications.
- Dialysis patients (DP): ESRD patients receiving dialysis for ≥1 year were suspected of having thyroid complications.
2.3. Sample Collection
2.4. Measurement of T3, T4 and TSH Levels
2.5. Statistical Analysis
3. Results
3.1. Participant Demographics and Hormonal Level Determination
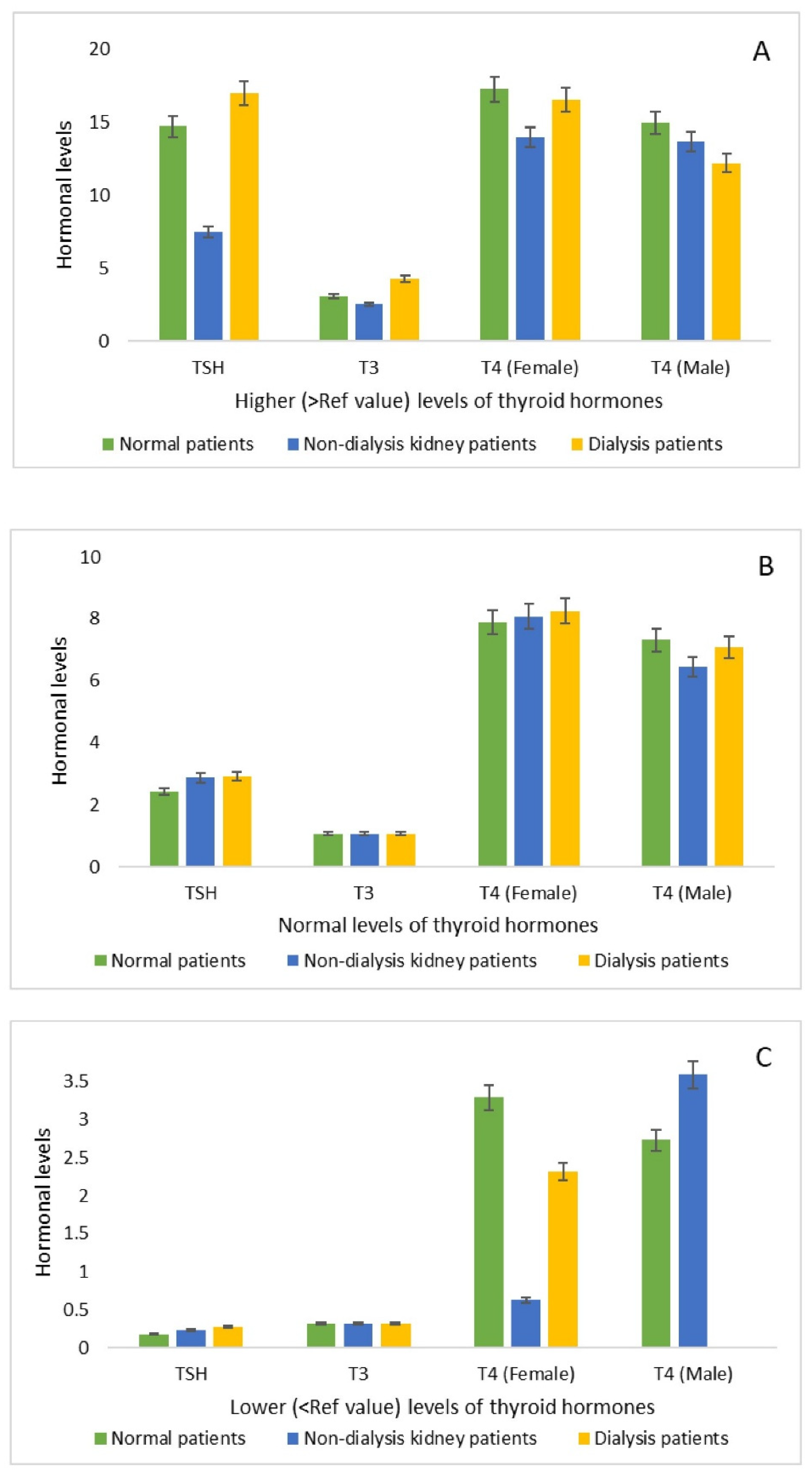
3.2. Comparison of Thyroid Hormone Levels
3.3. Comparison of Hormone Levels Based on Sex and Age
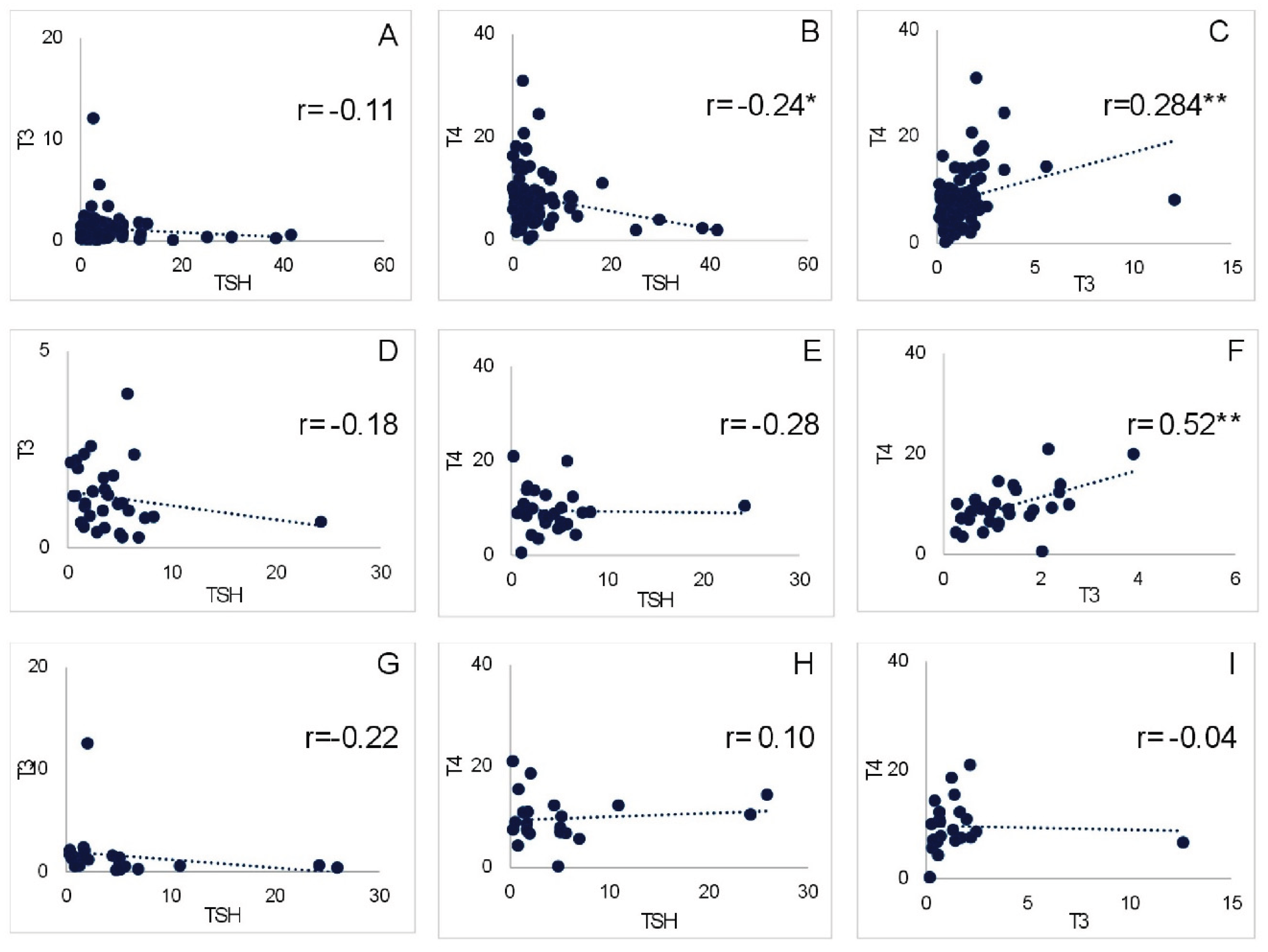
3.4. Association Between Hormone Levels
4. Discussion
5. Limitations of This Study
6. Future Perspectives and Recommendations
7. Conclusions
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Neuen, Brendon L; Bello, Aminu K; Levin, Adeera; Lunney, Meaghan; Osman, Mohamed A; Ye, Feng; Ashuntantang, Gloria E; Bellorin-Font, Ezequiel; Benghanem Gharbi, Mohammed; Davison, Sara. National Health Policies and Strategies for Addressing Chronic Kidney Disease: Data from the International Society of Nephrology Global Kidney Health Atlas. PLOS Global Public Health 2023, 3(no. 2), e0001467. [Google Scholar] [CrossRef]
- Khandker, Shahad Saif; Jahan, Safrin; Khan, Adiba Ayesha; Abrittee, Begum Faijunnesa; Nanjiba, Rifah; Islam, Dewan Zubaer; Suez, Ehsan; Rahman, Md Habibur; Farahim, Farha; Ali, Talat. Global Epidemiology of Hiv among Dialysis Patients: A Systematic Review and Meta-Analysis. International Urology and Nephrology 2025, 1–18. [Google Scholar]
- Cotoi, Laura; Borcan, Florin; Sporea, Ioan; Amzar, Daniela; Schiller, Oana; Schiller, Adalbert; Dehelean, Cristina A; Nicusor Pop, Gheorghe; Borlea, Andreea; Stoian, Dana. Thyroid Pathology in End-Stage Renal Disease Patients on Hemodialysis. Diagnostics 2020, 10(no. 4), 245. [Google Scholar] [CrossRef] [PubMed]
- Khandker, Shahad Saif; Jannat, Nurani; Sarkar, Deepannita; Pranto, Alif Hasan; Hoque, Ismoth Ara; Zaman, Jemema; Uddin, Md Nizam; Suez, Ehsan. Association between Glomerular Filtration Rate and Β-Thalassemia Major: A Systematic Review and Meta-Analysis. Thalassemia Reports 2023, 13(no. 3), 195–205. [Google Scholar] [CrossRef]
- Zoccali, Carmine; Kramer, Anneke; Jager, Kitty J. Chronic Kidney Disease and End-Stage Renal Disease—a Review Produced to Contribute to the Report ‘the Status of Health in the European Union: Towards a Healthier Europe’. NDT plus 2010, 3(no. 3), 213–24. [Google Scholar] [CrossRef]
- Fan, Jingxian; Yan, Peng; Wang, Yingdeng; Shen, Bo; Ding, Feng; Liu, Yingli. Prevalence and Clinical Significance of Low T3 Syndrome in Non-Dialysis Patients with Chronic Kidney Disease. Medical science monitor: international medical journal of experimental and clinical research 2016, 22, 1171. [Google Scholar] [PubMed]
- Shahid, Muhammad A; Ashraf, Muhammad A; Sharma, Sandeep. Physiology, Thyroid Hormone; 2018. [Google Scholar]
- Schroeder, Amy C; Privalsky, Martin L. Thyroid Hormones, T3 and T4, in the Brain. Frontiers in endocrinology 2014, 5, 40. [Google Scholar]
- Gomes-Lima, Cristiane; Wartofsky, Leonard; Burman, Kenneth. Can Reverse T3 Assay Be Employed to Guide T4 Vs. T4/T3 Therapy in Hypothyroidism? Frontiers in endocrinology 2019, 10, 856. [Google Scholar] [CrossRef]
- Wiersinga, WM. L-T4 and L-T3 Combined Treatment Vs L-T4 Alone. Paper presented at the Annales d’endocrinologie, 2007. [Google Scholar]
- Sapin, R; Schlienger, JL. Thyroxine (T4) and Tri-Iodothyronine (T3) Determinations: Techniques and Value in the Assessment of Thyroid Function. Paper presented at the Annales de biologie clinique, 2003. [Google Scholar]
- Biondi, Bernadette; Cappola, Anne R; Cooper, David S. Subclinical Hypothyroidism: A Review. Jama 2019, 322(no. 2), 153–60. [Google Scholar]
- Nillni, Eduardo A. Regulation of the Hypothalamic Thyrotropin Releasing Hormone (Trh) Neuron by Neuronal and Peripheral Inputs. Frontiers in neuroendocrinology 2010, 31(no. 2), 134–56. [Google Scholar]
- Duntas, LH. New Insights into the Hypothalamic-Pituitary-Thyroid Axis. Acta Endocrinologica (Bucharest) 2016, 12(no. 2), 125. [Google Scholar] [CrossRef]
- Salih, Sama S; Yenzeel, Jabbar H. Evaluation of Thyroid Hormones and Some Biochemical Variables in Patients with Chronic Kidney Disease. Iraqi Journal of Science 2020, 985–92. [Google Scholar] [CrossRef]
- Mohamedali, Mohamed; Reddy Maddika, Srikanth; Vyas, Anix; Iyer, Viswanathan; Cheriyath, Pramil. Thyroid Disorders and Chronic Kidney Disease. International journal of nephrology 2014, no. 1, 520281. [Google Scholar]
- Rhee, Connie M; You, Amy S; Nguyen, Danh V; Brunelli, Steven M; Budoff, Matthew J; Streja, Elani; Nakata, Tracy; Kovesdy, Csaba P; Brent, Gregory A; Kalantar-Zadeh, Kamyar. Thyroid Status and Mortality in a Prospective Hemodialysis Cohort. The Journal of Clinical Endocrinology & Metabolism 2017, 102(no. 5), 1568–77. [Google Scholar] [CrossRef]
- Agahi, Sadaf; Amouzegar, Atieh; Honarvar, Mohammadjavad; Azizi, Fereidoun; Mehran, Ladan. Interrelationship between Thyroid Hormones and Reduced Renal Function, a Review Article. Thyroid Research 2024, 17(no. 1), 14. [Google Scholar] [CrossRef]
- Raj, Rishav; Kumar, Vijay; Bhushan, Divendu; Biswas, Ratnadeep; Ojha, Vishnu S; KUMAR, VIJAY. The Prevalence of Thyroid Abnormalities in Patients with Chronic Kidney Disease: A Cross-Sectional Study at a Tertiary Care Hospital. Cureus 2023, 15(no. 8). [Google Scholar] [CrossRef]
- Kaka, Nirja; Sethi, Yashendra; Patel, Neil; Kaiwan, Okashah; Al-Inaya, Yana; Manchanda, Kshitij; Uniyal, Nidhi. Endocrine Manifestations of Chronic Kidney Disease and Their Evolving Management: A Systematic Review. Disease-a-Month 2022, 68(no. 12), 101466. [Google Scholar] [CrossRef]
- Horacek, Jiri; Dusilova Sulkova, Sylvie; Malirova, Eva; Dlabalova, Blanka; Safranek, Roman; Kubisova, Michaela; Kalousova, Marta; Maly, Jaroslav; Zak, Pavel. Haemodialysis-Induced Changes in Thyroid Hormones and Thyrotropin. Paper presented at the Endocrine Abstracts, 2013. [Google Scholar]
- Weaver, Virginia M; Fadrowski, Jeffrey J; Jaar, Bernard G. Global Dimensions of Chronic Kidney Disease of Unknown Etiology (Ckdu): A Modern Era Environmental and/or Occupational Nephropathy? BMC nephrology 2015, 16(no. 1), 145. [Google Scholar]
- Lo, Joan C; Chertow, Glenn M; Go, Alan S; Hsu, Chi-Yuan. Increased Prevalence of Subclinical and Clinical Hypothyroidism in Persons with Chronic Kidney Disease. Kidney international 2005, 67(no. 3), 1047–52. [Google Scholar] [CrossRef] [PubMed]
- Delanaye, Pierre; Ebert, Natalie; Melsom, Toralf; Gaspari, Flavio; Mariat, Christophe; Cavalier, Etienne; Björk, Jonas; Christensson, Anders; Nyman, Ulf; Porrini, Esteban. Iohexol Plasma Clearance for Measuring Glomerular Filtration Rate in Clinical Practice and Research: A Review. Part 1: How to Measure Glomerular Filtration Rate with Iohexol? Clinical kidney journal 2016, 9(no. 5), 682–99. [Google Scholar] [CrossRef]
- Zahra, Sabahat; Saleem, Muhammad Khurram; Ejaz, Khawaja Faizan; Akbar, Amna; Khan Jadoon, Sarosh; Hussain, Shoukat; Ali, Amir Iqbal; Ifty, Mehzabeen; Jannati, Sadia Zafur; Armin, Fariza. Prevalence of Nephropathy among Diabetic Patients in North American Region: A Systematic Review and Meta-Analysis. Medicine 2024, 103(no. 38), e39759. [Google Scholar] [CrossRef]
- Kashif, Md; Hussain, Md S; Anis, Mudassir; Shah, Papu K; Siddiqui, Mudassir A, Sr. Thyroid Dysfunction and Chronic Kidney Disease: A Study among the Northeastern Population of India. Cureus 2023, 15(no. 5). [Google Scholar] [CrossRef]
- Chehade, Joe M; Belal, Heiba F. Cross-Section of Thyroidology and Nephrology: Literature Review and Key Points for Clinicians. Journal of clinical & translational endocrinology 2024, 37, 100359. [Google Scholar]
- Rhee, Connie M; Brent, Gregory A; Kovesdy, Csaba P; Soldin, Offie P; Nguyen, Danh; Budoff, Matthew J; Brunelli, Steven M; Kalantar-Zadeh, Kamyar. Thyroid Functional Disease: An under-Recognized Cardiovascular Risk Factor in Kidney Disease Patients. Nephrology Dialysis Transplantation 2015, 30(no. 5), 724–37. [Google Scholar] [CrossRef]
- Reque Santivañez, Javier; Garcia Peris, Beatriz; Panizo Gonzalez, Nayara; Perez Alba, Alejandro; D’Marco, Luis; Collado Boira, Eládio. Subclinical Hypothyroidism in Advanced Chronic Kidney Disease Patients: Prevalence and Associated Factors. Journal of Thyroid Research 2022, no. 1, 1077553. [Google Scholar] [CrossRef] [PubMed]
- Sanai, Toru; Okamura, Ken; Onoue, Tomoaki; Ono, Takashi; Motomura, Kenichi; Miyazono, Motoaki; Shimamatsu, Kazumasa. Hemodilution Impacts Assessment of Thyroid Status before and after Hemodialysis in Patients with End-Stage Renal Disease. American Journal of Nephrology 2021, 51(no. 12), 988–94. [Google Scholar] [CrossRef]
- Shamsadini, S; Darvish-Moghaddam, S; Abdollahi, H; Fekri, AR; Ebrahimi, HA. Creatinine, Blood Urea Nitrogen and Thyroid Hormone Levels before and after Haemodialysis. Eastern Mediterranean Health Journal 2006, 12(no. 1/2), 231. [Google Scholar]
- Bauer, Michael; Glenn, Tasha; Pilhatsch, Maximilian; Pfennig, Andrea; Whybrow, Peter C. Gender Differences in Thyroid System Function: Relevance to Bipolar Disorder and Its Treatment. Bipolar disorders 2014, 16(no. 1), 58–71. [Google Scholar] [CrossRef] [PubMed]
- Mirahmad, Maryam; Mansour, Asieh; Moodi, Mitra; Safkhani, Elaheh; Haghpanah, Vahid; Asili, Pooria; Fakhrzadeh, Hossein; Payab, Moloud; Ebrahimpur, Mahbube; Khorashadi, Masoumeh. Prevalence of Thyroid Dysfunction among Iranian Older Adults: A Cross-Sectional Study. Scientific Reports 2023, 13(no. 1), 21651. [Google Scholar] [CrossRef] [PubMed]
- Samuels, Mary H. Hyperthyroidism in Aging. In Endotext [Internet]; 2021. [Google Scholar]
- Kumar, Manjula S; Safa, Ali M; Deodhar, Sharad D; Schumacher, O Peter. The Relationship of Thyroid-Stimulating Hormone (Tsh), Thyroxine (T4), and Triiodothyronine (T3) in Primary Thyroid Failure. American Journal of Clinical Pathology 1977, 68(no. 6), 747–51. [Google Scholar] [CrossRef]
- Fitzgerald, Stephen Paul; Bean, Nigel Geoffrey. The Relationship between Population T4/Tsh Set Point Data and T4/Tsh Physiology. Journal of Thyroid Research 2016, no. 1, 6351473. [Google Scholar] [CrossRef] [PubMed]
- Wiersinga, Wilmar M. T4+ T3 Combination Therapy: An Unsolved Problem of Increasing Magnitude and Complexity. Endocrinology and Metabolism 2021, 36(no. 5), 938–51. [Google Scholar] [CrossRef] [PubMed]
- Li, Hong; Yuan, Xiaolan; Liu, Lu; Zhou, Jiaojiao; Li, Chunyan; Yang, Peng; Bu, Le; Zhang, Manna; Qu, Shen. Clinical Evaluation of Various Thyroid Hormones on Thyroid Function. International journal of endocrinology 2014, no. 1, 618572. [Google Scholar] [CrossRef] [PubMed]

| NP | NDKP | DP | |
|---|---|---|---|
| Overall, patients, n | 106 | 32 | 23 |
| Age in years (mean ± SD) | 38.64 ± 17.05 | 43.75 ± 17.54 | 43.00 ± 17.51 |
| Male, n | 32 | 10 | 8 |
| Age in years (mean ± SD) | 37.55 ± 17.01 | 45.7 ± 18.22 | 45 ± 15.90 |
| Female, n | 74 | 22 | 15 |
| Age in years (mean ± SD) | 39.12 ± 17.10 | 42.86 ± 17.53 | 41.93 ± 17.51 |
| Patients of different groups, n (%) | Normal Level, n (%) | Higher level, n (%) | Lower level, n (%) |
|---|---|---|---|
| NP, n= 106 (100) | |||
| TSH | 80 (75.47) | 19 (17.92) | 7 (6.60) |
| T3 | 67 (63.20) | 17 (16.03) | 22 (20.75) |
| T4 (female) | 43 (40.56) | 11 (10.37) | 18 (16.98) |
| T4 (male) | 19 (17.92) | 9 (8.49) | 6 (5.66) |
| T4 overall | 62 (58.49) | 20 (18.86) | 24 (22.64) |
| NDKP, n= 32 (100) | |||
| TSH | 26 (81.25) | 5 (15.62) | 1 (3.12) |
| T3 | 20 (62.50) | 7 (21.32) | 5 (15.62) |
| T4 (female) | 17 (53.12) | 5 (15.62) | 1 (3.12) |
| T4 (male) | 4 (12.5) | 4 (12.5) | 1 (3.12) |
| T4 overall | 21 (65.62) | 9 (28.12) | 2 (6.25) |
| DP, n= 23 (100) | |||
| TSH | 17 (73.91) | 4 (17.39) | 2 (8.69) |
| T3 | 13 (56.52) | 5 (21.73) | 5 (21.73) |
| T4 (female) | 9 (39.13) | 4 (17.39) | 2 (8.69) |
| T4 (male) | 4 (17.39) | 4 (17.39) | 0 (0.0) |
| T4 overall | 13 (56.52) | 8 (34.78) | 2 (8.69) |
| Category | Thyroid hormones | Hormonal levels (mean) | ||
|---|---|---|---|---|
| NP | NDKP | DP | ||
| Male | TSH | 3.97 | 4.10 | 4.26 |
| T3 | 1.54 | 1.39 | 1.13 | |
| T4 | 8.2 | 9.33 | 9.65 | |
| Female | TSH | 4.71 | 3.96 | 5.60 |
| T3 | 1.10 | 1.24 | 1.86 | |
| T4 | 8.36 | 9.55 | 9.67 | |
| Age<45 y | TSH | 3.94 | 4.64 | 5.54 |
| T3 | 1.24 | 1.40 | 2.32 | |
| T4 | 8.59 | 11.07 | 8.74 | |
| Age>45 y | TSH | 5.89 | 3.25 | 4.64 |
| T3 | 1.24 | 1.23 | 1.12 | |
| T4 | 8.11 | 7.95 | 10.77 | |
| Patient Group | Thyroid Hormone Levels/Activity | Implications |
|---|---|---|
| Dialysis patients with renal complications | Moderately enhanced thyroid hormone levels and activity | Suggests potential benefits of routine dialysis for CKD/ESRD patients |
| Non-dialysis patients with kidney disease | Not significantly enhanced thyroid hormone levels and activity | Supports the need for further investigation with larger cohorts |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




