Submitted:
22 February 2026
Posted:
28 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Protocol and Registration
Eligibility Criteria
Population
Concept
Context
Other
Information Sources and Search
Selection of Sources and Evidence
Data Charting Process and Data Items
Synthesis
3. Results
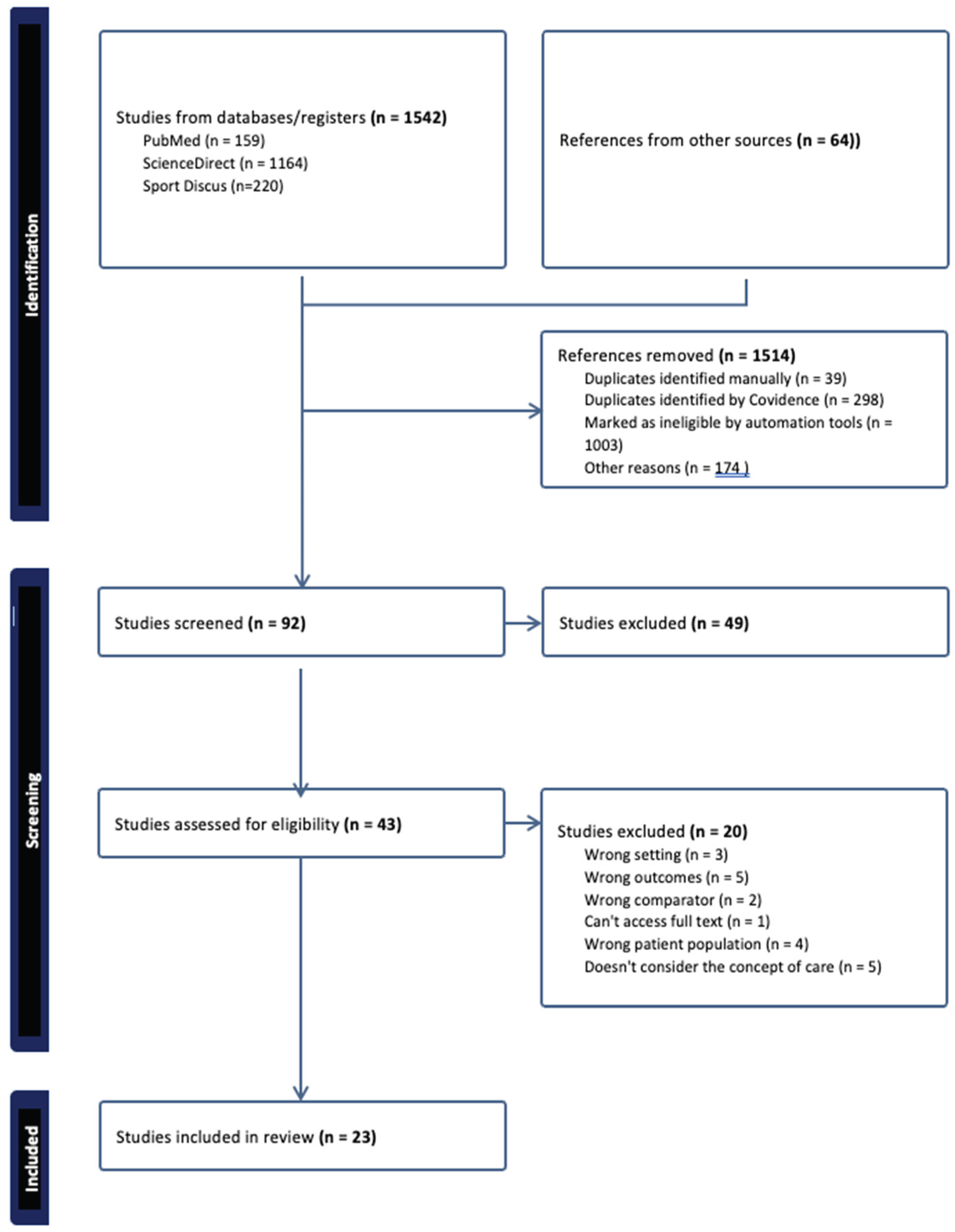
Selection of Sources of Evidence
Characteristics of Sources of Evidence
| Authors | Study Type | Location of study | Participants- SEM/Athlete | Gender | Key Findings |
| Aitchison, Rushton, Martin, Soundy and Heneghan (2021) [21] | Qualitative- Interviews | United Kingdom | 8 athletes | 5 Female, 3 Male | 1. Tangible aid- Emotional support, listening caring, information on injury prevention. provided emotional support through listening and caring, and informational support through offering advice on injury prevention. 2. Physiotherapy was also viewed as having the potential to be an educational tool if utilised correctly |
| Arvinen-Barrow, Massey and Hemmings (2014) [34] | Qualitative- Interviews | United Kingdom | 10 athletes | 10 males | 1. Athletes expect SEM to show a real interest in them and 100% effort to get them back fit. 2. Honest and open communication needed. 3. Expect SEM are able to pick up and read the athletes emotional state. 4. Motivate you and friend like behaviour |
| Barrette and Harman (2020) [22] | Qualitative- Interviews | North America | 4 athletes and 3 Rehabilitation specialists | 5 Female, 2 Male | 1. SEM a resource when unsure what is happening with body and trust the physio to guide 2. Supportive when injured but aware there was an element of risk taking due to pressure 3. Having a strong rapport improved rehab as athlete trusted it |
| Charmant, van der Wees, Staal, van Cingel, Sieben and de Bie (2021) [23] | Qualitative- Interviews | Netherlands | 10 physios and 10 athletes | 15 women and 5 males | 1. Relationship is entirely built upon trust 2. Communication- both parties need to see the other one as equals and small talk is an important aspect. 3. Good communication with the wider interdisciplinary team is required. 4. Athletes want to feel listened to, respected, shared-decision making and taken seriously. |
| Ekstrand, Lundqvist, Davison, D’Hooghe and Pensgaard (2018) [40] | Quantitative - Survey | Europe | 77 medical staff | Not stated | 1. Ranking low quality communication with the head coach had a higher injury burden and incidence. 2. High quality communication within the medical team- lower injury rates and better training attendance. 3. Attendance to training was lower if there was a lower quality communication between medics and fitness team. |
| Francis, Andersen and Maley (2000) [41] | Quantitative - Survey | Australia | 57 Physios and 28 athletes | Physios- 21 Female and 36 Male. Athletes 28 Male | 1. Positive communication an important factor. 2. Enthusiastic and knowledgeable physio. 3. Listening skills- interpersonal skills |
| Horan, Kelly, Hägglund, Blake, Roe and Delahunt (2023) [24] | Qualitative- Interviews | Ireland | 17 athletes and 8 medics | Medical- 2 Females and 6 male. Players 17 females | 1. Interpersonal skills and communication were key attributes in injury management. 2. Players believe that medics should put the athletes best interests first but it isn’t always the case. 3. Trust an important aspect- to report an injury and when to push them on through an injury |
| Kerai, Wadey, and Salim (2019) [35] | Qualitative- Interviews | United Kingdom | 10 physios | 5 Female and 5 Male | 1. Stress, burnout and transaction side of relationship. 2. Sport is high pressured and expected to be like that and impacts the culture 3. Relationship with MDT and athletes- Conflict as the organisation pays them when making difficult decisions |
| Knott (2024) [6] | Qualitative- Interviews | United Kingdom | 15 Physios | 7 females and 8 males | 1. A willingness to constantly go above and beyond for the athlete. 2. Often a poor work/life balance as need to sacrifice for the athlete. 2. There can be conflict between performance decision and health decisions. 3. Communication is important and style situational |
| Mann, Grana, Indelicato, O’Neill and George (2007) [42] | Quantitative - Survey | USA | 827 Doctors | Not stated | 1. Discomfort over discussing psychological and sensitive issues |
| Marks, Courtney and Healey (2023) [26] | Qualitative- Interviews | USA | 35 athletes | 15 Female and 20 Male | 1. A trusting relationship is a key factor, managing information not going further than they want to. 2. A previous or established history improves the trust |
| Marshall, Donovan-Hall and Ryall (2012) [36] | Qualitative- Interviews | United Kingdom | 9 athletes | 3 Females and 5 Males | 1. Athlete intrinsic motivation not to let the physio down. 2. Physio should be supportive, sympathetic, attentive, approachable, listens to their views. 3. Trusting the physio. |
| McKenna, Delaney and Phillips (2002) [37] | Qualitative- Interviews | United Kingdom | 10 Physios | 5 Female and 5 Male | 1. Having previous exp as an ex-athlete helped rapport and knowing the athletes world. 2. Knowing the athlete as a person. 3. Respect sometimes lacking from athlete to physio |
| Bonell Monsonís, Verhagen, Kaux and Bolling (2021) [27] | Qualitative- Interviews | Belgium | 8 athletes, 2 physical therapists and 1 medical doctor | Not stated | 1. Constant communication between athletes and SEM creates a trusting relationship. 2. Athlete has confidence in the SEM team |
| Noesgaard and Sæther (2024) [28] | Qualitative- Interviews | Norway | 2 athletes and 1 physio | Not stated | 1. Players and medical staff feel SEM must manage the performance and athlete health risks balance. 2. Players need to trust the SEM to make the right decision for them. 3. Trust, communication and collaboration are fundamental elements |
| Paraskevopoulos, Gioftsos, Georgoudis and Papandreou (2023) [29] | Qualitative- Interviews | Greece | 8 athletes | 5 female and 3 male | 1. Physio provides mental support. 2. Confidence in the physio through their years of experience and level of team |
| Rees and Hardy (2000) [38] | Qualitative- Interviews | United Kingdom | 10 athletes | 5 Female and 5 Male | 1. Reassurance from the physiotherapist 2. Physio experience in the sport themselves as an ex-athlete |
| Scott and Malcolm (2015) [39] | Qualitative- Interviews | United Kingdom | 14 physios and 14 doctors | Not stated | 1. Physios and doctors have a strong rapport and communicate well together, rarely have conflict. 2. Physios feel immersed with their athletes working with them closely. 3. Strong emotional element around managing the athlete and injury. 4. Need to establish trust with the athlete |
| Stewart, Fletcher, Arnold and McEwan (2023) [30] | Qualitative- Interviews | United Kingdom | 4 physios (18 MDT) | 5 female and 13 males | 1. Interpersonal compatibility, role clarity, culture, hierarchy affect the team effectiveness. 2. Shared objectives. 3. Communication a crucial aspect of team effectiveness and performance |
| Stewart, Fletcher, Arnold and McEwan (2024) [31] | Narrative review | N/A | N/A | N/A | 1. Desirable- disciplinary knowledge, technical competency, and interpersonal qualities |
| VanEtten, Briggs, DeWitt, Mansfield and Kaeding (2021) [32] | Case Report | USA | 1 athlete and 1 physio | 1 Therapist male and 1 athlete Male | 1. Communication and goal setting that was achievable and relatable to the athlete. 2. Rapport and trust improved adherence 3. Shared decision making on when to adjust interventions 4. Therapeutic alliance framework |
| Vella, Bolling, Verhagen and Moore (2022) [33] | Qualitative- Interviews | Malta | 7 athletes and 3 medics | 4 females and 9 males | 1. Relationship between physio and athlete can affect how much they are willing to push them |
| Woods and Woods (2012) [43] | Quantitative - Survey | Ireland | 13 athletes | 5 female and 8 males | 1. Good qualities- being accessible, interested in you, patient, persistent, communicator, understand the high emotional and psychological demands of the sport. 2. Communication to the athlete and wider MDT |
Synthesis of Results
- Communication
- 2.
- Trust
- 3.
- Desired characteristics of a sports medicine practitioner
4. Discussion
Limitations and Future Research
Clinical Implications
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Donabedian, A. (1974). Aspects of Medical Care Administration. Harvard University Press: Cambridge, Mass.
- Krause, F. and Boldt, J. (2018) Care in Healthcare: Reflections on Theory and Practice. Palgrave Macmillan.
- Care Quality Commission. (2025). UK. Available at: https://www.cqc.org.uk.
- Dijkstra HP, Pollock N, Chakraverty R, Alonso JM. Managing the health of the elite athlete: a new integrated performance health management and coaching model. Br J Sports Med. 2014;48(7):523–31.
- Anderson, L. (2009) Writing a new code of ethics for sports physicians: principles and challenges. British Journal of Sports Medicine. 43: 1079-1082. [CrossRef]
- Knott, S. and Phillips, N. (2025) Speaking Up about Athlete Welfare in Sport – A Physio’s Challenge. IJSPT. 20(6):766-769. [CrossRef]
- White C., Garner, P., Horsley, I., Soundy, A. (2025) Experiences of Female Rugby Union Players and Practitioners in Rehabilitation Following a Shoulder Injury. Sports (Basel). May 28;13(6):166. PMID: 40559678; PMCID: PMC12196548. [CrossRef]
- Rees, H., J. Matthews, U. McCarthy Persson, E. Delahunt, C. Boreham and C. Blake (2022). “The knowledge and attitudes of field hockey athletes to injury, injury reporting and injury prevention: A qualitative study.” J Sci Med Sport 25(10): 820-827.
- Noddings, N. (1988). An ethic of caring and its implications for instructional arrangements. American Journal of 581 Education, 96(2), 215- 230. [CrossRef]
- Cronin, C., Z. R. Knowles and K. Enright (2019). “The challenge to care in a Premier League Football Club.” Sports Coaching Review 9(2): 123-146.
- Burns, L., Weissensteiner, J. and Cohen, M. (2019) Supportive interpersonal relationships: a key component to high- performance sport. British Journal of Sports Medicine. 53:22.
- Salcinovic, B., Drew, M., Dijkstra, P., Waddington, G. and Serpell, B. (2022) Factors Influencing Team Performance: What Can Support Teams in High-Performance Sport Learn from Other Industries? A Systematic Scoping Review. Sports Medicine Open. 8:25. [CrossRef]
- Behnia, B. (2008) Trust Development: A Discussion of Three Approaches and a Proposed Alternative. British Journal of Social Work. 38, 1425-1441. [CrossRef]
- Walton, C., Purcell, R., Pilkington, V., Hall, K., Kentta, G., Vella, S. and Rice, S. (2024) Psychological Safety for Mental Health in Elite Sport: A Theoretically Informed Model. Sports Medicine. 54:557-564. [CrossRef]
- Hall A, Ferreira P, Maher C., Latimer, J. and Ferreira, M. (2010) The influence of the therapist- patient relationship on treatment outcome in physical rehabilitation: a systematic review. Physical Therapy. 90:8, 1099 –1110.
- Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, et al. (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 169:467–73. [CrossRef]
- Peters MD. In no uncertain terms: the importance of a defined objective in scoping reviews. JBI Database System Rev Implement Rep. 2016;14(2):1–4.
- McEwan, I. and Taylor, W. (2010) ‘When do I get to run on with the magic sponge?’ The twin illusions of meritocracy and democracy in the professions of sports medicine and physiotherapy, Qualitative Research in Sport and Exercise, 2:1, 77-91. [CrossRef]
- Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at www.covidence.org.
- Westphaln, K., Regoeczi, W., Masotya, M., Vazquez-Westphaln, B., Lounsbury, K., McDavid, L., Lee, H., Johnson, J. and Ronis, S. (2021) From Arksey and O’Malley and Beyond: Customizations to enhance a team-base d, mixe d approach to scoping review methodology. MethodsX. 8.
- Aitchison, B., Rushton, A., Martin, P., Soundy, A. and Heneghan, N. (2021) The podium illusion: a phenomenological study of the influence of social support on well-being and performance in elite para swimmers. BMC Sports science, medicine and Rehabilitation. 13:42. [CrossRef]
- Barrette, A., & Harman, K. (2020). Athletes Play Through Pain-What Does That Mean for Rehabilitation Specialists? J Sport Rehabil, 29(5), 640-649. [CrossRef]
- Charmant, W. M., van der Wees, P. J., Staal, J. B., van Cingel, R., Sieben, J. M., & de Bie, R. A. (2021). A framework exploring the therapeutic alliance between elite athletes and physiotherapists: a qualitative study. BMC Sports Sci Med Rehabil, 13(1), 122. [CrossRef]
- Horan, D., Kelly, S., Hagglund, M., Blake, C., Roe, M., & Delahunt, E. (2023). Players’, Head Coaches’, And Medical Personnels’ Knowledge, Understandings and Perceptions of Injuries and Injury Prevention in Elite-Level Women’s Football in Ireland. Sports Med Open, 9(1), 64. [CrossRef]
- Knott, S. (2024) Speaking Up in Elite Sport: An exploratory-descriptive qualitative study of UK physiotherapists’ experiences. Thesis. Cardiff University.
- Marks, A., Courtney, C. A., & Healey, W. E. (2023). Perceptions of Physical Therapy and The Role of Physical Therapists In Injury Prevention Among Professional Basketball Players: A Qualitative Study. Int J Sports Phys Ther, 18(5), 1186-1195. [CrossRef]
- Bonell Monsonís O, Verhagen E, Kaux J-F, et al. ‘I always considered I needed injury prevention to become an elite athlete’: the road to the Olympics from the athlete and staff perspective. BMJ Open Sport & Exercise Medicine 2021;7:e001217. [CrossRef]
- Noesgaard, M. and Sæther, S. (2024) Decision-making on injury prevention and rehabilitation in professional football – A coach, medical staff, and player perspective. The Sport Journal.
- Paraskevopoulos, E., Gioftsos, G., Georgoudis, G., & Papandreou, M. (2023). Perceived Barriers and Facilitators of Sports Rehabilitation Adherence in Injured Volleyball Athletes: A Qualitative Study From Greece. Journal of Clinical Sport Psychology, 17(1), 86-105. [CrossRef]
- Stewart, P., Fletcher, D., Arnold, R., & McEwan, D. (2023). Exploring perceptions of performance support team effectiveness in elite sport. Sport Management Review, 27(2), 300-321. [CrossRef]
- Stewart, P., Fletcher, D., Arnold, R., & McEwan, D. (2024). Performance support team effectiveness in elite sport: a narrative review. International Review of Sport and Exercise Psychology, 1-24. [CrossRef]
- VanEtten, L., Briggs, M., DeWitt, J., Mansfield, C., & Kaeding, C. (2021). The Implementation of Therapeutic Alliance in the Rehabilitation of an Elite Pediatric Athlete with Salter-Harris Fracture: A Case Report. Int J Sports Phys Ther, 16(2), 539-551. [CrossRef]
- Vella, S., Bolling, C., Verhagen, E., & Moore, I. S. (2022). Perceiving, reporting and managing an injury - perspectives from national team football players, coaches, and health professionals. Sci Med Footb, 6(4), 421-433. [CrossRef]
- Arvinen-Barrow, M., Massey, W. V., & Hemmings, B. (2014). Role of sport medicine professionals in addressing psychosocial aspects of sport-injury rehabilitation: professional athletes’ views. J Athl Train, 49(6), 764-772. [CrossRef]
- Kerai, S., Wadey, R., & Salim, J. (2019). Stressors experienced in elite sport by physiotherapists. Sport, Exercise, and Performance Psychology, 8(3), 255-272. [CrossRef]
- Marshall, A., Donovan-Hall, M. and Ryall, S. (2012) An exploration of athletes’ views on their adherence to physiotherapy rehabilitation after sport injury. Journal of sport rehabilitation. 21, 18-25.
- McKenna, J., Delaney, H., & Phillips, S. (2002). Physiotherapists’ lived experience of rehabilitating elite athletes. Physical Therapy in Sport, 3(2), 66-78. [CrossRef]
- Rees, T and Hardy, L. (2000) An investigation of the social support experiences of high-level sports performers. The Sports Psychologists. 14, 327-347.
- Scott, A., & Malcolm, D. (2014). ‘Involved in every step’: how working practices shape the influence of physiotherapists in elite sport. Qualitative Research in Sport, Exercise and Health, 7(4), 539-556. [CrossRef]
- Ekstrand, J., Lundqvist, D., Davison, M., D’Hooghe, M., & Pensgaard, A. M. (2019). Communication quality between the medical team and the head coach/manager is associated with injury burden and player availability in elite football clubs. Br J Sports Med, 53(5), 304-308. [CrossRef]
- Francis, S., Andersen, M. and Maley, P. (2000) Physiotherapists’ and male professional athletes’ views on psychological skills for rehabilitation. Journal of Science and Medicine in Sport 3 {1):17-29.
- Mann, B. J., Grana, W. A., Indelicato, P. A., O’Neill, D. F., & George, S. Z. (2007). A survey of sports medicine physicians regarding psychological issues in patient-athletes. Am J Sports Med, 35(12), 2140-2147. [CrossRef]
- Woods, A., & Woods, C. B. (2012). An exploration of the perspectives of elite Irish rowers on the role of the sports physiotherapist. Phys Ther Sport, 13(1), 16-21. [CrossRef]
- Rousseau, D. M., Sitkin, S. B., Burt, R. S. and Camerer, C. (1998) ‘Not so different after all: A cross-discipline view of trust’, Academy of Management Review, 23(3), pp. 393–404.
- Giffin, K. (1973) ‘Interaction variables of interpersonal trust’, Humanitias, 9(3), pp. 297–315.
- Noddings, N. (2013). Caring; A relational approach to ethics and moral education. London: University of California Press.
- Kleiner, M., Kinsell, E., Miciak, M., Teachman, G. and Walton, D. (2022) “Passion to do the right thing”: searching for the ‘good’ in physiotherapist practice. Physiotherapy Theory and Practice. 40:2, 288-303. [CrossRef]
- Buetow, S. (2011) Person-centred care: Bridging current models of the clinician- patient relationship. The international Journal of Person Centred Medicine. 1:1. 196-203.
- Garner, P., Roberts, W., Baker, C. and Cote, J. (2022) Characteristics of a person-centred coaching approach. International Journal of Sports Science & Coaching. 17(4) 722–733. [CrossRef]
- Dohsten, J., Barker-Ruchti, N., & Lindgren, E. C. (2020). Caring as sustainable coaching in elite athletics: benefits and challenges. Sports Coaching Review, 9(1), 48–70. [CrossRef]
- Morris, S., Fisher, L., Moore, M., Schools, J., Knust, S. and Christy, Z. (2023) “Make someone love something and share your passion”: Perceptions of coach caring amongst Elite women’s rugby sevens athletes, Sports Coaching Review, 12:1, 87-107. [CrossRef]
- Nelis S, Dijkstra HP, Damman OC, Farooq, A. and Verhagen, E. (2024) Shared decision-making with athletes: a survey study of healthcare professionals’ perspectives. BMJ Open Sport & Exercise Medicine;10:e001913. [CrossRef]
- Armour, K. (2014) Pedagogical cases in physical education and youth sport. (1st edition) Oxon: Routledge.
- Tomaselli G, Buttigieg SC, Rosano A, Cassar M and Grima G (2020) Person-Centered Care From a Relational Ethics Perspective for the Delivery of High Quality and Safe Healthcare: A Scoping Review. Front. Public Health 8:44. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.





