Submitted:
20 February 2026
Posted:
27 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Research Scope
2.2. Inclusion/Exclusion Criteria
2.3. Search Strategy
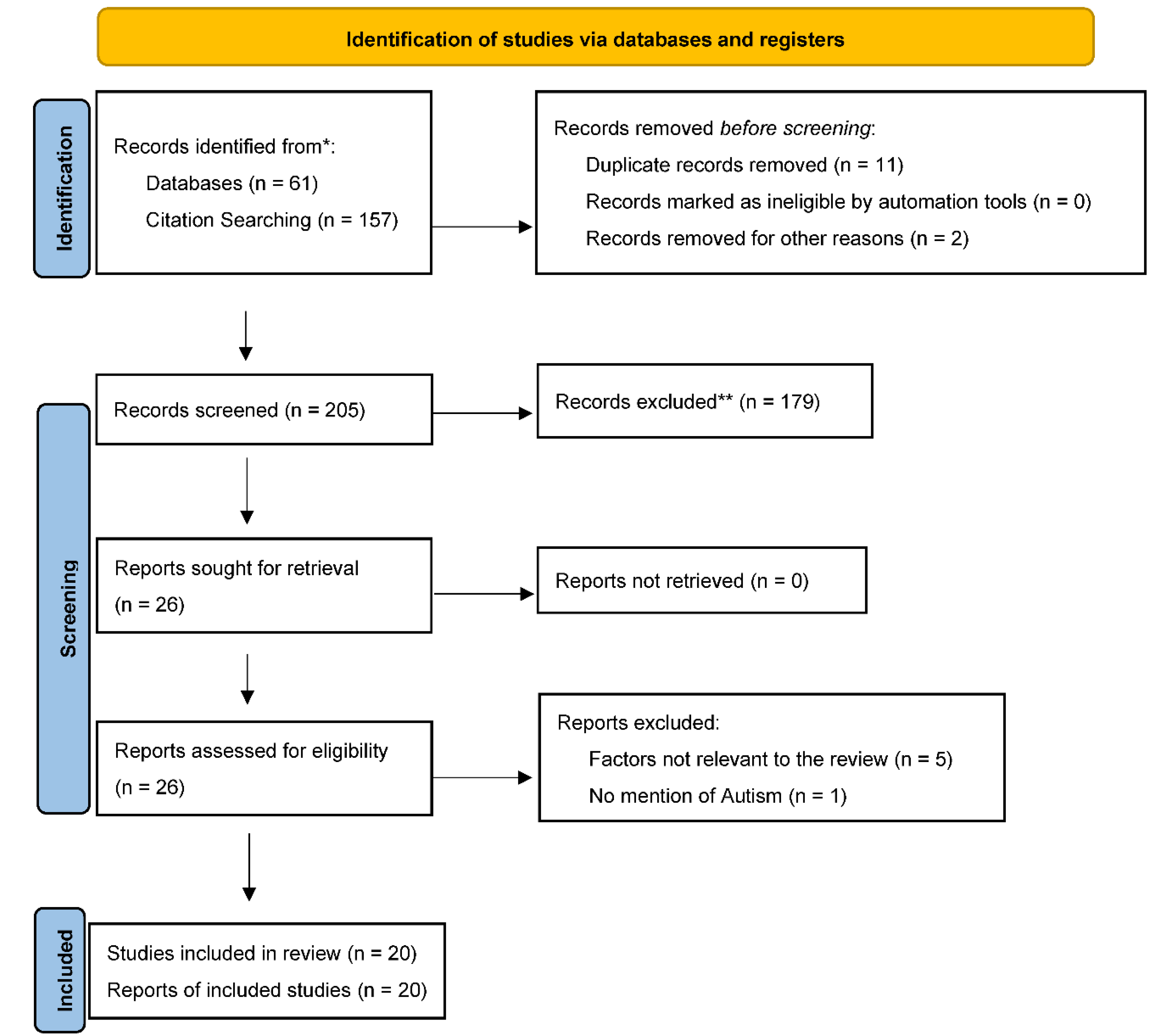
2.4. Screening and Selection Process
2.5. Data Extraction
3. Results
4. Integration and Future Recommendations
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- English, M. C.; Gignac, G. E.; Visser, T. A.; Whitehouse, A. J.; Enns, J. T.; Maybery, M. T. The Comprehensive Autistic Trait Inventory (CATI): Development and validation of a new measure of autistic traits in the general population. Molecular autism 2021, 12(1), 37. [Google Scholar] [CrossRef] [PubMed]
- Smith, A. A combined effects approach to the Demands-Resources-Individual Effects (DRIVE) model of well-being. International Journal of Humanities, Social Sciences and Education 2021, 8(9), 28–38. [Google Scholar]
- Lunia, D.; Smith, A. P. Exploring the associations between autistic traits, sleep quality and well-being in university students: A narrative review. Healthcare 2024, Vol. 12(No. 20), 2027. [Google Scholar] [CrossRef]
- Flegenheimer, C.; Scherf, K. S. College as a developmental context for emerging adulthood in autism: A systematic review of what we know and where we go from here. Journal of Autism and Developmental Disorders 2022, 52(5), 2075–2097. [Google Scholar] [CrossRef] [PubMed]
- Alaghband-Rad, J.; Hajikarim-Hamedani, A.; Motamed, M. Camouflage and masking behaviours in adults with autism. Frontiers in psychiatry 2023, 14, 1108110. [Google Scholar] [CrossRef]
- Lane, S. J.; Leão, M. A.; Spielmann, V. Sleep, sensory integration/processing, and autism: A scoping review. Frontiers in psychology 2022, 13, 877527. [Google Scholar] [CrossRef] [PubMed]
- Nelson, K. L.; Davis, J. E.; Corbett, C. F. Sleep quality: An evolutionary concept analysis. Nursing forum, 2022, January; Vol. 57, pp. 144–151. [Google Scholar]
- Li, W.; Chen, J.; Li, M.; Smith, A. P.; Fan, J. The effect of exercise on academic fatigue and sleep quality among university students. Frontiers in Psychology 2022, 13, 1025280. [Google Scholar] [CrossRef]
- Lai, M. C.; Kassee, C.; Besney, R.; Bonato, S.; Hull, L.; Mandy, W.; Ameis, S. H. Prevalence of co-occurring mental health diagnoses in the autism population: a systematic review and meta-analysis. The Lancet Psychiatry 2019, 6(10), 819–829. [Google Scholar] [CrossRef]
- Page, M. J.; McKenzie, J. E.; Bossuyt, P. M.; Boutron, I.; Hoffmann, T. C.; Mulrow, C. D.; Moher, D. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 2021, 372. [Google Scholar] [CrossRef]
- Grant, S.; Norton, S.; Hoekstra, R. A. Central Sensitivity Symptoms and Autistic Traits in Autistic and Non-Autistic Adults. Autism Research 2025, 18(3), 660–674. [Google Scholar] [CrossRef] [PubMed]
- Lodi-Smith, J.; Rodgers, J. D.; Kozlowski, K.; Khan, S.; Marquez Luna, V.; Long, C. J.; Thomeer, M. L. Autism characteristics and self-reported health in older adulthood. The Journals of Gerontology: Series B 2021, 76(9), 1738–1744. [Google Scholar] [CrossRef]
- Sampson, K. N.; Upthegrove, R.; Abu-Akel, A.; Haque, S.; Wood, S. J.; Reniers, R. Co-occurrence of autistic and psychotic traits: implications for depression, self-harm and suicidality. Psychological medicine 2021, 51(8), 1364–1372. [Google Scholar] [CrossRef] [PubMed]
- Nankoo, M. M.; Palermo, R.; Bell, J. A.; Pestell, C. M. Examining the rate of self-reported ADHD-related traits and endorsement of depression, anxiety, stress, and autistic-like traits in Australian university students. Journal of Attention Disorders 2019, 23(8), 869–886. [Google Scholar] [CrossRef] [PubMed]
- Mantzalas, J.; Richdale, A. L.; Li, X.; Dissanayake, C. Measuring and validating autistic burnout. Autism Research 2024, 17(7), 1417–1449. [Google Scholar] [CrossRef]
- Pelton, M. K.; Crawford, H.; Bul, K.; Robertson, A. E.; Adams, J.; De Beurs, D.; Cassidy, S. The role of anxiety and depression in suicidal thoughts for autistic and non-autistic people: A theory-driven network analysis. Suicide and Life-Threatening Behavior 2023, 53(3), 426–442. [Google Scholar] [CrossRef] [PubMed]
- Levi, M. K.; Schreuer, N.; Granovsky, Y.; Bar-Shalita, T.; Weissman-Fogel, I.; Hoffman, T.; Gal, E. “Feeling unwanted, when nobody wants you around”: Perceptions of social pain among people with autism. The American Journal of Occupational Therapy 2023, 77(2), 7702185050. [Google Scholar] [CrossRef]
- Augustin, M.; Eichhammer, P.; Haas, J.; Schiekofer, S.; Busch, V. Increased alexithymia but no profound emotion processing disorder in burnout syndrome. The Journal of Nervous and Mental Disease 2020, 208(10), 794–802. [Google Scholar] [CrossRef]
- Lian, Y.; Zhang, J.; Jia, C. X. Sleep duration change and cognitive function: a national cohort study of Chinese people older than 45 years. The Journal of Nervous and Mental Disease 2020, 208(6), 498–504. [Google Scholar] [CrossRef]
- Tanielian, M.; Doghramji, K.; Certa, K. Obstructive sleep apnea in psychiatric inpatients. The Journal of nervous and mental disease 2020, 208(3), 190–193. [Google Scholar] [CrossRef]
- Yildiz, E.; Sac, R.; Işik, Ü.; Özaydin, M. S.; Taşar, M. A.; Cakir, I.; Alioglu, B. Comparison of the sleep problems among adolescents who attempted suicide and healthy adolescents. The Journal of nervous and mental disease 2020, 208(4), 294–298. [Google Scholar] [CrossRef]
- Richdale, A. L.; Chetcuti, L.; Hayward, S. M.; Abdullahi, I.; Morris, E. M.; Lawson, L. P. The impact of sleep quality, fatigue and social well-being on depressive symptomatology in autistic older adolescents and young adults. Autism Research 2023, 16(4), 817–830. [Google Scholar] [CrossRef] [PubMed]
- Charlton, R. A.; McQuaid, G. A.; Bishop, L.; Lee, N. R.; Wallace, G. L. Predictors of sleep quality for autistic people across adulthood. Autism research 2023, 16(4), 757–771. [Google Scholar] [CrossRef] [PubMed]
- Martini, M. I.; Kuja-Halkola, R.; Butwicka, A.; Du Rietz, E.; D’Onofrio, B. M.; Happé, F.; Taylor, M. J. Sex differences in mental health problems and psychiatric hospitalization in autistic young adults. JAMA psychiatry 2022, 79(12), 1188–1198. [Google Scholar] [CrossRef]
- Williams, Z. J.; Gotham, K. O. Current and lifetime somatic symptom burden among transition-aged autistic young adults. Autism Research 2022, 15(4), 761–770. [Google Scholar] [CrossRef]
- Mantzalas, J.; Richdale, A. L.; Dissanayake, C. A conceptual model of risk and protective factors for autistic burnout. Autism Research 2022, 15(6), 976–987. [Google Scholar] [CrossRef]
- Weir, E.; Allison, C.; Baron-Cohen, S. Identifying and managing autism in adults. Prescriber 2020, 31(2), 12–16. [Google Scholar] [CrossRef]
- Richdale, A. L.; Morris, E. M.; Lawson, L. P. Suicidality in Autistic Adolescents and Adults: Sleep the Unexplored Connection? Autism Research 2025, 18(3), 468–475. [Google Scholar] [CrossRef]
- Santos, S.; Ferreira, H.; Martins, J.; Gonçalves, J.; Castelo-Branco, M. Male sex bias in early and late onset neurodevelopmental disorders: Shared aspects and differences in Autism Spectrum Disorder, Attention Deficit/Hyperactivity Disorder, and Schizophrenia. Neuroscience & Biobehavioral Reviews 2022, 135, 104577. [Google Scholar] [CrossRef]
- Vannucchi, G.; Masi, G.; Toni, C.; Dell’Osso, L.; Marazziti, D.; Perugi, G. Clinical features, developmental course, and psychiatric comorbidity of adult autism spectrum disorders. CNS spectrums 2014, 19(2), 157–164. [Google Scholar] [CrossRef]
| POSITIVE | NEGATIVE | |
|---|---|---|
| General Characteristics | Social support | Demands |
| Appraisals | Life satisfaction | Perceived stress |
| Individual characteristics | Positive personality | Negative coping |
| Outcomes | Happiness | Anxiety and Depression |
| Inclusion | Exclusion | |
|---|---|---|
| Well-being | Well-being, mental well-being, emotional well-being, psychological well-being, social well-being | Physical health, specifically gut problems, and skin disorders |
| Co-morbidities | Depression, Anxiety | ADHD, Epilepsy, Schizophrenia |
| Autistic Traits | Autistic trait, autistic traits, broad autism phenotype | Autism, autism spectrum disorder |
| Sleep Quality | Sleep, sleep quality, poor sleep quality, sleep problems, daytime sleepiness | Sleep disorders such as sleep apnea and delayed sleep-wake phase disorder |
| Age | Adults, university students | Child, children, toddler, toddlers |
| Study type | Reviews, experiments, qualitative research | Brain imaging |
| Authors and year | Objective | Demographic information | Design | Measures |
|---|---|---|---|---|
| Grant, Norton & Hoekstra (2025) [11] | Understand the impact of sensory sensitivity in autistic individuals | 534 adults aged 18 or over. | Online, self-report Survey | Central Sensitisation Inventory (CSI) Sensory Perception Quotient (SPQ) Autism Spectrum Quotient (AQ) PHQ-9 GAD-7 |
| Lodi-Smith et al. (2021) [12] | Exploring the relationship between autistic traits, fatigue and psychological well-being | 294 adults, aged 53 to 96 (average age: approx. 70); 97% white and 57% female. |
Online, self-report Survey | AQ-Short Patient-Reported Outcomes Measurement Information System (PROMIS) Behavioural Risk Factor Surveillance System (BRFSS) PROMIS Depression and Anxiety Scales Satisfaction With Life Scale (SLS) Ryff Psychological Well-Being Scale (short form) |
| Sampson et al. (2021) [13] | Exploring the co-occurrence of autistic traits and psychotic traits | 653 adults, aged between 18 and 65; approx. 81% female | Online, self-report Survey | AQ Community Assessment of Psychic Experiences- positive dimensions (CAPE-p) Centre for Epidemiological Study Depression Scale – Revised (CESDS-R) Deliberate Self-Harm Inventory (DSHI) Suicide Behaviours Questionnaire – Revised (SBQ-R) |
| Nankoo et al. (2019) [14] | Examining the overlaps between autistic traits and ADHD traits, their impact on well-being | 332 university students aged between 17 and 49 (average age: 22) | Lab self-report survey | Adult ADHD Self-Report Scale DASS-21 AQ short with 28 items |
| Authors and year | Objectives | Demographic information | Design | Measures |
|---|---|---|---|---|
| Mantzalas et al. (2024) [15] | Understanding the autistic burnout experience and its impact on well-being | 238 autistic adults aged between 18 and 75; 71% female | Online self-report survey | AASPIRE Autistic Burnout Measure Copenhagen Burnout Inventory |
| Pelton et al. (2023) [16] | Exploring the role of depression and suicidal thoughts in autistic people | 805 adults; 463 autistic and 342 non-autistic. | Online self-report survey | PHQ-9 GAD-7 Interpersonal Needs Questionnaire – 10-item version (INQ-10 Suicidal Behaviours Questionnaire – Revised (SBQ-R) Autism Spectrum Quotient – Short Form) (AQ-short) |
| Levi et al. (2023) [17] | Understanding the experience of social pain in autistic people | 15 autistic adults aged between 18 and 45. | Qualitative research based on interviews | NA |
| Augustin et al. (2020) [18] | Exploring the impact of alexithymia on mental health and well-being. | 60 adults (average age: 42 years) | Mixed methods: interviews, questionnaires and performance tests | Maslach Burnout Inventory (MBI) Beck Depression Inventory (BDI-II) State-Trait Anxiety Inventory (STAI) Toronto Alexithymia Scale (TAS-26) Childhood Trauma Questionnaire (CTQ) |
| Authors and year | Objectives | Demographic information | Design | Measures |
|---|---|---|---|---|
| Lian, Zhang & Jia (2020) [19] | Exploring the impact of sleep duration on brain function and mental health | 5,811 adults aged 45 or over (average age 57.3 years); 56.2% female. | Mixed methods: self-report surveys, cognitive tasks and interviews; longitudinal study. |
Measure developed by CHARLS that includes background, family, health status and functioning, work and retirement, income and expenditure, and COVID-19. |
| Tanielian, Doghramji & Certa (2020) [20] | Exploring the risk factors and predictors of obstructive sleep apnea | 91 adult psychiatric inpatients (59% male, average age 43) | In-person self-report survey. | STOP-BANG questionnaire Epworth Sleepiness Scale (ESS) |
| Yildiz et al. (2020) [21] | Understanding the Correlation between Sleep Problems and Suicidality | 100 participants between the ages of 12 and 18 | Mixed methods: questionnaire and interviews | Pittsburgh Sleep Quality Index (PSQI) Epworth Sleepiness Scale (ESS) Children’s Sleep Habits Questionnaire |
| Authors and year | Objectives | Demographic information | Design | Measures |
|---|---|---|---|---|
| Richdale et al. (2023) [22] | Exploring the impact of sleep quality, fatigue and well-being on depression in autistic adults | 114 autistic people between the ages of 15 and 25 | Online self-report longitudinal study | Pittsburgh Sleep Quality Index (PSQI) Flinders Fatigue Scale (FFS) Hospital Anxiety and Depression Scale – Depression (HADS-D) Social Integration and Social Contribution Scales (SWS-I, SWS-C) |
| Charlton et al. (2022) [23] | Investigating the risk factors of poor sleep quality in autistic people and their impact on mental health | 730 autistic adults aged between 18 and 78 (60% female) recruited through SPARK | Online self-report survey | Pittsburgh Sleep Quality Index (PSQI) GAD-7 PHQ-9 Perceived Stress Scale (PSS) AQ-28 |
| Martini et al. (2022) [24] | Exploring the differences in sex in autistic adults, understanding the impact on well-being and sleep quality | Over 1.3 million people, including 1.6% autistic individuals, are between the ages of 16 and 25. 34% female | Investigative analysis of Swedish medical registers | NA |
| Williams & Gotham (2022) [25] | Investigating the impact of sleep problems on mental health and quality of life in autistic people | 290 autistic young adults between the ages of 18 and 26 (average age: 23) recruited through SPARK | Online self-report survey | Modified PHQ-1 Social Responsiveness Scale – Second Edition (SRS-2) Beck Depression Inventory – Second Edition (BDI-2 GAD-7 World Health Organisation Quality of Life – 4-item version (WHOQoL-4) |
| Authors and year | Proposed conceptual framework |
|---|---|
| Richdale, Morris & Lawson (2025) [28] | Evidence-based commentary explaining that autistic people often have sleep issues, which strongly correlate with suicidality, anxiety and depression. |
| Pelton et al. (2023) [16] | Theoretical framework based on the Interpersonal Theory of Suicide explaining the association between autism and suicidality. |
| Mantzalas, Richdale & Dissanayake (2022) [26] | Theoretical framework linking autistic traits to autistic burnout. |
| Santos et al. (2022) [29] | A review of sex differences between males and females suggests that females are more likely to be misdiagnosed or underdiagnosed. |
| Weir, Allison & Baron-Cohen (2020) [27] | Screening and diagnostic article explaining the common traits of autism and their impact on well-being. |
| Vannucchi et al. (2014) [30] | Review article reporting standard features of autism and their implications. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





