Submitted:
30 January 2026
Posted:
03 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Research Background and Motivation
1.2. Research Gaps
1.2.1. Therapeutic Landscapes in Multicultural Contexts
1.2.2. AI-Driven Evacuation Modeling and Agent-Based Simulation
1.2.3. Multilingual Metaverse for Inclusive Healthcare
1.3. Research Objectives and Contributions
- Develop and validate an AI driven agent based evacuation simulation framework that accounts for role based behavioral heterogeneity among doctors, nurses, and patients, and systematically compares the performance of a Q learning based strategy with a knowledge biased stochastic walk baseline under earthquake induced emergency scenarios.
- Design and prototype a multilingual Medical Metaverse interface that supports inclusive and barrier free interaction for linguistically diverse users across both virtual and physical healthcare environments, with a particular focus on accessibility for elderly and ethnic minority populations.
- Integrate evacuation modeling and digital interface design within a holistic evidence based framework that connects therapeutic landscape principles, emergency preparedness, and digital health innovation, thereby informing resilient hospital planning and improving building level seismic resilience.
- Methodological innovation in evacuation simulation.This study develops a comparative agent based evacuation modeling framework that employs a Q learning based strategy and a knowledge biased stochastic walk baseline to simulate heterogeneous crowd behaviors during hospital evacuation scenarios. Through quantitative analysis of evacuation trajectories, flow patterns, and performance indicators including distance time relationships and T50 and T90 metrics, the framework provides empirical evidence on how algorithm supported strategies can improve evacuation efficiency and consistency in healthcare specific spatial environments under emergency conditions.
- Prototype development of a multilingual digital interface for healthcare accessibility.A proof of concept Medical Metaverse platform is introduced to support multilingual interaction and inclusive access to healthcare information. By integrating a bilingual digital human interface that supports Mandarin Chinese, the Yi language, and English, the system demonstrates the technical feasibility of reducing linguistic and cognitive barriers in minority serving hospitals. The prototype highlights the potential role of culturally adaptive digital interfaces in improving communication, wayfinding, and preparedness in both routine and emergency contexts.
- Holistic integration into evidence based hospital design.The study synthesizes therapeutic landscape principles, AI driven spatial evaluation, and inclusive digital service design into a unified framework for hospital planning in resource constrained and culturally diverse regions. By bridging architectural design, computational modeling, and healthcare operations, the proposed framework supports building level seismic resilience and emergency preparedness while offering practical insights for policy and practice in underserved regions.
2. Theoretical Background
2.1. Therapeutic Landscapes and Evidence-Based Design
2.2. Medical Metaverse and Digital Twins
2.3. Agent-Based Modeling for Human Behavior Simulation
2.4. Reinforcement Learning and Spatial Optimization
3. Materials and Methods
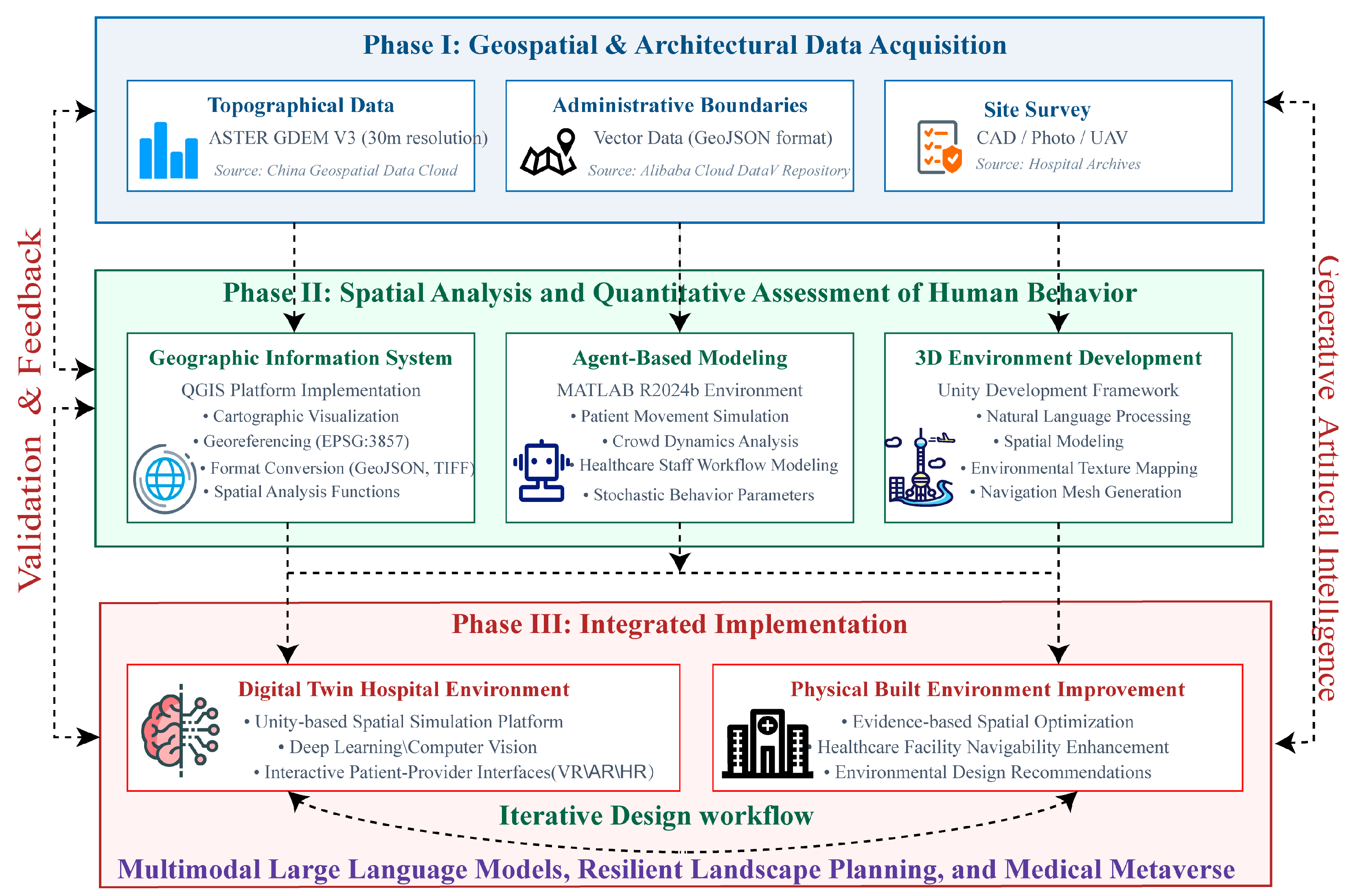
3.1. Research Framework and Process
3.2. Site Selection, Context and Date Source
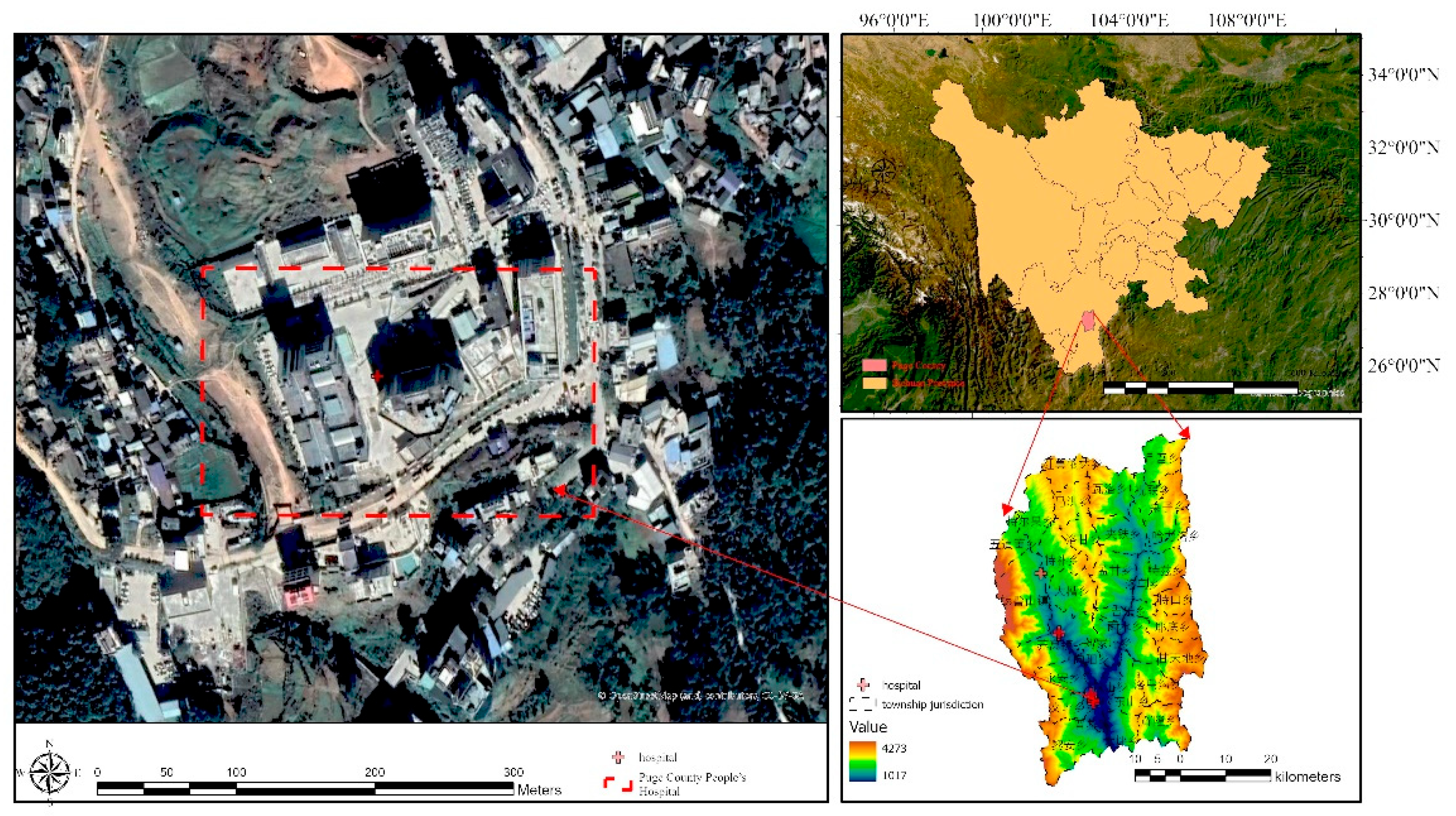
3.2.1. Site Selection
3.2.2. Cultural Context
3.2.3. Data Selection
3.3. Evidence-Based Design
3.4. Behavioral Simulation Framework
3.4.1. Spatial Dynamics and Role Heterogeneity
3.4.2. Baseline Model: Knowledge-Biased Stochastic Walk
3.4.3. Advanced Model: Q-Learning Enhanced Navigation
4. Results
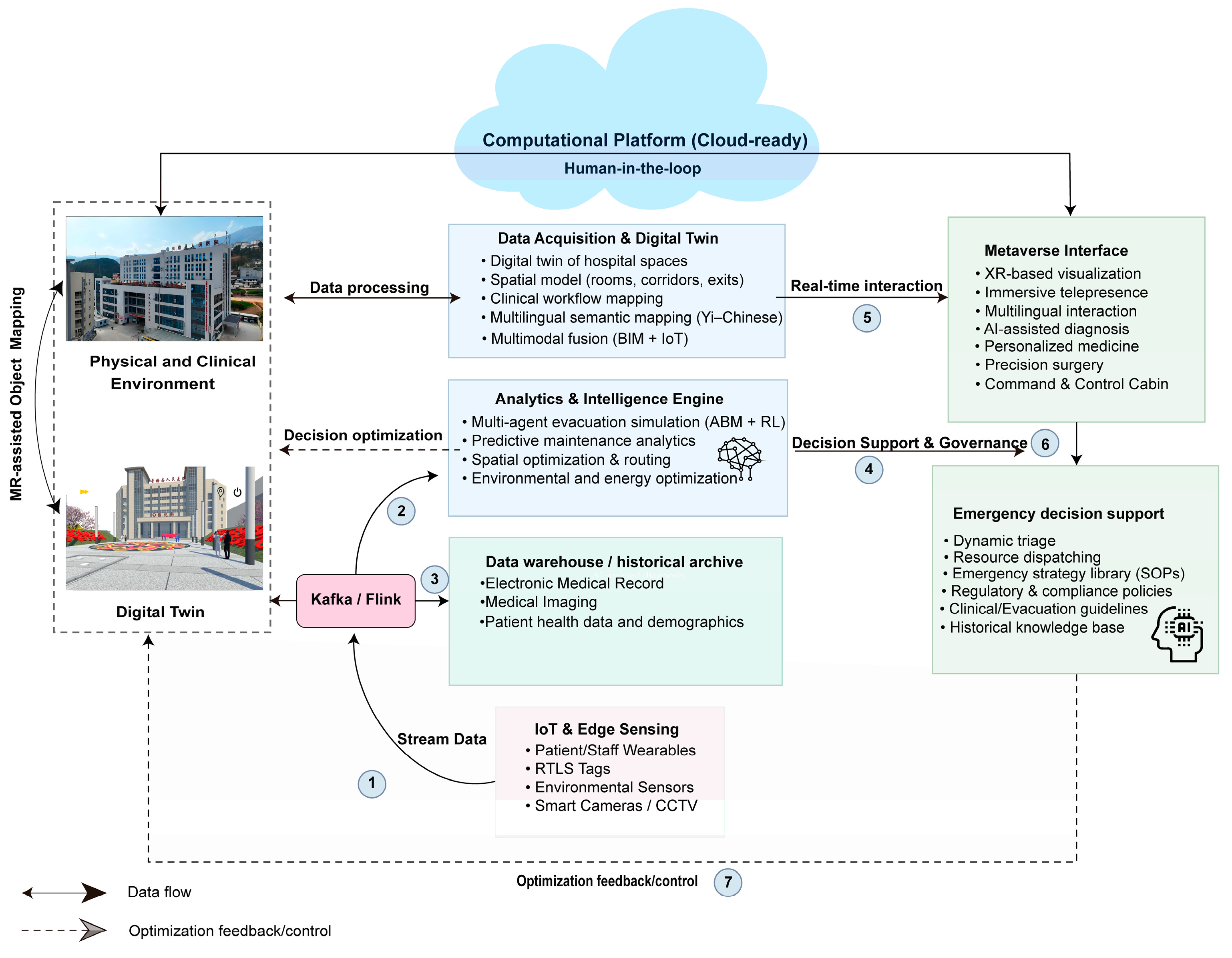
4.1. Construction of the Medical Metaverse Architecture
4.1.1. Digital Twin Integration
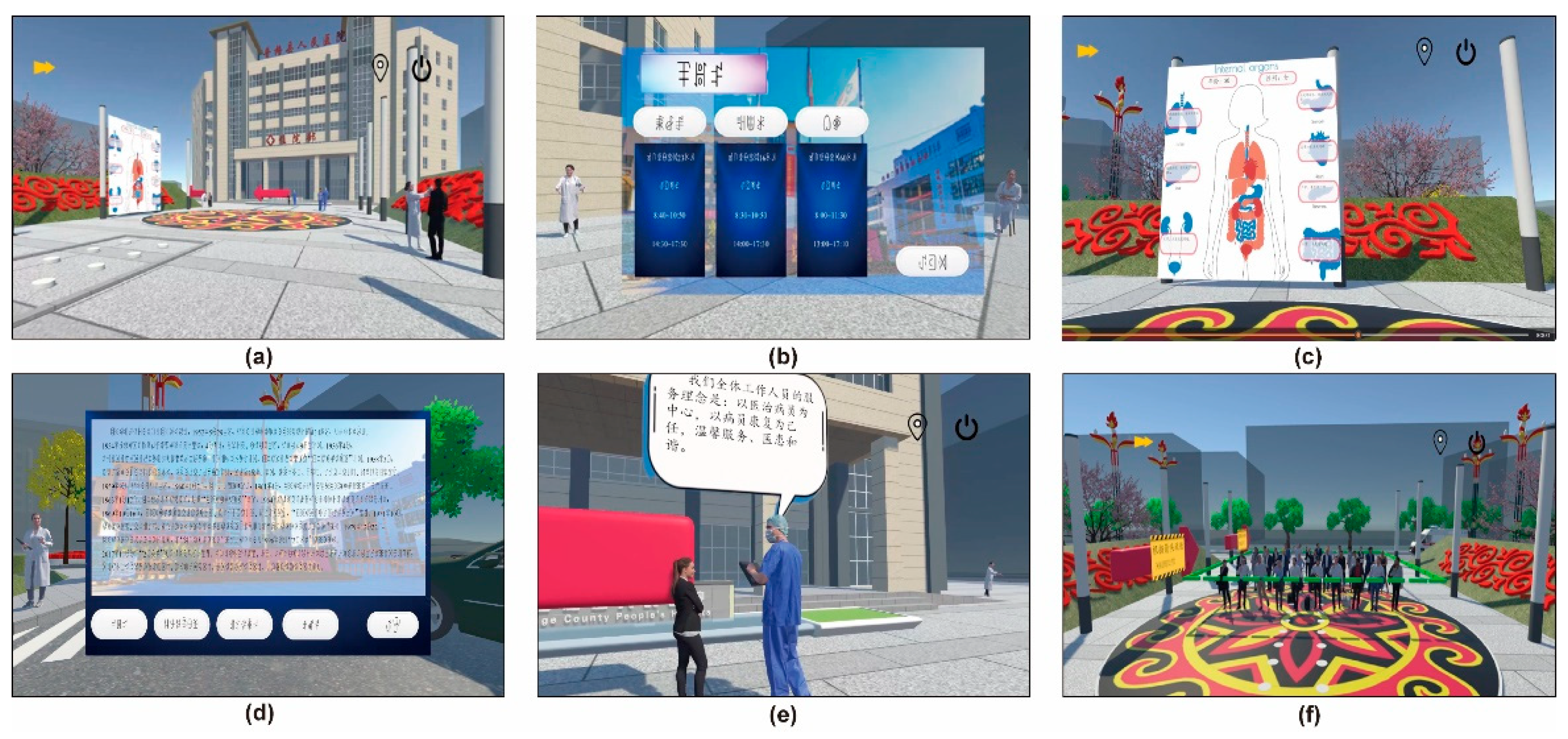
4.1.2. Multilingual Interface and Inclusive Interaction
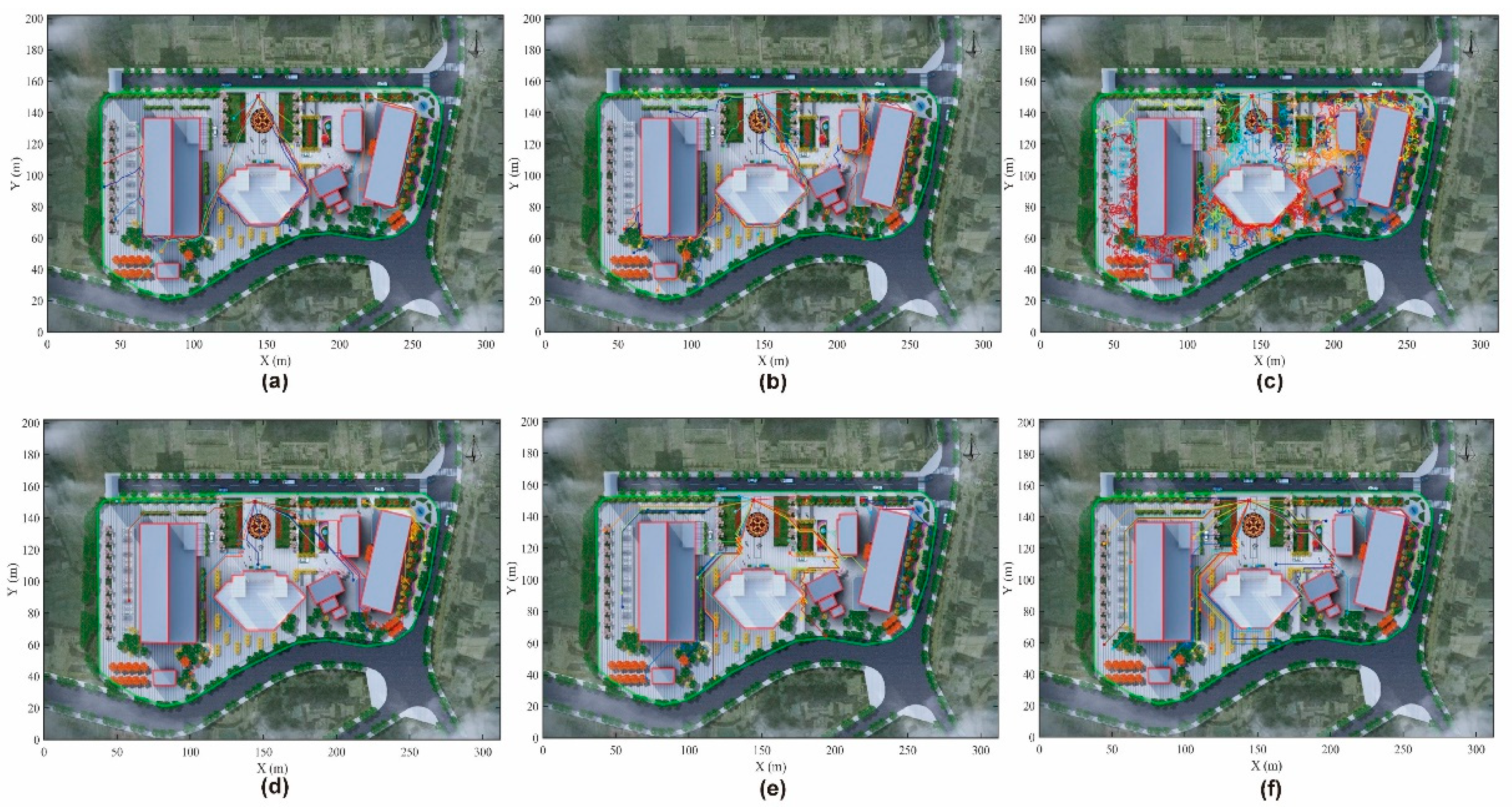
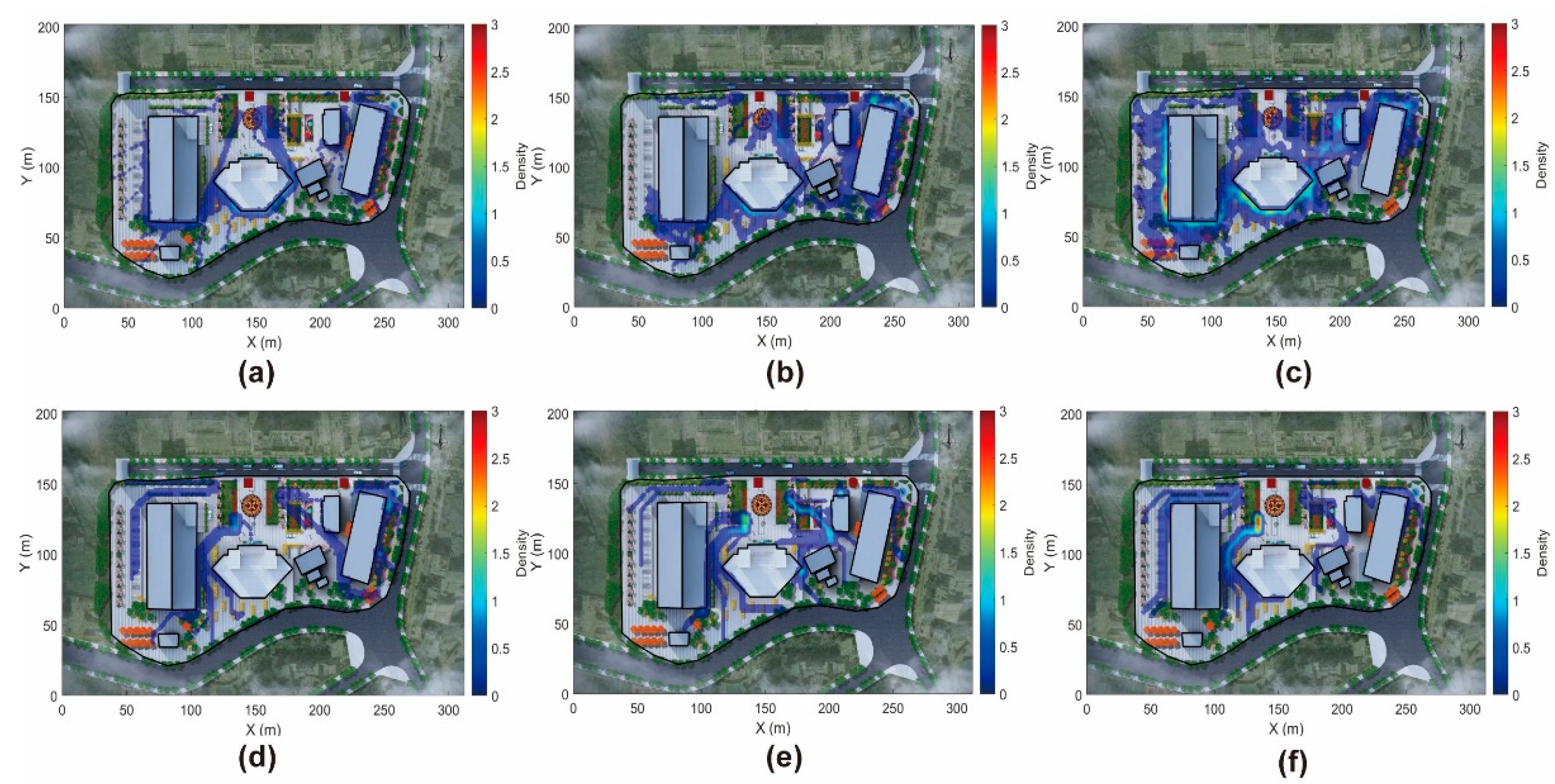
4.2. Spatial Patterns and Evacuation Dynamics
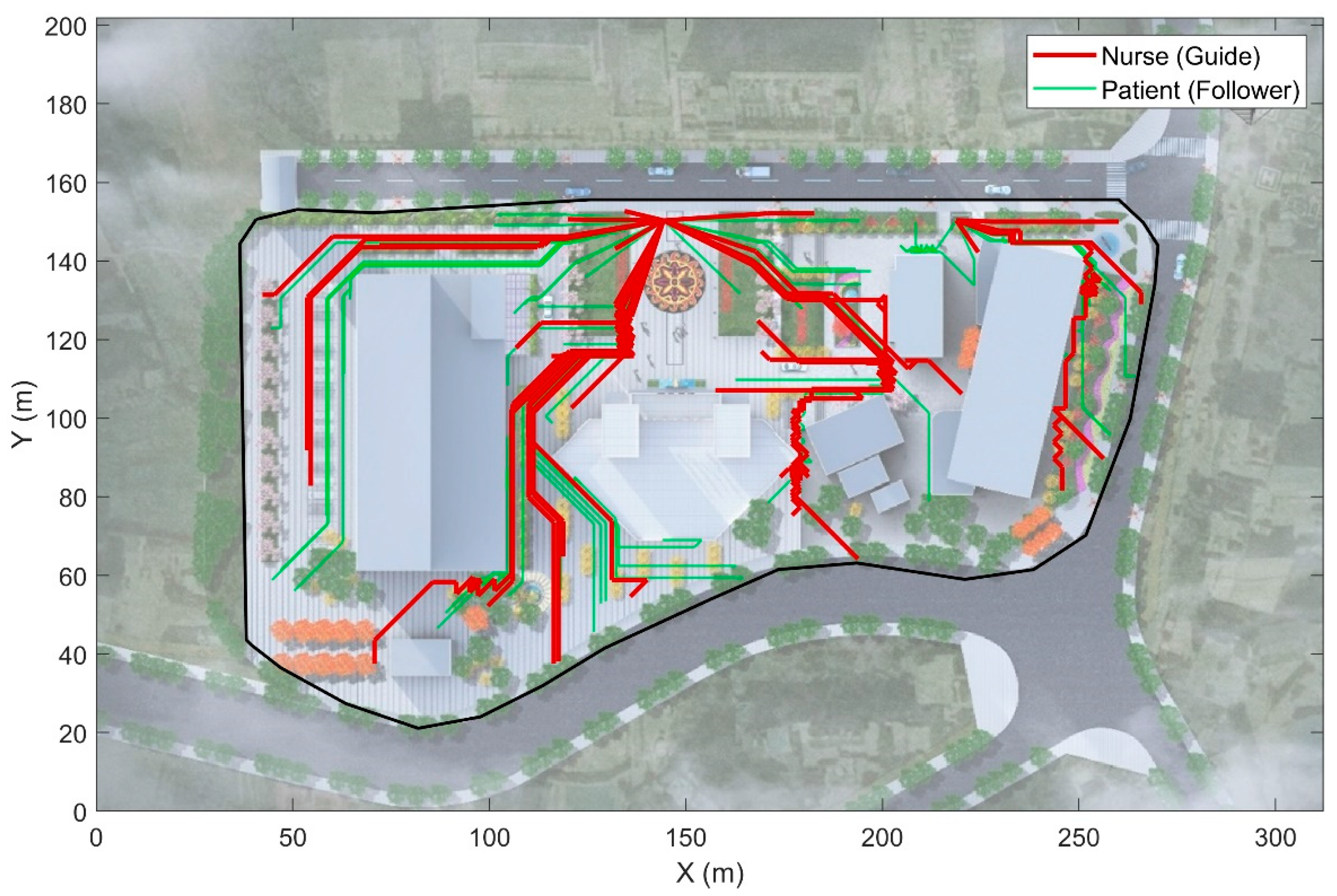
4.2.1. Role-Based Spatial Distribution and Behavioral Heterogeneity
4.2.2. Emergent Social Behaviors
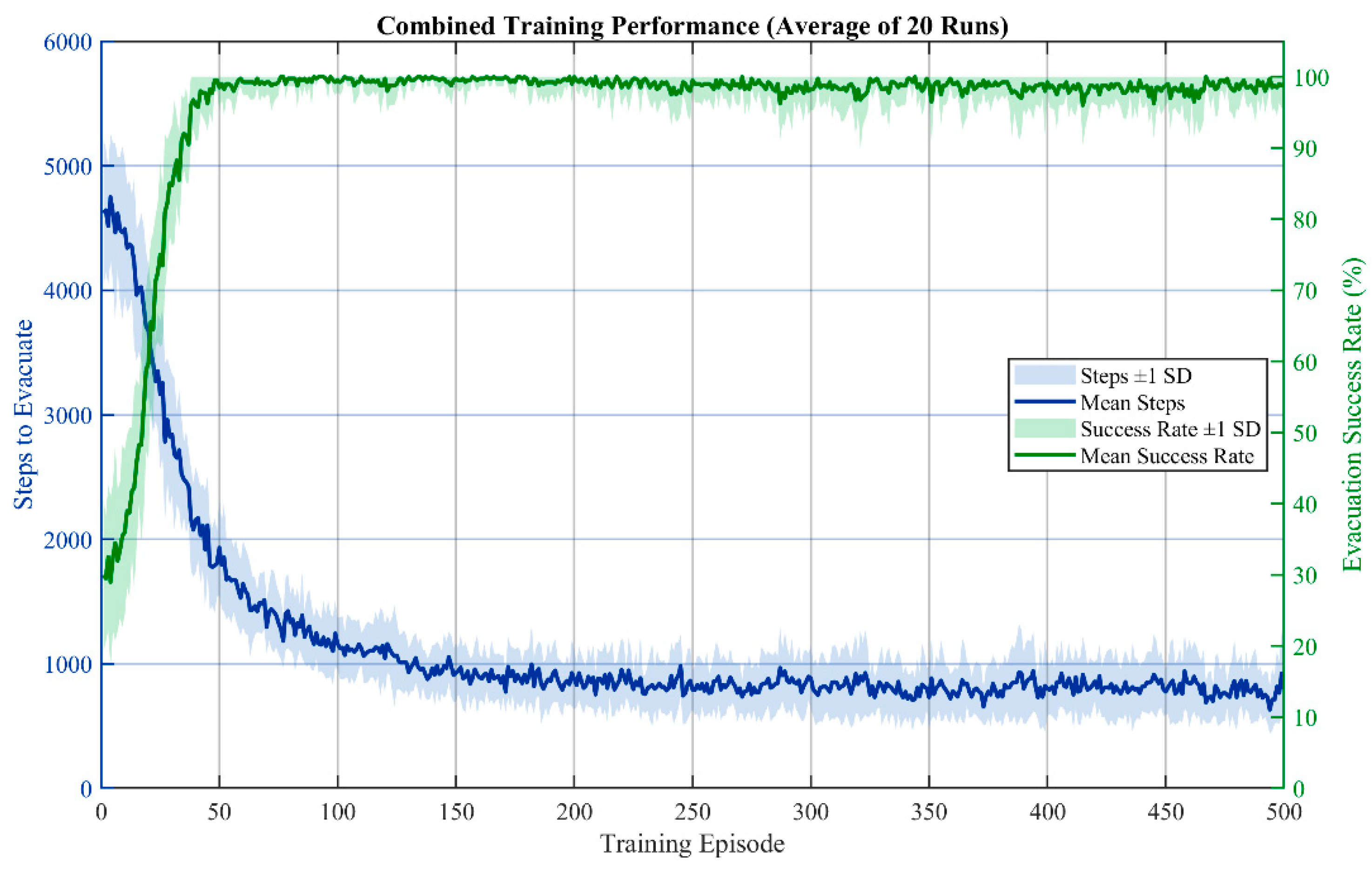
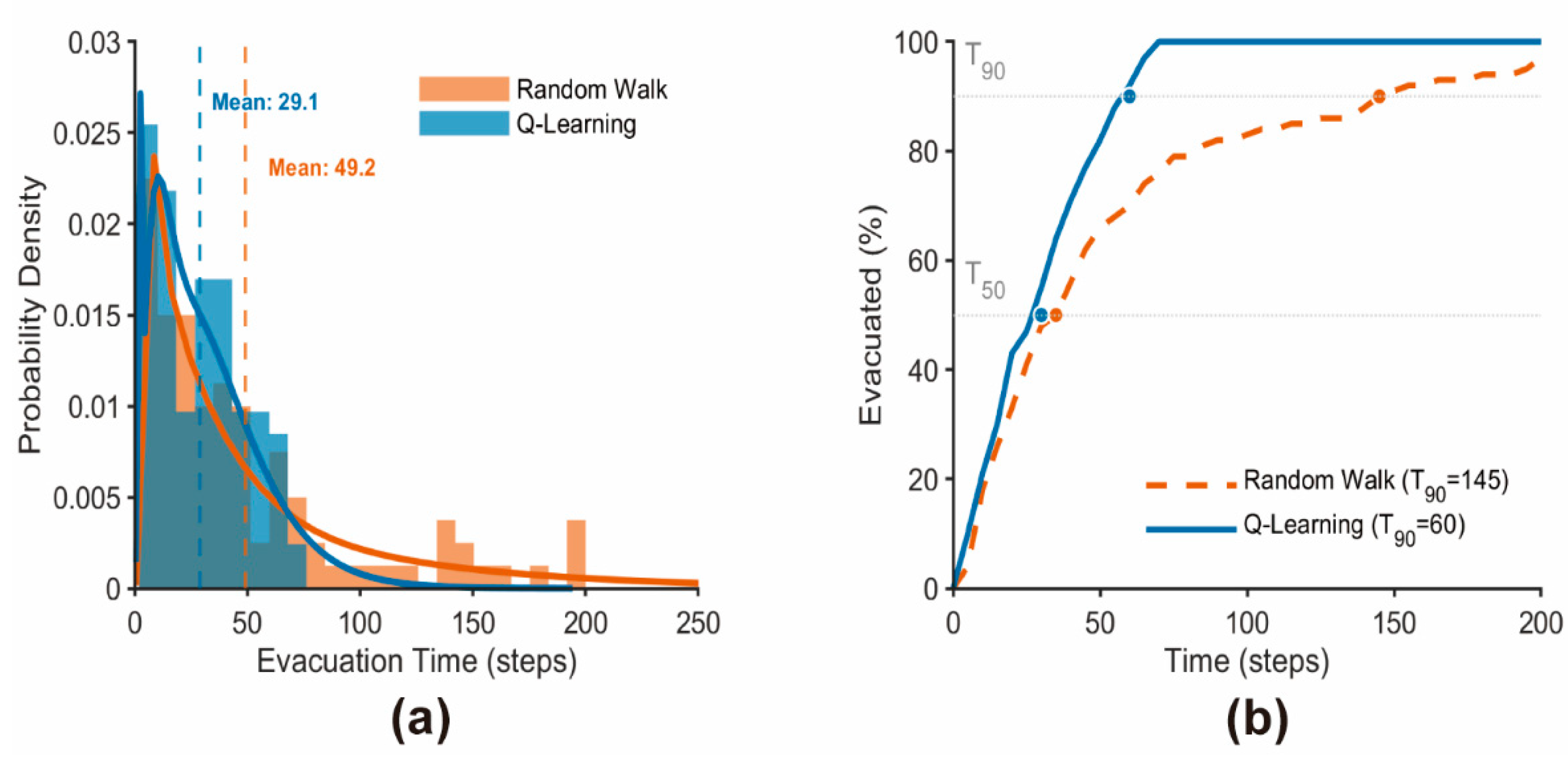
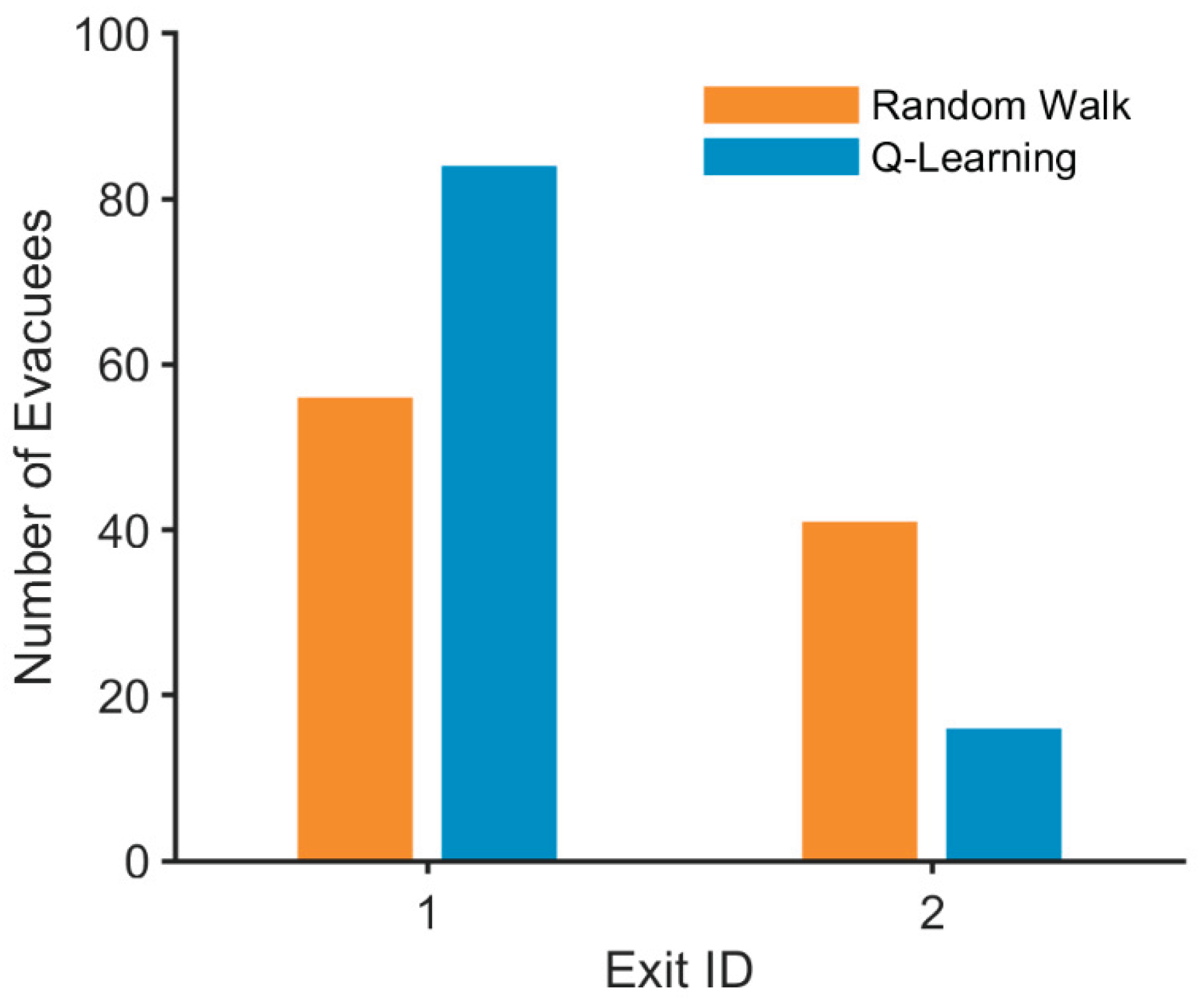
4.2.3. Algorithmic Performance and Evacuation Efficiency
5. Discussion
5.1. Promoting Resilience through AI-Driven Design
5.2. Bridging the Digital Divide for Social Sustainability
5.3. Limitations and Future Directions
6. Conclusions
Author Contributions
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ABM | Agent-Based Modeling |
| AI | Artificial Intelligence |
| AWR | Area-Weighted Reward |
| DT | Digital Twin |
| GIS | Geographic Information System |
| PCPH | Puge County People's Hospital |
| RL | Reinforcement Learning |
| RW | Random Walk |
| Time to 90% Evacuation Completion |
Appendix A
Appendix A.1. Additional Quantitative Analyses of Evacuation Performance
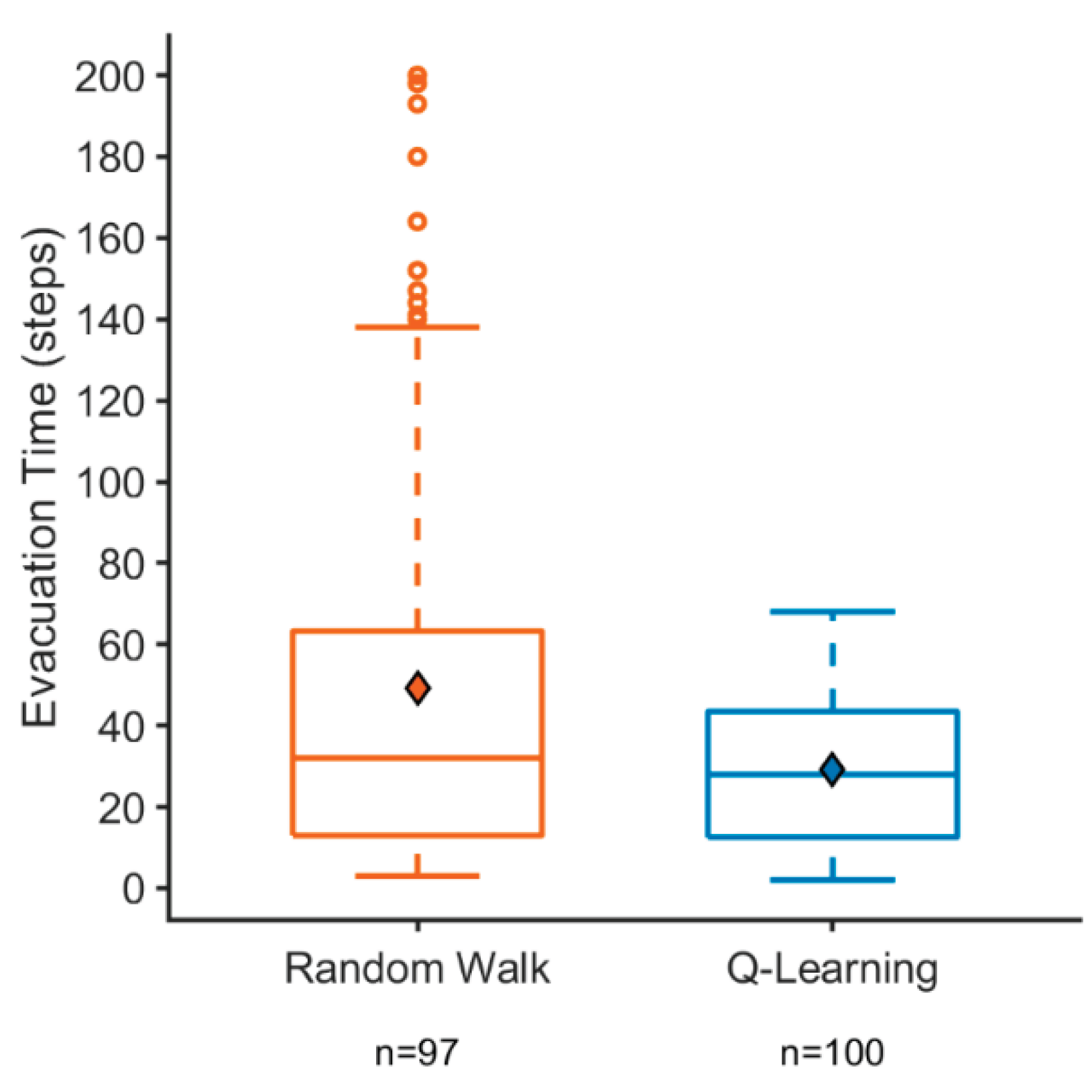
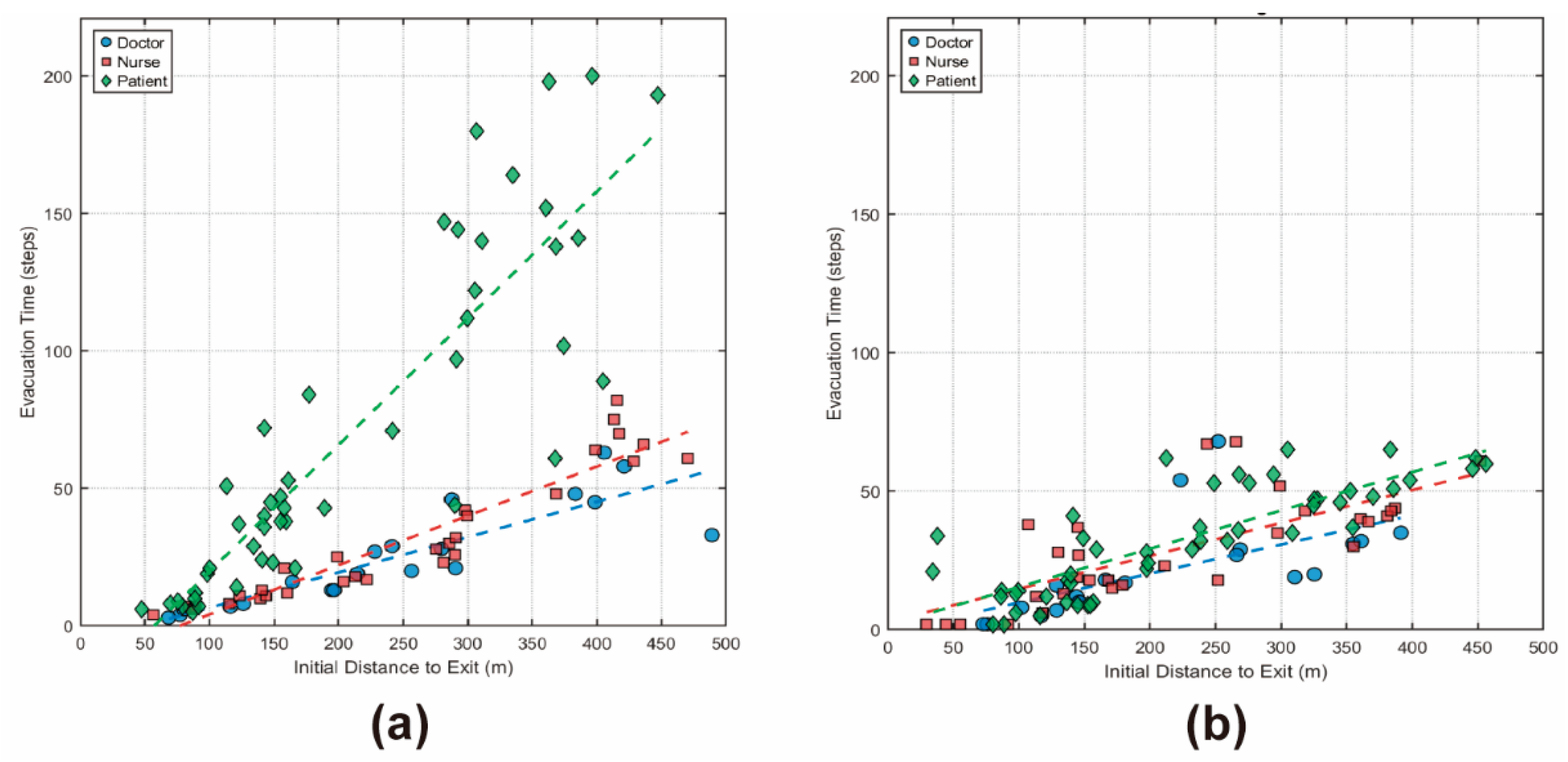
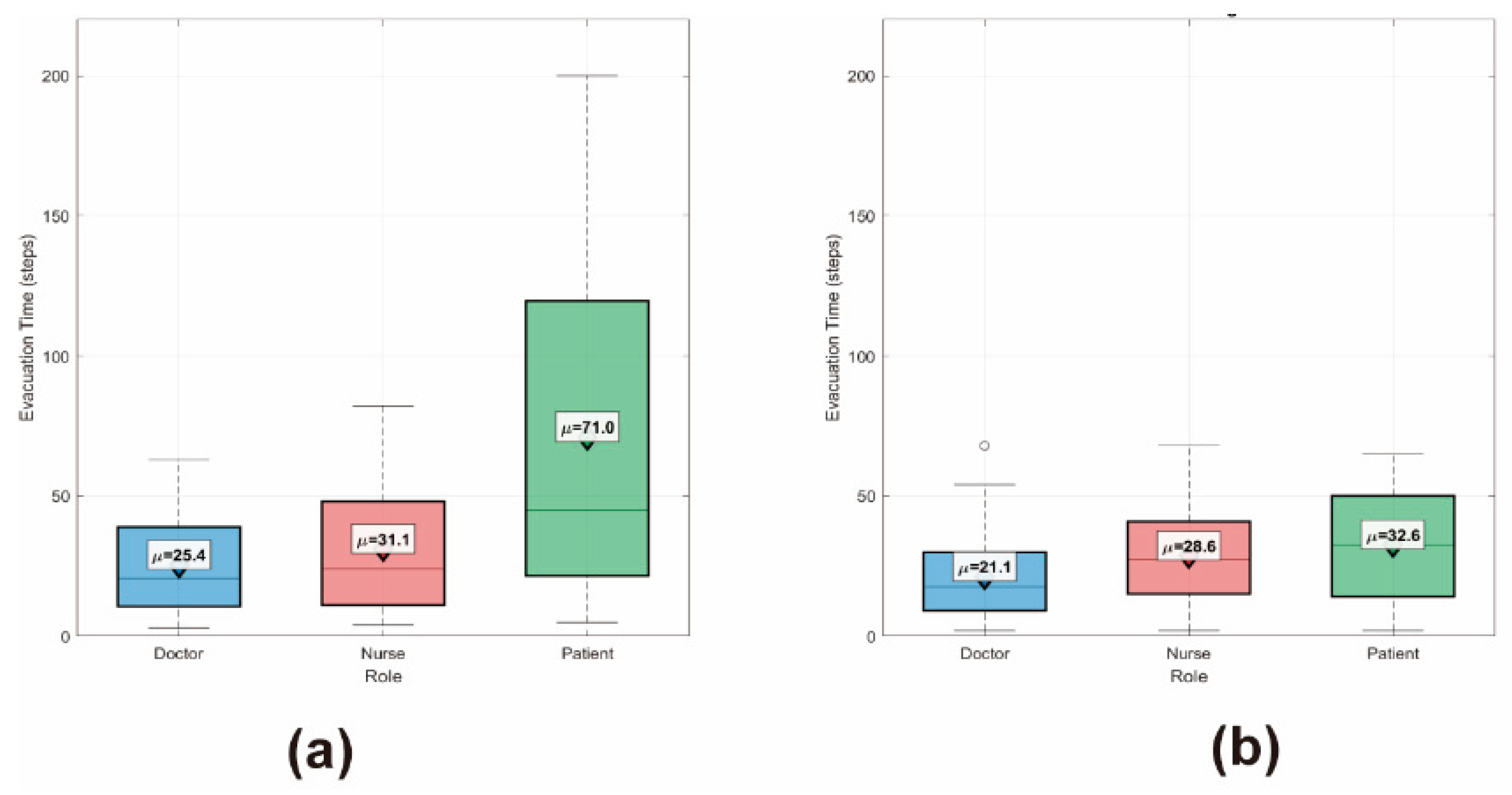
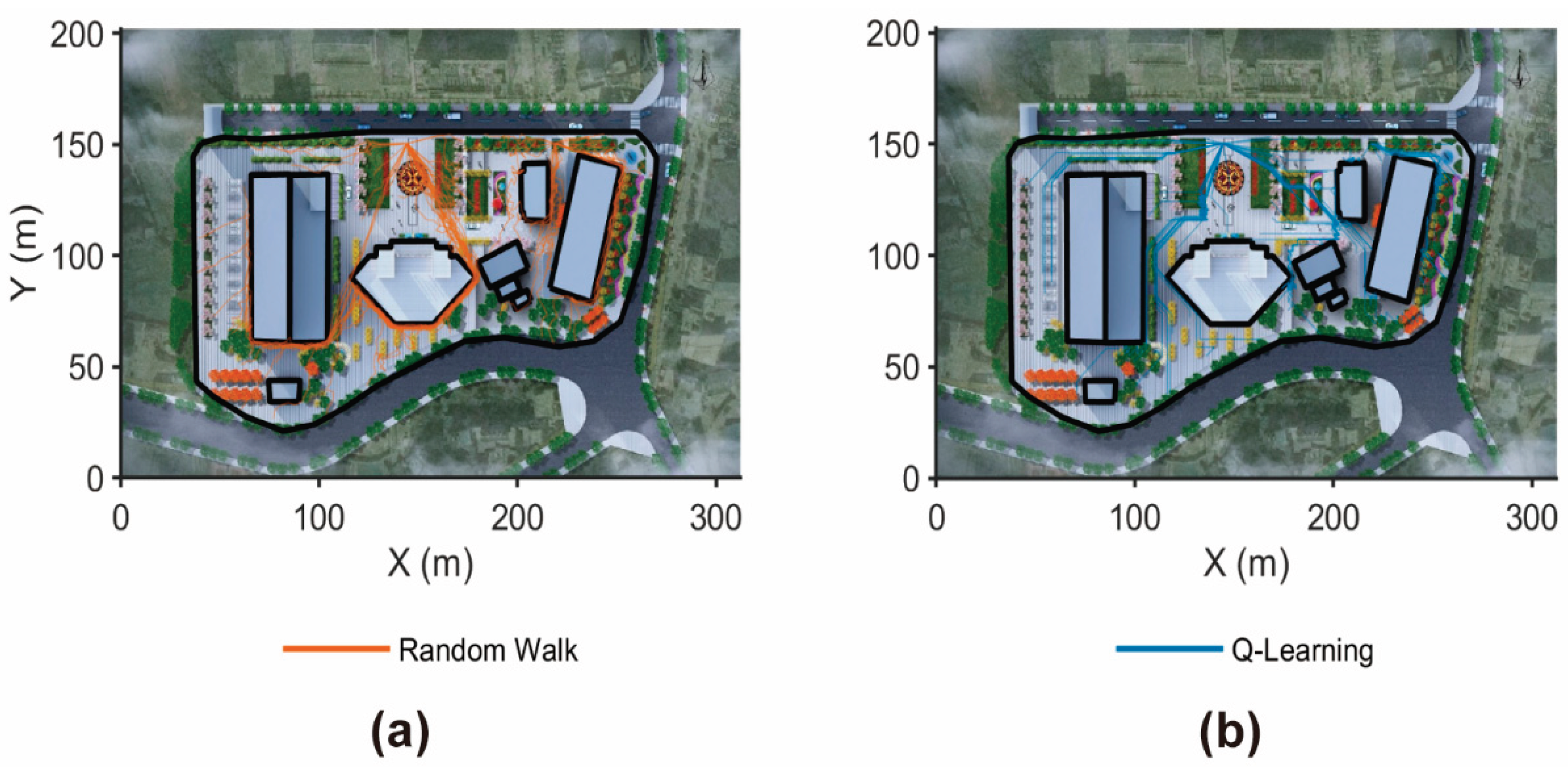
References
- State Council of the People’s Republic of China. Healthy China 2030 planning outline. Available online: https://www.gov.cn/xinwen/2016-10/25/content_5124174.htm (accessed on 27 October 2025).
- United Nations Transforming Our World: The 2030 Agenda for Sustainable Development. Available online: https://sdgs.un.org/2030agenda (accessed on 20 January 2026).
- Zhang, Y.; Wu, T.; Yu, H.; Fu, J.; Xu, J.; Liu, L.; Tang, C.; Li, Z. Green Spaces Exposure and the Risk of Common Psychiatric Disorders: A Meta-Analysis. SSM - Popul. Health 2024, 25, 101630. [Google Scholar] [CrossRef] [PubMed]
- Gao, H.; Li, J.; Chen, X.; Shen, Y. Combined Concrete and Cable Restrainers to Prevent Longitudinal Unseating of Highway Bridges during Earthquakes. Engineering Structures 2024, 314, 118388. [Google Scholar] [CrossRef]
- Bruneau, M.; Reinhorn, A. Exploring the Concept of Seismic Resilience for Acute Care Facilities. Earthquake Spectra 2007, 23, 41–62. [Google Scholar] [CrossRef]
- Schultz, C.; Koenig, K.; Lewis, R. Implications of Hospital Evacuation after the Northridge, California, Earthquake. The New England journal of medicine 2003, 348, 1349–1355. [Google Scholar] [CrossRef]
- Ceferino, L.; Mitrani-Reiser, J.; Kiremidjian, A.; Deierlein, G.; Bambarén, C. Effective Plans for Hospital System Response to Earthquake Emergencies. Nat Commun 2020, 11, 4325. [Google Scholar] [CrossRef]
- Al Khatib, I.; Samara, F.; Ndiaye, M. A Systematic Review of the Impact of Therapeutical Biophilic Design on Health and Wellbeing of Patients and Care Providers in Healthcare Services Settings. Front. Built Environ. 2024, 10. [Google Scholar] [CrossRef]
- Wang, J.; Luo, Y.; Zhou, X.; Zhao, W.; Lei, Y.; Xie, W. Impact of Assistance Behavior on Evacuation Efficiency in High-Rise Hospital Inpatient Buildings: An Agent-Based Simulation Study. J. Build. Eng. 2025, 112, 113780. [Google Scholar] [CrossRef]
- Ali, S.; Abdullah; Armand, T.P.T.; Athar, A.; Hussain, A.; Ali, M.; Yaseen, M.; Joo, M.-I.; Kim, H.-C. Metaverse in Healthcare Integrated with Explainable AI and Blockchain: Enabling Immersiveness, Ensuring Trust, and Providing Patient Data Security. Sens. 2023, 23, 565. [Google Scholar] [CrossRef]
- Chen, C.; Koll, C.; Wang, H.; Lindell, M.K. An Interdisciplinary Agent-Based Evacuation Model: Integrating the Natural Environment, Built Environment, and Social System for Community Preparedness and Resilience. [CrossRef]
- Fattahi Maassoum, A.S.; Farkisch, H.; Taji, M. AI-Based Hospital Design Process through Neuro-Symbolic Strategies. Arch. Bone Jt. Surg. 2025, 13, 442–456. [Google Scholar] [CrossRef]
- Islas-Toski, M.; Cuevas, E.; Pérez-Cisneros, M.; Escobar, H. Agent-Based Evacuation Modeling: Enhancing Building Safety in Emergency Scenarios. Smart Cities 2024, 7, 3165–3187. [Google Scholar] [CrossRef]
- Haghpanah, F.; Ghobadi, K.; Schafer, B.W. Multi-Hazard Hospital Evacuation Planning during Disease Outbreaks Using Agent-Based Modeling. Int J Disaster Risk Reduct 2021, 66, 102632. [Google Scholar] [CrossRef] [PubMed]
- Wan, Z.; Yang, F.; Zhou, T.; Li, C. The Effects of Spatial Layout on Efficiency of Safe Evacuation After Conversion of an Exhibition Building to a Fangcang Shelter Hospital. Buildings 2025, 15, 2880. [Google Scholar] [CrossRef]
- Geoerg, P.; de Schot, L.; Lovreglio, R. Decoding Hospital Evacuation Drills: Pre-Movement and Movement Analysis in New Zealand. Fire Technol 2025, 61, 4303–4329. [Google Scholar] [CrossRef]
- Wang, G.; Badal, A.; Jia, X.; Maltz, J.S.; Mueller, K.; Myers, K.J.; Niu, C.; Vannier, M.; Yan, P.; Yu, Z.; et al. Development of Metaverse for Intelligent Healthcare. Nat. Mach. Intell. 2022, 4, 922–929. [Google Scholar] [CrossRef]
- Buragohain, D.; Khichar, S.; Deng, C.; Meng, Y.; Chaudhary, S. Analyzing Metaverse-Based Digital Therapies, Their Effectiveness, and Potential Risks in Mental Healthcare. Sci. Rep. 2025, 15. [Google Scholar] [CrossRef]
- Building Climate-Resilient Health Systems. Available online: https://www.who.int/teams/environment-climate-change-and-health/climate-change-and-health/country-support/building-climate-resilient-health-systems (accessed on 8 November 2025).
- Gesler, W.M. Therapeutic Landscapes: Medical Issues in Light of the New Cultural Geography. Soc. Sci. Med. 1992, 34, 735–746. [Google Scholar] [CrossRef]
- Healing Gardens: Therapeutic Benefits and Design Recommendations; Marcus, C.C., Barnes, M., Eds.; Wiley series in healthcare and senior living design; Wiley: New York, 1999; ISBN 978-0-471-19203-9.
- Hamilton, D.K.; Watkins, D.H. Evidence-Based Design for Multiple Building Types; Wiley: Hoboken (N.J), 2009; ISBN 978-0-470-12934-0. [Google Scholar]
- Stier-Jarmer, M.; Throner, V.; Kirschneck, M.; Immich, G.; Frisch, D.; Schuh, A. The Psychological and Physical Effects of Forests on Human Health: A Systematic Review of Systematic Reviews and Meta-Analyses. International Journal of Environmental Research and Public Health 2021, 18, 1770. [Google Scholar] [CrossRef]
- Ulrich, R.S. View through a Window May Influence Recovery from Surgery. Science 1984, 224, 420–421. [Google Scholar] [CrossRef] [PubMed]
- Guo, F.; Miao, S.; Xu, S.; Luo, M.; Dong, J.; Zhang, H. Multi-Objective Optimization Design for Cold-Region Office Buildings Balancing Outdoor Thermal Comfort and Building Energy Consumption. Energies 2025, 18, 62. [Google Scholar] [CrossRef]
- Liu, T.; Wang, J.; Zhou, D.; Meng, X.; Luo, X.; Wang, Y. Research on Optimization Design Strategies for Natural Ventilation in Living Units of Institutional Elderly Care Facilities Based on Computational Fluid Dynamics Simulation. Buildings 2024, 14, 1648. [Google Scholar] [CrossRef]
- Shao, L.; Tang, W.; Zhang, Z.; Chen, X. Medical Metaverse: Technologies, Applications, Challenges and Future. J. Mech. Med. Biol. 2023, 23, 2350028. [Google Scholar] [CrossRef]
- Katsoulakis, E.; Wang, Q.; Wu, H.; Shahriyari, L.; Fletcher, R.; Liu, J.; Achenie, L.; Liu, H.; Jackson, P.; Xiao, Y.; et al. Digital Twins for Health: A Scoping Review. npj Digital Med. 2024, 7, 77. [Google Scholar] [CrossRef] [PubMed]
- Ringeval, M.; Sosso, F.A.E.; Cousineau, M.; Paré, G. Advancing Health Care with Digital Twins: Meta-Review of Applications and Implementation Challenges. J Med Internet Res 2025, 27, e69544. Available online: https://www.jmir.org/2025/1/e69544. [CrossRef] [PubMed]
- Rehan, M.W.; Rehan, M.M. Survey, Taxonomy, and Emerging Paradigms of Societal Digital Twins for Public Health Preparedness. npj Digital Med. 2025, 8, 520. [Google Scholar] [CrossRef] [PubMed]
- Tudor, B.H.; Shargo, R.; Gray, G.M.; Fierstein, J.L.; Kuo, F.H.; Burton, R.; Johnson, J.T.; Scully, B.B.; Asante-Korang, A.; Rehman, M.A.; et al. A Scoping Review of Human Digital Twins in Healthcare Applications and Usage Patterns. npj Digital Med. 2025, 8, 587. [Google Scholar] [CrossRef]
- Asciak, L.; Kyeremeh, J.; Luo, X.; Kazakidi, A.; Connolly, P.; Picard, F.; O’Neill, K.; Tsaftaris, S.A.; Stewart, G.D.; Shu, W. Digital Twin Assisted Surgery, Concept, Opportunities, and Challenges. npj Digital Med. 2025, 8, 32. [Google Scholar] [CrossRef]
- Vallée, A. Digital Twin for Healthcare Systems. [CrossRef]
- Dinu Roman Szabo, M.; Dumitras, A.; Mircea, D.-M.; Doroftei, D.; Sestras, P.; Boscaiu, M.; Brzuszek, R.F.; Sestras, A.F. Touch, Feel, Heal. The Use of Hospital Green Spaces and Landscape as Sensory-Therapeutic Gardens: A Case Study in a University Clinic. [CrossRef]
- Sung, W.-P.; Huang, C.-S.; Wang, P.-T.; Yang, M.-Y. Integrating AI Generation and CFD Simulation in Coastal Hospital Landscape Design: A Case Study of Penghu, Taiwan. Buildings 2025, 15, 3283. [Google Scholar] [CrossRef]
- Bonabeau, E. Agent-Based Modeling: Methods and Techniques for Simulating Human Systems. Proc. Natl. Acad. Sci. 2002, 99, 7280–7287. [Google Scholar] [CrossRef] [PubMed]
- Helbing, D.; Farkas, I.; Vicsek, T. Simulating Dynamical Features of Escape Panic. Nature 2000, 407, 487–490. [Google Scholar] [CrossRef]
- Park, J.S.; O’Brien, J.; Cai, C.J.; Morris, M.R.; Liang, P.; Bernstein, M.S. Generative Agents: Interactive Simulacra of Human Behavior. In Proceedings of the Proceedings of the 36th Annual ACM Symposium on User Interface Software and Technology, 2023; Association for Computing Machinery: New York, NY, USA; pp. 1–22. [Google Scholar]
- Macal, C.M.; North, M.J. Tutorial on Agent-Based Modelling and Simulation. Journal of Simulation 2010, 4, 151–162. [Google Scholar] [CrossRef]
- An, L.; Grimm, V.; Sullivan, A.; Turner, B.L., II; Malleson, N.; Heppenstall, A.; Vincenot, C.; Robinson, D.; Ye, X.; Liu, J.; et al. Challenges, Tasks, and Opportunities in Modeling Agent-Based Complex Systems. Ecological Modelling 2021, 457, 109685. [Google Scholar] [CrossRef]
- Manson, S.M.; Sun, S.; Bonsal, D. Agent-Based Modeling and Complexity. In Agent-Based Models of Geographical Systems; Heppenstall, A.J., Crooks, A.T., See, L.M., Batty, M., Eds.; Springer Netherlands: Dordrecht, 2012; pp. 125–139. ISBN 978-90-481-8927-4. [Google Scholar]
- Grimm, V.; Railsback, S.F.; Vincenot, C.E.; Berger, U.; Gallagher, C.; DeAngelis, D.L.; Edmonds, B.; Ge, J.; Giske, J.; Groeneveld, J.; et al. The ODD Protocol for Describing Agent-Based and Other Simulation Models: A Second Update to Improve Clarity, Replication, and Structural Realism. J. Artif. Soc. Soc. Simul. 2020, 23, 7. [Google Scholar] [CrossRef]
- Manson, S.; An, L.; Clarke, K.C.; Heppenstall, A.; Koch, J.; Krzyzanowski, B.; Morgan, F.; O’Sullivan, D.; Runck, B.C.; Shook, E.; et al. Methodological Issues of Spatial Agent-Based Models. J. Artif. Soc. Soc. Simul. 2020, 23, 3. [Google Scholar] [CrossRef]
- Huang, R.; He, H.; Su, Q. Towards a Fossil-Free Urban Transport System: An Intelligent Cross-Type Transferable Energy Management Framework Based on Deep Transfer Reinforcement Learning. Applied Energy 2024, 363, 123080. [Google Scholar] [CrossRef]
- Tian, W.; Fu, G.; Xin, K.; Zhang, Z.; Liao, Z. Improving the Interpretability of Deep Reinforcement Learning in Urban Drainage System Operation. Water Research 2024, 249, 120912. [Google Scholar] [CrossRef]
- Shen, J.; Zheng, F.; Ma, Y.; Deng, W.; Zhang, Z. Urban Travel Carbon Emission Mitigation Approach Using Deep Reinforcement Learning. Sci Rep 2024, 14, 27778. [Google Scholar] [CrossRef]
- Equihua, J.; Beckmann, M.; Seppelt, R. Connectivity Conservation Planning through Deep Reinforcement Learning. Methods in Ecology and Evolution 2024, 15, 779–790. [Google Scholar] [CrossRef]
- Heinbach, B.; Burggräf, P.; Steinberg, F. From Theory to Application: Investigating the Generalizability of Facility Layout Problems Using a Deep Reinforcement Learning Approach. Prod. Eng. Res. Devel. 2025, 19, 975–991. [Google Scholar] [CrossRef]
- Chung, K.T.; Lee, C.K.M.; Tsang, Y.P. Neural Combinatorial Optimization with Reinforcement Learning in Industrial Engineering: A Survey. Artificial Intelligence Review 2025, 58, 130. [Google Scholar] [CrossRef]
- Liang, H.; Wang, S.; Li, H.; Zhou, L.; Chen, H.; Zhang, X.; Chen, X. Sponet: Solve Spatial Optimization Problem Using Deep Reinforcement Learning for Urban Spatial Decision Analysis. International Journal of Digital Earth 2024, 17, 2299211. [Google Scholar] [CrossRef]
- Kakooee, R.; Dillenburger, B. Reimagining Space Layout Design through Deep Reinforcement Learning. J Comput Des Eng 2024, 11, 43–55. [Google Scholar] [CrossRef]
- Kool, W.; van Hoof, H.; Gromicho, J.; Welling, M. Deep Policy Dynamic Programming for Vehicle Routing Problems. In Proceedings of the Integration of Constraint Programming, Artificial Intelligence, and Operations Research; Schaus, P., Ed.; Springer International Publishing: Cham, 2022; pp. 190–213. [Google Scholar]
- Chiboub, A.; Francois, J.; Alix, T.; Dupas, R. Contribution of Deep Reinforcement Learning to Solve Reconfigurable Facilities Layout Problems. Manuf. Lett. 2025, 46, 16–20. [Google Scholar] [CrossRef]
- Li, Y.; Zhang, X.; Zeng, T.; Duan, J.; Wu, C.; Wu, D.; Chen, X. Task Placement and Resource Allocation for Edge Machine Learning: A GNN-Based Multi-Agent Reinforcement Learning Paradigm. IEEE Trans. Parallel Distrib. Syst. 2023, 34, 3073–3089. [Google Scholar] [CrossRef]
- Xu, Y.; Fang, M.; Chen, L.; Xu, G.; Du, Y.; Zhang, C. Reinforcement Learning with Multiple Relational Attention for Solving Vehicle Routing Problems. IEEE Trans. Cybern. 2022, 52, 11107–11120. [Google Scholar] [CrossRef]
- Kool, W.; van Hoof, H.; Welling, M. Attention, Learn to Solve Routing Problems! 2019.
- Guo, W.; Wang, R.; Xu, Y.; Jin, Y. Unified and Generalizable Reinforcement Learning for Facility Location Problems on Graphs; 29 January 2025. [Google Scholar]
- Oroojlooyjadid, A.; Nazari, M.; Snyder, L.V.; Takáč, M. A Deep Q-Network for the Beer Game: Deep Reinforcement Learning for Inventory Optimization. Manufacturing & Service Operations Management 2021. [Google Scholar] [CrossRef]
- Spanò, S.; Cardarilli, G.C.; Di Nunzio, L.; Fazzolari, R.; Giardino, D.; Matta, M.; Nannarelli, A.; Re, M. An Efficient Hardware Implementation of Reinforcement Learning: The Q-Learning Algorithm. IEEE Access 2019, 7, 186340–186351. [Google Scholar] [CrossRef]
- Qi, L.; Sun, Y.; Luan, W. Large-Scale Traffic Signal Control Based on Multi-Agent Q-Learning and Pressure. IEEE Access 2024, 12, 1092–1101. [Google Scholar] [CrossRef]
- Zhou, C.; Stephen, A.; Tan, K.C.; Chew, E.P.; Lee, L.H. Multiagent Q-Learning Approach for the Recharging Scheduling of Electric Automated Guided Vehicles in Container Terminals. Transp. Sci. 2024, 58, 664–683. [Google Scholar] [CrossRef]
- Sharma, J.; Andersen, P.-A.; Granmo, O.-C.; Goodwin, M. Deep Q-Learning with Q-Matrix Transfer Learning for Novel Fire Evacuation Environment. IEEE Trans. Syst., Man, Cybern., Syst. 2021, 51, 7363–7381. [Google Scholar] [CrossRef]
- Takabatake, T.; Asai, K.; Kakuta, H.; Hasegawa, N. Optimizing Evacuation Paths Using Agent-Based Evacuation Simulations and Reinforcement Learning. Int. J. Disaster Risk Reduct. 2025, 117, 105173. [Google Scholar] [CrossRef]
- Zhang, D.; Wang, M.; Mango, J.; Li, X.; Xu, X. A Survey on Applications of Reinforcement Learning in Spatial Resource Allocation. Computational Urban Science 2024, 4, 14. [Google Scholar] [CrossRef]
- Zhao, Y.; Duan, D. Workshop Facility Layout Optimization Based on Deep Reinforcement Learning. Processes 2024, 12, 201. [Google Scholar] [CrossRef]
- Zheng, Y.; Lin, Y.; Zhao, L.; Wu, T.; Jin, D.; Li, Y. Spatial Planning of Urban Communities via Deep Reinforcement Learning. Nat Comput Sci 2023, 3, 748–762. [Google Scholar] [CrossRef]
- Li, D.; Zhang, Z.; Alizadeh, B.; Zhang, Z.; Duffield, N.; Meyer, M.A.; Thompson, C.M.; Gao, H.; Behzadan, A.H. A Reinforcement Learning-Based Routing Algorithm for Large Street Networks. International Journal of Geographical Information Science 2023, 38, 183–215. [Google Scholar] [CrossRef]
- Klar, M.; Langlotz, P.; Aurich, J.C. A Framework for Automated Multiobjective Factory Layout Planning Using Reinforcement Learning. Procedia CIRP 2022, 112, 555–560. [Google Scholar] [CrossRef]
- Zhao, Y.; Duan, D. Workshop Facility Layout Optimization Based on Deep Reinforcement Learning. Processes 2024, 12, 201. [Google Scholar] [CrossRef]
- The People’s Hospital of Puge County. Available online: https://www.scpgyy.com/ (accessed on 6 November 2025).
- Harrell, S. Ways of Being Ethnic in Southwest China; Studies on ethnic groups in China; University of Washington Press: Seattle, 2001; ISBN 978-0-295-80407-1.
- Sun, Q.; Xue, X.; Chen, C. How the Body Gets Healthy: An Empirical Case of Animism and Naturalism Working Together in the Treatment of Disease among the Nuosu People of Southwest China. Religions 2025, 16, 533. [Google Scholar] [CrossRef]
- Lu, H.; Ismail, S. binti; Rahman, K.A.A. bin A. A Study on the Expression of Three Colors - Black, Red, and Yellow and Related Aesthetic Ideas of the Yi People | Journal of Namibian Studies : History Politics Culture. 2023.
- Meng, K.; Li, H.; Shu, Y.; Chen, M.; Han, X.; He, L. Database Construction and Remodeling Method on Traditional Yi Nationality Patterns of China with GAN Model. Npj Herit. Sci. 2025, 13, 181. [Google Scholar] [CrossRef]
- Kokal, I.; Engel, A.; Kirschner, S.; Keysers, C. Synchronized Drumming Enhances Activity in the Caudate and Facilitates Prosocial Commitment - If the Rhythm Comes Easily. [CrossRef] [PubMed]
- Shamay-Tsoory, S.G.; Mendelsohn, A. Real-Life Neuroscience: An Ecological Approach to Brain and Behavior Research. Perspect. Psychol. Sci. 2019, 14, 841–859. [Google Scholar] [CrossRef]
- Durkheim, E. The Elementary Forms of the Religious Life; CreateSpace Independent Publishing Platform, 2014; ISBN 978-1-4973-3220-1.
- Collins, R. Interaction Ritual Chains; Princeton University Press: Princeton, 2014; ISBN 978-0-691-12389-9.
- Earth Science Data Systems, N. ASTER Global Digital Elevation Model V003 | NASA Earthdata 2025.
- DataV GeoAtlas: Web-Based Geospatial Toolkit Series. Available online: https://datav.aliyun.com/portal/school/atlas/area_selector (accessed on 6 November 2025).
- 3D Model Library for 3ds Max (Aigei). Available online: https://www.aigei.com/3d/model/ (accessed on 8 November 2025).
- Peng, W.; Jin, C.; Chen, X.; Wang, X. Assessing Urban Human Settlement Quality via Ecological Niche-Fitness: A Case Study of Wuhan Metropolitan Area. Sustainability 2025, 17, 9578. [Google Scholar] [CrossRef]
- Amap Open Platform: Amap Maps API. Available online: https://lbs.amap.com/ (accessed on 8 November 2025).
- Stichler, J.F.; Hamilton, D.K. Evidence-Based Design: What Is It? Herd 2008, 1, 3–4. [Google Scholar] [CrossRef] [PubMed]
- Alfonsi, E.; Capolongo, S.; Buffoli, M. Evidence Based Design and Healthcare: An Unconventional Approach to Hospital Design. Ann. Ig.: Med. Prev. Comunita 2014, 26, 137–143. [Google Scholar] [CrossRef]
- Edelstein, L. The Hippocratic Oath: Text, Translation and Interpretation; Johns Hopkins Press, 1943; ISBN 978-0-8018-0184-6. [Google Scholar]
- Helbing, D.; Molnár, P. Social Force Model for Pedestrian Dynamics. Phys. Rev. E 1995, 51, 4282–4286. [Google Scholar] [CrossRef]
- Drury, J.; Cocking, C.; Reicher, S. Everyone for Themselves? A Comparative Study of Crowd Solidarity among Emergency Survivors. Br J Soc Psychol 2009, 48, 487–506. [Google Scholar] [CrossRef]
- Rahgozar, N.; Rahgozar, N. Experimental and Numerical Investigation on Flexural Strengthening of Precast Concrete Corbel Connections with Fiber-Reinforced Plastic Sheet. Buildings 2024, 14, 387. [Google Scholar] [CrossRef]
- Rieke, N.; Hancox, J.; Li, W.; Milletarì, F.; Roth, H.R.; Albarqouni, S.; Bakas, S.; Galtier, M.N.; Landman, B.A.; Maier-Hein, K.; et al. The Future of Digital Health with Federated Learning. npj Digital Med. 2020, 3, 119. [Google Scholar] [CrossRef] [PubMed]
- Mandel, J.C.; Kreda, D.A.; Mandl, K.D.; Kohane, I.S.; Ramoni, R.B. SMART on FHIR: A Standards-Based, Interoperable Apps Platform for Electronic Health Records. J. Am. Med. Inf. Assoc. 2016, 23, 899–908. [Google Scholar] [CrossRef]
- API Document for Machine Translation | iFLYTEK Open Platform Documents. Available online: https://global.xfyun.cn/doc/nlp/xftrans/API.html#description-of-the-interface (accessed on 20 January 2026).
- Baichuan AI Baichuan Large Language Model Documentation. Available online: https://platform.baichuan-ai.com/docs/api (accessed on 20 January 2026).
- Shang, X.; Jiang, R.; Wong, S.C.; Gao, Z.; Weng, W. Advancing Lane Formation and High-Density Simulations in Bidirectional Flow: A Humanoid Pedestrian Model Incorporating Gait Dynamics and Body Rotation. Transportation Research Part C: Emerging Technologies 2025, 174, 105086. [Google Scholar] [CrossRef]
- Yang, J.; Zang, X.; Chen, W.; Luo, Q.; Wang, R.; Liu, Y. Improved Social Force Model Based on Pedestrian Collision Avoidance Behavior in Counterflow. Physica A: Statistical Mechanics and its Applications 2024, 642, 129762. [Google Scholar] [CrossRef]
- Deighan, M.T.; Ayobi, A.; O’Kane, A.A. Social Virtual Reality as a Mental Health Tool: How People Use VRChat to Support Social Connectedness and Wellbeing. In Proceedings of the Proceedings of the 2023 CHI Conference on Human Factors in Computing Systems; Association for Computing Machinery: New York, NY, USA, April 19 2023; pp. 1–13. 1–13.
- Wang, Y.; Duan, B.; Chen, X.; Song, Y.; Liu, X. The Application of Metaverse in Mental Health. Front. Public Health 2025, 13. [Google Scholar] [CrossRef] [PubMed]
- Stefanidi, Z.; Margetis, G.; Ntoa, S.; Papagiannakis, G. Real-Time Adaptation of Context-Aware Intelligent User Interfaces, for Enhanced Situational Awareness. IEEE Access 2022, 10, 1–1. [Google Scholar] [CrossRef]
- Carrera-Rivera, A.; Larrinaga, F.; Lasa, G.; Martinez-Arellano, G.; Unamuno, G. AdaptUI: A Framework for the Development of Adaptive User Interfaces in Smart Product-Service Systems. User Modeling and User-Adapted Interaction 2024, 34, 1929–1980. [Google Scholar] [CrossRef]
- Hatfield, E.; Cacioppo, J.T.; Rapson, R.L. Emotional Contagion; Cambridge University Press: Cambridge, 2002; ISBN 978-0-521-44948-9. [Google Scholar]
- Helbing, D.; Farkas, I.; Vicsek, T. Simulating Dynamical Features of Escape Panic. Nature 2000, 407, 487–490. [Google Scholar] [CrossRef]
- McCrae, R.R.; Jr, P.T.C. Personality in Adulthood: A Five-Factor Theory Perspective; The Guilford Press: New York, NY, 2006; ISBN 978-1-59385-260-3. [Google Scholar]


| Role | Speed Multiplier | Exit Knowledge | Behavioral Traits |
|---|---|---|---|
| Doctor | High (≈0.9) | Helping / Rescue | |
| Nurse | Medium (≈0.7) | Guiding / Flocking | |
| Patient | Low (≈0.2–0.5) | Following / Panic |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




