Submitted:
30 January 2026
Posted:
03 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. EEG Recording and Classification
2.2. Outcome Assessment
2.3. Statistical Analysis
2.4. Standard Protocol Approvals, Registrations, and Patient Consent
3. Results
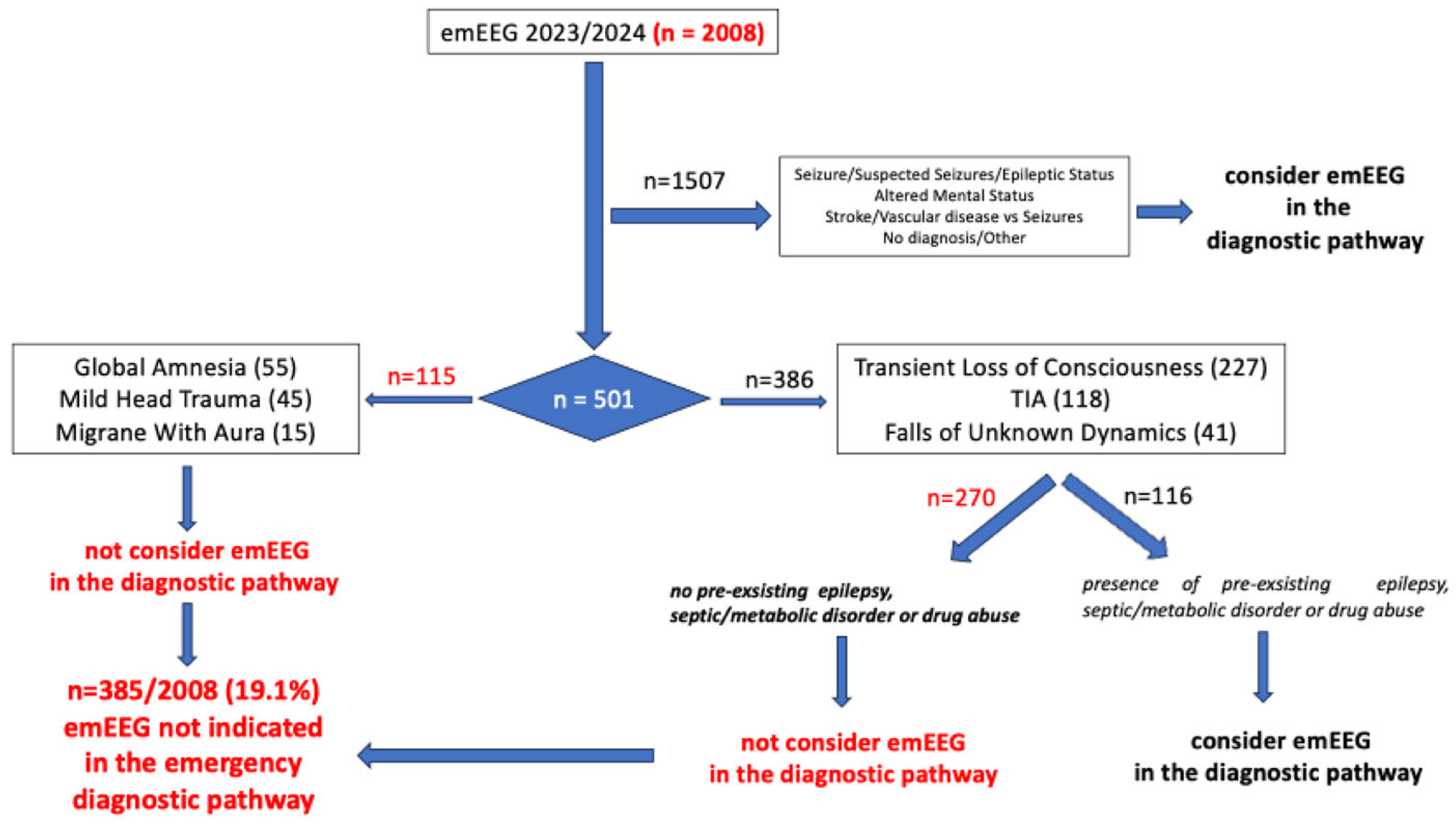
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ACNS | American Clinical Neurophysiology Society |
| ASM | Antiseizure Medication |
| CT | Computed Tomograpgy |
| ED | emergency department |
| EEG | Electroencephalography |
| emEEG | emergency EEG |
| ES | Epileptic Status |
| ICU | intensive care unit |
| IQR | Interquartile Range |
| NCSE | non-convulsive Epileptic Status |
| TIA | transient ischaemic attack |
| TLC | transient loss of consciousness |
References
- Praline, J.; Grujic, J.; Corcia, P.; Lucas, B.; Hommet, C.; Autret, A.; et al. Emergent EEG in clinical practice. Clin. Neurophysiol. 2007, 118, 2149–2155. [Google Scholar] [CrossRef]
- Scarpino, M.; Verna, M.T.; Grippo, A.; Lolli, F.; Piccardi, B.; Nazerian, P.; et al. The role of EEG in the emergency department: Its contribution to the patient’s diagnostic-therapeutic pathway. The EMINENCE study. Clin. Neurophysiol. Pract. 2025, 10, 70–77. [Google Scholar] [CrossRef]
- Scarpino, M.; Grippo, A.; Verna, M.T.; Lolli, F.; Piccardi, B.; Nazerian, P.; et al. Contribution of the EEG in the Diagnostic Workup of Patients with Transient Neurological Deficit and Acute Confusional State at the Emergency Department: The EMINENCE Study. Diagnostics (Basel). 2025, 15, 863. [Google Scholar] [CrossRef]
- 4. ACEP Clinical Policies Committee Clinical Policies Subcommittee on Seizures (2004) Clinical policy: critical issues in the evaluation and management of adult patients present into the emergency department with seizures. Ann. Emerg. Med. 2004, 43, 605–625.
- Bellini, A.; Gusmeo Curti, D.; Cursi, M.; Cecchetti, G.; Agosta, F.; Fanelli, G.; et al. Predictors of seizure detection and EEG clinical impact in an Italian tertiary emergency department. J. of Neurology. 2024, 271, 5137–5145. [Google Scholar] [CrossRef]
- Feyissa, A.M.; Tatum, W.O.; Adult, E.E.G. Handbook of Clinical Neurology; Elsevier B.V: Amsterdam, 2019; pp. 103–124. [Google Scholar]
- Varelas, P.N.; Spanaki, M.V.; Hacein-Bey, L.; Hether, T.; Terranova, B. Emergent EEG Indications and diagnostic yield. Neurology 2003, 61, 702–704. [Google Scholar] [CrossRef]
- Vignatelli, L.; Tontini, V.; Meletti, S.; Camerlingo, M.; Mazzoni, S.; Giovannini, G.; et al. Clinical practice guidelines on the management of status epilepticus in adults: a systematic review. Epilepsia. 2024, 65, 1512–1530. [Google Scholar] [CrossRef]
- Conference de consensus sur les indications de l’EEG en urgence Rapport redigé par J Perret, president du jury, apres les presentations des experts. Neurophysiol. Clin. 1996, 28, 103–110.
- Kaplan, P.W. Assessing the outcomes in patients with nonconvulsive status epilepticus: nonconvulsive status epilepticus is underdiagnosed, potentially overtreated, and confounded by comorbidity. J. Clin. Neurophysiol. 1999, 16, 341–353. [Google Scholar] [CrossRef]
- Rodriguez Quintana, J.H.; Silvia Juliana Bueno, F.; Zuleta-Motta, J.L.; Ramos, M.F.; V́elez-van-Meerbeke, A. and the Neuroscience Research Group (NeuRos). Utility of Routine EEG in Emergency Department and Inpatient Service. Neurology Clinical Practice. 2021, e681 11, e677. [Google Scholar]
- Privitera, M.D.; Strawsburg, R.H. Electroencephalographic monitoring in the emergency department. Emerg. Med. Clin. North. Am. 1994, 12, 1089–1100. [Google Scholar] [CrossRef]
- Yigit, O.; Eray, O.; Mihci, E.; Yilmaz, D.; Arslan, S.; Eray, *!!! REPLACE !!!*. BThe utility of EEGin the emergency department. Emerg Med, J 2012, 29, 301–305. [Google Scholar] [CrossRef]
- Praline, J.; de Toffol, B.; Mondon, K.; Hommet, C.; Prunier, C.; Corcia, P.; et al. EEG d’urgence: indications reelles et resultats. Neurophysiol. Clin. 2004, 34, 175–181. [Google Scholar] [CrossRef]
- Scarpino, M.; Grippo, A.; Lanzo, G.; Lolli, F. The burden of clinical neurophysiology for the neurologicalprognosis of coma. Future Medicine. 2018, 13, 127–129. [Google Scholar]
- Scarpino, M.; Lolli, F.; Hakiki, B.; et al. The prognostic value of the EEG, according to the American Clinical Neurophysiology Society terminology, recorded at the postacute stage in patients with unresponsive wakefulness syndrome. Neurophysiol. Clin. 2019, 49, 317–327. [Google Scholar] [CrossRef] [PubMed]
- Scarpino, M.; Lolli, F.; Hakiki, B.; Lanzo, G.; Sterpu, R.; Atzori, T.; et al. for the Intensive Rehabilitation Unit Study Group of the IRCCS Don Gnocchi Foundation, Italy. EEG and Coma Recovery Scale-Revised prediction of neurological outcome in Disorder of Consciousness patients. Acta Neurol. Scand. 2020, 142, 221–228. [Google Scholar] [CrossRef] [PubMed]
- Scarpino, M.; Lanzo, G.; Hakiki, B.; Sterpu, R.; Maiorelli, A.; Cecchi, F.; et al. Acquired brain injuries: neurophysiology in early prognosis and rehabilitation pathway. Signa Vitae 2021, 2–11. [Google Scholar]
- Hirsch, L.J.; LaRoche, S.M.; Gaspard, N.; Gerard, E.; Svoronos, A.; Herman, S.T.; et al. American Clinical Neurophysiology Society’s standardized critical care EEG terminology: 2012 version. J. Clin. Neurophysiol. 2013, 30, 1–27. [Google Scholar] [CrossRef]
- Manez ˜ Miro, J.U.; Dıaz de Teran, F.J.; Alonso Singer, P.; Aguilar-Amat Prior, M.J. Uso de la electroencefalografıa urgente por el neurologo de guardia: utilidad en el diagnostico del estatusepilepticono convulsivo. Neurologıa. 2018, 33, 71–77. [Google Scholar] [CrossRef]
- Lozeron, P.; Tcheumeni, N.C.; Turki, S.; Amiel, H.; Meppiel, E.; Masmoudi, S.; et al. Contribution of EEG in transient neurological deficits. J. Neurol. 2018, 265, 89–97. [Google Scholar] [CrossRef]
- Prud’hon, S.; Amiel, H.; Zanin, A.; Revue, E.; Kubis, N.; Lozeron, P. EEG and acute confusional state at the emergency department. Neurophysiol. Clin. 2024, 54, 102966. [Google Scholar] [CrossRef] [PubMed]
- Khan, R.B.; Yerremsetty, P.K.; Lindstrom, D.; McGill, L.J. Emergency EEG and factors associated with nonconvulsive status epilepticus. J. Natl. Med. Assoc. 2001, 93, 359–362. [Google Scholar] [PubMed]
- Quigg, M.; Shneker, B.; Domer, P. Current practice in administration and clinical criteria of emergent EEG. J. Clin. Neurophysiol. 2001, 18, 162–165. [Google Scholar] [CrossRef]
- Zawar, I.; Briskin, I.; Hantus, S. Risk factors that predict delayed seizure detection on continuous electroencephalogram (cEEG) in a large sample size of critically ill patients. Epilepsia Open. 2022, 7, 131–143. [Google Scholar] [CrossRef] [PubMed]
| Characteristics | |
|---|---|
| Age year, median (IQR) | 70 (IQR 29) |
| Male gender, n (%) | 1004 (50.0%) |
| Previous Epileptic Seizures | 566 (28.1%) |
| Unknown aetiology | 213 (10.6%) |
| Structural aetiology | 353 (17.6%) |
| Antiseizures medications | 510 (25.4%) |
| Under-dosed antiseizures medications | 122 (6.1%) |
| Fever | 262 (13.1%) |
| Sepsis | 314 (15.6%) |
| Metabolic disturbance | 129 (6.4%) |
| Electrolyte disturbance | 235 (11.7%) |
| Drug abuse | 95 (4.7%) |
| Previous Neurological history | 691 (34.4%) |
| Stroke | 159 (7.8%) |
| Neurosurgery | 238 (11.9%) |
| Cardiac disorders | 462 (23.0%) |
| Diabetes | 327 (16.3%) |
| Dyslipidemia | 540 (26.9%) |
| Thyroid disease | 218 (10.9%) |
| Brain CT | 1844 (91.8%) |
| Recent CT Lesions | 297 (14.7%) |
| Home discharge | 1331 (66.3%) |
| Hospitalization | 628 (31.3%) |
| Hospitalization Refused | 49 (2.4%) |
| Normal | Epileptiform | Triphasic sharp waves |
Frequency reduced |
No Reactivity | Asymmetry | Theta | Delta | |
|---|---|---|---|---|---|---|---|---|
| Cramer’s V ED ADMISSION DIAGNOSIS |
0.280 |
0.421 | 0.158 | 0.170 | 0.255 | 0.173 | 0.203 | 0.179 |
| Seizure (n=520) | 96 (18.5) | 217 (41.7) | 7 (1.3) | 197 (37.9) | 218 (41.9) | 111 (21.3) | 246 (47.3) | 270 (51.9) |
| Suspected Seizures (n=263) | 84 (31.9) | 64 (48.7) | 7 (2.6) | 99 (37.6) | 74 (28.1) | 50 (19.0) | 105 (39.9) | 17 (6.4) |
| Epileptic Status (n=61) | 3 (4.9%) | 41 (67.2) | 0 (0.0) | 34 (55.7) | 42 (68.8) | 30 (49.2) | 32 (52.5) | 50 (81.9) |
| Altered Mental Status (n=158) | 20 (18.4) | 24 (27.3) | 21 (13.2) | 109 (68.9) | 123 (77.8) | 28 (17.07) | 35 (22.1) | 80 (50.6) |
| TLC (n=227) | 144 (63.4) | 9 (4.0) | 1 (0.4) | 41 (18.0) | 19 (8.3) | 8 (3.6) | 32 (14.1) | 28 (12.3) |
| TIA (n=118) | 62 (52.5) | 0 (0.0) | 2 (1.7) | 26 (22.0) | 9 (7.9) | 4 (3.4) | 27 (22.9) | 22 (18.6) |
| Stroke (n=124) | 34 (27.4) | 11 (8.8) | 8 (6.4) | 57 (45.9) | 48 (35.8) | 24 (19.3) | 35 (28.2) | 56 (45.1) |
| Vascular disease vs seizures (n=111) | 24 (21.6) | 25 (22.5) | 0 (0.0) | 49 (44.1) | 36 (32.4) | 30 (27.0.) | 56 (50.5) | 53 (47.7) |
| Falls Of Unknow Dynamics (n=41) | 17 (41.5) | 1 (2.4) | 2 (4.9) | 19 (46.3) | 12 (29.3) | 2 (4.9) | 7 (17.1) | 12 (29.2) |
| Global Amnesia (n=55) | 42 (76.4) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 2 (3.6) | 0 (0.0) | 8 (14.5) | 6 (10.9) |
| Mild head Trauma (n=45) | 25 (55.6) | 0 (0.0) | 0 (0.0) | 10 (22.2) | 8 (17.8) | 4 (8.9) | 11 (24.4) | 8 (17.7) |
| Migraine with aura (n=15) | 12 (80.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 2 (13.3) | 1 (6.7) |
| No Diagnosis/Other (n=250) | 90 (36.0) | 28 (11.5) | 7 (2.9) | 99 (39.6) | 69 (27.6) | 40 (16.4) | 68 (27.2) | 82 (32.8) |
| Total (n=2008) | 653 (32.5) | 420 (20.9) | 55 (2.7) | 740 (36.8) | 660 (32.8) | 331 (16.4) | 664 (33.1) | 414 (20.6) |
| Normal | Epileptiform | Triphasic sharp waves |
Frequency reduced |
No Reactivity |
Asymmetry | Theta | Delta | |
|---|---|---|---|---|---|---|---|---|
|
Neurological Signs/Symptoms on admission |
n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) | n (%) |
| TLC (n=687) | 265 (38.6) | 142 (20.7) | 6 (0.9) | 232 (33.7) | 30 (4.4) | 85 (12.4) | 243 (35.4) | 232 (33.7) |
| Language Disorder (n=512) | 126 (24.6) | 92 (18.0) | 13 (2.5) | 238 (46.4) | 195 (38.1) | 114 (22.2) | 192 (37.5) | 235 (45.8) |
| Confusion (n=477) | 134 (28.1) | 81 (17.0) | 22 (4.6) | 230 (48.2) | 198 (41.5) | 74 (15.5) | 153 (32.1) | 197 (41.2) |
| Motor Manifestation (n=715) | 159 (22.2) | 264 (36.9) | 15 (2.1) | 212 (29.7) | 234 (32.7) | 97 (13.6) | 302 (42.2) | 365 (51.0) |
| Altered Mental Status (n=267) | 24 (9.0) | 72 (27.0) | 29 (10.8) | 206 (77.1) | 209 (78.2) | 60 (22.5) | 88 (33.0) | 159 (59.5) |
| Absence (n=124) | 34 (27.4) | 33 (26.6.) | 5 (4.0) | 50 (40.4) | 34 (33.0) | 23 (18.2) | 51 (41.1) | 53 (41.7) |
| Behavioural impairment (n=195) | 46 (23.5) | 41 (21.0) | 12 (6.1) | 116 (59.4) | 100 (51.2.) | 35 (17.9) | 73 (37.4.) | 94 (48.2) |
| Sensory symptoms (n=140) | 72 (51.4) | 25 (17.9) | 2 (1.4) | 17 (19.2) | 26 (18.6) | 20 (14.3) | 38 (27.1) | 38 (27.1) |
| Hypostenia (n=282) | 70 (24.8) | 62 (22.0) | 5 (1.7) | 104 (36.8) | 119 (42.1) | 77 (27.3) | 113 (40.1) | 134 (47.5) |
| Headache (n=148) | 77 (52.0) | 23 (15.5) | 1 (0.6) | 21 (14.1) | 33 (22.3) | 20 (13.5) | 46 (31.1) | 37 (25.0) |
| Asthenia (n=53) | 24 (45.3) | 4 (7.5) | 2 (3.7) | 13 (24.5) | 18 (33.9) | 8 (15.0) | 17 (32.1) | 17 (32.1) |
| Amnesia (n=197) | 107 (54.3) | 23 (11.7) | 1 (0.5) | 28 (14.2) | 30 (15.2) | 11 (5.5) | 57 (28.9) | 37 (18.7) |
| Hallucinations (n=22) | 7 (31.8) | 1 (4.5) | 1 (4.5) | 9 (40.9) | 7 (31.8) | 7 (31.8) | 5 (22.7) | 8 (36.3) |
| Catatonic state (n= 18) | 4 (22.2) | 3 (16.7) | 1 (5.5) | 9 (50.0) | 8 (44.4) | 2 (11.1) | 9 (50.0) | 6 (33.3) |
| Visual disturbance (n=66) | 18 (27.1) | 16 (24.6) | 0 (0.0) | 18 (27.2) | 29 (44.6) | 18 (27.2) | 23 (35.4) | 28 (42.4) |
| Morsus (n= 139) | 40 (28.8) | 46 (33.1) | 1 (0.7) | 36 (25.8) | 41 (29.5) | 13 (9.3) | 59 (42.4) | 59 (42.4) |
| Postural instability (n=39) | 17 (43.6) | 4 (10.3) | 0 (0.0) | 17 (43.6) | 13 (33.3) | 4 (10.3) | 10 (25.6) | 8 (20.6) |
| Discharge Diagnosis | ||||
|---|---|---|---|---|
| Diagnosi at patient admission (n) | Confirmed Diagnosis |
Seizures/ Suspected seizure |
Encephalopatic disease | Others Diagnosis |
| TLC (227) | ||||
| Normal/non-specific emEEG (N=217) | 178 | 6 | 5 | 26 |
| Epileptic emEEG (n=9) | 7 | 2 | 0 | 0 |
| Triphasic emEEG (n=1) | 0 | 0 | 1 | 0 |
| TIA (118) | ||||
| Normal/non-specific emEEG (n=116) | 41 | 6 | 2 | 67 |
| Epileptic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Triphasic emEEG (n=2) | 0 | 0 | 2 | 0 |
| Falls Of Unknow Dynamics(41) | ||||
| Normal/non-specific emEEG (n=38) | 18 | 0 | 3 | 17 |
| Epileptic emEEG (n=1) | 0 | 1 | 0 | 0 |
| Triphasic emEEG (n=2) | 0 | 0 | 2 | 0 |
| Global Amnesia (55) | ||||
| Normal/non-specific emEEG (n=55) | 50 | 0 | 0 | 5 |
| Epileptic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Triphasic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Head Trauma (45) | ||||
| Normal/non-specific emEEG (n=45) | 37 | 0 | 0 | 8 |
| Epileptic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Triphasic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Migraine with aura(15) | ||||
| Normal/non-specific emEEG (n=15) | 14 | 0 | 0 | 1 |
| Epileptic emEEG (n=0) | 0 | 0 | 0 | 0 |
| Triphasic emEEG (n=0) | 0 | 0 | 0 | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




