Submitted:
19 January 2026
Posted:
20 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| AL | Anastomotic leakage |
| DM | Diabetes Mellitus |
| CV | Cardiovascular |
| ASA | American Society of Anesthesiologists (physical status classification) |
| BMI | Body Mass Index |
| INR | International Normalized Ratio |
| KDE | Kernel Density Estimation |
| nCRT | Neoadjuvant Chemoradiotherapy |
| OR | Odds Ratio |
| SD | Standard Deviation |
| WBC | White Blood Cells |
| INR | International normalized ratio |
| CRP | C-Reactive Protein |
References
- D.-D. Chitca, V. Popescu, A. Dumitrescu, C. Botezatu, and B. Mastalier, “Advancing Colorectal Cancer Diagnostics from Barium Enema to AI-Assisted Colonoscopy,” Diagnostics, vol. 15, no. 8, p. 974, Apr. 2025. [CrossRef]
- J. Bruce, Z. H. Krukowski, G. Al-Khairy, E. M. Russell, and K. G. M. Park, “Systematic review of the definition and measurement of anastomotic leak after gastrointestinal surgery,” Br J Surg, vol. 88, no. 9, pp. 1157–1168, 2001. [CrossRef]
- W. H. Isbister, “Anastomotic leak in colorectal surgery: a single surgeon’s experience,” ANZ J Surg, vol. 71, no. 9, pp. 516–520, 2001. [CrossRef]
- P. Matthiessen, O. Hallböök, M. Andersson, J. Rutegård, and R. Sjödahl, “Risk factors for anastomotic leakage after anterior resection of the rectum,” Colorectal Dis, vol. 6, no. 6, pp. 462–469, Nov. 2004. [CrossRef]
- B. C. Paun, S. Cassie, A. R. MacLean, E. Dixon, and W. D. Buie, “Postoperative complications following surgery for rectal cancer,” Ann Surg, vol. 251, no. 5, pp. 807–818, May 2010. [CrossRef]
- I. J. Park, “Influence of anastomotic leakage on oncological outcome in patients with rectal cancer,” Journal of Gastrointestinal Surgery, vol. 14, no. 7, pp. 1190–1196, 2010. [CrossRef]
- K. Y. Lee et al., “Totally robotic surgery for rectal cancer: from splenic flexure to pelvic floor in one setup,” Surg Endosc, vol. 24, no. 3, pp. 715–720, 2010. [CrossRef]
- H. S. Snijders et al., “Meta-analysis of the risk for anastomotic leakage, the postoperative mortality caused by leakage in relation to the overall postoperative mortality,” European Journal of Surgical Oncology, vol. 38, no. 11, pp. 1013–1019, Nov. 2012. [CrossRef]
- D. M. Richards, R. C. Heel, R. N. Brogden, T. M. Speight, and G. S. Avery, “Ceftriaxone A Review of its Antibacterial Activity, Pharmacological Properties and Therapeutic Use,” Drugs, vol. 27, no. 6, pp. 469–527, Jun. 1984. [CrossRef]
- G. Akkus and M. Sert, “Diabetic foot ulcers: A devastating complication of diabetes mellitus continues non-stop in spite of new medical treatment modalities,” World J Diabetes, vol. 13, no. 12, pp. 1106–1121, Dec. 2022. [CrossRef]
- A. E. Arslanköylü, S. Kuyucu, S. Balcı, and Y. Usta, “İlk doz seftriakson enjeksiyonu sonrası anafilaksi,” Turk Pediatri Ars, vol. 46, no. 1, pp. 81–83, Mar. 2011. [CrossRef]
- B. D. Shogan, E. M. Carlisle, J. C. Alverdy, and K. Umanskiy, “Do We Really Know Why Colorectal Anastomoses Leak?,” Journal of Gastrointestinal Surgery, vol. 17, no. 9, pp. 1698–1707, Sep. 2013. [CrossRef]
- E. Rullier, C. Laurent, J. L. Garrelon, P. Michel, J. Saric, and M. Parneix, “Risk factors for anastomotic leakage after resection of rectal cancer,” Br J Surg, vol. 85, no. 3, pp. 355–358, 1998. [CrossRef]
- E. C. Zarnescu, N. O. Zarnescu, and R. Costea, “Updates of Risk Factors for Anastomotic Leakage after Colorectal Surgery,” Diagnostics (Basel), vol. 11, no. 12, Dec. 2021. [CrossRef]
- J. He, M. He, J. H. Tang, and X. H. Wang, “Anastomotic leak risk factors following colon cancer resection: a systematic review and meta-analysis,” Langenbecks Arch Surg, vol. 408, no. 1, Dec. 2023. [CrossRef]
- D. Asklid, O. Ljungqvist, Y. Xu, and U. O. Gustafsson, “Risk Factors for Anastomotic Leakage in Patients with Rectal Tumors Undergoing Anterior Resection within an ERAS Protocol: Results from the Swedish ERAS Database,” World J Surg, vol. 45, no. 6, pp. 1630–1641, Jun. 2021. [CrossRef]
- D. Andras et al., “Analyzing postoperative complications in colorectal cancer surgery: a systematic review enhanced by artificial intelligence,” Front Surg, vol. 11, Oct. 2024. [CrossRef]
- C. T. Ellis and J. A. Maykel, “Defining Anastomotic Leak and the Clinical Relevance of Leaks,” Clin Colon Rectal Surg, vol. 34, no. 6, pp. 359–365, Nov. 2021. [CrossRef]
- S. R. Steele, T. L. Hull, N. Hyman, J. A. Maykel, T. E. Read, and C. B. Whitlow, “The ASCRS Textbook of Colon and Rectal Surgery: Fourth Edition,” The ASCRS Textbook of Colon and Rectal Surgery: Fourth Edition, pp. 1–1216, Jan. 2021. [CrossRef]
- D. Nekrosius, E. Gvozdas, G. M. Pratkute, A. Tamelis, and P. Lizdenis, “Impact of Surgical Approach, Patient Risk Factors, and Diverting Ileostomy on Anastomotic Leakage and Outcomes After Rectal Cancer Resection: A 5-Year Single-Center Study,” Medicina 2025, Vol. 61, Page 1751, vol. 61, no. 10, p. 1751, Sep. 2025. [CrossRef]
- E. Myrseth, L. S. Nymo, P. F. Gjessing, and S. Norderval, “Diverting stomas reduce reoperation rates for anastomotic leak but not overall reoperation rates within 30 days after anterior rectal resection: a national cohort study,” Int J Colorectal Dis, vol. 37, no. 7, pp. 1681–1688, Jul. 2022. [CrossRef]
- K. Phan et al., “Does a stoma reduce the risk of anastomotic leak and need for re-operation following low anterior resection for rectal cancer: systematic review and meta-analysis of randomized controlled trials,” J Gastrointest Oncol, vol. 10, no. 2, pp. 179–187, Apr. 2019. [CrossRef]
- H. Nishigori, M. Ito, and Y. Nishizawa, “A novel transanal tube designed to prevent anastomotic leakage after rectal cancer surgery: the WING DRAIN,” Surgery Today 2016 47:4, vol. 47, no. 4, pp. 513–520, Aug. 2016. [CrossRef]
- Z. Adamova, “Transanal Tube as a Means of Prevention of Anastomotic Leakage after Rectal Cancer Surgery,” Viszeralmedizin, vol. 30, no. 6, pp. 422–426, Dec. 2014. [CrossRef]
- H. Nishigori et al., “Effectiveness of a transanal tube for the prevention of anastomotic leakage after rectal cancer surgery,” World J Surg, vol. 38, no. 7, pp. 1843–1851, Jul. 2014. [CrossRef]
- E. Hidaka et al., “Efficacy of transanal tube for prevention of anastomotic leakage following laparoscopic low anterior resection for rectal cancers: a retrospective cohort study in a single institution,” Surgical Endoscopy 2014 29:4, vol. 29, no. 4, pp. 863–867, Jul. 2014. [CrossRef]
- M. K. Kim, D. Y. Won, J. K. Lee, W. K. Kang, J. G. Kim, and S. T. Oh, “Comparative study between transanal tube and loop ileostomy in low anterior resection for mid rectal cancer: a retrospective single center trial,” Ann Surg Treat Res, vol. 88, no. 5, pp. 260–268, May 2015. [CrossRef]
- A. Brandl, S. Czipin, R. Mittermair, S. Weiss, J. Pratschke, and R. Kafka-Ritsch, “Transanal drainage tube reduces rate and severity of anastomotic leakage in patients with colorectal anastomosis: A case controlled study,” Annals of Medicine and Surgery, vol. 6, pp. 12–16, Mar. 2016. [CrossRef]
- M. Matsuda et al., “Transanal drainage tube placement to prevent anastomotic leakage following colorectal cancer surgery with double stapling reconstruction,” Surgery Today 2015 46:5, vol. 46, no. 5, pp. 613–620, Aug. 2015. [CrossRef]
- C. S. Yang et al., “Rectal tube drainage reduces major anastomotic leakage after minimally invasive rectal cancer surgery,” Colorectal Disease, vol. 18, no. 12, pp. O445–O452, Dec. 2016. [CrossRef]
- S. Goto et al., “Multicenter analysis of transanal tube placement for prevention of anastomotic leak after low anterior resection,” J Surg Oncol, vol. 116, no. 8, pp. 989–995, Dec. 2017. [CrossRef]
- T. Ito et al., “Usefulness of transanal tube placement for prevention of anastomotic leakage following laparoscopic low anterior resection,” Asian J Endosc Surg, vol. 10, no. 1, pp. 17–22, Feb. 2017. [CrossRef]
- K. Kawada, R. Takahashi, K. Hida, and Y. Sakai, “Impact of transanal drainage tube on anastomotic leakage after laparoscopic low anterior resection,” International Journal of Colorectal Disease 2017 33:3, vol. 33, no. 3, pp. 337–340, Dec. 2017. [CrossRef]
- S. Zhao et al., “Transanal Drainage Tube Use for Preventing Anastomotic Leakage After Laparoscopic Low Anterior Resection in Patients With Rectal Cancer: A Randomized Clinical Trial,” JAMA Surg, vol. 156, no. 12, pp. 1151–1158, Dec. 2021. [CrossRef]
- S. Kojima, T. Sakamoto, Y. Nagai, Y. Matsui, K. Nambu, and K. Masamune, “Laser Speckle Contrast Imaging for Intraoperative Quantitative Assessment of Intestinal Blood Perfusion During Colorectal Surgery: A Prospective Pilot Study,” Surg Innov, vol. 26, no. 3, pp. 293–301, Jun. 2019. [CrossRef]
- M. S. Renna et al., “Intraoperative bowel perfusion assessment methods and their effects on anastomotic leak rates: meta-analysis,” Br J Surg, vol. 110, no. 9, pp. 1131–1142, Sep. 2023. [CrossRef]
- K. Buxey, F. Lam, M. Muhlmann, and S. Wong, “Does indocyanine green improve the evaluation of perfusion during laparoscopic colorectal surgery with extracorporeal anastomosis?,” ANZ J Surg, vol. 89, no. 11, pp. E487–E491, Nov. 2019. [CrossRef]
- K. Safiejko et al., “Safety and Efficacy of Indocyanine Green in Colorectal Cancer Surgery: A Systematic Review and Meta-Analysis of 11,047 Patients,” Cancers (Basel), vol. 14, no. 4, Feb. 2022. [CrossRef]
- S. Xia, W. Wu, L. Luo, L. Ma, L. Yu, and Y. Li, “Indocyanine green fluorescence angiography decreases the risk of anastomotic leakage after rectal cancer surgery: a systematic review and meta-analysis,” Front Med (Lausanne), vol. 10, p. 1157389, May 2023. [CrossRef]
- C. B. Neutzling, S. A. Lustosa, I. M. Proenca, E. M. da Silva, and D. Matos, “Stapled versus handsewn methods for colorectal anastomosis surgery,” Cochrane Database Syst Rev, vol. 2012, no. 2, Feb. 2012. [CrossRef]
- P. Y. G. Choy, I. P. Bissett, J. G. Docherty, B. R. Parry, A. Merrie, and A. Fitzgerald, “Stapled versus handsewn methods for ileocolic anastomoses,” Cochrane Database Syst Rev, no. 9, Sep. 2011. [CrossRef]
- A. Oliveira, S. Faria, N. Gonçalves, A. Martins, and P. Leão, “Surgical approaches to colonic and rectal anastomosis: systematic review and meta-analysis,” Int J Colorectal Dis, vol. 38, no. 1, Dec. 2023. [CrossRef]
- S. Abounozha, A. Kheder, T. Alshahri, and R. Ibrahim, “Best evidence topic: Is ileocolic anastomotic leak rate higher in handsewn or stapler’s anastomosis?,” Annals of Medicine and Surgery, vol. 60, pp. 619–622, Dec. 2020. [CrossRef]
- M. Frasson et al., “Risk Factors for Anastomotic Leak After Colon Resection for Cancer: Multivariate Analysis and Nomogram From a Multicentric, Prospective, National Study With 3193 Patients,” Ann Surg, vol. 262, no. 2, pp. 321–330, Aug. 2015. [CrossRef]
- B. Wallace, F. Schuepbach, S. Gaukel, A. I. Marwan, R. F. Staerkle, and R. N. Vuille-Dit-Bille, “Evidence according to Cochrane Systematic Reviews on Alterable Risk Factors for Anastomotic Leakage in Colorectal Surgery,” Gastroenterol Res Pract, vol. 2020, no. 1, p. 9057963, Jan. 2020. [CrossRef]
- Y. Y. Tsai and W. T. L. Chen, “Management of anastomotic leakage after rectal surgery: a review article,” J Gastrointest Oncol, vol. 10, no. 6, pp. 1229–1237, Dec. 2019. [CrossRef]
- H. Xu and F. Kong, “Malnutrition-Related Factors Increased the Risk of Anastomotic Leak for Rectal Cancer Patients Undergoing Surgery,” Biomed Res Int, vol. 2020, no. 1, p. 5059670, Jan. 2020. [CrossRef]
- V. C. Nikolian et al., “Anastomotic leak after colorectal resection: A population-based study of risk factors and hospital variation,” Surgery (United States), vol. 161, no. 6, pp. 1619–1627, Jun. 2017. [CrossRef]
- S. L. R. Rodriguez, D. F. S. Montoro, G. De la Cruz Ku, C. del Rocio Luna Munoz, and C. R. R. Bustamante, “Risk factors of anastomotic leak in colorectal cancer: a multicentric study in a Latin American country,” Ecancermedicalscience, vol. 18, 2024. [CrossRef]
- C. Tsalikidis et al., “Predictive Factors for Anastomotic Leakage Following Colorectal Cancer Surgery: Where Are We and Where Are We Going?,” Curr Oncol, vol. 30, no. 3, pp. 3111–3137, Mar. 2023. [CrossRef]
- C. Y. Kang et al., “Risk Factors for Anastomotic Leakage After Anterior Resection for Rectal Cancer,” JAMA Surg, vol. 148, no. 1, pp. 65–71, Jan. 2013. [CrossRef]
- M. Thornton et al., “Management and outcome of colorectal anastomotic leaks,” International Journal of Colorectal Disease 2010 26:3, vol. 26, no. 3, pp. 313–320, Nov. 2010. [CrossRef]
- T. Akasu, M. Takawa, S. Yamamoto, T. Yamaguchi, S. Fujita, and Y. Moriya, “Risk factors for anastomotic leakage following intersphincteric resection for very low rectal adenocarcinoma,” Journal of Gastrointestinal Surgery, vol. 14, no. 1, pp. 104–111, Jan. 2010. [CrossRef]
- H. Doran, T. Pătraşcu, E. Catrina, and O. Mihalache, “[Hartmann ’s procedure. A 30 years one-centre clinical experience].,” Chirurgia (Bucur), vol. 103, no. 4, pp. 413–6, 2008.
- “Host-related predictive factors for anastomotic leakage following large bowel resections for colorectal cancer - PubMed.” Accessed: Jan. 03, 2026. [Online]. Available: https://pubmed.ncbi.nlm.nih.gov/18836623/.
- D. E. Huisman et al., “LekCheck: A Prospective Study to Identify Perioperative Modifiable Risk Factors for Anastomotic Leakage in Colorectal Surgery,” Ann Surg, vol. 275, no. 1, pp. E189–E197, Jan. 2022. [CrossRef]
- D. M. Hayden, M. C. Mora Pinzon, A. B. Francescatti, and T. J. Saclarides, “Patient factors may predict anastomotic complications after rectal cancer surgery: Anastomotic complications in rectal cancer,” Ann Med Surg (Lond), vol. 4, no. 1, pp. 11–16, Mar. 2014. [CrossRef]
- M. Morimoto, K. Taniguchi, O. Yamamoto, T. Naka, A. Sugitani, and Y. Fujiwara, “Preoperative white blood cell count predicts anastomotic leakage in patients with left-sided colorectal cancer,” PLoS One, vol. 16, no. 10, p. e0258713, Oct. 2021. [CrossRef]
- B. A. Messias, R. V. Botelho, S. S. Saad, E. R. Mocchetti, K. C. Turke, and J. Waisberg, “Serum C-reactive protein is a useful marker to exclude anastomotic leakage after colorectal surgery,” Scientific Reports 2020 10:1, vol. 10, no. 1, pp. 1687–, Feb. 2020. [CrossRef]
- A. Jina and U. C. Singh, “Factors influencing intestinal anastomotic leak and their predictive value,” International Surgery Journal, vol. 6, no. 12, pp. 4495–4501, Nov. 2019. [CrossRef]
- V. E. Dias et al., “Preoperative risk factors associated with anastomotic leakage after colectomy for colorectal cancer: a systematic review and meta-analysis,” Rev Col Bras Cir, vol. 49, 2022. [CrossRef]
- C. J. van Beekum et al., “Predictors of Morbidity and Mortality After Colorectal Surgery in Patients With Cirrhotic Liver Disease–A Retrospective Analysis of 54 Cases at a Tertiary Care Center,” Front Med (Lausanne), vol. 9, p. 886566, Jun. 2022. [CrossRef]
- S. A. Käser, I. Hofmann, N. Willi, F. Stickel, and C. A. Maurer, “Liver Cirrhosis/Severe Fibrosis Is a Risk Factor for Anastomotic Leakage after Colorectal Surgery,” Gastroenterol Res Pract, vol. 2016, 2016. [CrossRef]
- E. F. Midura et al., “Risk factors and consequences of anastomotic leak after colectomy: a national analysis,” Dis Colon Rectum, vol. 58, no. 3, pp. 333–338, 2015. [CrossRef]
- A. Rencuzogullari, C. Benlice, M. Valente, M. A. Abbas, F. H. Remzi, and E. Gorgun, “Predictors of Anastomotic Leak in Elderly Patients After Colectomy: Nomogram-Based Assessment From the American College of Surgeons National Surgical Quality Program Procedure-Targeted Cohort,” Dis Colon Rectum, vol. 60, no. 5, pp. 527–536, May 2017. [CrossRef]
- D. Ionescu, C. Tibrea, and C. Puia, “Pre-operative hypoalbuminemia in colorectal cancer patients undergoing elective surgery - a major risk factor for postoperative outcome.,” Chirurgia (Bucur), vol. 108, no. 6, pp. 822–8, 2013.
- D. A. Telem, E. H. Chin, S. Q. Nguyen, and C. M. Divino, “Risk factors for anastomotic leak following colorectal surgery: a case-control study,” Arch Surg, vol. 145, no. 4, pp. 371–376, Apr. 2010. [CrossRef]
- T. Shimura et al., “Monitoring perioperative serum albumin can identify anastomotic leakage in colorectal cancer patients with curative intent,” Asian J Surg, vol. 41, no. 1, pp. 30–38, Jan. 2018. [CrossRef]
- P. K. Anandan, M. Mohammed, N. Hassan, and M. Mathew, “Pre-operative hypoalbuminemia is a major risk factor for anastomotic leak in emergency gastrointestinal resection and anastomosis,” International Surgery Journal, vol. 4, no. 4, pp. 1405–1408, Mar. 2017. [CrossRef]
- S. L. R. Rodriguez, D. F. S. Montoro, G. De la Cruz Ku, C. del Rocio Luna Munoz, and C. R. R. Bustamante, “Risk factors of anastomotic leak in colorectal cancer: a multicentric study in a Latin American country,” Ecancermedicalscience, vol. 18, 2024. [CrossRef]
- X.-Y. Tang, Y. Chen, Y.-C. Liu, J.-X. Lang, X.-Y. Li, and C.-D. Zhang, “Relationship between preoperative albumin level and risk of site-specific anastomotic leakage in digestive tract surgery: a systematic review and meta-analysis,” Int J Surg, Nov. 2025. [CrossRef]
- M. Parthasarathy, M. Greensmith, D. Bowers, and T. Groot-Wassink, “Risk factors for anastomotic leakage after colorectal resection: a retrospective analysis of 17 518 patients,” Colorectal Disease, vol. 19, no. 3, pp. 288–298, Mar. 2017. [CrossRef]
- O. Jannasch et al., “Risk factors, short and long term outcome of anastomotic leaks in rectal cancer,” Oncotarget, vol. 6, no. 34, pp. 36884–36893, Sep. 2015. [CrossRef]
- I. S. Bakker, I. Grossmann, D. Henneman, K. Havenga, and T. Wiggers, “Risk factors for anastomotic leakage and leak-related mortality after colonic cancer surgery in a nationwide audit,” British Journal of Surgery, vol. 101, no. 4, pp. 424–432, Feb. 2014. [CrossRef]
- C. L. Sparreboom et al., “Different Risk Factors for Early and Late Colorectal Anastomotic Leakage in a Nationwide Audit,” Dis Colon Rectum, vol. 61, no. 11, pp. 1258–1266, 2018. [CrossRef]
- P. M. Krarup, L. N. Jorgensen, A. H. Andreasen, and H. Harling, “A nationwide study on anastomotic leakage after colonic cancer surgery,” Colorectal Dis, vol. 14, no. 10, Oct. 2012. [CrossRef]
- M. Arron et al., “Trends in risk factors of anastomotic leakage after colorectal cancer surgery (2011-2019), a Dutch population based study,” European Journal of Surgical Oncology, vol. 48, no. 2, p. e90, Feb. 2022. [CrossRef]
- Z. Hao, A. & Shing, W. Wong, Z. Hao Ang, and S. W. Wong, “Prevention of Anastomotic Leak in Colorectal Surgery: Current Knowledge and Next Steps,” Open Access Surgery, vol. Volume 17, pp. 11–20, Feb. 2024. [CrossRef]
- C. H. A. Lee, J. C. H. Kong, A. G. Heriot, S. Warrier, J. Zalcberg, and P. Sitzler, “Short-term outcome of emergency colorectal cancer surgery: results from Bi-National Colorectal Cancer Audit,” Int J Colorectal Dis, vol. 34, no. 1, pp. 63–69, Jan. 2019. [CrossRef]
- L. Hajirawala, C. Leonardi, G. Orangio, K. Davis, and J. Barton, “Urgent Inpatient Colectomy Carries a Higher Morbidity and Mortality than Elective Surgery,” Journal of Surgical Research, vol. 268, pp. 394–404, Dec. 2021. [CrossRef]
- H. K. Choi, W. L. Law, and J. W. C. Ho, “Leakage after resection and intraperitoneal anastomosis for colorectal malignancy: analysis of risk factors,” Dis Colon Rectum, vol. 49, no. 11, pp. 1719–1725, Nov. 2006. [CrossRef]
- W. A. A. Borstlap, E. Westerduin, T. S. Aukema, W. A. Bemelman, and P. J. Tanis, “Anastomotic Leakage and Chronic Presacral Sinus Formation After Low Anterior Resection: Results From a Large Cross-sectional Study,” Ann Surg, vol. 266, no. 5, pp. 870–877, Nov. 2017. [CrossRef]
- J. Yang, Y. Luo, T. Tian, P. Dong, and Z. Fu, “Effects of Neoadjuvant Radiotherapy on Postoperative Complications in Rectal Cancer: A Meta-Analysis,” J Oncol, vol. 2022, no. 1, p. 8197701, Jan. 2022. [CrossRef]
- M. M. Mankarious et al., “Neoadjuvant chemotherapy does not increase risk for anastomotic leak for simultaneous resection of primary colon cancer with synchronous liver metastasis: A NSQIP-colectomy analysis,” J Surg Oncol, vol. 128, no. 1, pp. 58–65, Jul. 2023. [CrossRef]
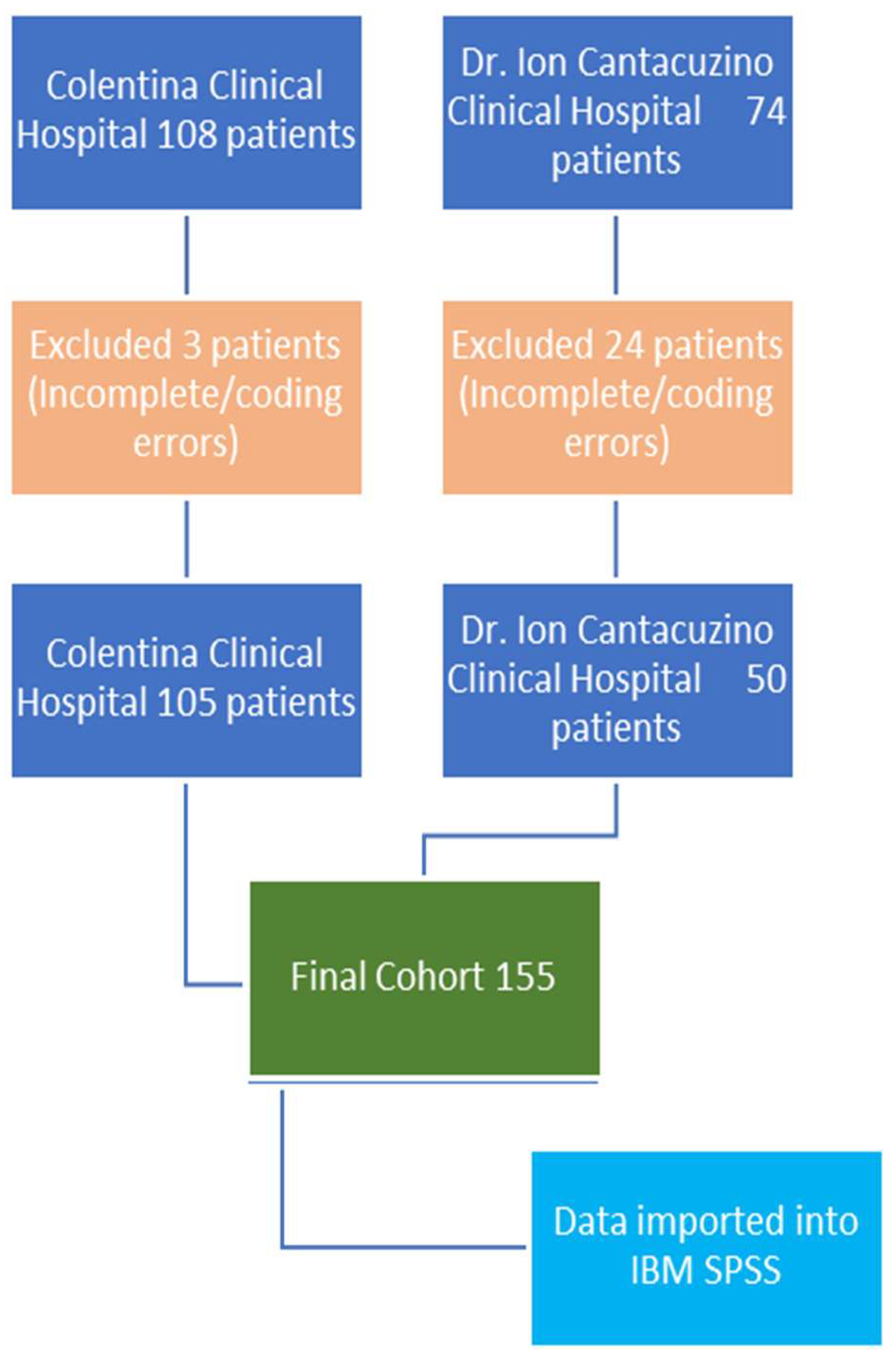
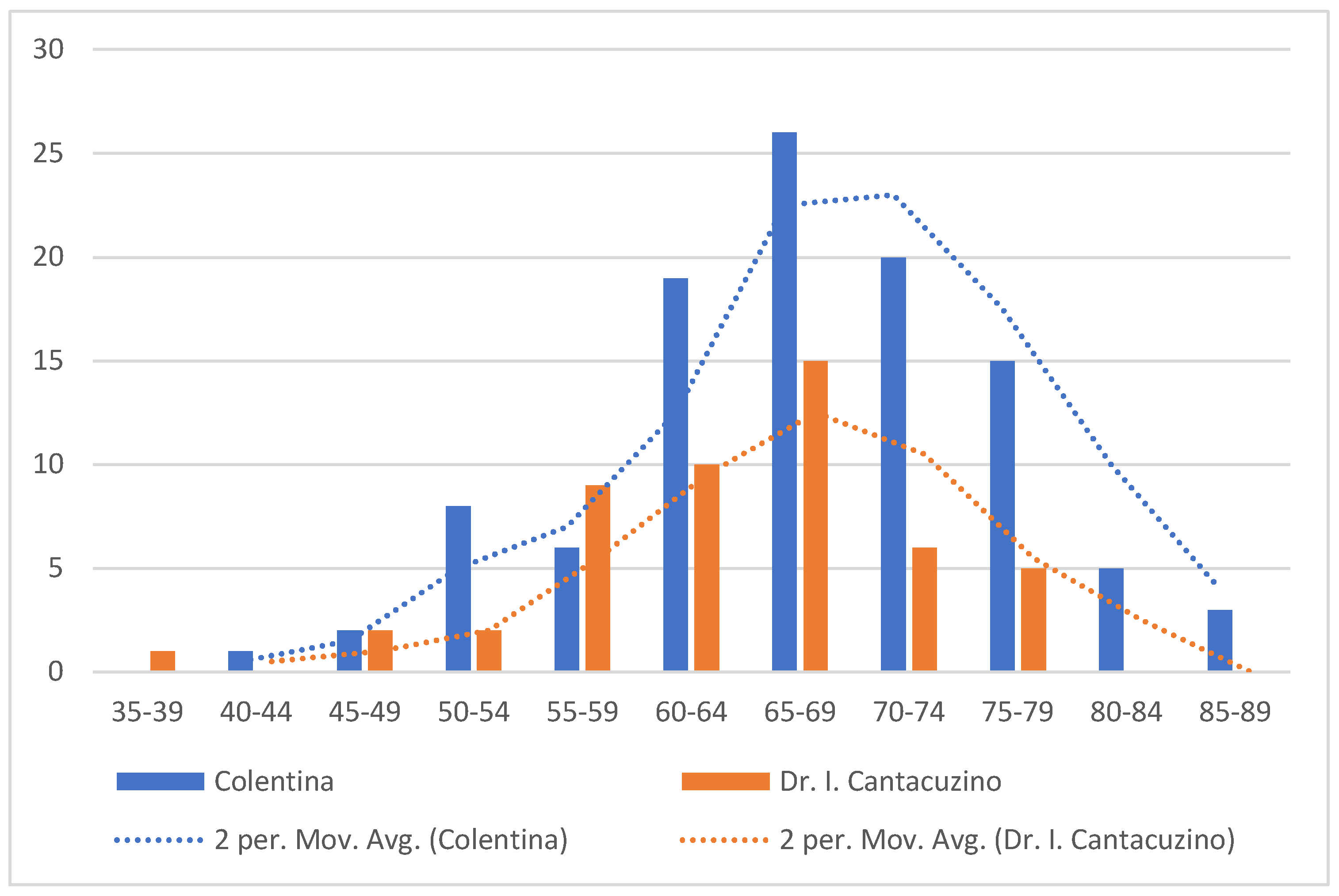
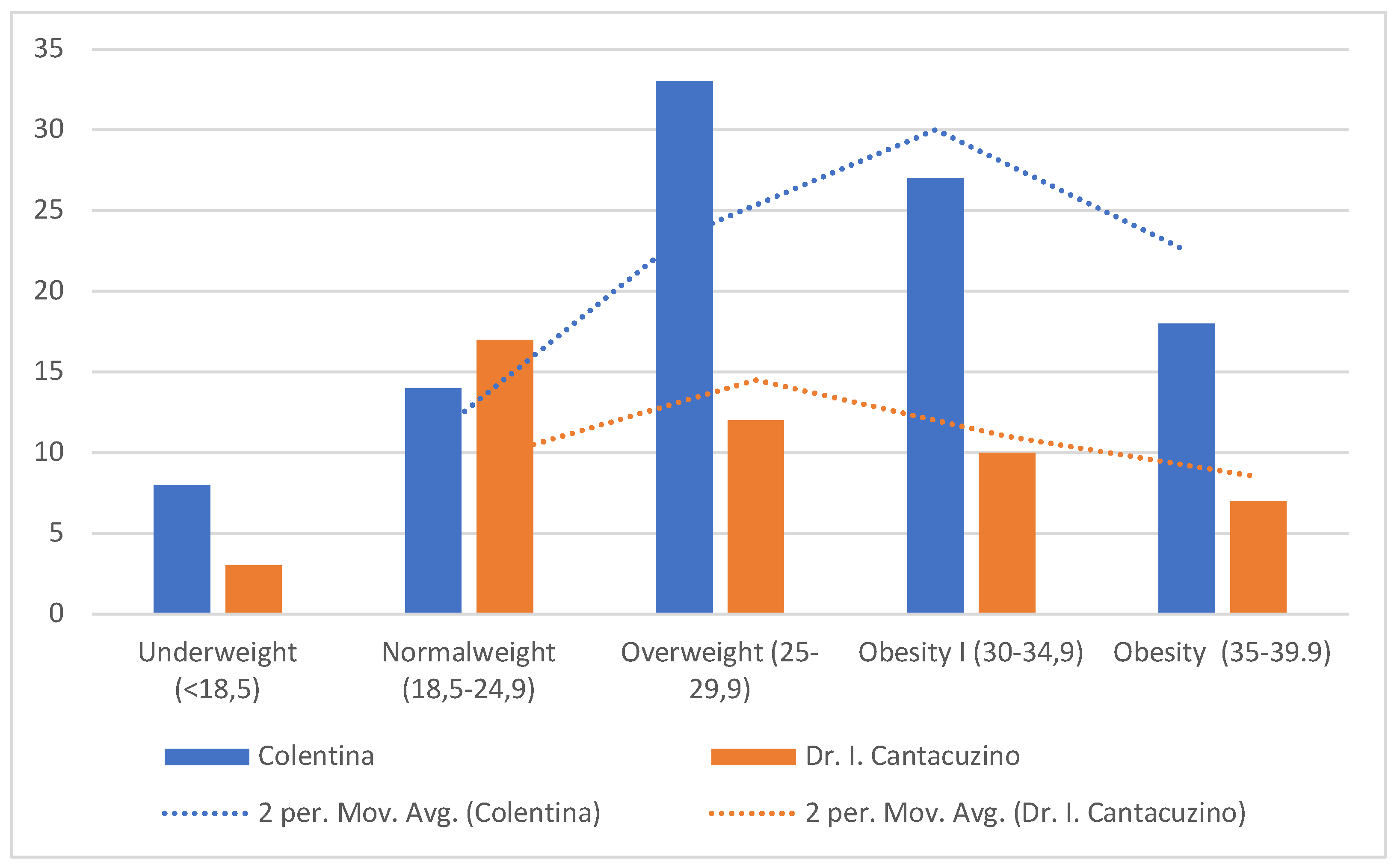
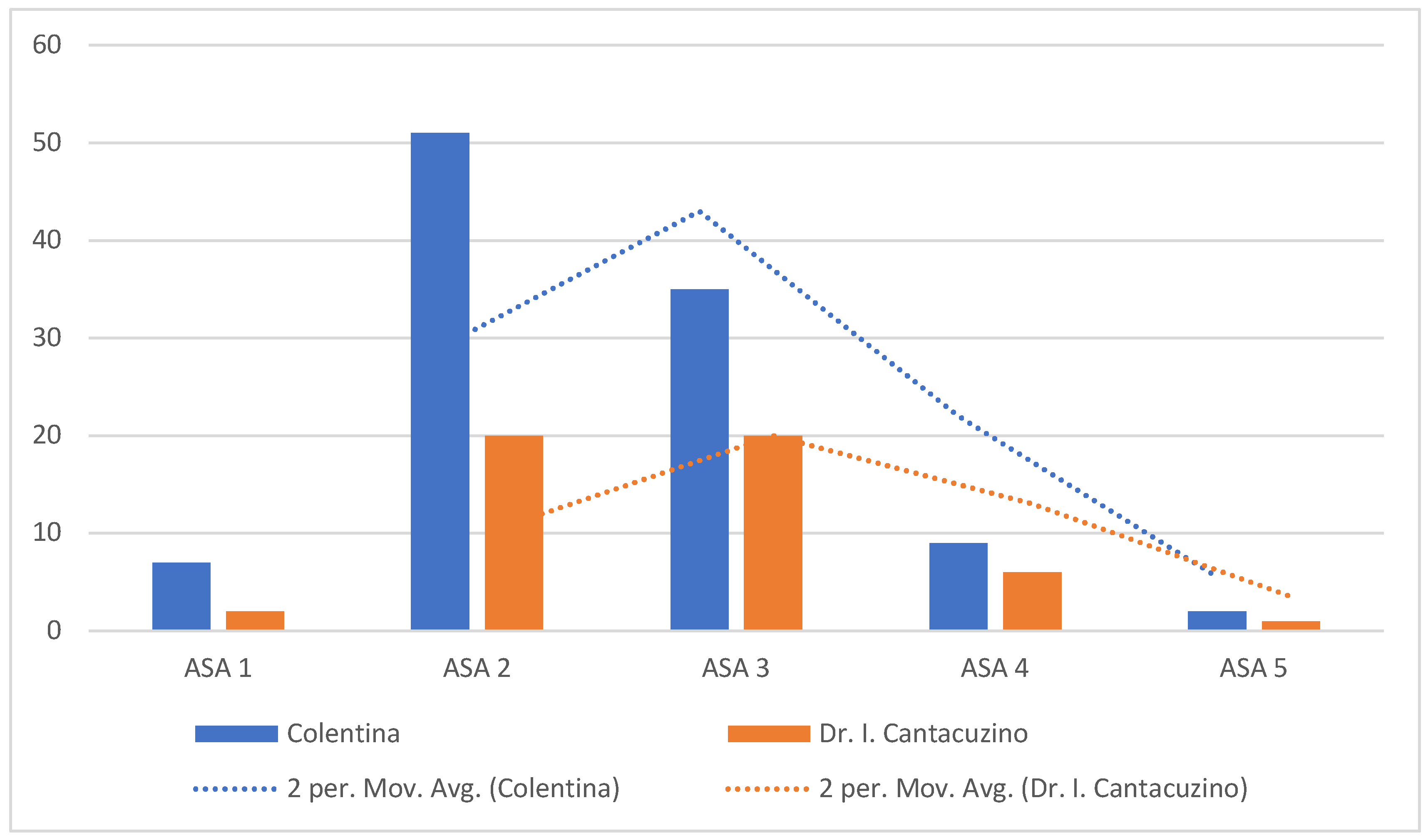
| Characteristic | Colentina (n=104) | Dr. I. Cantacuzino (n=49) | p-value |
| Age,years (mean±SD) | 67.4±9.0 | 64.0±8.2 | 0.021 |
| Female sex, n (%) | 42 (40.4%) | 22 (44.9%) | 0.72 |
| Diabetes (yes), n (%) | 23 (22.1%) | 9 (18.4%) | 0.75 |
| Cardio - Vascular comorbidity (yes), n (%) | 63 (60.6%) | 32 (65.3%) | 0.70 |
| Other comorbidity (yes), n (%) | 61 (58.7%) | 28 (57.1%) | 1.00 |
| Neoadjuvant chemotherapy (yes), n (%) | 16 (15.4%) | 16 (32.7%) | 0.025 |
| Neoadjuvant radiotherapy (yes), n (%) | 16 (15.4%) | 20 (40.8%) | 0.001 |
| Laparoscopic surgery, n (%) | 40 (38.5%) | 4 (6.1%) | <0.001 |
| Emergency surgery, n (%) | 5 (4.8%) | 0 (0%) | 0.28 |
| Protective stoma (yes), n (%) | 3 (2.9%) | 1 (2.0%) | 1.00 |
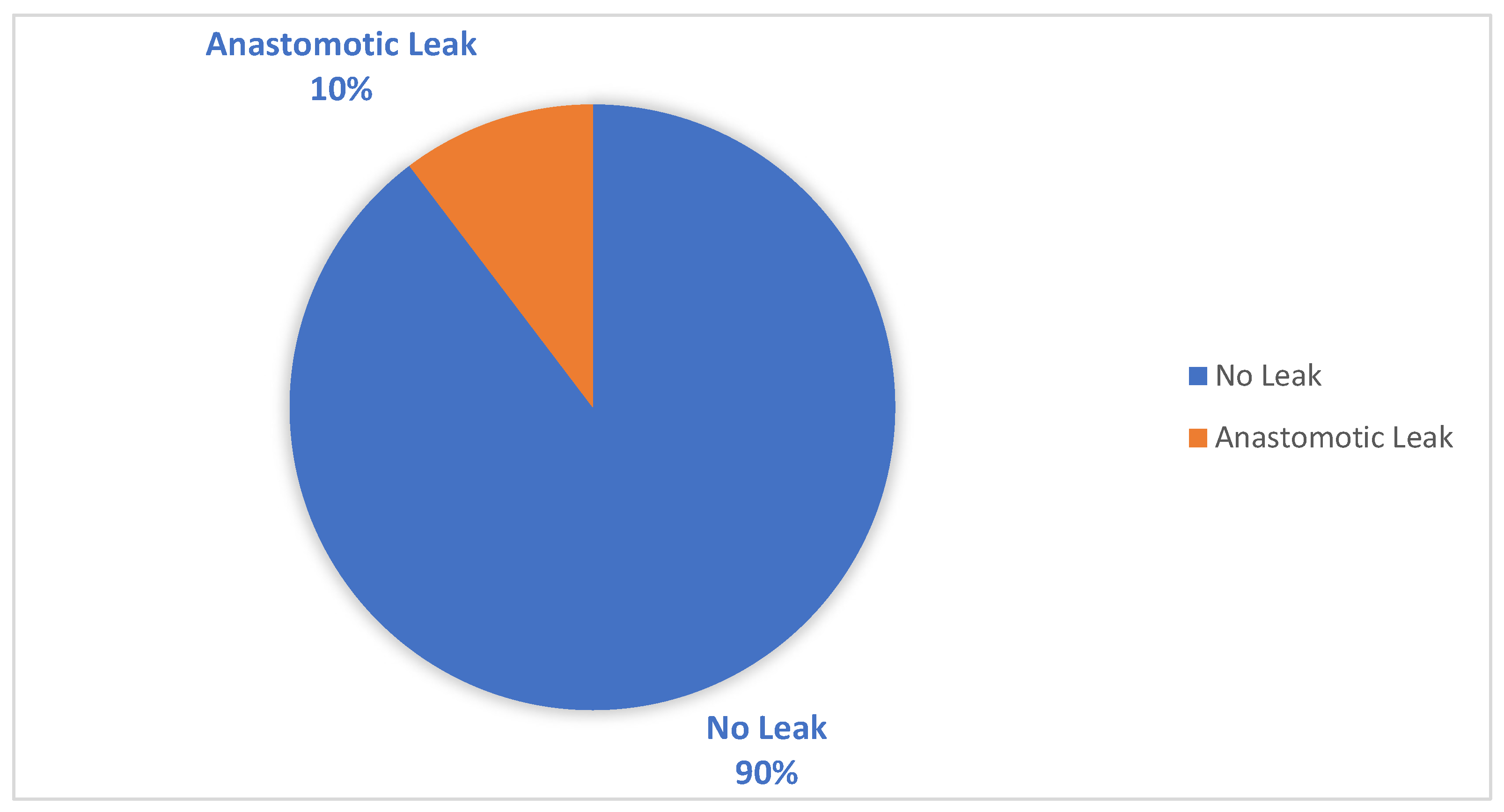
| Anastomotic leak, n (%) | 11 (10.6%) | 5 (10.2%) | 1.00 |
| Variable | Odds Ratio (OR) | 95% CI | p-value |
| Hemoglobin (g/dL) | 1.58 | 0.41–6.12 | 0.51 |
| WBC (10³/μL) | 1.68 | 0.43–6.54 | 0.45 |
| CRP (mg/L) | 1.17 | 0.14–10.0 | 0.89 |
| Albumin (g/dL) | 2.41 | 0.25–23.1 | 0.45 |
| Total Protein (g/dL) | 1.03 | 0.12–8.75 | 0.98 |
| Creatinine (mg/dL) | 1.66 | 0.49–5.64 | 0.42 |
| INR | 4.89 | 0.42–57.4 | 0.21 |
| Variable | Odds Ratio (95% CI) | p-value |
| Emergency surgery (vs elective) | 32.2 (4.34–238.0) | 0.0007 |
| Neoadjuvant radiotherapy (yes) | 4.80 (0.57–40.55) | 0.15 |
| Neoadjuvant chemotherapy (yes) | 1.09 (0.13–9.24) | 0.93 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




