Submitted:
18 December 2025
Posted:
22 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Measurement Instruments
- Static test: assessment of plantar load distribution between the left and right foot, and between the forefoot and rearfoot.
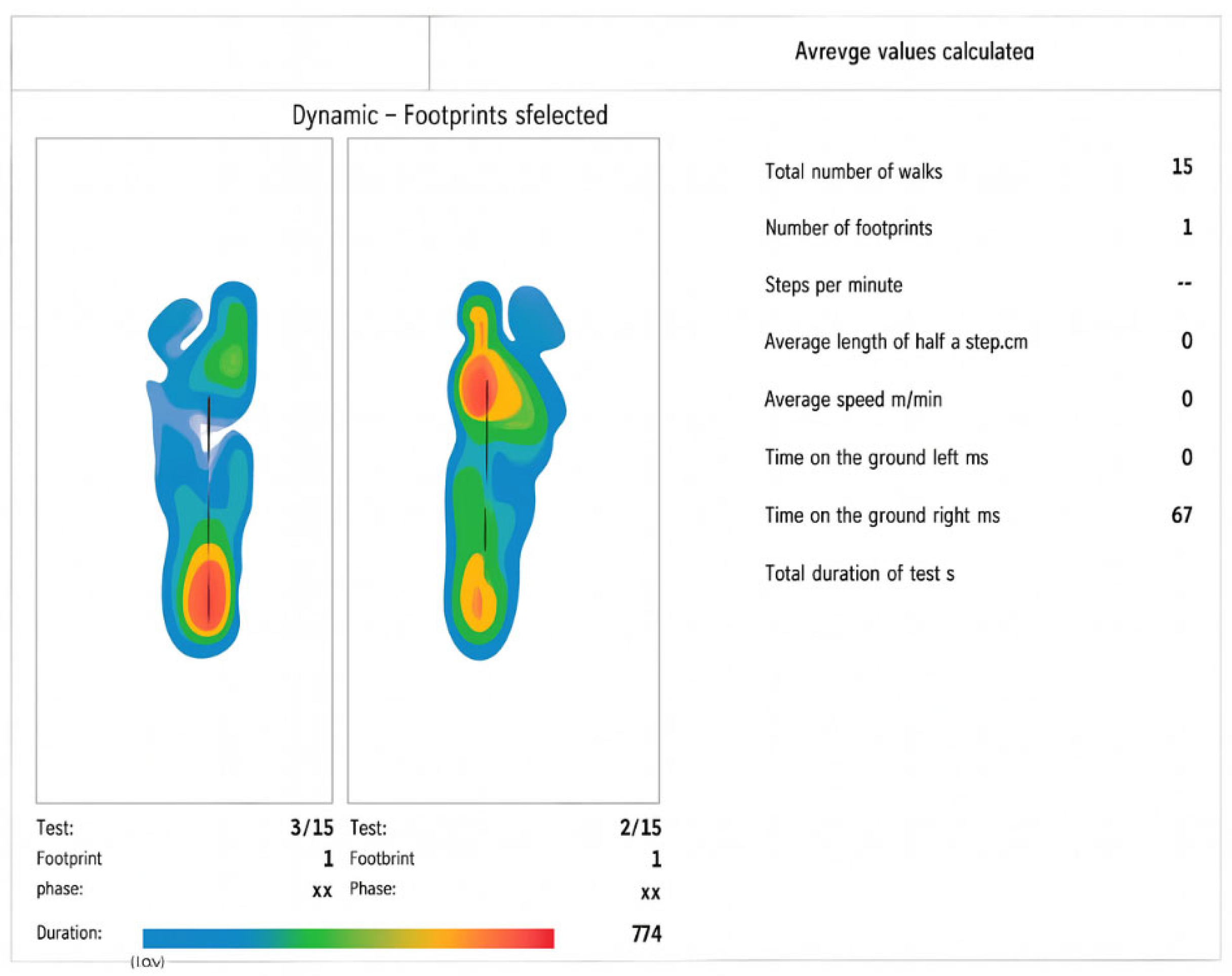
- Dynamic test: Analysis of successive footprints during gait, including stance and propulsion phases.
- Romberg test (eyes open and closed) was used to evaluate postural control and visual dependence.
- Computation of the sway ellipse area and CoP trajectory (path length and area) as indicators of balance stability.
2.3. Experimental Protocol
2.4. Parameters Analyzed
- Plantar load distribution: % load on the left vs. right foot; % load on the forefoot vs. rearfoot.
- Dynamic gait parameters: step length (cm), contact time (ms), and peak propulsion pressure (kPa).
- Stabilometric parameters:
- CoP sway area (mm²) and path length (mm)
- Anteroposterior and mediolateral oscillations (mm)
- Romberg index (ratio of eyes closed to eyes open).
| Category | Parameter | Unit | Description |
| Static plantar pressure | Left vs. right load distribution | % | Relative distribution of plantar load between left and right foot |
| Static plantar pressure | Forefoot vs. rearfoot load distribution | % | Relative distribution of plantar load between forefoot and rearfoot |
| Dynamic gait | Step length | cm | Distance between two successive steps |
| Dynamic gait | Contact time | ms | Duration of foot–ground contact |
| Dynamic gait | Peak propulsion pressure | kPa | Maximum plantar pressure generated during propulsion |
| Stabilometry | CoP sway area | mm² | Area covered by center of pressure oscillations |
| Stabilometry | CoP path length | mm | Total length of the CoP trajectory during test |
| Stabilometry | Romberg index | ratio (eyes closed/open) | Ratio of postural stability with eyes closed vs. eyes open |
3. Results
- HW1 (Baropodometric analysis): Static plantar pressure distribution indicated a slight left–right asymmetry, with a predominance of left-foot loading (51%) compared to the right (49%), and a posterior tendency with greater rearfoot support (62%). Dynamic analysis confirmed this pattern, with the left side contributing to a longer stance duration, while the right side generated higher propulsion forces. These findings support HW1 by demonstrating detectable asymmetries, even in a healthy subject.
- HW2 (Stabilometric analysis): Stabilometric testing revealed increased postural sway under visual deprivation, with a larger sway ellipse area and a Romberg index exceeding 2.0. These results are consistent with those of HW2, indicating that children exhibit a strong reliance on vision to maintain balance.
- HW3 (Combined feasibility): Together, the baropodometric and stabilometric results demonstrate the feasibility of integrating these complementary methods for symmetry and asymmetry assessment in pediatric populations, supporting HW3.
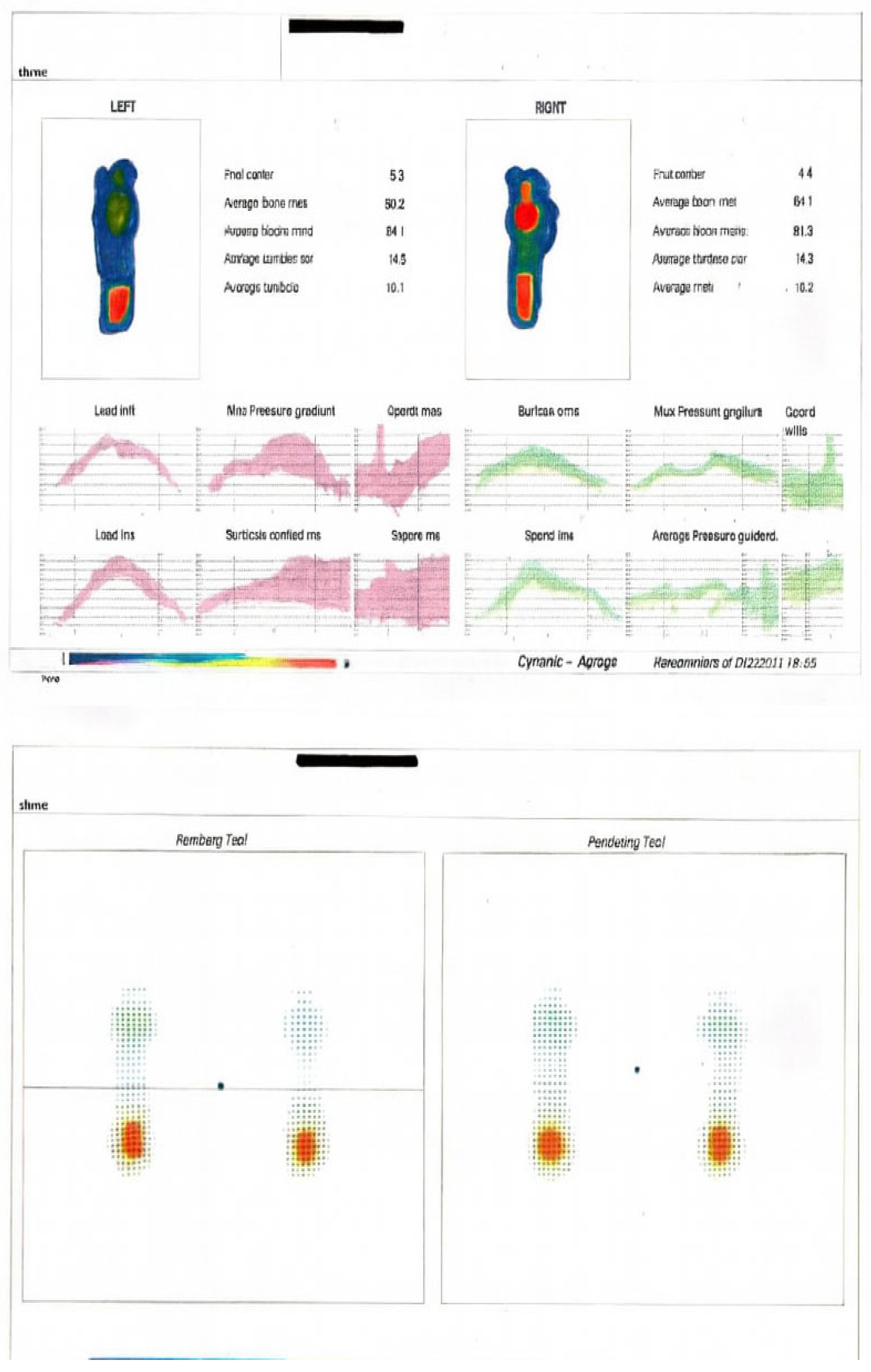
3.1. Static Baropodometric Analysis
| Foot | Load (%) | Forefoot (%) | Rearfoot (%) |
|---|---|---|---|
| Left | 51 | 37 | 63 |
| Right | 49 | 39 | 61 |
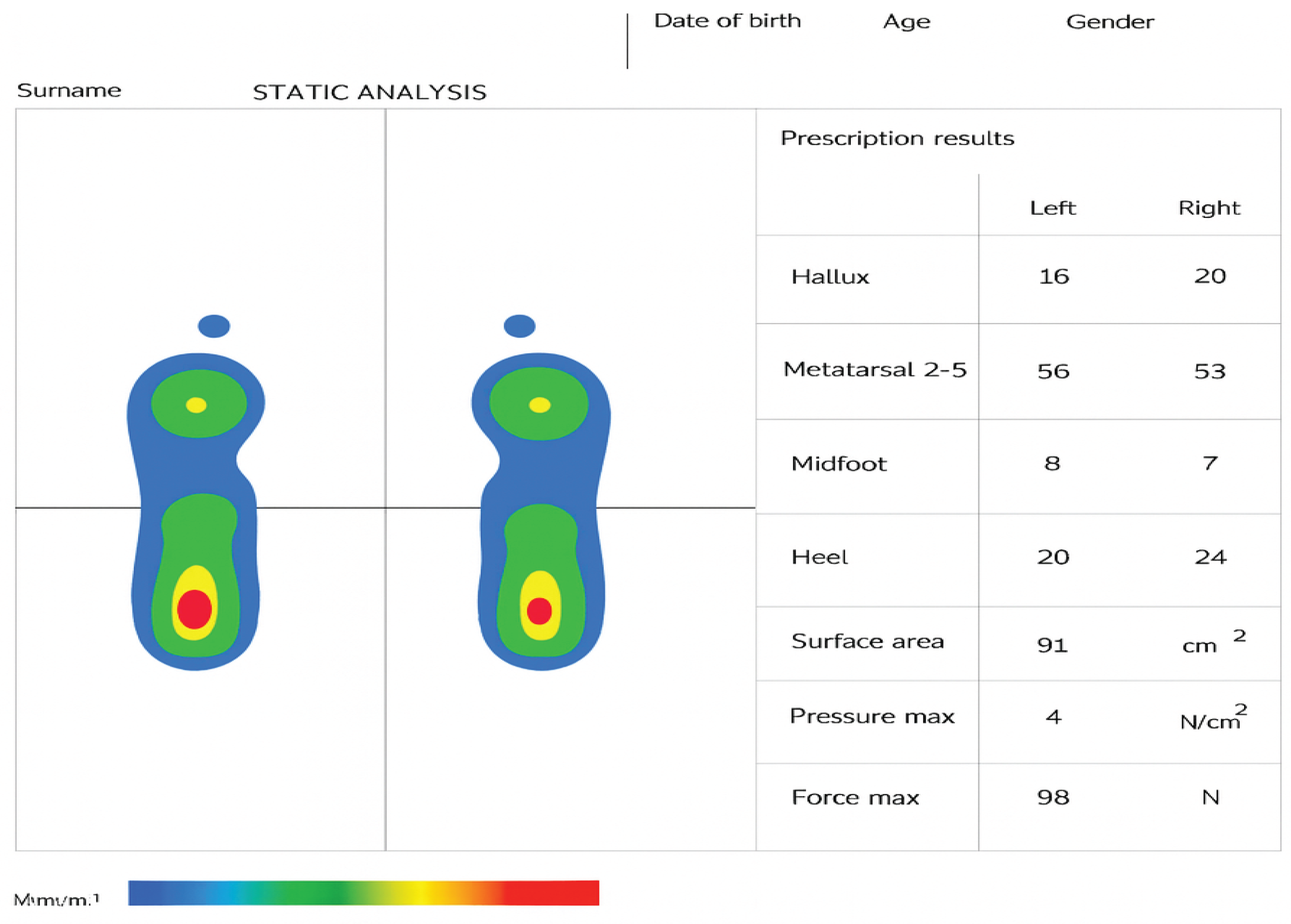
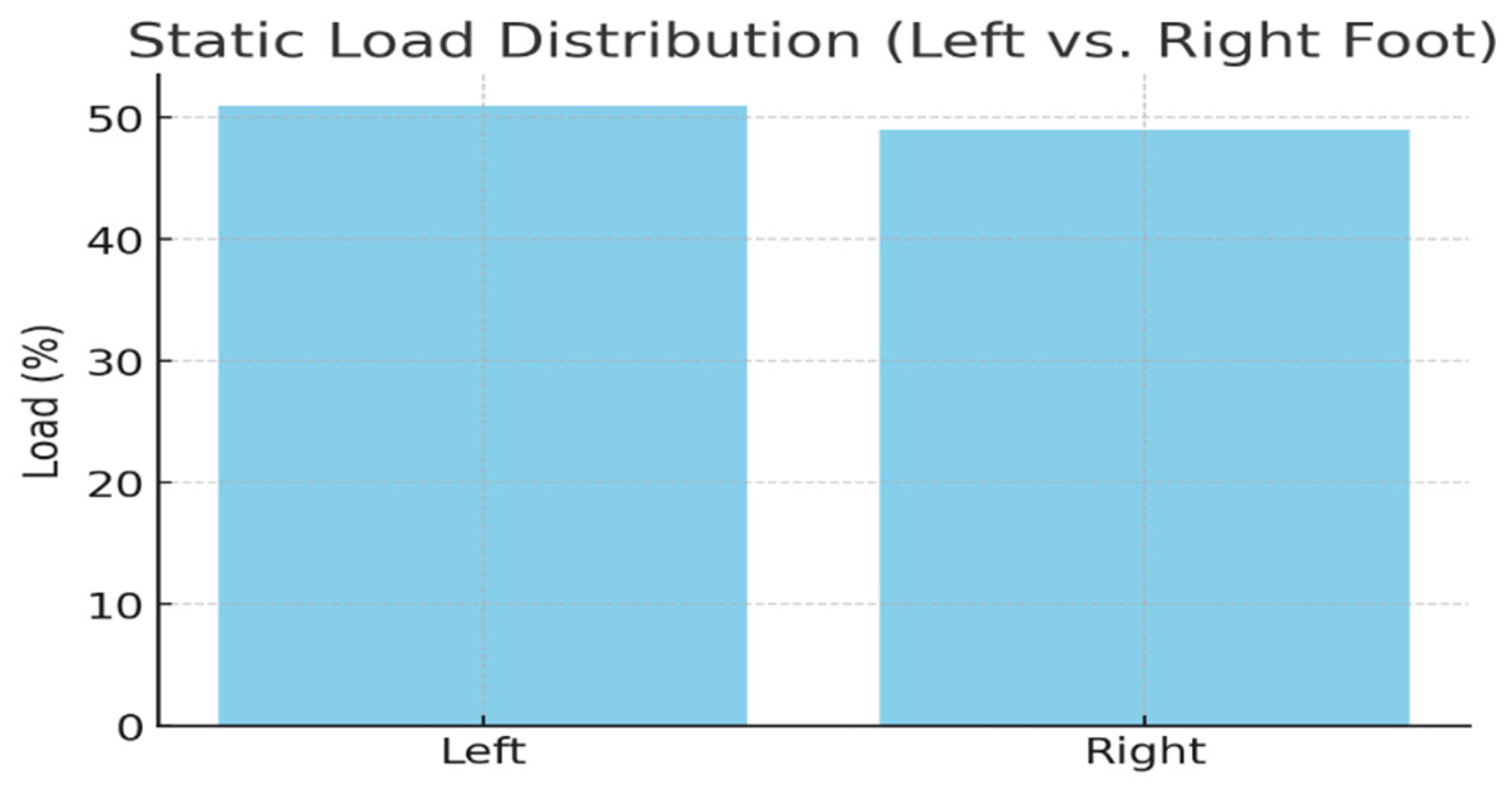
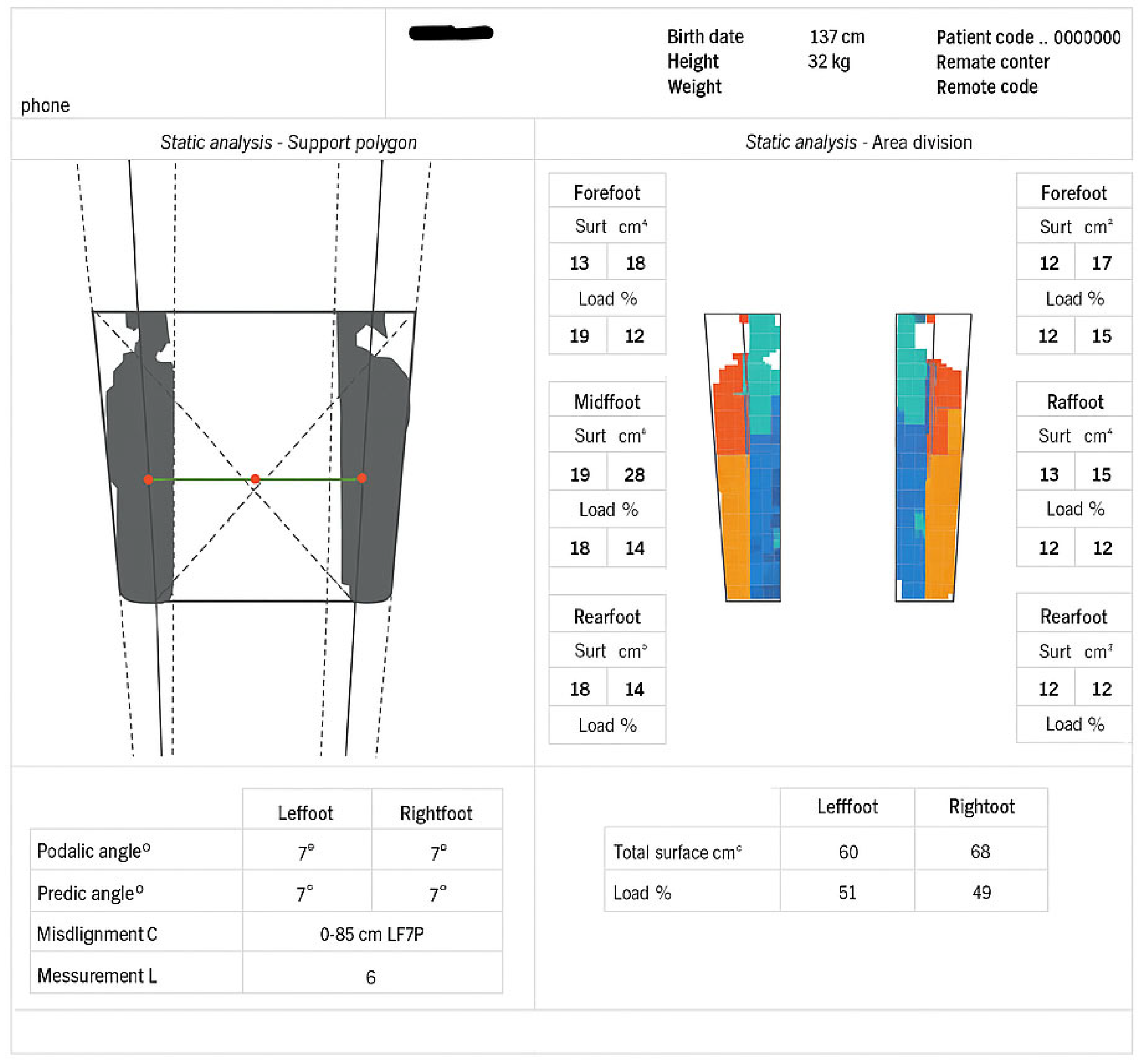
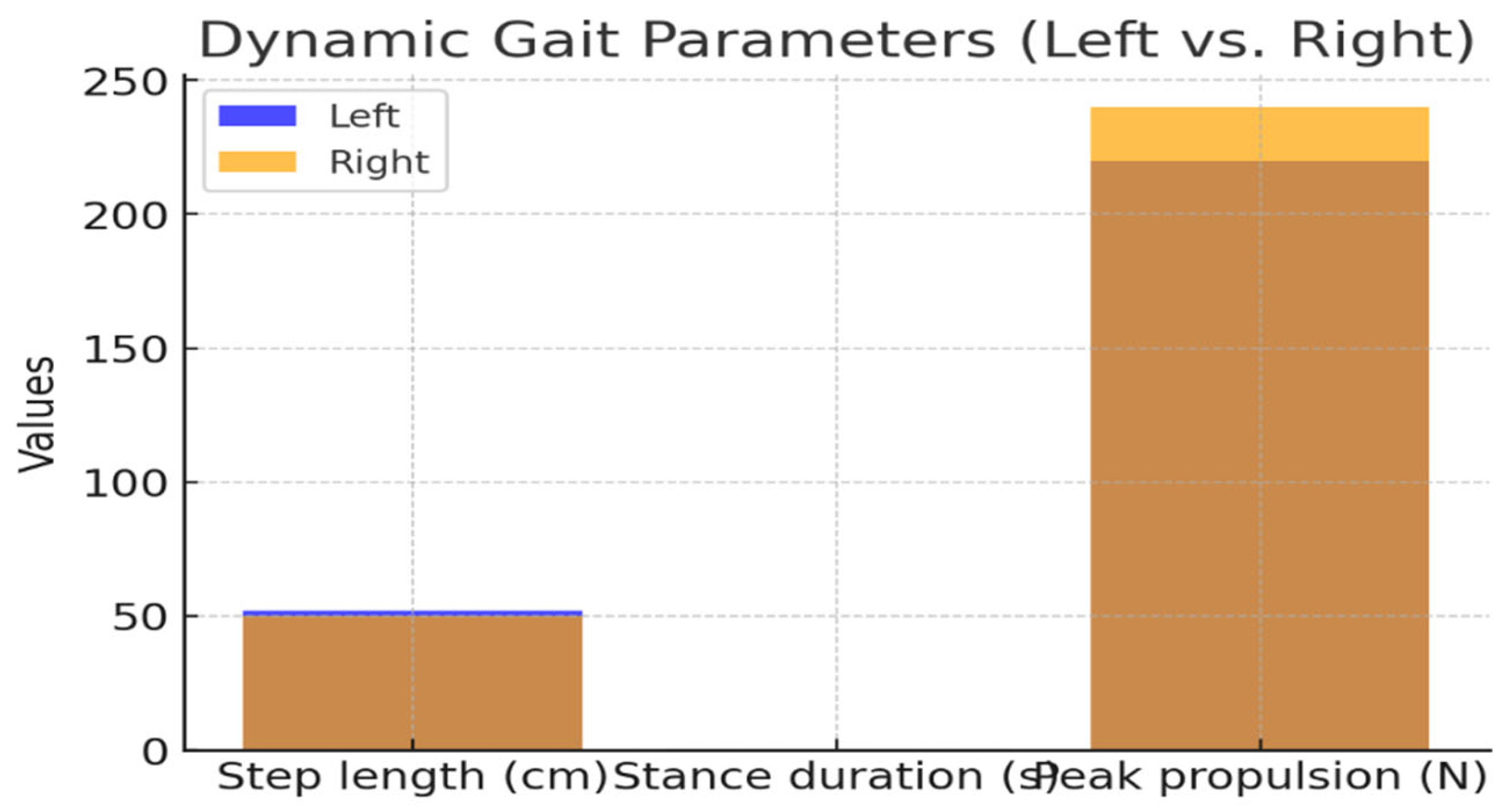
3.2. Dynamic Baropodometric Analysis
| Parameter | Left Foot | Right Foot |
|---|---|---|
| Step length (cm) | 52 | 50 |
| Stance duration (s) | 0.72 | 0.68 |
| Peak propulsion (N) | 220 | 240 |
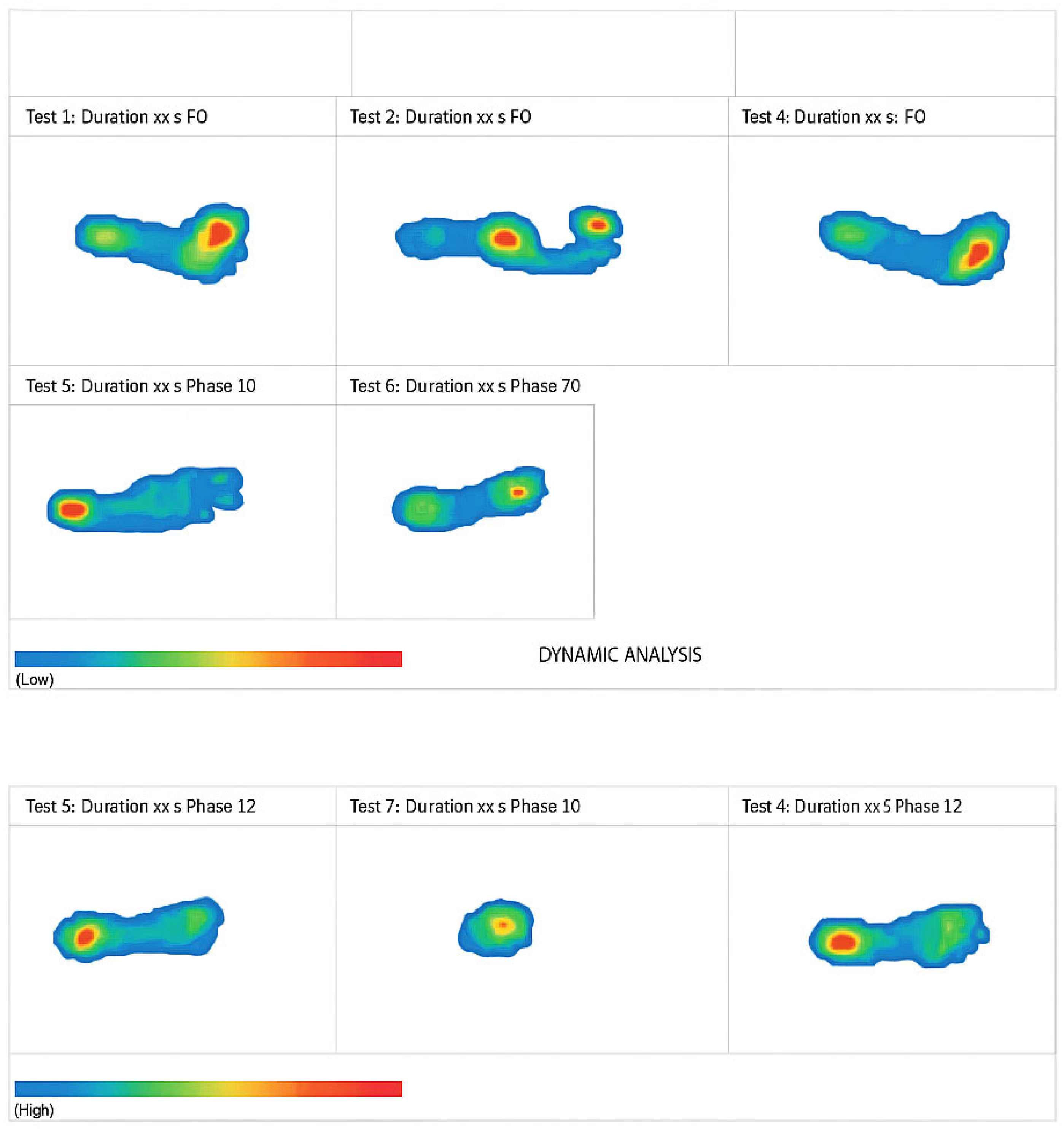
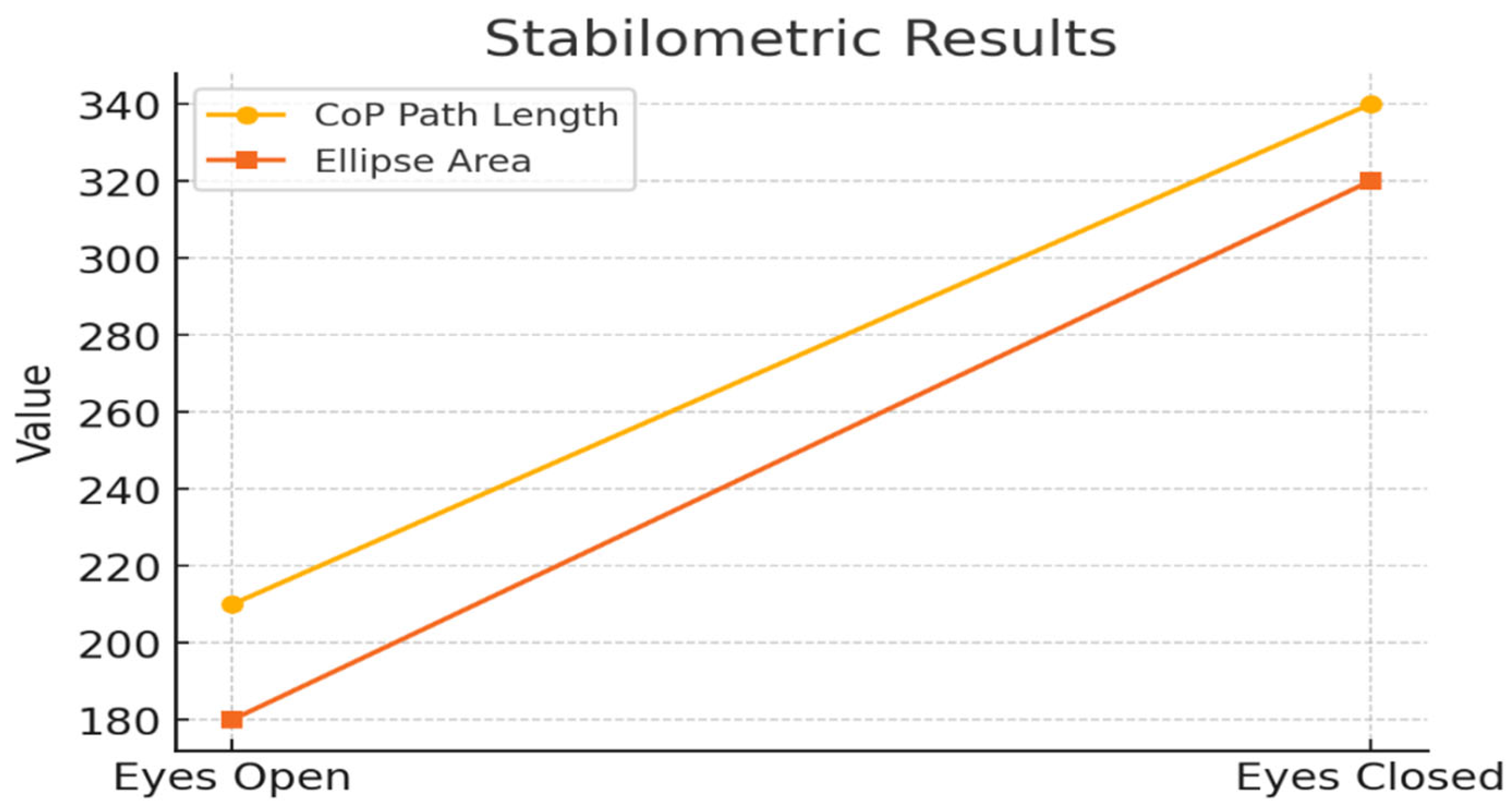
3.3. Stabilometric Analysis
| Condition | CoP Path Length (mm) | Ellipse Area (mm²) | Romberg Index |
|---|---|---|---|
| Eyes Open | 210 | 180 | 1.0 |
| Eyes Closed | 340 | 320 | 2.1 |
4. Discussion
4.1. HW1 – Baropodometric Analysis and Plantar Load Asymmetries
4.2. HW2 – Stabilometric Analysis and Visual Dependence in Postural Control
4.3. HW3 – Combined Feasibility of Baropodometric and Stabilometric Assessment
4.4. Clinical Implications
4.5. Gait and Postural Symmetry Assessment in Pediatric Prevention and Rehabilitation
4.6. Future Research Directions
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CoP | Center of Pressure |
References
- De Menezes, L.T.; Barbosa, P.H.F.A.; Costa, A.S.; Mundim, A.C.; Ramos, G.C.; Paz, C.C.S.C.; Martins, E.F. Baropodometric technology used to analyze types of weight-bearing during hemiparetic upright position. Fisioter. em Mov. 2012, 25(3), 583–594. [Google Scholar] [CrossRef]
- Paolucci, T.; Fusco, A.; Iosa, M.; Grasso, M.R.; Spadini, E.; Paolucci, S.; Saraceni, V.M.; Morone, G. The efficacy of a perceptive rehabilitation on postural control in patients with chronic nonspecific low back pain. Clin. Rehabil. 2012, 26(4), 335–345. [Google Scholar] [CrossRef] [PubMed]
- Marin, L.; Kawczyński, A.; Carnevale Pellino, V.; Febbi, M.; Silvestri, D.; Pedrotti, L.; Lovecchio, N.; Vandoni, M. Displacement of centre of pressure during rehabilitation exercise in adolescent idiopathic scoliosis patients. J. Clin. Med. 2021, 10(13), 2837. [Google Scholar] [CrossRef] [PubMed]
- Doshi, K.B.; Moon, S.H.; Whitaker, M.D.; Lockhart, T.E. Assessment of gait and posture characteristics using a smartphone wearable system for persons with osteoporosis with and without falls. Sci. Rep. 2023, 13(1), 538. [Google Scholar] [CrossRef]
- Maden, T.K.; Bayramlar, K.Y.; Yakut, Y. The effect of cervical mobilization on balance and static plantar loading distribution in patients with multiple sclerosis: A randomized crossover study. Neurosciences 2022, 27(1), 31–39. [Google Scholar] [CrossRef]
- Monteiro-Rodrigues, L.; Nuno, S.L.; Granja, T.; Florindo, M.E.; Gregório, J.; Atalaia, T. Perfusion, stance and plantar pressure asymmetries in the absence of disease—A pilot study. Symmetry 2022, 14(3), 441. [Google Scholar] [CrossRef]
- Shibata, D.; Yoshida, Y. Self-Mobilization Exercise Program Improved Postural Stability in the Anterior-Posterior Direction with Eyes Closed. Symmetry 2023, 15(7), 1321. [Google Scholar] [CrossRef]
- Glowinski, S.; et al. Gait analysis with an upper limb prosthesis in a child: Influence on plantar pressures and gait symmetry. J. Clin. Med. 2025, 14(7), 2245. [Google Scholar] [CrossRef]
- Molina-García, C.; Álvarez-Salvago, F.; Pujol-Fuentes, C.; López-del-Amo-Lorente, A.; Ramos-Petersen, L.; Martínez-Sebastián, C.; Martínez-Amat, A.; Jiménez-García, J.D.; De Diego-Moreno, M. Influence of foot type on physical characteristics, laxity, strength and baropodometry in children aged 5–10 years. Appl. Sci. 2024, 14(19), 8578. [Google Scholar] [CrossRef]
- Mocanu, G.; et al. Analysis of the influence of age stages on static plantar pressure indicators using a baropodometric platform. Appl. Sci. 2021, 11(16), 7320. [Google Scholar] [CrossRef]
- Kojić, M.; et al. The relationship between foot status and motor status in preschool-aged children. Healthcare 2021, 9(8), 936. [Google Scholar] [CrossRef] [PubMed]
- Daunoravičienė, K.; et al. EMG-based analysis of gait symmetry in healthy children. Sensors 2021, 21(17), 5983. [Google Scholar] [CrossRef] [PubMed]
- Chernik, N.D.; Young, M.W.; Jacobson, R.N.; Kantounis, S.J.; Lynch, S.K.; Virga, J.Q.; Cannata, M.J. Effects of high-intensity training on gait symmetry and locomotor performance in neurodivergent children: A pilot study. Symmetry 2025, 17(7), 1073. [Google Scholar] [CrossRef]
- Fullin, A.; Caravaggi, P.; Picerno, P.; Mosca, M.; Caravelli, S.; De Luca, A.; Lucariello, A.; De Blasiis, P. Variability of postural stability and plantar pressure parameters in healthy subjects evaluated by a novel pressure plate. Int. J. Environ. Res. Public Health 2022, 19(5), 2913. [Google Scholar] [CrossRef]
- Abou Ghaida, H.; Poffo, L.; Le Page, R.; Goujon, J.-M. Effect of Sensor Size, Number and Position under the Foot to Measure the Center of Pressure (CoP) Displacement and Total Center of Pressure (CoPT) Using an Anatomical Foot Model. Sensors 2023, 23(10), 4848. [Google Scholar] [CrossRef]
- Liu, W.; et al. Biomechanical characteristics of typically developing toddlers. Children 2022, 9(3), 406. [Google Scholar] [CrossRef]
- Serrato-Pedrosa, J.A.; et al. Biomechanical evaluation of plantar pressure distribution in soft tissue during standing. Appl. Sci. 2024, 14(4), 1650. [Google Scholar] [CrossRef]
- Taborri, J.; et al. Comparison of Machine Learning Algorithms Fed with Mobility-Related and Baropodometric Measurements to Identify Temporomandibular Disorders. Sensors 2024, 24(11), 3646. [Google Scholar] [CrossRef]
- Loukovitis, A.; et al. Test–retest reliability of PODOSmart® gait analysis insoles. Sensors 2021, 21(22), 7532. [Google Scholar] [CrossRef]
- Babović, S.S.; et al. Labeling of baropodometric analysis data using computer vision: Evaluation of foot progression angle. Medicina 2023, 59(5), 840. [Google Scholar] [CrossRef]
- Fan, Y.; Fan, Y.; Li, Z.; Lv, C.; Luo, D. Natural gaits of the non-pathological flat foot and high-arched foot. arXiv. 2010. Available online: https://arxiv.org/abs/1012.3816.
- Patwari, M.; Chazistergos, P.; Sundar, L.; Chockalingam, N.; Ramachandran, A.; Naemi, R. A quantitative comparison of plantar soft tissue strainability distribution and homogeneity between ulcerated and non-ulcerated patients using ultrasound strain elastography. Proc Inst Mech Eng H. 2022, 236(5), 722–729. [Google Scholar] [CrossRef] [PubMed]
- Serrato-Pedrosa, J.A.; et al. Numerical Analysis of the Plantar Pressure Points during the Stance Phases for the Design of a 3D-Printable Patient-Specific Insole. Symmetry 2024, 6(3), 429–456. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, P.; Chen, G.; Jiang, T.; Zou, Y. Comparison of the asymmetries in foot posture, gait and plantar pressure between patients with unilateral and bilateral knee osteoarthritis based on a cross-sectional study. Sci. Rep. 2024, 14, 26761. [Google Scholar] [CrossRef] [PubMed]
- Gurău, T.V.; et al. Static Baropodometric Assessment for Musculoskeletal Rehabilitation: Plantar Pressure and Postural Load Distribution in Young Adults. Life 2025, 15(9), 1354. [Google Scholar] [CrossRef]
- Bittar K.C.B..; et al. Reliability of plantar pressure and postural control measures of children from 4 to 12 years: analysis by baropodometry. Motriz: rev. educ. fis. 2020, 26 (03). [CrossRef]
- Baptista, C.R.J.A.; et al. Characterizing postural oscillation in children and adolescents with hereditary sensorimotor neuropathy. PLoS ONE 2018, 13(10), e0204949. [Google Scholar] [CrossRef]
- Purpura, G.; et al. Use of Virtual Reality in School-Aged Children with Developmental Coordination Disorder: A Novel Approach. Sensors 2024, 24(17), 5578. [Google Scholar] [CrossRef]
- Kiefer, A.W.; et al. Postural control development from late childhood through young adulthood. Gait Posture 2021, 86, 169–173. [Google Scholar] [CrossRef]
- Feng, Z.Y.; Li, J.Y.; Li, Y.W.; et al. Long term gait postural characteristics of children with general foot pain using smartphone connected wearable sensors. Sci. Rep. 2025, 15, 7767. [Google Scholar] [CrossRef]
- Shulman, D.; et al. Gait Symmetry Analysis in Patients after Treatment of Pilon Fractures by the Ilizarov Method. Symmetry 2021, 13(2), 349. [Google Scholar] [CrossRef]
- Eldridge, S. M.; Lancaster, G. A.; Campbell, M. J.; Thabane, L.; Hopewell, S.; Coleman, C. L.; Bond, C. M. Defining feasibility and pilot studies in preparation for randomised controlled trials: Development of a conceptual framework. PLoS ONE 2016, 11(3), e0150205. [Google Scholar] [CrossRef]
- Hertzog, M. A. Considerations in determining sample size for pilot studies. Research in Nursing & Health 2008, 31(2), 180–191. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




