Submitted:
17 December 2025
Posted:
18 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Research Methods
2.2. Study Organisation and Procedure
2.3. Participants
3. Results
4. Discussion
Implications for Practice
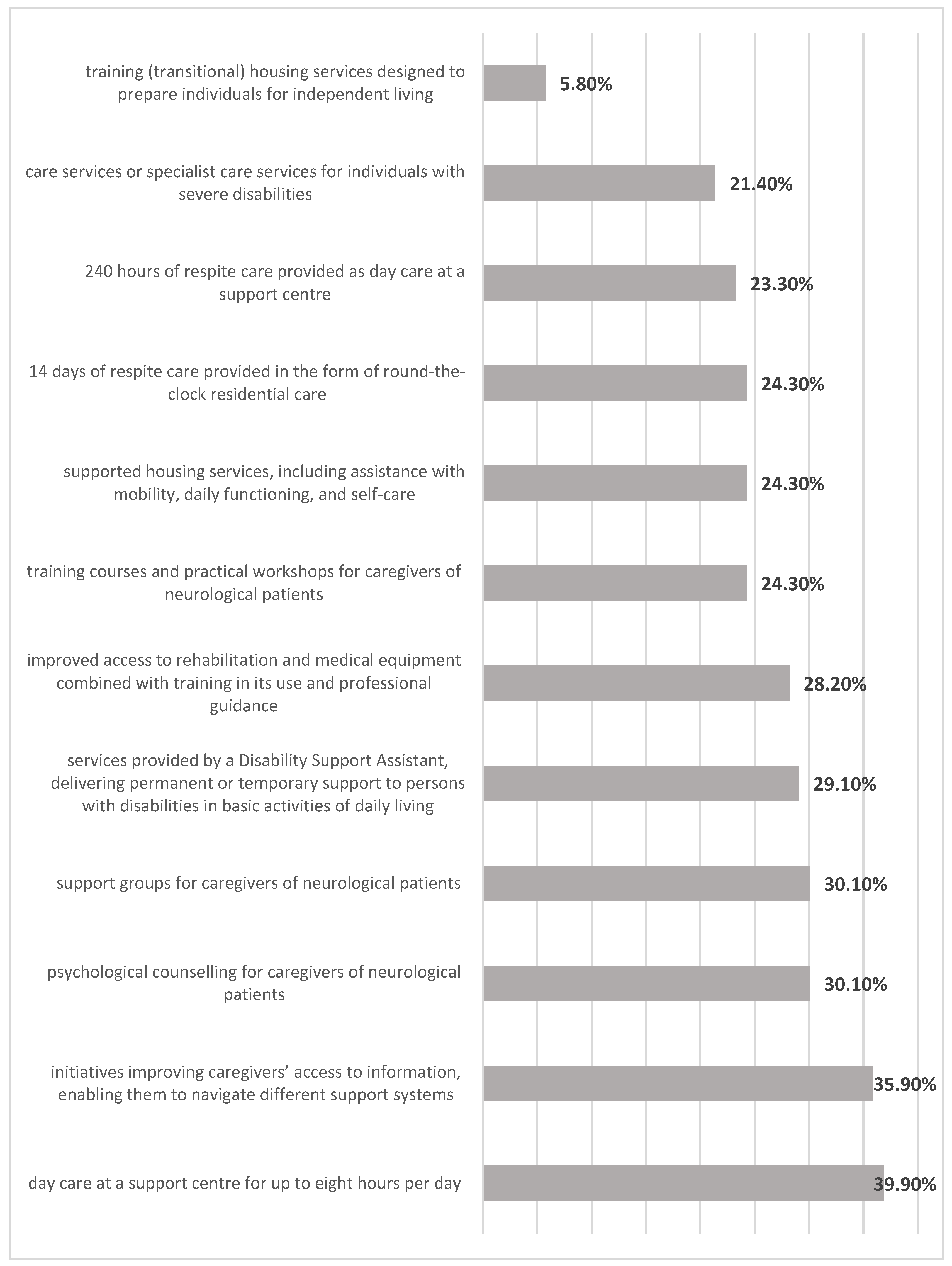
- Expansion of respite care services, including both day care and 24-hour options.Caregivers clearly need opportunities for temporary relief from caregiving. Access to respite care can substantially reduce the risk of physical and emotional exhaustion.
- Improved access to rehabilitation, neurological consultations, and publicly funded healthcare services., Limited availability of these services was one of the most frequently reported barriers. Improving access may reduce waiting times, ease the burden on caregivers, and increase the effectiveness of formal care.
- Strengthening information and educational support systems.Caregivers require clear, reliable, and practical information about the illness, available benefits, medical equipment, and care organisation. Closing information gaps may reduce uncertainty and enhance caregivers’ confidence and sense of competence.
- Provision of psychological support and support groups. Although not the most commonly selected forms of assistance, psychological support and peer groups can make a difference in preventing caregiver burnout and supporting emotional wellbeing.
- Training and educational programmes for caregivers, focusing on home-based care, managing crisis situations, navigating the healthcare system, and using medical and rehabilitation equipment.
- Development of coordinated, interdisciplinary care pathways that consider the needs of both care recipients and caregivers, in line with Integrated Care initiatives promoted across Europe.
Strengths and limitations of the Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| BSSS | Berlin Social Support Scales |
References
- Bartoszek, A; Slusarska, B; Deluga, A; Nowicki, G; Piasecka, K; Kocka, K; et al. Selected determinants of burden among informal caregivers according to the COPE Index in home care for patients with functional impairment. 2019, 59, 164–71. [Google Scholar]
- Wei, L; Zhao, X; Chen, X; He, Y; Liu, J; Xian, J; et al. Caregiver Burden and Its Associated Factors Among Family Caregivers of Hospitalized Patients with Neurocritical Disease: A Cross-Sectional Study. J Multidiscip Healthc 2024, 17, 5593–603. [Google Scholar] [CrossRef]
- Ryś, B; Bąk, E. Factors Determining the Burden of a Caregiver Providing Care to a Post-Stroke Patient. Journal of Clinical Medicine 2025, 14(9), 3008. [Google Scholar] [CrossRef]
- Walkowiak, D; Jabkowski, P; Domaradzki, J. Validation of the Zarit Burden Interview for Polish caregivers of individuals with rare diseases: a multidimensional approach to assessing caregiver burden. BMC Psychol 2025, 13(1), 1024. [Google Scholar] [CrossRef]
- Liu, Z; Heffernan, C; Tan, J. Caregiver burden: A concept analysis. Int J Nurs Sci 2020, 7(4), 438–45. [Google Scholar] [CrossRef]
- Maksymowicz-Śliwińska A, Lulé D, Nieporęcki K, Ciećwierska K, Ludolph AC, Kuźma-Kozakiewicz M. The quality of life and depression in primary caregivers of patients with amyotrophic lateral sclerosis is affected by patient-related and culture-specific conditions. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration [Internet]. 2023 [cited 2025 Dec 7];24(3–4). Available online: https://ppm.wum.edu.pl/info/article/WUM.
- George, LK; Gwyther, LP. Caregiver Weil-Being: A Multidimensional Examination of Family Caregivers of Demented Adults. The Gerontologist [Internet] 1986, 26(3), 253–9. Available online: https://academic.oup.com/gerontologist/article-lookup/doi/10.1093/geront/26.3.253. [CrossRef] [PubMed]
- Xie, Y; Shen, S; Liu, C; Hong, H; Guan, H; Zhang, J; et al. Internet-Based Supportive Interventions for Family Caregivers of People With Dementia: Randomized Controlled Trial. JMIR Aging 2024, 7, e50847. [Google Scholar] [CrossRef]
- Ting CY, Ahmed Z. Impact of caregiver interventions on caregiver burden in adult traumatic brain injury: a systematic review and meta-analysis. Front Public Health [Internet]. 2025 Dec 3 [cited 2025 Dec 7];13. Available online: https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2025.1698592/full.
- Bleijlevens, MHC; Stolt, M; Stephan, A; Zabalegui, A; Saks, K; Sutcliffe, C; et al. Changes in caregiver burden and health-related quality of life of informal caregivers of older people with Dementia: evidence from the European RightTimePlaceCare prospective cohort study. Journal of Advanced Nursing [Internet] 2015, 71(6), 1378–91. Available online: https://onlinelibrary.wiley.com/doi/10.1111/jan.12561. [CrossRef] [PubMed]
- Hvalič-Touzery, S; Trkman, M; Dolničar, V. Caregiving Situation as a Predictor of Subjective Caregiver Burden: Informal Caregivers of Older Adults during the COVID-19 Pandemic. IJERPH [Internet]. 2022 Nov 4 [cited 2025 Dec 15];19(21):14496. Available online: https://www.mdpi.com/1660-4601/19/21/14496.
- Winblad, B; Amouyel, P; Andrieu, S; Ballard, C; Brayne, C; Brodaty, H; et al. Defeating Alzheimer’s disease and other dementias: a priority for European science and society. The Lancet Neurology [Internet] 2016, 15(5), 455–532. Available online: https://linkinghub.elsevier.com/retrieve/pii/S1474442216000624. [CrossRef]
- Brodaty, H; Donkin, M. Family caregivers of people with dementia. Dialogues Clin Neurosci 2009, 11(2), 217–28. [Google Scholar] [CrossRef] [PubMed]
- Macchi, ZA; Koljack, CE; Miyasaki, JM; Katz, M; Galifianakis, N; Prizer, LP; et al. Patient and caregiver characteristics associated with caregiver burden in Parkinson’s disease: a palliative care approach. Ann Palliat Med. 2020, 9 Suppl 1, S24–33. [Google Scholar] [CrossRef]
- Mekhuri, S; Dale, C; Buchanan, F; Hammash, N; Ambreen, M; Saha, S; et al. Family Caregivers of Individuals With Neuromuscular Disease Participating in a Randomized Controlled Trial of a Digital Peer Support Program: Nested Qualitative Study. J Med Internet Res. 2025, 27, e72141–e72141. [Google Scholar] [CrossRef]
- Mourão, CML; Fernandes, AFC; Moreira, DP; Martins, MC. Motivational interviewing in the social support of caregivers of patients with breast cancer in chemotherapy. Rev Esc Enferm USP 2017, 51, e03268. [Google Scholar] [PubMed]
- Alfakhri, AS; Alshudukhi, AW; Alqahtani, AA; Alhumaid, AM; Alhathlol, OA; Almojali, AI; et al. Depression Among Caregivers of Patients With Dementia. Inquiry 2018, 55, 46958017750432. [Google Scholar] [CrossRef] [PubMed]
- Donzuso, G; Brunelli, P; Milesi, G; Mancini, S; Martillotti, F; Cicero, CE; et al. Caregiver burden in Parkinson’s disease: a nationwide observational survey. Neurol Sci. 2025, 46(10), 5093–103. [Google Scholar] [CrossRef]
- Middleton, JW; Simpson, GK; De Wolf, A; Quirk, R; Descallar, J; Cameron, ID. Psychological Distress, Quality of Life, and Burden in Caregivers During Community Reintegration After Spinal Cord Injury. Archives of Physical Medicine and Rehabilitation [Internet] 2014, 95(7), 1312–9. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0003999314002573. [CrossRef] [PubMed]
- Zhao, S; Scholcz, A; Rouse, MA; Klar, VS; Ganse-Dumrath, A; Toniolo, S; et al. Self- versus caregiver-reported apathy across neurological disorders. Brain Communications [Internet] 2025, 7(3), fcaf235. [Google Scholar] [CrossRef]
- Suksatan, W; Tankumpuan, T; Davidson, PM. Heart Failure Caregiver Burden and Outcomes: A Systematic Review. J Prim Care Community Health [Internet] 2022, 13, 21501319221112584. [Google Scholar] [CrossRef]
- del-Pino-Casado, R; Priego-Cubero, E; López-Martínez, C; Orgeta, V. Subjective caregiver burden and anxiety in informal caregivers: A systematic review and meta-analysis. PLoS ONE [Internet] 2021, 16(3), e0247143. [Google Scholar] [CrossRef]
- Meurer, KJ; Presciutti, AM; Bannon, SM; Kubota, R; Baskaran, N; Kim, J; et al. Characterizing Stressors and Coping Strategies Among Caregivers of Patients with Severe Acute Brain Injury by Level of Distress. Neurocrit Care [Internet]. 2025 June 6 [cited 2025 Dec 15]. [CrossRef]
- Bártolo, A; Sousa, H; Ribeiro, O; Figueiredo, D. Effectiveness of psychosocial interventions on the burden and quality of life of informal caregivers of hemodialysis patients: a systematic review. Disability and Rehabilitation [Internet] 2022, 44(26), 8176–87. [Google Scholar] [CrossRef]
- Ransmayr, G. Challenges of caregiving to neurological patients. Wien Med Wochenschr [Internet] 2021, 171(11–12), 282–8. [Google Scholar] [CrossRef]
- Pugh, JD; McCoy, K; Williams, AM; Pienaar, CA; Bentley, B; Monterosso, L. Neurological patient and informal caregiver quality of life, and caregiver burden: A cross-sectional study of postdischarge community neurological nursing recipients. Contemporary Nurse [Internet] 2022, 58(2–3), 138–52. [Google Scholar] [CrossRef] [PubMed]
- Rokach, A; Findler, L; Chin, J; Lev, S; Kollender, Y. Cancer patients, their caregivers and coping with loneliness. Psychology, Health & Medicine [Internet] 2013, 18(2), 135–44. [Google Scholar] [CrossRef]
- Tabata-Kelly, M; Ruan, M; Dey, T; Sheu, C; Kerr, E; Kaafarani, H; et al. Postdischarge Caregiver Burden Among Family Caregivers of Older Trauma Patients. JAMA Surg [Internet] 2023, 158(9), 945. Available online: https://jamanetwork.com/journals/jamasurgery/fullarticle/2806773. [CrossRef] [PubMed]
- D’Onofrio, G; Sancarlo, D; Addante, F; Ciccone, F; Cascavilla, L; Paris, F; et al. Caregiver burden characterization in patients with Alzheimer’s disease or vascular dementia. Int J Geriat Psychiatry [Internet] 2015, 30(9), 891–9. [Google Scholar] [CrossRef]
- Hunt, CK. Concepts in Caregiver Research. J Nursing Scholarship [Internet] 2003, 35(1), 27–32. [Google Scholar] [CrossRef]
| Variable | Category | N | % |
| Gender | female | 89 | 86.4% |
| male | 14 | 13.6% | |
| Age (years) | 18–35 | 28 | 27.2% |
| 36–45 | 17 | 16.5% | |
| 46–55 | 39 | 37.9% | |
| ≥ 56 | 19 | 18.4% | |
| Marital status | single | 24 | 23.3% |
| married | 73 | 70.9% | |
| informal partnership | 1 | 1.0% | |
| widowed | 3 | 2.9% | |
| divorced | 2 | 1.9% | |
| Place of residence | rural | 68 | 66.0% |
| urban | 35 | 34.0% | |
| Education | primary | 0 | 0.0% |
| vocational | 8 | 7.8% | |
| secondary | 39 | 37.9% | |
| higher (tertiary) | 56 | 54.4% | |
| Main source of income | paid employment | 89 | 86.4% |
| old-age pension | 6 | 5.8% | |
| disability benefit | 1 | 1.0% | |
| financially dependent on family | 7 | 6.8% |
| Variable | N | % | |
| Age (years) | ≤ 60 | 24 | 23.3% |
| 61–70 | 23 | 22.3% | |
| 71–80 | 28 | 27.2% | |
| ≥ 81 | 28 | 27.2% | |
| Functional status | Fully dependent on others | 39 | 37.9% |
| Partially dependent on others | 36 | 35.0% | |
| Requires minimal assistance with self-care | 28 | 27.2% | |
| Primary diagnosis | Stroke (post-stroke condition) | 39 | 37.9% |
| Epilepsy | 5 | 4.9% | |
| Dementia | 34 | 33.0% | |
| Parkinson’s disease | 8 | 7.8% | |
| Meningitis | 1 | 1.0% | |
| Multiple sclerosis | 6 | 5.8% | |
| Amyotrophic lateral sclerosis | 1 | 1.0% | |
| Spina bifida | 1 | 1.0% | |
| Spinal muscular atrophy | 1 | 1.0% | |
| Huntington’s disease | 1 | 1.0% | |
| other | 6 | 5.8% |
| Statistic | Currently provided emotional social support (0–27 points) | Currently provided instrumental social support (0–9 points) | Currently provided informational social support (0–6 points) | Satisfaction with currently received social support (0–3 points) |
Buffering (protective) support (0–18) |
| Mean | 21.44 | 7.26 | 4.19 | 1.99 | 12.42 |
| Median | 22.00 | 8.00 | 4.00 | 2.00 | 13.00 |
| SD | 4.68 | 1.79 | 1.58 | 0.88 | 3.87 |
| Minimum | 10.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| Maximum | 27.00 | 9.00 | 6.00 | 3.00 | 18.00 |
| Variable | Gender | p | ||||
| Women | Men | |||||
| N | % | N | % | |||
| Currently provided emotional social support | low | 0 | 0.0% | 0 | 0.0% | χ2=7.738; p = 0.0054 |
| moderate | 24 | 72.7% | 9 | 27.3% | ||
| high | 65 | 92.9% | 5 | 7.1% | ||
| Currently provided instrumental social support | low | 3 | 75.0% | 1 | 25.0% | χ2 = 7.175; p = 0.0277 |
| moderate | 22 | 73.3% | 8 | 26.7% | ||
| high | 64 | 92.8% | 5 | 7.2% | ||
| Currently provided informational social support | low | 14 | 77.8% | 4 | 22.2% | χ2 = 1.452; p = 0.484 |
| moderate | 34 | 87.2% | 5 | 12.8% | ||
| high | 41 | 89.1% | 5 | 10.9% | ||
| Satisfaction with currently received social support | low | 21 | 80.8% | 5 | 19.2% | χ2 = 0.972; p = 0.615 |
| moderate | 40 | 88.9% | 5 | 11.1% | ||
| high | 28 | 87.5% | 4 | 12.5% | ||
| Buffering (protective) support | low | 3 | 75.0% | 1 | 25.0% | χ2 = 0.981; p = 0.6122 |
| moderate | 37 | 84.1% | 7 | 15.9% | ||
| high | 49 | 89.1% | 6 | 10.9% | ||
| Variable | Age | p | ||||
| ≤45 years | > 45 years | |||||
| N | % | N | % | |||
| Currently provided emotional social support | low | 0 | 0.0% | 0 | 0.0% | χ2 = 2.117; p = 0.1457 |
| moderate | 11 | 33.3% | 22 | 66.7% | ||
| high | 34 | 48.6% | 36 | 51.4% | ||
| Currently provided instrumental social support | low | 2 | 50.0% | 2 | 50.0% | χ2 = 0.274; p = 0.8721 |
| moderate | 12 | 40.0% | 18 | 60.0% | ||
| high | 31 | 44.9% | 38 | 55.1% | ||
| Currently provided informational social support | low | 7 | 38.9% | 11 | 61.1% | χ2 = 0.266; p = 0.8756 |
| moderate | 18 | 46.2% | 21 | 53.8% | ||
| high | 20 | 43.5% | 26 | 56.5% | ||
| Satisfaction with currently received social support | low | 9 | 34.6% | 17 | 65.4% | χ2 = 1.399; p = 0.4969 |
| moderate | 20 | 44.4% | 25 | 55.6% | ||
| high | 16 | 50.0% | 16 | 50.0% | ||
| Buffering (protective) support | low | 3 | 75.0% | 1 | 25.0% | χ2 = 6.388; p = 0.041 |
| moderate | 24 | 54.5% | 20 | 45.5% | ||
| high | 18 | 32.7% | 37 | 67.3% | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




