Submitted:
10 October 2025
Posted:
15 October 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
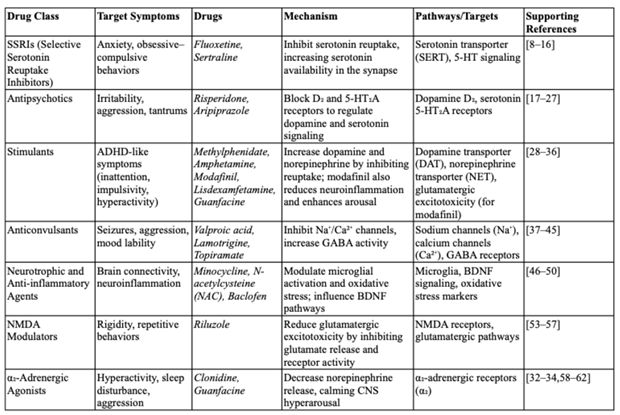 |
2. SSRIs and Serotonergic Modulation
2.1. Mechanistic Rationale
2.2. Clinical Evidence
2.3. Preclinical Insights
2.4. Other SSRIs
2.5. Clinical Considerations
3. Antipsychotics
3.1. Historical Context
3.2. Risperidone and Aripiprazole
3.3. Other Atypical Antipsychotics
3.4. Safety Considerations
3.5. Guideline Recommendations
4. Stimulants
4.1. Methylphenidate and Other Stimulants
4.2. α2-Adrenergic Agonists (Clonidine, Guanfacine)
4.3. Modafinil and Novel Approaches
5. Anticonvulsants
5.1. Epilepsy and ASD
5.2. Valproate
5.3. Lamotrigine
5.4. Levetiracetam
5.5. Topiramate and Other Antiseizure Drugs
6. Neurotrophic, Oxidative Stress, and Immune-Modulating Agents
6.1. N-Acetylcysteine (NAC)
6.2. Minocycline
6.3. Brain-Derived Neurotrophic Factor (BDNF) and Oxidative Stress
6.4. Immune and Inflammatory Mechanisms
7. Glutamatergic Agents and NMDA Modulators
7.1. Mechanistic Rationale
7.2. Riluzole
7.3. Ketamine and NMDA Antagonists
7.4. Broader NMDA-Targeting Strategies
8. Adrenergic Agents (Clonidine and Guanfacine)
8.1. Mechanistic Rationale
8.2. Clonidine
8.3. Guanfacine
8.4. Clinical Considerations
9. Discussion and Future Directions
9.1. Mechanistic Insights
9.2. Safety and Long-Term Outcomes
9.3. Guidelines and Consensus
9.4. Emerging and Preventive Approaches
9.5. Future Research Priorities
- Large, well-controlled trials of promising novel agents (e.g., NAC, riluzole, ketamine).
- Longitudinal safety studies, particularly for antipsychotics and stimulants used in children.
- Preventive strategies that target maternal immune activation and early neurodevelopmental pathways [52].
- Combination therapies that integrate behavioral interventions, psychopharmacology, and family support, reflecting the multifaceted nature of ASD.
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Maenner MJ, Shaw KA, Baio J, et al. Prevalence of Autism Spectrum Disorder Among Children Aged 8 Years — Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2016. MMWR Surveill Summ 2020, 69, 1–12. [Google Scholar] [CrossRef]
- Jobski K, Höfer J, Hoffmann F, Bachmann C. Use of psychotropic drugs in patients with ASD: A systematic review. Acta Psychiatr. Scand. 2017, 135, 8–28. [Google Scholar] [CrossRef] [PubMed]
- Coleman DM, Adams JB, Anderson AL, Frye RE. Rating of the effectiveness of 26 psychiatric and seizure medications for autism spectrum disorder: Results of a national survey. J. Child Adolesc. Psychopharmacol. 2019, 29, 107–123. [Google Scholar] [CrossRef]
- Deb S, Akrout Brizard B, Limbu B. Association between epilepsy and challenging behaviour in adults with intellectual disabilities: Systematic review and meta-analysis. BJPsych Open 2020, 6, e114. [Google Scholar] [CrossRef]
- Vasa RA, Carroll LM, Nozzolillo AA, Mahajan R, Mazurek MO, Bennett AE, et al. Systematic review of treatments for anxiety in youth with ASD. J. Autism Dev. Disord. 2014, 44, 3215–3229. [Google Scholar] [CrossRef]
- Deb S, Kwok H, Bertelli M, Salvador-Carulla L, Bradley E, Torr J, et al. International guide to prescribing psychotropic medication for the management of problem behaviours in adults with intellectual disabilities. World Psychiatry 2009, 8, 181–186. [Google Scholar] [CrossRef]
- Vohra R, Madhavan S, Sambamoorthi U, St Peter C. Access to services, quality of care, and family impact for children with autism, other developmental disabilities, and other mental health conditions. Autism 2014, 18, 815–826. [Google Scholar] [CrossRef]
- Chugani, D. Role of altered brain serotonin mechanisms in autism. Mol Psychiatry 2002, 7 (Suppl. S2), S16–S17. [Google Scholar] [CrossRef]
- Muller CL, Anacker AM, Veenstra-VanderWeele J. The serotonin system in autism spectrum disorder: From biomarker to animal models. Neuroscience 2016, 321, 24–41. [Google Scholar] [CrossRef]
- Williams K, Brignell A, Randall M, Silove N, Hazell P. Selective serotonin reuptake inhibitors (SSRIs) for autism spectrum disorders (ASD). Cochrane Database Syst. Rev. 2013, 8, CD004677. [Google Scholar] [CrossRef]
- Reddihough DS, Marraffa C, Mouti A, O’Sullivan M, Lee KJ, Orsini F, et al. Effect of fluoxetine on obsessive-compulsive behaviours in children and adolescents with ASD: A randomized clinical trial. JAMA 2019, 322, 1561–1569. [Google Scholar] [CrossRef] [PubMed]
- Wood, J.J. , Drahota, A., Sze, K., Har, K., Chiu, A. and Langer, D.A.Cognitive behavioral therapy for anxiety in children with autism spectrum disorders: a randomized, controlled trial. Journal of Child Psychology and Psychiatry 2009, 50, 224–234. [Google Scholar] [CrossRef] [PubMed]
- Golub MS, Hogrefe CE, Bulleri AM. Peer social interaction is facilitated in juvenile rhesus monkeys treated with fluoxetine. Neuropharmacology 2016, 105, 553–560. [Google Scholar] [CrossRef] [PubMed]
- He Y, Hogrefe C, Grapov D, et al. Identifying individual differences of fluoxetine response in juvenile rhesus monkeys by metabolite profiling. Transl. Psychiatry 2014, 4, e478. [Google Scholar] [CrossRef]
- King BH, Hollander E, Sikich L, McCracken JT, Scahill L, Bregman JD, et al. Lack of efficacy of citalopram in children with autism spectrum disorders and high levels of repetitive behavior: Citalopram ineffective in children with autism. Arch. Gen. Psychiatry 2009, 66, 583–590. [Google Scholar] [CrossRef]
- Potter LA, Scholze DA, Biag HMB, Schneider A, Chen Y, Nguyen DV, Rajaratnam A, Rivera SM, Dwyer PS, Tassone F, Al Olaby RR, Choudhary NS, Salcedo-Arellano MJ, Hagerman RJ. A randomized controlled trial of sertraline in young children with autism spectrum disorder. Front Psychiatry 2019, 10, 810. [Google Scholar] [CrossRef]
- Anderson LT, Campbell M, Grega DM, Perry R, Small AM, Green WH. Haloperidol in the treatment of infantile autism: Effects on learning and behavioral symptoms. Am. J. Psychiatry 1984, 141, 1195–1202. [Google Scholar] [CrossRef]
- McDougle CJ, Scahill L, McCracken JT, Aman MG, Tierney E, Arnold LE, et al. Risperidone for the core symptom domains of autism: Results from the RUPP Autism Network. Am. J. Psychiatry 2005, 162, 1142–1148. [Google Scholar] [CrossRef]
- Marcus RN, Owen R, Kamen L, Manos G, McQuade RD, Carson WH, et al. A placebo-controlled, fixed-dose study of aripiprazole in children and adolescents with irritability associated with autistic disorder. J. Am. Acad. Child Adolesc. Psychiatry 2009, 48, 1110–1119. [Google Scholar] [CrossRef]
- D’Alò GL, De Crescenzo F, Amato L, Cruciani F, Davoli M, Fulceri F, et al. Impact of antipsychotics in children and adolescents with ASD: A systematic review and meta-analysis. Health Qual. Life Outcomes 2021, 19, 33. [Google Scholar] [CrossRef]
- Fung LK, Mahajan R, Nozzolillo A, Bernal P, Krasner A, Jo B, et al. Pharmacologic treatment of severe irritability and problem behaviors in autism: A systematic review and meta-analysis. Pediatrics 2016, 137 (Suppl. S2), S124–S135. [CrossRef]
- Stavrakaki C, Antochi R, Emery PC. Olanzapine in the treatment of pervasive developmental disorders: A case series analysis. J Psychiatry Neurosci. 2004, 29, 57–60. [Google Scholar] [CrossRef]
- Golubchik P, Sever J, Weizman A. Low-dose quetiapine for adolescents with ASD and aggressive behavior: Open-label trial. Clin. Neuropharmacol. 2011, 34, 216–219. [Google Scholar] [CrossRef]
- Dominick K, Wink LK, McDougle CJ, Erickson CA. A retrospective naturalistic study of ziprasidone for irritability in youth with ASD. J. Child Adolesc. Psychopharmacol. 2015, 25, 397–401. [Google Scholar] [CrossRef]
- Stigler KA, Mullett JE, Erickson CA, Posey DJ, McDougle CJ. Paliperidone for irritability in adolescents and young adults with autistic disorder. Psychopharmacology 2012, 223, 237–245. [Google Scholar] [CrossRef]
- da Rosa ALST, Bezerra OS, Rohde LA, Graeff-Martins AS. Exploring clozapine use in severe psychiatric symptoms associated with autism spectrum disorder: A scoping review. J. Psychopharmacol. 2024, 38, 324–343. [Google Scholar] [CrossRef]
- Deb S, Kwok H, Bertelli M, Salvador-Carulla L, Bradley E, Torr J, et al. International guide to prescribing psychotropic medication for the management of problem behaviours in adults with intellectual disabilities. World Psychiatry 2009, 8, 181–186. [Google Scholar] [CrossRef]
- Handen BL, Johnson CR, Lubetsky M, Sacco K. Efficacy of methylphenidate among children with autism and symptoms of attention-deficit hyperactivity disorder. J. Autism Dev. Disord. 2000, 30, 245–255. [Google Scholar] [CrossRef]
- Sturman N, Deckx L, van Driel ML. Methylphenidate for children and adolescents with autism spectrum disorder. Cochrane Database Syst. Rev. 2017, 11, CD011144. [Google Scholar] [CrossRef]
- Del Sol Calderon, P. , Izquierdo de la Puente, A., García Moreno, M., & Fernández Fernandez, R. Lisdexamfetamine in combination with guanfacine as an effective treatment in the management of behavioral disturbances in patients with Attention Deficit Hyperactivity Disorder (ADHD) and Autism Spectrum Disorder (ASD). Case report. European Psychiatry. [CrossRef]
- Faraone, SV. The pharmacology of amphetamine and methylphenidate: Relevance to the neurobiology of attention-deficit/hyperactivity disorder and other psychiatric comorbidities. Neurosci Biobehav Rev. 2018, 87, 255–270. [Google Scholar] [CrossRef]
- Scahill L, Aman MG, McDougle CJ, Arnold LE, McCracken JT, Tierney E, et al. A prospective open trial of guanfacine in children with pervasive developmental disorders. J. Child Adolesc. Psychopharmacol. 2006, 16, 589–598. [Google Scholar] [CrossRef]
- Jaselskis, C. A. , Cook, E. H., Jr, Fletcher, K. E., & Leventhal, B. L. Clonidine treatment of hyperactive and impulsive children with autistic disorder. Journal of clinical psychopharmacology 1992, 12, 322–327. [Google Scholar] [PubMed]
- Banas K, Sawchuk B. Clonidine as a treatment of behavioural disturbances in autism spectrum disorder: A systematic literature review. J. Can. Acad. Child Adolesc. Psychiatry 2020, 29, 110–120. [Google Scholar]
- Bagcioglu, E. , Solmaz, V., Erbas, O., Özkul, B., Çakar, B., Uyanikgil, Y., & Söğüt, İ. Modafinil Improves Autism-like Behavior in Rats by Reducing Neuroinflammation. Journal of neuroimmune pharmacology : the official journal of the Society on NeuroImmune Pharmacology 2023, 18, 9–23. [Google Scholar] [CrossRef] [PubMed]
- Gerrard, P. , & Malcolm, R. Mechanisms of modafinil: A review of current research. Neuropsychiatric Disease and Treatment 2007, 3, 349–364. [Google Scholar] [CrossRef] [PubMed]
- Tuchman, R. , & Rapin, I. Epilepsy in autism. The Lancet. Neurology 2002, 1, 352–358. [Google Scholar] [CrossRef]
- Chomiak T, Turner N, Hu B. What we have learned about autism spectrum disorder from valproic acid. Pathol. Res. Int. 2013, 2013, 712758. [Google Scholar] [CrossRef]
- Hollander E, Soorya L, Wasserman S, Esposito K, Chaplin W, Anagnostou E. Divalproex sodium vs placebo in the treatment of repetitive behaviours in autism spectrum disorder. Int. J. Neuropsychopharmacol. 2006, 9, 209–213. [Google Scholar] [CrossRef]
- Belsito KM, Law PA, Kirk KS, Landa RJ, Zimmerman AW. Lamotrigine therapy for autistic disorder: A randomized, double-blind, placebo-controlled trial. J. Autism Dev. Disord. 2001, 31, 175–181. [Google Scholar] [CrossRef]
- Deriaz N, Willi JP, Orihuela-Flores M, Galli Carminati G, Ratib O. Treatment with levetiracetam in a patient with pervasive developmental disorders, severe intellectual disability, self-injurious behavior, and seizures: A case report. Neurocase 2012, 18, 386–391. [Google Scholar] [CrossRef]
- Farooq MU, Bhatt A, Majid A, Gupta R, Khasnis A, Kassab MY. Levetiracetam for managing neurologic and psychiatric disorders. Am. J. Health Syst. Pharm. 2009, 66, 541–561. [Google Scholar] [CrossRef]
- Halma, E. , de Louw, A. J., Klinkenberg, S., Aldenkamp, A. P., IJff, D. M., & Majoie, M. Behavioral side-effects of levetiracetam in children with epilepsy: a systematic review. Seizure 2014, 23, 685–691. [Google Scholar] [CrossRef] [PubMed]
- Rezaei V, Mohammadi MR, Ghanizadeh A, Sahraian A, Tabrizi M, Karami R, et al. Double-blind, placebo-controlled trial of risperidone plus topiramate in children with autistic disorder. Prog. Neuropsychopharmacol. Biol. Psychiatry 2010, 34, 1269–1272. [Google Scholar] [CrossRef] [PubMed]
- Frye RE, Rossignol D, Casanova MF, Brown GL, Martin V, Edelson S, et al. A review of traditional and novel treatments for seizures in autism spectrum disorder: Findings from a systematic review and expert panel. Front. Public Health 2013, 1, 31. [Google Scholar] [CrossRef]
- Hardan AY, Fung LK, Libove RA, Obukhanych TV, Nair S, Herzenberg LA, et al. A randomized controlled pilot trial of oral N-acetylcysteine in children with autism. Biol. Psychiatry 2012, 71, 956–961. [Google Scholar] [CrossRef]
- Ghanizadeh A, Derakhshan N. N-acetylcysteine for treatment of autism, a case report. J. Res. Med. Sci. 2012, 17, 985–987. [Google Scholar]
- Ghaleh A, Alikhani R, Kazemi MR, Mohammadi MR, Mohammadinejad P, Zeinoddini A, et al. Minocycline as adjunctive treatment to risperidone in children with autistic disorder: A randomized, double-blind placebo-controlled trial. J. Child Adolesc. Psychopharmacol. 2016, 26, 827–832. [Google Scholar] [CrossRef]
- Zheng Z, Zhang L, Zhu T, Huang J, Qu Y, Mu D. Peripheral brain-derived neurotrophic factor in autism spectrum disorder: a systematic review and meta-analysis. Sci Rep. 2016, 6, 31241. [Google Scholar] [CrossRef]
- Chauhan A, Chauhan V. Oxidative stress in autism. Pathophysiology 2006, 13, 171–181. [Google Scholar] [CrossRef]
- Asadabadi M, Mohammadi MR, Ghanizadeh A, et al. Celecoxib as adjunctive treatment to risperidone in children with autistic disorder: A randomized, double-blind, placebo-controlled trial. Psychopharmacology 2013, 225, 51–59. [Google Scholar] [CrossRef]
- Bolandparvaz A, Harriman R, Alvarez K, Lilova K, Zang Z, Lam A, Edmiston E, Navrotsky A, Vapniarsky N, Van De Water J, Lewis JS. Towards a nanoparticle-based prophylactic for maternal autoantibody-related autism. Nanomedicine: Nanotechnology, Biology and Medicine. 2019, 21, 102067. [Google Scholar] [CrossRef]
- Uzunova G, Pallanti S, Hollander E. Excitatory/inhibitory imbalance in autism spectrum disorders: Implications for interventions and therapeutics. World J. Biol. Psychiatry 2016, 17, 174–186. [Google Scholar] [CrossRef] [PubMed]
- de Boer JN, Vingerhoets C, Hirdes M, McAlonan GM, van Amelsvoort T, Zinkstok JR. Efficacy and tolerability of riluzole in psychiatric disorders: A systematic review and preliminary meta-analysis. Psychiatry Res. 2019, 278, 294–302. [Google Scholar] [CrossRef] [PubMed]
- Dessus-Gilbert ML, Nourredine M, Zimmer L, Rolland B, Geoffray MM, Auffret M, et al. NMDA antagonist agents for the treatment of symptoms in autism spectrum disorder: A systematic review and meta-analysis. Front Pharmacol. 2024, 15, 1395867. [CrossRef]
- Qin, X. Y. , Feng, J. C., Cao, C., Wu, H. T., Loh, Y. P., & Cheng, Y. Association of Peripheral Blood Levels of Brain-Derived Neurotrophic Factor With Autism Spectrum Disorder in Children: A Systematic Review and Meta-analysis. JAMA pediatrics 2016, 170, 1079–1086. [Google Scholar] [CrossRef]
- Erickson CA, Posey DJ, Stigler KA, McDougle CJ. A retrospective study of memantine in children and adolescents with pervasive developmental disorders. Psychopharmacology 2007, 191, 141–147. [Google Scholar] [CrossRef]
- Scahill L, McCracken JT, King BH, Rockhill C, Shah B, Politte L, et al. Extended-release guanfacine for hyperactivity in children with autism spectrum disorder. Am. J. Psychiatry 2015, 172, 1197–1206. [Google Scholar] [CrossRef]
- Ming, X. , Gordon, E., Kang, N., & Wagner, G. C. Use of clonidine in children with autism spectrum disorders. Brain & development 2008, 30, 454–460. [Google Scholar] [CrossRef]
- Banas K, Sawchuk B. Clonidine as a treatment of behavioural disturbances in autism spectrum disorder: A systematic literature review. J. Can. Acad. Child Adolesc. Psychiatry 2020, 29, 110–120. [Google Scholar]
- Charman, T. Mapping Early Symptom Trajectories in Autism Spectrum Disorder: Lessons and Challenges for Clinical Practice and Science. Journal of the American Academy of Child and Adolescent Psychiatry 2018, 57, 820–821. [Google Scholar] [CrossRef]
- Posey DJ, Puntney JI, Sasher TM, Kem DL, Swiezy NB, McDougle CJ. Guanfacine treatment of hyperactivity and inattention in pervasive developmental disorders: A retrospective analysis of 80 cases. J. Child Adolesc. Psychopharmacol. 2004, 14, 233–241. [Google Scholar] [CrossRef]
- Ecker C, Bookheimer SY, Murphy DG. Neuroimaging in autism spectrum disorder: Brain structure and function across the lifespan. Lancet Neurol. 2015, 14, 1121–1134. [Google Scholar] [CrossRef] [PubMed]
- Courchesne E, Campbell K, Solso S. Brain growth across the life span in autism: Age-specific changes in anatomical pathology. Brain Res. 2011, 1380, 138–145. [Google Scholar] [CrossRef] [PubMed]
- Loth E, Poline JB, Thyreau B, Jia T, Tao C, Lourdusamy A, et al. Oxytocin receptor genotype modulates ventral striatal activity to social cues in ASD. Transl. Psychiatry 2014, 4, e480. [Google Scholar] [CrossRef]
- Zhang HF, Dai YY, Zhong JY, Hu CJ, Bai ZZ, An Y, et al. Plasma oxytocin and arginine-vasopressin levels in children with autism spectrum disorder in China: Associations with symptom severity. Neurosci. Bull. 2016, 32, 423–432. [Google Scholar] [CrossRef]
- Dorph-Petersen KA, Pierri JN, Sun Z, Sampson AR, Lewis DA. Effects of chronic exposure to antipsychotics on brain size and cell numbers in macaque monkeys. Neuropsychopharmacology 2005, 30, 1649–1661. [Google Scholar] [CrossRef]
- Mandell DS, Morales KH, Marcus SC, Stahmer AC, Doshi J, Polsky DE. Psychotropic medication use among Medicaid-enrolled children with autism spectrum disorders. Pediatrics 2008, 121, e441–e448. [Google Scholar] [CrossRef]
- Murray ML, Hsia Y, Glaser K, Simonoff E, Murphy DG, Asherson PJ, et al. Pharmacological treatments prescribed to people with autism spectrum disorder (ASD) in primary health care. Psychopharmacology 2014, 231, 1011–1021. [Google Scholar] [CrossRef]
- National Institute for Health and Care Excellence (NICE). Autism spectrum disorder in under 19s: Support and management. NICE guideline [CG170] 2013. Available online: https://www.nice.org.uk/guidance/cg170 (accessed on 2 September 2025).
- Lai, M. C. , Lombardo, M. V., & Baron-Cohen, S. Autism. Lancet 2014, 383, 896–910. [Google Scholar] [CrossRef]
- Lord C, Elsabbagh M, Baird G, Veenstra-VanderWeele J. Autism spectrum disorder. Lancet 2018, 392, 508–520. [Google Scholar] [CrossRef]
- Rose, S. , Frye, R. E., Slattery, J., Wynne, R., Tippett, M., Pavliv, O., Melnyk, S., & James, S. J. Oxidative stress induces mitochondrial dysfunction in a subset of autism lymphoblastoid cell lines in a well-matched case control cohort. PloS one 2014, 9, e85436. [Google Scholar] [CrossRef]
- Sharma SR, Gonda X, Tarazi FI. Autism spectrum disorder: Classification, diagnosis and therapy. Pharmacol. Ther. 2018, 190, 91–104. [Google Scholar] [CrossRef]
- Matta SM, Hill-Yardin EL, Crack PJ. The influence of neuroinflammation in autism spectrum disorder. Brain Behav Immun. 2019, 79, 75–90. [CrossRef]
- Kolevzon A, Gross R, Reichenberg A. Prenatal and perinatal risk factors for autism: A review and integration of findings. Arch. Pediatr. Adolesc. Med. 2007, 161, 326–333. [Google Scholar] [CrossRef]
- Sandin S, Lichtenstein P, Kuja-Halkola R, Larsson H, Hultman CM, Reichenberg A. The familial risk of autism. JAMA 2014, 311, 1770–1777. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




