Submitted:
04 October 2025
Posted:
06 October 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Patient Population
2.3. Surgical Technique
- Billroth I surgical procedure involved gastroduodenostomy through end-to-end or end-to-side anastomosis between the stomach remnant and duodenum when a safe tension-free anastomosis can be achieved.
- Billroth II (gastrojejunostomy) procedure with Braun enteroenterostomy as an option based on surgeon preference for patients who needed a longer resection margin or had limited duodenal mobility.
- The Roux-en-Y procedure (gastrojejunostomy with Roux limb) serves as an antecolic Roux-en-Y gastro-jejunostomy with standardized limb length for patients who need an alternative method to minimize bile reflux and achieve secure tension-free reconstruction.
2.4. Data Collection and Variables
2.5. Outcome Measures
2.6. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Short-Term Surgical Outcomes
3.3. Mid-Term Functional Outcomes
3.3. Postoperative Complications
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ASA— | American Society of Anesthesiologists |
| BI— | Billroth I |
| BII/RY— | Billroth II/Roux-en-Y |
| BMI— | Body Mass Index |
| BRG— | Bile Reflux Gastritis |
| CI— | Confidence Interval |
| CONUT— | Controlling Nutritional Status |
| CRP— | C-Reactive Protein |
| IPTW— | Inverse Probability of Treatment Weighting |
| IQR— | Interquartile Range |
| JGCA— | Japanese Gastric Cancer Association |
| LOS— | Length of Stay |
| OR— | Odds Ratio |
| PPI— | Proton Pump Inhibitor |
| QoL— | Quality of Life |
| RCT— | Randomized Controlled Trial |
| SD— | Standard Deviation |
| SMD— | Standardized Mean Difference |
References
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [CrossRef]
- Japanese Gastric Cancer Association. Japanese Gastric Cancer Treatment Guidelines 2021 (6th edition). Gastric Cancer 2023, 26, 1–25. [CrossRef]
- National Comprehensive Cancer Network. Gastric Cancer (Version 2.2025). NCCN Clinical Practice Guidelines in Oncology. Available online: https://www.nccn.org/professionals/physician_gls/pdf/gastric.pdf (accessed on 9 September 2025).
- Digklia, A.; Wagner, A.D. Advanced Gastric Cancer: Current Treatment Landscape and Future Perspectives. World J. Gastroenterol. 2016, 22, 2403–2414. [CrossRef]
- Smyth, E.C.; Nilsson, M.; Grabsch, H.I.; van Grieken, N.C.T.; Lordick, F. Gastric Cancer. Lancet 2020, 396, 635–648. [CrossRef]
- Ajani, J.A.; In, H.; Sano, T.; Gaspar, L.E.; Hart, L.; Almhanna, K.; Bang, Y.J.; Benson, A.; Das, P.; Fuchs, C.S.; et al. Gastric Cancer, Version 3.2016, NCCN Clinical Practice Guidelines in Oncology. J. Natl. Compr. Canc. Netw. 2016, 14, 1286–1312. [CrossRef]
- Van Cutsem, E.; Sagaert, X.; Topal, B.; Haustermans, K.; Prenen, H. Gastric Cancer. Lancet 2016, 388, 2654–2664. [CrossRef]
- Karimi, P.; Islami, F.; Anandasabapathy, S.; Freedman, N.D.; Kamangar, F. Gastric Cancer: Descriptive Epidemiology, Risk Factors, Screening, and Prevention. Cancer Epidemiol. Biomarkers Prev. 2014, 23, 700–713. [CrossRef]
- Strong, V.E.; Wu, A.-W.; Selby, L.V.; Gonen, M.; Hsu, M.; Song, K.Y.; Park, C.H.; Coit, D.G.; Brennan, M.F. Differences in Gastric Cancer Survival between the U.S. and China. J. Surg. Oncol. 2015, 112, 31–37. [CrossRef]
- Kang, K.-C.; Cho, G.S.; Han, S.U.; Kim, W.; Kim, H.-H.; Kim, M.-C.; Hyung, W.J.; Ryu, S.Y.; Ryu, S.W.; Lee, H.J.; Song, K.Y.; Korean Laparoscopic Gastrointestinal Surgery Study (KLASS) Group. Comparison of Billroth I and Billroth II Reconstructions after Laparoscopy-Assisted Distal Gastrectomy: A Retrospective Analysis of Large-Scale Multicenter Results from Korea. Surg. Endosc. 2011, 25, 1953–1961. [CrossRef]
- Oh, J.; Park, Y.K. Clinicopathological Features and Surgical Treatment of Gastric Cancer in South Korea: Results of 2009 Nationwide Survey on Surgically Treated Gastric Cancer Patients. J. Gastric Cancer 2011, 11, 69–77. [CrossRef]
- Kim, H.H.; Hyung, W.J.; Cho, G.S.; Kim, M.C.; Han, S.U.; Kim, W.; Ryu, S.W.; Lee, H.J. Morbidity and Mortality of Laparoscopic Gastrectomy versus Open Gastrectomy for Gastric Cancer: Interim Report of a Phase III Trial (KLASS). Ann. Surg. 2010, 251, 417–420. [CrossRef]
- Zong, L.; Chen, P. Billroth I vs. Billroth II vs. Roux-en-Y Following Distal Gastrectomy: A Meta-Analysis Based on 15 Studies. Hepatogastroenterology 2011, 58, 1413–1424. [CrossRef]
- Xiong, J.J.; Altaf, K.; Javed, M.A.; Nunes, Q.M.; Huang, W.; Mai, G.; Tan, C.; Liu, X.-B. Roux-en-Y versus Billroth I Reconstruction after Distal Gastrectomy for Gastric Cancer: A Meta-Analysis. World J. Gastroenterol. 2013, 19, 1124–1134. [CrossRef]
- He, L.; Zhao, Y. Is Roux-en-Y or Billroth-II Reconstruction the Preferred Choice for Gastric Cancer Patients Undergoing Distal Gastrectomy when Billroth I is not Applicable? A Meta-Analysis. Medicine (Baltimore) 2019, 98, e17093. [CrossRef]
- Inokuchi, M.; Kojima, K.; Yamada, H.; Kato, K.; Hayashi, M.; Motoyama, K.; Sugihara, K. Long-Term Outcomes of Roux-en-Y and Billroth I Reconstruction after Laparoscopic Distal Gastrectomy. Gastric Cancer 2013, 16, 67–73. [CrossRef]
- Kinoshita, T.; Honda, M.; Matsuki, A.; Enomoto, N.; Aizawa, M.; Nunobe, S.; Yabusaki, H.; Abe, T.; Hiki, N. Billroth-I vs Roux-en-Y after Distal Gastrectomy: Comparison of Long-Term Nutritional Status and Survival in a Multicenter Study. Ann. Gastroenterol. Surg. 2020, 4, 142–150. [CrossRef]
- Kimura, Y.; Mikami, J.; Yamasaki, M.; Hirao, M.; Imamura, H.; Fujita, J.; et al. Comparison of 5-Year Postoperative Outcomes after Billroth I and Roux-en-Y Reconstruction following Distal Gastrectomy: Results from an RCT. Ann. Gastroenterol. Surg. 2021, 5, 93–101. [CrossRef]
- Nishizaki, D.; Ganeko, R.; Hoshino, N.; Hida, K.; Obama, K.; Furukawa, T.A. Roux-en-Y versus Billroth-I Reconstruction after Distal Gastrectomy for Gastric Cancer. Cochrane Database Syst. Rev. 2021, CD012998. [CrossRef]
- Chen, Y.-X.; Huang, Q.-Z.; Wang, P.-C.; Zhu, Y.-J.; Chen, L.-Q.; Wu, C.-Y.; Wang, J.-T.; Chen, J.-X.; Ye, K. Short- and Long-Term Outcomes of Roux-en-Y and Billroth II with Braun Reconstruction in Total Laparoscopic Distal Gastrectomy. World J. Surg. Oncol. 2023, 21, 361. [CrossRef]
- Min, J.S.; Kim, E.H.; Park, S.; Kim, H.I.; Hyung, W.J. Optimal Reconstruction after Distal Gastrectomy: A Systematic Review and Meta-Analysis. J. Gastric Cancer 2022, 22, e9. [CrossRef]
- Yan, Y.; Zhao, J.; Chen, X.; Zhao, G.; Zhao, Z. Optimal Reconstruction after Laparoscopic Distal Gastrectomy: A Systematic Review and Network Meta-Analysis. Surg. Innov. 2022, 29, 589–603. [CrossRef]
- Yang, K.; Zhang, W.-H.; Liu, K.; Chen, X.-Z.; Zhou, Z.-G.; Hu, J.-K. Comparison of Quality of Life between Billroth-I and Roux-en-Y Anastomosis after Distal Gastrectomy: A Randomized Controlled Trial. Sci. Rep. 2017, 7, 11245. [CrossRef]
- Nakamura, M.; Nakamori, M.; Ojima, T.; Iwahashi, M.; Horiuchi, T.; Kobayashi, Y.; et al. RCT Comparing Long-Term QoL for Billroth I versus Roux-en-Y after Distal Gastrectomy. Br. J. Surg. 2016, 103, 337–347. [CrossRef]
- Hirao, M.; Takiguchi, S.; Imamura, H.; Yamamoto, K.; Kurokawa, Y.; Fujita, J.; et al. Comparison of Billroth I and Roux-en-Y Reconstruction after Distal Gastrectomy for Gastric Cancer: One-Year Postoperative Effects (RCT). Ann. Surg. Oncol. 2013, 20, 1591–1597. [CrossRef]
- Imamura, H.; Takiguchi, S.; Yamamoto, K.; Hirao, M.; Fujita, J.; Yano, M.; et al. Morbidity and Mortality Results from an RCT Comparing Billroth I and Roux-en-Y after Distal Gastrectomy. World J. Surg. 2012, 36, 632–637. [CrossRef]
- Tran, T.B.; Worhunsky, D.J.; Squires, M.H.; Jin, L.X.; Spolverato, G.; Votanopoulos, K.I.; et al. To Roux or Not to Roux: A Comparison between Roux-en-Y and Billroth II Reconstruction following Partial Gastrectomy. Gastric Cancer 2016, 19, 994–1001. [CrossRef]
- Imai, Y.; Hata, T.; Miyake, M.; Kanno, T.; Toyama, H.; Motoi, F.; et al. Comparison of the Gastric Microbiome in Billroth I and Roux-en-Y Reconstructions after Distal Gastrectomy. Sci. Rep. 2022, 12, 10754. [CrossRef]
- Wei, T.; Wu, Z.; Chen, Y.; Li, Y.; Pang, F.; Shan, F.; Li, Z.; Ji, J. Comparison of Uncut Roux-en-Y and Billroth II with Braun Anastomosis after Distal Gastrectomy. Front. Surg. 2024, 11, 1390876. [CrossRef]
- Takiguchi, S.; Yamamoto, K.; Hirao, M.; Imamura, H.; Fujita, J.; Yano, M.; Kobayashi, K.; Kimura, Y.; Kurokawa, Y.; Mori, M.; Doki, Y. A Comparison of Postoperative Quality of Life and Dysfunction after Billroth I and Roux-en-Y Reconstruction following Distal Gastrectomy for Gastric Cancer: Results from a Multi-Institutional RCT. Gastric Cancer 2012, 15, 198–205. [CrossRef]
- Fujiya, K.; Kawamura, T.; Omae, K.; Makuuchi, R.; Irino, T.; Tokunaga, M.; Tanizawa, Y.; Bando, E.; Terashima, M. Impact of Malnutrition after Gastrectomy for Gastric Cancer on Long-Term Survival. Ann. Surg. Oncol. 2018, 25, 974–983. [CrossRef]
- Tokunaga, M.; Makuuchi, R.; Miki, Y.; Tanizawa, Y.; Bando, E.; Kawamura, T.; et al. Late Complications and Nutritional Impact of Billroth I vs Roux-en-Y. World J. Surg. 2015, 39, 1803–1810. [CrossRef]
- Maehara, Y.; Kakeji, Y.; Oda, S.; et al. Long-Term Functional Outcomes after Distal Gastrectomy with Billroth I or Roux-en-Y. Surg. Today 2012, 42, 255–260. [CrossRef]
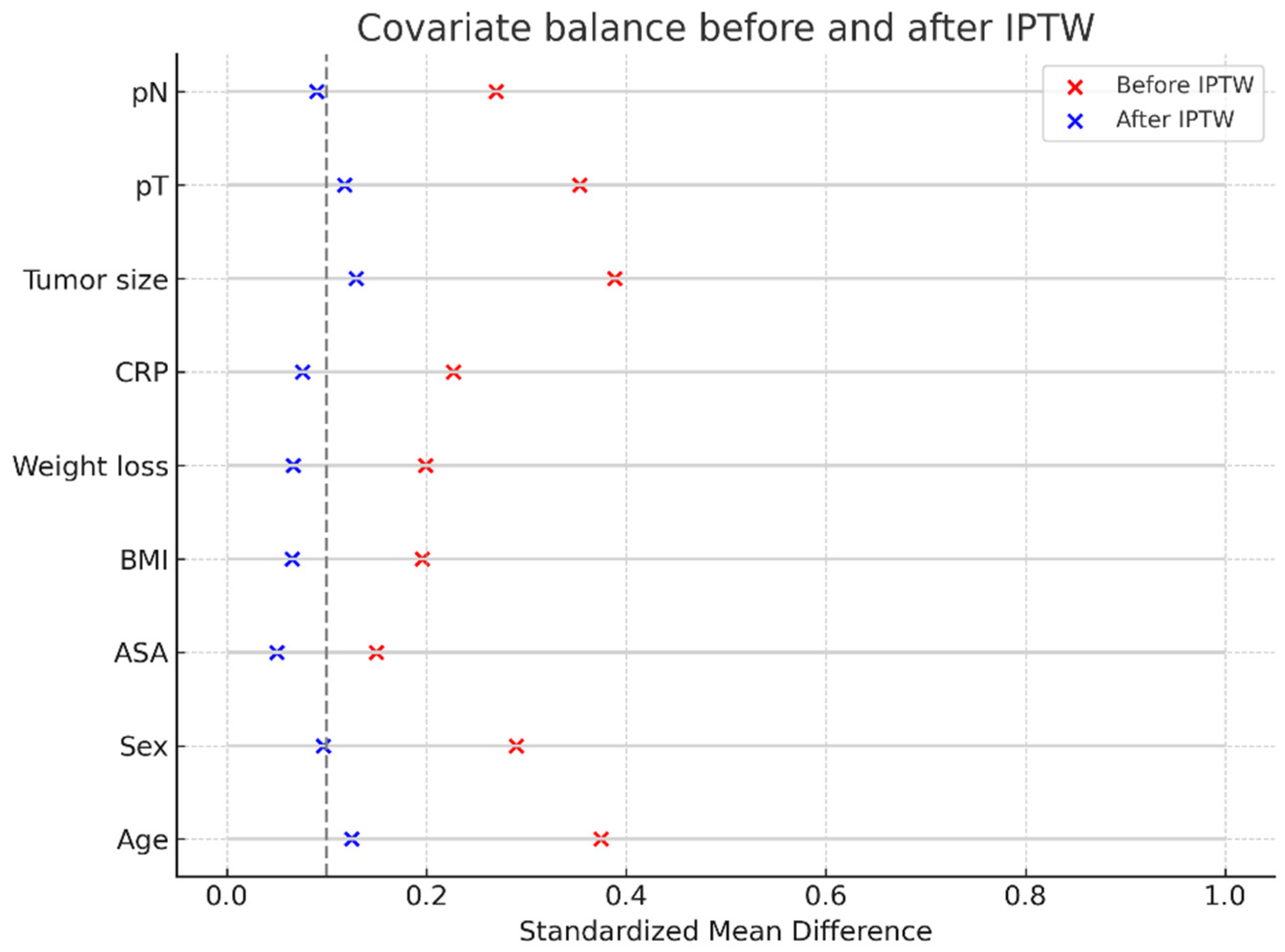
| Variable | Billroth I (n=72) | Billroth II/RY (n=78) | Total (N=150) | p-value | SMD | |
|---|---|---|---|---|---|---|
| Demographics | ||||||
| Age, years (mean ± SD; median [IQR]) | 60.4 ± 10.6; 60.0 [51.8–71.0] | 62.5 ± 11.0; 64.5 [53.0–71.0] | 61.5 ± 10.8; 61.0 [52.0–71.0] | 0.21 | 0.19 | |
| Sex, n (%) | Male 42 (58.3) Female 30 (41.7) |
Male 49 (62.8) Female 29 (37.2) |
Male 91 (60.7) Female 59 (39.3) |
0.59 | 0.09 | |
| General status | ||||||
| ASA class, n (%) | I: 9 (12.5) II: 35 (48.6) III: 19 (26.4) IV: 9 (12.5) |
I: 9 (11.5) II: 38 (48.7) III: 26 (33.3) IV: 5 (6.4) |
I: 18 (12.0) II: 73 (48.7) III: 45 (30.0) IV: 14 (9.3) |
0.54 | 0.14 | |
| BMI (kg/m2) | 23.8 ± 3.3; 24.3 [20.8–26.0] | 23.6 ± 3.6; 23.8 [20.9–25.9] | 23.7 ± 3.5; 24.1 [20.8–25.9] | 0.72 | 0.05 | |
| Weight loss 3–6 m (%) | 10.4 ± 6.1; 11.2 [5.6–16.1] | 10.2 ± 6.3; 10.8 [4.8–15.4] | 10.3 ± 6.2; 10.9 [5.6–15.7] | 0.82 | 0.03 | |
| CRP (mg/L) | 25.8 ± 19.5; 24.7 [7.9–39.2] | 22.9 ± 18.7; 20.4 [7.7–35.6] | 24.2 ± 19.1; 22.9 [7.7–37.1] | 0.34 | 0.16 | |
| Tumor characteristics | ||||||
| Tumor site, n (%) | Distal: 44 (61.1) Body: 19 (26.4) Multicentric: 9 (12.5) |
Distal: 50 (64.1) Body: 20 (25.6) Multicentric: 8 (10.3) |
Distal: 94 (62.7) Body: 39 (26.0) Multicentric: 17 (11.3) |
0.89 | 0.05 | |
| Tumor size (cm) | 5.4 ± 1.9; 5.5 [4.5–6.6] | 5.6 ± 2.2; 5.4 [4.2–7.2] | 5.5 ± 2.1; 5.4 [4.3–6.9] | 0.58 | 0.10 | |
| pT stage | T1: 12 (16.7) T2: 24 (33.3) T3: 27 (37.5) T4: 9 (12.5) |
T1: 11 (14.1) T2: 27 (34.6) T3: 28 (35.9) T4: 12 (15.4) |
T1: 23 (15.3) T2: 51 (34.0) T3: 55 (36.7) T4: 21 (14.0) |
0.91 | 0.07 | |
| pN stage | N0: 20 (27.8) N1: 22 (30.6) N2: 21 (29.2) N3: 9 (12.5) |
N0: 18 (23.1) N1: 25 (32.1) N2: 22 (28.2) N3: 13 (16.7) |
N0: 38 (25.3) N1: 47 (31.3) N2: 43 (28.7) N3: 22 (14.7) |
0.74 | 0.09 | |
| Margin status | R0: 66 (91.7) R1: 6 (8.3) |
R0: 70 (89.7) R1: 8 (10.3) |
R0: 136 (90.7) R1: 14 (9.3) |
0.69 | 0.06 | |
| Neoadjuvant therapy | Yes: 24 (33.3) No: 48 (66.7) |
Yes: 28 (35.9) No: 50 (64.1) |
Yes: 52 (34.7) No: 98 (65.3) |
0.75 | 0.05 | |
| Surgical factors | ||||||
| Lymphadenectomy (D1+/D2) | D1+: 20 (27.8) D2: 52 (72.2) |
D1+: 24 (30.8) D2: 54 (69.2) |
D1+: 44 (29.3) D2: 106 (70.7) |
0.68 | 0.07 | |
| Operative time (min) | 201 ± 38; 198 [173–224] | 205 ± 41; 201 [179–229] | 203 ± 40; 199 [176–226]] | 0.49 | 0.10 | |
| Blood loss (mL) | 289 ± 65; 286 [240–330] | 295 ± 71; 292 [246–342] | 292 ± 68; 290 [242–336] | 0.57 | 0.09 | |
| Outcome | Billroth I (n=72) | Billroth II/RY (n=78) | Total (N=150) | p-value | SMD |
|---|---|---|---|---|---|
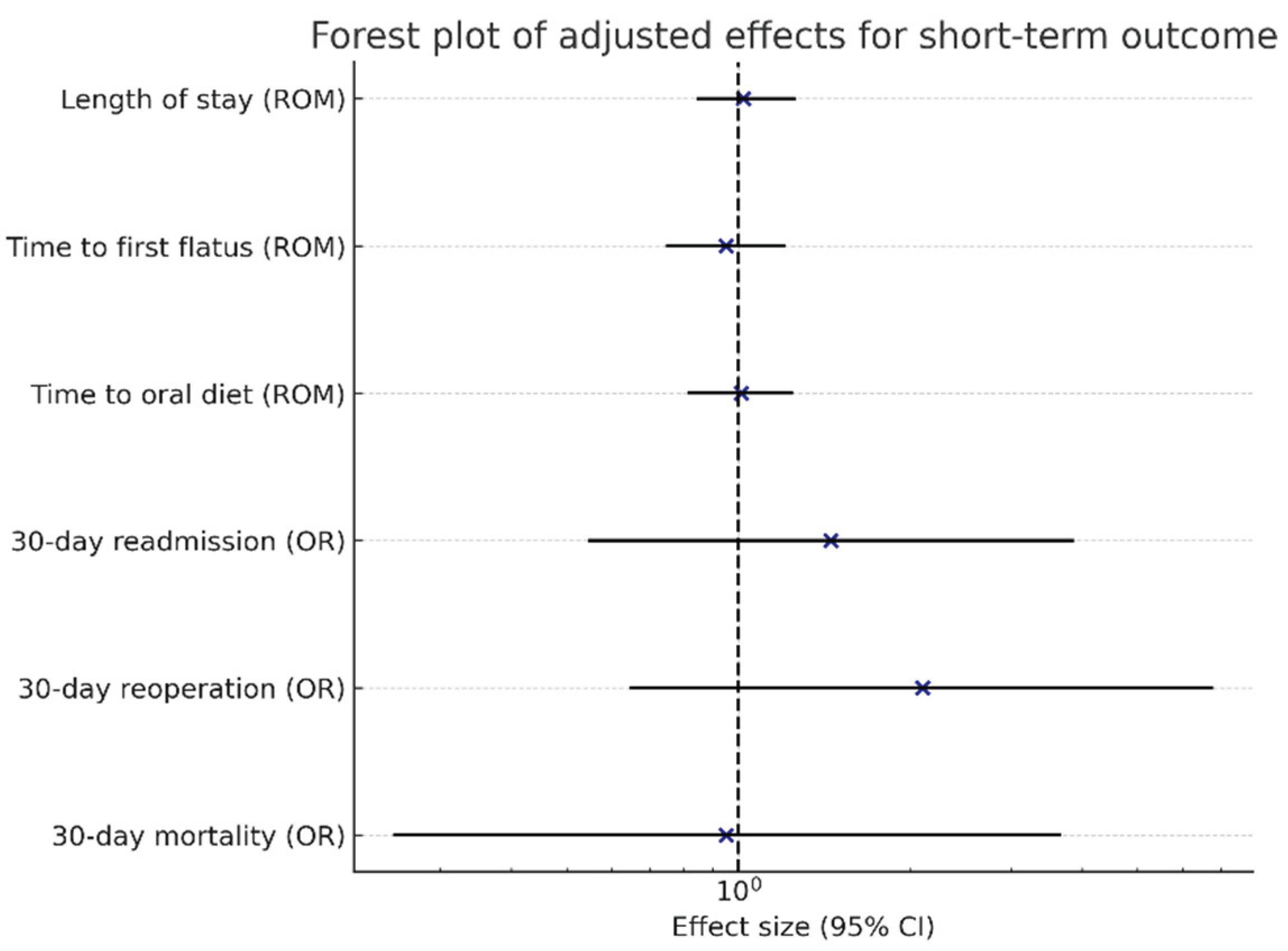
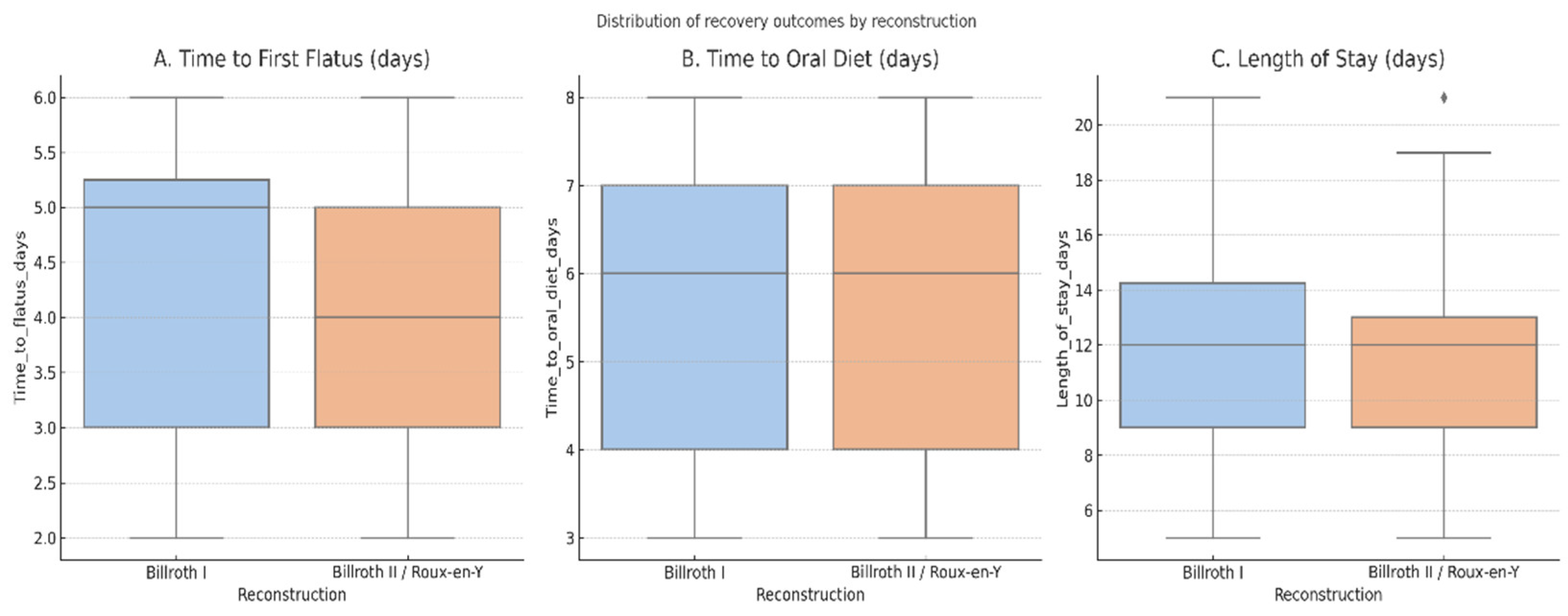
| Time to first flatus (days) | 4.3 ± 1.4; 5.0 [3.0–5.2] | 3.9 ± 1.4; 4.0 [3.0–5.0] | 4.1 ± 1.4; 4.0 [3.0–5.0] | 0.12 | 0.25 |
| Time to oral diet (days) | 5.7 ± 1.8; 6.0 [4.0–7.0] | 5.8 ± 1.7; 6.0 [4.0–7.0] | 5.7 ± 1.7; 6.0 [4.0–7.0] | 0.70 | −0.07 |
| Length of stay (days) | 11.8 ± 3.8; 12.0 [9.0–14.2] | 11.6 ± 3.4; 12.0 [9.0–13.0] | 11.7 ± 3.6; 12.0 [9.0–14.0] | 0.69 | 0.06 |
| 30-day readmission | 6 (8.3%) | 11 (14.1%) | 17 (11.3%) | 0.39 | −0.18 |
| 30-day reoperation | 2 (2.8%) | 6 (7.7%) | 8 (5.3%) | 0.33 | −0.22 |
| 30-day mortality | 3 (4.2%) | 3 (3.8%) | 6 (4.0%) | 1.00 | 0.02 |
| 90-day mortality | 4 (5.6%) | 4 (5.1%) | 8 (5.3%) | 1.00 | 0.02 |
| Any complication | 37 (51.4%) | 35 (44.9%) | 72 (48.0%) | 0.53 | 0.13 |
| Outcome | Billroth I (n=72) | Billroth II/RY (n=78) | Total (N=150) | p-value | SMD |
|---|---|---|---|---|---|
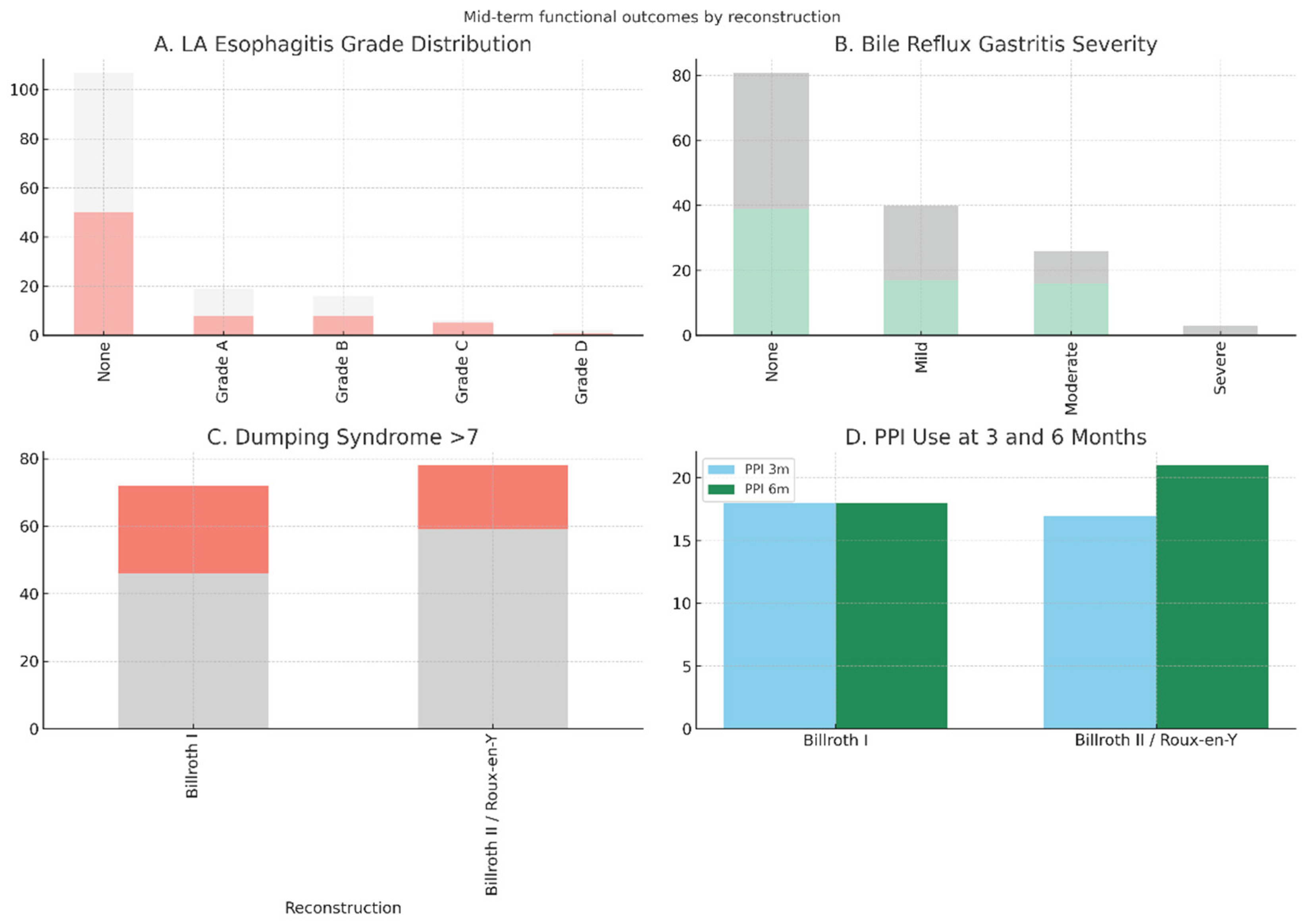
| PPI use at 3 months | 18 (25.0%) | 17 (21.8%) | 35 (23.3%) | 0.79 | 0.08 |
| PPI use at 6 months | 18 (25.0%) | 21 (26.9%) | 39 (26.0%) | 0.93 | −0.04 |
| LA esophagitis | None: 50 (69.4); A: 8 (11.1); B: 8 (11.1); C: 5 (6.9); D: 1 (1.4) | None: 57 (73.1); A: 11 (14.1); B: 8 (10.3); C: 1 (1.3); D: 1 (1.3) | - | 0.50 | – |
| Bile reflux gastritis | None: 39 (54.2); Mild: 17 (23.6); Moderate: 16 (22.2) | None: 42 (53.8); Mild: 23 (29.5); Moderate: 10 (12.8); Severe: 3 (3.8) | - | 0.16 | – |
| Dumping score (Sigstad) | 4.9 ± 4.9; 5.0 [1.6–8.8] | 4.4 ± 4.5; 4.8 [1.1–7.0] | 4.6 ± 4.7; 4.9 [1.2–7.5] | 0.40 | 0.12 |
| Dumping syndrome >7 | 26 (36.1%) | 19 (24.4%) | 45 (30.0%) | 0.16 | 0.26 |
| Complication type | Billroth I (n=72) | Billroth II/RY (n=78) | Total (N=150) | p-value |
|---|---|---|---|---|
| Anastomotic leak | 2 (2.8%) | 3 (3.8%) | 5 (3.3%) | 1.00 |
| Duodenal stump leak | – | 2 (2.6%) | 2 (1.3%) | – |
| Intra-abdominal abscess | 3 (4.2%) | 4 (5.1%) | 7 (4.7%) | 0.74 |
| Postoperative bleeding | 2 (2.8%) | 2 (2.6%) | 4 (2.7%) | 1.00 |
| Wound infection | 5 (6.9%) | 6 (7.7%) | 11 (7.3%) | 0.87 |
| Pulmonary | 6 (8.3%) | 7 (9.0%) | 13 (8.7%) | 0.88 |
| Cardiovascular | 3 (4.2%) | 4 (5.1%) | 7 (4.7%) | 0.74 |
| Venous thromboembolism | 1 (1.4%) | 1 (1.3%) | 2 (1.3%) | 1.00 |
| Stricture | 1 (1.4%) | 2 (2.6%) | 3 (2.0%) | 1.00 |
| Reoperation | 2 (2.8%) | 6 (7.7%) | 8 (5.3%) | 0.33 |
| Clavien–Dindo grade | Billroth I (n=72) | Billroth II/RY (n=78) | Total (N=150) | p-value |
|---|---|---|---|---|
| Grade 0 (no complication) | 45 (62.5%) | 44 (56.4%) | 89 (59.3%) | 0.47 |
| Grade II (minor) | 14 (19.4%) | 15 (19.2%) | 29 (19.3%) | 0.97 |
| Grade III (major) | 6 (8.3%) | 13 (16.7%) | 19 (12.7%) | 0.17 |
| Grade V (death) | 7 (9.7%) | 6 (7.7%) | 13 (8.7%) | 0.69 |
| Any complication (≥II) | 27 (37.5%) | 34 (43.6%) | 61 (40.7%) | 0.47 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




