Submitted:
26 September 2025
Posted:
30 September 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
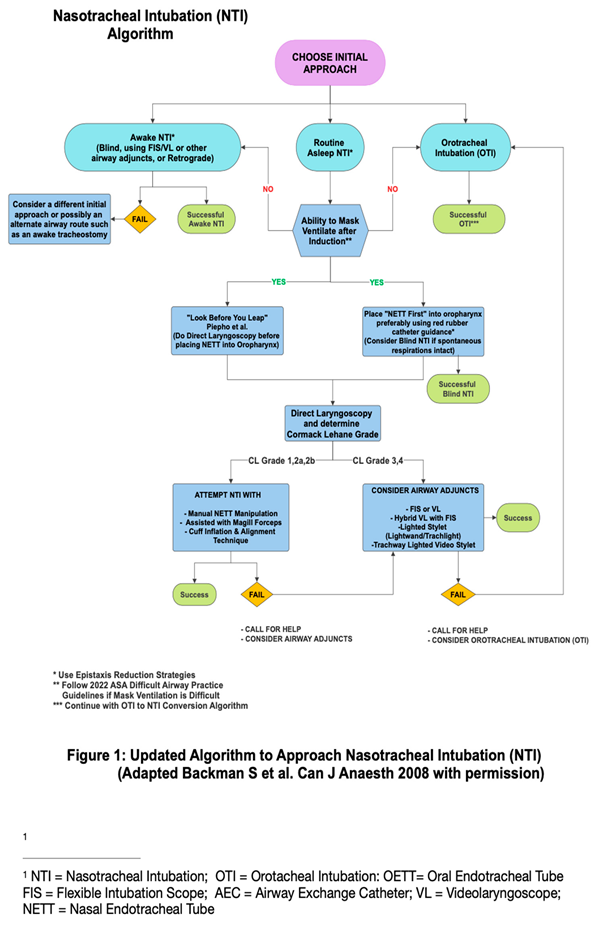
2. Choosing an Initial Nti Approach
2.1. Routine Asleep Nti (Rnti) Approach
- 1)“Look before you leap” option advocated by Piepho et al. which involves obtaining a glottic view with DL before placing the NETT into the oropharynx. Piepho et al. recommends passing the NETT through the nares only in patients with a grade 1 or 2 Cormack-Lehane (CL) view and using alternate adjunct guided techniques otherwise.[5] Lesser experienced clinicians may find this approach more reassuring.
- 2) More traditional option of placing the NETT into the oropharynx first (“NETT first”) before obtaining a glottic view with DL. The downside to this approach is the clinician may encounter a difficult 3/4 CL grade during subsequent DL, making it challenging to advance the NETT situated in the oropharynx through the glottis. Albeit rare, there is also potential for severe epistaxis with initial NETT insertion which may lead to aspiration of blood and render alternative options such as FIS assisted NTI difficult.[11] Telescoping the NETT with a red rubber catheter, amongst other epistaxis reduction measures, is strongly encouraged to reduce the possibility of severe epistaxis.[12]
2.1.1. RNTI Scenario with CL grade 1/2 view:
2.1.2. RNTI Scenario with CL grade 3/4 view:
2.2. Awake Nti Approach
2.3. Initial Orotracheal Intubation (Oti) Approach
3. Orotracheal Intubation (Oti) to Nasotracheal Intubation (Nti) Conversion:
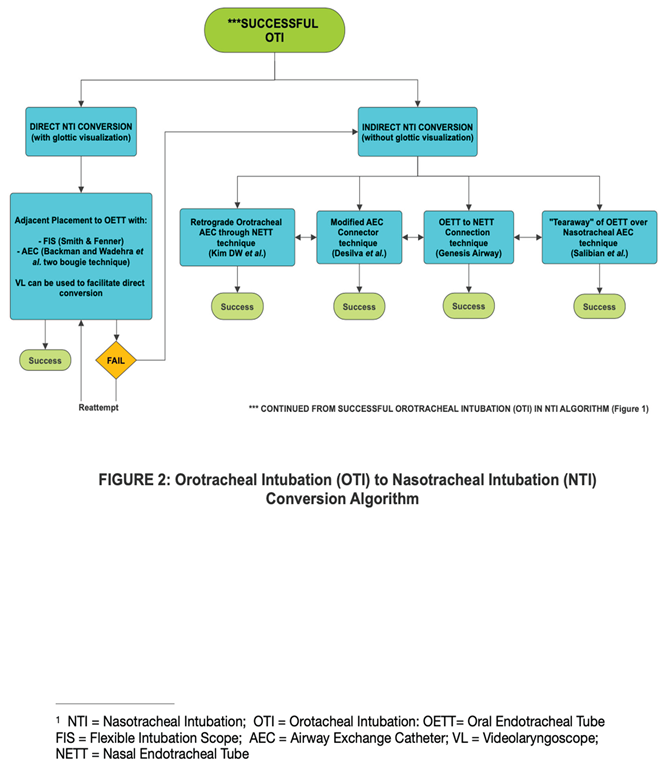
3.1. Direct OTI to NTI Conversion with Glottic Visualization:
3.2. Indirect OTI to NTI Conversion without Glottic Visualization
4. Controlling Epistaxis
5. Conclusion
Supplementary Materials
Acknowledgements
Conflicts of Interest
References
- Park DH, Lee CA, Jeong CY, Yang HS. Nasotracheal intubation for airway management during anesthesia. Anesth Pain Med (Seoul). 2021 Jul;16(3):232-247. [CrossRef]
- Hall CE, Shutt LE. Nasotracheal intubation for head and neck surgery. Anaesthesia. 2003 Mar;58(3):249-56. [CrossRef]
- Chauhan V, Acharya G. Nasal intubation: A comprehensive review. Indian J Crit Care Med. 2016 Nov;20(11):662-667. [CrossRef]
- Yoo H, Choi JM, Jo JY, Lee S, Jeong SM. Blind nasal intubation as an alternative to difficult intubation approaches. J Dent Anesth Pain Med. 2015 Sep;15(3):181-184. [CrossRef]
- Piepho T, Thierbach A, Werner C. Nasotracheal intubation: look before you leap. Br J Anaesth. 2005 Jun;94(6):859-60. [CrossRef]
- Backman SB, Uria M, Kost K, Schricker T. Case report: nasotracheal intubation--look before leaping to assess the laryngeal view. Can J Anaesth. 2008 May;55(5):302-5. [CrossRef]
- Prasanna D, Bhat S. Nasotracheal Intubation: An Overview. J Maxillofac Oral Surg. 2014 Dec;13(4):366-72. [CrossRef]
- Cincotta FA, Neidorff C. Blind awake nasotracheal intubation. Anesth Prog. 1977 Jan-Feb;24(1):15-7. PMCID: PMC2516107.
- Dhasmana S, Singh V, Pal US. Awake Blind Nasotracheal Intubation in Temporomandibular Joint Ankylosis Patients under Conscious Sedation Using Fentanyl and Midazolam. J Maxillofac Oral Surg. 2010 Dec;9(4):377-81. PMID: 22190828 . [CrossRef]
- Apfelbaum JL, Hagberg CA, Connis RT, Abdelmalak BB, Agarkar M, Dutton RP, Fiadjoe JE, Greif R, Klock PA, Mercier D, Myatra SN, O’Sullivan EP, Rosenblatt WH, Sorbello M, Tung A. 2022 American Society of Anesthesiologists Practice Guidelines for Management of the Difficult Airway. Anesthesiology. 2022 Jan 1;136(1):31-81. [CrossRef]
- Jeon DG, Song J, Kim SK, Ji SH. Massive Epistaxis during Nasotracheal Intubation. J Korean Dent Soc Anesthesiol. 2013 Jun;13(2):51-54. [CrossRef]
- Lera, S. Lera, S., Machan, M. and Derefaka, G. (2017) A Safer Technique for Nasal Intubation: A Literature Review. Open Journal of Anesthesiology, 7, 275-285. [CrossRef]
- Nakamura S, Watanabe T, Hiroi E, Sasaki T, Matsumoto N. Hori T: [cuff damage during naso-tracheal intubation for general anesthesia in oral surgery]. Masui. 1997;46(11):1508–14. PMID: 9404138.
- Gorback, MS. Gorback MS. Inflation of the endotracheal tube cuff as an aid to blind nasal endotracheal intubation. Anesth Analg. 1987;66:916–7 PMID: 3619105.
- Kumar R, Gupta E, Kumar S, Rani Sharma K, Rani Gupta N. Cuff inflation-supplemented laryngoscope-guided nasal intubation: a comparison of three endotracheal tubes. Anesth Analg. 2013;116(3):619–24. [CrossRef]
- Goodine C, Sparrow K, Asselin M, Hung D, Hung O. The alignment approach to nasotracheal intubation. Can J Anaesth. 2016 Aug;63(8):991-2. [CrossRef]
- Choudhry DK, Brenn BR, Lutwin-Kawalec M, Sacks K, Nesargi S, He Z. Effect of 90° counterclockwise rotation of the endotracheal tube on its advancement through the larynx during nasal fiberoptic intubation in children: a randomized and blinded study. Paediatr Anaesth. 2016 Apr;26(4):378-83. [CrossRef]
- Abrons RO, Vansickle RA, Ouanes JP. Seldinger technique for nasal intubation: a case series. J Clin Anesth. 2016 Nov;34:609-11. PMID: 27687457. [CrossRef]
- Techanivate A, Kumwilaisak K, Worasawate W, Tanyong A. Estimation of the proper length of nasotracheal intubation by Chula formula. J Med Assoc Thai. 2008 Feb;91(2):173-80. PMID: 18389981.
- Use Of A Nasal Airway To Assist Ventilation During Fiberoptic Intubation. Anyone Can Intubate, 5th Edition, C. Whitten MD https://airwayjedi.com/2015/09/16/use-of-a-nasal-airway-to-assist-ventilation-during-fiberoptic-intubation/.
- Mohammadzadeh A, Haghighi M, Naderi B, Chaudhry A, Khan ZH, Rasouli MR, Saadat S. Comparison of two different methods of fiber-optic nasal intubation: conventional method versus facilitated method (NASAL-18). Ups J Med Sci. 2011 May;116(2):138-41. [CrossRef]
- Syal R, Parvez M, Kothari N, Abbas H, Kumar R, Singh S, Choudhary G. Comparison of Conventional Technique versus Modified Tube First Technique of Awake Nasotracheal Fiber-optic Intubation: A Randomized Control Open-Label Trial. Anesth Essays Res. 2020 Jul-Sep;14(3):395-400. [CrossRef]
- Spinella MK, Nathan H, Wilson T, Perez DE. A Reliable Protocol for Fiberoptic Nasal Intubation. J Oral Maxillofac Surg. 2025 Feb;83(2):148-155. [CrossRef]
- Ryoo SH, Park KN, Karm MH. The utilization of video laryngoscopy in nasotracheal intubation for oral and maxillofacial surgical procedures: a narrative review. J Dent Anesth Pain Med. 2024 Feb;24(1):1-17. [CrossRef]
- Tseng KY, Lu IC, Shen YC, Lin CH, Chen PN, Cheng KI. A comparison of the video laryngoscopes with Macintosh laryngoscope for nasotracheal intubation. Asian J Anesthesiol. 2017 Mar;55(1):17-21. [CrossRef]
- Jiang J, Ma DX, Li B, Wu AS, Xue FS. Videolaryngoscopy versus direct laryngoscopy for nasotracheal intubation: A systematic review and meta-analysis of randomised controlled trials. J Clin Anesth. 2019 Feb;52:6-16. [CrossRef]
- Kwak HJ, Lee SY, Lee SY, Cho SH, Kim HS, Kim JY. McGrath Video Laryngoscopy Facilitates Routine Nasotracheal Intubation in Patients Undergoing Oral and Maxillofacial Surgery: A Comparison With Macintosh Laryngoscopy. J Oral Maxillofac Surg. 2016. [CrossRef]
- Yeom JH, Oh MK, Shin WJ, Ahn DW, Jeon WJ, Cho SY. Randomized comparison of the effectiveness of nasal intubation using a GlideScope video laryngoscope with Magill forceps versus vascular forceps in patients with a normal airway. Can J Anaesth. 2017 Dec;64(12):1176-1181. [CrossRef]
- Kang R, Jeong JS, Ko JS, Ahn J, Gwak MS, Choi SJ, Hwang JY, Hahm TS. Neutral Position Facilitates Nasotracheal Intubation with a GlideScope Video Laryngoscope: A Randomized Controlled Trial. Journal of Clinical Medicine. 2020; 9(3):671. [CrossRef]
- Nedrud SM, Baasch DG, Cabral JD, McEwen DS, Dasika J. Combined Video Laryngoscope and Fiberoptic Nasal Intubation. Cureus. 2021 Nov 11;13(11):e19482. PMID: 34912623 . [CrossRef]
- Hodgson RE, Gunning MDG. Oral to nasal endotracheal tube exchange using both video and flexible laryngoscopes. South Afr J Anesth Analg. 2018;24:168–169. [CrossRef]
- Douglas B, Stacey N, Salam S, Jayanth D. A hybrid nasal intubation technique for the head and neck surgical patient: a case series and review of the literature. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology. Volume 131, Issue 1, 2021, Pages e38-e39.
- Dong Y, Li G, Wu W, Su R, Shao Y. Lightwand-guided nasotracheal intubation in oromaxillofacial surgery patients with anticipated difficult airways: a comparison with blind nasal intubation. Int J Oral Maxillofac Surg. 2013 Sep;42(9):1049-53. PMID: 23712007. [CrossRef]
- Kuang-I Cheng, Hung-T Hsu, Chia-H Lin, Kuang-Y Tseng, Ya-C Shen, Chung-H Chen, Wen-M Chuang, Trachway in Assistance of Nasotracheal Intubation with a Preformed Nasotracheal Tube in Patients Undergoing Oro-Maxillofacial Surgery, BJA: British Journal of Anaesthesia, Volume 113, Issue eLetters Supplement, 29 December 2014. [CrossRef]
- Yu J, Hu R, Wu L, Sun P, Zhang Z. A comparison between the Disposcope endoscope and fibreoptic bronchoscope for nasotracheal intubation: a randomized controlled trial. BMC Anesthesiol. 2019;19(1):163. [CrossRef]
- Morgan JP 3rd, Haug RH, Holmgreen WC. Awake blind nasoendotracheal intubation: a comprehensive review. J Oral Maxillofac Surg. 1994 Dec;52(12):1303-11. [CrossRef]
- Blind nasotracheal intubation video courtesy of Therese Canares, MD, and Jonathan Valente, MD, Rhode Island Hospital, Brown University https://emedicine.medscape.com/article/1663655-technique?form=fpf#showall.
- Dyson A, Saunders PR, Giesecke AH. Awake blind nasal intubation: use of a simple whistle. Anaesthesia. 1990 Jan;45(1):71-2. [CrossRef]
- King HK, Wooten JD. Blind nasal intubation by monitoring end-tidal CO2. Anesth Analg. 1989 Sep;69(3):412-3. PMID: 2505644.
- Asai, T. Asai T. Use of the endotrol endotracheal tube and a light wand for blind nasotracheal intubation. Anesthesiology. 1999 Nov;91(5):1557. [CrossRef]
- Tsukamoto M, Hitosugi T, Yokoyama T. Awake fiberoptic nasotracheal intubation for patients with difficult airway. J Dent Anesth Pain Med. 2018 Oct;18(5):301-304. [CrossRef]
- Ahmad, I. Ahmad, I. NYSORA: Regional and Topical Anesthesia for Awake Endotracheal Intubation. https://www.nysora.com/techniques/head-and-neck-blocks/airway/regional-topical-anesthesia-awake-endotracheal-intubation/#toc.
- Liu JH, Xue FS, Liao X, Zhang YM. Awake nasal intubation using a combination of the EndoFlex tube and fibreoptic bronchoscopy in patients with difficult airways. Acta Anaesthesiol Scand. 2010 Jan;54(1):121-2; author reply 122. [CrossRef]
- Sharma D, Bithal PK, Rath GP, Pandia MP. Effect of orientation of a standard polyvinyl chloride tracheal tube on success rates during awake flexible fibreoptic intubation. Anaesthesia. 2006 Sep;61(9):845-8. [CrossRef]
- Lomax SL, Johnston KD, Marfin AG, Yentis SM, Kathawaroo S, Popat MT. Nasotracheal fibreoptic intubation: a randomised controlled trial comparing the GlideRite® (Parker-Flex® Tip) nasal tracheal tube with a standard pre-rotated nasal RAE™ tracheal tube. Anaesthesia. 2011 Mar;66(3):180-4. [CrossRef]
- Johnston KD, Rai MR. Conscious sedation for awake fibreoptic intubation: a review of the literature. Can J Anaesth. 2013 Jun;60(6):584-99. [CrossRef]
- Kramer A, Müller D, Pförtner R, Mohr C, Groeben H. Fibreoptic vs videolaryngoscopic (C-MAC(®) D-BLADE) nasal awake intubation under local anaesthesia. Anaesthesia. 2015 Apr;70(4):400-6. [CrossRef]
- Gupta N, Garg R, Saini S, Kumar V. GlideScope video laryngoscope-assisted nasotracheal intubation by cuff-inflation technique in head and neck cancer patients. Br J Anaesth. 2016 Apr;116(4):559-60. [CrossRef]
- Kumar, A. Kumar A. Nasal Retrograde Intubation in Oromaxillofacial Surgery Patients with Limited Mouth Opening: A Cross- sectional Study. Int J Sci Stud 2018;6(3):57-61.
- Vadepally AK, Sinha R, Kumar AVSSS. Retrograde intubation through nasal route in patients with limited mouth opening undergoing oral and maxillofacial surgery. J Oral Biol Craniofac Res. 2018 Jan-Apr;8(1):30-34. [CrossRef]
- Smith JE, Fenner SG. Conversion of orotracheal to nasotracheal intubation with the aid of the fibreoptic laryngoscope. Anaesthesia. 1993 Nov;48(11):1016. [CrossRef]
- Backman SB, Uria M, Kost K, Schricker T. Case report: nasotracheal intubation--look before leaping to assess the laryngeal view. Can J Anaesth. 2008 May;55(5):302-5. [CrossRef]
- Wadehra A, Tandon MS, Ganjoo P. A two-bougie technique for safer oro- to nasotracheal tube exchange in a difficult airway. Anaesthesia. 2010 Dec;65(12):1231-2. [CrossRef]
- Yogo N, Sasaki T, Kozumi M, Kinoshita Y, Muto Y, Hirai K, Yoshino Y. Oral to nasal endotracheal tube exchange using tracheal tube guide and video laryngoscope in a pediatric patient with facial burns: a case report. Int J Emerg Med. 2022 Sep 5;15(1):42. [CrossRef]
- Ji S, Song J, Kim SK, Kim MY, Kim S. Fiberoptic bronchoscope and C-MAC video laryngoscope assisted nasal-oral tube exchange: two case reports. J Dent Anesth Pain Med. 2017 Sep;17(3):219-223. Epub 2017 Sep 25. [CrossRef]
- Gentry WB, Shanks CA. Reevaluation of a maneuver to visualize the anterior larynx after intubation. Anesth Analg. 1993 Jul;77(1):161-3. [CrossRef]
- Kim DW, Kim KN, Sun JE, Lim HJ. Conversion of an oral to nasal intubation in difficult nasal anatomy patients: two case reports. BMC Anesthesiol. 2021 Mar 9;21(1):72. [CrossRef]
- Nakata Y, Niimi Y. Oral-to-nasal endotracheal tube exchange in patients with bleeding esophageal varices. Anesthesiology. 1995 Dec;83(6):1380-1. [CrossRef]
- Desilva M, Maan R, Helwany ME, Bhuller AS. Oral to Nasal Endotracheal Tube Exchange: Modification to Enable Wider Applicability of an “Old Connector” Technique-A Case Report. A A Pract. 2023 Jul 21;17(7):e01703. [CrossRef]
- Salibian H, Jain S, Gabriel D, Azocar RJ. Conversion of an oral to nasal orotracheal intubation using an endotracheal tube exchanger. Anesth Analg. 2002 Dec;95(6):1822. [CrossRef]
- https://genesisairway.com/genesis-oral-nasal-endotracheal-tube-posterior-facing-bevel/.
- Sanuki T, Hirokane M, Matsuda Y, Sugioka S, Kotani J. The Parker Flex-Tip tube for nasotracheal intubation: the influence on nasal mucosal trauma. Anaesthesia. 2010 Jan;65(1):8-11. [CrossRef]
- Jafari A, Gharaei B, Kamranmanesh MR, Aghamohammadi H, Nobahar MR, Poorzamany M, Shahrabi M, Solhpour A. Wire reinforced endotracheal tube compared with Parker Flex-Tip tube for oral fiberoptic intubation: a randomized clinical trial. Minerva Anestesiol. 2014 Mar;80(3):324-9. PMID: 24193173.
- Vivian VH, Anaes D, L Pardon T, Van Zundert AAJ. Modified Retrograde Nasal Intubation: A New Airway Technique and Devices. Anesth Prog. 2021 Jun 1;68(2):107-113. [CrossRef]
- Dutta A, Chari P, Mohan RA, Manhas Y. Oral to nasal endotracheal tube exchange in a difficult airway: a novel method. Anesthesiology. 2002 Nov;97(5):1324-5. [CrossRef]
- De-Armendi A, Shukry M, Mayhew JF. Changing an oral endotracheal tube to a nasal tube in Pierre-Robin sequence. Paediatr Anaesth. 2009 Dec;19(12):1240-1. [CrossRef]
- Benumof JL, Augoustides JG. Rigorously Maintaining a “Targeted Depth of Insertion” for an Airway Exchange Catheter During Tracheal Tube Exchange. J Cardiothorac Vasc Anesth. 2019 Dec;33(12):3414-3415. [CrossRef]
- Jeon DG, Song J, Kim SK, Ji SH. Massive Epistaxis during Nasotracheal Intubation. J Korean Dent Soc Anesthesiol. 2013 Jun;13(2):51-54. [CrossRef]
- Inoue S, Fujimoto Y, Kawano Y, Furuya H. Difficult passage of the endotracheal tube and massive nasal bleeding during awake nasal fiberoptic intubation in a patient with airway obstruction caused by neck hematoma--a case report. Middle East J Anaesthesiol. 2011 Feb;21(1):125-7. PMID: 21991746.
- Sim WS, Chung IS, Chin JU, Park YS, Cha KJ, Lee SC, Kim YC. Risk factors for epistaxis during nasotracheal intubation. Anaesth Intensive Care. 2002 Aug;30(4):449-52. [CrossRef]
- Lim HS, Kim D, Lee J, Son JS, Lee JR, Ko S. Reliability of assessment of nasal flow rate for nostril selection during nasotracheal intubation. J Clin Anesth. 2012 Jun;24(4):270-4. [CrossRef]
- Tong JL, Tung A. A Randomized Trial Comparing the Effect of Fiberoptic Selection and Guidance Versus Random Selection, Blind Insertion, and Direct Laryngoscopy, on the Incidence and Severity of Epistaxis After Nasotracheal Intubation. Anesth Analg. 2018 Aug;127(2):485-489. [CrossRef]
- Thota RS, Doctor JR. Evaluation of paranasal sinuses on available computed tomography in head and neck cancer patients: An assessment tool for nasotracheal intubation. Indian J Anaesth. 2016 Dec;60(12):960-961. [CrossRef]
- Tan YL, Wu ZH, Zhao BJ, Ni YH, Dong YC. For nasotracheal intubation, which nostril results in less epistaxis: right or left?: A systematic review and meta-analysis. Eur J Anaesthesiol. 2021 Nov 1;38(11):1180-1186. [CrossRef]
- Boku A, Hanamoto H, Hirose Y, Kudo C, Morimoto Y, Sugimura M, Niwa H. Which nostril should be used for nasotracheal intubation: the right or left? A randomized clinical trial. J Clin Anesth. 2014 Aug;26(5):390-4. Epub 2014 Aug 10.. [CrossRef]
- Sanuki T, Hirokane M, Kotani J. Epistaxis during nasotracheal intubation: a comparison of nostril sides. J Oral Maxillofac Surg. 2010 Mar;68(3):618-21. Epub 2009 Nov 22. [CrossRef]
- Moore, Daniel C. M.D.. Middle Turbinectomy: A Complication of IMPROPER Nasal Intubation?. The Journal of the American Society of Anesthesiologists 92(5):p 1504, May 1, 2000. [CrossRef]
- Park JY, Yu J, Kim CS, Mun T, Jeong WS, Choi JW, Lee K, Kim YK. Reverse tube direction and epistaxis in left nasotracheal intubation: a randomized controlled trial. Korean J Anesthesiol. 2024 Dec;77(6):596-604. [CrossRef]
- Wong A, Subar P, Witherell H, Ovodov KJ. Reducing nasopharyngeal trauma: the urethral catheter-assisted nasotracheal intubation technique. Anesth Prog. 2011 Spring;58(1):26-30. Anesth Prog. 2011 Summer;58(2):107. [CrossRef]
- Lim CW, Min SW, Kim CS, Chang JE, Park JE, Hwang JY. The use of a nasogastric tube to facilitate nasotracheal intubation: a randomised controlled trial. Anaesthesia. 2014 Jun;69(6):591-7. Epub 2014 Apr 18. [CrossRef]
- Bahk JH, Ahn WS, Lim YJ. Use of esophageal stethoscope as an introducer during nasotracheal intubation. Anesthesiology. 2000 May;92(5):1503-4. PMID: 10781307. [CrossRef]
- Watt S, Pickhardt D, Lerman J, Armstrong J, Creighton PR, Feldman L. Telescoping tracheal tubes into catheters minimizes epistaxis during nasotracheal intubation in children. Anesthesiology. 2007 Feb;106(2):238-42. [CrossRef]
- Enk D, Palmes AM, Van Aken H, Westphal M. In Nasotracheal intubation: a simple and effective technique to reduce nasopharyngeal trauma and tube contamination. Anesth Analg. 2002 Nov; 95(5): 1432-6, table of contents. https://doi/10.1097/00000539-200211000-00061; 83. Enk D, Palmes AM, Van Aken H, Westphal M. Nasotracheal intubation: a simple and effective technique to reduce nasopharyngeal trauma and tube contamination. Anesth Analg. 2002 Nov;95(5):1432-6, table of contents. [Google Scholar] [CrossRef]
- Prasanna D, Bhat S. Nasotracheal Intubation: An Overview. J Maxillofac Oral Surg. 2014 Dec;13(4):366-72. Epub 2013 May 1. [CrossRef]
- Ahmed-Nusrath A, Tong JL, Smith JE. Pathways through the nose for nasal intubation: a comparison of three endotracheal tubes. Br J Anaesth. 2008 Feb;100(2):269-74. Epub 2007 Dec 14. [CrossRef]
- Kim H, Lee JM, Lee J, Hwang JY, Chang JE, No HJ, Won D, Choi S, Min SW. Influence of Nasal Tip Lifting on the Incidence of the Tracheal Tube Pathway Passing Through the Nostril During Nasotracheal Intubation: A Randomized Controlled Trial. Anesth Analg. 2018 Dec;127(6):1421-1426. [CrossRef]
- Katz RI, Hovagim AR, Finkelstein HS, Grinberg Y, Boccio RV, Poppers PJ. A comparison of cocaine, lidocaine with epinephrine, and oxymetazoline for prevention of epistaxis on nasotracheal intubation. J Clin Anesth. 1990 Jan-Feb;2(1):16-20. [CrossRef]
- Dhakate VR, Singam AP, Bharadwaj HS. Evaluation of Nasopharyngeal Airway to Facilitate Nasotracheal Intubation. Ann Maxillofac Surg. 2020 Jan-Jun;10(1):57-60. Epub 2020 Jun 8. [CrossRef]
- Kim YC, Lee SH, Noh GJ, Cho SY, Yeom JH, Shin WJ, Lee DH, Ryu JS, Park YS, Cha KJ, Lee SC. Thermosoftening treatment of the nasotracheal tube before intubation can reduce epistaxis and nasal damage. Anesth Analg. 2000 Sep;91(3):698-701. [CrossRef]
- Kim EM, Chung MH, Lee MH, Choi EM, Jun IJ, Yun TH, Ko YK, Kim JH, Jun JH. Is Tube Thermosoftening Helpful for Videolaryngoscope-Guided Nasotracheal Intubation?: A Randomized Controlled Trial. Anesth Analg. 2019 Sep;129(3):812-818. [CrossRef]
- Seo KS, Kim JH, Yang SM, Kim HJ, Bahk JH, Yum KW. A new technique to reduce epistaxis and enhance navigability during nasotracheal intubation. Anesth Analg. 2007 Nov;105(5):1420-4. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



