Submitted:
11 September 2025
Posted:
12 September 2025
Read the latest preprint version here
Abstract
Keywords:
1. The Condition, Its Prevalence and Its Comorbidities
2. The Multifaceted Pathophysiology of IBS
3. The Role of Diet in IBS
4. Limitations to Dietary Symptom Management
5. The Role of the Microbiome in IBS
6. Can Insights from IBD be Helpful for Understanding IBS?
7. The Therapeutic Potential of Fasting

8. Underappreciated Need for Renewal in IBS?
9. Mechanisms by Which IF May Improve Gut Homeostasis in IBS
9.1. Reduction in Pro-Inflammatory Signalling
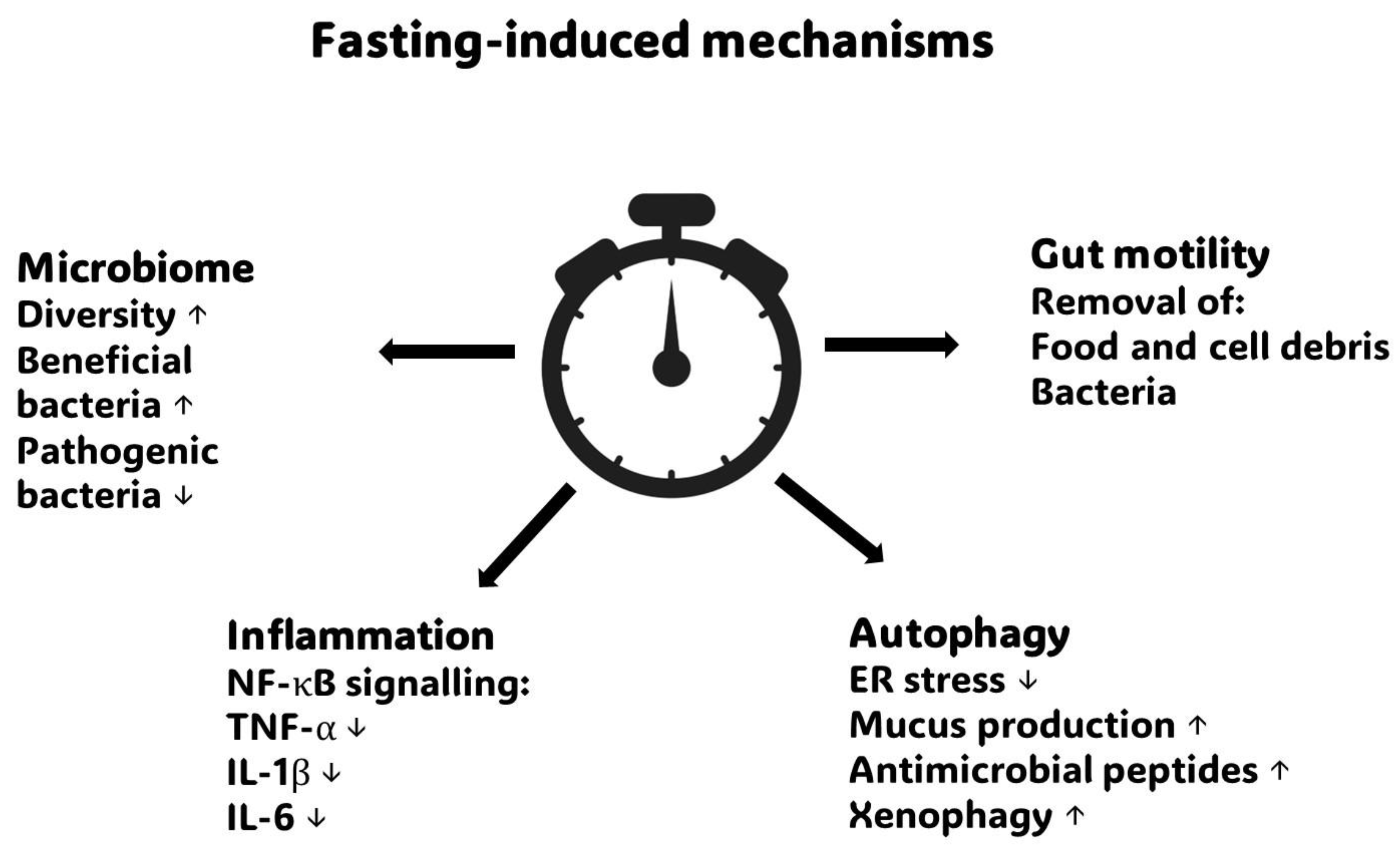
9.2. Migrating Motor Complex Activity
9.3. Modulation of Gut Microbiota
9.4. Enhancement of Autophagy
9.5. Considerations for the Application of Intermittent Fasting Regimes in IBS Treatment
Acknowledgments
Conflicts of Interest
Use of AI
References
- Drossman, DA. Functional Gastrointestinal Disorders: History, Pathophysiology, Clinical Features and Rome IV. Gastroenterology. 2016;S0016-5085(16)00223-7. [CrossRef]
- Fikree A, Byrne P. Management of functional gastrointestinal disorders. Clin Med. 2021;21(1):44–52.
- Kim JH, Lin E, Pimentel M. Biomarkers of Irritable Bowel Syndrome. J Neurogastroenterol Motil. 2017;23(1):20–6.
- Oka P, Parr H, Barberio B, Black CJ, Savarino EV, Ford AC. Global prevalence of irritable bowel syndrome according to Rome III or IV criteria: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2020;5(10):908–17. [CrossRef]
- Shiha MG, Aziz I. Review article: Physical and psychological comorbidities associated with irritable bowel syndrome. Aliment Pharmacol Ther. 2021;54 Suppl 1:S12–23. [CrossRef]
- Holtmann GJ, Ford AC, Talley NJ. Pathophysiology of irritable bowel syndrome. Lancet Gastroenterol Hepatol. 2016;1(2):133–46.
- El-Salhy M, Johansson M, Klevstul M, Hatlebakk JG. Quality of life, functional impairment and healthcare experiences of patients with irritable bowel syndrome in Norway: an online survey. BMC Gastroenterol. 2025;25(1):143. [CrossRef]
- Canavan C, West J, Card T. Review article: the economic impact of the irritable bowel syndrome. Aliment Pharmacol Ther. 2014;40(9):1023–34. [CrossRef]
- IFFGD’s IBS Patients’ Illness Experience and Unmet Needs Survey - IFFGD. https://iffgd.org/news/press-release/2020-iffgd-s-ibs-patients-illness-experience-and-unmet-needs-survey/.
- Ford AC, Sperber AD, Corsetti M, Camilleri M. Irritable bowel syndrome. The Lancet. 2020;396(10263):1675–88.
- Simrén M, Månsson A, Langkilde AM, Svedlund J, Abrahamsson H, Bengtsson U, mfl. Food-related gastrointestinal symptoms in the irritable bowel syndrome. Digestion. 2001;63(2):108–15. [CrossRef]
- Capili B, Anastasi JK, Chang M. Addressing the Role of Food in Irritable Bowel Syndrome Symptom Management. J Nurse Pract. 2016;12(5):324–9. [CrossRef]
- Atkinson W, Sheldon TA, Shaath N, Whorwell PJ. Food elimination based on IgG antibodies in irritable bowel syndrome: a randomised controlled trial. Gut. 2004;53(10):1459–64. [CrossRef]
- Böhn L, Störsrud S, Törnblom H, Bengtsson U, Simrén M. Self-Reported Food-Related Gastrointestinal Symptoms in IBS Are Common and Associated With More Severe Symptoms and Reduced Quality of Life. Off J Am Coll Gastroenterol ACG. 2013;108(5):634. [CrossRef]
- Young E, Stoneham MD, Petruckevitch A, Barton J, Rona R. A population study of food intolerance. Lancet Lond Engl. 1994;343(8906):1127–30.
- Murray HB, Doerfler B, Harer KN, Keefer L. Psychological Considerations in the Dietary Management of Patients With DGBI. Am J Gastroenterol. 2022. [CrossRef]
- Valeur J, Øines E, Helvik Morken M, Juul Holst J, Berstad A. Plasma glucagon-like peptide 1 and peptide YY levels are not altered in symptomatic fructose-sorbitol malabsorption. Scand J Gastroenterol. 2008;43(10):1212–8. [CrossRef]
- Valeur J, Morken MH, Norin E, Midtvedt T, Berstad A. Carbohydrate intolerance in patients with self-reported food hypersensitivity: Comparison of lactulose and glucose. Scand J Gastroenterol. 2009;44(12):1416–23. [CrossRef]
- Francis CY, Whorwell PJ. Bran and irritable bowel syndrome: time for reappraisal. Lancet Lond Engl. 1994;344(8914):39–40.
- Fritscher-Ravens A, Schuppan D, Ellrichmann M, Schoch S, Röcken C, Brasch J, Bethge J, Böttner M, Klose J, Milla PJ. Confocal endomicroscopy shows food-associated changes in the intestinal mucosa of patients with irritable bowel syndrome. Gastroenterology. 2014;147(5):1012-1020.e4. [CrossRef]
- Aguilera-Lizarraga J, Florens MV, Viola MF, Jain P, Decraecker L, Appeltans I, Cuende-Estevez M, Fabre N, Van Beek K, Perna E, Balemans D, Stakenborg N, Theofanous S, Bosmans G, Mondelaers SU, Matteoli G, Ibiza Martínez S, Lopez-Lopez C, Jaramillo-Polanco J, Talavera K, Alpizar YA, Feyerabend TB, Rodewald HR, Farre R, Redegeld FA, Si J, Raes J, Breynaert C, Schrijvers R, Bosteels C, Lambrecht BN, Boyd SD, Hoh RA, Cabooter D, Nelis M, Augustijns P, Hendrix S, Strid J, Bisschops R, Reed DE, Vanner SJ, Denadai-Souza A, Wouters MM, Boeckxstaens GE. Local immune response to food antigens drives meal-induced abdominal pain. Nature. 2021;590(7844):151–6. [CrossRef]
- Pedersen N, Ankersen DV, Felding M, Wachmann H, Végh Z, Molzen L, Burisch J, Andersen JR, Munkholm P. Low-FODMAP diet reduces irritable bowel symptoms in patients with inflammatory bowel disease. World J Gastroenterol. 2017;23(18):3356–66. [CrossRef]
- Halmos EP, Power VA, Shepherd SJ, Gibson PR, Muir JG. A diet low in FODMAPs reduces symptoms of irritable bowel syndrome. Gastroenterology. 2014;146(1):67-75.e5. [CrossRef]
- Algera JP, Demir D, Törnblom H, Nybacka S, Simrén M, Störsrud S. Low FODMAP diet reduces gastrointestinal symptoms in irritable bowel syndrome and clinical response could be predicted by symptom severity: A randomized crossover trial. Clin Nutr Edinb Scotl. 2022;41(12):2792–800. [CrossRef]
- Austin GL, Dalton CB, Hu Y, Morris CB, Hankins J, Weinland SR, Westman EC, Yancy WS Jr, Drossman DA. A Very Low-carbohydrate Diet Improves Symptoms and Quality of Life in Diarrhea-Predominant Irritable Bowel Syndrome. Clin Gastroenterol Hepatol Off Clin Pract J Am Gastroenterol Assoc. juni 2009;7(6):706-708.e1.
- Nybacka S, Törnblom H, Josefsson A, Hreinsson JP, Böhn L, Frändemark Å, mfl. A low FODMAP diet plus traditional dietary advice versus a low-carbohydrate diet versus pharmacological treatment in irritable bowel syndrome (CARIBS): a single-centre, single-blind, randomised controlled trial. Lancet Gastroenterol Hepatol. 2024. [CrossRef]
- Tuck CJ, Reed DE, Muir J, Vanner S. A236 A REAL-WORLD EVALUATION OF THE LOW FODMAP DIET IMPLEMENTATION: POOR COMPLIANCE IS SIGNIFICANTLY IMPROVED BY GUIDANCE FROM A DIETITIAN. J Can Assoc Gastroenterol. 2019;2(Suppl 2):461. [CrossRef]
- Scarlata K, Eswaran S, Baker JR, Chey WD. Utilization of Dietitians in the Management of Irritable Bowel Syndrome by Members of the American College of Gastroenterology. Off J Am Coll Gastroenterol ACG. 2022;117(6):923. [CrossRef]
- Ioniță-Mîndrican CB, Ziani K, Mititelu M, Oprea E, Neacșu SM, Moroșan E, mfl. Therapeutic Benefits and Dietary Restrictions of Fiber Intake: A State of the Art Review. Nutrients. 2022;14(13):2641. [CrossRef]
- Heizer WD, Southern S, McGovern S. The Role of Diet in Symptoms of Irritable Bowel Syndrome in Adults: A Narrative Review. J Am Diet Assoc. 2009;109(7):1204–14. [CrossRef]
- Wu S, Yang Z, Yuan C, Liu S, Zhang Q, Zhang S, Zhu S. Coffee and tea intake with long-term risk of irritable bowel syndrome: a large-scale prospective cohort study. Int J Epidemiol. 2023;52(5):1459–72. [CrossRef]
- Shaikh SD, Sun N, Canakis A, Park WY, Weber HC. Irritable Bowel Syndrome and the Gut Microbiome: A Comprehensive Review. J Clin Med. 2023;12(7):2558. [CrossRef]
- Chong PP, Chin VK, Looi CY, Wong WF, Madhavan P, Yong VC. The Microbiome and Irritable Bowel Syndrome - A Review on the Pathophysiology, Current Research and Future Therapy. Front Microbiol. 2019;10:1136.
- Vich Vila A, Imhann F, Collij V, Jankipersadsing SA, Gurry T, Mujagic Z, mfl. Gut microbiota composition and functional changes in inflammatory bowel disease and irritable bowel syndrome. Sci Transl Med. 2018;10(472):eaap8914. [CrossRef]
- Tap J, Derrien M, Törnblom H, Brazeilles R, Cools-Portier S, Doré J, mfl. Identification of an Intestinal Microbiota Signature Associated With Severity of Irritable Bowel Syndrome. Gastroenterology. 2017;152(1):111-123.e8. [CrossRef]
- Halkjær SI, Lo B, Cold F, Højer Christensen A, Holster S, König J, Brummer RJ, Aroniadis OC, Lahtinen P, Holvoet T, Gluud LL, Petersen AM. Fecal microbiota transplantation for the treatment of irritable bowel syndrome: A systematic review and meta-analysis. World J Gastroenterol. 2023. 28;29(20):3185-3202. [CrossRef]
- Lee J-Y, Bays DJ, Savage HP, Bäumler AJ. The human gut microbiome in health and disease: time for a new chapter? Infect Immun. 2024. 12;92(11):e0030224. [CrossRef]
- Akdis, CA. Does the epithelial barrier hypothesis explain the increase in allergy, autoimmunity and other chronic conditions? Nat Rev Immunol. 2021. 21(11):739-751. [CrossRef]
- Parrish A, Boudaud M, Kuehn A, Ollert M, Desai MS. Intestinal mucus barrier: a missing piece of the puzzle in food allergy. Trends Mol Med. 2022. 28(1):36-50. [CrossRef]
- Laudisi F, Di Fusco D, Dinallo V, Stolfi C, Di Grazia A, Marafini I, Colantoni A, Ortenzi A, Alteri C, Guerrieri F, Mavilio M, Ceccherini-Silberstein F, Federici M, MacDonald TT, Monteleone I, Monteleone G.The Food Additive Maltodextrin Promotes Endoplasmic Reticulum Stress-Driven Mucus Depletion and Exacerbates Intestinal Inflammation. Cell Mol Gastroenterol Hepatol. 2019;7(2):457–73. [CrossRef]
- Chassaing B, Koren O, Goodrich JK, Poole AC, Srinivasan S, Ley RE, mfl. Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Nature. 2015;519(7541):92–6. [CrossRef]
- Szałwińska P, Włodarczyk J, Spinelli A, Fichna J, Włodarczyk M. IBS-Symptoms in IBD Patients—Manifestation of Concomitant or Different Entities. J Clin Med. 2021;10(1):31. [CrossRef]
- Fairbrass KM, Costantino SJ, Gracie DJ, Ford AC. Prevalence of irritable bowel syndrome-type symptoms in patients with inflammatory bowel disease in remission: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. Baumgartner M, Lang M, Holley H, Crepaz D, Hausmann B, Pjevac P, Moser D, Haller F, Hof F, Beer A, Orgler E, Frick A, Khare V, Evstatiev R, Strohmaier S, Primas C, Dolak W, Köcher T, Klavins K, Rath T, Neurath MF, Berry D, Makristathis A, Muttenthaler M, Gasche C.2020;5(12):1053–62.
- Baumgartner M, Lang M, Holley H, Crepaz D, Hausmann B, Pjevac P, Moser D, Haller F, Hof F, Beer A, Orgler E, Frick A, Khare V, Evstatiev R, Strohmaier S, Primas C, Dolak W, Köcher T, Klavins K, Rath T, Neurath MF, Berry D, Makristathis A, Muttenthaler M, Gasche C. Mucosal Biofilms Are an Endoscopic Feature of Irritable Bowel Syndrome and Ulcerative Colitis. Gastroenterology. 2021;161(4):1245-1256.e20. [CrossRef]
- Casén C, Vebø HC, Sekelja M, Hegge FT, Karlsson MK, Ciemniejewska E, Dzankovic S, Frøyland C, Nestestog R, Engstrand L, Munkholm P, Nielsen OH, Rogler G, Simrén M, Öhman L, Vatn MH, Rudi K. Deviations in human gut microbiota: a novel diagnostic test for determining dysbiosis in patients with IBS or IBD. Aliment Pharmacol Ther. 2015;42(1):71–83. [CrossRef]
- Cox SR, Lindsay JO, Fromentin S, Stagg AJ, McCarthy NE, Galleron N, Ibraim SB, Roume H, Levenez F, Pons N, Maziers N, Lomer MC, Ehrlich SD, Irving PM, Whelan K. Effects of Low FODMAP Diet on Symptoms, Fecal Microbiome, and Markers of Inflammation in Patients With Quiescent Inflammatory Bowel Disease in a Randomized Trial. Gastroenterology. 2020;158(1):176-188.e7.
- Norwitz NG, Soto-Mota A. Case report: Carnivore–ketogenic diet for the treatment of inflammatory bowel disease: a case series of 10 patients. Front Nutr. 2024;11:1467475. [CrossRef]
- Li S, Zhuge A, Wang K, Lv L, Bian X, Yang L, Xia J, Jiang X, Wu W, Wang S, Wang Q, Li L. Ketogenic diet aggravates colitis, impairs intestinal barrier and alters gut microbiota and metabolism in DSS-induced mice. Food Funct. 2021;12(20):10210–25. [CrossRef]
- Kong C, Yan X, Liu Y, Huang L, Zhu Y, He J, Gao R, Kalady MF, Goel A, Qin H, Ma Y. Ketogenic diet alleviates colitis by reduction of colonic group 3 innate lymphoid cells through altering gut microbiome. Signal Transduct Target Ther. 2021;6(1):154. [CrossRef]
- Gubatan J, Kulkarni CV, Talamantes SM, Temby M, Fardeen T, Sinha SR. Dietary Exposures and Interventions in Inflammatory Bowel Disease: Current Evidence and Emerging Concepts. Nutrients. 2023;15(3):579. [CrossRef]
- Koppold DA, Breinlinger C, Hanslian E, Kessler C, Cramer H, Khokhar AR, Peterson CM, Tinsley G, Vernieri C, Bloomer RJ, Boschmann M, Bragazzi NL, Brandhorst S, Gabel K, Goldhamer AC, Grajower MM, Harvie M, Heilbronn L, Horne BD, Karras SN, Langhorst J, Lischka E, Madeo F, Mitchell SJ, Papagiannopoulos-Vatopaidinos IE, Papagiannopoulou M, Pijl H, Ravussin E, Ritzmann-Widderich M, Varady K, Adamidou L, Chihaoui M, de Cabo R, Hassanein M, Lessan N, Longo V, Manoogian ENC, Mattson MP, Muhlestein JB, Panda S, Papadopoulou SK, Rodopaios NE, Stange R, Michalsen A. International consensus on fasting terminology. Cell Metab. 2024;36(8):1779-1794.e4. [CrossRef]
- de Cabo R, Mattson MP. Effects of Intermittent Fasting on Health, Aging, and Disease. N Engl J Med. 2019;381(26):2541–51.
- Longo VD, Mattson MP. Fasting: Molecular Mechanisms and Clinical Applications. Cell Metab. 2014;19(2):181–92. [CrossRef]
- Kanazawa M, Fukudo S. Effects of fasting therapy on irritable bowel syndrome. Int J Behav Med. 2006;13(3):214–20. [CrossRef]
- Wang R, Lv X, Xu W, Li X, Tang X, Huang H, Yang M, Ma S, Wang N, Niu Y. Effects of the periodic fasting-mimicking diet on health, lifespan, and multiple diseases: a narrative review and clinical implications. Nutr Rev. 2024; nuae003. [CrossRef]
- Roco-Videla Á, Villota-Arcos C, Pino-Astorga C, Mendoza-Puga D, Bittner-Ortega M, Corbeaux-Ascui T. Intermittent Fasting and Reduction of Inflammatory Response in a Patient with Ulcerative Colitis. Medicina (Mex). 2023;59(8):1453. [CrossRef]
- Weill Medical College of Cornell University. The Impact of Time Restricted Feeding in Crohn’s Disease. clinicaltrials.gov; 2023. Report No.: NCT04271748. https://clinicaltrials.gov/study/NCT04271748.
- Sinha SR. The Influence of a Fasting Mimicking Diet on Ulcerative Colitis. clinicaltrials.gov; 2023. Report No.: NCT03615690. https://clinicaltrials.gov/study/NCT03615690.
- Sinha SR. Effects of an Intermittent Reduced Calorie Diet on Crohn’s Disease. clinicaltrials.gov; 2023. Report No.: NCT04147585. https://clinicaltrials.gov/study/NCT04147585.
- Park JH, Kotani T, Konno T, Setiawan J, Kitamura Y, Imada S, Usui Y, Hatano N, Shinohara M, Saito Y, Murata Y, Matozaki T. Promotion of Intestinal Epithelial Cell Turnover by Commensal Bacteria: Role of Short-Chain Fatty Acids. PLoS ONE. 2016;11(5):e0156334. [CrossRef]
- Barker, N. Adult intestinal stem cells: critical drivers of epithelial homeostasis and regeneration. Nat Rev Mol Cell Biol. 2014;15(1):19–33. [CrossRef]
- Haasis E, Bettenburg A, Lorentz A. Effect of Intermittent Fasting on Immune Parameters and Intestinal Inflammation. Nutrients. 2024;16(22):3956. [CrossRef]
- Deloose E, Janssen P, Depoortere I, Tack J. The migrating motor complex: control mechanisms and its role in health and disease. Nat Rev Gastroenterol Hepatol. 2012;9(5):271–85. [CrossRef]
- Vantrappen G, Janssens J, Hellemans J, Ghoos Y. The interdigestive motor complex of normal subjects and patients with bacterial overgrowth of the small intestine. J Clin Invest. 1977. [CrossRef]
- Ducarmon QR, Grundler F, Le Maho Y, Wilhelmi de Toledo F, Zeller G, Habold C, Mesnage R. Remodelling of the intestinal ecosystem during caloric restriction and fasting. Trends Microbiol. 2023. [CrossRef]
- Paukkonen I, Törrönen EN, Lok J, Schwab U, El-Nezami H. The impact of intermittent fasting on gut microbiota: a systematic review of human studies. Front Nutr. 2024. [CrossRef]
- Pérez-Gerdel T, Camargo M, Alvarado M, Ramírez JD. Impact of Intermittent Fasting on the Gut Microbiota: A Systematic Review. Adv Biol. n/a(n/a):2200337. [CrossRef]
- Bagherniya M, Butler AE, Barreto GE, Sahebkar A. The effect of fasting or calorie restriction on autophagy induction: A review of the literature. Ageing Res Rev. 2018;47:183–97. [CrossRef]
- Telpaz S, Bel S. Autophagy in intestinal epithelial cells prevents gut inflammation. Trends Cell Biol. 2023. [CrossRef]
- Fu R, Liu S, Zhu M, Zhu J, Chen M. Apigenin reduces the suppressive effect of exosomes derived from irritable bowel syndrome patients on the autophagy of human colon epithelial cells by promoting ATG14. World J Surg Oncol. 2023;21(1):95. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



