Submitted:
11 August 2025
Posted:
12 August 2025
Read the latest preprint version here
Abstract
Keywords:
Introduction
Methods
| Sex, male | 116(79,45%) | |
| Age,years | 63.23 ±12.50 | min:29 /max:85 |
| Hypertension | 124(84.9%) | |
| COPD | 41(28,1%) | |
| Renal insufficiency | 33(22.6%) | |
| Diabetes | 23(15.8%) | |
| Coronary artery disease | 71(48,6%) | |
| History of smoking | 61(41.8%) | |
| History of Cerebrovascular disease | 6 (4.1%) | |
| Preoperative aspirin | 85(58.2%) | |
| Preoperative statin | 46(31.5%) | |
| Elective | 121(82.8%) | |
| Urgent | 25(17.1%) |
Results
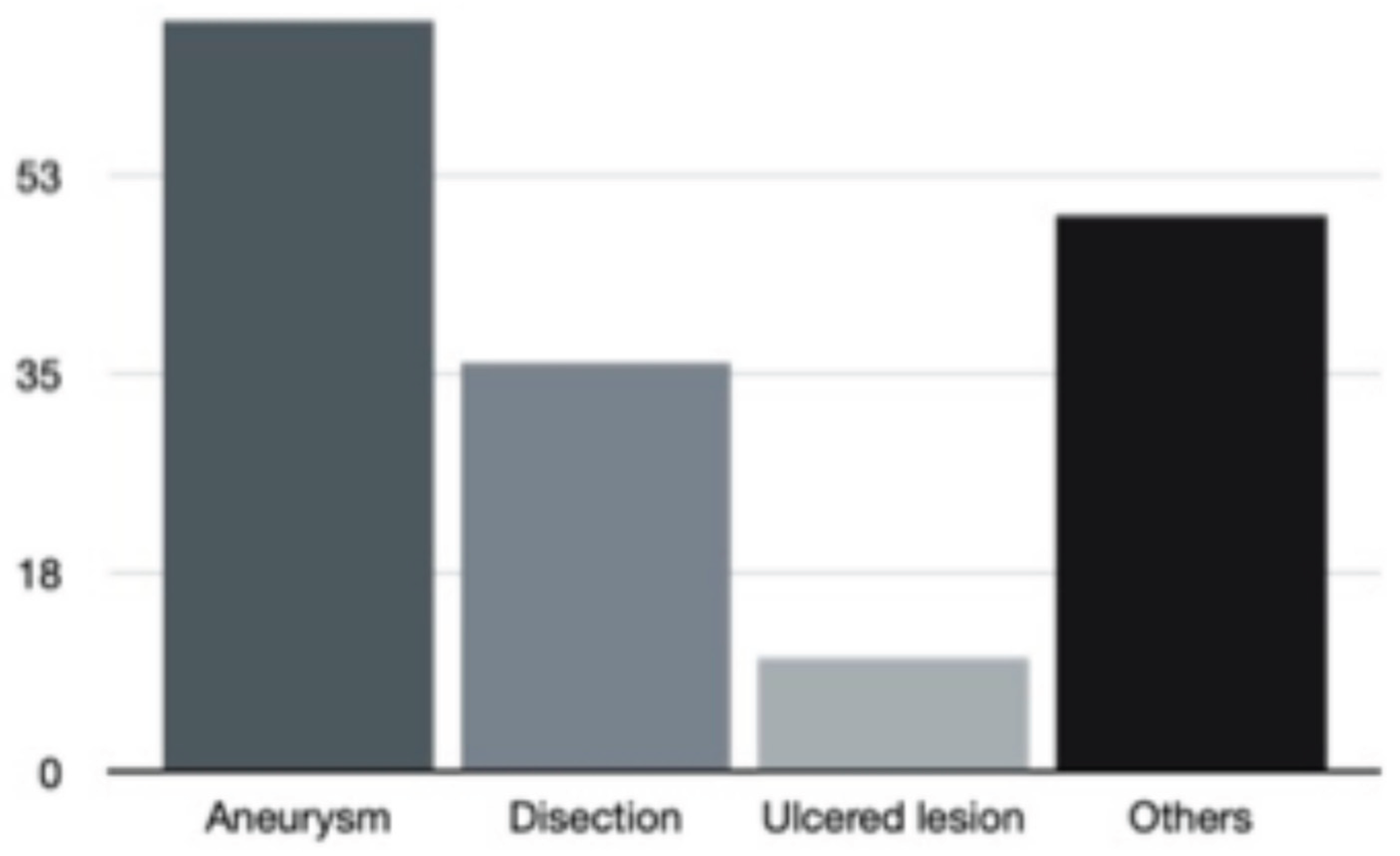
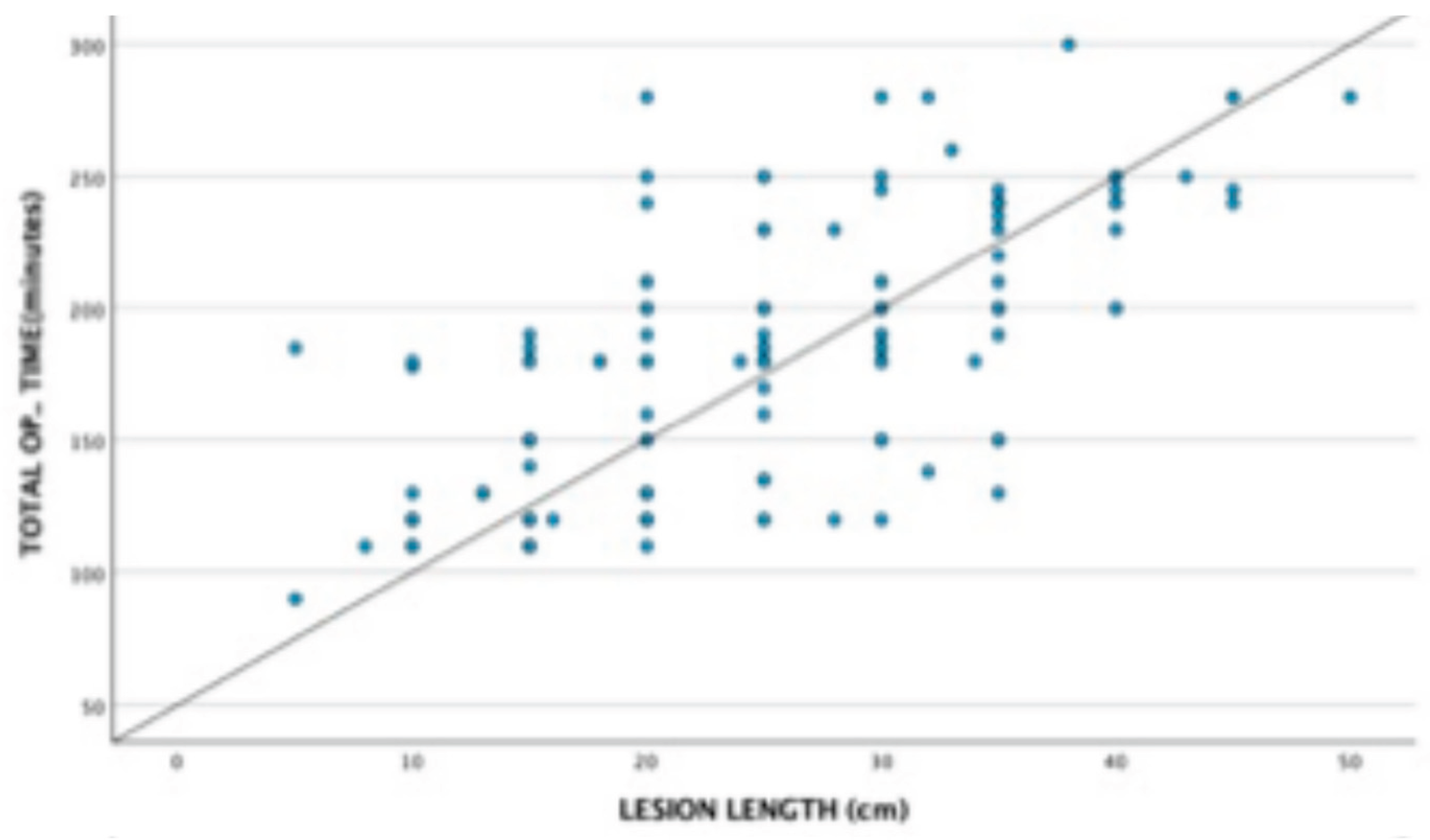
Discussion
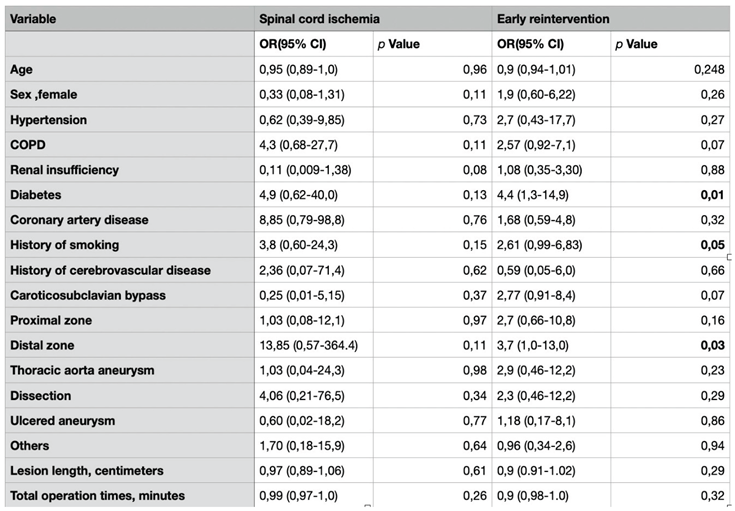 |
Limitations
Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chen SW, Lee KB, et al. Complications and management of the thoracic endovascular aortic repair. Aorta (Stamford). 2020;8(3):49–58. [CrossRef]
- Badran A, Elghazouli Y, Shirke MM, et al. Elective thoracic aortic aneurysm surgery: A tertiary center experience. Cureus. 2023;15(5):e39102. [CrossRef]
- Sattah AP, Secrist MH, Sarin S. Complications and perioperative management of patients undergoing thoracic endovascular aortic repair. J Intensive Care Med. 2018;33(7):394–406. [CrossRef]
- Grabenwöger M, Alfonso F, Bachet J. Thoracic endovascular aortic repair (TEVAR) for the treatment of aortic diseases: A position statement from the European Association for Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur Heart J. 2012;33(13):1558–1563. [CrossRef]
- Sugiura J, Oshima H, et al. The efficacy and risk of cerebrospinal fluid drainage for thoracoabdominal aortic aneurysm repair: A retrospective observational comparison between drainage and non-drainage. Interact Cardiovasc Thorac Surg. 2017;24:609–614. [CrossRef]
- Feezor RJ, Martin T, et al. Extent of aortic coverage and incidence of spinal cord ischemia after thoracic endovascular aneurysm repair. The Society of Thoracic Surgeons. 2008.
- Riambau V, Capoccia L, et al. Spinal cord protection and related complications in endovascular management of B dissection: LSA revascularization and CSF drainage. Ann Cardiothorac Surg. 2014;3(3):336–338. [CrossRef]
- Geisbüsch P, Hoffmann S, et al. Reinterventions during midterm follow-up after endovascular treatment of thoracic aortic disease. J Vasc Surg. 2011;53(6):1528–1535.
- Cheng L. Reintervention after thoracic endovascular aortic repair of uncomplicated type B aortic dissection. J Clin Med. 2023;12(4):1418.
- Faure EM, Canaud L, Agostini C, et al. Reintervention after thoracic endovascular aortic repair of complicated aortic dissection. J Vasc Surg. 2014;59:327–333. [CrossRef]
- Goodney PP, et al. Survival after open versus endovascular thoracic aortic aneurysm repair in an observational study of the Medicare population. Circulation. 2011;124(24):2761–2769. [CrossRef]
- Naazie IN, et al. Risk calculator predicts 30-day mortality after thoracic endovascular aortic repair for intact descending thoracic aortic aneurysms in the Vascular Quality Initiative. Clin Res Thorac Aneurysm. 2022;75(3):833–841.e1.
- Scali ST, et al. National incidence, mortality outcomes, and predictors of spinal cord ischemia after thoracic endovascular aortic repair. J Vasc Surg. 2020;72(1):152–160.
- Bavaria JE, Appoo JJ, Makaroun MS, et al. Endovascular stent grafting versus open surgical repair of descending thoracic aortic aneurysms in low-risk patients: A multicenter comparative trial. J Thorac Cardiovasc Surg. 2007;133:369–377. [CrossRef]
- Farber MA, et al. Five-year outcomes with conformable GORE TAG endoprosthesis used in traumatic aortic transections. Ann Thorac Surg. 2022;113(5):1536–1542. [CrossRef]
- Coselli JS, LeMaire SA, et al. Cerebrospinal fluid drainage reduces paraplegia after thoracoabdominal aortic aneurysm repair: Results of a randomized clinical trial. J Vasc Surg. 2002;35(4):631–639.
- Son SA, Jung H, et al. Long-term outcomes of intervention between open repair and endovascular aortic repair for descending aortic pathologies: A propensity-matched analysis. BMC Surg. 2020;20:266. [CrossRef]
- Parsa CJ, Schroder JN, Daneshmand MA, et al. Midterm results for endovascular repair of complicated acute and chronic type B aortic dissection. Ann Thorac Surg. 2010;89:97–102.
- Böckler D, Schumacher H, Ganten M. Complications after endovascular repair of acute symptomatic and chronic expanding Stanford type B aortic dissections. J Thorac Cardiovasc Surg. 2006;132:361–368. [CrossRef]
- Zhang L, Zhao Z, et al. Reintervention after endovascular repair for aortic dissection: A systematic review and meta-analysis. J Thorac Cardiovasc Surg. 2016;152(5):1279–1288.e3.
- Takagi H, Umemoto T, ALICE (All-Literature Investigation of Cardiovascular Evidence) Group. Negative association of diabetes with thoracic aortic dissection and aneurysm. Angiology. 2016;67(3):229–236. [CrossRef]
- Theivacumar NS, Stephenson MA, Mistry H, et al. Diabetics are less likely to develop thoracic aortic dissection: A 10-year single-center analysis. Ann Vasc Surg. 2014;28:427–432. [CrossRef]
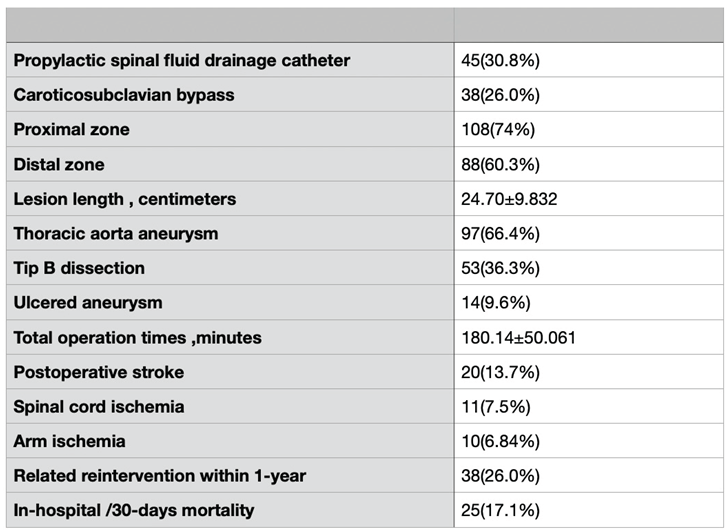 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




