Submitted:
01 April 2025
Posted:
02 April 2025
You are already at the latest version
Abstract
Keywords:
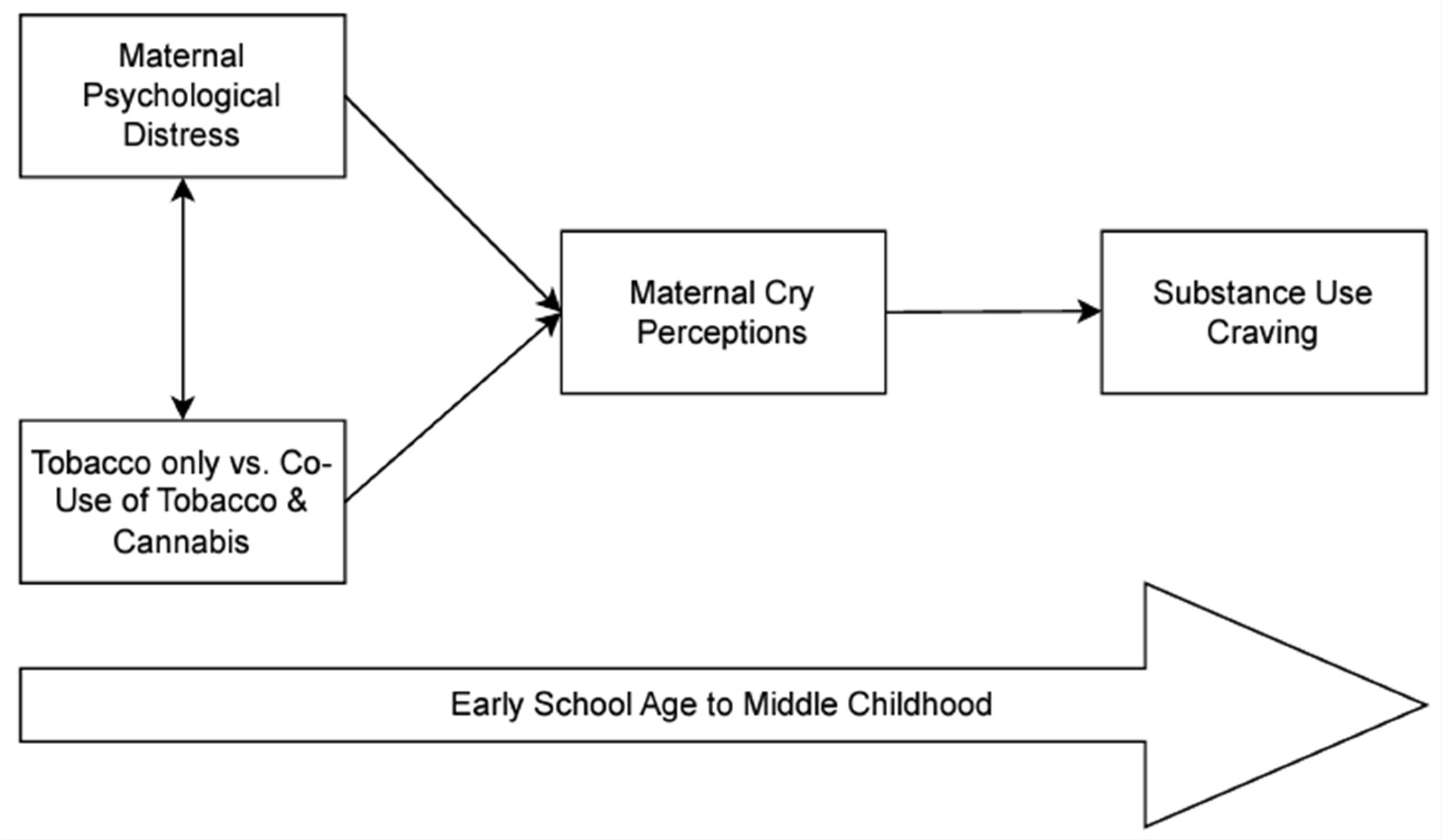
1. Introduction
1.1. Tobacco and Cannabis Cravings
1.2. Maternal Tobacco and Cannabis Use and Maternal Negative Affect
1.3. Maternal Tobacco and Cannabis Use, Negative Affect and Responsiveness to Infant Signals
2. Materials and Methods
2.1. Participants
2.2. Procedures
2.3. Measures
2.3.1. Depressive Symptoms
2.3.2. Anger/Hostility
2.3.3. Substance Use
2.3.4. Maternal Perceptions of Infant Cries
2.3.5. Tobacco and Cannabis Craving
2.4. Missing Data
2.5. Analytic Plan
3. Results
3.1. Preliminary Analyses
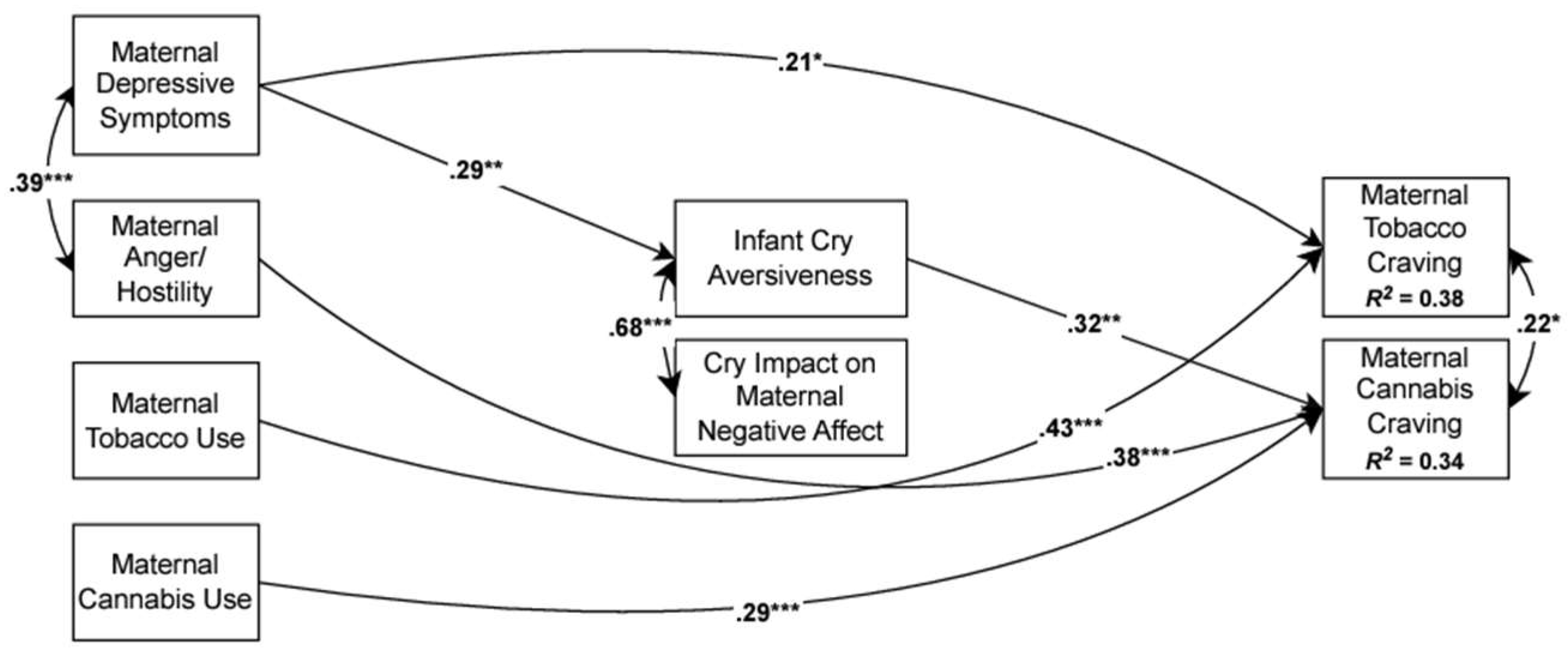
3.2. Primary Analyses
3.2.1. Overall Model
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| TLFB | Timeline Followback Interview |
| BSI | Brief Symptom Inventory |
| BPAQ | Buss-Perry Aggression Questionnaire |
| QSU-4 | Questionnaire of Smoking Urges-4 |
| RMSEA | Root mean square error or approximation |
| SRMR | Standardized root mean square residual |
| CFI | Comparative fit index |
References
- Cornelius, M.E. , Loretan, C.G., Jamal, A., et al. (2023). Tobacco product use among adults – United States, 2021. Morbidity and Mortality Weekly Report, 72(18), 475–483.
- Substance Abuse and Mental Health Services Administration. (2022). Key substance use and mental health indicators in the United States: Results from the 2021 National Survey on Drug Use and Health (HHS Publication No. PEP22-07-01-005, NSDUH Series H-57). Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/data/report/2021-nsduh-annual-national-report.
- Monte, A. A., Zane, R. D., & Heard, K. J. (2015). The implications of marijuana legalization in Colorado. JAMA, 313(3), 241–242.
- Calvigioni, D., Hurd, Y. L., Harkany, T., & Keimpema, E. (2014). Neuronal substrates and functional consequences of prenatal cannabis exposure. European Child & Adolescent Psychiatry, 23(10), 931–941. [CrossRef]
- Mehmedic, Z., Chandra, S., Slade, D., Denham, H., Foster, S., Patel, A. S., Ross, S. A., Khan, I. A., & ElSohly, M. A. (2010). Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. Journal of Forensic Sciences, 55(5), 1209–1217. [CrossRef]
- El Marroun, H., Tiemeier, H., Jaddoe, V.W., Hofman, A., Mackenbach, J.P., Steegers, E.A., Verhulst, F. C., van den Brink, W., & Huizink, A. C. (2008). Demographic, emotional and social determinants of cannabis use in early pregnancy: The Generation R study. Drug Alcohol Dependance, 98(3), 218–226. [CrossRef]
- U.S. Department of Health and Human Services. The Health Consequences of Smoking—50 Years of Progress: A Report of the Surgeon General. Atlanta (GA): U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2014.
- Passey, M. E., Sanson-Fisher, R. W., D'Este, C. A., & Stirling, J. M. (2014). Tobacco, alcohol and cannabis use during pregnancy: clustering of risks. Drug and Alcohol Dependence, 134, 44–50. [CrossRef]
- Serre, F., Fatseas, M., Swendsen, J. & Auriacombe, M. (2015). Ecological momentary.
- assessment in the investigation of craving and substance use in daily life: A systematic review. Drug and Alcohol Dependence, 148, 1-20. [CrossRef]
- Serre, F., Fatseas, M., Denis, C., Swendsen, J., & Auriacombe, M. (2018). Predictors of craving and substance use among patients with alcohol, tobacco, cannabis or opiate addictions: Commonalities and specificities across substances. Addictive Behaviors, 83, 123-129.
- Shiyko, M., Naab, P., Shiffman, S. & Li, R. (2014). Modeling complexity of EMA data: Time-varying lagged effects of negative affect on smoking urges for subgroups of nicotine addiction. Nicotine & Tobacco Research, 16(Supple.2), 144-150.
- Epstein, D.H., Willner-Reid, J., Vahabzadeh, M., Mezghanni, M., Lin, J.L., & Preston, K. L. (2009). Real-time electronic diary reports of cue exposure and mood in the hours before cocaine and heroin craving and use. Archives of General Psychiatry, 66, 88-94.
- Krahn, D.D., Bohn, M.J., Henk, H.J., Gorssman, J.L., & Gosnell, B. (2005). Patterns of urges during early abstinence in alcohol-dependent subjects. The American Journal on Addictions, 14(3), 248-255.
- Trujillo, M. A., Khoddam, R., Greenberg, J. B., Dyal, S. R., Ameringer, K. J., Zvolensky, M. J., & Leventhal, A. M. (2017). Distress tolerance as a correlate of tobacco dependence and motivation: Incremental relations over and above anxiety and depressive symptoms. Behavioral Medicine, 43 (2), 120-128. [CrossRef]
- Perkins, K.A., Karelitz, J.L., Giedgowd, C.E., & Conklin, C. A. (2013). Negative mood effects on craving to smoke in women versus men. Addictive Behaviors, 38(2), 1527-1531. [CrossRef]
- Heishman, S.J., Evans, R.J., Singleton, E.G., Levin, K.H., Copersino, M.L., & Gorelick, D.A. (2009). Reliability and validity of a short form of the Marijuana Craving Questionnaire. Drug and Alcohol Dependence, 102 (1-3), 35-40. [CrossRef]
- Swendsen, J., Ben-Zeev, D., & Granholm, E. (2011). Real-time electronic ambulatory monitoring of substance use and symptom expression in schizophrenia. The American Journal of Psychiatry, 168(2), 202-209. [CrossRef]
- Ludman, E.J., McBride, C.M., Nelson, J.C., Curry, S.J., Grothaus, L.C., Lando, H.A., & Pirie, P.L. (2000). Stress, depressive symptoms, and smoking cessation among pregnant women. Health Psychology, 13, 149-155. [CrossRef]
- Munafò, M.R., Heron, Jon, & Araya, R. (2008). Smoking patterns during pregnancy and postnatal period and depressive symptoms. Nicotine and Tobacco Research, 10, 1620. [CrossRef]
- Goodwin, R.D., Zhu, J., Heisler, Z., et al. (2020). Cannabis use during pregnancy in the United States: The role of depression. Drug & Alcohol Dependence; 210,107881. [CrossRef]
- Young-Wolff, K.C., Sarovar, V., Tucker, L.Y., et al. (2020). Association of depression, anxiety, and trauma with cannabis use during pregnancy. JAMA Network Open; 3(2),e1921333.
- Level, R., Shisler, S., Seay, D., Ivanova, M., Kelm, M., Eiden, R. D., & Schuetze, P. (2021). Within- and between-family transactions of maternal depression, parenting, and child engagement in the first two years of life: Role of prenatal maternal risk and tobacco use. Depression and Anxiety, 38(12), 1279-1288. [CrossRef]
- Eiden, R. D., Leonard, K. E., Colder, C. R., Homish, G. G., Schuetze, P., Gray, T. R., & Huestis, M. A. (2011). Anger, hostility, and aggression as predictors of persistent smoking during pregnancy. Journal of studies on alcohol and drugs, 72(6), 926–932.
- Schuetze, P., Eiden, R.D., Colder, C., R., Huestis, M. & Leonard, K. (2018). Prenatal risk and infant regulation: Indirect Pathways via Fetal Growth, Prenatal Stress and Maternal Aggression/Hostility. Child Development, 89(2), s e123–e13. [CrossRef]
- Ostlund, B., Perez-Edgar, K. E., Shisler, S., Terrell, S., Godleski, S., Schuetze, P. & Eiden, R. D. (2021). Prenatal substance exposure and maternal hostility from pregnancy to toddlerhood: Associations with temperament profiles at 16-months of age. Development and Psychopathology, 33, 1566-1583. [CrossRef]
- Suchman, N.E., DeCoste, C, Castiglion, N., McMahon, T.J., Rounsaville, B. & Mayes, L. (2010). The Mothers and Toddlers Program, an attachment-based parenting intervention for substance using women: Post-treatment results from a randomized clinical pilot. Attachment & Human Development, 12, 483-504. [CrossRef]
- Punamäki, R. L., Flykt, M., Belt, R., & Lindblom, J. (2021). Maternal substance use disorder predicting children's emotion regulation in middle childhood: the role of early mother-infant interaction. Heliyon, 7(4), e06728. [CrossRef]
- Landi, N., Montoya, J., Kober, H., Rutherford, H. J., Mencl, W. E., Worhunsky, P. D., Potenza, M. N., & Mayes, L. C. (2011). Maternal neural responses to infant cries and faces: relationships with substance use. Frontiers in Psychiatry, 2, 32. [CrossRef]
- Schuetze, P. , Zeskind, P. S., & Eiden, R. D. (2003). The perceptions of infant distress signals varying in pitch by cocaine-using mothers. Infancy, 4, 65-83.
- Rutherford, H. J., & Mayes, L. C. (2017). Parenting and addiction: Neurobiological insights. Current Opinion in Psychology, 15, 55–60.
- Brunton, P.J., & Russell, J.A.. (2010). Endocrine induced changes in brain function during pregnancy. Brain Research, 1364,198–215. [CrossRef]
- Mackie, K. (2008). Signaling via CNS cannabinoid receptors. Molecular and Cellular Endocrinology, 286(1-2 Suppl 1), S60–S65. [CrossRef]
- Schuetze P., & Zeskind P. S. (2001). Relations between women's depressive symptoms and perceptions of infant distress signals varying in pitch. Infancy, 2, 483–499.
- Esposito, G., Manian, N., Truzzi, A., & Bornstein, M. H. (2017). Response to infant cry in clinically depressed and non-depressed mothers. PloS One, 12(1), e0169066.
- Donovan, W. L., Leavitt L. A., & Walsh R. O. (1998). Conflict and depression predict maternal sensitivity to infant cries. Infant Behavior & Development, 21, 505–517. [CrossRef]
- Derogatis, L. R. (1993). BSI brief symptom inventory: Administration, scoring, and procedures manual (4th ed.). Minneapolis, MN: National Computer Systems.
- Buss, A. H., & Perry, M. (1992). The aggression questionnaire. Journal of personality and social psychology, 63(3), 452–459.
- Sobell, L. C. , & Sobell, M. B. (1992). Timeline follow-back: A technique for assessing self-reported alcohol consumption. In R. Z. Litten & J. P. Allen (Eds.), Measuring alcohol consumption: Psychosocial and biochemical methods (pp. 41–72). Humana Press/Springer Nature. [CrossRef]
- Robinson, S. M., Sobell, L. C., Sobell, M. B., & Leo, G. I. (2014). Reliability of the Timeline Followback for cocaine, cannabis, and cigarette use. Psychology of Addictive Behaviors: Journal of the Society of Psychologists in Addictive Behaviors, 28(1), 154–162. [CrossRef]
- Brown, R. A., Burgess, E. S., Sales, S. D., Whiteley, J. A., Evans, D. M., & Miller, I. W. (1998). Reliability and validity of a smoking timeline follow-back interview. Psychology of Addictive Behaviors, 12(2), 101–112.
- Tiffany, S. T., & Drobes, D. J. (1991). The development and initial validation of a questionnaire on smoking urges. British Journal of Addiction, 86(11), 1467-1476.
- Little, R. J. A. (1988). A test of missing completely at random for multivariate data with missing values. Journal of the American Statistical Association 83, 1198–1202.
- Arbuckle, J.L. (1996). Full Information Estimation in the Presence of Incomplete Data.007.
- Muthén, L.K. & Muthén, B.O. (1998-2022). Mplus User’s Guide. Eighth Edition. Los Angeles,CA: Muthén & Muthén.
- MacKinnon, D. P., Lockwood, C. M., & Williams, J. (2004). Confidence limits for the indirect effect: Distribution of the product and resampling methods. Multivariate Behavioral Research, 39(1), 99-128.
- Suchman, N.E., DeCoste, C., Leigh, D., & Borelli J. (2010). Reflective functioning in mothers with drug use disorders: implications for dyadic interactions with infants and toddlers. American Journal of Bioethics, 12(6), 567–585.
- Ashare, R.L., Sinha, R., Lampert, R., Weinberger, A.H., Anderson, G.M., Lavery, M.E., Yanagisawa, K., & McKee, S.A. (2012). Blunted vagal reactivity predicts stress-precipitated tobacco smoking. Psychopharmacology, 220(2), 259–268. [CrossRef]
- Speck, B., Isenhour, J.L., Goa, M.M. et al. (2023). Pregnant women’s autonomic responses to an infant cry predict young infants’ behavioral avoidance during the still-face paradigm. Developmental Psychology, 59(12). [CrossRef]
- Volkow, N.D., Wang, G.J., Fowler, J.S., Tomasi, D., & Telang, F. (2011). Addiction: Beyond dopamine reward circuitry. Proceedings of the National Academy of Sciences, 108, 15037–15042. [CrossRef]
- Marsden, D. G., Loukas, A., Chen, B., Perry, C. L., & Wilkinson, A. V. (2019). Associations between frequency of cigarette and alternative tobacco product use and depressive symptoms: A longitudinal study of young adults. Addictive behaviors, 99, 106078. [CrossRef]
- Nguyen, N., Peyser, N. D., Olgin, J. E., Pletcher, M. J., Beatty, A. L., Modrow, M. F., Carton, T. W., Khatib, R., Djibo, D. A., Ling, P. M., & Marcus, G. M. (2023). Associations between tobacco and cannabis use and anxiety and depression among adults in the United States: Findings from the COVID-19 citizen science study. PloS one, 18(9), e0289058.
- Obisesan, O. H., Mirbolouk, M., Osei, A. D., Orimoloye, O. A., Uddin, S. M. I., Dzaye, O., El Shahawy, O., Al Rifai, M., Bhatnagar, A., Stokes, A., Benjamin, E. J., DeFilippis, A. P., & Blaha, M. J. (2019). Association Between e-Cigarette Use and Depression in the Behavioral Risk Factor Surveillance System, 2016-2017. JAMA network open, 2(12), e1916800. [CrossRef]
- Weinberger, A.H., Chaiton, M.O., Zhu, J., Wall, M.M., Hasin, D.S. & Goodwin, R. D. (20201). Trends in the prevalence of current, daily, and nondaily cigarette smoking and quit ratios by depression status in the U.S.: 2005-2017. American Journal of Preventative Medicine, 58(5), 691-698.
- Ansell, E.B., Laws H.B., Roche M.J., & Sinha R. (2015). Effects of marijuana use on impulsivity and hostility in daily life. Drug and Alcohol Dependence; 148,136–142. [CrossRef]
- Dillon K.H., Van Voorhees E.E., Elbogen E.B., Beckham J.C., Calhoun P.S., Brancu M. & Yoash-Gantz R.E. (2021). Cannabis use disorder, anger, and violence in Iraq/Afghanistan-era veterans. Journal of Psychiatric Research, 138, 375–379. [CrossRef]
- Pahl K., Brook J.S., & Koppel J. (2011). Trajectories of marijuana use and psychological adjustment among urban African American and Puerto Rican women. Psychological Medicine, 41(8), 1775–1783. [CrossRef]
- Wycoff, A. M., Metrik, J., & Trull, T. J. (2018). Affect and cannabis use in daily life: A review and recommendations for future research. Drug and Alcohol Dependence, 191, 223–233. [CrossRef]
- Chase H. W., Moses-Kolko E. L., Zevallos C., Wisner K. L., & Phillips M. L. (2014). Disrupted posterior cingulate—amygdala connectivity in postpartum depressed women as measured with resting BOLD fMRI. Social Cognitive and Affective Neuroscience, 9(8), 1069–1075. [CrossRef]
- Laurent, H. K., & Ablow J. C. (2012). A cry in the dark: depressed mothers show reduced neural activation to their own infant’s cry. Social Cognitive and Affective Neuroscience, 7(2), 125–134. [CrossRef]
- Cohn, J.F., Campbell, S.B., Matias, R., & Hopkins, J. (1990). Face-to-face interactions of postpartum depressed and nondepressed mother-infant pairs at 2 months. Developmental Psychology, 26(1), 15-23. [CrossRef]
- Graham, C.A., & Easterbrooks, M.A. (2000). School-aged children’s vulnerability to depressive symptomatology: The role of attachment security, maternal depressive symptomatology, and economic risk. Developmental Psychopathology, 12(2), 201-213. [CrossRef]
- Cornelius, M.D. & Day, N. (2009). Developmental consequences of prenatal tobacco exposure. Current Opinion in Neurology, 22, 121-125. [CrossRef]
- Schuetze, P., Zhao, J., Eiden, R.D., & Shisler, S. (2019). Prenatal Exposure to Tobacco and Marijuana and Child Autonomic Regulation and Reactivity: An Analysis of Indirect Pathways via Maternal Psychopathology and Parenting. Developmental Psychobiology,6, 1022–1034.
- Loman, M. M., & Gunnar, M. R., (2010). Early experience and the development of stress reactivity and regulation in children. Neuroscience and Biobehavioral Reviews, 34(6), 867–876.
- Stams, G. J., Juffer, F., & van IJzendoorn, M. H. (2002). Maternal sensitivity, infant attachment, and temperament in early childhood predict adjustment in middle childhood: the case of adopted children and their biologically unrelated parents. Developmental Psychology, 38(5), 806–821. [CrossRef]
- Tronick, E., & Beeghly, M. (2011). Infants' meaning-making and the development of mental health problems. The American Psychologist, 66(2), 107–119. [CrossRef]
| M | SD | Range | |
|---|---|---|---|
| Maternal Substance Use | |||
| Cigarettes Per Day | 6.77 | 5.86 | 20.77 |
| Joints Per Day | 1.40 | 3.34 | 17.23 |
| Maternal Psychological Distress | |||
| BPAQ Score (Anger/Hostility) | 2.42 | 0.71 | 3.69 |
| BSI Subscale Score (Depressive Symptoms) | 0.62 | 0.71 | 2.83 |
| Maternal Cry Perception Ratings | |||
| Cry Impact on Negative Affect | 2.93 | 1.05 | 4.00 |
| Cry Aversiveness | 3.32 | 0.98 | 4.00 |
| Craving Scale Score | |||
| Tobacco | 3.88 | 3.57 | 10.00 |
| Cannabis | 2.04 | 2.21 | 8.75 |
| Demographics | |||
| Parity | 1.08 | 1.46 | 8 |
| Maternal Age (years) | 24.41 | 5.32 | 21 |
| 1 | 2 | 3 | 4 | 5 | 6 | |
|---|---|---|---|---|---|---|
| 1. Co-Use vs. Tobacco Use | -- | |||||
| 2. Maternal Stress | -- | |||||
| 3. Maternal Depression | .39*** | -- | ||||
| 4. Cry Impact on Negative Affect | .07 | .19 | -- | |||
| 5. Cry Aversiveness | .13 | .28** | .69*** | -- | ||
| 6. Tobacco Craving | .42*** | .23* | .01 | 20 | -- | |
| 7. Cannabis Craving | -.03 | .35*** | .16 | .20 | .20* |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




