Submitted:
16 February 2024
Posted:
19 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusion
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mattiuzzi, C.; Sanchis-Gomar, F.; Lippi, G. Concise update on colorectal cancer epidemiology. Ann Transl Med. 2019 Nov;7(21):609–609. [CrossRef]
- Baidoun F, Elshiwy K, Elkeraie Y, Merjaneh Z, Khoudari G, Sarmini MT, et al. Colorectal Cancer Epidemiology: Recent Trends and Impact on Outcomes. Curr Drug Targets. 2021 Nov 19. [CrossRef]
- Morgan E, Arnold M, Gini A, Lorenzoni V, Cabasag CJ, Laversanne M, et al. Global burden of colorectal cancer in 2020 and 2040: incidence and mortality estimates from GLOBOCAN. Gut. 2023 Feb 1;72(2):338–44. [CrossRef]
- Sawicki T, Ruszkowska M, Danielewicz A, Niedźwiedzka E, Arłukowicz T, Przybyłowicz KE. A Review of Colorectal Cancer in Terms of Epidemiology, Risk Factors, Development, Symptoms and Diagnosis. Cancers (Basel). 2021 May 1;13(9). [CrossRef]
- Bluegrass Coalition for Colorectal Screening; KMA Cancer Committee. Colorectal cancer facts. J Ky Med Assoc. 2005 Mar;103(3of):118.
- Kim SE, Paik HY, Yoon H, Lee JE, Kim N, Sung MK. Sex- and gender-specific disparities in colorectal cancer risk. World J Gastroenterol. 2015 May 7;21(17):5167–75. [CrossRef]
- Schmuck R, Gerken M, Teegen EM, Krebs I, Klinkhammer-Schalke M, Aigner F, et al. Gender comparison of clinical, histopathological, therapeutic and outcome factors in 185,967 colon cancer patients. Langenbecks Arch Surg. 2020 Feb 1;405(1):71–80. [CrossRef]
- Keum NN, Giovannucci E. Global burden of colorectal cancer: emerging trends, risk factors and prevention strategies. Nat Rev Gastroenterol Hepatol. 2019 Dec 1;16(12):713–32. [CrossRef]
- Amersi F, Agustin M, Ko CY. Colorectal cancer: epidemiology, risk factors, and health services. Clin Colon Rectal Surg. 2005 Aug;18(3):133–40. [CrossRef]
- Thélin C, Sikka S, Thélin C, Sikka S. Epidemiology of Colorectal Cancer — Incidence, Lifetime Risk Factors Statistics and Temporal Trends. Screening for Colorectal Cancer with Colonoscopy. 2015 Dec 2, Editor Rajunor Ettarh, IntechOpen.
- Rawla P, Sunkara T, Barsouk A. Epidemiology of colorectal cancer: incidence, mortality, survival, and risk factors. Prz Gastroenterol. 2019;14(2):89–103. [CrossRef]
- Goodarzi E, Beiranvand R, Naemi H, Momenabadi V, Khazaei Z. Worldwide Incidence and Mortality of Colorectal Cancer and Human Development Index (HDI): An Ecological Study. World Cancer Research Journal. 2019;6.
- Peterse EFP, Meester RGS, Siegel RL, Chen JC, Dwyer A, Ahnen DJ, et al. The impact of the rising colorectal cancer incidence in young adults on the optimal age to start screening: Microsimulation analysis I to inform the American Cancer Society colorectal cancer screening guideline. Cancer. 2018 Jul 15;124(14):2964–73. [CrossRef]
- Vuik FER, Nieuwenburg SAV, Bardou M, Lansdorp-Vogelaar I, Dinis-Ribeiro M, Bento MJ, et al. Increasing incidence of colorectal cancer in young adults in Europe over the last 25 years. Gut. 2019;68(10). [CrossRef]
- Simon, K. Colorectal cancer development and advances in screening. Clin Interv Aging [Internet]. 2016 Jul 19;11:967–76. [CrossRef]
- Moiel D, Thompson J. Early detection of colon cancer-the kaiser permanente northwest 30-year history: how do we measure success? Is it the test, the number of tests, the stage, or the percentage of screen-detected patients? Perm J. 2011 Dec.
- Moreno CC, Mittal PK, Sullivan PS, Rutherford R, Staley CA, Cardona K, et al. Colorectal Cancer Initial Diagnosis: Screening Colonoscopy, Diagnostic Colonoscopy, or Emergent Surgery, and Tumor Stage and Size at Initial Presentation. Clin Colorectal Cancer. 2016 Mar 1;15(1):67–73. [CrossRef]
- Thompson MR, O’Leary DP, Flashman K, Asiimwe A, Ellis BG, Senapati A. Clinical assessment to determine the risk of bowel cancer using Symptoms, Age, Mass and Iron deficiency anaemia (SAMI). Br J Surg. 2017 Sep 1;104(10):1393–404. [CrossRef]
- Hreinsson JP, Jonasson JG, Bjornsson ES. Bleeding-related symptoms in colorectal cancer: a 4-year nationwide population-based study. Aliment Pharmacol Ther. 2014 Jan 1;39(1):77–84. [CrossRef]
- Yoo RN, Cho HM, Kye BH. Management of obstructive colon cancer: Current status, obstacles, and future directions. World J Gastrointest Oncol. 2021 Dec 12;13(12):1850. [CrossRef]
- Muldoon, RL. Bowel Obstructions: Malignant Large Bowel Obstruction. Clin Colon Rectal Surg. 2021 Jul 1;34(4):251. [CrossRef]
- Baer C, Menon R, Bastawrous S, Bastawrous A. Emergency Presentations of Colorectal Cancer. Surgical Clinics of NA. 2017;97:529–45. [CrossRef]
- Barnett, A.; Cedar, A.; Siddiqui, F.; Herzig, D.; Fowlkes, E.; Thomas, C.R. Colorectal Cancer Emergencies. J. Gastrointest. Cancer 2013, 44, 132–142. [Google Scholar] [CrossRef] [PubMed]
- Gunnarsson H, Holm T, Ekholm A, Olsson LI. Emergency presentation of colon cancer is most frequent during summer. Colorectal Disease. 2011 Jun 1;13(6):663–8. [CrossRef]
- Elmessiry MM, Mohamed EA. Emergency curative resection of colorectal cancer, do it with caution. A comparative case series. Annals of Medicine and Surgery. 2020 Jul 1;55:70–6. [CrossRef]
- Pavlidis TE, Marakis G, Ballas K, Rafailidis S, Psarras K, Pissas D, et al. Does emergency surgery affect resectability of colorectal cancer? Acta Chir Belg. 2008;108(2):219–25. [CrossRef]
- Costa G, Tomassini F, Tierno S, Venturini L, Frezza B, Cancrini G, Mero A, Lepre L. Emergency colonic surgery: analysis of risk factors predicting morbidity and mortality. Chir Ital. 2009;61(5-6):565-71.
- Sjo OH, Larsen S, Lunde OC, Nesbakken A. Short term outcome after emergency and elective surgery for colon cancer. Colorectal Disease. 2009;11(7):733–9. [CrossRef]
- Bayar B, Yilmaz KB, Akinci M, Şahin A, Kulaçoʇlu H. An evaluation of treatment results of surgery in emergency versus elective colorectal cancer patients. Turk J Surg. 2016;32(1):011–7. [CrossRef]
- Alvarez JA, Baldonedo RF, Bear IG, Truán N, Pire G, Alvarez P. Presentation, treatment, and multivariate analysis of risk factors for obstructive and perforative colorectal carcinoma. The American Journal of Surgery. 2005 Sep 1;190(3):376–82. [CrossRef]
- Bass G, Fleming C, Conneely J, Martin Z, Mealy K. Emergency first presentation of colorectal cancer predicts significantly poorer outcomes: a review of 356 consecutive Irish patients. Dis Colon Rectum. 2009 Apr;52(4):678–84. [CrossRef]
- Biondo S, Kreisler E, Millan M, Marti-Rague J, Fraccalvieri, D, Golda T, De Oca J, Osorio A, Fradera R, Salazar R, Rodriguez-Moranta F, Sanjuan, X. Long-term results of emergency surgery for colon cancer compared with elective surgery. Cir Esp. 2007;82(2):89-98. [CrossRef]
- Bufill, JA. Colorectal cancer: Evidence for distinct genetic categories based on proximal or distal tumor location. Ann Intern Med. 1990 Nov 15;113(10):779–88. [CrossRef]
- Gervaz P, Bucher P, Morel P. Two colons-two cancers: Paradigm shift and clinical implications. J Surg Oncol. 2004 Dec 15;88(4):261–6. [CrossRef]
- Iacopetta, B. Are there two sides to colorectal cancer? Int J Cancer. 2002;101(5):403–8. [CrossRef]
- Stintzing S, Tejpar S, Gibbs P, Thiebach L, Lenz HJ. Understanding the role of primary tumour localisation in colorectal cancer treatment and outcomes. Eur J Cancer. 2017 Oct 1;84:69–80. [CrossRef]
- Topdaği Ö, Timuroglu A. Eighteen Years’ Retrospective Review of Colorectal Cancer Cases in Eastern Population. Eurasian J Med. 2018 Feb 1;50(1):19. [CrossRef]
- Dubé C, Rostom A, Lewin G, Tsertsvadze A, Barrowman N, Code C, et al. The use of aspirin for primary prevention of colorectal cancer: A systematic review prepared for the U.S. Preventive Services Task Force. Ann Intern Med. 2007 Mar 6;146(5):365–75. [CrossRef]
- Gao Z, Guo B, Gao R, Zhu Q, Qin H. Microbiota disbiosis is associated with colorectal cancer. Front Microbiol. 2015;6(FEB). [CrossRef]
- Kohoutova D, Smajs D, Moravkova P, Cyrany J, Moravkova M, Forstlova M, et al. Escherichia coli strains of phylogenetic group B2 and D and bacteriocin production are associated with advanced colorectal neoplasia. BMC Infect Dis. 2014 Dec 24;14(1). [CrossRef]
- Zhang Y, Hoffmeister M, Weck M, Chang-Claude J, Brenner H. Helicobacter pylori Infection and Colorectal Cancer Risk: Evidence From a Large Population-based Case-Control Study in Germany. Am J Epidemiol. 2012;175(5):441-50. [CrossRef]
- Flemer B, Lynch DB, Brown JMR, Jeffery IB, Ryan FJ, Claesson MJ, et al. Tumour-associated and non-tumour-associated microbiota in colorectal cancer. Gut. 2017;66(4):633-643. [CrossRef]
- Nitsche U, Stögbauer F, Späth C, Haller B, Wilhelm D, Friess H, et al. Right sided colon cancer as a distinct histopathological subtype with reduced prognosis. Dig Surg. 2016;33(2):157-63. [CrossRef]
- Sinicrope F, Mahoney M, Yoon H, Smyrk T, Thibodeau S, Goldberg R, Nelson G, Sargent D, Alberts S, Alliance for Clinical Trials in Oncology. Analysis of molecular markers by anatomic tumor site in stage III colon carcinomas from adjuvant chemotherapy trial NCCTG N0147 (Alliance). Clin Cancer Res; 2015;21(23):5294-304. [CrossRef]
- Mouradov D, Sloggett C, Jorissen R, Love C, Li S, Burgess A, Arango D, Strausberg R, Buchanan D, Wormald S, O’Connor L, Wilding J, Bicknell D, Tomlinson I, Bodmer W, Mariadson J, Sieber O. Colorectal cancer cell lines are representative models of the main molecular subtypes of primary cancer. Cancer Res. 2014;74(12):3238-47. [CrossRef]
- Sugai T, Habano W, Nakamura SI, Sato H, Uesugi N, Takahashi H, et al. Genetic alterations in DNA diploid, aneuploid and multiploid colorectal carcinomas identified by the crypt isolation technique. Int J Cancer; 2000;88(4):614-9. [CrossRef]
- Missiaglia E, Jacobs B, D’ario G, Di Narzo A, Soneson C, Budinska E, Popovici V, Vecchione L, Gerster S, Pan Y, Roth A, Klingbiel D, Bosman F, Delorenzi M, Tejpar S. Distal and proximal colon cancers differ in terms of molecular, pathological, and clinical features. Ann Oncol. 2014;25(10):1995-2001. [CrossRef]
- Shen H, Yang J, Huang Q, Jiang M, Tan Y, Fu J, Zhu L, Fang X, Yuan Y. Different treatment strategies and molecular features between right-sided and left-sided colon cancers. World J Gastroenterol. 2015;21(21):6470-6478. [CrossRef]
- Alius C, Cirstoveanu CG, Badiu CD, Ardeleanu V, Dumitru VA. Immunohistochemical pattern– a prognostic factor for synchronous gastrointestinal cancer. Journal of Mind and Medical Sciences. 2020 Sep 29;7(2):250–6. [CrossRef]
- Hemminki K, Santi I, Weires M, Thomsen H, Sundquist J, Bermejo JL. Tumor location and patient characteristics of colon and rectal adenocarcinomas in relation to survival and TNM classes. BMC Cancer. 2010 Dec 21;10. [CrossRef]
- Loupakis F, Yang D, Yau L, Feng S, Cremolini C, Zhang W, Maus M, Antoniotti C, Langer C, Scherer S, Muller T, Hurwitz H, Saltz L, Falcone A, Lenz H. J Natl Cancer Inst. 2015;107(3):dju247.
- Weiss J, Pfau P, O’Connor E, King J, LoConte N, Kennedy G, Smith M. Mortality by stage for right-versus left-sided colon cancer: analysis of surveillance, epidemiology, and end results – Medicare data. J Clin Oncol. 2011;29(33):4401-9. [CrossRef]
- Morris VK, Kennedy EB, Baxter NN, Benson AB, Cercek A, Cho M, et al. Treatment of Metastatic Colorectal Cancer: ASCO Guideline. J Clin Oncol. 2023 Jan 20;41(3):678–700. [CrossRef]
- Dohrn N, Klein MF. Colorectal cancer: current management and future perspectives. British Journal of Surgery. 2023 Sep 6;110(10):1256–9. [CrossRef]
- You YN, Hardiman KM, Bafford A, Poylin V, Francone TD, Davis K, et al. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for the Management of Rectal Cancer. Dis Colon Rectum. 2020 Sep 1;63(9):1191–222. [CrossRef]
- Vogel JD, Felder SI, Bhama AR, Hawkins AT, Langenfeld SJ, Shaffer VO, et al. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for the Management of Colon Cancer. Dis Colon Rectum. 2022 Feb 1;65(2):148–77. [CrossRef]
- Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S. Standardized surgery for colonic cancer: complete mesocolic excision and central ligation--technical notes and outcome. Colorectal Dis. 2009;11(4):354–64. [CrossRef]
- Heald R, Ryall, R. Recurrence and survival after total mesorectal excision for rectal cancer. Lancet. 1986 Jun 28;1(8496):1479-82. [CrossRef]
- Liscu H, Miron A, Rusea A, Oprea A, Mitre R, Herdea A, et al. Short-Course Radiotherapy versus Long-Course Radio-Chemotherapy as Neoadjuvant Treatment for Locally Advanced Rectal Cancer: Meta-Analysis from a Toxicity Perspective. Maedica (Bucur). 2021 Sep 15;16(3):382. [CrossRef]
- Alexandrescu ST, Dumitru AV, Babiuc RD, Costea RV. Assessment of clinical and pathological complete response after neoadjuvant chemoradiotherapy in rectal adenocarcinoma and its therapeutic implications. Romanian Journal of Morphology and Embryology. 2021 Apr 1;62(2):411–25. [CrossRef]
- Morton D, Seymour M, Magill L, Handley K, Glasbey J, Glimelius B, et al. Preoperative Chemotherapy for Operable Colon Cancer: Mature Results of an International Randomized Controlled Trial. J Clin Oncol. 2023 Mar 10;41(8):1541–52. [CrossRef]
- Baxter NN, Kennedy EB, Bergsland E, Berlin J, George TJ, Gill S, et al. Adjuvant Therapy for Stage II Colon Cancer: ASCO Guideline Update. J Clin Oncol. 2022 Mar 10;40(8):892–910. [CrossRef]
- Liscu HD, Liscu BR, Mitre R, Anghel IV, Antone-Iordache IL, Balan A, et al. The Conditioning of Adjuvant Chemotherapy for Stage II and III Rectal Cancer Determined by Postoperative Pathological Characteristics in Romania. Medicina 2023, Vol 59, Page 1224. 2023 Jun 29;59(7):1224. [CrossRef]
- Chalabi M, Fanchi LF, Dijkstra KK, Van den Berg JG, Aalbers AG, Sikorska K, et al. Neoadjuvant immunotherapy leads to pathological responses in MMR-proficient and MMR-deficient early-stage colon cancers. Nat Med. 2020 Apr 1;26(4):566–76. [CrossRef]
- Cercek A, Lumish M, Sinopoli J, Weiss J, Shia J, Lamendola-Essel M, et al. PD-1 Blockade in Mismatch Repair-Deficient, Locally Advanced Rectal Cancer. N Engl J Med. 2022 Jun 23;386(25):2363–76. [CrossRef]
- Jin Z, Sinicrope FA. Mismatch Repair-Deficient Colorectal Cancer: Building on Checkpoint Blockade. J Clin Oncol. 2022;40(24). [CrossRef]
- Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018 Nov;68(6):394–424. [CrossRef]
- Wong MCS, Huang J, Lok V, Wang J, Fung F, Ding H, et al. Differences in Incidence and Mortality Trends of Colorectal Cancer Worldwide Based on Sex, Age, and Anatomic Location. Clin Gastroenterol Hepatol. 2021 May 1;19(5):955-966.e61. [CrossRef]
| Type of Variables Analyzed | Type of Statistical Test | p-Value |
|---|---|---|
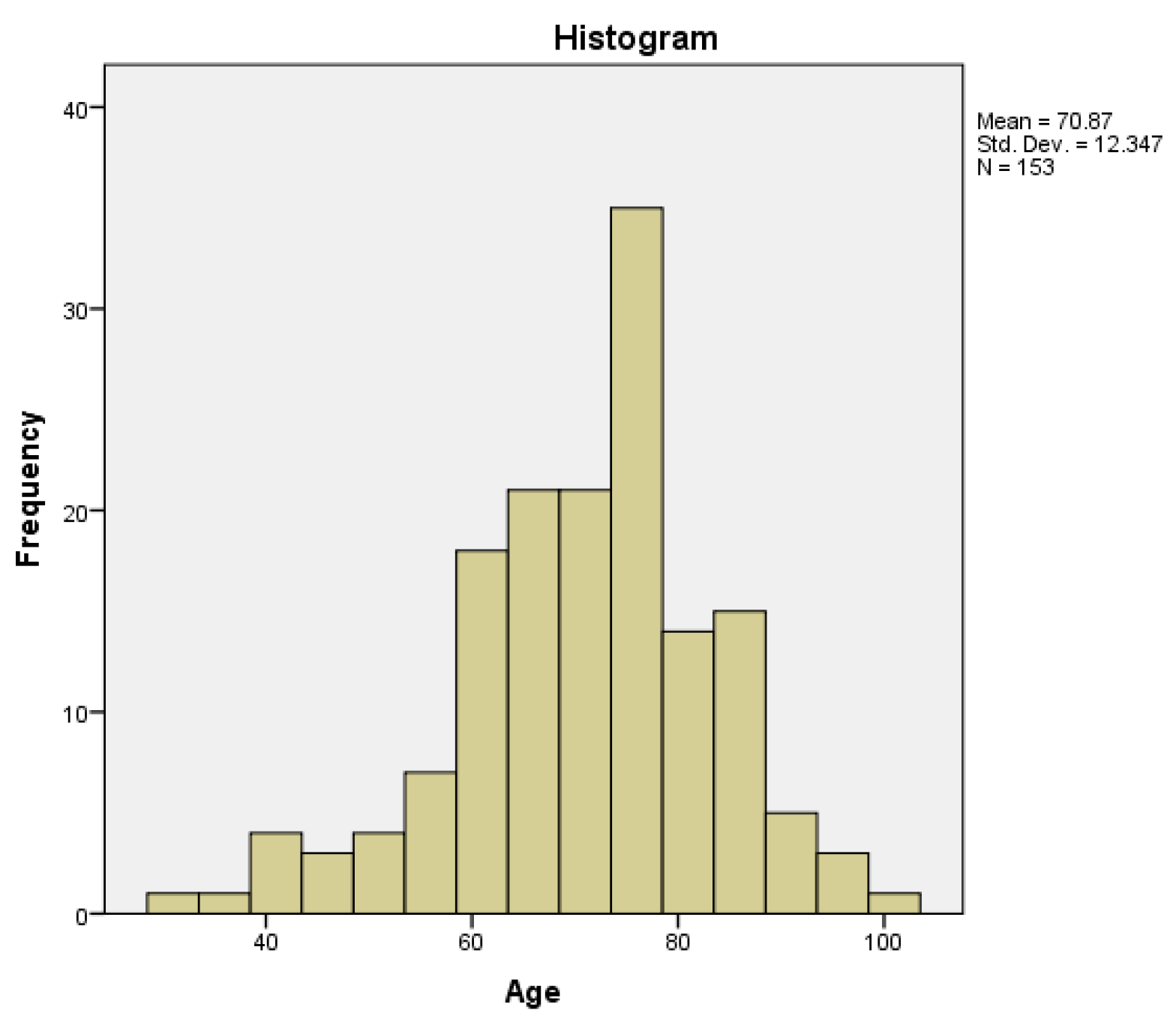
| Emergency vs Age | Two-sample t-test | 0.733 |
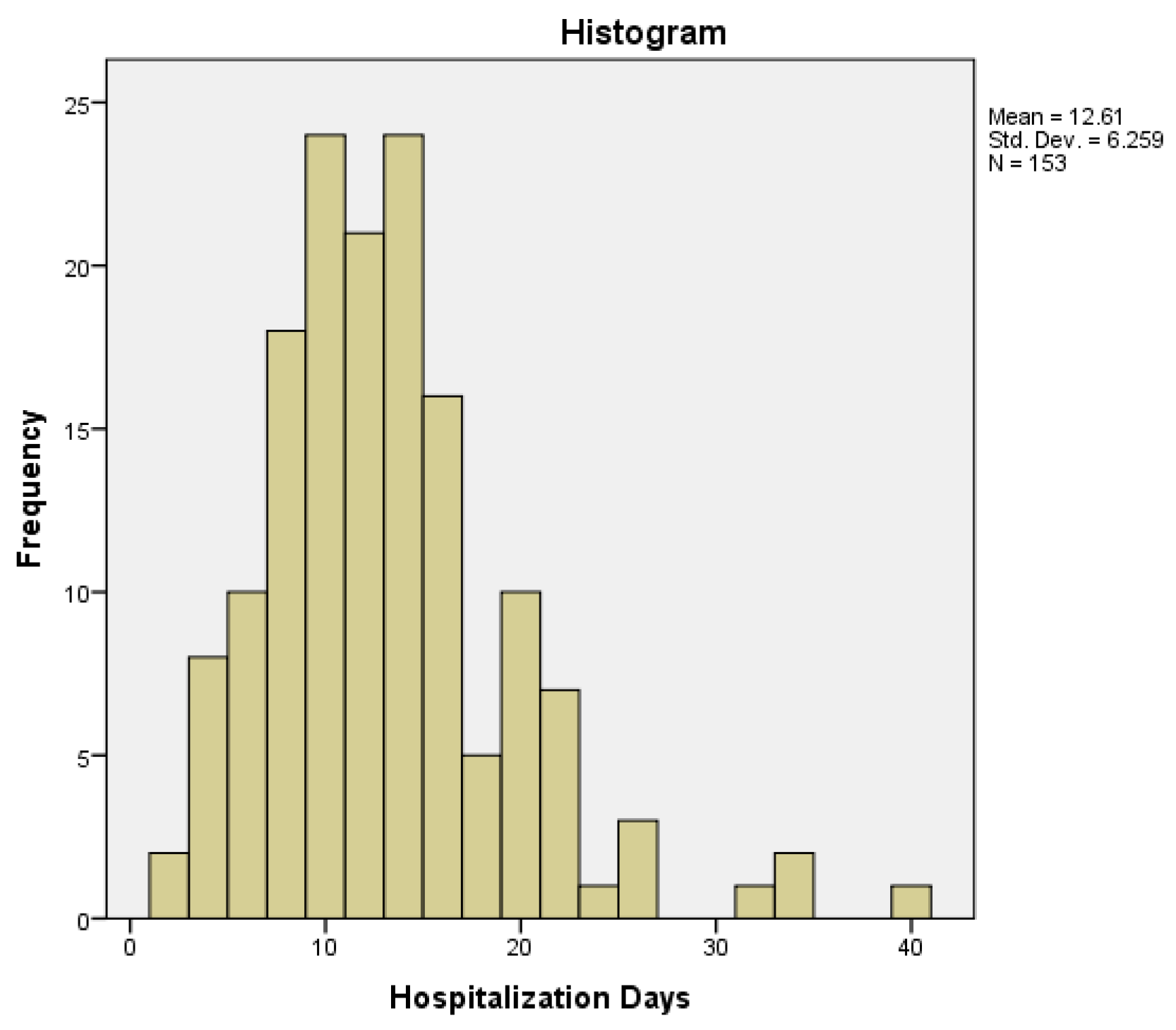
| Emergency vs Hospitalization days | Mann Whitney U test | 0.823 |
| Emergency vs Gender | Chi-square test | 0.414 |
| Emergency vs Urban/Rural | Chi-square test | 0.497 |
| Preoperative CT scan | ||||
|---|---|---|---|---|
| No | Yes | Total | ||
| Emergency procedure | No | 43 | 41 | 84 |
| Yes | 25 | 44 | 69 | |
| Total | 68 | 85 | 153 | |
| Topography | Number of patients | Number of patients by type of surgery (Em=Emergency; El=Elective) | P-value |
|---|---|---|---|
| Ileocecal valve | 13 | Em=7; El=6 | 0.568 |
| Cecum | 3 | El=1; Em=2 | 1.000 |
| Ascending colon | 8 | Em=1; El=7 | 0.074 |
| Hepatic flexure | 6 | Em=1; El=5 | 0.223 |
| Transverse colon | 9 | Em=5; El=4 | 0.732 |
| Splenic flexure | 8 | Em=6; El=2 | 0.141 |
| Descending colon | 9 | Em=4; El=5 | 1.000 |
| Sigmoid colon | 30 | Em=21; El=9 | 0.004 |
| Rectosigmoidian junction | 24 | Em=10; El=14 | 0.824 |
| Superior rectum | 17 | Em=7; El=10 | 0.800 |
| Medium rectum | 9 | Em=2; El=7 | 0.186 |
| Inferior rectum and anus | 17 | Em=3; El=14 | 0.072 |
| Type surgery |
p-value |
||||
|---|---|---|---|---|---|
| Elective | Emergency | Total | |||
|
Topographical segment |
Right colon % within right colon |
24 61.5% |
15 38.5% |
39 100.0% |
0.002 |
|
Left colon % within left colon |
16 34.0% |
31 66.0% |
47 100% |
||
|
Rectum % within rectum |
44 65.7% |
23 34.3% |
67 100% |
||
|
Total % within total |
84 54.9% |
69 45.1% |
153 100% |
||
| Type of surgery | Result of surgical procedure | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Elective | Emergency | Total | p-value | Ostomy | Anastomosis | Neither | Total | p-value | ||
| Type of surgical procedure |
Right hemicolectomy % within |
22 66.7% |
11 33.3% |
33 100% |
0.167 | 8 24.2% |
25 75.8% |
0 | 33 100% |
0.002 |
|
Left hemicolectomy % within |
11 45.8% |
13 54.2% |
24 100% |
0.367 | 10 41.7% |
14 58.3% |
0 | 24 100% |
0.253 | |
|
Segmentary resection of transverse colon % within |
3 23.1% |
10 76.9% |
13 100% |
0.020 | 5 38.5% |
8 61.5% |
0 | 13 100% |
0.440 | |
|
Segmentary resection of sigmoid colon % within |
7 33.3% |
14 66.7% |
21 100% |
0.037 | 14 66.7% |
7 33.3% |
0 | 21 100% |
0.044 | |
|
Rectosigmoid resection % within |
21 65.6% |
11 34.4% |
32 100 |
0.231 |
11 34.4% |
21 65.6% |
0 | 32 100% |
0.046 | |
|
Upward ostomy on sigmoid colon % within |
7 58.3% |
5 41.7% |
12 100% |
1.000 |
7 100% |
0 | 0 | 7 100% |
- | |
|
Abdominoperineal resection % within |
6 75% |
2 25% |
8 100% |
0.295 | 8 100% |
0 | 0 | 8 100% |
- | |
|
Tumoral biopsy % within |
17 70.8% |
7 29.2% |
24 100% |
0.118 | 12 50% |
0 | 12 50% |
24 100% |
- | |
| Number | Age | Gender (M=male, F=female) | Hospitalization days | Emergency (Em)/Elective (El) | Topography of the tumor | Surgical procedure |
|---|---|---|---|---|---|---|
| 1. | 74 | M | 13 | Em | Sigmoid colon | Colectomy with ostomy |
| 2. | 67 | M | 4 | Em | Descending colon | Left hemicolectomy with ostomy |
| 3. | 84 | M | 39 | Em | Transverse colon | Colectomy with ostomy |
| 4. | 63 | M | 12 | Em | Splenic flexure | Colectomy with ostomy |
| 5. | 78 | F | 21 | Em | Colorectal junction | Left rectohemicolectomy with ostomy |
| 6. | 55 | F | 10 | El | Colorectal junction | Rectosigmoid resection with ostomy |
| 7. | 78 | M | 3 | Em | Transverse colon | Extended right hemicolectomy with ileostomy |
| 8. | 59 | M | 6 | Em | Sigmoid colon | Colectomy with ostomy |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




