Submitted:
15 January 2024
Posted:
16 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Description of OLIF51 and LCA surgical procedures
Evaluation of vascular anatomy in supine position on MRI
Intraoperative evaluation of vein anatomy in right decubitus position on enhanced CT
3. Results
Evaluation of vascular anatomy in supine position
Intraoperative evaluation of vein anatomy in right decubitus position
Case presentation
4. Discussion
5. Conclusion
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hodgson, A.R.; Stock, F.E.; Fang, H.S.Y.; et al. Anterior spinal fusion the operative approach and pathological findings in 412 patients with Pott’s disease of the spine. Br J Surg 1960, 48, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Kaneda, K.; Taneichi, H.; Abumi, K.; et al. Anterior decompression and stabilization with the Kaneda device for thoracolumbar burst fractures associated with neurological deficits. J Bone Joint Surg 1997, 79, 69–83. [Google Scholar] [CrossRef]
- Woods, K.; Billy, J.B.; Hynes, R. Technical description of oblique lateral interbody fusion at L1–L5 (OLIF25) and at L5–S1 (OLIF51) and evaluation of complication and fusion rates. The Spine J 2017, 17, 545–553. [Google Scholar] [CrossRef]
- Graham, R.B.; Wong, A.P.; Liu, J.C. Minimally invasive lateral transpsoas approach to the lumbar spine: pitfalls and complication avoidance. Neurosurg Clin N Am 2014, 25, 219–231. [Google Scholar] [CrossRef] [PubMed]
- Houten, J.K.; Alexandre, L.C.; Nasser, R.; Wollowick, A.L. Nerve injury during the transpsoas approach for lumbar fusion: report of 2 cases. J Neurosurg Spine 2011, 15, 280–284. [Google Scholar] [CrossRef] [PubMed]
- Nalbandian, M.W.; Hoashi, J.S.; Errico, T.J. Variations in the iliolumbar vein during the anterior approach for spinal procedures. Spine 2013, 38, e445–e450. [Google Scholar] [CrossRef] [PubMed]
- Deukmedjian, A.R.; Le, T.V.; Dakwar, E. Movement of abdominal structures on magnetic resonance imaging during positioning changes related to lateral lumbar spine surgery: a morphometric study. J Neurosurg Spine J Neurosurg Spine, 16, 615–615. [Google Scholar] [CrossRef]
- Choi, J.; Rhee, I.; Ruparel, S. Assessment of great vessels for anterior access of L5/S1 using patient positioning. Asian Spine J 2020, 14, 438–444. [Google Scholar] [CrossRef] [PubMed]
- Nagamatsu, M.; Ruparel, S.; Tanaka, M.; et al. Assessment of 3D lumbosacral vascular anatomy for OLIF51 by non-enhanced MRI and CT medical image fusion techniques. Diagnostics 2021, 11, 1744. [Google Scholar] [CrossRef]
- Liu, L.; Liang, Y.; Zhang, H.; et al. Imaging anatomical research on the operative windows of oblique lumbar interbody fusion. Plos one 2016, 29. [Google Scholar] [CrossRef] [PubMed]
- Davis, T.T.; Hynes, R.; Fung, D.A. Retroperitoneal oblique corridor to the L2-S1 intervertebral discs in the lateral position: an anatomic study. J Neurosurg Spine 2014, 21, 785–793. [Google Scholar] [CrossRef] [PubMed]
- Molinares, D.M.; Davis, T.T.; Fung, D.A. Retroperitoneal oblique corridor to the L2-s1 intervertebral discs: an MRI study. J Neurosurg Spine 2016, 24, 248–255. [Google Scholar] [CrossRef] [PubMed]
- Kleeman, T.J.; Michael, A.U.; Clutterbuck, W.B. Laparoscopic anterior interbody fusion at L4-5: an anatomic evaluation and approach classification. Spine 2002, 27, 1390–5. [Google Scholar] [CrossRef] [PubMed]
- Chung, N.S.; Jeon, C.H.; Lee, H.D. Preoperative evaluation of left common iliac vein in oblique lateral interbody fusion at L5-S1. Eur Spine J. [CrossRef] [PubMed]

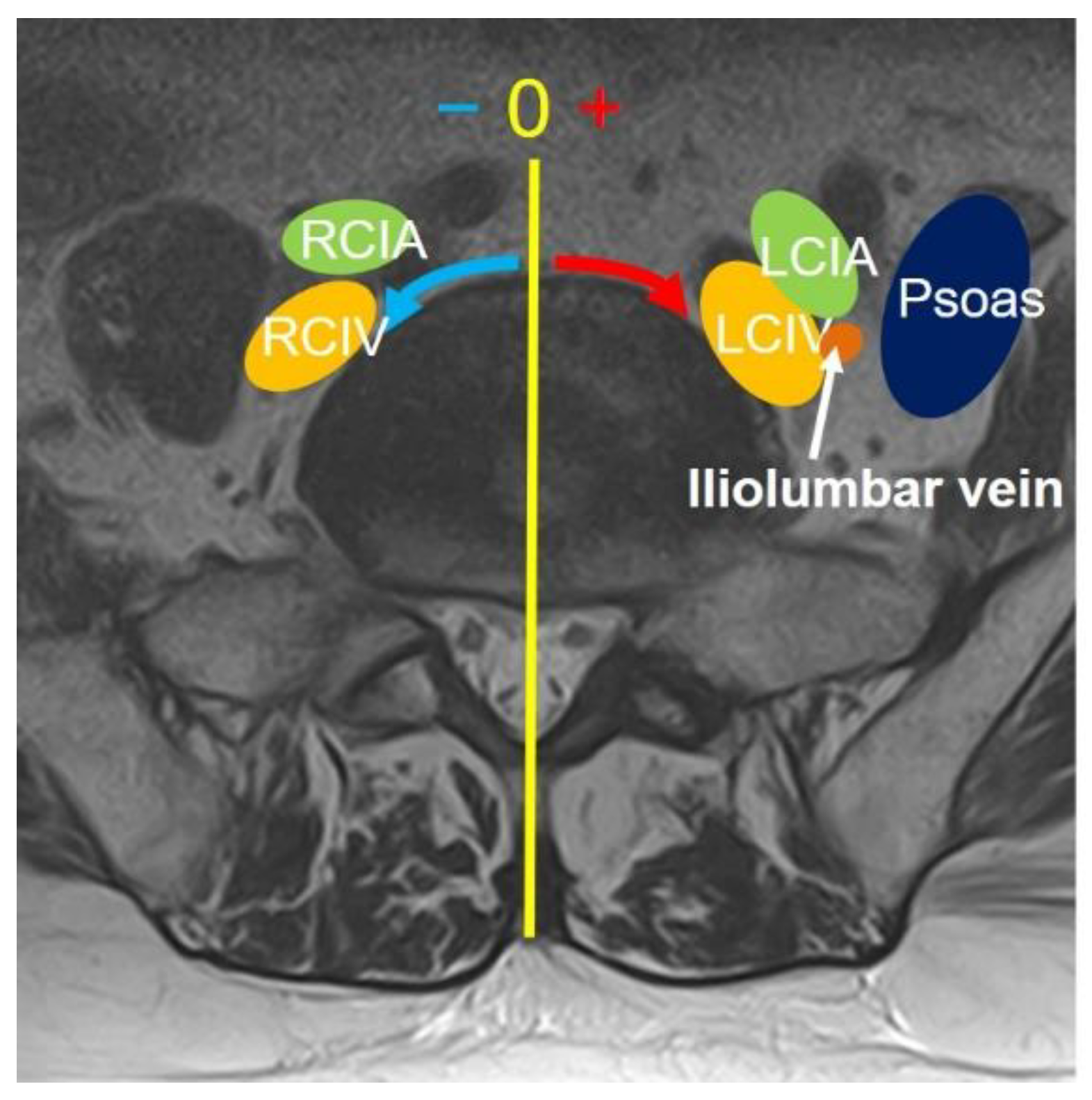
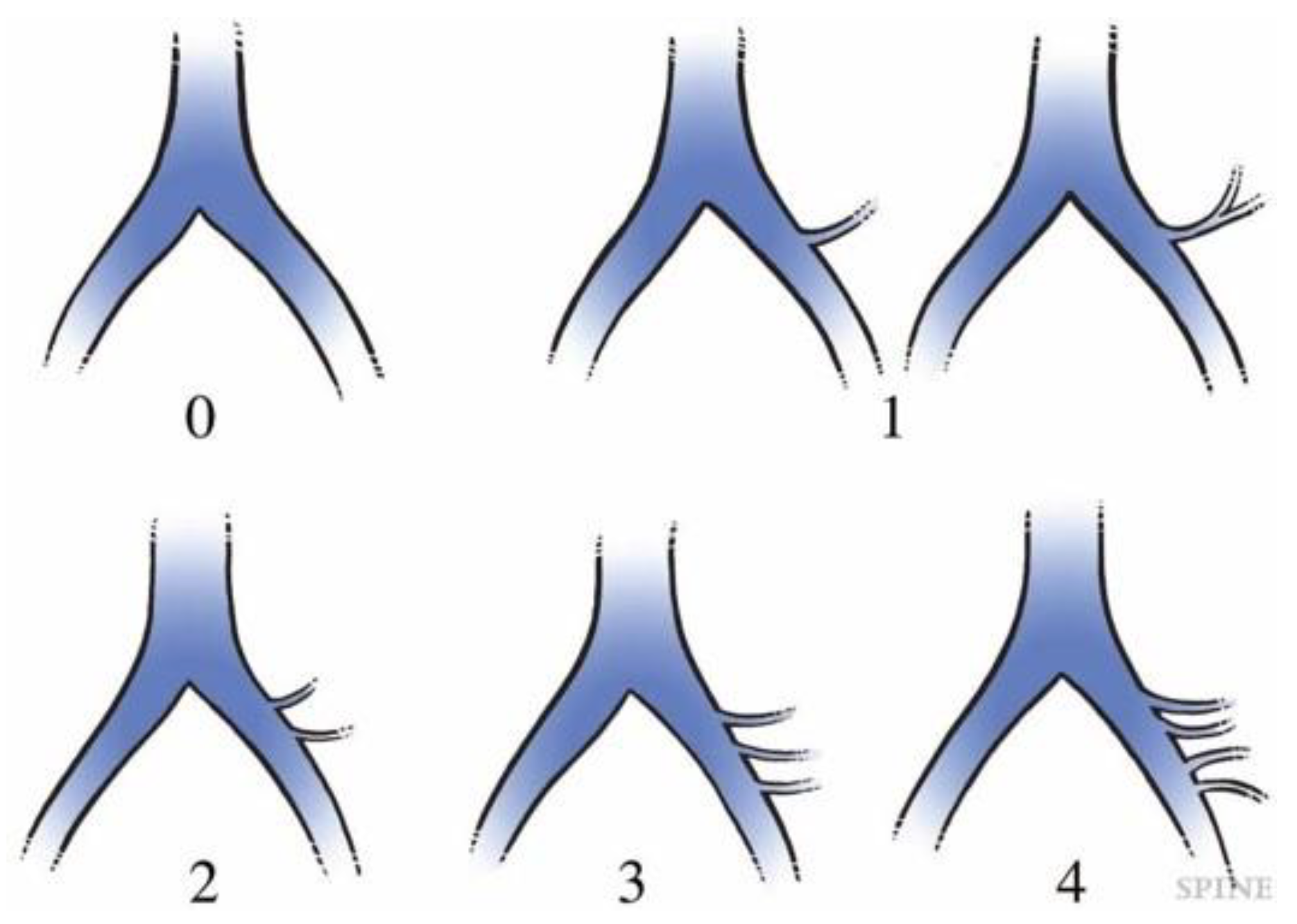
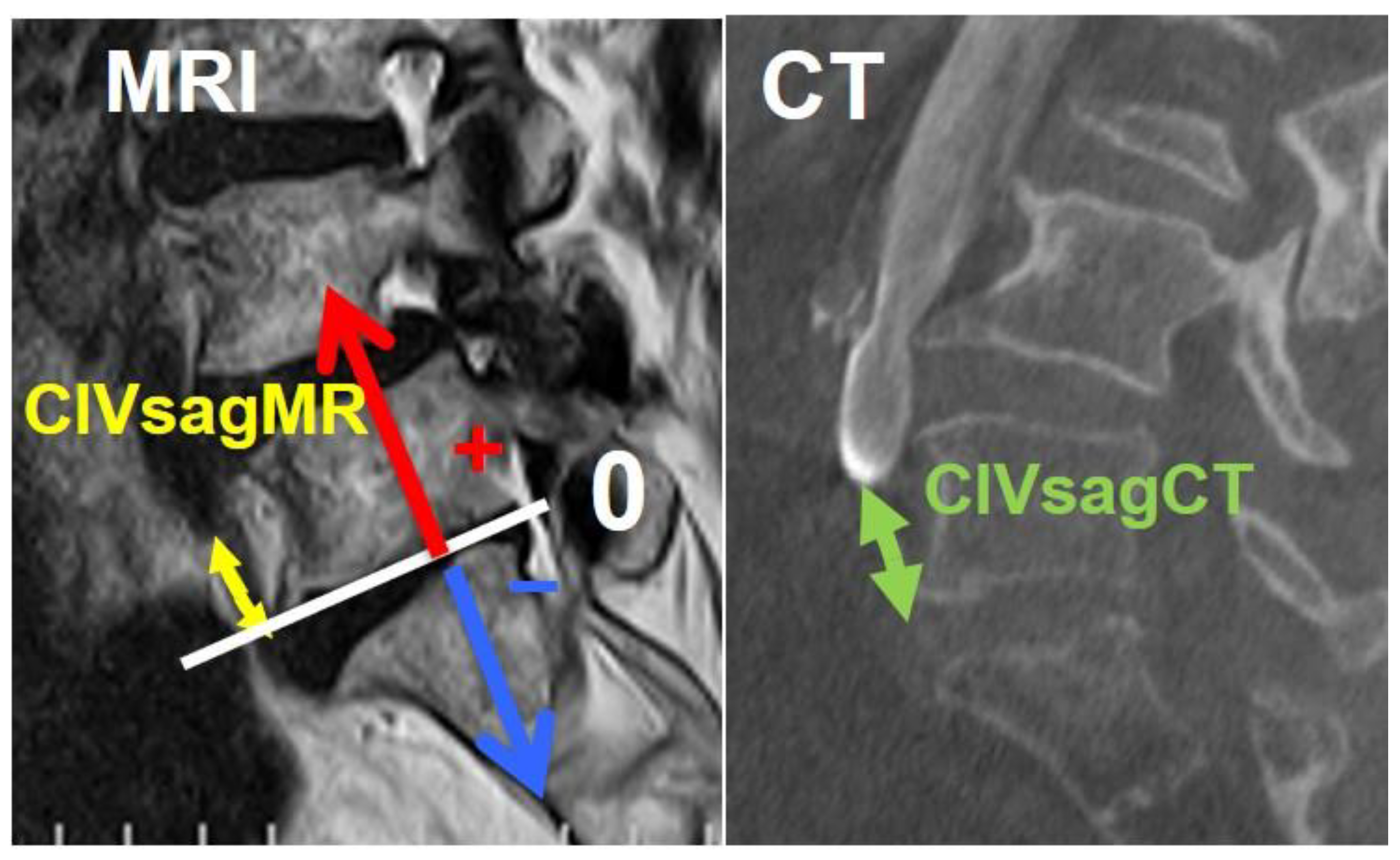
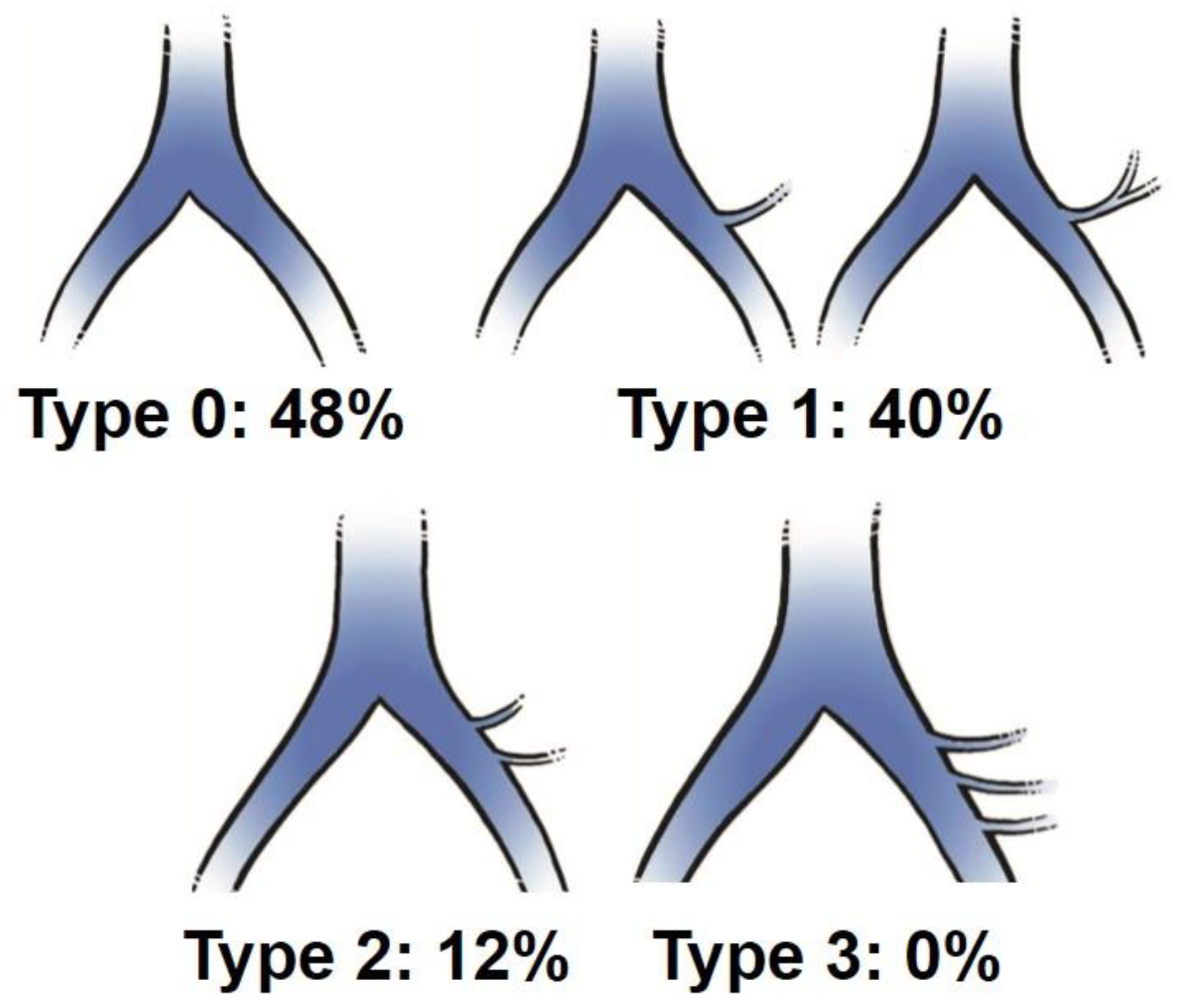
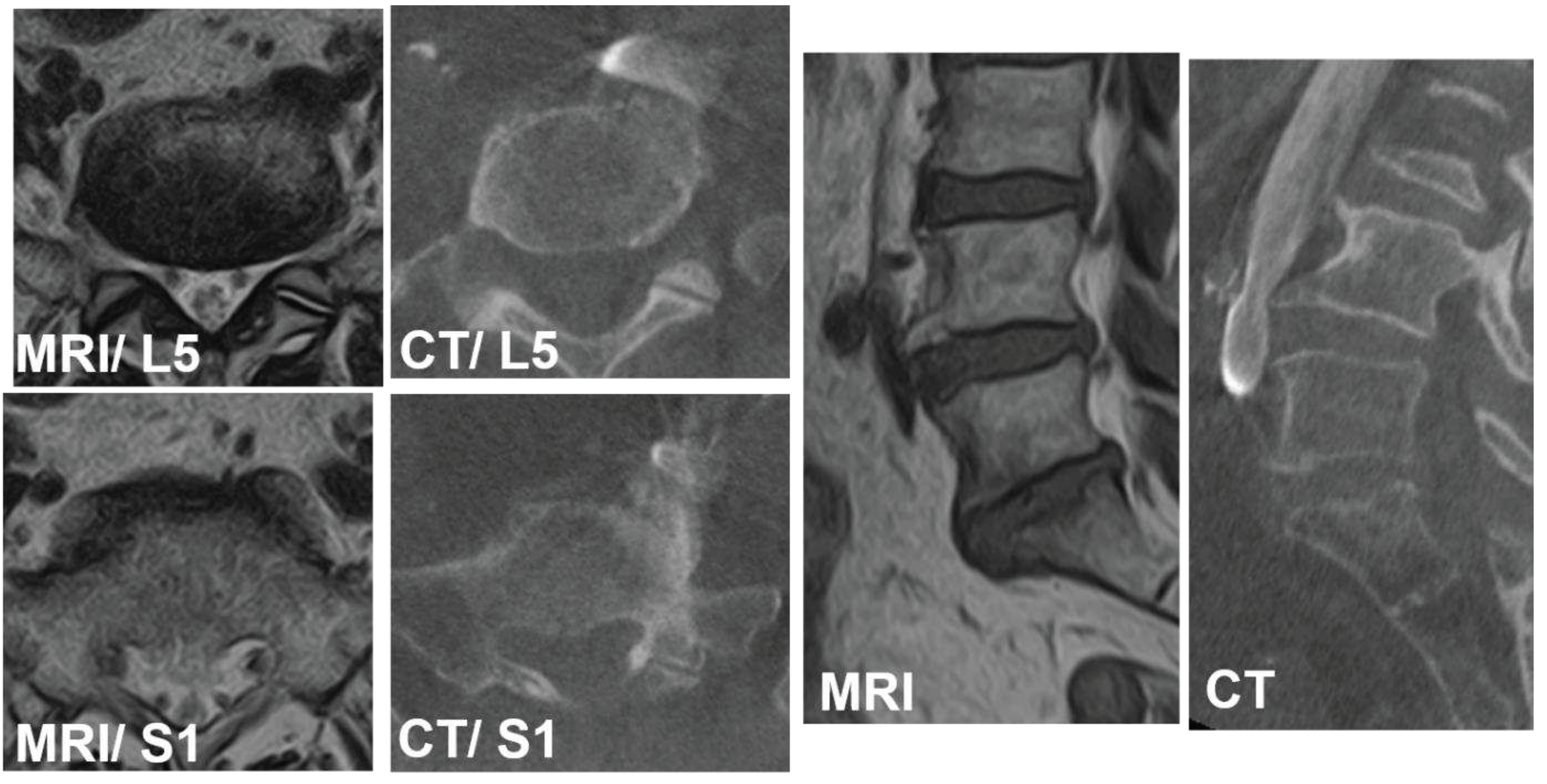
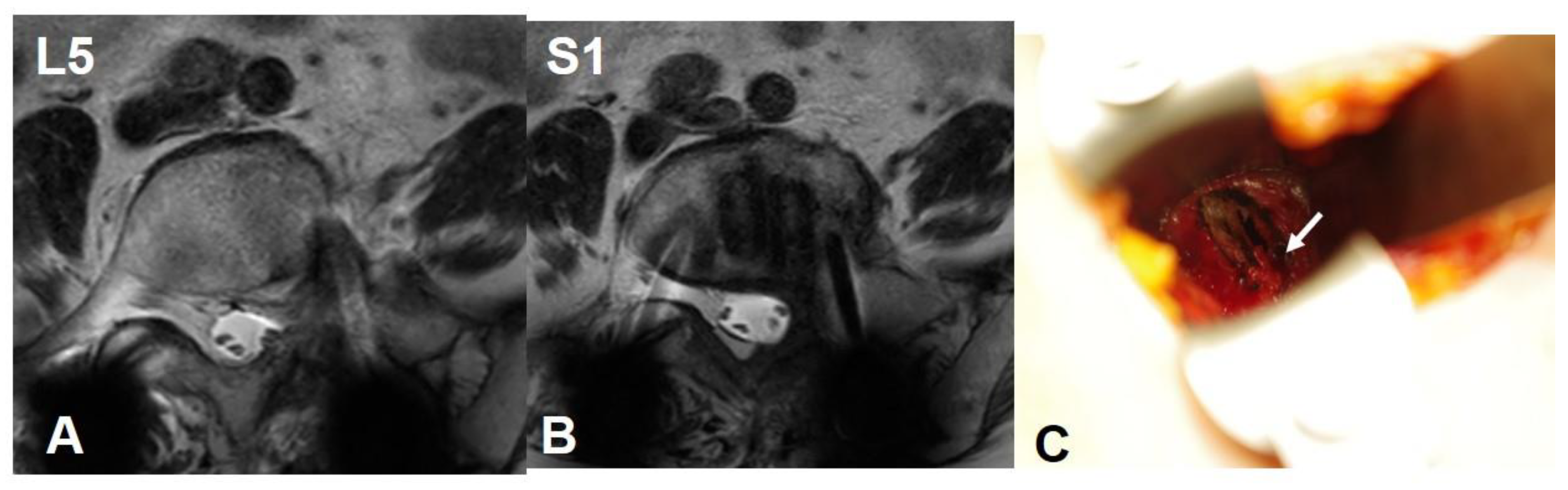
| CIV | CIA | CCW | LCW | ILV | |
| L5 Right | -22.2 (4.1) | -17.9 (4.5) | 22.8 (7.3) | 14.2 (4.8) | 31.1 (5.7) |
| L5 Left | 8.2 (4.0) | 17.8 (5.7) | |||
| S1 Right | -27.9 (2.9) | -21.3 (4.0) | 34.1 (7.3) | 12.6 (3.6) | 30.9 (8.1) |
| S1 Left | 16.0 (4.4) | 25.1 (5.3) |
| CIV | CCW | Vein Bifurcation | |
| L5 Right | -0.8 (2.3) | -3.6 (2.7) | 6.3 (2.3) |
| L5 Left | -3.8 (3.1) | ||
| S1 Right | 0.3 (2.2) | -2.5 (1.6) | |
| S1 Left | -6.9 (3.0) |
| Modality | Mean(mm) | SD(mm) | Max(mm) | Min(mm) | |
|---|---|---|---|---|---|
| CCW | |||||
| This study (L5 caudal) | MRI | 22.9 | 7.3 | 63 | 0 |
| This study (S1 cephalad) | MRI | 34.1 | 7.3 | 59.7 | 6.8 |
| Choi (Mid disc) [8] | MRI | 27 | 9.4 | 46 | 8 |
| Nagamatsu (L5 caudal) [9] | MRI/CT | 29.7 | 10.7 | ||
| Nagamatsu (S1 cephalad) [9] | MRI/CT | 36.9 | 10.3 | ||
| Midline to Lt CIV | |||||
| This study (L5 caudal) | MRI | 8.7 | 5.4 | 21.4 | 0 |
| This study (S1 cephalad) | MRI | 16.0 | 4.4 | 31.3 | -6.5 |
| Liu [10] | CT angiography | 15.9 | 9.3 | 30.2 | 0 |
| Davis [11] | Cadaver | 14.75 | 6.90 | 25.0 | 0 |
| Molinares [12] | MRI | 10.0 | 8.3 | 28.4 | 0 |
| IVC bifurcation from L5 caudal | |||||
| This study | MRI | 25.3 | 14.1 | 59.6 | 0 |
| Davis [11] | Cadaver | 23.8 | 13.3 | 58.0 | 10.0 |
| Nagamatsu [9] | MRI/CT | 23.7 | 10.9 | ||
| LCW | |||||
| This study (L5 caudal) | MRI | 14.3 | 9.6 | 38.5 | 3.0 |
| Molinares [12] | MRI | 10.8 | 9.2 | 24.6 | 4.6 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




