Submitted:
29 November 2023
Posted:
30 November 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
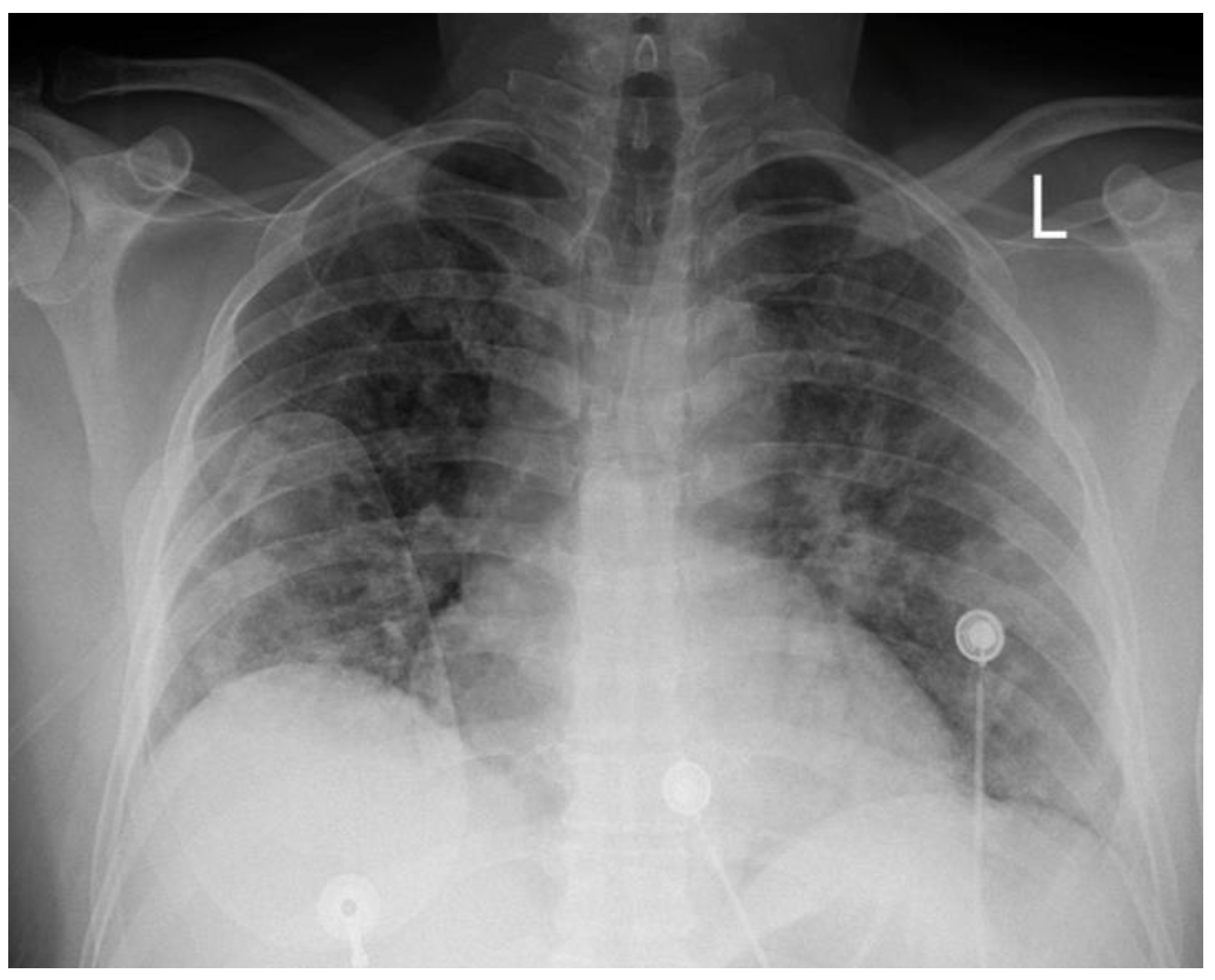
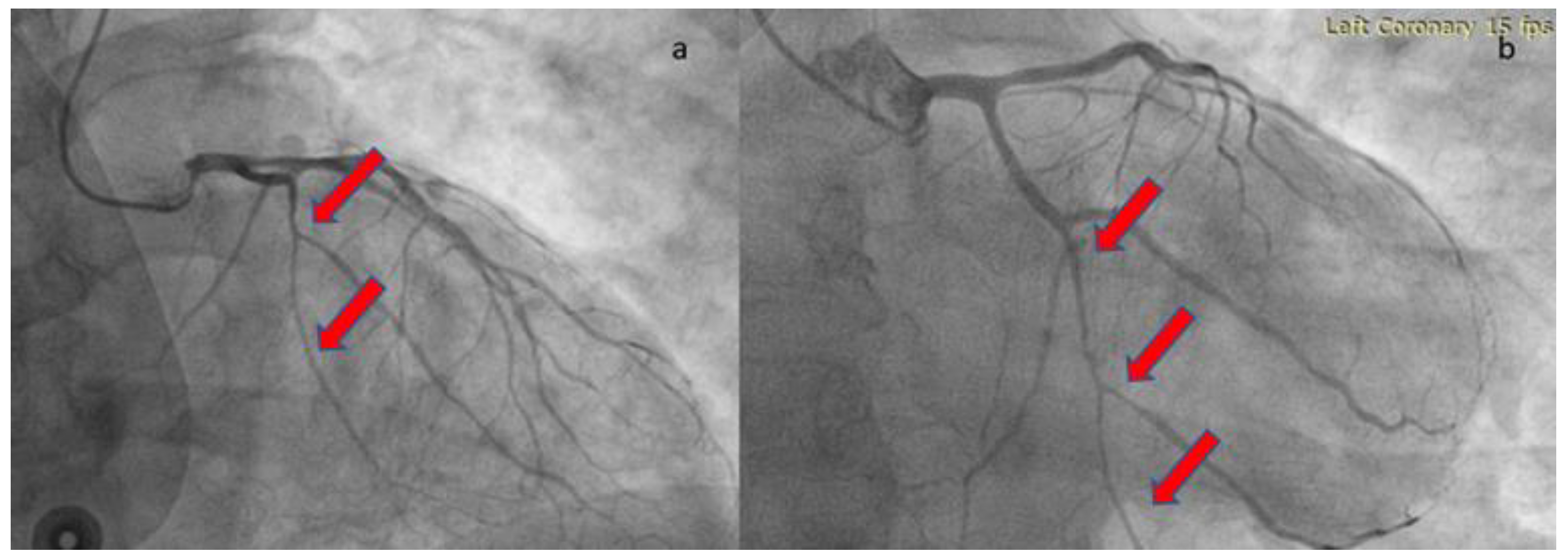
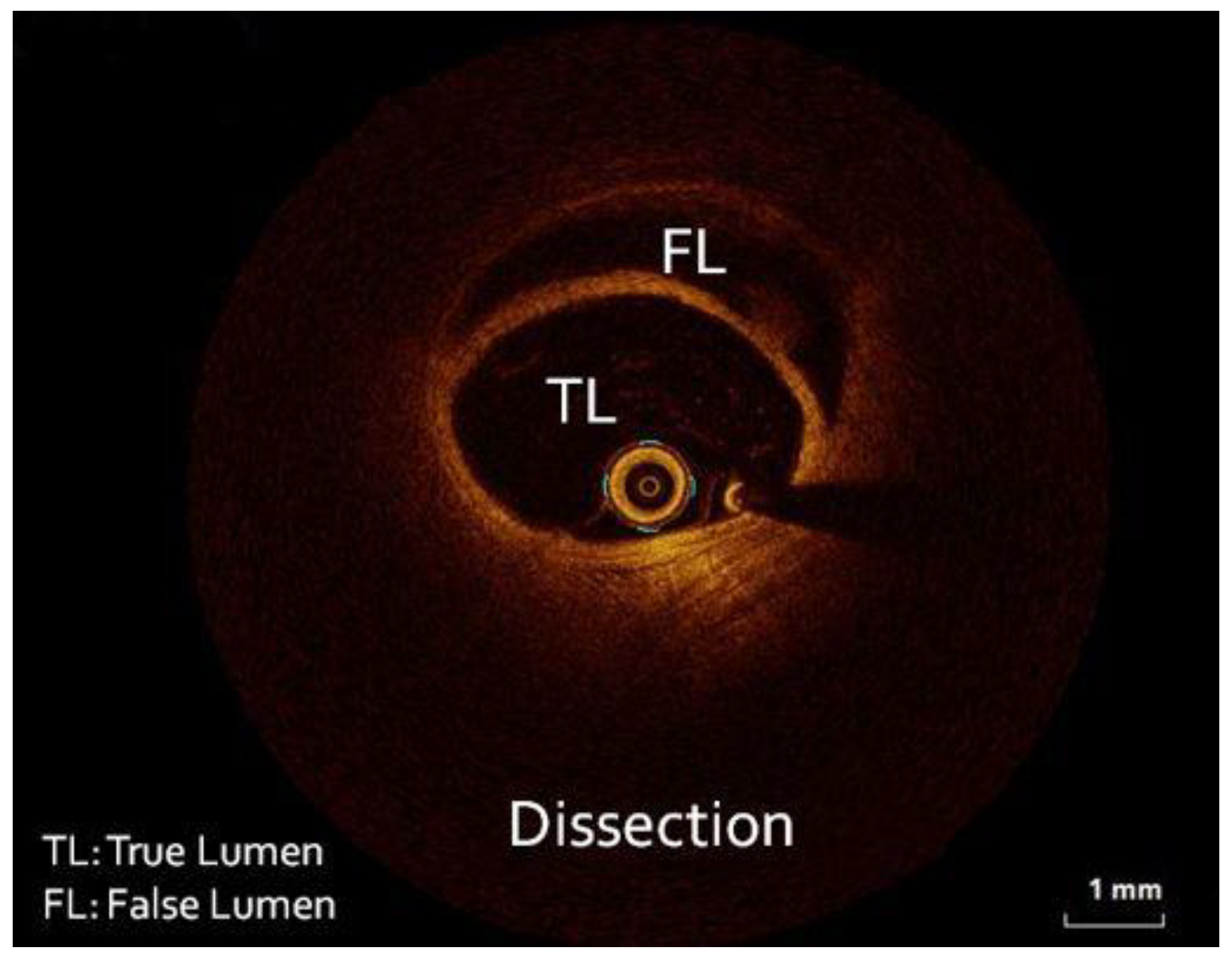
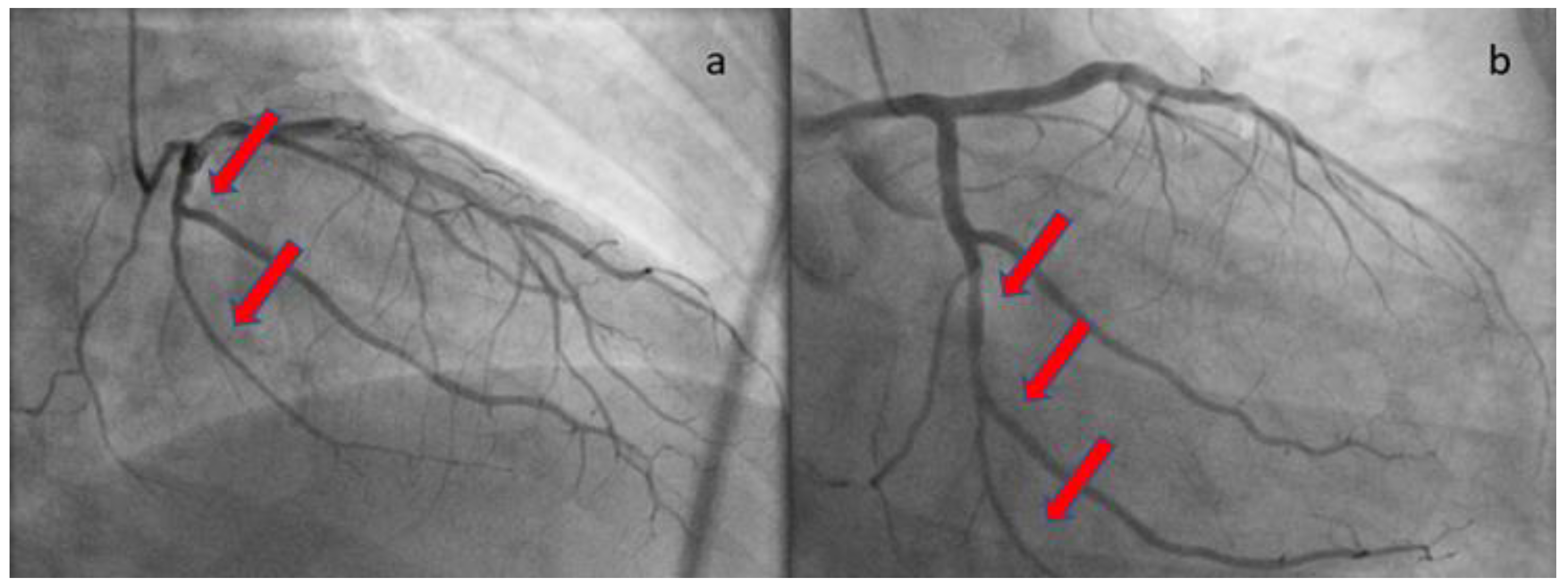
2. Case presentation
3. Discussion
3.1. Potential pathophysiologic mechanisms of SCAD related with COVID-19
- The accumulation of macrophages and T cells in coronary adventitia and periadventitial fat, found in autopsies of COVID-19 patients, could induce excessive levels of cytokines and other mediators of the inflammatory response, resulting in disruption of the vessel wall layers and coronary dissection. Furthermore, the provoked sympathetic over-stimulation is an important factor of endothelial dysfunction and vulnerability [8].
- The infiltration of the vasa vasorum by the inflammatory cells may cause direct damage and rupture with the formation of intramural hematoma. Apart from this, an additional factor contributing to the generation of intramural hematoma may be the excessive angiogenesis of the vasa vasorum, owing to the cytokines and the other inflammatory molecules’ signaling [9].
- Except for the indirect damage mediated by the cytokines and the inflammatory cells, SARS-CoV-2 virus binds directly to the ACE-2 receptors in the vascular endothelial and smooth cells, and can cause inflammation in the coronary vessel wall, impairment of the vascular tone, and deregulation of the coagulation and fibrinolytic systems, making the vessel wall more prone to dissection [7].
- The dysregulation of the vascular tone can cause coronary artery spasm, an identified precipitant of SCAD [6].
- Finally, the administration of high doses of corticosteroids, commonly used in the treatment of COVID-19 patients, may also cause intimal tear of the weakened arterial wall, resulting in formation of intramural hematoma [10].
3.2. Review of case reports on SCAD and COVID-19 infection
| Author, Published date | Sex, age (years) | Past Medical History | Timing of COVID-19 infection, regarding SCAD occurrence | COVID-19 severity | Diagnosis of ACS | Initial EF | Culprit arteries | Treatment/Antithrombotics | Survival |
|---|---|---|---|---|---|---|---|---|---|
| Gasso et al., 2020 [14] | Male, 39 | None | Index hospitalization | Severe/ intubation | STEMI with no CV symptoms | 50-55%, hypokinetic RV | LAD+ OM1 | Conservative/ DAPT | Yes |
| Papanikolaou et al., 2020 [13] | Female, 51 | HTN, smoking | Index hospitalization | Severe, high-flow-nasal-cannula | STEMI | N/A | LAD | Conservative/ DAPT+ anticoagulation | Yes with SCAD healing |
| Cannata et al., 2020 [22] | Female, 45 | None | 8 weeks ago typical symptoms of COVID-19 | Mild | STEMI | Anterior wall hypokinesia | LAD | Conservative/ DAPT | Yes with EF improvement |
| Kireev et al., 2020 [10] | Male, 35 | Serpinginous choroiditis (low CS dose), smoking, overweight | 2 weeks ago | Mild | STEMI | N/A | RI+ RCA | PCI in RI+ conservative in RCA/ DAPT+ anticoagulation (IV UFH) | Yes |
| Kumar et al., 2020 [12] | Female, 48 | Migraines, hyperlipidemia | Index presentation | No symptoms | STEMI | 45-50% | LAD | Conservative/ DAPT for a year | Yes |
| Courand et al., 2020 [15] | Male, 55 | PAD | Index hospitalization | Mild | NSTEMI | 60% | RCA | Conservative/ ASA | Yes |
| Albiero et al., 2020 [16] | Male, 70 | HTN, type 2 diabetes, PCI in LCX, Smoking | Index hospitallization | Mild | NSTEMI | 40-45% | LAD | PCI with DES/ ASA+ clopidogrel | Yes with EF improvement |
| Emren et al., 2021 [17] | Male, 50 | None | Index presentation | Mild | NSTEMI | 55% | RCA | PCI with BMS/ ASA+ clopidogrel | Yes |
| Aparisi et al., 2021 [18] | Male, 40 | None | Index hospitalilzation | Severe/ intubation | Cardiogenic shock | 35% | LAD | Conservative, ASA | Yes |
| Ahmad et al., 2021 [23] | Female, 43 | AF | 12 weeks ago | Mild | Cardiogenic shock | 20% | LCX | Conservative/ Not reported | EF=60% |
| Pettinato et al., 2022 [11] | Female, 43 | MIS-A after COVID-19 (CS treatment), hypothyroidism | 3 month ago | Mild at first- MIS-A later | NSTEMI | 40%+ apical thrombus | LAD | Conservative/ ASA+ clopidogrel+ warfarin for 1 month | Yes with EF=60%, thrombus resolution |
| Lewars et al., 2022 [19] | Female, 51 | Anxiety, recovered postpartum CMP 15 years ago | At index presentation | No symptoms | NSTEMI | Dyskinetic apex, EF=60% | LAD | Conservative/ N/A | Yes with SCAD healing |
| Ansari et al., 2022 [24] | Female, 58 | Hyperlipidemia | 2 months ago | Mild lung involvement, severe thrombocytopenia | NSTEMI | 50% | LCX | Conservative/ ASA+ clopidogrel | Yes |
| Shah et al., 2023 [20] | Female, 67 | FHCAD | Index presentation | No symptoms | STEMI | 65%, apical akinesia | LAD | POBA in LAD/ ASA | Yes, recovery |
| Bashir et al., 2023 [21] | Female, 36 | Morbid obesity (BMI=49kg/m2) | Index presentation | Mild, fever | NSTEMI | 35%, thrombus formation | LAD | Conservative/ Clopidogrel+ warfarin | Yes, EF=60%, thrombus resolution |
| Papageorgiou et al., 2023 | Male, 51 | HTN | Index presentation | Severe, continuous positive airway pressure-helmet | STEMI | 50% | LCX | Conservative/ ASA for 1 year+ rivaroxaban 10mg OD for 35 days | Yes, EF= 60%, SCAD healing |
3.3. STEMI management during the COVID-19 pandemic
3.4. Optimal antithrombotic therapy in SCAD patients with concomitant COVID-19 infection
4. Conclusions
Author Contributions
Funding
Informed Consent Statement
Conflicts of Interest
References
- Shi S, Qin M, Shen B, et al. Association of Cardiac Injury with Mortality in Hospitalized Patients with COVID-19 in Wuhan, China. JAMA Cardiol. 2020;5(7). [CrossRef]
- Guo T, Fan Y, Chen M, et al. Cardiovascular Implications of Fatal Outcomes of Patients with Coronavirus Disease 2019 (COVID-19). JAMA Cardiol. 2020;5(7). [CrossRef]
- López-Otero D, López-Pais J, Antúnez-Muiños PJ, Cacho-Antonio C, González-Ferrero T, González-Juanatey JR. Association between myocardial injury and prognosis of COVID-19 hospitalized patients, with or without heart disease. CARDIOVID registry. Rev Española Cardiol (English Ed. 2021;74(1). [CrossRef]
- Akhmerov A, Marbán E. COVID-19 and the Heart. Circ Res. Published online May 8, 2020:1443-1455. [CrossRef]
- Hayes SN, Tweet MS, Adlam D, et al. Spontaneous Coronary Artery Dissection: JACC State-of-the-Art Review. J Am Coll Cardiol. 2020;76(8). [CrossRef]
- Hayes SN, Kim CESH, Saw J, et al. Spontaneous coronary artery dissection: Current state of the science: A scientific statement from the American Heart Association. Circulation. 2018;137(19). [CrossRef]
- ESC. ESC Guidance for the Diagnosis and Management of CV Disease during the COVID-19 Pandemic. Eur Heart J. Published online 2020.
- Adlam D, Alfonso F, Maas A, Vrints C. European Society of Cardiology, acute cardiovascular care association, SCAD study group: a position paper on spontaneous coronary artery dissection. In: European Heart Journal. Vol 39. ; 2018. [CrossRef]
- Pine AB, Meizlish ML, Goshua G, et al. Circulating markers of angiogenesis and endotheliopathy in COVID-19. Pulm Circ. 2020;10(4). [CrossRef]
- Kireev K, Genkel V, Kuznetsova A, Sadykov R. Multivessel spontaneous coronary artery dissection in a patient after mild COVID-19: A case report. SAGE Open Med Case Reports. 2020;8:2050313X2097598. [CrossRef]
- Pettinato AM, Ladha FA, Zeman J, Ingrassia JJ. Spontaneous Coronary Artery Dissection Following SARS-CoV-2-Associated Multisystem Inflammatory Syndrome. Cureus. 2022;14(7):2-7. [CrossRef]
- Kumar K, Vogt JC, Divanji PH, Cigarroa JE. Spontaneous coronary artery dissection of the left anterior descending artery in a patient with COVID-19 infection. Catheter Cardiovasc Interv. 2021;97(2):E249-E252. [CrossRef]
- Papanikolaou J, Alharthy A, Platogiannis N, et al. Spontaneous coronary artery dissection in a patient with COVID-19. Coron Artery Dis. 2021;32(4):354-355. [CrossRef]
- Gasso LF, Maneiro Melon NM, Cebada FS, Solis J, Tejada JG. Multivessel spontaneous coronary artery dissection presenting in a patient with severe acute SARS-CoV-2 respiratory infection. Eur Heart J. 2020;41(32):3100-3101. [CrossRef]
- Courand PY, Harbaoui B, Bonnet M, Lantelme P. Spontaneous Coronary Artery Dissection in a Patient With COVID-19. JACC Cardiovasc Interv. 2020;13(12):e107-e108. [CrossRef]
- Albiero R, Seresini G, Liga R, et al. Atherosclerotic spontaneous coronary artery dissection (A-SCAD) in a patient with COVID-19: Case report and possible mechanisms. Eur Hear J - Case Reports. 2020;4(FI1):1-6. [CrossRef]
- Emren ZY, Emren V, Özdemir E, Karagöz U, Nazli C. Spontaneous right coronary artery dissection in a patient with COVID-19 infection: A case report and review of the literature. Turk Kardiyol Dern Ars. 2021;49(4):334-338. [CrossRef]
- Aparisi Á, Ybarra-Falcón C, García-Granja PE, Uribarri A, Gutiérrez H, Amat-Santos IJ. COVID-19 and spontaneous coronary artery dissection: Causality? REC Interv Cardiol. 2021;3(2):141-143. [CrossRef]
- LEWARS J, MOHTA A, HL LAL H. Case Report of Spontaneous Coronary Artery Dissection in a Patient Positive for Covid-19. Chest. 2022;162(4):A283. [CrossRef]
- Shah N, Shah N, Mehta S, Murray E, Grodzinsky A. Spontaneous Coronary Artery Dissection (SCAD) in an Atypical Patient Without Risk Factors and Prior Asymptomatic COVID-19 Infection. Cureus. 2023;2023(6):1-6. [CrossRef]
- Bashir H, Muhammad Haroon D, Mahalwar G, Kalra A, Alquthami A. The Coronavirus Double Threat: A Rare Presentation of Chest Pain in a Young Female. Cureus. 2023;8(4):8-12. [CrossRef]
- Cannata S, Birkinshaw A, Sado D, Dworakowski R, Pareek N. Spontaneous coronary artery dissection after COVID-19 infection presenting with ST segment elevation. Eur Heart J. 2020;41(48):4602. [CrossRef]
- AHMAD F, AHMED A, RAJENDRAPRASAD S, LORANGER A, VIVEKANANDAN R, MOORE D. Spontaneous Coronary Artery Dissection: a Rare Sequela of Covid-19. Chest. 2021;160(4):A94-A95. [CrossRef]
- ansari.pdf.
- Ramacciotti E, Barile Agati L, Calderaro D, et al. Rivaroxaban versus no anticoagulation for post-discharge thromboprophylaxis after hospitalisation for COVID-19 (MICHELLE): an open-label, multicentre, randomised, controlled trial. Lancet. 2022;399(10319):50-59. [CrossRef]
- Bu J, Chen M, Cheng X, et al. [Consensus of Chinese experts on diagnosis and treatment processes of acute myocardial infarction in the context of prevention and control of COVID-19 (first edition)]. Nan Fang Yi Ke Da Xue Xue Bao. 2020;40(2):147-151. [CrossRef]
- Ndao SCT, Zabalawi A, Ka MM, et al. Sudden Cardiac Death Following Thrombolysis in a Young Woman with Spontaneous Coronary Artery Dissection: A Case Report. Am J Case Rep. 2021;22(1):e931683-1. [CrossRef]
- Shamloo BK, Chintala RS, Nasur A, et al. Spontaneous coronary artery dissection: Aggressive vs. conservative therapy. J Invasive Cardiol. 2010;22(5).
- Mcalister C, Samuel R, Alfadhel M, et al. TCT-21 Thrombolysis in Spontaneous Coronary Artery Dissection: Angiographic Findings and Clinical Outcomes. J Am Coll Cardiol. 2021;78(19):B10. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




