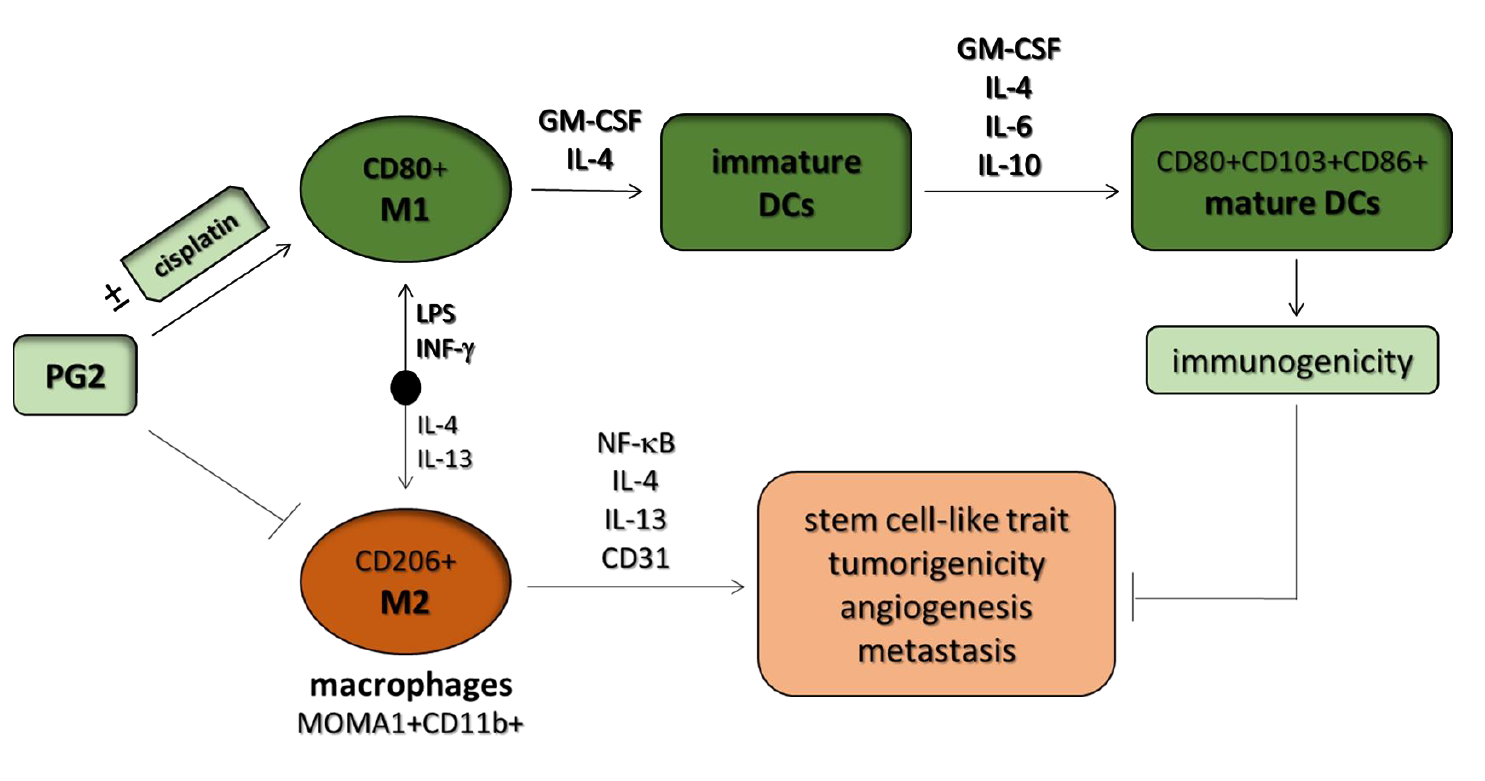
Background: Recently we demonstrated that Astragalus polysaccharide (PG2), the active ingredient in dried roots of astragalus membranaceus, ameliorates cancer symptom clusters and improve quality of life (QoL) in patients with metastatic disease by modulating inflammatory cascade, against the background that inflammatory cells including macrophages, dendritic cells (DCs), and cytotoxic T lymphocytes (CTLs) in tumor initiation, metastasis, and progression. Nevertheless, the role of PG2 in the modulation of anticancer immunogenicity and therapeutic response remains relatively underexplored and unclear. Purpose: The present study investigates how and to what extent PG2 modulates cellular and biochemical components of the inflammatory cascade, enhance anticancer immunity, and the therapeutic implication of same in patients with lung cancer. Methods and Results: Herein, we demonstrated that PG2 significantly increased the M1/M2 macrophage polarization ratio in non-small cell carcinoma (NSCLC) H441 and H1299 cells. This PG2-induced preferential pharmacologic up-regulation of tumoral M1 population in vitro, positively correlated with the downregulation of tumor-promoting IL-6 and IL-10 expression in NSCLC cell-conditioned medium, with concomitant marked inhibition of cell proliferation, clonogenicity and tumorsphere formation. Our ex vivo results, using clinical sample from our NSCLC cohort, demonstrated that PG2 also promoted the functional maturation of DCs with consequent enhancement of T cell-mediated anticancer immune responses. Consistent with the in vitro and ex vivo results, our in vivo studies showed that mice treated with PG2 exhibited significant time-dependent depletion of the tumor-associated M2 population, synergistically enhanced the anti-M2-based anticancer effect of cisplatin, and inhibition of xenograft tumor growth in the NSCLC mice models. Moreover, in the presence of PG2, cisplatin-associated dyscresia and weight-loss was markedly suppressed. Conclusion: These results do indicate a therapeutically-relevant role for PG2 in modulating the M1/M2 macrophage pool, facilitating DC maturation, and synergistically enhancing the anticancer effect of conventional chemotherapeutic agent, cisplatin; thus laying the foundation for further exploration of the curative relevance of PG2 as surrogate immunotherapy and/or clinical feasibility of its use for maintenance therapy in patients with lung cancer.