Submitted:
30 April 2026
Posted:
05 May 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methodology
2.1. Understanding Neurodegenerative Diseases and the Role of Augmented Reality
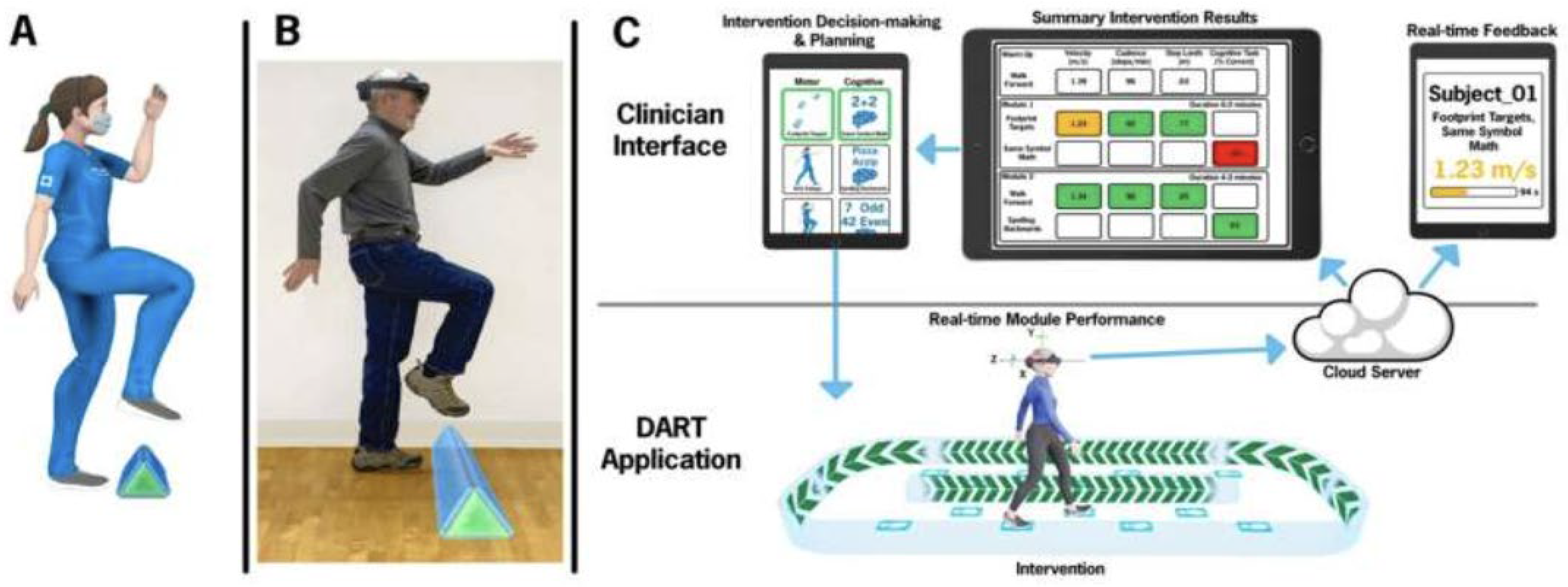
2.2. Designing Supportive Environments for Parkinson’s Using Augmented Reality
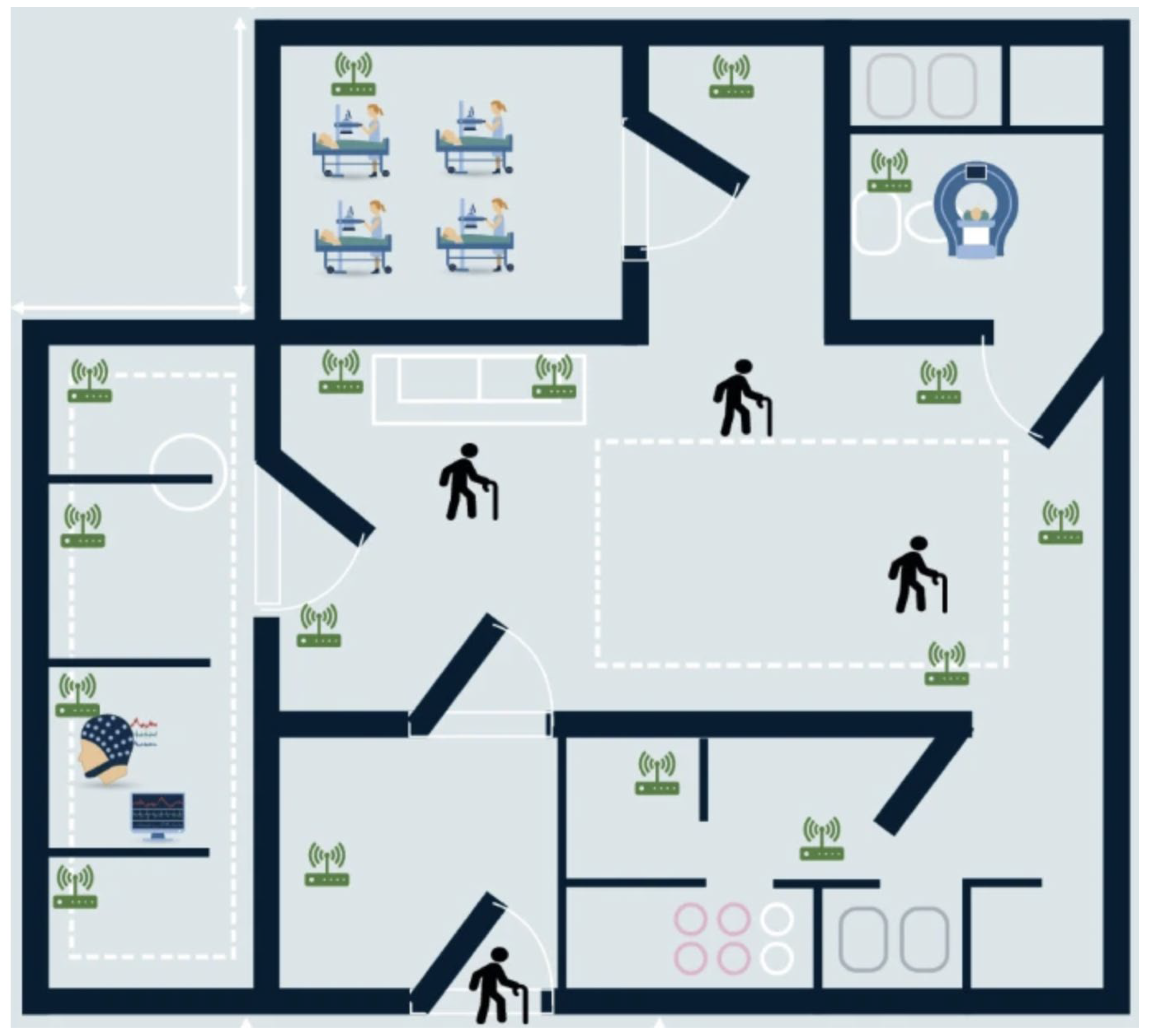
2.3. Augmented Reality for Dementia-Friendly Spaces
2.4. Augmented Reality–Enabled Interior Design for Cerebral Palsy and Huntington’s Disease Rehabilitation
3. Reality Check: When Augmented Care Meets Ethical Care
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Farooq, M. S.; Zahid, Z.; Omer, U.; Tehseen, R.; Alvi, A.; Farooq, U.; Atal, Z. Applications of Augmented Reality in Neurology: Architectural Model and Guidelines. IEEE Access 2022, 10, 102804–102830. [Google Scholar] [CrossRef]
- Hariharan, V.; Pk, M. P. K.; Rajanandh, M. G.; Kumari, P. M. P. Extended Reality in Revolutionizing Neurological Disease: A New Era for Chronic Condition Treatment. Cureus 2024, 16(8). [Google Scholar] [CrossRef] [PubMed]
- Anene, J. I.; Sharma, A.; Sharma, A.; Fatima, I.; Kancherla, N.; Ponnada, S. C.; et al. Exploring the Potential of Artificial Intelligence (AI) and Augmented Reality (AR) in Neurological Disease Management: A Narrative Review. Cureus 2025, 17(6). [Google Scholar] [CrossRef] [PubMed]
- Janssen, S.; van Steveninck, J. de Ruyter; Salim, H. S.; Cockx, H. M.; Bloem, B. R.; Heida, T.; Van Wezel, R. J. The Effects of Augmented Reality Visual Cues on Turning in Place in Parkinson’s Disease Patients with Freezing of Gait. Front. Neurol. 2020, 11, 185. [Google Scholar] [CrossRef]
- Cleveland Clinic. Using Augmented Reality to Make Parkinson’s Disease Physical Therapy More Accessible. MedicalXpress. 18 September 2023. Available online: https://medicalxpress.com/news/2023-09-augmented-reality-parkinson-disease-physical.html.
- Zanwar, P.; Heyn, P. C.; McGrew, G.; Raji, M. Assistive Technology Megatrends to Support Persons with Alzheimer’s Disease and Related Dementias Age in Habitat. In Proceedings of the Workshop on Human-Habitat for Health; 2018; pp. 1–9. [Google Scholar]
- Taghian, A.; Abo-Zahhad, M.; Sayed, M. S.; Abd El-Malek, A. H. Virtual and Augmented Reality in Biomedical Engineering. Biomed. Eng. Online 2023, 22(1), 76. [Google Scholar] [CrossRef]
- do Nascimento, L. G. G.; Correia, W. F. M.; Campos, F.; van Gisbergen, M. S.; Barros, M. D. L. N.; Lins, A.; Teixeira, J. M. X. Augmented Reality for Cognitive Screening in Neurodegenerative Diseases: A Ten-Year Systematic Review. J. Braz. Comput. Soc. 2025, 31(1), 742–760. [Google Scholar] [CrossRef]
- Zhao, Y.; Gagnon, H.; Stefanucci, J.; Creem-Regehr, S.; Bodenheimer, B. A Systematic Review of the Use of Augmented Reality in Pedestrian Navigation. ACM Comput. Surv. 2025, 58(5), 1–32. [Google Scholar] [CrossRef]
- Biswas, M.; Rahman, A.; Kaiser, M. S.; Al Mamun, S.; Mizan, K. S. Ebne; Islam, M. S.; Mahmud, M. Indoor Navigation Support System for Patients with Neurodegenerative Diseases. In International Conference on Brain Informatics; Springer International Publishing: Cham, 2021; pp. 411–422. [Google Scholar]
- Malick, W. H.; Butt, R.; Awan, W. A.; Ashfaq, M.; Mahmood, Q. Effects of Augmented Reality Interventions on the Function of Upper Extremity and Balance in Children with Spastic Hemiplegic Cerebral Palsy: A Randomized Clinical Trial. Front. Neurol. 2022, 13, 895055. [Google Scholar] [CrossRef]
- Balloufaud, M.; Boujut, A.; Marie, R.; Okassa, M. B. M.; Fourcade, L.; Hamonet-Torny, J.; Perrochon, A. User Experience of a Custom Augmented Reality-Based Exergame for Children with Cerebral Palsy and Acquired Brain Injuries. 2025. [Google Scholar] [CrossRef]
- Maggio, M. G.; Billeri, L.; Cardile, D.; Quartarone, A.; Calabrò, R. S. The Role of Innovation Technology in the Rehabilitation of Patients Affected by Huntington’s Disease: A Scoping Review. Biomedicines 2024, 12(1), 39. [Google Scholar] [CrossRef]
- Ganesh, S.; Chithambaram, T.; Krishnan, N. R.; Vincent, D. R.; Kaliappan, J.; Srinivasan, K. Exploring Huntington’s Disease Diagnosis via Artificial Intelligence Models: A Comprehensive Review. Diagnostics 2023, 13(23), 3592. [Google Scholar] [CrossRef]
- Muntian, L. Virtual and Augmented Reality in Healthcare Management Mechanisms for Maintaining Public Health: Literature Overview. Ukr. J. Med. Biol. Sports 2025, 10(3), 36–50. [Google Scholar]
- Ara, J.; Karim, F. B.; Alsubaie, M. S. A.; Bhuiyan, Y. A.; Bhuiyan, M. I.; Bhyan, S. B.; Bhuiyan, H. Comprehensive Analysis of Augmented Reality Technology in Modern Healthcare System. Int. J. Adv. Comput. Sci. Appl. 2021, 12(6), 840–849. [Google Scholar] [CrossRef]
- Goulet, M. H.; Dellazizzo, L.; Goyer, S.; Dollé, S.; Hudon, A.; Phraxayavong, K.; et al. What Are the Ethical Issues Surrounding Extended Reality in Mental Health? A Scoping Review of the Different Perspectives. Behav. Sci. 2025, 15(10), 1431. [Google Scholar] [CrossRef]
- Slater, M.; Gonzalez-Liencres, C.; Haggard, P.; Vinkers, C.; Gregory-Clarke, R.; Jelley, S.; et al. The Ethics of Realism in Virtual and Augmented Reality. Front. Virtual Real. 2020, 1, 1. [Google Scholar] [CrossRef]
- Ray, S.; Tawar, S.; Singh, N.; Singh, G. Transition toward Technological Transformation: Challenges of Implementing Virtual Reality and Augmented Reality in the Health Sector. J. Mar. Med. Soc. 2024, 26(2), 161–164. [Google Scholar] [CrossRef]
- Bruno, R. R.; Wolff, G.; Wernly, B.; Masyuk, M.; Piayda, K.; Leaver, S.; et al. Virtual and Augmented Reality in Critical Care Medicine: The Patient’s, Clinician’s, and Researcher’s Perspective. Crit. Care 2022, 26(1), 326. [Google Scholar] [CrossRef]
- Ray, J.; Kumar, S.; Pandey, S.; Akram, S. V. The Role of Augmented Reality and Virtual Reality in Shaping the Future of Health Psychology. In Proceedings of the 3rd International Conference on Pervasive Computing and Social Networking (ICPCSN); IEEE, 2023; pp. 1604–1608. [Google Scholar]
- Evans, J. White Pap. IEEE Glob. Initiat. Ethics Ext. Real. (XR) Report: Extended Reality (XR) Ethics Med. 2022, 1–31.
- Werner, L.; Brey, P.; Henschke, A. Augmented Reality and Ethics: Key Issues. Virtual Real. 2025, 29(3), 122. [Google Scholar] [CrossRef]
- Siddiqui, M. Faizan; Jabeen, S.; Alwazzan, A.; Vacca, S.; Dalal, L.; Al-Haddad, B.; et al. Integration of Augmented Reality, Virtual Reality, and Extended Reality in Healthcare and Medical Education: A Glimpse into the Emerging Horizon in LMICs-A Systematic Review. J. Med. Educ. Curric. Dev. 2025, 12, 23821205251342315. [Google Scholar]
- Iqbal, A. I.; Aamir, A.; Hammad, A.; Hafsa, H.; Basit, A.; Oduoye, M. O.; et al. Immersive Technologies in Healthcare: An In-Depth Exploration of Virtual Reality and Augmented Reality in Enhancing Patient Care, Medical Education, and Training Paradigms. J. Prim. Care Community Health 2024, 15, 21501319241293311. [Google Scholar] [CrossRef] [PubMed]
- Moawad, G. N.; Elkhalil, J.; Klebanoff, J. S.; Rahman, S.; Habib, N.; Alkatout, I. Augmented Realities, Artificial Intelligence, and Machine Learning: Clinical Implications and How Technology Is Shaping the Future of Medicine. J. Clin. Med. 2020, 9(12), 3811. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



