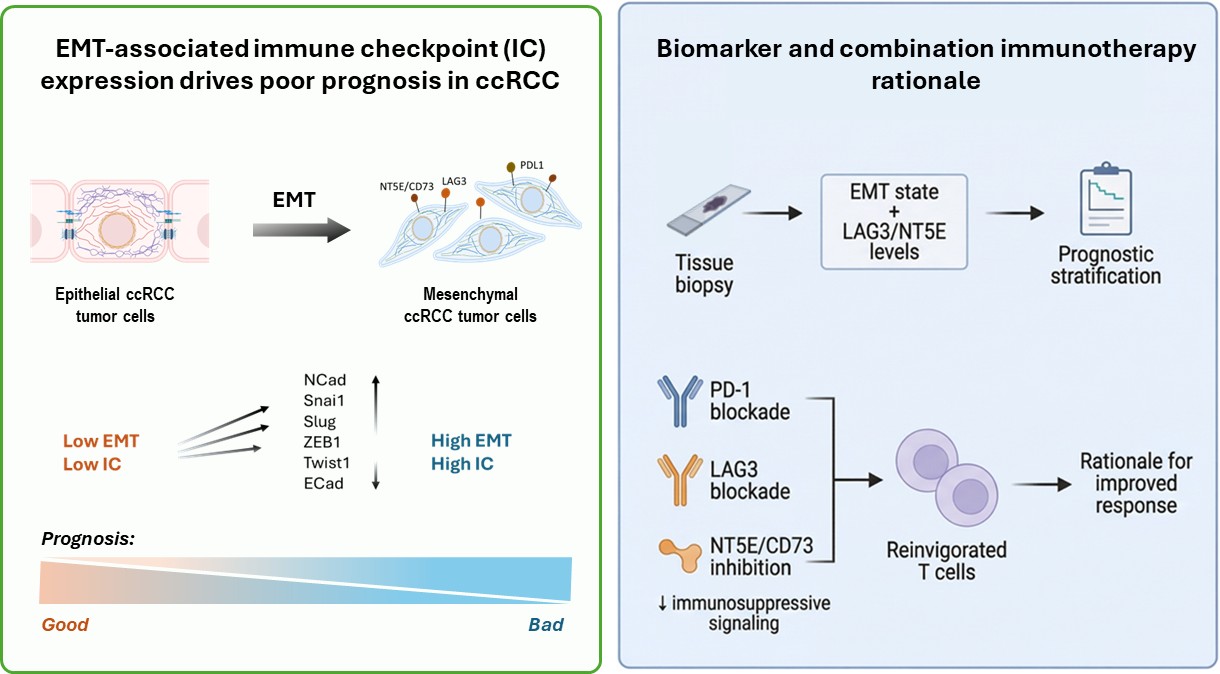
Background/Objectives: Clear cell renal cell carcinoma (ccRCC), the predominant malignant subtype of kidney cancer, is the leading cause of death among renal cell carcinoma patients. Although a subset of ccRCC patients benefit from select immune checkpoint inhibitors (ICIs), prognosis remains poor. While PD-1 and PD-L1 have been extensively studied, the prevalence and distribution of other immune checkpoints (ICs) and their relationship with epithelial-to-mesenchymal transition (EMT) remain poorly characterized. Here, we investigated the interplay between twenty ICs and EMT markers and assessed their combined prognostic relevance in ccRCC patients. Methods: Transcriptomic profiling and integrated bioinformatic analyses were performed, including differential expression, correlation analyses, survival analyses, forest plot analyses, ROC curve evaluation, and OncoPrint visualisation, complemented by analysis of single-cell RNA sequencing data, immunohistochemistry, and multiplex secretory IC (LegendPlex) assays. Results: Transcriptomic profiling of over 500 ccRCC tumors versus normal kidney tissue revealed dysregulation of ICs, particularly LAG3 and NT5E. Notably, expression of ICs, including LAG3 and NT5E, was associated with poor overall survival in 415 ccRCC patients. ICs that synergised with EMT phenotype provided improved prognostic discrimination compared to individual ICs. Correlation analyses, single-cell RNA sequencing and immunohistochemistry demonstrated that EMT-associated tumor cells exhibit coordinated expression of LAG3 and NT5E. Receiver operating characteristic analysis highlighted the potential clinical utility of LAG3 and NT5E. Conclusions: Collectively, this study defines an EMT-IC axis in ccRCC and demonstrates its relevance to tumor biology and patient outcomes, highlighting LAG3 and NT5E as potential prognostic markers and therapeutic targets.