Submitted:
15 April 2026
Posted:
15 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials & Methods
2.1. Research Questions
- 1)
- To what extent do emotion regulation difficulties differ among drug users according to indicators of substance use severity (hospitalization, detoxification treatment, injection drug use)?
- 2)
- Are there associations between type of substance used, polysubstance use, and emotion regulation difficulties?
- 3)
- Does impulse control deficit predict the use of maladaptive coping strategies, such as aggressive and antisocial action?
- 4)
- To what extent do behavioral coping strategies predict the level of emotion regulation difficulties, particularly impulsivity?
- 5)
- What is the relationship between emotion regulation difficulties and behavioral coping strategies among drug users?
2.2. Assessment of Emotion Regulation Difficulties
2.3. Assessment of Coping Strategies
3. Results
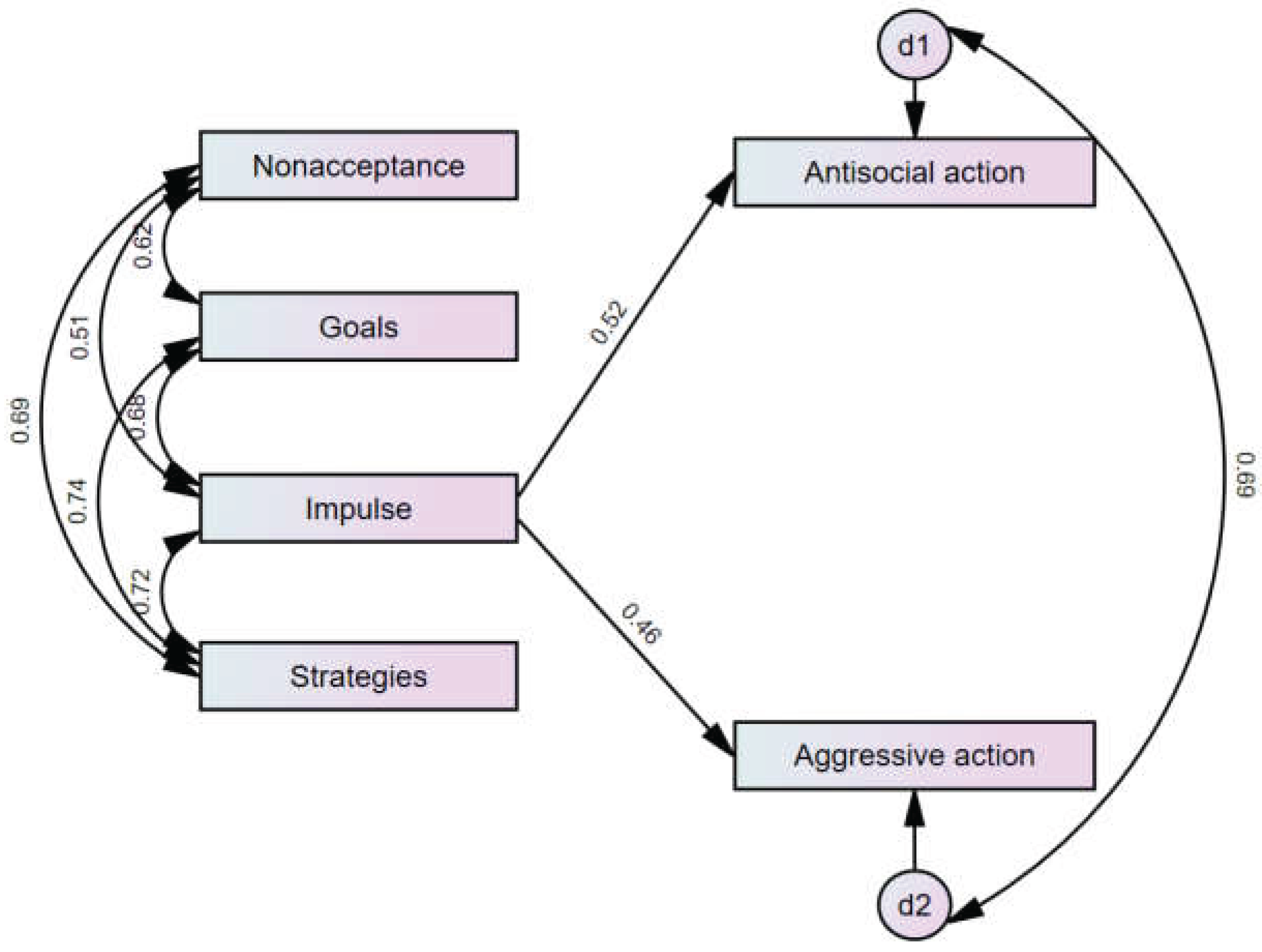
3.1. Path Analysis
3.2. Linear Regression Analysis
4. Discussion
4.1. Emotional Regulation Difficulties in Relation to Substance Use Severity (Hospitalization and Need for Detoxification Treatment)
4.2. The Influence of Type of Substance on Emotion Regulation Difficulties
4.3. Impulsivity, Coping, and Difficulties in Emotional Regulation
4.4. Correlations Between Emotional Regulation Difficulties and Behavioral Coping Strategies
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Over 3 million annual deaths due to alcohol and drug use, majority among men. 25 Jun 2024. Available online: https://www.who.int/news/item/25-06-2024-over-3-million-annual-deaths-due-to-alcohol-and-drug-use-majority-among-men.
- An, J.; Wang González-Roza, Q.; Bai, Z.; et al. Global burden and trend of substance use disorders, self-harm, and interpersonal violence from 1990 to 2021, with projection to 2040. BMC Public Health 2025, 25, 1632. [Google Scholar] [CrossRef]
- González-Roza; Castaño, Y.; Krotter, A.; Salazar-Cedillo, A.; Gervilla, E. Emotional dysregulation in relation to substance use and behavioral addictions: findings from five separate meta-analyses. International Journal of Clinical and Health Psychology 2024, 24(3), 100502. [Google Scholar] [CrossRef]
- Hainagiu, S.M.; Neagu, S.N. Caught in the web—emotional regulation difficulties and internet addiction among Romanian medical and technical university students: a pilot cross-sectional study. Healthcare 2025, 13(19), 2528. [Google Scholar] [CrossRef] [PubMed]
- Stellern, J.; Xiao, K.B.; Grennell, E.; Sanches, M.; Gowin, J.L.; Sloan, M.E. Emotion regulation in substance use disorders: a systematic review and meta-analysis. Addiction 2023, 118(1), 30–47. [Google Scholar] [CrossRef]
- Weiss, N.H.; Bold, K.W.; Sullivan, T.P.; Armeli, S.; Tennen, H. Testing bidirectional associations among emotion regulation strategies and substance use: a daily diary study. Addiction 2017, 112(4), 695–704. [Google Scholar] [CrossRef] [PubMed]
- Lunga, R.A.; Dina, M.M.; Rada, C. The role of executive functions and emotional regulation in substance use: a systematic review. Anthropol Res Stud. 2025, 15, 222–246. [Google Scholar] [CrossRef]
- Hand, L.J.; Paterson, L.M.; Lingford-Hughes, A.R. Re-evaluating our focus in addiction: emotional dysregulation is a critical driver of relapse to drug use. Transl Psychiatry 2024, 14, 467. [Google Scholar] [CrossRef]
- Fischer, R.; Scheunemann, J.; Moritz, S. Coping strategies and subjective well-being: context matters. Journal of Happiness Studies 2021, 22, 3413–3434. [Google Scholar] [CrossRef]
- May, A.C.; Jacobus, J.; Stewart, J.L.; Simmons, A.N.; Paulus, M.P.; Tapert, S.F. Do adolescents use substances to relieve uncomfortable sensations? A preliminary examination of negative reinforcement among adolescent cannabis and alcohol users. Brain Sciences 2020, 10(4), 214. [Google Scholar] [CrossRef]
- Moss, H.B.; Chen, C.M.; Yi, H.Y. Coping motives for alcohol and cannabis use better reflect negative reinforcement: implications for substance use behaviors. Addictive Behaviors Reports 2025, 21, 101500. [Google Scholar] [CrossRef]
- Bostan, C.M.; Zaharia, D.V. Emotional dysregulation—factor structure and consistency in the Romanian version of the Difficulties in Emotion Regulation Scale (DERS). Annals of “Alexandru Ioan Cuza” University of Iași – Psychology Series 2016, 25(2), 57. Available online: https://www.ceeol.com/search/journal-detail?id=537.
- Gratz, K.L.; Roemer, L. Multidimensional assessment of emotion regulation and dysregulation: development, factor structure, and initial validation of the Difficulties in Emotion Regulation Scale. Journal of Psychopathology and Behavioral Assessment 2004, 26, 41–54. [Google Scholar] [CrossRef]
- Hobfoll, S.E. Conservation of resources: a new attempt at conceptualizing stress. American Psychologist 1989, 44(3), 513–524. [Google Scholar] [CrossRef]
- Budău, O.; Albu, M. Scala de Abordare Strategică a Copingului (SACS)[ Strategic Approach to Coping Scale]; Editura ASCR: Cluj-Napoca, Romania, 2010; ISBN 978-606-8244-05-1. [Google Scholar]
- Sequeda, G.; Acosta-López, J.E.; Diaz-Camargo, E.; Torres-Santos, E.A.; López-Ramírez, V.; Rivera-Porras, D. Third-generation therapies for the management of psychoactive substance use in young people: a scoping review. Behavioral Sciences 2024, 14(12), 1192. [Google Scholar] [CrossRef]
- Chrétien, S.; Giroux, I.; Smith, I.; et al. Emotional Regulation in Substance-Related and Addictive Disorders Treatment: A Systematic Review. J Gambl Stud 2025, 17 41, 353–448. [Google Scholar] [CrossRef]
- Torrejón Guirado, M.C.; Baena Jiménez, M.Á; Lima Serrano, M.; de Vries, H.; Mercken, L. The influence of peer’s social networks on adolescent’s cannabis use: a systematic review of longitudinal studies. Frontiers in Psychiatry 2023, 14, 1306439. [Google Scholar] [CrossRef] [PubMed]
- Grecucci, A.; Messina, I.; Amodeo, L.; Lapomarda, G.; Crescentini, C.; Dadomo, H.; Panzeri, M.; Theuninck, A.; Frederickson, J. A dual route model for regulating emotions: comparing models, techniques and biological mechanisms. Front Psychol. 2020, 11, 930. [Google Scholar] [CrossRef]
- Garke, M.Å; Isacsson, N.H.; Sörman, K.; Bjureberg, J.; Hellner, C.; Gratz, K.L.; Berghoff, C.R.; Sinha, R.; Tull, M.T.; Jayaram-Lindström, N. Emotion dysregulation across levels of substance use. Psychiatry Research 2021, 296, 113662. [Google Scholar] [CrossRef] [PubMed]
- Mansueto, G.; Palmieri, S.; Nikčević, A.V.; Caselli, G.; Spada, M.M. The mediating role of emotion dysregulation in the association between impulsivity and severity of substance dependence. Clinical Psychology & Psychotherapy 2026, 33(2), e70250. [Google Scholar] [CrossRef] [PubMed]
- Weiss, N.H.; Kiefer, R.; Goncharenko, S.; Raudales, A.M.; Forkus, S.R.; Schick, M.R.; Contractor, A.A. Emotion regulation and substance use: a meta-analysis. Drug and Alcohol Dependence 2022, 230, 109131. [Google Scholar] [CrossRef]
- Stahl, S.M. Stahl’s essential psychopharmacology: neuroscientific basis and practical applications, 5th ed.; Cambridge University Press: Cambridge, 2021. [Google Scholar]
- Robledo, P. Cannabinoids, opioids and MDMA: neuropsychological interactions related to addiction. Neuroscience & Biobehavioral Reviews 2010, 11(4), 429–439. [Google Scholar] [CrossRef]
- Aldao, A.; Nolen-Hoeksema, S.; Schweizer, S. Emotion-regulation strategies across psychopathology: A meta-analytic review. Clin Psychol Rev. 2010, 30(2), 217–237. [Google Scholar] [CrossRef] [PubMed]
- Kozak, K.; Lucatch, A.M.; Lowe, D.J.E.; Balodis, I.M.; MacKillop, J.; George, T.P. The neurobiology of impulsivity and substance use disorders: implications for treatment. Annals of the New York Academy of Sciences 2019, 1451(1), 71–91. [Google Scholar] [CrossRef]
- Pei, R.; Courtney, A.L.; Ferguson, I.; Brennan, C.; Zaki, J. A neural signature of social support mitigates negative emotion. Scientific Reports 2023, 13, 17293. [Google Scholar] [CrossRef]
- Lunga, R.A.; Rada, C.; Neagu, A.E.; Marinescu, V.; Rodideal, A.A. Substance use and violence in adolescence: emotional and relational dynamics. Anthropol Res Stud. 2026, 16, 1–20. [Google Scholar] [CrossRef]
- Avcı, M. Adolescents’ experiences with substance use: risks, protective factors and interventions. BMC Psychol 2025, 13, 802. [Google Scholar] [CrossRef]
- Muniz, F.B.; Kalina, E.; Patock-Peckham, J.A.; Berberian, S.; Fulop, B.; Williams, J.; Leeman, R.F. A test of the self-medication hypothesis using a latent measurement model: are stress and impaired control over alcohol mediating mechanisms of parenting styles on heavy episodic drinking and alcohol-related problems among university students? Behavioral Sciences 2024, 14(5), 384. [Google Scholar] [CrossRef]
- Gong, H.; Xie, C.; Yu, C.; Sun, N.; Lu, H.; Xie, Y. Psychosocial factors predict the level of substance craving of people with drug addiction: a machine learning approach. International Journal of Environmental Research and Public Health 2021, 18(22), 12175. [Google Scholar] [CrossRef]
- Shafie, A.A.H.; Walid, D.A.; Aziz, A.R.B.A.; Yassin, N.M.; Baharudin, D.F.B.; Othman, K.; Jaladin, R.A.B.M.; Amat, S.; Wahab, S. The effectiveness of a drug abuse prevention module based on self-assertiveness, spirituality and belief in the detriments of drug abuse (MPDASK). Islamic Guidance and Counseling Journal 2023, 6(2). [Google Scholar] [CrossRef]
| DERS Subscales | Alpha | Items | Mean | Standard Deviation | Median | Variance |
|---|---|---|---|---|---|---|
| Nonacceptance | 0.883 | 6 | 15.62 | 6.12 | 15.00 | 37.51 |
| Goals | 0.798 | 5 | 14.12 | 4.61 | 14.00 | 21.29 |
| Impulse | 0.865 | 6 | 14.72 | 5.89 | 14.00 | 34.70 |
| Awareness | 0.740 | 6 | 14.96 | 4.62 | 15.00 | 21.38 |
| Strategies | 0.866 | 8 | 19.09 | 6.93 | 18.00 | 48.07 |
| Clarity | 0.811 | 5 | 10.42 | 4.18 | 10.00 | 17.46 |
| SACS Subscales | Alpha | Items | Mean | Standard Deviation | Variance |
|---|---|---|---|---|---|
| Assertive action | 0.406 | 9 | 29.31 | 4.929 | 24.296 |
| Social Joining | 0.605 | 5 | 15.18 | 4.232 | 17.908 |
| Seeking social support | 0.757 | 7 | 18.52 | 5.659 | 32.021 |
| Cautious action | 0.665 | 5 | 15.41 | 4.288 | 18.384 |
| Instinctive action | 0.704 | 6 | 20.33 | 5.022 | 25.222 |
| Avoidance | 0.736 | 6 | 16.40 | 5.260 | 27.671 |
| Indirect action | 0.678 | 4 | 10.28 | 3.732 | 13.924 |
| Antisocial action | 0.785 | 5 | 11.88 | 4.867 | 23.686 |
| Aggressive action | 0.710 | 5 | 12.10 | 4.005 | 16.044 |
| Subscale / Total DERS |
Hospitalized group (M ± SD) | Non-hospitalized group (M ± SD) | t | p | Cohen d |
|---|---|---|---|---|---|
| NONACCEPTANCE | 16.61 ± 5.88 | 14.21 ± 6.22 | -2.77 | .006 | -0.39 |
| GOALS | 14.98 ± 4.40 | 12.90 ± 4.66 | -3.22 | .002 | -0.46 |
| IMPULSE | 16.13 ± 6.22 | 12.71 ± 4.73 | -4.22 | < .001 | -0.60 |
| STRATEGIES | 20.40 ± 6.94 | 17.21 ± 6.51 | -3.28 | < .001 | -0.47 |
| AWARENESS | — | — | — | ns | — |
| CLARITY | — | — | — | ns | — |
| Total DERS | 93.81 ± 23.40 | 81.98 ± 21.79 | -3.62 | < .001 | -0.52 |
| Substance | Subscale / Total DERS |
Substance users group (M ± SD) |
Non-users group (M ± SD) |
Difference (t, p, d) |
|---|---|---|---|---|
| Opioids | IMPULSE | 15.13 ± 5.96 | 11.31 ± 3.60 | t=-2.92, p=.004, d=-0.66 |
| Canabis | CLARITY | 11.74 ± 4.24 | 9.52 ± 3.90 | t=-3.81, p<.001, d=-0.54 |
| MDMA | GOALS | 15.24 ± 4.23 | 13.75 ± 4.68 | t=-1.98, p=.048, d=-0.32 |
| Cocaine | GOALS IMPULSE CLARITY Total DERS |
15.03 ± 4.91 15.03 ± 4.91 15.03± 4.91 94.06 ± 24.25 |
13.50 ± 4.31 13.50 ± 4.31 13.50± 4.31 85.46 ± 22.31 |
t=-2.32, p=.021, d=-0.33; Total: t=-2.58, p=.010, d=-0.37 |
| NPS (New Psychoactive Substances) | GOALS IMPULSE | 15.50 ± 4.10 16.40 ± 5.69 |
13.57 ± 4.70 14.05 ± 5.85 |
t=-2.72, p=.007, d=-0.42; t=-2.58, p=.011, d=-0.40 |
| 95%CI for B | |||||||
|---|---|---|---|---|---|---|---|
| Variable | B | SE | beta | t | p | Lower | Upper |
| (Constant) | 13.89 | 2.409 | 5.770 | <.001 | 9.15 | 18.65 | |
| AA | -.202 | .074 | -.169 | -2.729 | .007 | -.348 | -.056 |
| SS | -.172 | .062 | -.166 | -2.773 | .006 | -.295 | -.050 |
| AS | .413 | .111 | .341 | 3.722 | <.001 | .194 | .632 |
| AG | .415 | .142 | .282 | 2.924 | .004 | .135 | .695 |
| Variable | SACS subscale | r | p | 95% CI (Lower) |
95% CI (Upper) |
|---|---|---|---|---|---|
| DERS | AA (Assertive Action) | -0.307*** | < .001 | -0.427 | -0.176 |
| DERS | AV (Avoidance) | 0.299*** | < .001 | 0.167 | 0.420 |
| DERS | IAc (Indirect Action) | 0.306*** | < .001 | 0.175 | 0.426 |
| DERS | AS (Antisocial Action) | 0.371*** | < .001 | 0.245 | 0.485 |
| DERS | AG (Aggressive Action) | 0.225** | .001 | 0.090 | 0.353 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




