Submitted:
09 April 2026
Posted:
10 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Handpieces Tested, Clinical Use, Sterilization, and Maintenance Conditions
2.3. Functional Performance Testing and Rotor Surface Characterization Protocol
2.4. Rotor Surface Characterization
2.5. Statistical Analysis
3. Results
3.1. Functional Performance Changes Following Clinical Use
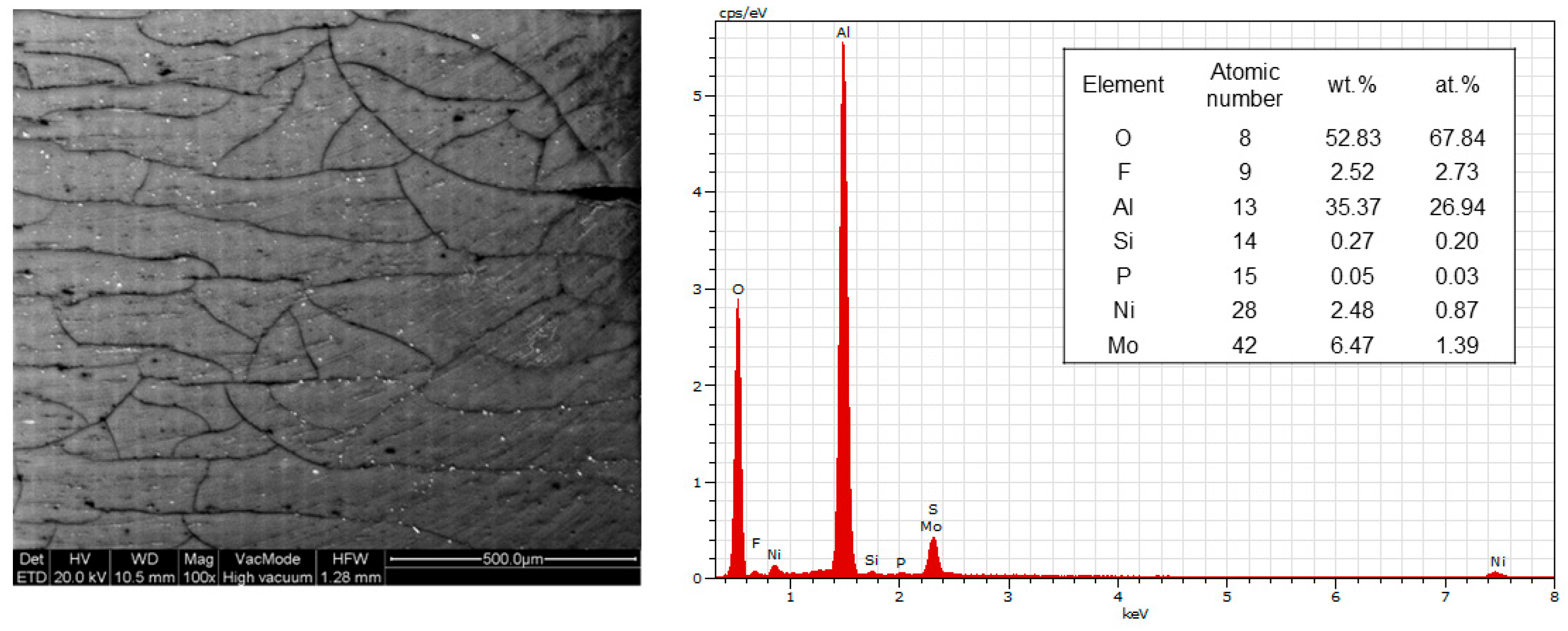
3.2. Rotor Surface Characterization

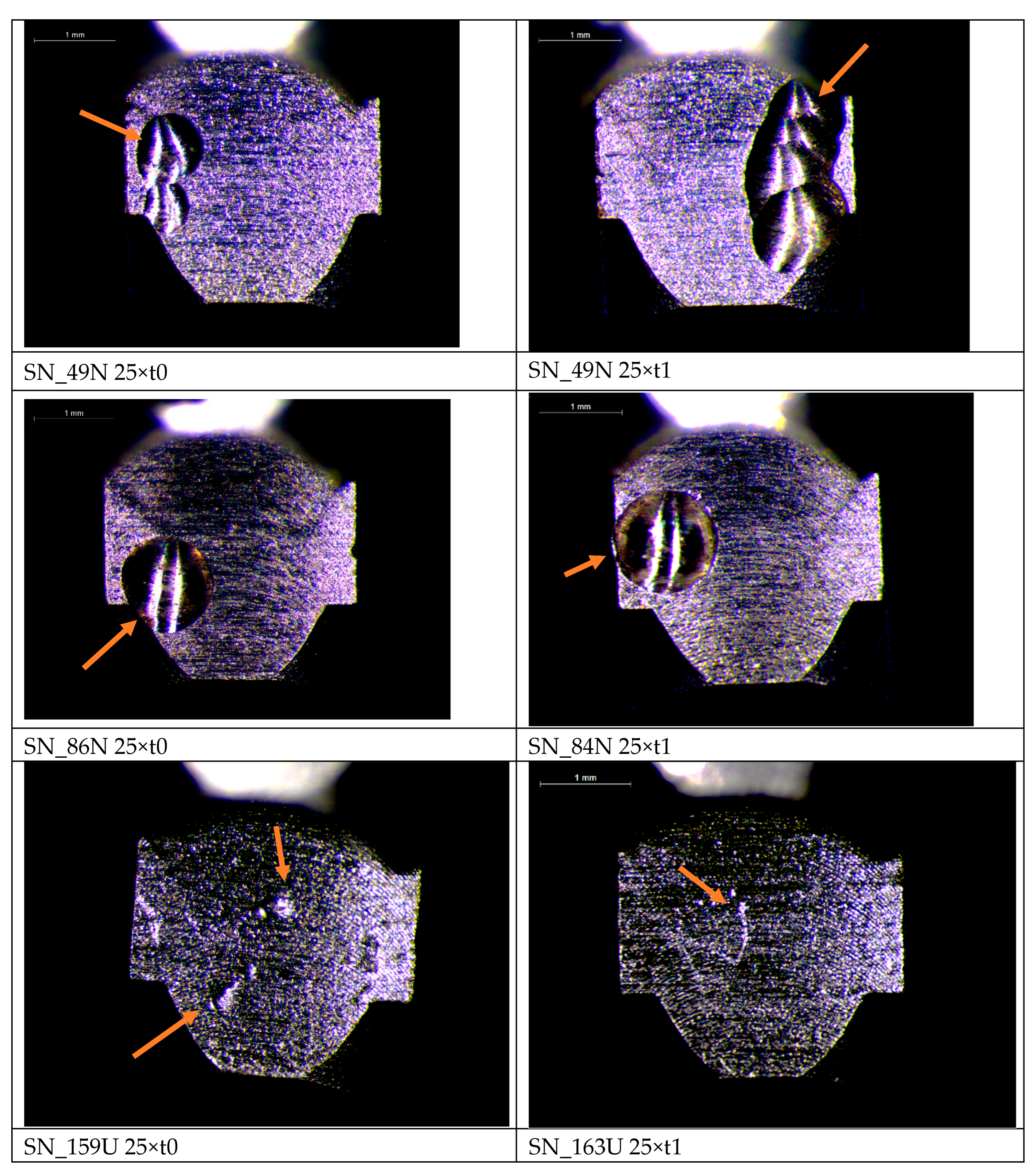
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Stephens, R. R. The dental handpiece-a history of its development. Aust Dent J 1986, 31, 165–180.
- Dyson, J.E.; Darvell, B.W. The development of the dental high-speed air turbine handpiece. Part 1. Aust Dent J 1993, 38, 49-58.
- Dyson, J.E.; Darvell, B.W. The development of the dental high-speed air turbine handpiece. Part 2. Aust Dent J 1993, 38, 131-43.
- Chen, Y.; Zhang, H.; Li, X.; Xiao, S.; Gu, F.; Shi, Z. Effects of Wear on Lubrication Performance and Vibration Signatures of Rotor System Supported by Hydrodynamic Bearings. Lubricants 2023, 11, 107. [CrossRef]
- Leonard, L.D.; Charlton, D.G. Performance of high-speed dental Handpeces subjected to simulated clinical use and sterilization. J Amer Dent Assoc 1999, 130, 1301-11.
- Lewis, D. L.; Arens, M.; Appleton, S. S.; Nakishima, K.; Ryn, J.; Boe, R. K.; Patrick, J. B.; Watanabe, D. T.; Suziki, M. Cross contamination potential with dental equipment. Lancet 1992, 340, 1252-1254.
- Lewis, D. L. Handpiece sterilisation. J Amer Dent Assoc 1992, 123, 14-15.
- Lewis, D.L.; Boe, R.K. Cross-infection risks associated with current procedures for using high-speed dental handpieces. J Clin Microbiol. 1992,30,401-6. [CrossRef]
- Centers for Disease Control and Prevention. Guidelines for Infection Control in Dental Health-Care Settings — 2003. MMWR 2003, 52, 30.
- Infection Prevention and Control in Dental Practice: Revised version adopted by the General Assembly 27-29 September 2021, Sydney, AustraliaRevised version adopted by the General Assembly: September 2019, San Francisco, United States of AmericaOriginal version adopted by the General Assembly: September 2009, Singapore, Singapore. Int Dent J. 2022 Feb;72(1):16-18. [CrossRef]
- Winter, S. Investigating the steam sterilization of dental handpieces. (Doctoral Dissertation). University of Glasgow. Glascow, United Kingdom, 2016. Available online: https://theses.gla.ac.uk/7057/.
- Sasaki, J.I.; Imazato, S. Autoclave sterilization of dental handpieces: A literature review. J Prosthodont Res 2020, 64, 239-242.
- Wu, S.-X.; Gong, X.; Ni, Y.-Q.; Chen, W.-L.; Wang, C.-Y. Material Removal and Surface Damage in High-Speed Grinding of Enamel. J. Mech. Behav. Biomed. Mater. 2022, 136, 105532. [CrossRef]
- Pegg, J.E.; Lothamer, C.; Rawlinson, J.E. The Air-Driven Dental Unit: Form and Function at a Mechanical Level. J Vet Dent 2019,36, 202-208.
- Williams, G. Anatomy of a handpiece: Understanding handpiece maintenance and repairs. 2021. Available online: https://dentalacademyofce.com/wp-content/uploads/2022/03/Anatomy-of-a-handpiece.pdf (accessed on 11 December 2025).
- Marin, E.; Lanzutti, A. Biomedical Applications of Titanium Alloys: A Comprehensive Review. Materials 2024, 17, 114. [CrossRef]
- Angelini, E. Influence of sterilization on the corrosion resistance of high-speed dental handpieces. Quintessence Int. 1992, 23, 215-22.
- Wei, W.; Dyson, J.E.; Darvell, B.W. Factors Affecting Dental Air-Turbine Handpiece Bearing Failure Oper Dent 2012, 37, E1-12.
- Su, B.; Lu, C.; Li, C. Current Status of Research on Hybrid Ceramic Ball Bearings. Machines 2024, 12, 510. [CrossRef]
- Wei, M.; Dyson, J.E.; Darvell, B.W. Failure analysis of the ball bearings of dental air turbine handpieces. Aust Dent J. 2013, 58, 514-21.
- Dreier, J.; Brütting, C.; Ruckdäschel, H.; Altstädt, V.; Bonten, C. Investigation of the Thermal and Hydrolytic Degradation of Polylactide during Autoclave Foaming. Polymers 2021, 13, 2624. [CrossRef]
- Holliday, R.; Venugopal, S.; Howell, A.; Keys, W. Operator's ability at assessing a high-speed (air turbine) handpiece before use: an audit. Br Dent J 2015, 218, E3.
- Gegauff, A.G.; Rosenstiel, S.F.; Johnston, W.M.; Gangji, R.K. Handpiece degradation associated with performance testing of diamond rotary cutting instruments. Aust Dent J. 1998 Oct;43(5):342-8. PMID: 9848987. [CrossRef]
- Dyson, J.E.; Darvell, B.W. Torque, power and efficiency characterization of dental air turbine handpieces. J Dent 1999, 27, 573-586.
- Dyson, J.E.; Darvell, B.W. Flow and free running speed characterization of dental air turbine handpieces. J Dent 1999,27,465-77. PMID: 10507202. [CrossRef]
- Brockhurst, P.J.; Shams, R. Dynamic measurement of the torque-speed characteristics of dental high speed air turbine handpieces. Aust Dent J 1994, 39, 33-8. PMID: 8185538. [CrossRef]
- Huang, Y.C.; Chen, P.C. Failure Diagnosis for Dental Air Turbine Handpiece with Payload Using Feature Engineering and Temporal Convolution Network. Bioengineering 2024, 11, 555.
- Hunter, T. Dental handpieces: Maintenance, repair, and infection control, 3rd edition. 2021. Available online: https://dentalacademyofce.com/wp-content/uploads/2022/03/2102CEDhun-1.pdf (accessed on 11 December 2025).
- Monagahn, D.M.; Wilson, N.H.; Darvell, B.W. The performance of air-turbine handpieces in general dental practice. Oper Dent. 2005, 30, 16-25.
- Edwardsson, S.; Svensäter, G.; Birkhed, D. Steam sterilization of air turbine dental handpieces. Acta Odontol Scand. 1983, 41, 321-6. PMID: 6362319. [CrossRef]
- Bhandary, N.; Desai, A.; Shetty, Y.B. High speed handpieces. J Int Oral Health. 2014 Feb;6(1):130-2. Epub 2014 Feb 26. PMID: 24653618; PMCID: PMC3959152. https://www.asaphandpiece.com/handpiece-terminology.
- Winter, S.; Smith, A.; Lappin, D.; McDonagh, G.; Kirk, B. Failure of non-vacuum steam sterilization processes for dental handpieces. J Hosp Infect. 2017,97,343-347. PMID: 28903057. Epub 2017 Sep 10. [CrossRef]
- ISO 25178-2; ISO 25178-2:2021. Geometrical product specifications (GPS) — Surface texture: Areal. Part 2: Terms, definitions and surface texture parameters. Edition 2, 2021.
- Worthington, L.; Martin, M.V. An investigation of the effect of repeated autoclaving on the speed of some dental turbines in general dental practice. J Dent. 1998, 26, 75-7.
- Lloyd, L., Burke, F. J. T.; Cheung, S. W. Handpiece asepsis: a survey of the attitudes of dental practitioners, Br Dent J 1995, 178, 23-27.
- Christensen, GJ. The high-speed handpiece dilemma. J Am Dent Assoc. 1999,130,1494-6. PMID: 10570597. [CrossRef]
- Stachowiak, G.W.; Batchelor, A.W. Engineering Tribology, 4th ed.; Butterworth-Heinemann, 2014. https://www.sciencedirect.com/book/9780123970473/engineering-tribology.
- Hutchings, I.M.; Shipway, P. Tribology: Friction and Wear of Engineering Materials, 2nd ed.; Butterworth-Heinemann, 2017. https://www.sciencedirect.com/book/9780081009109/tribology.
- The complete guide to dental handpieces. DD Group. Available online: https://www.ddgroup.com/news/guide-to-dental-handpieces/ (accessed on 11 December 2025).
- White, F.M. Fluid Mechanics, 8th ed.; McGraw-Hill, 2016.

| Turbine | Serial Number (SN) | Speed (t0)/rpm | Speed (t1)/rpm |
| 1 | CTMN0084 | 340000 | 317000 |
| 2 | CTMN0068 | 329000 | 329000 |
| 3 | CTMN0107 | 335000 | Off |
| 4 | CTMN0101 | 325000 | 307000 |
| 5 | CTMN0115 | 327000 | Off |
| 6 | CTMN0110 | 330000 | 292000 |
| 7 | CTMN0075 | 334000 | 333700 |
| 8 | CTMN0124 | 326700 | 312000 |
| 9 | CTMN0049 | 331000 | 298000 |
| 10 | CTMN0070 | 336000 | 289000 |
| 11 | CTMN0086 | 328000 | 323000 |
| 12 | CTMN0118 | 334000 | 307000 |
| 13 | CTMN0119 | 332200 | 317000 |
| 14 | CTMN0090 | 340000 | 311000 |
| 15 | CTMN0116 | 325000 | 287000 |
| Means and standard deviations | 331608 (5051)a | 309438 (14851)b |
| Turbine | Serial Number (SN) | Friction grip (t0)/N | Friction grip (t1)/N |
| 1 | CTMN0084 | 28.1 | 25.8 |
| 2 | CTMN0068 | 29.4 | 29 |
| 3 | CTMN0107 | 28.8 | Off |
| 4 | CTMN0101 | 27.7 | 11.8 |
| 5 | CTMN0115 | 30.5 | Off |
| 6 | CTMN0110 | 30.2 | 13.7 |
| 7 | CTMN0075 | 29.4 | 18.9 |
| 8 | CTMN0124 | 28.3 | 16.1 |
| 9 | CTMN0049 | 29.6 | 16.1 |
| 10 | CTMN0070 | 29.3 | 24.5 |
| 11 | CTMN0086 | 28.5 | 24.2 |
| 12 | CTMN0118 | 29.7 | 12.5 |
| 13 | CTMN0119 | 29.1 | 21.4 |
| 14 | CTMN0090 | 28.7 | 16 |
| 15 | CTMN0116 | 28.1 | 22.6 |
| Means and standard deviations | 28.9 (0.8)a | 19.4 (5.5)b |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




