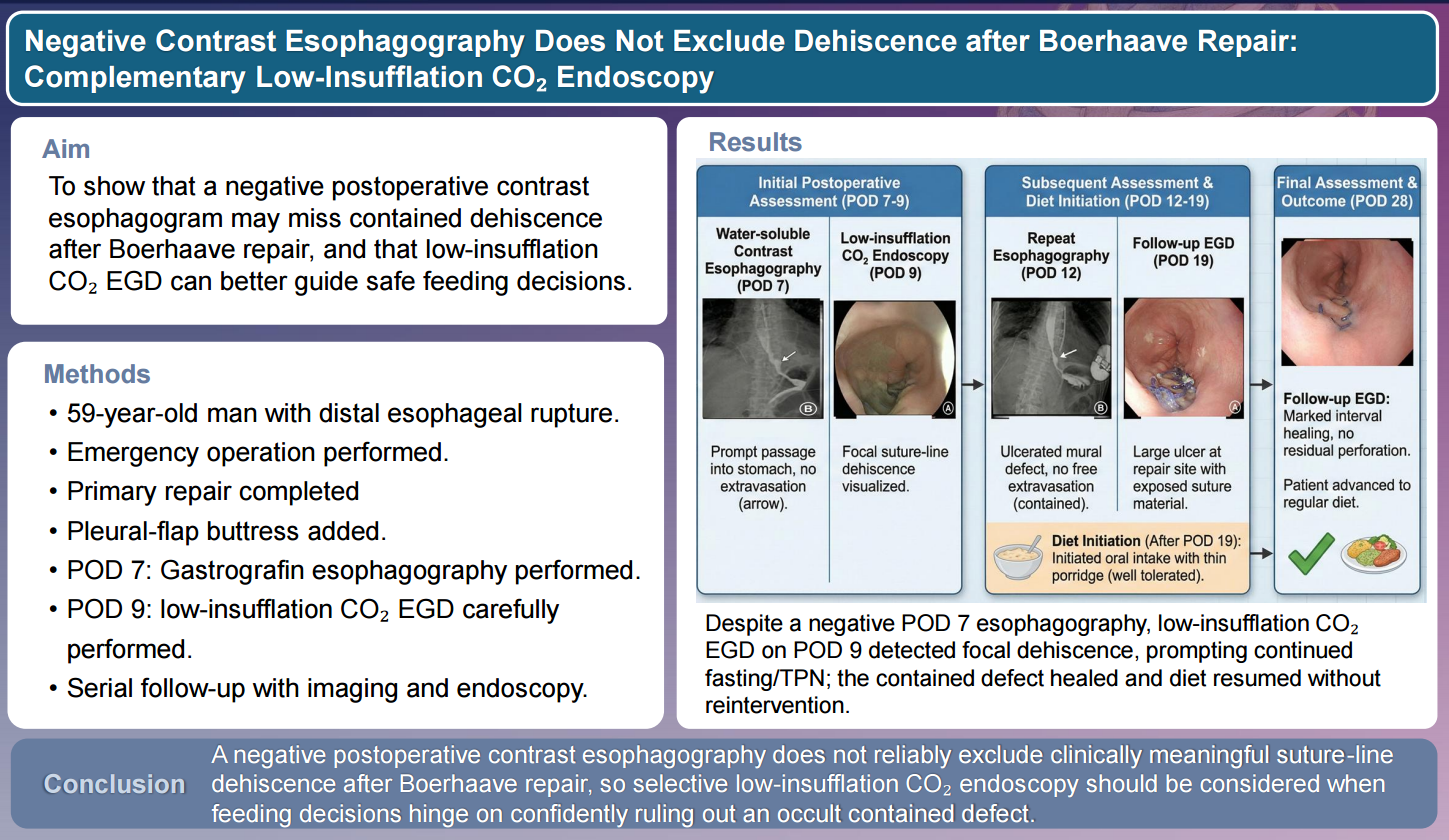
After repair of Boerhaave syndrome, assessment of repair integrity is important because occult dehiscence may progress to mediastinitis or pleural sepsis. Water-soluble contrast esophagography is commonly used before resuming oral intake, but absence of contrast extravasation does not necessarily exclude a small or contained defect. We report a 59-year-old man with post-emetic distal esophageal rupture who underwent emergency primary repair with pleural-flap buttress and drainage. Although he remained clinically stable, water-soluble contrast esophagography on postoperative day (POD) 7 showed no extravasation. Because feeding decisions required greater structural confidence, low-insufflation carbon dioxide (CO2) esophagogastroduodenoscopy (EGD) was performed on POD 9 and revealed focal suture-line dehiscence. Oral intake was deferred, and conservative management with fasting and total parenteral nutrition was continued. Serial reassessment suggested a contained defect, and oral intake was reintroduced cautiously. A regular diet was started only after POD 28 endoscopy showed marked interval healing, and follow-up endoscopy at 3 months confirmed complete mucosal healing. This case highlights that negative postoperative contrast esophagography does not exclude persistent dehiscence and that low-insufflation CO2 endoscopy may provide useful complementary structural information in selected patients.