Submitted:
02 April 2026
Posted:
03 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Type of Study
2.2. Study Location
2.3. Study Population
2.4. Data Collection and Study Variables
2.5. Data Analysis
2.6. Ethical Aspects
3. Results
4. Discussion
4.1. Overview and Summary of the Findings
4.2. Direct and Indirect Impact of the COVID-19 Pandemic
4.3. Racial Inequalities and the Persistence of Institutional Racism
4.4. Maternal Age: Increasing Risks with Advancing Age
4.5. Regional Inequality and the Organization of the Health System
4.6. Profile of Causes: Balance Between Direct and Indirect Causes
4.7. Portugal: Variability, Smaller Magnitude, and Data Limitations
4.8. Limitations, Implications, and Contributions to Clinical Practice
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Guidelines and Standards Statement
Use of Artificial Intelligence
Abbreviations
| ICU | Intensive Care Unit |
| INE | Instituto Nacional de Estatística |
| SDGs | Sustainable Development Goals |
| SIM | Sistema de Informação de Mortalidade |
| SINASC | Sistema de Informações sobre Nascidos Vivos |
| STROBE | Strengthening the Reporting of Observational Studies in Epidemiology |
References
- Silva, AD; Guida, JPS; Santos, DS; Santiago, SM; Surita, FG. Racial disparities and maternal mortality in Brazil: findings from a national database. Rev Saude Publica 2024, 58, 25. [Google Scholar] [CrossRef] [PubMed]
- Cambou, MC; David, H; Moucheraud, C; Nielsen-Saines, K; Comulada, WS; Macinko, J. Time series analysis of comprehensive maternal deaths in Brazil during the COVID-19 pandemic. Sci Rep. 2024, 14(1), 23960. [Google Scholar] [CrossRef] [PubMed]
- Carvalho-Sauer, R; Costa, MDCN; Teixeira, MG; Flores-Ortiz, R; Leal, JTFM; Saavedra, R; Paixao, ES. Maternal and perinatal health indicators in Brazil over a decade: assessing the impact of the COVID-19 pandemic and SARS-CoV-2 vaccination through interrupted time series analysis. Lancet Reg Health Am 2024, 35, 100774. [Google Scholar] [CrossRef]
- Ferreira, N; Ferreira, M; Santos, E; Ferreira, S; de Arriaga, MT; Costa, A. Health literacy and its determinants among pregnant women in Portugal. BMC Public Health 2025, 25(1), 2963. [Google Scholar] [CrossRef]
- Tavares, M; Alexandre-Sousa, P; Victória, A; Loureiro, S; Santos, AP; Mendes, J. Experience of Labour and Childbirth in a Sample of Portuguese Women: A Cross-Sectional Study. Healthcare (Basel) 2024, 12(21), 2125. [Google Scholar] [CrossRef] [PubMed]
- Lee, S; Kim, S; Lee, H; Park, J; Son, Y; López Sánchez, GF; Pizzol, D; Lee, J; Lee, YJ; Lee, H; Kim, HJ; Smith, L; Woo, S; Yon, DK. Global, Regional, and National Trends in Maternal Mortality Ratio Across 37 High Income Countries From 1990 to 2021, With Projections up to 2050: A Comprehensive Analysis From the WHO Mortality Database. J Korean Med Sci. 2025, 40(21), e85. [Google Scholar] [CrossRef]
- Barros, FC; Gunier, RB; Rego, A; Sentilhes, L; Rauch, S; Gandino, S; Teji, JS; et al. Maternal vaccination against COVID-19 and neonatal outcomes during Omicron: INTERCOVID-2022 study. Am J Obstet Gynecol 2024, 231(4), 460.e1–460.e17. [Google Scholar] [CrossRef]
- Oliveira, IMGD; Fonseca, EPD; França, FMG; Cortellazzi, KL; Pardi, V; Pereira, AC; Tagliaferro, EPDS. Age and Type of Delivery as Risk Indicators for Maternal Mortality. Rev Bras Ginecol Obstet 2023, 45(3), 134–141. [Google Scholar] [CrossRef]
- von Elm, E; Altman, DG; Egger, M; Pocock, SJ; Gøtzsche, PC; Vandenbroucke, JP; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008, 61(4), 344–9. [Google Scholar] [CrossRef]
- Cresswell, JA; Alexander, M; Chong, MYC; Link, HM; Pejchinovska, M; Gazeley, U; Ahmed, SMA; Chou, D; Moller, AB; Simpson, D; Alkema, L; Villanueva, G; Sguassero, Y; Tunçalp, Ö; Long, Q; Xiao, S; Say, L. Global and regional causes of maternal deaths 2009-20: a WHO systematic analysis. Lancet Glob Health 2025, 13(4), e626–e634. [Google Scholar] [CrossRef]
- Lee, S; Kim, S; Lee, H; Park, J; Son, Y; López Sánchez, GF; Pizzol, D; Lee, J; Lee, YJ; Lee, H; Kim, HJ; Smith, L; Woo, S; Yon, DK. Global, Regional, and National Trends in Maternal Mortality Ratio Across 37 High Income Countries From 1990 to 2021, With Projections up to 2050: A Comprehensive Analysis From the WHO Mortality Database. J Korean Med Sci. 2025, 40(21), e85. [Google Scholar] [CrossRef] [PubMed]
- Ward, ZJ; Atun, R; King, G; Sequeira Dmello, B; Goldie, SJ. Assessing differences in country-level estimates of maternal mortality: a comparison of GMatH, UN, and GBD model results for 2020. EClinicalMedicine 2025, 88, 103505. [Google Scholar] [CrossRef]
- Souza, JP; Day, LT; Rezende-Gomes, AC; Zhang, J; Mori, R; Baguiya, A; Jayaratne, K; Osoti, A; Vogel, JP; Campbell, O; Mugerwa, KY; Lumbiganon, P; Tunçalp, Ö; Cresswell, J; Say, L; Moran, AC; Oladapo, OT. A global analysis of the determinants of maternal health and transitions in maternal mortality. Lancet Glob Health 2024, 12(2), e306–e316. [Google Scholar] [CrossRef] [PubMed]
- Orellana, JDY; Leventhal, DGP; Flores-Quispe, MDP; Marrero, L; Jacques, N; Morón-Duarte, LS; Boschi-Pinto, C. Impact of the COVID-19 pandemic on excess maternal deaths in Brazil: A two-year assessment. PLoS One 2024, 19(4), e0298822. [Google Scholar] [CrossRef]
- La Verde, M; Riemma, G; Torella, M; Cianci, S; Savoia, F; Licciardi, F; Scida, S; Morlando, M; Colacurci, N; De Franciscis, P. Maternal death related to COVID-19: A systematic review and meta-analysis focused on maternal co-morbidities and clinical characteristics. Int J Gynaecol Obstet. 2021, 154(2), 212–219. [Google Scholar] [CrossRef] [PubMed]
- Cañedo, MC; Lopes, TIB; Rossato, L; Nunes, IB; Faccin, ID; Salomé, TM; Simionatto, S. Impact of COVID-19 pandemic in the Brazilian maternal mortality ratio: A comparative analysis of Neural Networks Autoregression, Holt-Winters exponential smoothing, and Autoregressive Integrated Moving Average models. PLoS One 2024, 19(1), e0296064. [Google Scholar] [CrossRef]
- Scheler, CA; Discacciati, MG; Vale, DB; Lajos, GJ; Surita, FG; Teixeira, JC. Maternal Deaths from COVID-19 in Brazil: Increase during the Second Wave of the Pandemic. Rev Bras Ginecol Obstet [Internet] 2022J, 44(6), 567–72. [Google Scholar] [CrossRef]
- Kassa, ZY; Scarf, V; Turkmani, S; Fox, D. Impact of COVID-19 on Maternal Health Service Uptake and Perinatal Outcomes in Sub-Saharan Africa: A Systematic Review. Int J Environ Res Public Health 2024, 21(9), 1188. [Google Scholar] [CrossRef]
- Diniz, D; Brito, L; Rondon, G. Maternal mortality and the lack of women-centered care in Brazil during COVID-19: Preliminary findings of a qualitative study. Lancet Reg Health Am 2022, 10, 100239. [Google Scholar] [CrossRef]
- Montalmant, KE; Ettinger, AK. The Racial Disparities in Maternal Mortality and Impact of Structural Racism and Implicit Racial Bias on Pregnant Black Women: A Review of the Literature. J Racial Ethn Health Disparities 2024, 11(6), 3658–3677. [Google Scholar] [CrossRef]
- Santana, AT; Couto, TM; Lima, KTRDS; Oliveira, PS; Bomfim, ANA; Almeida, LCG; Rusmando, LCS. Obstetric racism, a debate under construction in Brazil: perceptions of black women on obstetric violence. Cien Saude Colet Portuguese, English. 2024, 29(9), e09952023. [Google Scholar] [CrossRef]
- Ferreira, GAT; Cherchiglia, ML; Valk, M; Pilecco, FB. Mortality trends among Indigenous women of reproductive age in Brazil: a time series analysis. Lancet Reg Health Am 2025, 48, 101183. [Google Scholar] [CrossRef] [PubMed]
- Tenorio, DS; de Matos Brasil, AG; Nogueira, BG; Rolim Lima, NN; Araújo, JEB; Rolim Neto, ML. High maternal mortality rates in Brazil: Inequalities and the struggle for justice. Lancet Reg Health Am 2022, 14, 100343. [Google Scholar] [CrossRef] [PubMed]
- Hailu, EM; Maddali, SR; Snowden, JM; Carmichael, SL; Mujahid, MS. Structural racism and adverse maternal health outcomes: A systematic review. Health Place 2022, 78, 102923. [Google Scholar] [CrossRef]
- Tanaka, H; Hasegawa, J; Katsuragi, S; Tanaka, K; Arakaki, T; Nakamura, M; Hayata, E; Nakata, M; Murakoshi, T; Sekizawa, A; Ishiwata, I; Ikeda, T. High maternal mortality rate associated with advanced maternal age in Japan. Sci Rep. 2023, 13(1), 12918. [Google Scholar] [CrossRef]
- Hochler, H; Lipschuetz, M; Suissa-Cohen, Y; Weiss, A; Sela, HY; Yagel, S; Rosenbloom, JI; Grisaru-Granovsky, S; Rottenstreich, M. The Impact of Advanced Maternal Age on Pregnancy Outcomes: A Retrospective Multicenter Study. J Clin Med. 2023, 12(17), 5696. [Google Scholar] [CrossRef] [PubMed]
- Nyongesa, P; Ekhaguere, OA; Marete, I; Tenge, C; Kemoi, M; Bann, CM; Bucher, SL; Patel, AB; Hibberd, PL; Naqvi, F; Saleem, S; Goldenberg, RL; Goudar, SS; Derman, RJ; Krebs, NF; Garces, A; Chomba, E; Carlo, WA; Mwenechanya, M; Lokangaka, A; Tshefu, AK; Bauserman, M; Koso-Thomas, M; Moore, JL; McClure, EM; Liechty, EA; Esamai, F. Maternal age extremes and adverse pregnancy outcomes in low-resourced settings. Front Glob Womens Health 2023, 4, 1201037. [Google Scholar] [CrossRef]
- Pinho Neto, V; Machado, C; Lima, F; Roman, S; Dutra, G. Inequalities in the geographic access to delivery services in Brazil. BMC Health Serv Res. 2024, 24(1), 1598. [Google Scholar] [CrossRef]
- Albuquerque, PC; Almeida, LM; Sá, LMA; Silva, LL; Melo, TF; Camargo, KR; et al. Geographic accessibility to hospital childbirths in Brazil: a national spatial-temporal analysis. Lancet Reg Health Am. 2025, 43, 100303. [Google Scholar]
- Domingues, RMSM; Rodrigues, AS; Dias, MAB; Saraceni, V; Francisco, RPV; Pinheiro, RS; Coeli, CM. Maternal health surveillance panel: a tool for expanding epidemiological surveillance of women’s health and its determinants. Rev Bras Epidemiol 2024, 27, e240009. [Google Scholar] [CrossRef]
- Ranzani, OT; Marinho, MF; Bierrenbach, AL. Usefulness of the Hospital Information System for maternal mortality surveillance in Brazil. Rev Bras Epidemiol 2023, 26, e230007. [Google Scholar] [CrossRef] [PubMed]
- Alipour, J; Payandeh, A; Karimi, A. Prevalence of maternal mortality causes based on ICD-MM: a systematic review and meta-analysis. BMC Pregnancy Childbirth 2023, 23(1), 821. [Google Scholar] [CrossRef] [PubMed]
- Muriithi, FG; Ameh, CA; Gakuo, RW; Williams, CR; Devall, A; Coomarasamy, A; Fawcus, S. Variability in the Causes and Delay Factors Contributing to Maternal Mortality: Evidence From Maternal Death Surveillance Reports of 22 African Countries. BJOG 2025. [Google Scholar] [CrossRef]
- Jiang, J; Qin, L; Wang, B. Long-term dynamic burden and attributable risk analysis of indirect maternal mortality over the past 30 years: an observational study and insights for perioperative management in the next decade. Int J Surg 2025, 111(9), 5783–5795. [Google Scholar] [CrossRef]
- Sabr, Y; Lisonkova, S; Mayer, C; Joseph, KS. Temporal Changes in the Contribution of Chronic Disease to Maternal Mortality in the United States. Paediatr Perinat Epidemiol 2025, 39(6), 527–539. [Google Scholar] [CrossRef]
- Wu, N; Ye, E; Ba, Y; Caikai, S; Ba, B; Li, L; Zhu, Q. The global burden of maternal disorders attributable to iron deficiency related sub-disorders in 204 countries and territories: an analysis for the Global Burden of Disease study. Front Public Health 2024, 12, 1406549. [Google Scholar] [CrossRef]
- Ekwuazi, EK; Chigbu, CO; Ngene, NC. Reducing maternal mortality in low- and middle-income countries. Case Rep Womens Health 2023, 39, e00542. [Google Scholar] [CrossRef]
- Gomes, MC; Ventura, MT; Nunes, RS. How many maternal deaths are there in Portugal? J Matern Fetal Neonatal Med. 2012, 25(10), 1975–9. [Google Scholar] [CrossRef]
- Bouvier-Colle, MH; Mohangoo, AD; Gissler, M; Novak-Antolic, Z; Vutuc, C; Szamotulska, K; Zeitlin, J; Euro-Peristat Scientific Committee. What about the mothers? An analysis of maternal mortality and morbidity in perinatal health surveillance systems in Europe. BJOG 2012, 119(7), 880–9; discussion 890. [Google Scholar] [CrossRef]
- Peppe, MV; Costa, FBPD; Pedrilio, LS; Prado, CAC; Baraldi, ACP; Stefanello, J. Analysis of the influence of the COVID-19 pandemic on maternal mortality trends, 2011-2021. Rev Lat Am Enfermagem 2025, 33, e4668. [Google Scholar] [CrossRef] [PubMed]
| Variable/Category | n | % |
|---|---|---|
| Race | ||
| White | 2.436 | 31.7% |
| Black | 917 | 11.9% |
| Yellow | 21 | 0.3% |
| Brown | 4.036 | 52.5% |
| Indigenous | 139 | 1.8% |
| Unknown | 141 | 1.8% |
| Age range | ||
| 10–14 years | 37 | 0.5% |
| 15–19 years | 600 | 7.8% |
| 20–29 years | 2.880 | 37.5% |
| 30–39 years | 3.473 | 45.2% |
| 40–49 years | 686 | 8.9% |
| 50–59 years | 14 | 0.2% |
| Region of residence | ||
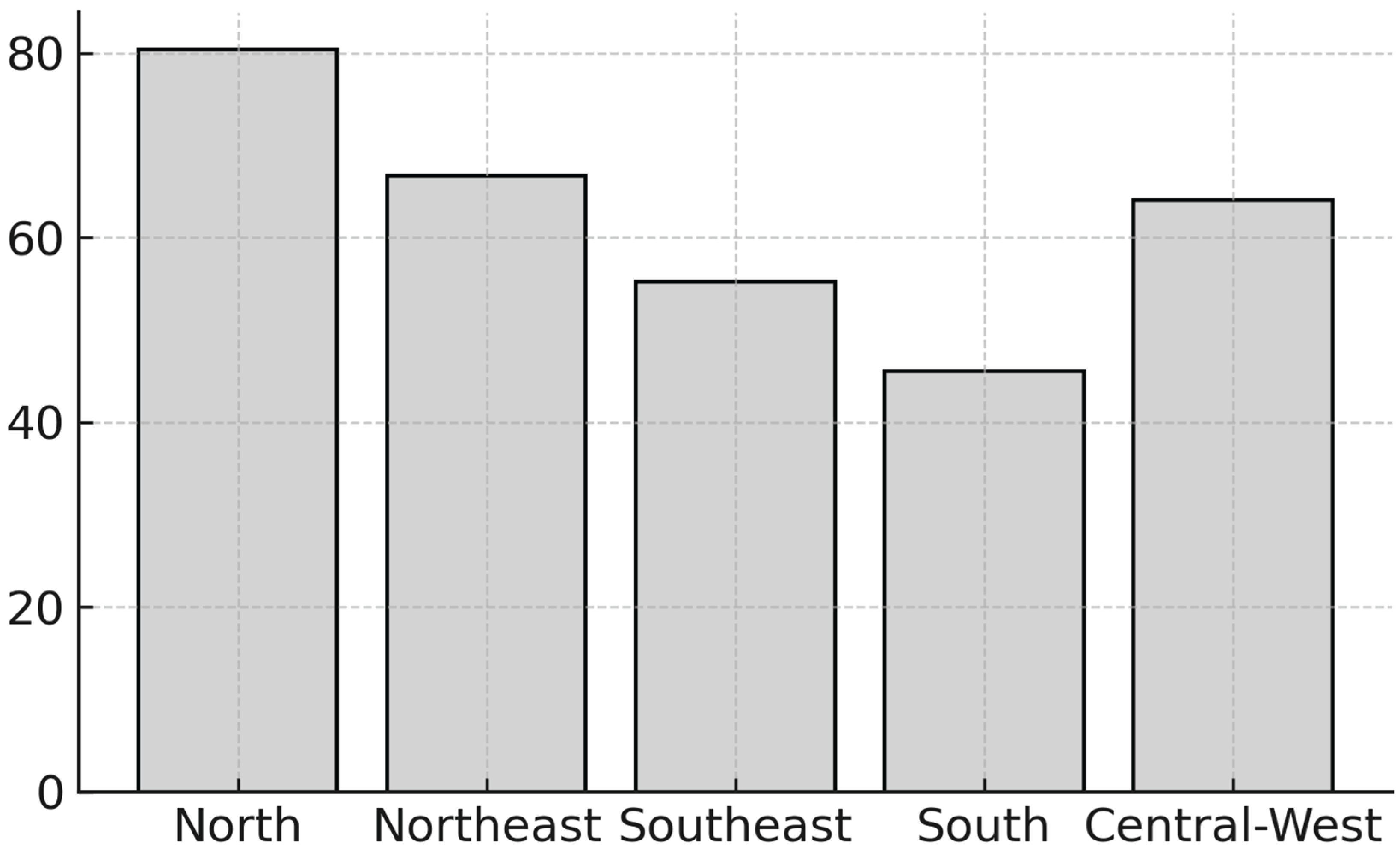
| North | 1.143 | 14.9% |
| North East | 2.343 | 30.5% |
| Southeast | 2.666 | 34.7% |
| South | 813 | 10.6% |
| Central-West | 725 | 9.4% |
| Education | ||
| None | 134 | 1.7% |
| 1–3 years | 435 | 5.7% |
| 4–7 years | 1.380 | 17.9% |
| 8–11 years | 3.650 | 47.5% |
| ≥ 12 years | 1.169 | 15.2% |
| Ignored | 922 | 12% |
| Marital status | ||
| Single | 3578 | 46.5% |
| Married | 2.309 | 30% |
| Widow | 34 | 0.4% |
| Legally separated | 166 | 2.2% |
| Other | 1.089 | 14.2% |
| Ignored | 514 | 6.7% |
| Variable/Category | n | % | 95% CI |
|---|---|---|---|
| Type of maternal death | |||
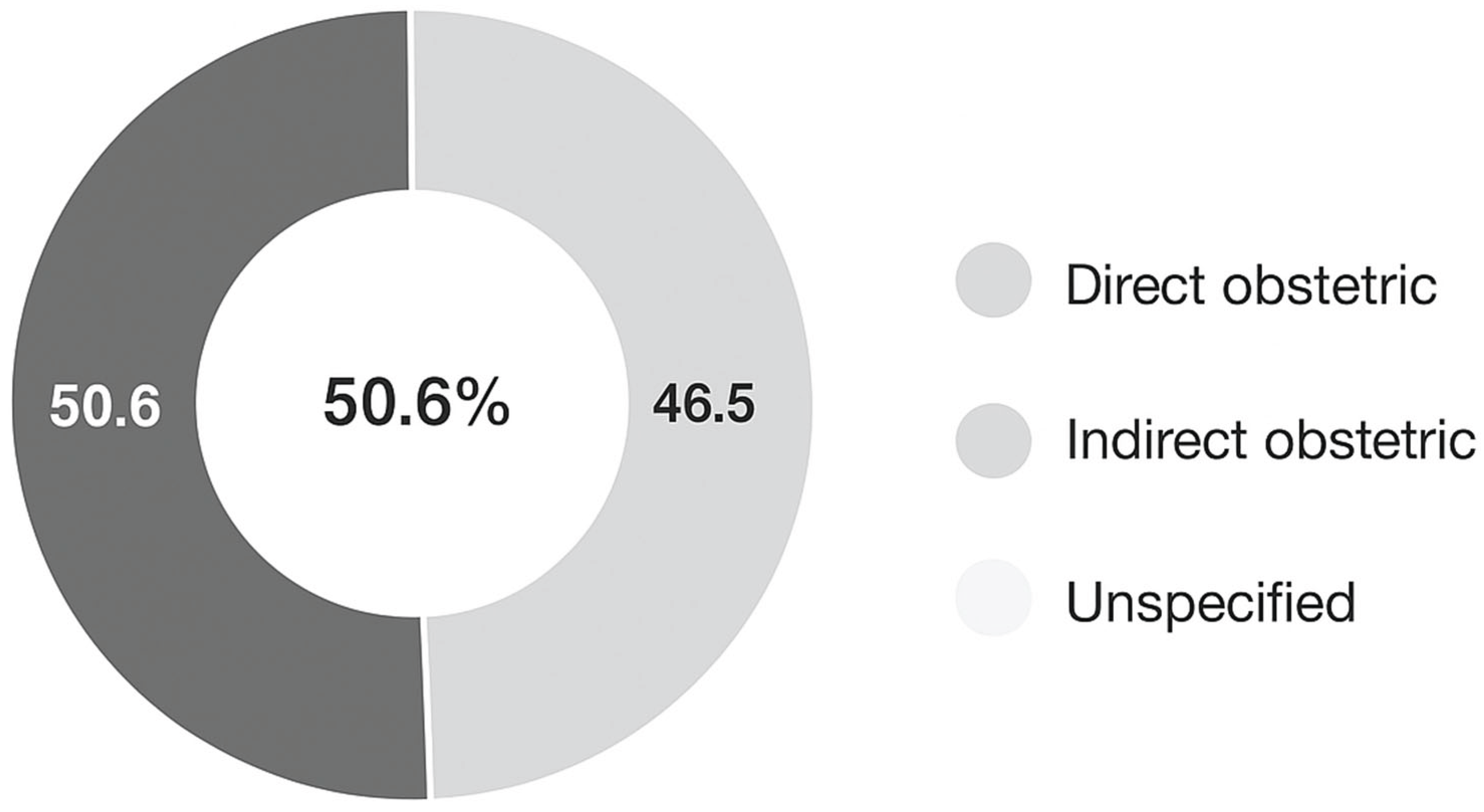
| Direct obstetric | 3.892 | 50.6% | 49.4– 51.8 |
| Indirect obstetric | 3.579 | 46.5% | 45.3–47.7 |
| Unspecified | 218 | 2.8% | 2.5–3.2 |
| Time of death | |||
| Pregnancy/childbirth/abortion | 2.054 | 26.7% | 25.6–27.8 |
| Postpartum up to 42 days | 4.768 | 62% | 60.9–63.1 |
| Postpartum 43 days–<1 year | 122 | 1.6% | 1.3–1.9 |
| Not during pregnancy/postpartum | 138 | 1.8% | 1.5–2.1 |
| Inconsistent period | 3 | 0.04% | 0.01–0.11 |
| Not informed/ignored | 605 | 7.9% | 7.3–8.5 |
| Specific obstetric causes (ICD O00–O99) | |||
| Behavioral syndromes | 2 | 0.03% | 0.004–0.11 |
| Pregnancy that ends in abortion | 488 | 6.3% | 5.8–6.9 |
| Hypertensive disorders | 1.245 | 16.2% | 15.4–17 |
| Other pregnancy disorders | 276 | 3.6% | 3.2–4 |
| Fetal/amniotic complications | 361 | 4.7% | 4.2–5.2 |
| Labor complications | 905 | 11.8% | 11.1–12.6 |
| Childbirth | 1 | 0.01% | 0.0002–0.07 |
| Postpartum complications | 730 | 9.5% | 8.9–10.2 |
| Other obstetric conditions | 3.682 | 47.8% | 46.6–49 |
| ICD-10 Chapters | |||
| V—Mental/behavioral disorders | 2 | 0.03% | 0.004—0.11 |
| XV—Pregnancy, childbirth and the postpartum period | 7.688 | 99.97% | 99.94–99.99 |
| Deaths | Live births (5 years) | Rate 100,000 |
IRR | 95% CI | p-value | |
|---|---|---|---|---|---|---|
| Race | ||||||
| Brown (ref) | 4.036 | 706,8200 | 57,10 | 1,00 | — | — |
| White | 2.436 | 420,0250 | 58,01 | 1,016 | 0,966–1,068 | 0,544 |
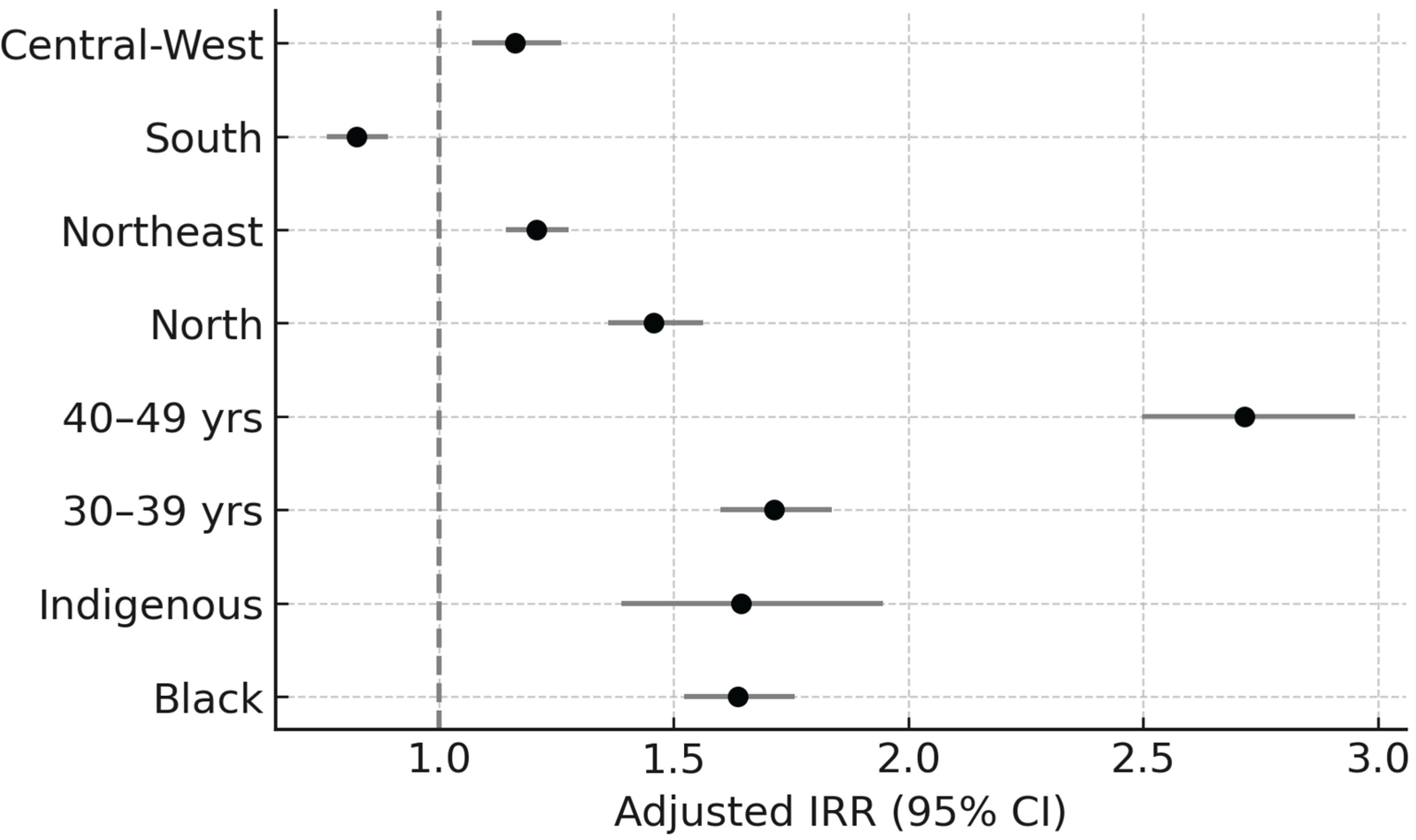
| Black | 917 | 981,625 | 93,45 | 1,636 | 1,523–1,758 | <0,001 |
| Yellow | 21 | 59,780 | 35,12 | 0,615 | 0,401–0,945 | 0,026 |
| Indigenous | 139 | 148,115 | 93,85 | 1,644 | 1,388–1,946 | <0,001 |
| Ignored | 141 | 229,910 | 61,33 | 1,074 | 0,908–1,270 | 0,404 |
| Age range | ||||||
| 20–29 (ref) | 2.880 | 623,5505 | 46,19 | 1,00 | — | — |
| 10–14 | 37 | 69,695 | 53,07 | 0,707 | 0,517–0,967 | 0,030 |
| 15–19 | 600 | 144,6700 | 41,49 | 0,552 | 0,515–0,592 | <0,001 |
| 30–39 | 3.473 | 438,6710 | 79,19 | 1,714 | 1,599–1,837 | <0,001 |
| 40–49 | 686 | 547,100 | 125,39 | 2,716 | 2,498–2,951 | <0,001 |
| 50–59 | 14 | 1915 | 730,87 | 16,015 | 9,362–26,760 | <0,001 |
| Region of residence | ||||||
| Southeast (ref) | 2.666 | 483,0800 | 55,20 | 1,00 | — | — |
| North | 1.143 | 142,0985 | 80,45 | 1,458 | 1,360–1,562 | <0,001 |
| North East | 2.343 | 351,7240 | 66,66 | 1,207 | 1,142–1,276 | <0,001 |
| South | 813 | 178,8060 | 45,47 | 0,824 | 0,762–0,891 | <0,001 |
| Central-West | 725 | 113,0795 | 64,12 | 1,162 | 1,070–1,261 | 0,00034 |
| Year | Live births | Deaths | TMM | 95% CI |
|---|---|---|---|---|
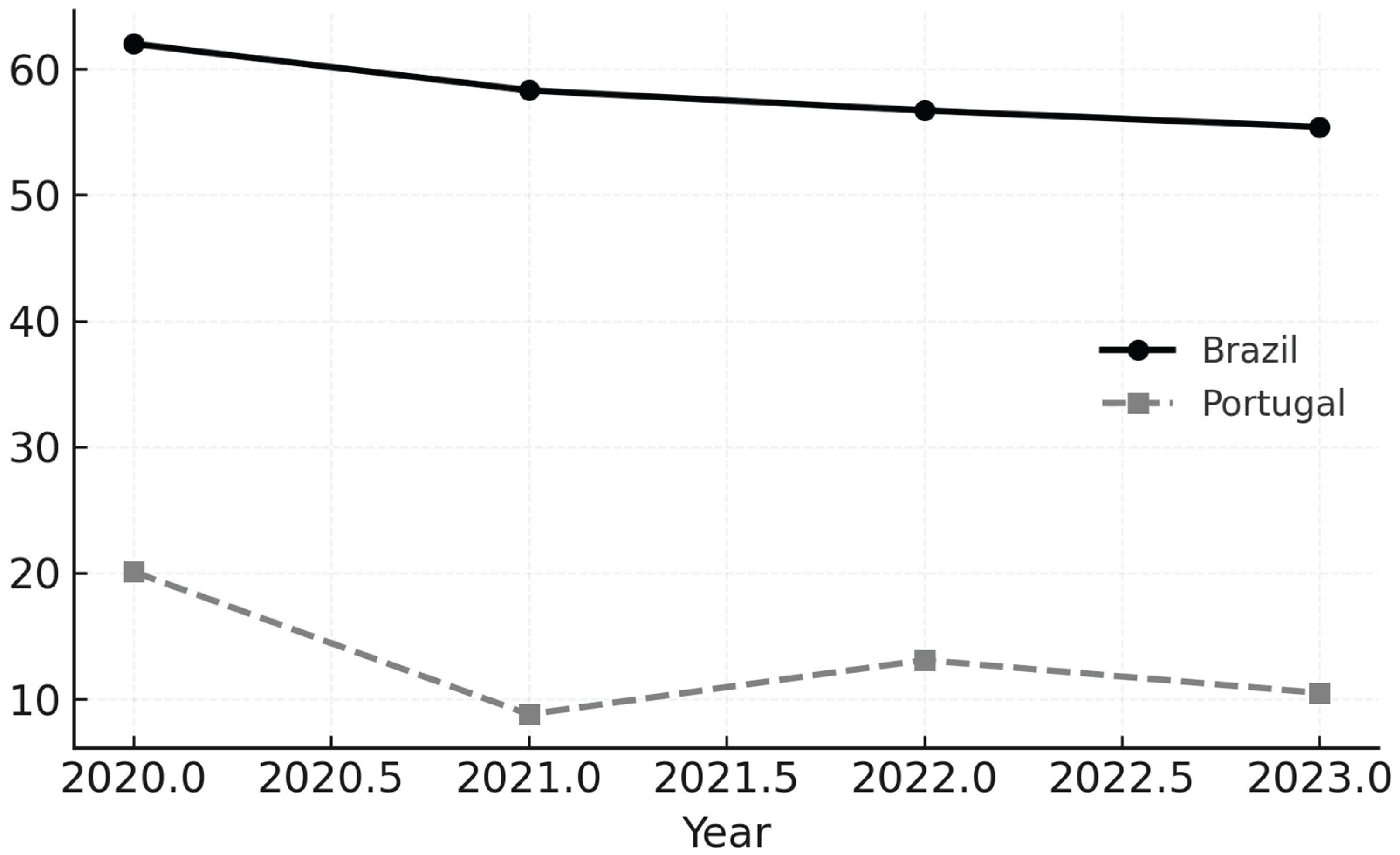
| 2020 | 84.371 | 16.96 | 20.1 | 10.5–29.7 |
| 2021 | 79.294 | 6.98 | 8.8 | 2.27–15.3 |
| 2022 | 82.632 | 10.82 | 13.1 | 5.30–20.9 |
| 2023 | 83.295 | 8.75 | 10.5 | 3.54–17.5 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




