Submitted:
03 April 2026
Posted:
07 April 2026
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
- Structural inadequacy: Simple mesothelial apposition cannot account for the highly organized, multilaminated architecture consistently observed in modern high-resolution microanatomy.
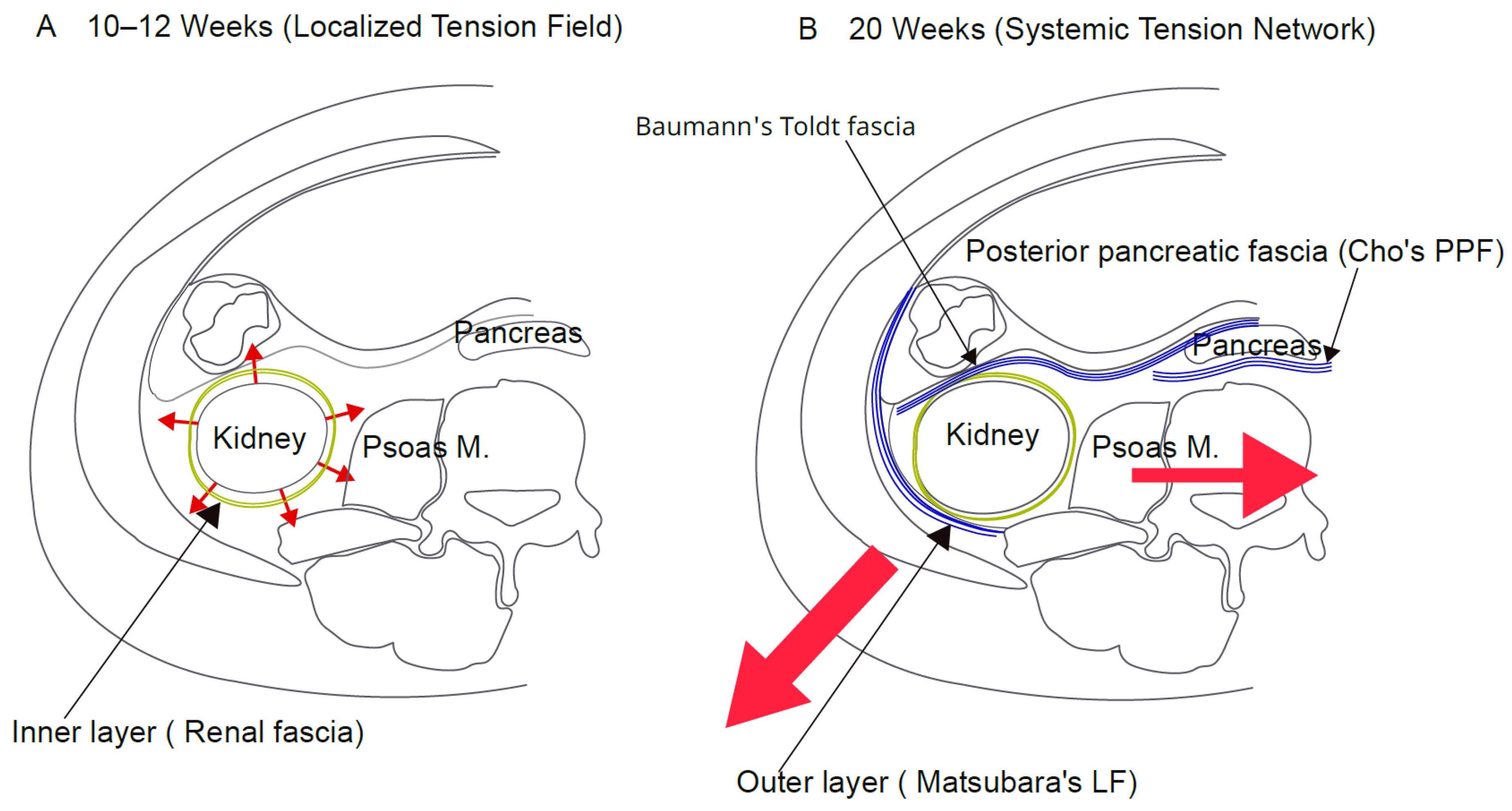
- Temporal discrepancy: A substantial 10-week latency exists between early organ fixation (10 weeks) and definitive fascial lamination (20 weeks) in the posterior pancreatic and renal regions (Cho et al., 2009).
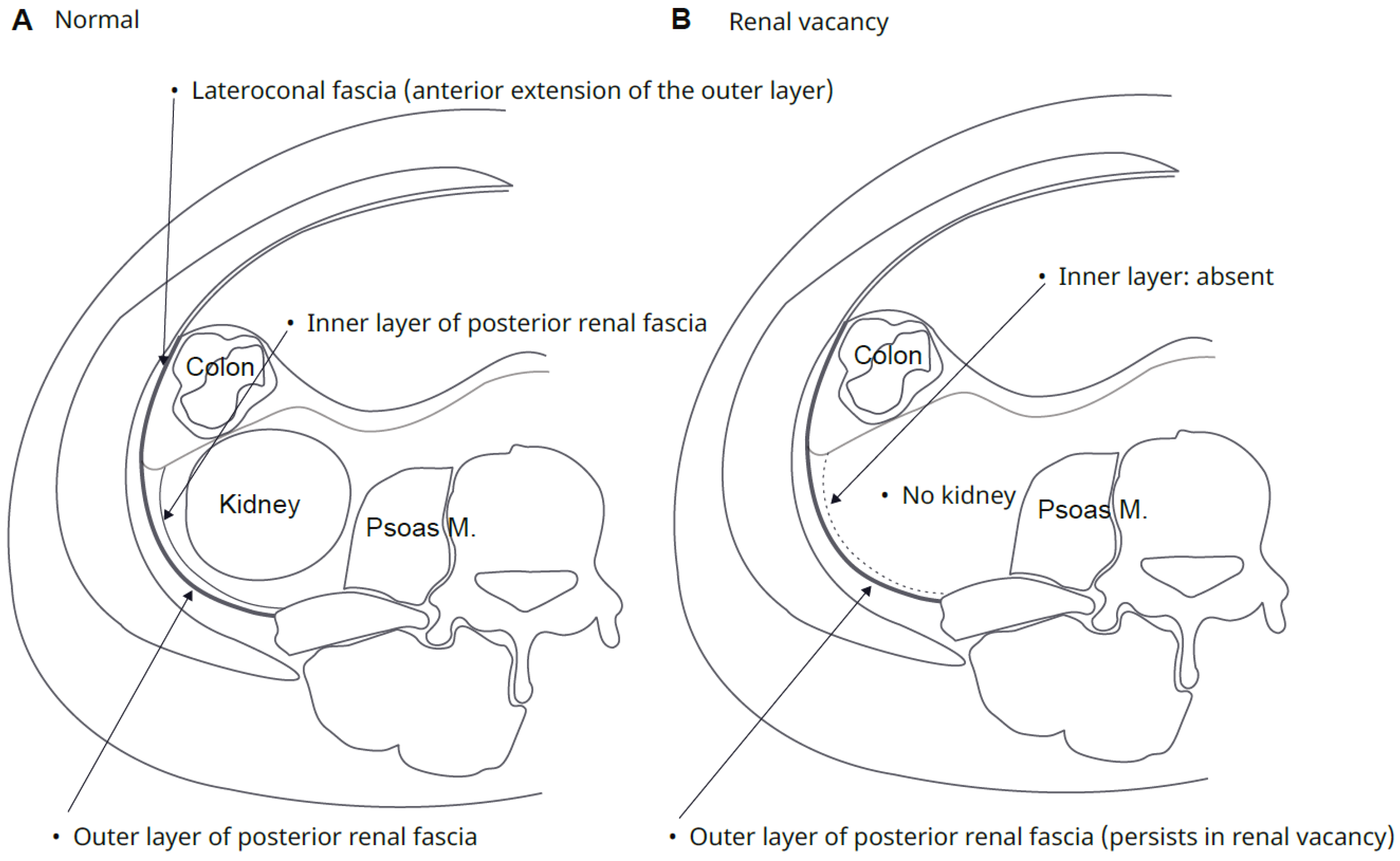
- Clinical contradiction: Historical macroscopic dissections suggest complete fascial agenesis in the absence of a kidney (Tobin, 1944), whereas modern cross-sectional imaging reveals that the normal posterior renal fascia is a bilaminar structure (Raptopoulos et al., 1986). How the connective tissue meshwork behaves in the developmental absence of the primary organ thus remains a contentious and unresolved question.
2. Methods (Conceptual and Analytical Approach)
3. Results
3.1. Radiological Subtraction Experiment (Adult Renal Vacancy)
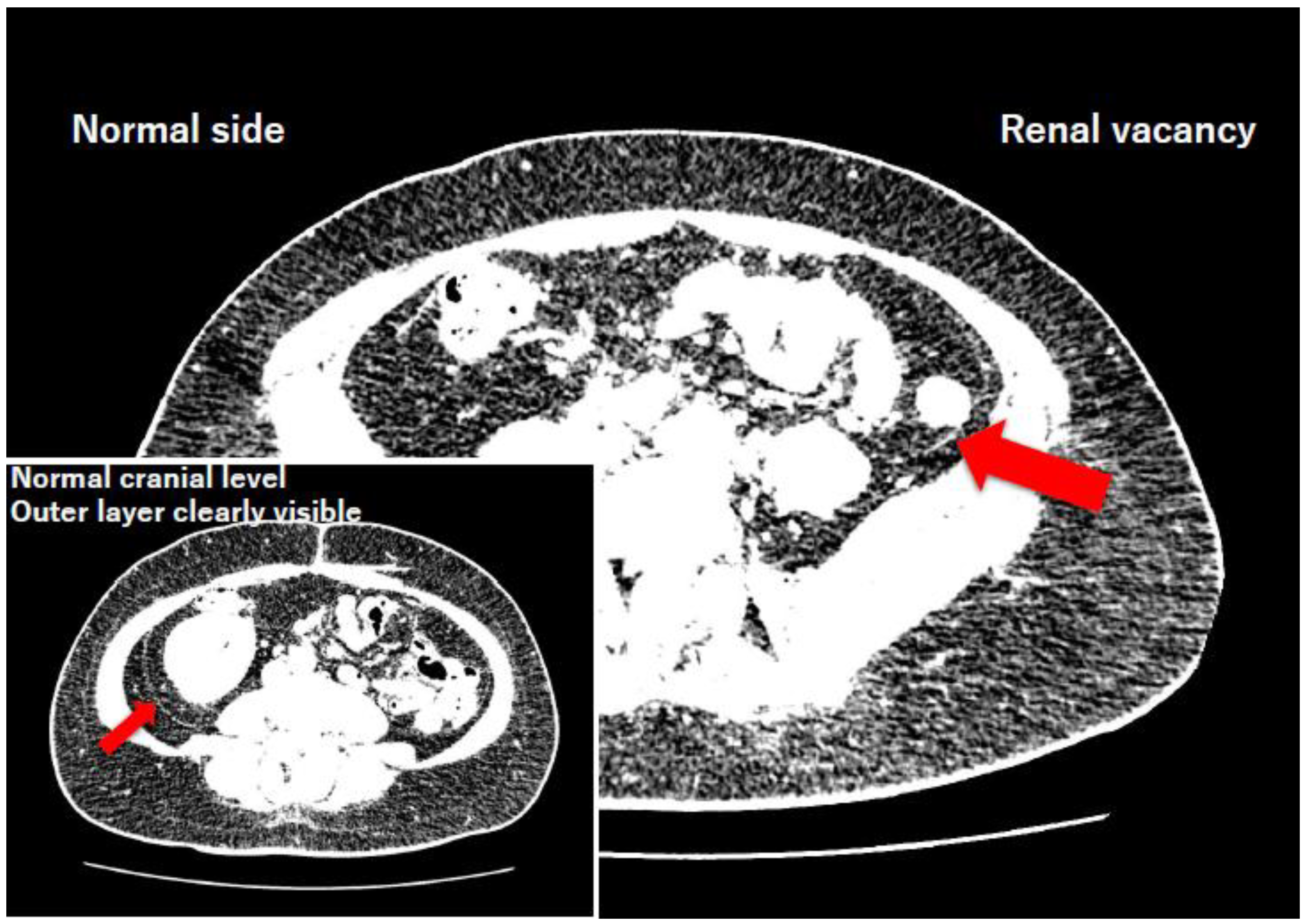
3.2. Chronological Synthesis of Fetal Fascial Development
4. Theoretical Integration and Discussion
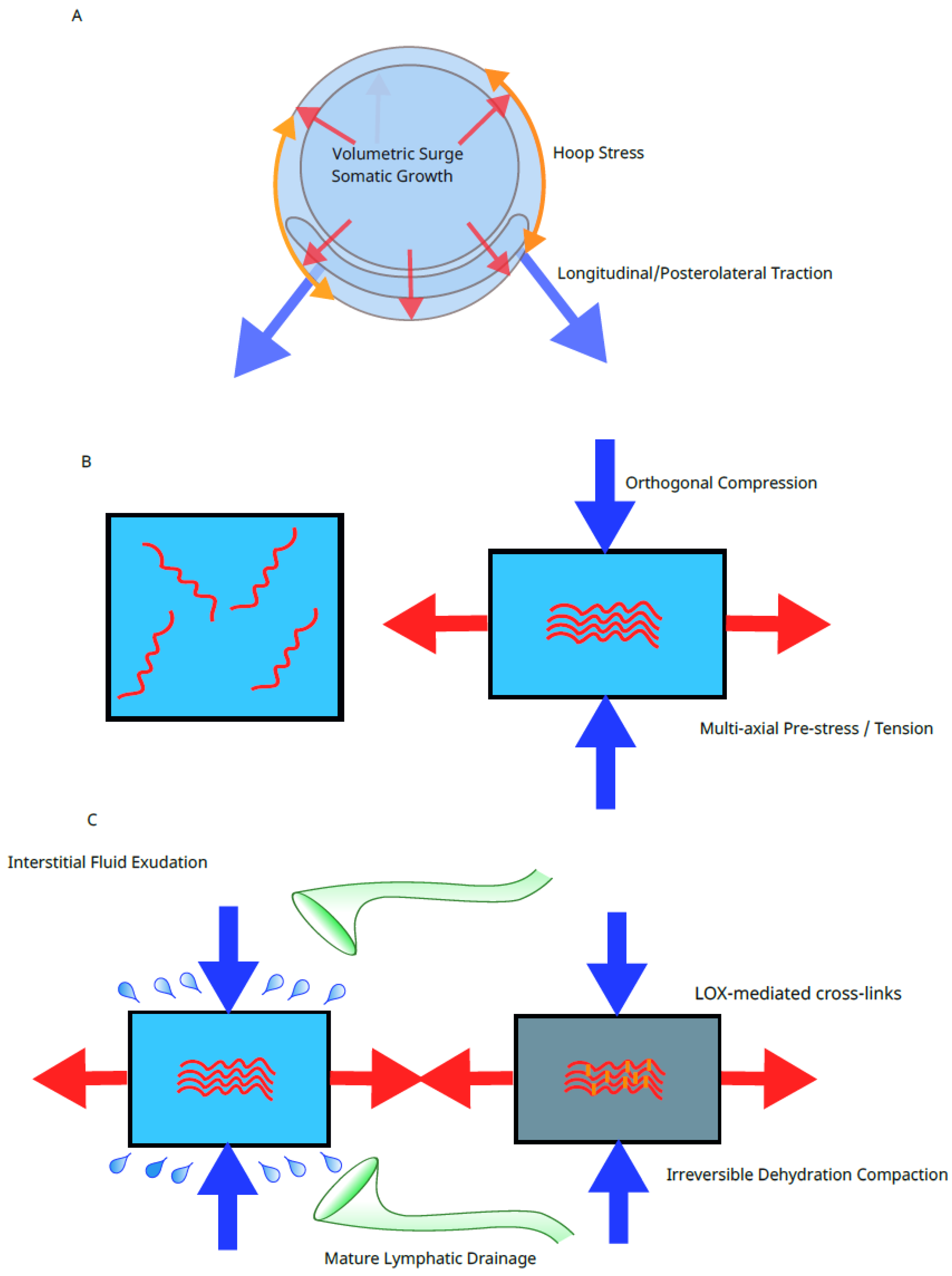
4.1. Mechanobiological Interpretation of the 20-Week Transition
- Fibroblast alignment along dominant macroscopic tension vectors (Ingber, 2003).
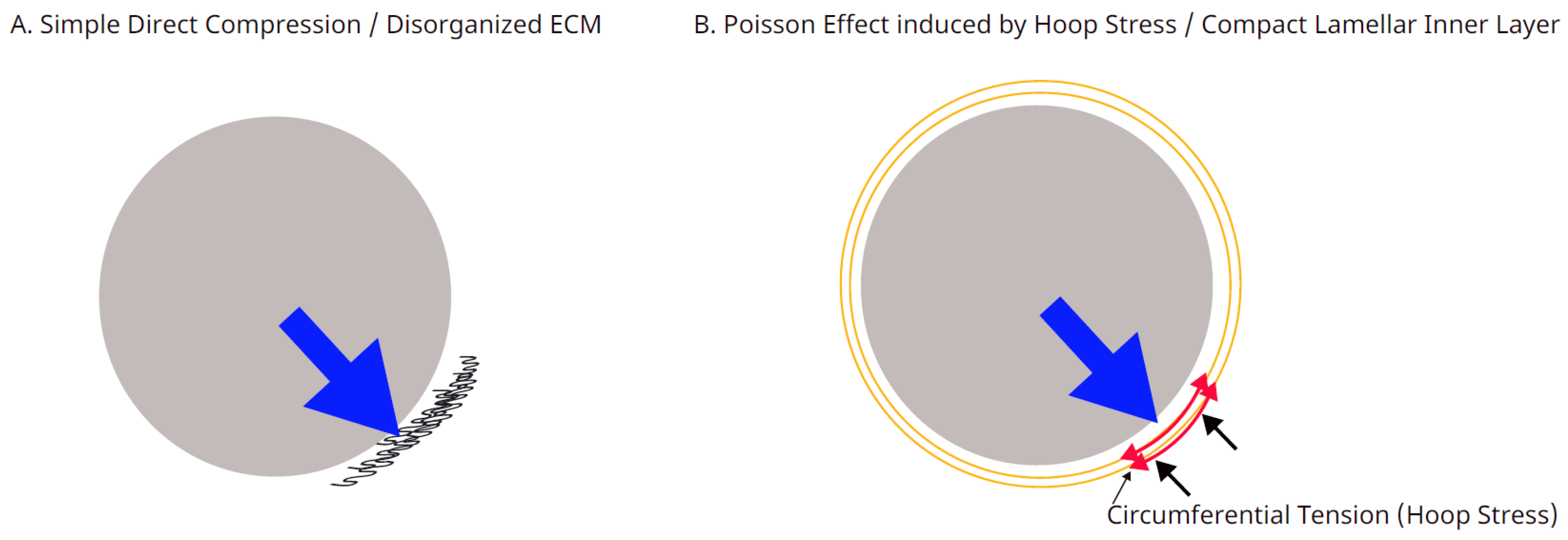
- Orthogonal extracellular matrix (ECM) compression dictated by the Poisson effect and poroelasticity (Lakes, 1991).
- Enzymatic stabilization via LOX-mediated cross-linking.
4.2. Systemic Tension Field and Poisson-Effect Lamination
4.3. Terminological Clarification and Clinical Implications
4.4. Resolving the Historical Debate on the Bilaminar Renal Fascia
4.5. The Square–Cube Law and the Emergence of a Fetal Tensegrity System
4.5.1. Developmental Prerequisites from Pelvic Morphogenesis
4.6. Lymphatic Maturation, Poroelastic Compaction, and Cross-Linking
4.7. Comparative Anatomy Implications
4.8. Limitations and Future Directions
5. Conclusions
| Clinical Gestational Age | Anatomical / Biomechanical Events | Mechanobiological Significance | Key References |
| 10–12 weeks | Early pancreatic fixation to the posterior wall; circumferential emergence of the inner layer of the renal fascia; morphogenetic blueprint of iliac flare geometry established via cartilage shift | Localized tension and spatial vector preparation: Viscera asynchronously integrate into the nascent tension network. Pelvic cartilage establishes the future posterolateral traction vector, though it remains too compliant at this stage to generate systemic tension. | Cho et al. (2009); Matsubara et al. (2009); Senevirathne et al. (2025) |
| 14–16 weeks | Functional maturation of the fetal lymphatic system (terminal venous connections) | Physiological preparation: Establishes systemic drainage capacity required for poroelastic fluid exudation during the subsequent Poisson-effect compression phase. | Berger (1999); Bekker et al. (2005) |
| 18–20 weeks | Progressive ossification of the vertebral column; epidermal keratinization and completion of the inextensible cutaneous envelope; volumetric growth begins to surge exponentially (square–cube law) | Dynamic preconditioning and the square–cube law: The spine stiffens into a central pillar. Volumetric expansion outpaces surface area, generating massive outward pressure. This collides with epidermal maturation to produce profound systemic hoop stress. | Bagnall et al. (1977); Singh & Archana (2008); Hadlock et al. (1991) |
| Around 20 weeks (The Chronological Intersection) | Somatic rigidification: cumulative three-dimensional pelvic expansion and ossification reach a biomechanical threshold; fascial lamination: synchronous, definitive clarification of Toldt's fascia, the posterior pancreatic fascia, and the multilaminated outer layer of the posterior renal fascia | The temporal mechanical trigger and Poisson effect: As anchors stiffen into rigid levers, growth forces are transmitted without dissipation. The resulting tension spike induces orthogonal compression (Poisson effect), forcing fluid exudation and subsequent LOX-mediated cross-linking to complete fascial lamination. | Baumann (1945); Cho et al. (2009); Matsubara et al. (2009); Verbruggen & Nowlan (2017); (Current Model) |
| Anatomical System | Event at ~20 Weeks | Biomechanical Significance | Key References |
| Skeletal System | Ossification of the vertebral column | Rigid central pillar for tension transmission | Bagnall et al. (1977) |
| Expansion and ossification of the iliac flare | Establishes the lateral lever arm for whole-body tension | Baumgart et al. (2018); Senevirathne et al. (2025) | |
| Cutaneous Envelope | Epidermal keratinization | Inextensible shell generating systemic hoop stress | Hardman et al. (1999) |
| Somatic Growth | Exponential volumetric expansion | Square–cube law drives global tension | Hadlock et al. (1991) |
| Musculoskeletal Motor System | Intensification of fetal kicking and gross body movements | Dynamic tension spikes actively align fibroblasts and accelerate poroelastic compaction | Nowlan (2015); de Vries et al. (1982); Patrick et al. (1982) |
| Respiratory Physiology | Sharp increase in fetal breathing movements (FBMs) | Rhythmic loading reinforces the tension network | Nowlan (2015) |
| Rib cage rigidity increases | Thorax becomes a stable mechanical frame | Bagnall et al. (1977); Verbruggen & Nowlan (2017) | |
| Surfactant production begins | Stabilizes alveoli, sustaining consistent FBMs | Avery & Fletcher (1974); Clements (1957) | |
| Lymphatic System | Systemic drainage capacity matures | Promotes irreversible poroelastic compaction | Bekker et al. (2005) |
| Fascial Structures | Lamination of Toldt's fascia | Reflects the systemic tension threshold | Baumann (1945) |
| Lamination of the posterior pancreatic fascia | Occurs after a 10-week latency period | Cho et al. (2009) | |
| Lamination of the outer layer of the posterior renal fascia | Multi-axial tension combined with Poisson-effect compression | Matsubara et al. (2009) | |
| Peripheral Nervous System | Compaction of sciatic nerve sheaths | Pelvic traction induces Poisson-effect compression | Pummi et al. (2004) |
| Case | Age/Sex | Radiological Diagnosis | Adrenal Morphology | Fascial Thickness (Vacancy Side) | Fascial Thickness (Normal Side) | Difference (Δ) |
| 1 | 53/F | True Left Renal Agenesis | "Pancake" (lying-down) | 1.49 mm | 1.88 mm | −0.39 mm |
| 2 | 47/F | Severe Left Renal Dysplasia / Involution (renal nubbin) | Normal | 1.46 mm | 1.82 mm | −0.36 mm |
| 3 | 89/M | True Left Renal Agenesis | "Pancake" (lying-down) | 1.62 mm | Excluded* | N/A |
| Mean | 1.52 mm | 1.85 mm | −0.38 mm |
Author Contributions
Ethics Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Avery, ME; Fletcher, BD. The Lung and Its Disorders in the Newborn Infant, 3rd ed.; WB Saunders: Philadelphia, 1974. [Google Scholar]
- Bagnall, KM; Harris, PF; Jones, PR. The appearance of ossification centers in the human fetal spine. J Anat 1977, 124, 791–802. [Google Scholar] [PubMed]
- Baumann, JA. Développement et anatomie de la loge rénale chez l'homme. Acta Anat (Basel) 1945, 1, 15–65. [Google Scholar] [CrossRef] [PubMed]
- Baumgart, M; Wiśniewski, M; Grzonkowska, M; et al. Quantitative anatomy of the ilium's primary ossification center in the human fetus. Surg Radiol Anat 2018, 40, 1047–1054. [Google Scholar] [CrossRef] [PubMed]
- Bekker, MN; van den Akker, NM; de Ruiter, MC; Gittenberger-de Groot, AC. The human fetal lymphatic system: a morphological study. Anat Embryol (Berl) 2005, 210, 167–175. [Google Scholar]
- Berger, G. First-trimester nuchal translucency and the fetal lymphatic system. Ultrasound Obstet Gynecol 1999, 13, 12–17. [Google Scholar]
- Cho, BH; Kimura, W; Iioka, T; Hirai, I; Koyama, T; Furuya, T; et al. Development of the posterior pancreatic fascia in human fetuses. J Hepatobiliary Pancreat Surg 2009, 16, 824–831. [Google Scholar] [CrossRef]
- Clements, JA. Surface tension of lung extracts. Proc Soc Exp Biol Med 1957, 95, 170–172. [Google Scholar] [CrossRef]
- Congdon, ED; Edson, JN. The cone of renal fascia in the adult white male. Anatomical Record 1941, 80, 289–313. [Google Scholar] [CrossRef]
- de Vries, JI; Visser, GH; Prechtl, HF. The emergence of fetal behaviour. I. Qualitative aspects. Early Hum Dev 1982, 7, 301–322. [Google Scholar] [CrossRef]
- Fung, YC. Biomechanics: Motion, Flow, Stress, and Growth; Springer-Verlag: New York, 1990. [Google Scholar]
- Gerota, D. Beiträge zur Kenntniss des Befestigungsapparates der Niere. In Archiv für Anatomie und Entwicklungsgeschichte; 1895; pp. 265–285. [Google Scholar]
- Hadlock, FP; Harrist, RB; Martinez-Poyer, J. In utero analysis of fetal growth: A sonographic weight standard. Radiology 1991, 181, 129–133. [Google Scholar] [CrossRef]
- Hardman, MJ; Sisi, P; Banbury, DN; Byrne, C. Barrier formation in the human fetus is patterned. J Invest Dermatol 1999, 113, 1106–1113. [Google Scholar] [CrossRef]
- Hayes, MA. Abdominopelvic fasciae. Am J Anat 1950, 87, 119–161. [Google Scholar] [CrossRef]
- Humphrey, JD. Continuum biomechanics of soft biological tissues. Proc Math Phys Eng Sci 2003, 459, 3–46. [Google Scholar] [CrossRef]
- Ingber, DE. Tensegrity I. Cell structure and hierarchical systems biology. J Cell Sci 2003, 116, 1157–1173. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, K; Idoguchi, K; Tanaka, H; et al. Classification of acute pancreatitis based on retroperitoneal extension: application of the concept of interfascial planes. Eur J Radiol 2006, 60, 445–452. [Google Scholar] [CrossRef] [PubMed]
- Kagan, HM; Li, W. Lysyl oxidase: properties, specificity, and biological roles inside and outside of the cell. J Cell Biochem 2003, 88, 660–672. [Google Scholar] [CrossRef]
- Kinugasa, Y; et al. Development of the human hypogastric nerve sheath with special reference to the topohistology between the nerve sheath and other prevertebral fascial structures. Clin Anat 2008, 21, 558–567. [Google Scholar] [CrossRef]
- Lakes, R. Deformation mechanisms in negative Poisson's ratio materials: structural aspects. J Mater Sci 1991, 26, 2287–2292. [Google Scholar] [CrossRef]
- Marks, SC, Jr.; Raptopoulos, V; Kleinman, P; Snyder, M. The anatomical basis for retrorenal extensions of pancreatic effusions: the role of the renal fasciae. Surg Radiol Anat 1986, 8(2), 89–97. [Google Scholar] [CrossRef]
- Matsubara, A; Kinugasa, Y; Murakami, G; Suzuki, D; Fujimiya, M; Sugihara, K. Development of the lateroconal fascia in human fetuses. Cells Tissues Organs 2009, 190, 286–296. [Google Scholar] [CrossRef]
- Molmenti, EP; Balfe, DM; Kanterman, RY; Bennett, HF. Anatomy of the retroperitoneum: observations of the distribution of pathologic fluid collections. Radiology 1996, 200, 95–103. [Google Scholar] [CrossRef]
- Mow, VC; Kuei, SC; Lai, WM; Armstrong, CG. Biphasic creep and stress relaxation of articular cartilage in compression: theory and experiments. J Biomech Eng 1980, 102, 73–84. [Google Scholar] [CrossRef] [PubMed]
- Nowlan, NC. Biomechanics of fetal movement. Eur Cell Mater 2015, 29, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Patrick, J; Campbell, K; Carmichael, L; Natale, R; Richardson, B. Patterns of gross fetal body movements over 24-hour observation intervals during the last 10 weeks of pregnancy. Am J Obstet Gynecol 1982, 142, 363–371. [Google Scholar] [CrossRef] [PubMed]
- Provenzano, PP; Vanderby, R. Collagen fibril morphology and organization: implications for force transmission in ligament and tendon. Matrix Biol 2006, 25, 71–84. [Google Scholar] [CrossRef]
- Pummi, K; Heape, AM; Grenell, S; Peltonen, J; Peltonen, S. Tight junction proteins ZO-1, occludin, and claudins in developing and adult human perineurium. J Histochem Cytochem 2004, 52, 1037–1046. [Google Scholar] [CrossRef]
- Raptopoulos, V; Kleinman, PK; Marks, S; Snyder, M; Silverman, PM. Renal fascial pathway: posterior extension of pancreatic effusions within the anterior pararenal space. Radiology 1986, 158, 367–374. [Google Scholar] [CrossRef]
- Senevirathne, G; Fernandopulle, SC; Richard, D; Capellini, TD; et al. The evolution of hominin bipedalism in two steps. Nature 2025, 645, 952–963. [Google Scholar] [CrossRef]
- Singh, G; Archana, G. Unraveling the mystery of vernix caseosa. Indian J Dermatol 2008, 53, 54–60. [Google Scholar] [CrossRef]
- Tobin, CE. The renal fascia and its relation to the transversalis fascia. Anatomical Record 1944, 89, 295–311. [Google Scholar] [CrossRef]
- Toldt, C. Bau und Wachsthumsveränderungen der Gekröse des menschlichen Darmkanales. Denkschr Akad Wiss Wien 1879, 41, 1–56. [Google Scholar]
- Treitz, W. Ueber einen neuen Muskel am Duodenum des Menschen. Vierteljahrsschr Prakt Heilkd 1853, 37, 113–144. [Google Scholar]
- Verbruggen, SW; Nowlan, NC. Ontogeny of the human pelvis. Anat Rec (Hoboken) 2017, 300, 643–652. [Google Scholar] [CrossRef]
- Zuckerkandl, E. Ueber den Fixationsapparat der Nieren. Med Jahrb 1883, 1883, 59–67. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




