Submitted:
02 May 2026
Posted:
04 May 2026
You are already at the latest version
Abstract
Background: The intake of mineral water for therapeutic purposes (crenotherapy) in digestive system disorders is a long-established practice, even though there are still few controlled clinical studies confirming the effect of natural mineral water rich in bicarbonate. Objective: To verify whether the daily intake of Aqua 3 bicarbonate natural mineral water is able to improve digestion in a population of patients with functional dyspepsia and gastroesophageal reflux disease symptoms. Methods: Patients had a diagnosis of functional dyspepsia formulated in accordance with the Rome IV criteria and were subjected to three periods of 2 weeks: tap water (wash-out), bicarbonate natural mineral water, and oligomineral water. The mineral water bottles had their labels removed. Primary efficacy endpoint: improvement in the PAGI-SYM total. Secondary endpoints: improvements in the PAGI-SYM subscales, in the use of antacids, and in the self-assessment of efficacy on digestion. Results: The PAGI-SYM total score and the six subscales significantly decreased after bicarbonate mineral water intake, while they significantly increased after oligomineral water supplementation. The antacid use was significantly different comparing the decrease after oligomineral water versus the increase after oligomineral water. In addition, the score of the subjective assessment of effectiveness of the patient’s digestion was significantly better after the intake of bicarbonate than after oligomineral water. Conclusions: In line with the evidence reported in the literature, the findings of this study provide additional support for recommending natural bicarbonate mineral water as a symptomatic treatment for functional dyspepsia and gastroesophageal reflux disease. The intake of Aqua 3 bicarbonate mineral water proved to be a simple, safe, and natural intervention capable of improving digestive symptoms in patients with functional dyspepsia and reflux-related disorders, while promoting the digestive process.
Keywords:
1. Introduction
1.1. Natural Mineral Waters
1.2. Classification of Natural Mineral Waters
1.3. Mineral Water and Digestion
1.4. Functional Gastrointestinal Disorders and Impaired Digestion
1.5. Aim of the Study
2. Materials and Methods
2.1. Study Design
2.2. Inclusion Criteria
2.3. Exclusion Criteria
2.4. Patients
2.5. Endpoints
2.6. Assessment of Upper Gastrointestinal Disorders: Symptom Severity Index (PAGI-SYM)
2.7. Antacid Intake
2.8. Patient Satisfaction
2.9. Safety
2.10. Statistical Methods
2.10.1. Sample Size Calculation
2.10.2. Statistical Analysis
2.11. Ethical Issues
3. Results
3.1. Patients
3.2. Protocol Deviations and Compliance
3.3. The PAGI-SYM Severity Index
3.4. Use of Antacid Drugs
3.5. Patient Satisfaction and Safety
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| EPS | Epigastric pain syndrome |
| FD | Functional dyspepsia |
| GERD | Gastroesophageal reflux disease |
| GI | Gastrointestinal |
| PDS | Postprandial distress syndrome |
References
- Raynal, C. La vente des eaux minérales par les pharmaciens. Rev. Hist. Pharm. 2004, 344, 587–606. [Google Scholar] [CrossRef]
- European Parliament. Directive 2009/54/EC of the European Parliament and of the Council of 18 June 2009 on the exploitation and marketing of natural mineral waters. Available online: https://eur-lex.europa.eu/eli/dir/2009/54/oj/eng.
- European Parliament. Directive 2001/83/EC of the European Parliament and of the Council of 6 November 2001 on the Community code relating to medicinal products for human use. Available online: https://eur-lex.europa.eu/eli/dir/2001/83/oj/eng.
- Zhixian, S.; Theng, M.; Zhang, M.; Rangan, A. Water and beverage consumption: analysis of the Australian 2011-2012 National Nutrition and Physical Activity Survey. Nutrients 2016, 8, 678. [Google Scholar]
- Drewnoski, A.; Rhem, C.D.; Constant, F. Water and beverage consumption among adults in the United States: cross-sectional study using data from NHANES 20. BMC Public Health 2013, 13, 1068. [Google Scholar]
- Gibson, S.; Shirreffs, S.M. Beverage consumption habits "24/7" among British adults: association with total water intake and energy intake. Nutr. J. 2013, 12, 9. [Google Scholar] [CrossRef]
- Petraccia, L.; Liberati, G.; Masciullo, S.G.; Grassi, M.; Fraioli, A. Water, mineral waters and health. Clin. Nutr. 2006, 25, 377–85. [Google Scholar] [CrossRef]
- D’Souza, A.; Zink, K.; Langhorst, J.; Widner, W.; Stuopp, C.; Keill, T. How effective is drinking natural mineral water against heartburn from functional dyspepsia, gastroesophageal reflux disease, or other causes? A systematic review of clinical intervention studies. Complement Med. Res. 2024, 31, 253–65. [Google Scholar] [CrossRef]
- Hearty, R.F.; Maico, D.G.; McGuigan, E.J. Role of calcium in antral gastrin release. Gastroenterology 1981, 80, 491–7. [Google Scholar] [CrossRef]
- Flemstrom, G.; Garner, A. Stimulation of gastric acid and bicarbonate secretions by calcium in guinea pig stomach and amphibian isolated mucosa. Acta Physiol. Scand. 1980, 110, 419–26. [Google Scholar] [CrossRef] [PubMed]
- Layer, P.; Hotz, J.; Schmitz-Moormann, H.P.; Goebell, H. Effects of experimental chronic hypercalcemia on exocrine pancreatic enzyme secretion by intravenous calcium infusion in rats: inhibition by atropine. Gastroenterology 1979, 76, 1181. [Google Scholar]
- Pace, F.; Morselli Labate, A.M.; Abu Issa, A.; Zanasi. A bicarbonate natural mineral water from source “Paltinis 2” facilitates digestion. A pilot study. Gastroint Disord. 2025, 7:47. [Google Scholar] [CrossRef]
- Bertoni, M.; Olivieri, F.; Manghetti, M.; Boccolini, E.; Bellomini, M.G.; Blandizzi, C.; et al. Effects of a bicarbonate-alkaline mineral water on gastric functions and functional dyspepsia: a preclinical and clinical study. Pharmacol. Res. 2002, 46, 525–31. [Google Scholar] [CrossRef]
- Labenz, J.; Anschütz, M.; Walstab, J.; Wedemeyer, R.S.; Wolters, H.; Schug, B. Heartburn relief with bicarbonate-rich mineral water: results of the randomised, placebo-controlled phase-III trial STOMACH STILL. BMJ Open Gastroenterol. 2023, 10(1), e001048. [Google Scholar] [CrossRef]
- Quattrini, S.; Pampaloni, B.; Brandi, M.L. Natural mineral waters: chemical characteristics and health effects. Clin. Cases Min. Bone Metab. 2016, 13, 173–80. [Google Scholar] [CrossRef]
- Cuomo, R.; Grasso, R.; Sarnelli, G.; Capuano, G.; Nicolai, E.; Nardone, G.; et al. Effects of carbonated water on functional dyspepsia and constipation. Eur. J. Gastroenterol. Hepatol. 2002, 14, 991–9. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.; Hong, J.H. The fundamental role of bicarbonate transporters and associated carbonic anhydrase enzymes in maintaining ion and pH homeostasis in non-secretory organs. Int. J. Mol. Sci. 2020, 21, 900–8. [Google Scholar] [CrossRef]
- Grassi, M.; Fraioli, A.; Pappalardo, G.; Messina, B.; Belardinelli, L.; Guadalaxara, A. Alkalizing activity of a calcium-bicarbonate-containing water, evaluated for pH, in patients with gastroesophageal reflux. Clin. Ter. 1993, 143, 131–6. [Google Scholar] [PubMed]
- Bortolotti, M.; Turba, E.; Mari, C.; Lopilato, C.; Porrazzo, G.; Scalabrino, A.; Miglioli, M. Changes caused by mineral water on gastrointestinal motility in patients with chronic idiopathic dyspepsia. Minerva Med. 1999, 90, 187–94. [Google Scholar]
- Barclay, G.; Maxwell, V.; Grossman, M.I.; et al. Effects of graded amounts of intragastric calcium on acid secretion, gastrin release, and gastric emptying in normal and duodenal ulcer subjects. Dig. Dis. Sci. 1983, 28, 385–91. [Google Scholar] [CrossRef]
- Fornai, M.; Antonioli, L.; Colucci, R.; Tuccori, M.; Awwad, O.; Serra, M.; et al. Role of crenotherapy with mineral waters in the treatment of functional disorders of digestive tract. Gazz. Med. Ital. 2012, 171, 213–26. [Google Scholar]
- Walsh, J.H.; Sleisenger, M.H.; Fordtran, J.S. Gastrointestinal peptide hormones. In Gastrointestinal disease (patophysiology, diagnosis, management); Saunders: PhiladeIphia, 1983; p. 54. [Google Scholar]
- Gasbarrini, G.; Candelli, M.; Graziosetto, R.G.; Coccheri, S.; Di Iorio, F.; Nappi, G. Evaluation of thermal water in patients with functional dispepsia and irritable bowel sindrome accompanying constipation. World J. Gastroenterol. 2006, 12, 2556–62. [Google Scholar] [CrossRef] [PubMed]
- Fornai, M.; Colucci, R.; Antonioli, L.; Ghisu, N.; Tuccori, M.; Gori, G.; et al. Effects of a bicarbonate-alkaline mineral water on digestive motility in experimental models of functional and inflammatory gastrointestinal disorders. Exp. Clin. Pharm. 2008, 30, 261–9. [Google Scholar] [CrossRef]
- Kurata, J.H.; Nogawa, An; Everhart, J.E. A prospective study of dyspepsia in primary care. Dig. Dis. Sci. 2002, 47, 797–803. [Google Scholar] [CrossRef]
- Chuah, K.H.; Cheong, S.Y.; Lim, S.Z.; Mahadeva, S. Functional dyspepsia leads to more healthcare utilization in secondary care compared with other functional gastrointestinal disorders. J. Dig. Dis. 2022, 23, 111–7. [Google Scholar] [CrossRef] [PubMed]
- Stanghellini, V.; Chan, F.K.; Hasler, W.L.; Malagelada, J.R.; Suzuki, H.; Tack, J.; et al. Gastroduodenal disorders. Gastroenterology 2016, 150, 1380–92. [Google Scholar] [CrossRef] [PubMed]
- Dragomiretska, N.V.; Iliescu, M.G.; Mazilu, L.; Micu, S.I.; Suceveanu, A.P.; Voinea, F.; et al. Application of mineral waters in the complex treatment of patients with gastroesophageal reflux disease. Minerva Gastroenterol. Dietol. 2020, 66, 225–7. [Google Scholar] [CrossRef] [PubMed]
- Domitrescu, M.; Iliescu, M.G.; Mazilu, L.; Micu, S.I.; Suceveanu, A.P.; Voinea, F.; et al. Benefits of crenotherapy in digestive tract pathology (Review). Exp. Ther. Med. 2021, 23, 122. [Google Scholar] [CrossRef]
- Revicki, D.A.; Rentz, A.M.; Tack, J.; Stanghellini, V.; Talley, N.J.; Kahrilas, P.; et al. Responsiveness and interpretation of a symptom severity index specific to upper gastrointestinal disorders. Clin. Gastroenterol. Hepatol. 2004, 2, 769–77. [Google Scholar] [CrossRef]
- Rentz, A.M.; Kahrilas, P.; Stanghellini, V.; Tack, J.; Talley, N.J.; de la Loge, C.; et al. Development and psychometric evaluation of the patient assessment of upper gastrointestinal symptom severity index (PAGI-SYM) in patients with upper gastrointestinal disorders. Qual. Life Res. 2004, 13, 1737–49. [Google Scholar] [CrossRef]
- Kindt, S.; Dubois, D.; Van Oudenhove, L.; Caenepeel, P.; Arts, J.; Bisschops, R.; Tack, J. Relationship between symptom pattern, assessed by the PAGI-SYM questionnaire, and gastric sensorimotor dysfunction in functional dyspepsia. Neurogastroenterol. Motil. 2009, 21, 1183–e105. [Google Scholar] [CrossRef]
- Dupont, W.D. Power calculations for matched case-control studies. Biometrics 1988, 44, 1157–68. [Google Scholar] [CrossRef] [PubMed]
- Dupont, W.D.; Plummer, W.D. Power and sample size calculations: A review and computer program. Control Clin. Trials 1990, 11, 116–28. [Google Scholar] [CrossRef]
- Revicki, D.A.; Rentz, A.M.; Tack, J.; Stanghellini, V.; Talley, N.J.; Kahrilas, P.; et al. Responsiveness and interpretation of a symptom severity index specific to upper gastrointestinal disorders. Clin. Gastroenterol. Hepatol. 2004, 2, 769–77. [Google Scholar] [CrossRef] [PubMed]
- Bellini, M.; Spataro, M.; Costa, F.; Tumino, E.; Ciapparrone, G.; Flandoli, F.; et al. Gallbladder motility following intake of mineral bicarbonate-alkaline water. Ultrasonographic assessment. Minerva Med. 1995, 86, 75–80. [Google Scholar] [PubMed]
- Foschi, M.; Arena, U. Effects of drinking Tettuccio di Montecatini mineral waters on gallbladder emptying and functioning hepatic mass. Clin. Ter. 1990, 135, 115–20. [Google Scholar] [PubMed]
- Fraioli, A.; Mennuni, G.; Petraccia, L.; Fontana, M.; Nocchi, S.; Grassi, M. Sulphate-bicarbonate mineral waters in the treatment of biliary and digestive tract diseases. Clin. Ter. 2010, 161, 163–8. [Google Scholar] [PubMed]
- Albertini, M.C.; Dachà, M.; Teodori, L.; Conti, M.E. Drinking mineral waters: biochemical effects and health implications - the state-of-the-art. Int. J. Env. Health 2007, 1, 153–69. [Google Scholar] [CrossRef]
- Coiro, V.; Volpi, R.; Vescovi, P.P. Choleretic and cholagogic effect of sulphuric sulfate water from the springs of Tabiano in cholestasis in alcohol related liver diseases. Clin. Ter. 1997, 148, 15–22. [Google Scholar] [PubMed]
- Grossi, F.; Fontana, M.; Conti, R.; Mastroianni, S.; Lazzari, S.; Messini, F.; et al. Motility of the gastric antrum and the gallbladder following oral administration of sulfate-bicarbonate. Clin. Ter. 1996, 147, 321–6. [Google Scholar] [PubMed]
- Koufman, J.A.; Johnston, N. Potential benefits of pH 8.8 alkaline drinking water as an adjunct in the treatment of reflux disease. Ann. Otol. Rhinol. Laryngol. 2012, 121, 431–4. [Google Scholar] [CrossRef]
- Grassi, M.; Fraioli, A. Gastroenteropancreatic endocrine system and crenotherapy with mineral waters. Clin. Ter. 1988, 127, 379–84. [Google Scholar]
- Maltinti, G.; Polloni, A.; Marchi, S.; Costa, F.; Bellini, M.; Guglielmini, R. Influenza degli ioni sull’assetto enterormonale. Clin. Term. 1988, 41, 129. [Google Scholar]
- Kuznetsov, B.G. Gastroenteropancreatic endocrine system and its role in the mechanism of action of potable mineral waters (a review of the literature). Vopr. Kurortol. Fizioter. Lech. Fiz. Kult. 1981, 3, 63–7. [Google Scholar]
- Layer, P.; Holtz, J.; Schmitz-Moormann, H.P.; et al. Effects of experimental chronic hypercalcemia on feline exocrine pancreatic secretion. Gastroenterolpgy 1982, 82, 309–16. [Google Scholar] [CrossRef]
- Hotz, J.; Goebell, H.; Ziegler, R. Interactions of calcium, magnesium and atropine on exocrine pancreatic secretion in man. Eur. J. Clin. Invest 1978, 8, 303–7. [Google Scholar] [CrossRef]
- Inoue, K.; Fried, G.M.; Wiener, I.; T Sakamoto, T.; P Lilja, P.; Greeley, G.H., Jr.; et al. Effect of divalent cations on gastrointestinal hormone release and exocrine pancreatic secretion in dogs. Am. J. Physiol. 1985, 248 1 Pt 1, G28–34. [Google Scholar] [CrossRef] [PubMed]
- Flemstrom, G. Effect of catecholamines, Ca++ and gastrin on gastric HCO3 secretion. Acta Physiol. Scand. (Suppl. Gastric Jon Transport). 1978, 81:90. [Google Scholar]
- Grassi, M.; Messina, B.; Fraioli, A. La secrezione di bicarbonato a livello gastroduodenale. Aspetti di fi siopatologia digestiva e di terapia. Clin. Ter. 1985, 115, 113–7. [Google Scholar]
- Schwartz, C.J.; Kimberg, D.V.; Sheerin, H.E.; Field, M.; Said, S.I. Vasoactive intestinal peptide stimulation of adenylate cyclase and active electrolyte secretion in intestinal mucosa. J. Clin. Invest 1974, 54, 536–44. [Google Scholar] [CrossRef]
- Christiansen, J.; Rehfeld, J.F.; Kirkegaard, P. Interaction of calcium, magnesium, and gastrin on gastric acid secretion. Gastroenterology 1979, 76, 57–61. [Google Scholar] [CrossRef] [PubMed]
- Inoue, K.; Wiener, I.; Fagan, C.J.; Watson, L.C.; Thompson, J.C. Correlation between gallbladder size and release of CCK after oral magnesium sulphate in man. Ann. Surg. 1983, 197, 412–5. [Google Scholar] [CrossRef]
- Kivilaakso, E. Contribution of ambient HCO3 to mucosal protection on intracellular pH in isolated amphibian gastric mucosa. Gastroenterology 1983, 85, 1284–9. [Google Scholar] [CrossRef]
| Fixed residue at 180°C | Definition |
| ≤50 mg/L | Very-low-mineral-content water (or light mineral water) |
| 50–500 mg/L | Low-mineral-content water |
| 500–1,500 mg/L | Medium-mineral-content water |
| >1,500 mg/L | Rich-mineral-content water |
| Ion | Concentration |
| Bicarbonate (HCO3-) | >600 mg/L |
| Sulfate (SO42-) | >200 mg/L |
| Chloride (Cl-) | >200 mg/L |
| Calcium (Ca2+) | >150 mg/L |
| Magnesium (Mg2+) | >50 mg/L |
| Fluoride (F-) | >1 mg/L |
| Ferrous (Fe2+) | >1 mg/L |
| Sodium (Na+) | >200 mg/L |
|
Bergamo aqueduct tap water (wash-out) |
Bicarbonate mineral water (Aqua 3) |
Oligomineral water (maintenance) |
|
| Fixed residual at 180°C | 218.0 mg/L | 672.1 mg/L | 132.9 mg/L |
| pH at source | 8.0 UpH | 6.1 UpH | 7.8 UpH |
| Free C02 at source | N/a | 821.1 mg/L | 3.5 mg/L |
| Bicarbonates (HCO3-) | 222.0 mg/L | 781.1 mg/L | 134.0 mgL |
| Sulfates | 20.0 mg/L | 7.8 mg/L | 1.8 mg/L |
| Potassium | 0.80 mg/L | 3.89 mg/L | 0.73 mg/L |
| Sodium | 6.5mg/L | 73.0 mg/L | 3.9 mg/L |
| Calcium | 50.0mg/L | 158.1 mg/L | 35.2 mg/L |
| Magnesium | 14.0 mg/L | 34.4 mg/L | 5.3 mg/L |
| Fluorides | 0.06 mg/L | 0.06 mg/L | 0.05 mg/L |
| Chlorides | 3.0 mg/L | 6.7 mg/L | 1.3 mg/L |
| Silica | N/a | N/a | 16.4 mg/L |
| Nitrates (NO3-) | 5.0 mg/L | <0.06 mg/L | 3.9 mg/L |
| Nitrogens | N/a | <0.02 mg/L | N/a |
| Basal | |
|
Gender - Males - Females |
21 (42.0%) 29 (58.0%) |
|
Age (years) - Mean±SD - Range |
52.8±14.9 28 - 80 |
|
Weight (kg) - Mean±SD - Range |
71.6±12.7 47 - 98 |
|
Height (cm) - Mean±SD - Range |
168±11 149 - 191 |
|
BMI (kg/m2) - Mean±SD - Range |
25.2±3.2 17.9 – 32.4 |
|
Weight status classes Underweight (BMI<18.5 kg/m2) Normal weight (BMI between 18.5 and <25 kg/m2) Overweight (BMI between 25 and <30 kg/m2) Obese (BMI 30 kg/m2 and above) |
1 (2.0%) 23 (46.0%) 22 (44.0%) 4 (8.0%) |
| Use of antacid drugs | 3 (6.0%) |
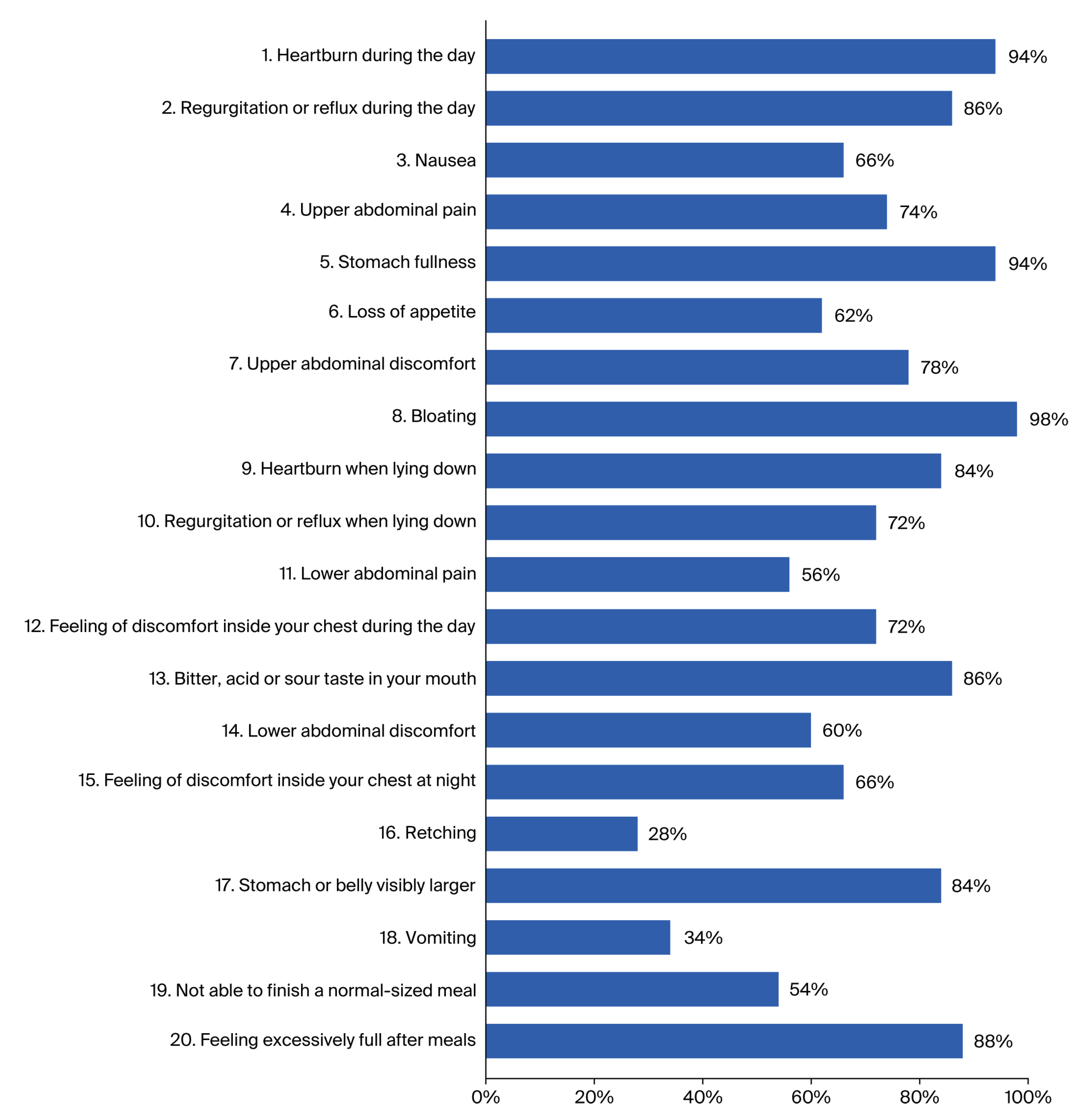
| Subscales of PAGI-SYM severity index |
PAGI-SYM total score |
||||||||||||||
|
Heartburn/ regurgitation |
Nausea/ vomiting |
Postprandial fullness/early satiety | Bloating |
Upper abdominal pain |
Lower abdominal pain |
||||||||||
| Basal (T0) | |||||||||||||||
| Mean±SD | 1.75±0.79 | 0.77±0.99 | 1.83±1.05 | 2.16±1.03 | 1.36±1.07 | 0.96±1.03 | 1.47±0.76 | ||||||||
| After wash-out (T1) | |||||||||||||||
| Mean±SD | 1.69±0.75 | 0.85±0.99 | 1.77±0.99 | 1.90±0.87 | 1.29±1.03 | 1.07±0.97 | 1.43±0.71 | ||||||||
| Effect (Difference vs. T0) | -0.06±0.23 | 0.08±0.24 | -0.06±0.31 | -0.26±0.39 | -0.07±0.31 | 0.11±0.35 | -0.04±0.15 | ||||||||
| (95% CI) | -0.13 to 0.01 | 0.01 to 0.15 | -0.15 to 0.03 | -0.37 to -10.14 | -0.16 to 0.03 | 0.01 to 0.22 | -0.09 to 0.00 | ||||||||
| P valuea | 0.116 | 0.026 | 0.164 | <0.001 | 0.157 | 0.040 | 0.084 | ||||||||
| After bicarbonate mineral water (T2) | |||||||||||||||
| Mean±SD | 1.00±0.78 | 0.42±0.66 | 1.01±0.68 | 1.07±0.77 | 0.72±0.70 | 0.56±0.77 | 0.80±0.62 | ||||||||
| Effect (Difference vs. T1) | -0.69±0.55 | -0.43±0.61 | -0.76±0.69 | -0.83±0.65 | -0.57±0.64 | -0.51±0.69 | -0.63±0.48 | ||||||||
| (95% CI) | -0.86 to -0.53 | -0.61 to -0.25 | -0.97 to -0.55 | -1.03 to -0.64 | -0.76 to -0.37 | -0.72 to -0.30 | -0.78 to -0.49 | ||||||||
| P valuea | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | ||||||||
| After oligomineral water (T3) | |||||||||||||||
| Mean±SD | 1.44±0.70 | 0.79±0.86 | 1.51±0.73 | 1.47±0.97 | 1.24±0.97 | 0.97±0.89 | 1.24±0.69 | ||||||||
| Effect (Difference vs. T2) | 0.45±0.50 | 0.36±0.57 | 0.50±0.47 | 0.40±0.81 | 0.52±0.83 | 0.41±0.71 | 0.44±0.50 | ||||||||
| (95% CI) | 0.30 to 0.60 | 0.19 to 0.53 | 0.36 to 0.64 | 0.16 to 0.64 | 0.27 to 0.77 | 0.20 to 0.62 | 0.29 to 0.59 | ||||||||
| P valuea | P<0.001 | P<0.001 | P<0.001 | 0.001 | P<0.001 | P<0.001 | P<0.001 | ||||||||
| Bicarbonate vs. oligomineral water | |||||||||||||||
| Difference of the effects | -1.14±0.99 | -0.79±1.09 | -1.26±1.06 | -1.23±1.26 | -1.09±1.33 | -0.92±1.34 | -1.07±0.93 | ||||||||
| (95% CI) | -1.44 to -0.84 | -1.12 to -0.46 | -1.58 to -0.94 | -1.61 to -0.85 | -1.49 to -0.69 | -1.33 to -0.52 | -1.35 to -0.79 | ||||||||
| P valueb | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | P<0.001 | ||||||||
|
No. of patients |
P vs. previous visita |
Changes vs. previous visit | ||||
| Suspension | Unchanged |
New assumption |
||||
| Basal (T0) | 2 (4.4%) | - | - | - | - | |
| After wash-out (T1) | 15 (33.3%) | <0.001 | - | 32 (71.1%) | 13 (28.9%) | |
| After bicarbonate mineral water (T2) | 6 (13.3%) | 0.004 | 9 (20.0%) | 36 (80.0%) | - | b |
| After oligomineral water (T3) | 12 (26.7%) | 0.070 | 1 (2.2%) | 37 (82.2%) | 7 (15.6%) | b |
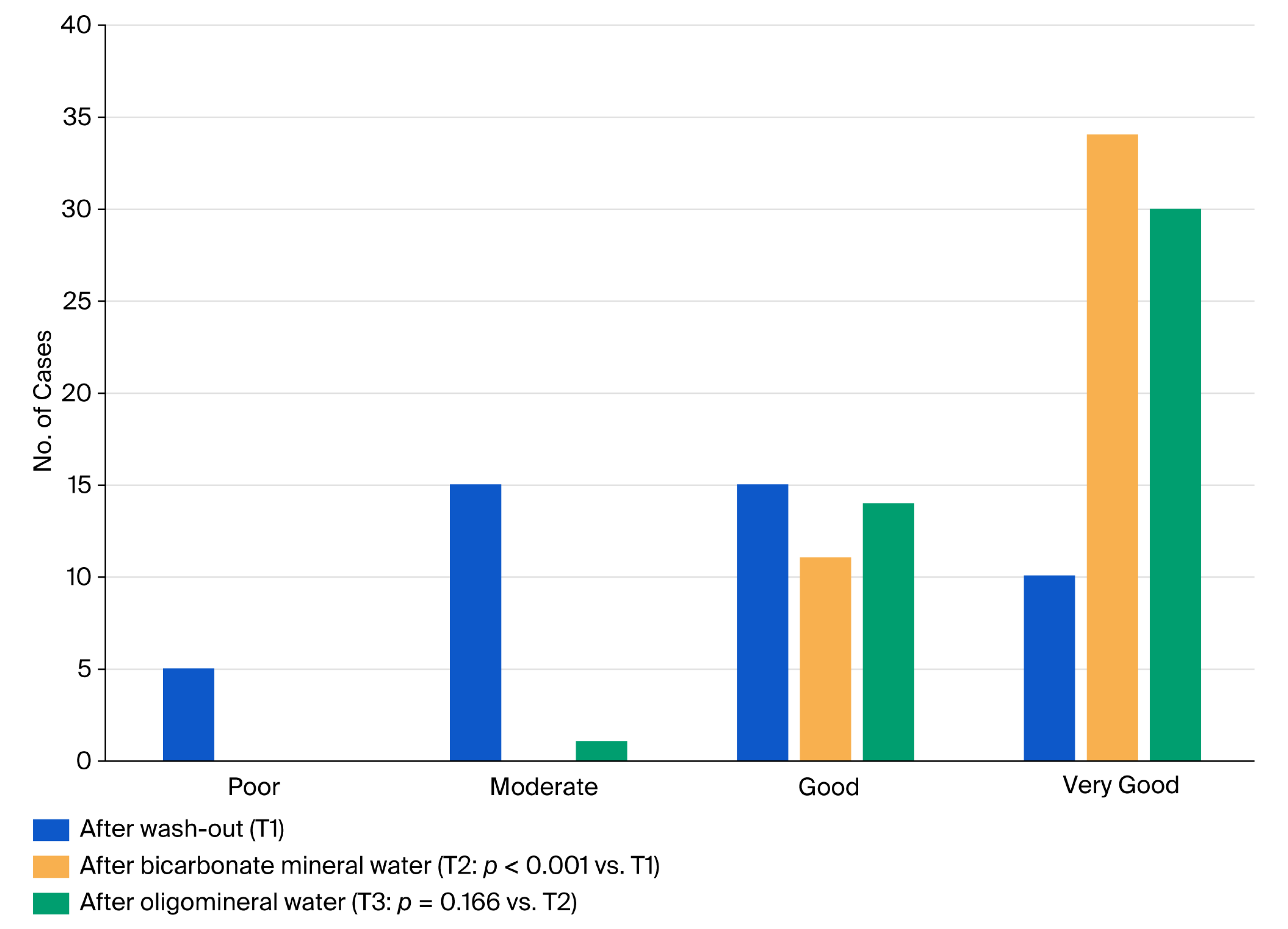
| Mean±SD | Range | |
| After bicarbonate mineral water (T2) | 7.2±2.2 a | 2-10 |
| After oligomineral water (T3) | 4.6±2.0 a | 1-9 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




