Submitted:
13 March 2026
Posted:
13 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Setting and Participants
- Home-dwelling HaH patients (HaH-home)
- Institutionalized HaH patients (HaH-institution)
2.3. Variables and Definitions
2.4. Outcomes
2.5. Statistical Analysis
2.6. Ethical Considerations
3. Results
3.1. Study Population
3.2. Prevalence of Hypernatremia
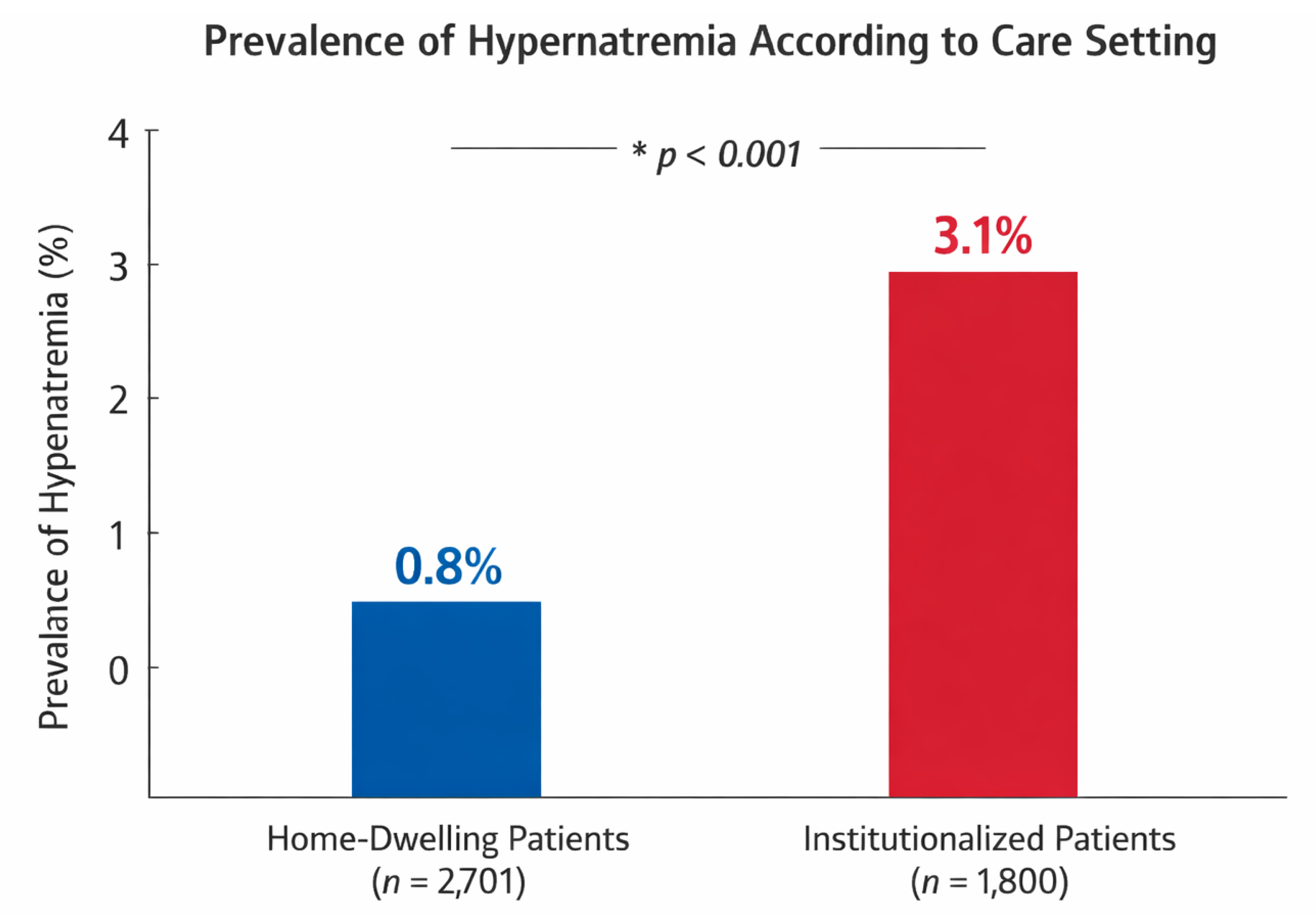
3.3. Clinical Characteristics of Institutionalized Patients with Hypernatremia
| Variable | No hypernatremia (n = 1743) | Hypernatremia (n = 57) | p value |
|---|---|---|---|
| Age, years, mean ± SD | 90 ± 8 | 88 ± 8 | NS |
| Male sex, % | 25 | 21 | NS |
| Barthel Index, mean | 15 | 11 | 0.041 |
| GDS stage, mean | 5.5 | 6.0 | 0.033 |
| Variable | Mild (146–155) | Severe (156–165) | Extreme (>165) | p value |
|---|---|---|---|---|
| n = 35 | n = 22 | n = 27 | ||
| Age, years, mean | 88 | 89 | 88 | NS |
| Barthel Index, mean | 12 | 13 | 10 | NS |
| GDS stage, mean | 6 | 6 | 6 | NS |
| In-hospital mortality, % | 37 | 27 | 33 | NS |
| 30-day mortality, % | 74 | 41 | 63 | 0.041 |
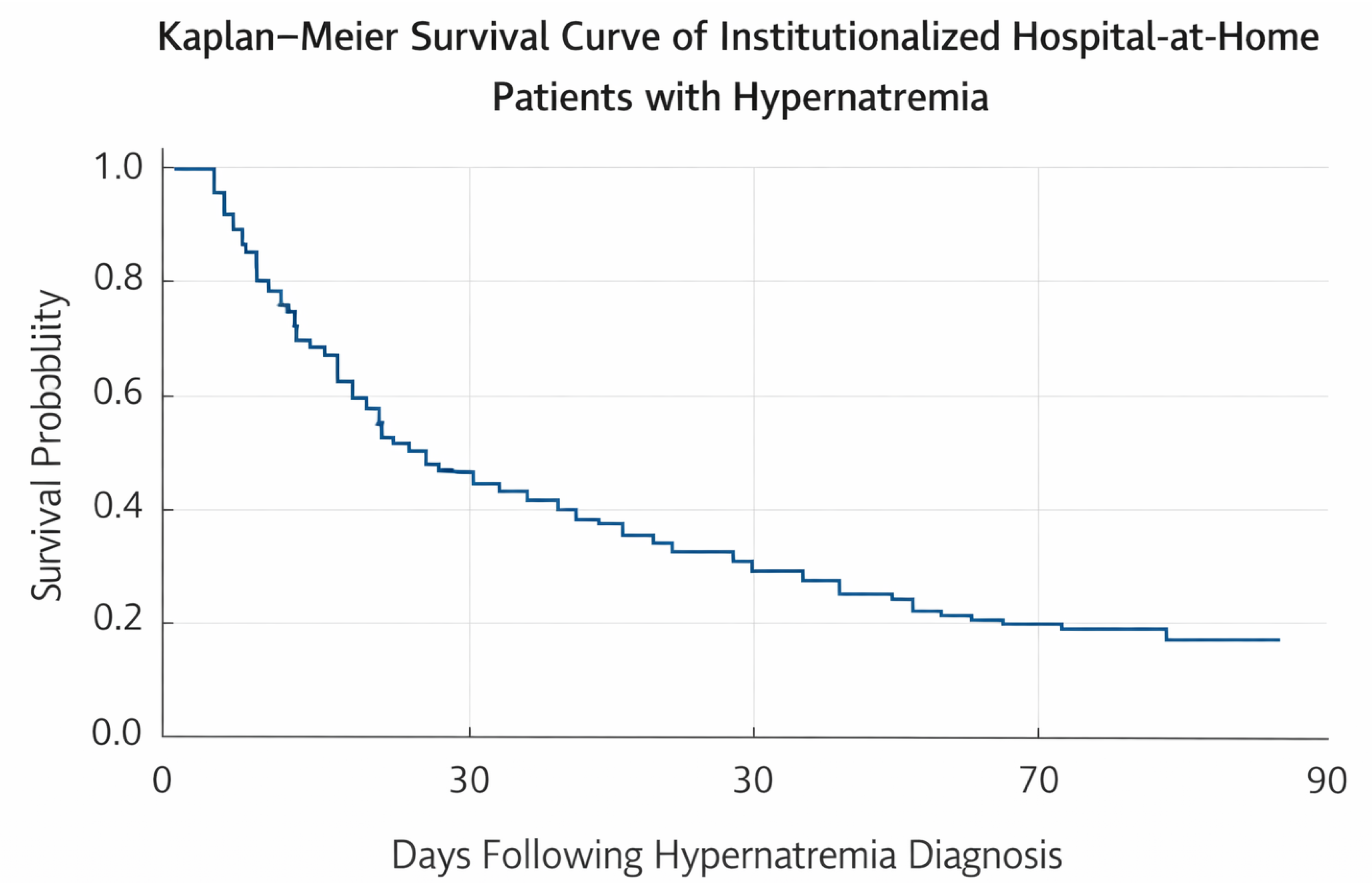
3.4. Mortality and Survival Analysis
4. Discussion
5. Limitations
6. Future Directions
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| HaH | Hospital at Home |
| DOAJ | Directory of open access journals |
| TLA | Three letter acronym |
| LD | Linear dichroism |
References
- Palevsky, P.M.; Bhagrath, R.; Greenberg, A. Hypernatremia in hospitalized patients. Annals of Internal Medicine 1996, 124, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Adrogué, H.J.; Madias, N.E. Hypernatremia. New England Journal of Medicine 2000, 342, 1493–1499. [Google Scholar] [CrossRef] [PubMed]
- Chassagne, P.; Druesne, L.; Capet, C.; Ménard, J.F.; Bercoff, E. Clinical presentation of hypernatremia in elderly patients: a case control study. Journal of the American Geriatrics Society 2006, 54, 1225–1230. [Google Scholar] [CrossRef] [PubMed]
- Tolea, M.I.; Morris, J.C.; Galvin, J.E. Dysnatremia in relation to frailty and age in community-dwelling adults in the National Health and Nutrition Examination Survey. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences 2017, 72, 376–382. [Google Scholar] [CrossRef]
- Corona, G.; Giuliani, C.; Parenti, G. Moderate hyponatremia is associated with increased risk of mortality: a systematic review and meta-analysis. European Journal of Endocrinology 2014, 170, 745–752. [Google Scholar] [CrossRef]
- Liamis, G.; Filippatos, T.D.; Elisaf, M.S. Evaluation and treatment of hypernatremia: a practical guide for physicians. Postgraduate Medicine 2016, 128, 299–306. [Google Scholar] [CrossRef] [PubMed]
- Wolff, A.; Stuck, A.E.; et al. Are patients admitted to hospitals from care homes dehydrated? A retrospective cohort study to develop a predictive model. Journal of the Royal Society of Medicine 2015, 108, 259–261. [Google Scholar] [CrossRef] [PubMed]
- Torrens, M.; et al. Hypernatremia in hospitalized patients: a large population-based study. Kidney360 2022, 3, 649–659. [Google Scholar] [CrossRef] [PubMed]
- Spasovski, G.; Vanholder, R.; Allolio, B. Clinical practice guidelines on diagnosis and treatment of hyponatraemia. Nephrology Dialysis Transplantation 2014, 29, i1–i39. [Google Scholar] [CrossRef] [PubMed]
- Burst, V. Hyponatremia and hypernatremia: A practical approach to disorders of sodium and water balance. Deutsches Ärzteblatt International 2015, 112, 745–752. [Google Scholar] [CrossRef]
- Wald, R.; Jaber, B.L.; Price, L.L.; Upadhyay, A.; Madias, N.E. Impact of hospital-associated hyponatremia and hypernatremia on mortality. Archives of Internal Medicine 2010, 170, 294–302. [Google Scholar] [CrossRef] [PubMed]
- Snyder, N.A.; Feigal, D.W.; Arieff, A.I. Hypernatremia in elderly patients. A heterogeneous, morbid, and iatrogenic entity. Annals of Internal Medicine 1987, 107, 309–319. [Google Scholar] [CrossRef] [PubMed]
- Assadi, F. Hypernatremia in the geriatric population. Clinical Interventions in Aging 2014, 9, 1987–1992. [Google Scholar] [CrossRef] [PubMed]
- Arampatzis, S.; Frauchiger, B.; Fiedler, G.M.; Leichtle, A.B.; Otto, T.; Ramineni, S.; Benz, C.; Schwarz, C. Characteristics, symptoms and outcome of severe dysnatremias present on hospital admission. The American Journal of Medicine 2012, 125, 1125.e1–1125.e7. [Google Scholar] [CrossRef] [PubMed]
- Lindner, G.; Funk, G.C. Hypernatremia in critically ill patients. Journal of Critical Care 2013, 28, 216.e11–216.e20. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Xu, X.; Fan, H.; et al. Hypernatremia is associated with mortality in severe elderly sepsis patients: a retrospective cohort study. PLoS ONE 2024, 19, e0310245. [Google Scholar] [CrossRef]
- El-Sharkawy, A.M.; Sahota, O.; Lobo, D.N. Acute and chronic effects of hydration status on health. Nutrition Reviews 2015, 73, 97–109. [Google Scholar] [CrossRef] [PubMed]
| Variable | HaH-home (n = 2701) | HaH-institution (n = 1800) | p value |
|---|---|---|---|
| Age, years, mean ± SD | 69.5 ± 18.0 | 90.1 ± 8.0 | <0.001 |
| Functional dependency (Barthel Index) | Lower | Higher | <0.001 |
| Cognitive impairment (GDS) | Lower | Higher | <0.001 |
| Hypernatremia prevalence, n (%) | 22 (0.8) | 57 (3.1) | <0.001 |
| Variable | Survivors (n = 56) | Non-survivors (n = 28) | p value |
|---|---|---|---|
| Age, years, mean | 89 | 87 | NS |
| Male sex, % | 20 | 25 | NS |
| Barthel Index, mean | 12 | 11 | NS |
| GDS stage, mean | 5.9 | 5.5 | NS |
| Serum sodium, mEq/L, mean | 160 | 160 | NS |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




