1. Introduction
The COVID-19 pandemic, caused by the highly contagious SARS-CoV-2 virus, has evolved into a global crisis [
1]. As of February 1, 2023, it has affected 670,597,192 people and resulted in 6,832,607 deaths, justifying its classification as a pandemic by the World Health Organization [
2]. Stringent preventive measures, including barrier methods and travel restrictions, were implemented with 513 946 confirmed cases and 6 710 deaths as of 30 July 2021 in the 16 countries of West Africa, [
3]. All these measures have affected the population psychologically. This pandemic has been perceived differently worldwide, particularly in West Africa. Each individual perceives the different aspects of risk perception of emerging infectious diseases differently and tends to view the situation as a risk, especially in a pandemic case [
4].
As a result of the COVID-19 pandemic disaster, the population has adopted protective measures such as using non-conventional medicine. In general, many reasons have led people to use alternative medicine, such as the perception of illness, the need for autonomy in health care, dissatisfaction and distrust of Western medicine, and individual values and beliefs [
5]. The benefits of using certain non-conventional medicines are recognised for diseases such as cancer, asthma, diabetes, cardiovascular disease, liver disease and rheumatology [
6]. As COVID-19 is an unknown disease, Africans have turned to non-conventional medicines as preventive and curative measures. This practice has affected the disease dynamics.
Level of exposure, certain socio-demographic factors, personality and other individual characteristics are risk factors for post-traumatic stress disorder [
7]. It is therefore important to understand the socio-demographic factors (gender, age, marital status, etc.) that are likely to influence COVID-19 risk perception (risk feeling, risk analysis, affective attitude), the use or not of non-conventional medicine and COVID-19 dynamics.
Structural Equation Modeling is the most appropriate method to understand the effect between these variables simultaneously. Structural equation models (SEM) are multivariate techniques for modeling causal structures in data. They allow the simultaneous assessment of the existence of causal relationships between several variables. Many variables may combine and interact to simultaneously influence a phenomenon, such as the risk perception associated with disease onset [
8]. Partial Least Squares is a more robust approach for testing substantive theories or psychological constructs that are generally complex [
8]. It handles data heterogeneity. This method is the most appropriate approach to understanding this complex relationship between socio-demographic factors, COVID-19 risk perception, use or not of non-conventional medicine and COVID-19 dynamics.
Numerous studies provide valuable insights into the perception of COVID-19 risk, highlighting the influence of sociodemographic factors. The study on COVID-19 risk perception and protective behavior in Italy revealed the significant impact of sociodemographic variables on risk perception, affecting protective measures and cultural worldview [
9]. Perception scores for COVID-19 risk can vary, focusing on dimensions such as severity, the likelihood of family and friends getting infected, and general worry [
8]. [
10] indicated heightened awareness of personal risks among sociodemographic groups during different phases of lockdown.
A great deal of work has been done on risk perceptions. The public risk perception of COVID-19 has been assessed around the world (America, Asia and Europe) using national samples [
8]. In addition, [
11] investigated the cognitive dimensions of Ebola risk perceptions. In the work of Anthony [
12], public opinion surveys were examined to determine their usefulness in explaining public risk perceptions of global climate change. The proliferation of misinformation, such as linking child deaths to Western vaccination in Guinea [
13], and the prevalent of non-conventional medicine use in West Africa [
14] have significantly influenced public responses to COVID-19. In Ivory Coast, the popular success of neem, whose leaves and seeds are believed to combat the new coronavirus, led to uncontrolled pruning of many trees. A survey conducted in Egypt, Morocco, South Africa, Côte d’Ivoire, Senegal, and Nigeria revealed that 40% of respondents believed that drinking lemon juice and vitamin C was effective against the virus [
15].
Although public risk perception of COVID-19 has been studied in Europe, America and Asia ([
16]), it has not yet been studied in Africa, particularly West Africa, with a focus on the use of traditional medicine. This study aims to assess the impact of non-conventional medicine on COVID-19 risk perception, taking into account various sociodemographic factors and comparing two algorithms (PLS-SEM and PLSc-SEM). Specifically, the study aims to: (i) to examine the influence of socio-demographic factors on the perception of risk related to COVID-19 and the use of non-conventional medicine in West Africa, (ii) to evaluate and compare the relative effectiveness of the PLS-SEM and Consistent PLS (PLSc-SEM) algorithms and (iii) to estimate and predict the impact of non-conventional medicine on the risk perception related to COVID-19. This research will enable policy makers and health workers to make correct decisions in the management of epidemics based on unconventional medicine and the emotional state of the local population.
2. Overview on PLS, PLS-SEM and Consistent PLS
2.1. Partial Least Squares Method
PLS regression was developed in economics by [
17] to overcome weaknesses in theory and data. It has since been applied to other fields such as chemistry and epidemiology. The management of small data sets, multicollinearity and missing values are real problems faced by researchers. The PLS method was developed to solve these problems. In [
18], Wold introduced PLS to structural equation methods. It is the prediction of dependent variables from explanatory variables (latent variables) and is primarily a prediction technique. It is mainly a predictive technique but it can be interpretive when the exploratory analysis is used before SEM is applied. The predictive power or global fit of the model can be assessed using the goodness of fit (GoF) index.
2.2. PLS-SEM Algorithm
Partial least square structural path modeling aims to (i) minimize the error terms, (ii) explain the variance, and (iii) maximize the value of the coefficient of determination of the endogenous constructs by using the available data to estimate the path relationships between the latent variables and their indicators in the model ([
19]). This algorithm is used to compute the model parameters, including external weights, external loadings and path coefficients ([
20]). However, as the sample size increases, the estimates produced by the algorithm do not approach the true value. In addition, the method tends to overestimate loadings in absolute terms ([
21]) and underestimate correlations between latent variables ([
22]. There are three steps:
step 1: Iterative estimation of weights and latent variable scores until convergence,
step 2 : Estimation of path and loading coefficients,
step 3 : Estimation of location parameters.
2.3. Consistent PLS Algorithm (PLSc)
Consistent PLS is an extension of PLS-SEM. It was developed by ([
22]) and has the advantage of correcting estimates when PLS is applied to reflective constructs: Path coefficients, inter-construct correlations and indicator loadings become consistent. PLSc aims to overcome the statistical inconsistency associated with the traditional PLS estimation algorithm ([
21]). The Estimates asymptomatically approach true values when this algorithm is used. There are four steps in the consistent PLS ([
22]).
Step 1: Traditional PLS
By using the means of the traditional iterative PLS algorithm calculate
Obtain the inconsistent latent variable correlations
Step 2: Calculate
Step 3: Correction for attenuation
Obtain consistent construct correlation r using the classical correction for attenuation:
Step 4: Estimation of path coefficients
Estimate the consistent path coefficients based on the consistent construct correlations by using ordinary least squares (OLS) in the recursive models.
-
Used other adequate estimators (e.g., two-stage) least squares for the nonrecursive models.
W is the estimated weight vector of the latent variable and S is the empirical covariance matrix of the latent variable’s indicators.
3. Materials and Methods
3.1. Theoritical Model and Measure
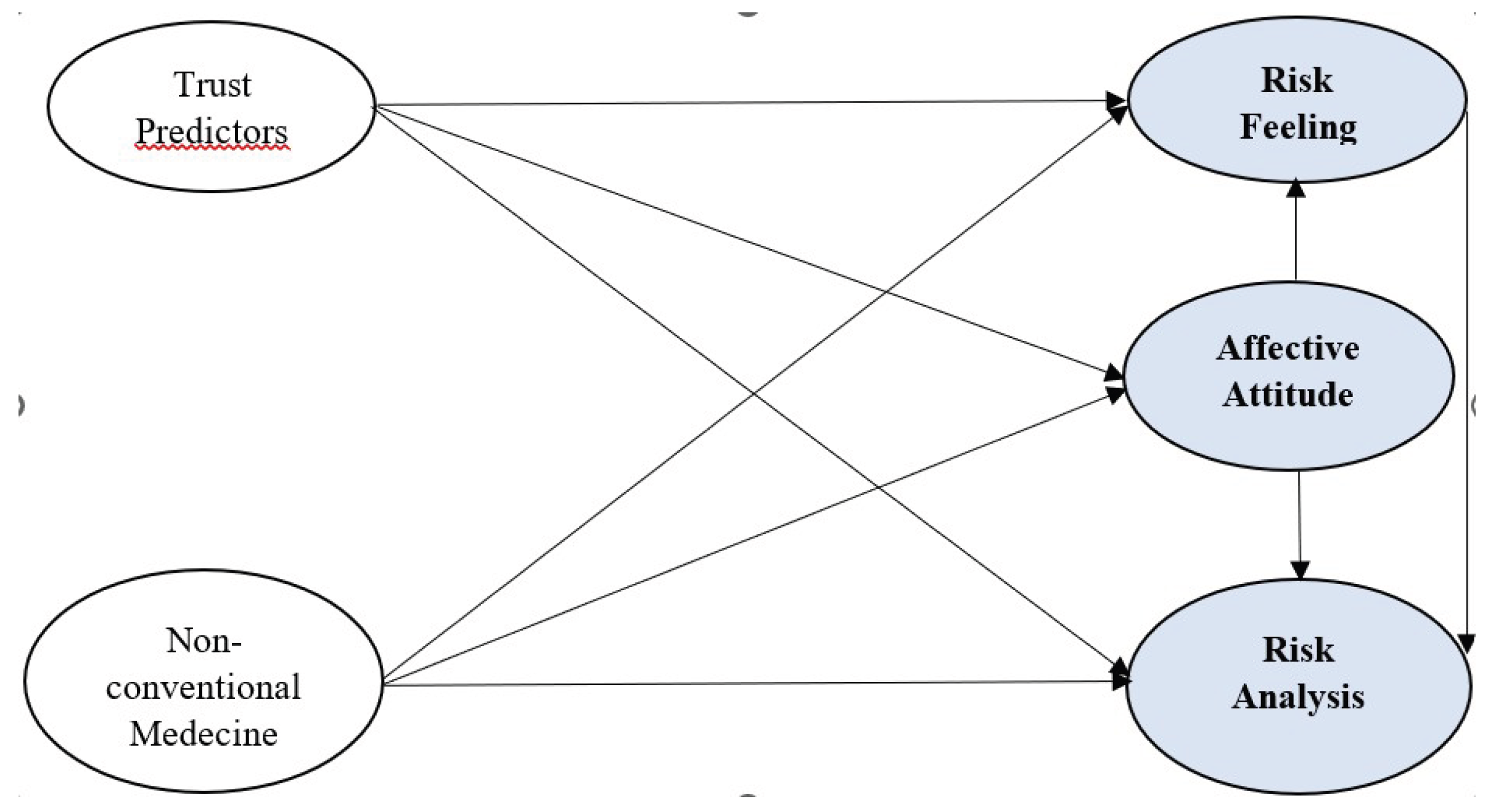
COVID-19 risk perception (risk feeling and risk analysis) and affective attitude are considered dependent variables. In our model (
Figure 1), the independent variables are the trust predictors (trust in the health professionals, Confidence in the government, trust in the media) and non-conventional medicine. The items linked to the variables are summarized in
Table 1 and measured using the Likert scale between 5 and 7 points.
3.2. Data Collection
To assess COVID-19 risk perception in West Africa and its association with non-conventional medicine, We interviewed people in 4 West African countries. An online quantitative survey was conducted over 5 week period from 25 August to 2 October 2023 and a physical survey was conducted from 28 September to 2 October 2023. Participation in the study was completely voluntary. Respondents aged 18 and over were informed of the purpose of the study and gave their implied verbal consent by completing the questionnaire. A written consent form was also available for the physical survey, but very few people signed it. The survey link was shared on various social platforms and participants over 18 years were encouraged to participate and share the link across Benin, Togo, Ghana and Ivory Coast. A physical survey was also conducted in these countries to ensure inclusivity. The process of selecting participants was based on selective data collection. It consisted of selecting a group of older people and a group of people with no formal education after observation and asking the participants. The study relies exclusively on the use of anonymized and non-identifiable data collected through voluntary questionnaires, without the collection of sensitive personal information. This means that the data collected cannot directly or indirectly identify the participants. No identity-related information such as names, addresses or contact details were collected. The study does not involve medical intervention or experimentation on human subjects, but focuses solely on questions related to emotional states. It is limited to investigating perceptions of COVID-19 risks and behaviors related to the use of non-conventional medicine, without direct involvement in clinical decision-making.
Following the rule of thumb, 10 for the minimum sample size (10 times the arrows pointing to latent variables), the questionnaire covered socio-demographic characteristics, risk perception, affective attitude, use and effectiveness of non-conventional medicine, and various risk predictors. These variables were derived from previous studies [
7,
8,
23,
24,
28,
30] and are measured using Likert scores [
19].
3.3. Statistical Analysis
3.3.1. Socio-Demographic Characteristics
Descriptive statistics were used to characterize the variables in this study. To investigate the influence of socio-demographic variables on risk perception and the impact of the use of non-conventional medicine, nominal polychotomous logistic regression and binary logistic regression were used. Due to the limited number of participants in some variable categories, recategorization was carried out to ensure meaningful analyses. Since the indicators within each construct were strongly correlated and shared similar measurement scales, they were aggregated to derive total scores. After estimating the scores for each construct, a three-level categorization was performed for analysis.
3.3.2. Performance of PLS-SEM and Consistence PLS (PLSc-SEM)
The external model validity was performed by comparing PLS-SEM and Consistent PLS through fit measures (NFI, GFI and SRMR) and selection criterion (AIC).
3.3.3. Estimation and Predictive Power of Non-Conventional Medicine on the Covid-19 Risk Perception
To assess the model’s predictive performance, the PLSpredict algorithm from [
31] was used and compared with linear regression (LM). The focus is on determining whether non-conventional medicine can predict risk perception, with the model being redefined accordingly. In addition, k-fold cross-validation was performed, where k is the number of data subgroups. For this study, k=10 is chosen based on the recommendation of [
32]. To evaluate the predictive power, the RMSE (root-mean-square error) metric was used to quantify the degree of prediction error [
20] and compared with LM values. The analysis was conducted using Rstudio software with SEMinR and cSEM packages.
4. Results
4.1. Demographic Profile of Respondents
688 participants were recruited (online and field survey) with 79 excluded because they did not belong to the eligible countries, namely Benin, Togo, Ghana and Ivory Coast. 609 adults participated including 360 (59.11%) from the physical survey. 171 (28.08%) were from Benin, 200 (32.84%) from Ivory Coast, 152 (24.96%) from Togo and 86 (14.12%) from Ghana (
Table 2). More than half (64%) of the respondents were male and 36% were female; 75% were aged between 21 and 40; 50% had no children and 47% had between 1 and 6 children; 63% of the respondents were single and 34% were married; 68% of the respondents’ educational level categories, to give us an overview, had either a secondary education, a bachelor’s degree or equivalent and a master’s degree (
Table 2). Respondents who used non-conventional medicine made up 68% of the total sample.
4.2. Impact of Socio-Demographic Factors on the Use of Non-Conventional Medicine
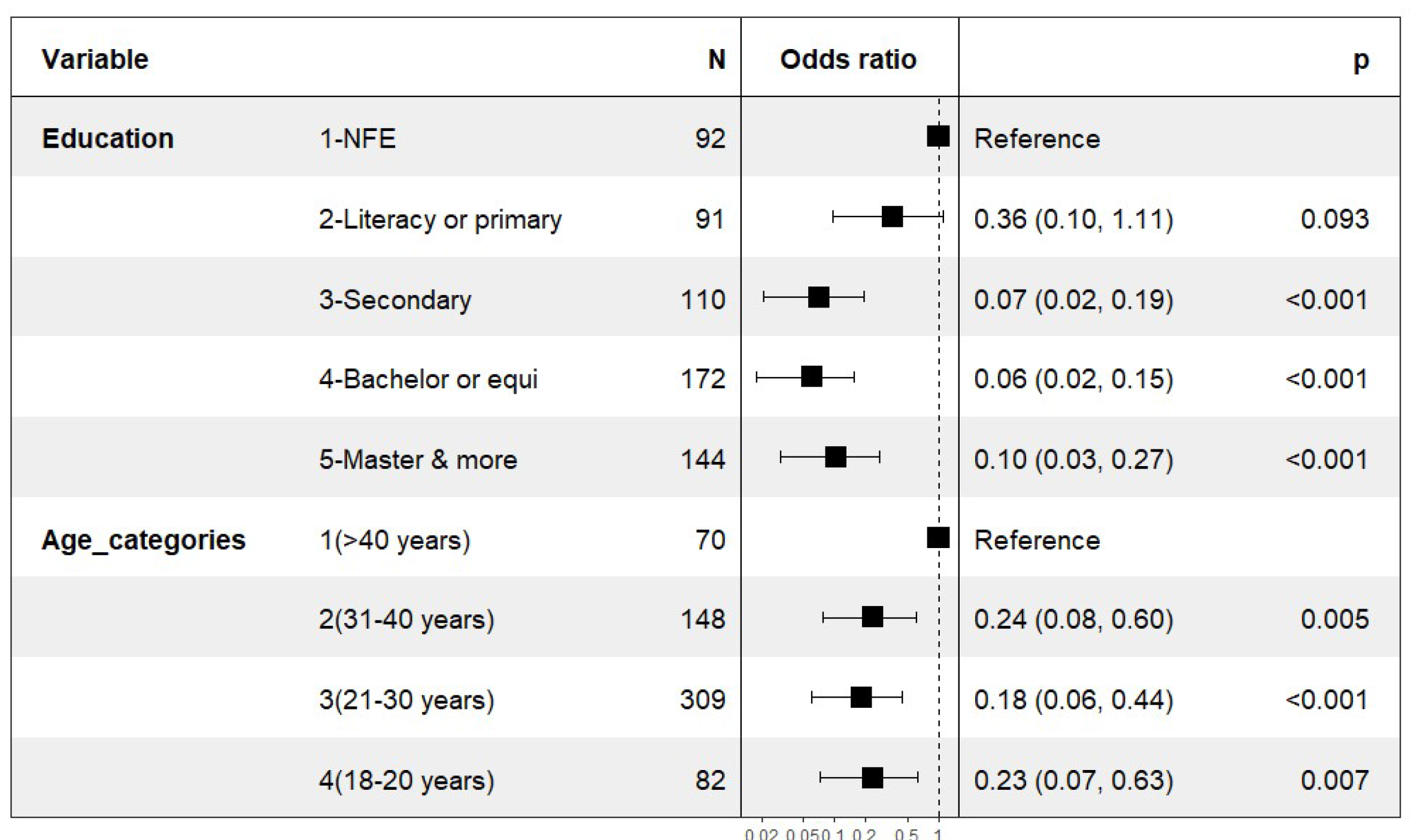
The variables such as Gender, number of children and marital status were not significant. Only educational level and age were significantly associated with using non-conventional medicine. Thus, compared with people with no formal education, the probability of respondents using non-conventional medicine decreased with odds ratios of 0.7 (95 % CI 0.02, 0.19) for secondary education, 0.06 (95 % CI 0.02, 0.15) for bachelor’s degree or equivalent, and 0.10 (95 % CI 0.03, 0.27) for master’s degree and above (
Figure 2). In terms of age categories, compared with participants aged over 40, the probability of other age categories using unconventional medicine was generally low (0.18 - 0.24).
4.3. Overview of COVID-19 Risk Perception
Overall COVID-19 risk perception is highly significant between countries (p-value = 2.2e-16) and education level (p-value = 7.29e-06)
Table 3. It was also significant between gender (p-value = 0.007) and age groups (p-value = 0.0479). Women and participants with no formal education were significantly associated with higher risk perception than men and those with higher education levels respectively. There was no significant difference in risk perception according to marital status and number of children.
4.4. Impact of Socio-Demographic Factors on the Covid-19 Risk Perception
There was a higher probability for males to feel low-risk perception (vs moderate) than females, with an odds ratio of 1.67 (95% CI: 1.02 to 2.75) (
Table 4). Respondents with a Bachelor’s degree or equivalent and those with a Master’s degree and above, compared to those with no formal education, had increased low-risk perception (vs moderate). In terms of age, there was a very higher probability for the category between 18 and 20 years to feel low-risk perception (vs moderate), compared to those over 40, with an odds ratio of 12.2 (95% CI: 4.28 to 34.9). High risk perception (vs moderate) was reduced among respondents with a Bachelor’s degree or equivalent and those with a Master’s degree and above, with odds ratios of 0.4 (95% CI: 0.22 to 0.73) and 0.49 (95% CI: 0.26 to 0.89), respectively.
The risk analysis shows that the level of low risk (vs moderate) was high among those with literacy or primary education, bachelor’s degree or equivalent and master’s degree and above compared to those with no formal education, with odds ratios of 2.24 (95% CI: 1.03, 4.88), 3.14 (95% CI: 1.53, 6.45) and 3.61 (95% CI: 1.74, 7.50), respectively. In the age category, the analysis of low risk (vs moderate risk) increased for participants aged 18 to 20 (OR: 18.4) and between 21 to 30 (OR: 2.44) compared to those over 40. Regarding marital status, the feeling of low risk compared to moderate risk was significantly higher for married compared to single status.
4.5. Relative Performance of PLS-SEM and PLSc-SEM
Items
and
(
Table 1) were removed from the analysis because of their low saturation. Except for
(0.44) in PLSc-SEM, all items have a loading greater than 0.5. We generally note that the loadings of PLS-SEM were greater compared to those of PLSc-SEM (
Table 5). According to [
33], the AVE is usually used to measure convergent validity and the value should be greater than 0.5 to indicate satisfactory convergent validity. All the AVEs were greater than 0.5 [
34] except that of the PLSc-SEM for affective attitude and the CRs greater than 0.7 [
35]. Despite these conditions, all the PLS-SEM values are higher than the PLSc-SEM values. Almost all the AVEs of the PLS-SEM were greater than 0.6 and only one was less than 0.58 and the CR were more than 0.8. As for PLSc-SEM, two values were less than 0.8 and more than 0.6 for CR and AVE respectively. In this study, the HTMTs (hétéro-trait-mono-trait) of PLSc-SEM and PLS-SEM were all less than 0.85[
36] indicating the good discriminant validity (
Table 6). To evaluate a model, it’s important to assess the goodness of fit of the model for improvement. The goodness-of-fit index (GFI) and the standardised root mean square residual (SRMR) are used to measure how well the parameter estimates generated in the proposed model fit the population matrix. An RMSEA less than or equal to 0.05 and a GFI greater than or equal to 0.95 indicates an excellent fit [
37]. The NFI measures a model by comparing the Chi-square test value of the model with the Chi-square value of the null model. An NFI greater than or equal to 0.9 is generally considered to indicate a good fit [
37,
38]. In this study, the Normed Fit Index (NFI) and the goodness-of-fit Index (GFI) are slightly close to 1 and the Standardize Root Mean Square Residual (SRMR) is 0.08 lower for the two models (
Table 7). Apart from the NFI (0.76) of the PLS-SEM which was equal to that of the PLSc-SEM, the other indices were better. However, the values of the indices are quite similar. The AICs of the PLSc-SEM model were all lower and therefore seem good compared to those of the PLS-SEM.
4.6. Estimation and Prediction of the Impact of Non-Conventional Medicine on the COVID-19 Risk Perception
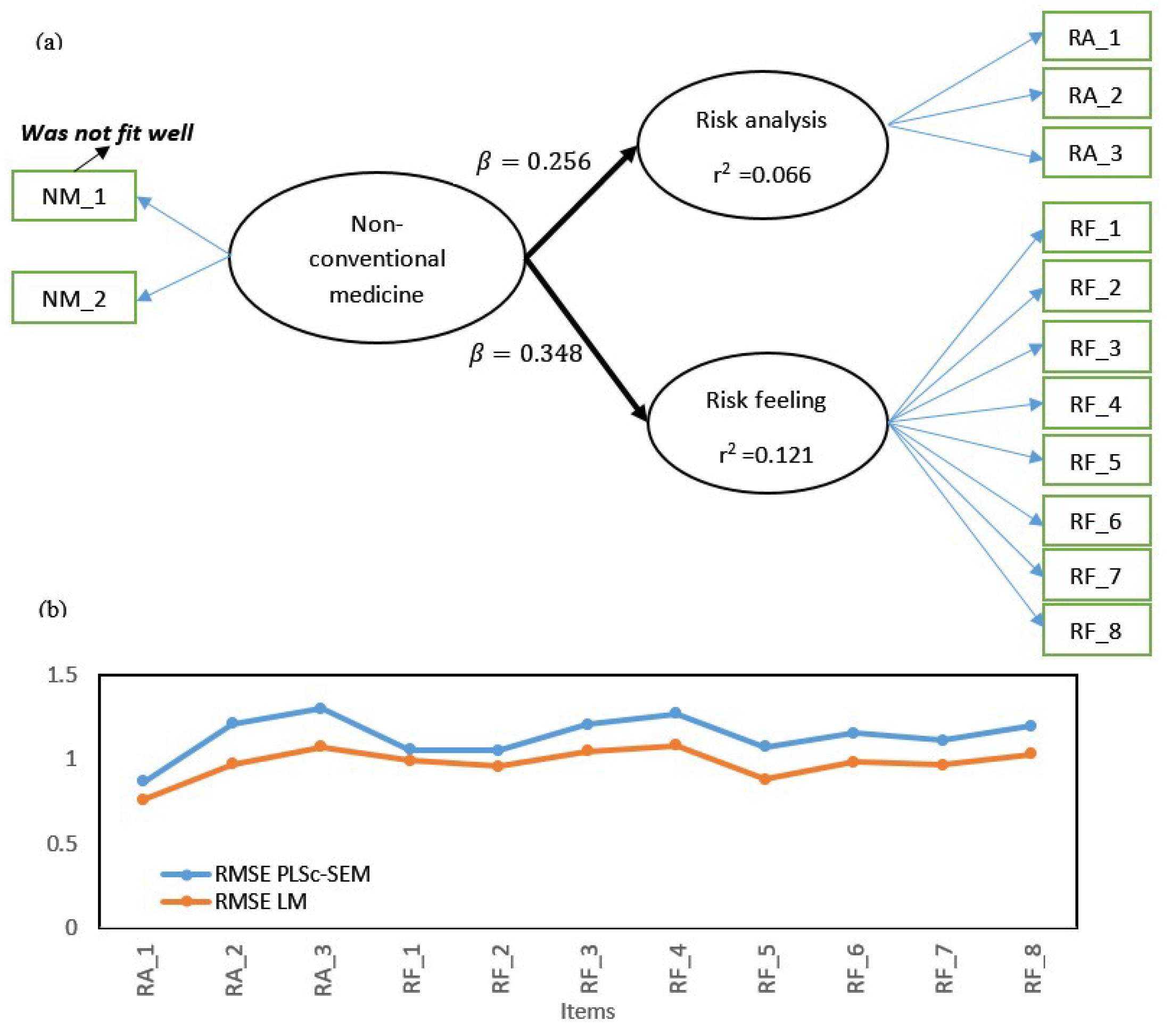
Figure 3 summarizes the estimation of the relationships (
Figure 3a) and the predictive power (
Figure 3b) of belief in non-conventional medicine to deal with COVID-19. In this analysis, we chose the consistent PLS (PLSc-SEM) for the predictive power due to its performance in terms of estimating the coefficients with the bootstrap. The relationships between non-conventional medicine and risk analysis and between non-conventional medicine and risk feeling were positive with respective coefficients of 0.256 and 0.348 (
Figure 3a). The root mean square error (RMSE) of the loadings of the linear model are all lower than those of the consistent PLS (
Figure 3b).
5. Discussion
5.1. Risk Perception of COVID-19 and the Effect of Socio-Demographic Factors
This study investigated the effect of socio-demographic factors on the risk perception of COVID-19. However, the results showed a very high level of risk perception (both in terms of feeling and analysis) between each country. Thus, this COVID-19 pandemic has been a very stressful issue for the population of West Africa. It has also been shown by [
7] (2021) that there is a high-risk perception among sub-Saharan Africans and those in the diaspora, which is associated with increased knowledge of COVID-19. The results reveal a notable gender disparity in the perception of low risk of COVID-19. Specifically, the odds of perceiving low risk (vs moderate) among men were significantly higher than among women. Indeed, women are more concerned about COVID-19 than men [
39]. This is why they generally express a higher risk [
10], while men tend to evaluate COVID-19 as less risky in terms of risk feeling and risk analysis [
9]. Again, educational level seemed to be a determining factor in risk perception. Participants with a bachelor’s degree or equivalent and those with a master’s degree or higher had a higher perception of low (vs moderate) risk than others. These results suggest that people with a low level of education or non-formal education often perceive a higher risk associated with COVID-19. This seems to contradict the result of [
7], who mention that unemployment and lower levels of education (primary/secondary) were significantly associated with lower risk perceptions towards COVID-19. However, [
10] states that higher levels of education would be associated with lower estimates of mortality from COVID-19 infection.
Age categories played a distinct role in risk perception. The category of 18-20 year olds had a particularly high perception of low risk compared to moderate risk. Age categories remain important in risk analysis. Participants aged between 18 and 30 years showed an increase in the odds ratio of perceived low (vs moderate) risk compared to those aged over 40 years. This suggests that younger people tend to perceive a lower risk of contracting COVID-19. In addition, a study of local and diaspora populations shows that risk perception was significantly lower among sub-Saharan Africans (SSA) in the 18-28 age group than among older groups [
7]. [
9] raise this point in their research by mentioning that young people were less afraid of the coronavirus and were less likely to avoid social proximity than older people. Marital status was another demographic variable of interest, where the perception of low risk versus moderate risk was significantly higher for those who were married than for those who were single.
5.2. Impact of Socio-Demographic Factors on the Use of Non-Conventional Medicine
The primary objective of this work was to assess the impact of socio-demographic factors on the use of non-conventional medicine and the perception of COVID-19 risk. The results highlight the significant impact of education and age on the use of non-conventional medicine. The remarkable contrast in the odds ratios associated with educational attainment suggests that education plays a central role in healthcare choices. Participants with no formal education were more likely to use non-conventional medicine than others. This could be explained by the reasons why families are attracted to this practice and taking into account the cultural context of [
6]. The work of [
40] in patients with epilepsy highlights that a higher level of education increases the likelihood of advising the use of conventional medicine (proven medicine). This work is consistent with our results and it also appears in this study that participants aged between 18 and 40 used less non-conventional medicine, i.e. 75% less than those of an older age.
5.3. Relative Performance of PLS-SEM and PLSc-SEM
We performed a comparative analysis of item loadings, validity and composite reliability of the PLS-SEM (Partial Least Squares Structural Equation Modeling) and Consistent PLS algorithms. The majority of elements present satisfactory loadings, thus demonstrating their suitability for measuring constructions. However, a notable distinction lies in the item loadings between the two models. The results reveal that, in general, the loadings of the PLS-SEM model were higher compared to those of the Consistent PLS(PLSc-SEM). These results are consistent with those of [
41] who also found that apart from one or two outliers, the Consistent PLS provided lower item loadings compared to the PLS. This is evidenced by the values of the AVE and CR of the PLS-SEM which surpass those of the Consistent PLS model in our study and in that of [
41]. This difference raises the question of the ability of the PLS-SEM model to capture more of the variance elements and to establish more robust relationships between the latter and the underlying constructs or the overestimation of the loadings of the indicators by the latter. Indeed, one of the problems of PLS-SEM according to [
22] is the overestimation of loadings and the underestimation of correlations between latent variables. This is also seen in the study of [
42] where the regular PLS-SEM produced higher indicator loadings than the consistent model; on the other hand, most of the beta coefficients of the proposed model are attenuated parallel to the bias literature.
In estimating the impact of non-conventional medicine on COVID-19 risk perception, our results reveal positive relationships. Specifically, believing in non-conventional medicine justifies an increase in populations’ perception of risk. However, the RMSE of Consistent PLS was lower than that of the linear model. This indicates that although there is a significant impact between confidence in non-conventional medicine and perception of the COVID-19 risk, we have a lack of predictive power. Indeed, when PLS-SEM analysis (compared to LM) produces low predictive errors in terms of RMSE for all indicators, this indicates that the model lacks predictive power [
20].
6. Conclusion
The present study evaluated the impact of socio-demographic factors in the use of non-conventional medicine and the perception of COVID-19 risk. It appears that age and level of education significantly influence the use of non-conventional medicine. Respondents over 40 years of age and those with no formal education are more likely to use this medicine. Country, Gender, age and level of education were found to be significant for risk perception. Males, age group (18 to 30 years) and high education levels (Bachelor and more) perceived the risk of COVID-19 less. Comparative analyses of item loadings, validity, composite reliability, path coefficients, fit indices and AICs reveal significant differences between the PLS-SEM and consistent PLS (PLSc-SEM) models. For the measurement model, PLS-SEM overestimated the loadings. However, in the structural model, we found that the consistent PLS showed robust values. It is important to note that the choice between PLS-SEM and Consistent PLS should take into account research objectives and methodological preferences. The result of this study reveals a lack of predictive power between trust in non-conventional medicine and perception of COVID-19 risk. However, there is a significant effect between these two constructs. These findings highlight the importance of carefully selecting the model based on the specific research objectives and desired rigor in the analysis of structural relationships. Ultimately, the choice of model should be guided by the needs of the study and the appropriate significance criteria for interpreting relationships between constructs. We urge health stakeholders at all levels in West Africa to strengthen and sustain their efforts to enhance health policies, ensuring they integrate non-conventional medicine practices and address the emotional well-being of the local population.
Author Contributions
B.R.O. conceptualized and wrote the methodology. N.T.O and B.R.O. performed the formal analysis and wrote the original draft. K.V.S. reviewed and edited the Methodology and the manuscript. J.M.K.A. reviewed and edited the manuscript. and R.G.K. conceptualized, reviewed and supervized the study.
Funding
The Organization for Women in Science for the Developing World (OWSD), a program unit of UNESCO supported by the Swedish International Development Cooperation Agency under grant number 3240324248, provided financial support to the first author during her Ph.D. studies.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki. The ethical review body at the University of Abomey-Calvi has approved and exempted this study from the Institutional Review Board (IRB) approval. It is purely academic research and does not involve medical interventions, clinical trials, or experimental treatments. Participation is also entirely voluntary. The exemption letter and questionnaire are uploaded to the submission site.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Acknowledgments
The authors would like to thank the European & Developing Countries Clinical Trials Partnership (EDCTP) of funder grand number CSA2020E-3131, for the generous financial support given to the second author throughout the two years of his training; we would also like to thank the Centre d’Excellence Africain en Sciences Mathématiques, Informatique et Applications (CEA-SMIA) for the financial support given to the first author. Also, R. Glèlè Kakaï acknowledges the Sub-Saharan Africa Advanced Consortium for Biostatistics (SSACAB) Phase II. The authors have reviewed and edited the output and take full responsibility for the content of this publication
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
The following abbreviations are used in this manuscript:
| AIC |
Akaike Information Criterion |
| CI |
Confidence Interval |
| CR |
Composite Reliability |
| GFI |
Goodness-of-Fit Index |
| HTMT |
Hétéro-Trait-Mono-Trait |
| LM |
Linear Model |
| NFE |
No Formal Education |
| NFI |
Normed Fit Index |
| OR |
Odd Ratio |
| RMSE |
Root Mean Square Error |
| SRMR |
Standardize Root Mean square Residual |
| TNM |
Trust to Non-conventional Medicine |
| UNM |
Use of Non-conventional Medicine |
References
- Mahase, E. Covid-19: WHO declares pandemic because of “alarming levels” of spread, severity, and inaction. Bmj 2020, 368, m1036. [Google Scholar] [CrossRef] [PubMed]
- Onafuwa, D. Suivi sur les Impacts de la COVID-19 en Afrique de l’Ouest. 2021. [Google Scholar]
- Sow, A.; Gueye, M.; Boiro, b.; Ba, A.; Ba, I.D.; Faye, P.M.; Fall, A.L.; Ndiaye, O. Impact de la COVID-19 sur la vaccination de routine en milieu hospitalier au Sénégal. The Pan African Medical Journal 2020, 37. [Google Scholar] [CrossRef]
- Yin, Q.; Chen, A.; Song, X.; Deng, G.; Dong, W. Risk Perception and PTSD Symptoms of Medical Staff Combating Against COVID-19: A PLS Structural Equation Model. In Frontiers in Psychiatry; Frontiers, 2021. [Google Scholar] [CrossRef]
- Sarsina, P.R.d.; Iseppato, I. Traditional and non-conventional medicines: the socio-anthropological and bioethical paradigms for person-centred medicine, the Italian context. In The EPMA Journal; Springer, 2011; Volume 2, p. 439. [Google Scholar] [CrossRef]
- Dilhuydy, J.M. Les médecines complémentaires et alternatives en cancérologie: traitements inéprouvés ou pratiques inapprouvées. In Proceedings of the 27° Journées de la Société française de sénologie et de pathologie mammaire (SFSPM) Dogmes et doutes. Datebe SAS, Deauville, 2005; pp. 396–416. [Google Scholar]
- Abu, E.K.; Oloruntoba, R.; Osuagwu, U.L.; Bhattarai, D.; Miner, C.A.; Goson, P.C.; Langsi, R.; Nwaeze, O.; Chikasirimobi, T.G.; Ovenseri-Ogbomo, G.O.; et al. Risk perception of COVID-19 among sub-Sahara Africans: a web-based comparative survey of local and diaspora residents. BMC Public Health 2021, 21, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Dryhurst, S.; Schneider, C.R.; Kerr, J.; Freeman, A.L.; Recchia, G.; Van Der Bles, A.M.; Spiegelhalter, D.; Van Der Linden, S. Risk perceptions of COVID-19 around the world. Journal of risk research 2020, 23, 994–1006. [Google Scholar] [CrossRef]
- Savadori, L.; Lauriola, M. Risk perception and protective behaviors during the rise of the COVID-19 outbreak in Italy. Frontiers in psychology 2021, 3822. [Google Scholar] [CrossRef]
- Attema, A.; L’Haridon, O.; Raude, J.; Seror, V.; Group, C.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Alleaume, C.; Fressard, L.; Beck, F.; Legleye, S.; L’Haridon, O.; Ward, J.; et al.; Peretti-Watel Beliefs and risk perceptions about COVID-19: Evidence from two successive French representative surveys during lockdown. Frontiers in Psychology 2021, 12. [Google Scholar] [CrossRef] [PubMed]
- Prati, G.; Pietrantoni, L. Knowledge, risk perceptions, and xenophobic attitudes: Evidence from Italy during the Ebola outbreak. Risk Analysis 2016, 36, 2000–2010. [Google Scholar] [CrossRef]
- Leiserowitz, A. Climate Change Risk Perception and Policy Preferences: The Role of Affect, Imagery, and Values. Climatic Change 2006, 77, 45–72. [Google Scholar] [CrossRef]
- Loungou, S.; Bignoumba, G.S.; Ropivia, M.L. L’Afrique à l’épreuve de la pandémie de COVID-19.. Représentations, incidences et réponses. In L’Espace Politique. Revue en ligne de géographie politique et de géopolitique; 2022. [Google Scholar]
- Mariam, M.D.; Djeneba, O.N.; Mireille, D.; Koumavi, E. La mesure de l’usage de la médecine traditionnelle en Afrique de l’Ouest. Revue Bio-Africa 2018, 18, 42–56. [Google Scholar]
- Foucault, M.; Bono, P.H.; Savoye, B. Perceptions des premiers mois de la crise de la COVID-19 dans six pays d’Afrique. Papiers de recherche 2022, 1–64. [Google Scholar]
- Dryhurst, S.; Schneider, C.R.; Kerr, J.; Freeman, A.L.J.; Recchia, G.; van der Bles, A.M.; Spiegelhalter, D.; van der Linden, S. Risk perceptions of COVID-19 around the world. In Journal of Risk Research; Routledge _eprint, 2020; Volume 23, pp. 994–1006. [Google Scholar] [CrossRef]
- Strotz, R.H.; Wold, H.O. Recursive vs. nonrecursive systems: An attempt at synthesis (part i of a triptych on causal chain systems). In Econometrica: Journal of the Econometric Society; JSTOR: Publisher, 1960; pp. 417–427. [Google Scholar]
- Wold, H. Soft modelling: the basic design and some extensions. Systems under indirect observation, Part II 1982, 36–37. [Google Scholar]
- Hair, J.F., Jr.; Hult, G.T.M.; Ringle, C.M.; Sarstedt, M. A primer on partial least squares structural equation modeling (PLS-SEM); Sage publications, 2014; pp. 95–203. [Google Scholar]
- Hair, J.F., Jr.; Hult, G.T.M.; Ringle, C.M.; Sarstedt, M.; Danks, N.P.; Ray, S. Partial least squares structural equation modeling (PLS-SEM) using R: A workbook; Springer Nature, 2021. [Google Scholar]
- Garson, G.D. Partial Least Squares: Regression & Structural Equation Models; 2016. [Google Scholar]
- Dijkstra, T.K.; Henseler, J. Consistent and asymptotically normal PLS estimators for linear structural equations. Computational Statistics & Data Analysis 2015, 81, 10–23. [Google Scholar] [CrossRef]
- Ferrer, R.A.; Klein, W.M.; Avishai, A.; Jones, K.; Villegas, M.; Sheeran, P. When does risk perception predict protection motivation for health threats? A person-by-situation analysis. PloS one 2018, 13, e0191994. [Google Scholar] [CrossRef]
- Kaufman, A.R.; Twesten, J.E.; Suls, J.; McCaul, K.D.; Ostroff, J.S.; Ferrer, R.A.; Brewer, N.T.; Cameron, L.D.; Halpern-Felsher, B.; Hay, J.L.; et al. Measuring cigarette smoking risk perceptions. Nicotine and Tobacco Research 2020, 22, 1937–1945. [Google Scholar] [CrossRef] [PubMed]
- Peters, E.; Hart, P.S.; Fraenkel, L. Informing patients: the influence of numeracy, framing, and format of side effect information on risk perceptions. Medical Decision Making 2011, 31, 432–436. [Google Scholar] [CrossRef]
- Dohmen, T.; Falk, A.; Huffman, D.; Sunde, U.; Schupp, J.; Wagner, G.G. Individual risk attitudes: Measurement, determinants, and behavioral consequences. Journal of the european economic association 2011, 9, 522–550. [Google Scholar] [CrossRef]
- Dillard, A.J.; Ferrer, R.A.; Ubel, P.A.; Fagerlin, A. Risk perception measures’ associations with behavior intentions, affect, and cognition following colon cancer screening messages. Health psychology 2012, 31, 106. [Google Scholar] [CrossRef]
- Van der Linden, S. The social-psychological determinants of climate change risk perceptions: Towards a comprehensive model. Journal of Environmental Psychology 2015, 41, 112–124. [Google Scholar] [CrossRef]
- Hadjichristidis, C.; Geipel, J.; Savadori, L. The effect of foreign language in judgments of risk and benefit: The role of affect. Journal of Experimental Psychology: Applied 2015, 21, 117. [Google Scholar] [CrossRef]
- Moyo, N.; Bhappu, A.D.; Bhebhe, M.; Ncube, F. Perceived risk of COVID-19 and employee decision-making: How psychological distress during the pandemic increases negative performance outcomes among healthcare workers. International Journal of Environmental Research and Public Health 2022, 19, 6762. [Google Scholar] [CrossRef]
- Shmueli, G.; Ray, S.; Velasquez Estrada, J.M.; Chatla, S.B. The elephant in the room: Predictive performance of PLS models. Journal of Business Research 2016, 69, 4552–4564. [Google Scholar] [CrossRef]
- Shmueli, G.; Sarstedt, M.; Hair, J.F.; Cheah, J.H.; Ting, H.; Vaithilingam, S.; Ringle, C.M. Predictive model assessment in PLS-SEM: guidelines for using PLSpredict. European journal of marketing 2019, 53, 2322–2347. [Google Scholar] [CrossRef]
- Fornell, C.; Larcker, D.F. Evaluating Structural Equation Models with Unobservable Variables and Measurement Error. In Journal of Marketing Research; SAGE Publications Inc, 1981; Volume 18, pp. 39–50. [Google Scholar] [CrossRef]
- Malhotra, N.K.; Décaudin, J.M.; Shahidi, N.; Macé, S. Etudes marketing avec SPSS; Pearson Education, 2007. [Google Scholar]
- Tenenhaus, M.; Vinzi, V.E.; Chatelin, Y.M.; Lauro, C. PLS path modeling. Computational statistics & data analysis 2005, 48, 159–205. [Google Scholar]
- Voorhees, C.M.; Brady, M.K.; Calantone, R.; Ramirez, E. Discriminant validity testing in marketing: an analysis, causes for concern, and proposed remedies. Journal of the academy of marketing science 2016, 44, 119–134. [Google Scholar] [CrossRef]
- Marsh, H.W.; Hau, K.T. Assessing Goodness of Fit: Is Parsimony Always Desirable? In The Journal of Experimental Education; Routledge _eprint, 1996; Volume 64, pp. 364–390. [Google Scholar] [CrossRef]
- Fong, P.; Chen, L. Governance of learning mechanisms: Evidence from construction firms. Journal of Construction Engineering and Management 2012, 138, 1053–1064. [Google Scholar] [CrossRef]
- Gerhold, L. COVID-19: Risk perception and Coping strategies. 2020. [Google Scholar] [CrossRef]
- Bounlu, M. Itinéraires thérapeutiques des personnes vivant avec une épilepsie en RDP Lao. PhD thesis, Limoges, 2018. [Google Scholar]
- Dash, G.; Paul, J. CB-SEM vs PLS-SEM methods for research in social sciences and technology forecasting. Technological Forecasting and Social Change 2021, 173, 121092. [Google Scholar] [CrossRef]
- Yıldız, O. PLS-SEM bias: traditional vs consistent. In Quality & Quantity; 2022. [Google Scholar] [CrossRef]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).