Submitted:
06 March 2026
Posted:
09 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
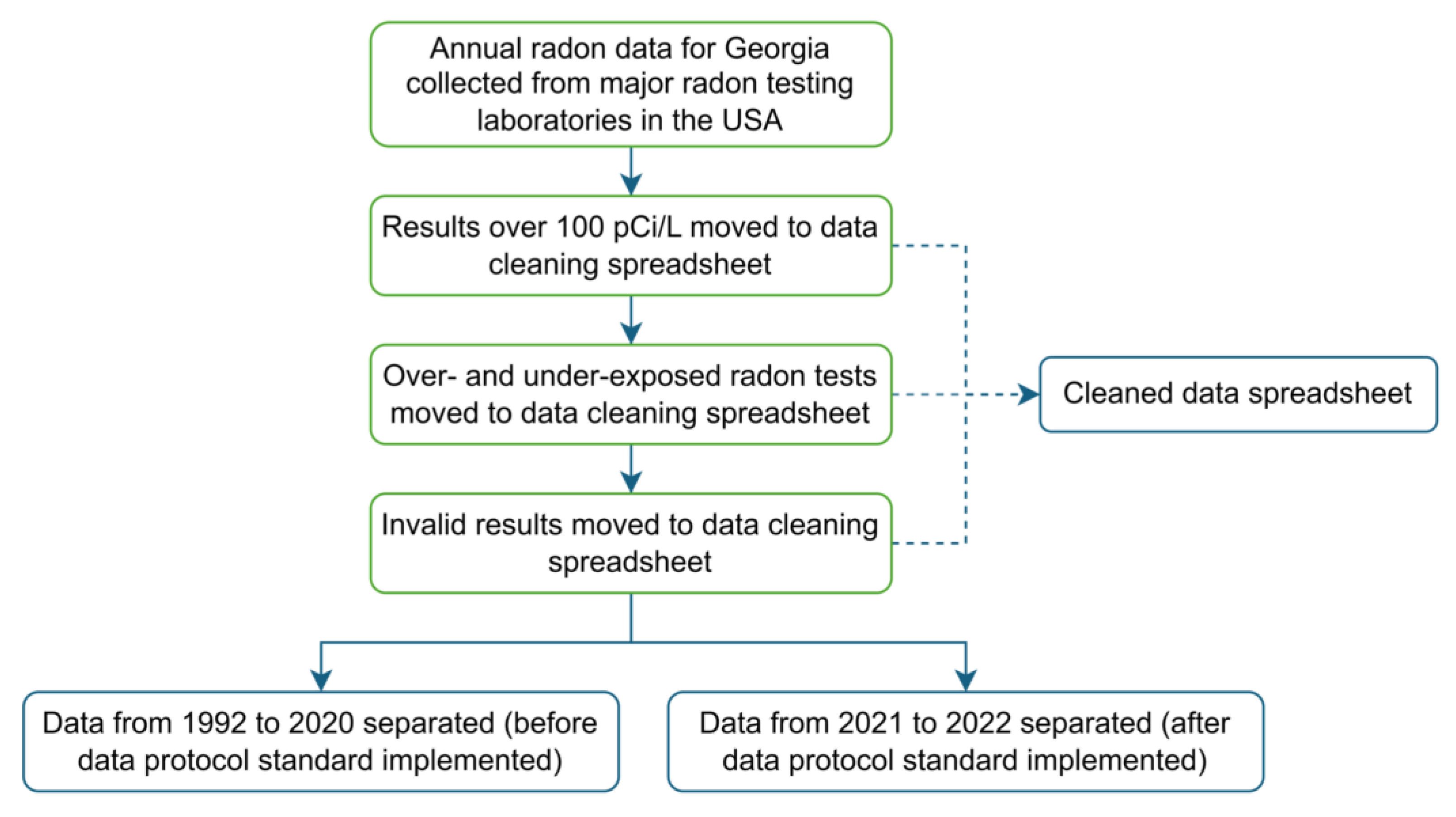
2.1. Indoor Air Radon Test Data
2.2. Socio-Economic and Public Health Data Collection
- Demographic, housing and occupancy characteristics, home value, income and poverty data were downloaded from the US Census Bureau in tabular forms (available online at: https://data.census.gov/table). These data were available for the year 2000, and for each year from 2010 to 2022.
- Literacy, numeracy, different tires of institutional education, employment status, type of occupations, poverty data were downloaded from the website of the Program for the International Assessment of Adulty Competencies (PIAAC) under National Center for Education Statistics under the US government (https://nces.ed.gov/surveys/piaac/state-county-estimates.asp). Most of these data were available for the years 2013 to 2017.
- Data for various public health variables were downloaded from County Health Rankings & Roadmaps (CHR&R) website, University of Wisconsin Population Health Institute (https://www.countyhealthrankings.org/). These data were available for each year from 2011 to 2022.
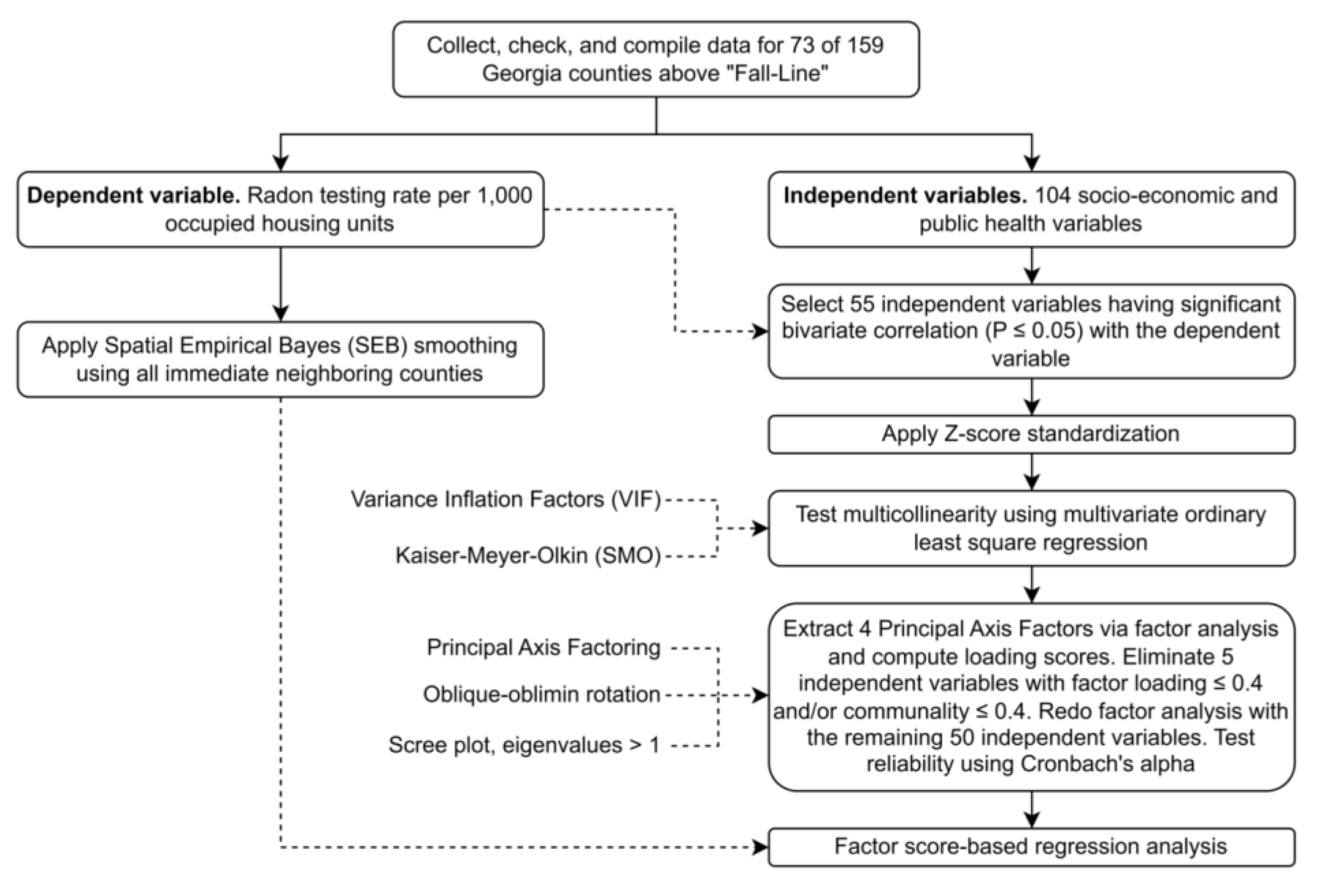
2.3. Data Analysis
3. Results
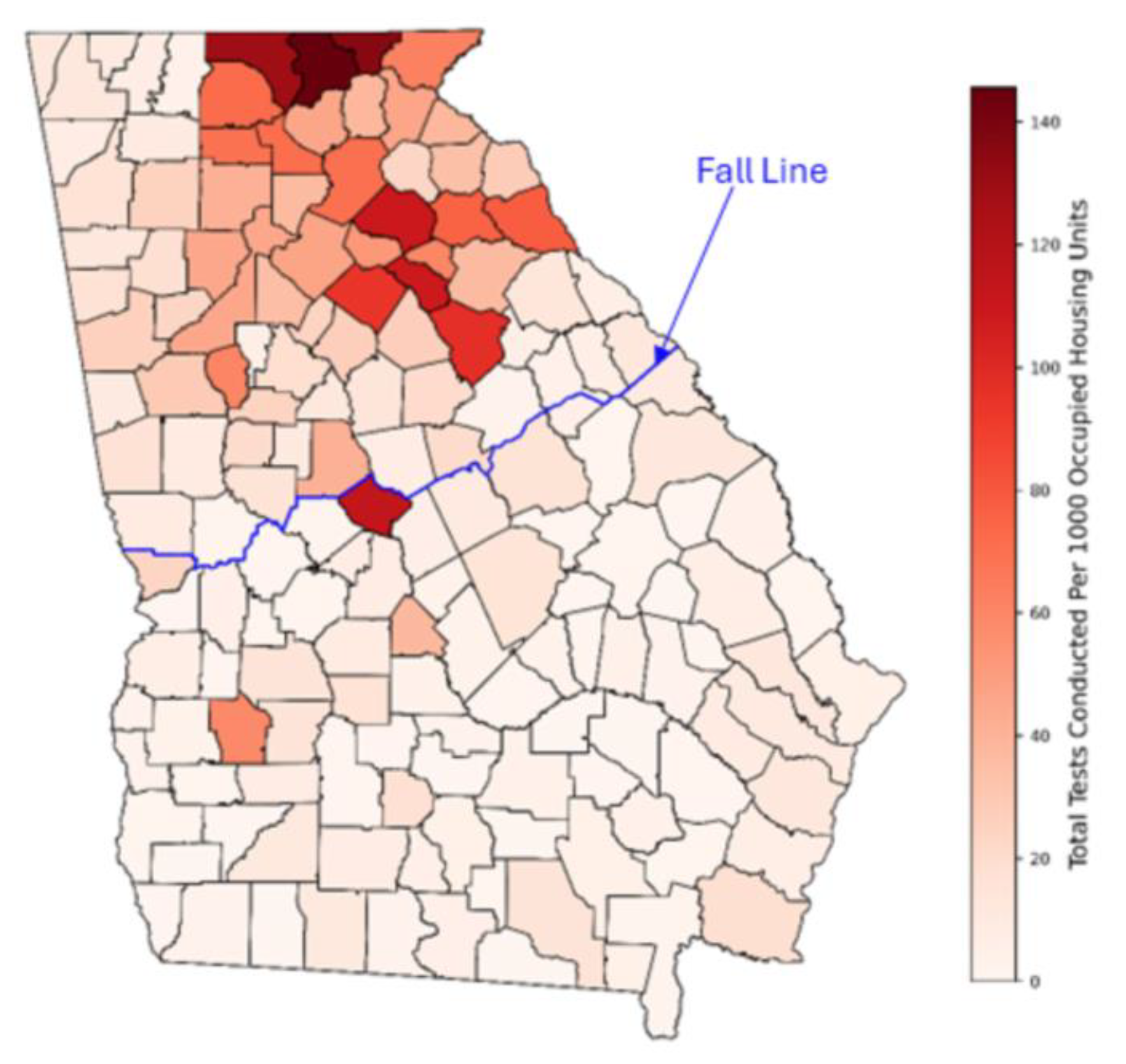
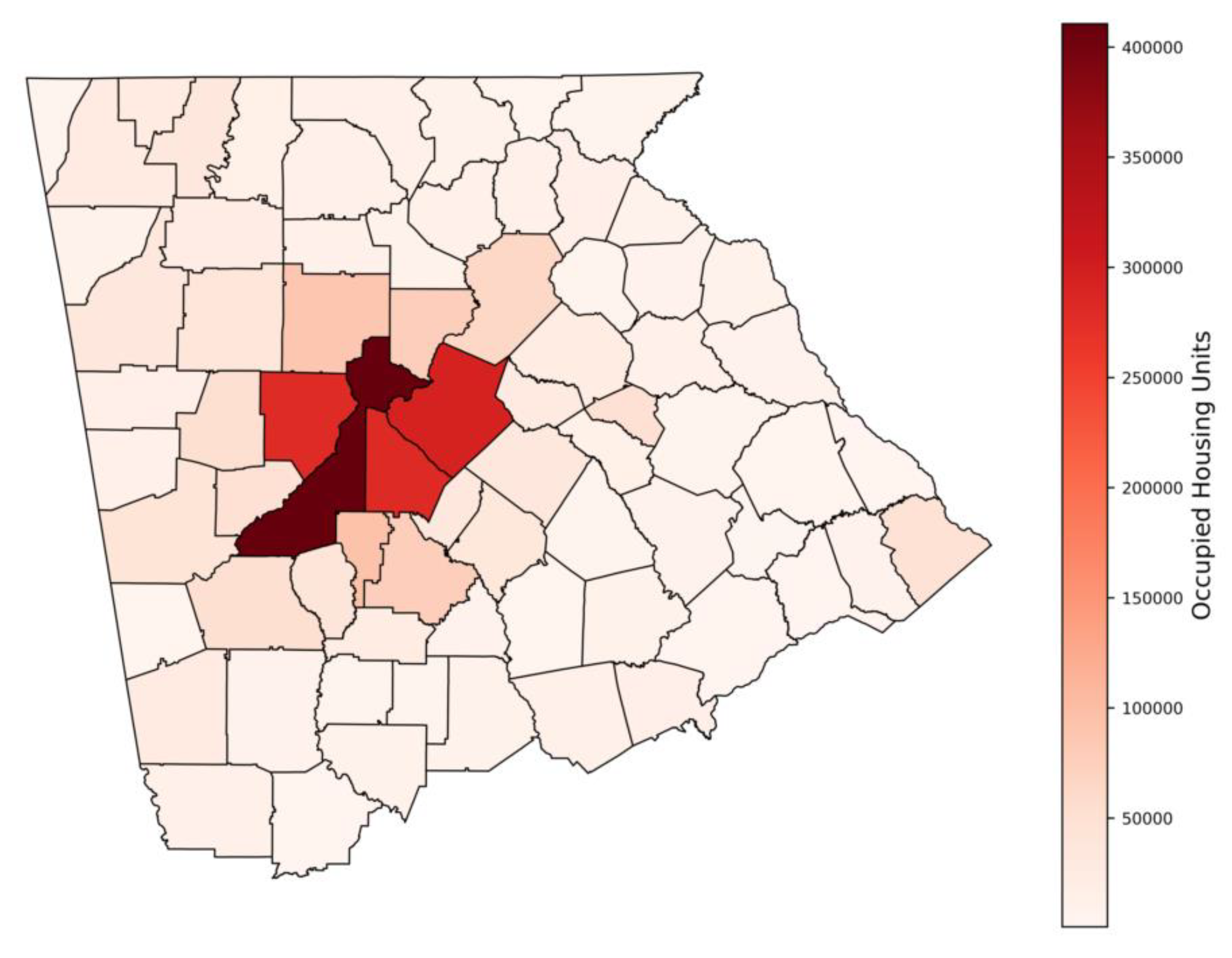
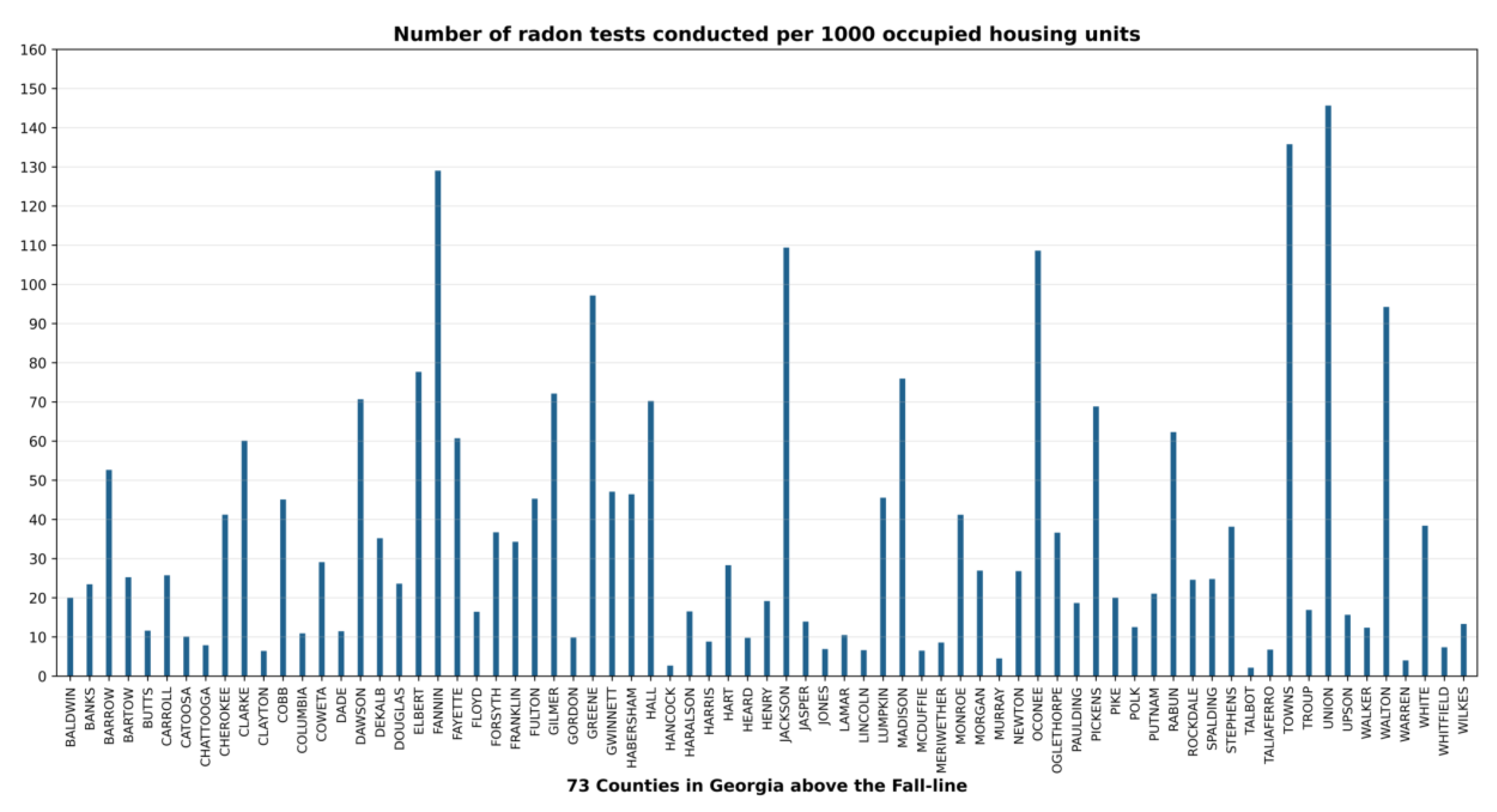
3.1. Number and Rates of Radon Tests
3.2. Bivariate Correlation of the 104 Independent Variables with the Radon Testing Rates
3.3. Correlation Matrix Among the 55 Independent Variables
3.4. Multivariate Least Square Regression Analysis of Radon Testing Rates (Independent) Versus 55 Independent Variables
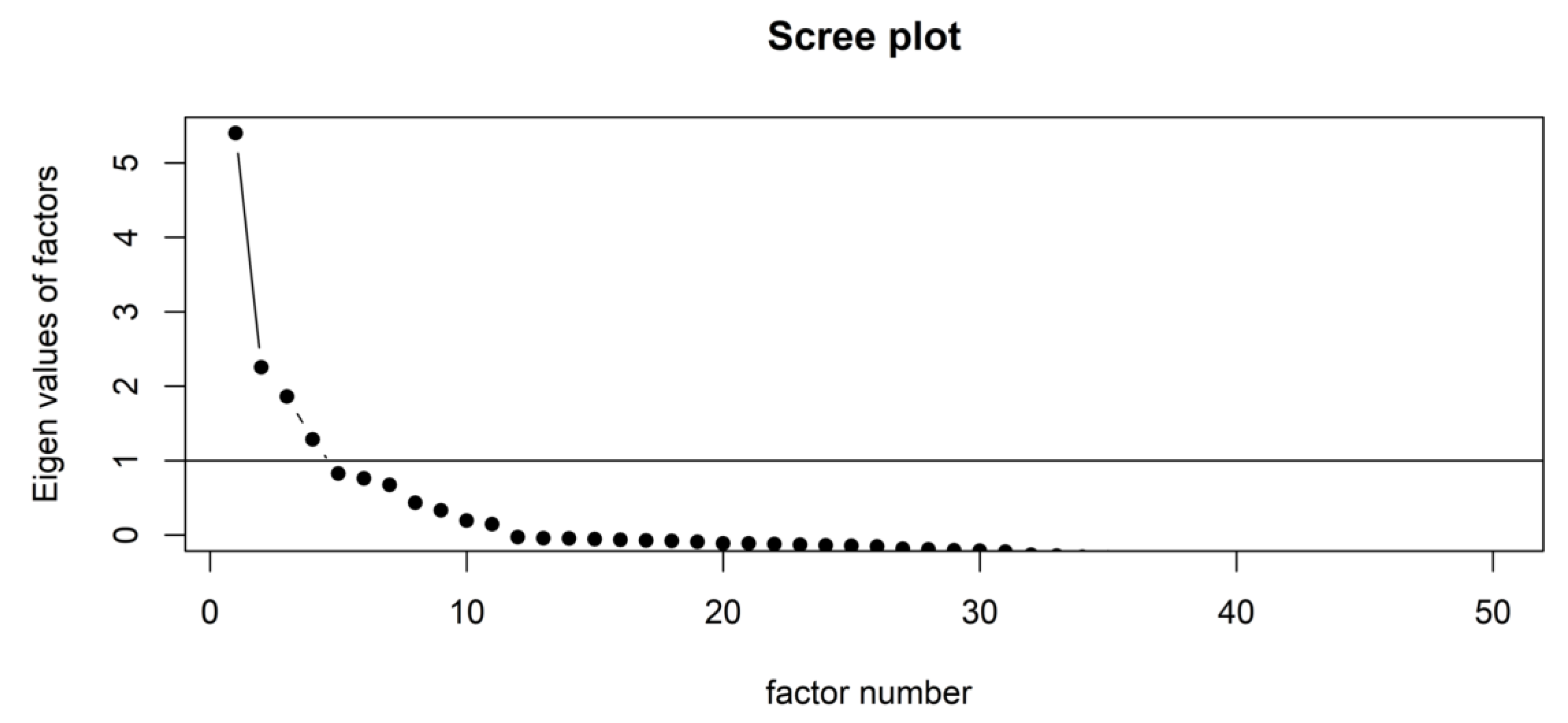
3.5. Factor Analysis and Factor Score-Based Regression Analysis
4. Discussion
5. Conclusion
Author Contributions
Funding
Data Availability Statement
Acknowledgments
References
- USEPA (U.S. Environmental Protection Agency). Health Risk of Radon. 2025a. Available online: https://www.epa.gov/radon/health-risk-radon.
- WHO (World Health Organization). WHO Handbook on Indoor Radon: A Public Health Perspective. 2009. Available online: https://www.who.int/publications/i/item/9789241547673.
- Saha, U; Cooper, D; Turner, PR; Cantrell, RA; Singh, K. An analysis of the impact of geology on indoor air radon concentration. Indoor Environments 2025, 2(4), 100143. [Google Scholar] [CrossRef]
- USEPA (U.S. Environmental Protection Agency). EPA Maps of Radon Zones and Supporting Documents by State. EPA. 2025b. Available online: https://www.epa.gov/radon/epa-maps-radon-zones-and-supporting-documents-state.
- USEPA (U.S. Environmental Protection Agency). EPA assessment of risks from radon in homes. In Office of Air and Radiation, USEPA; Washington, DC, 2003. [Google Scholar]
- King, BA; Dube, SR; Homa, DM. Exposure to secondhand smoke and radon: A national survey of U.S. homes. American Journal of Preventive Medicine 2012, 42(2), 148–154. [Google Scholar]
- Duckworth, LT; Frank-Stromborg, M; Oleckno, WA. Relationship of perception of radon as a health risk and willingness to engage in radon testing and mitigation. Oncology Nursing Forum 2002, 29(7), 1099–1107. [Google Scholar] [CrossRef] [PubMed]
- Ou, JY; Ramsay, JM; Smith, J; Akerley, W; Martel, L; Harding, G.; Divver, H; Kirchhoff, AC; Kepka, D. Public awareness and perceptions surrounding radon testing in a state with high radon emission potential and low smoking rates. J. Environ. Health 2019, 82, 8–17. Available online: https://www.jstor.org/stable/26800398.
- Dai, D. Neighborhood characteristics of low radon testing activities: A longitudinal study in Atlanta, Georgia, United States. Science of The Total Environment 2022, 834, 155290. [Google Scholar] [CrossRef]
- American National Standards Institute/American Association of Radon Scientistsand Technologists (ANSI/AARST). Protocol for Conducting Measurements ofRadon and Radon Decay Products in Homes. MAH-2023. AARST Consortium onNational Standards: Hendersonville, NC, 2023. [Google Scholar]
- Dai, D; Neal, FB; Diem, J; Deocampo, DM; Stauber, C; Dignam, T. Confluentimpact of housing and geology on indoor radon concentrations in Atlanta, Georgia,United States. Sci. Total Environ. 2019, 668, 500–511. [Google Scholar] [CrossRef] [PubMed]
- Anselin, L. Spatial Econometrics: Methods and Models; Kulwer Academic: Dordrecht, the Netherlands, 1988. [Google Scholar]
- Anselin, L; Syabri, I; Kho, Y. GeoDa: an introduction to spatial data analysis. Geogr. Anal. 2006, 38, 5–22. [Google Scholar] [CrossRef]
- Cressie, N. Smoothing regional maps using empirical Bayes predictors. Geogr. Anal. 1992, 24, 75–95. [Google Scholar] [CrossRef]
- Sharma, S. Applied Multivariate Techniques; John Wiley & Sons, Inc: New York, 1996; p. 493p. [Google Scholar]
- Acevedo-Garcia, D. Residential segregation and the epidemiology of infectious diseases. Soc. Sci. Med. 2000, 51, 1143–1161. [Google Scholar] [CrossRef]
- Kershaw, KN; Pender, AE. Racial/ethnic residential segregation, obesity, and diabetes mellitus. Curr. Diabetes Rep. 2016, 16, 11. [Google Scholar] [CrossRef]
- Landrine, H; Corral, I; Lee, JGL; Efird, JT; Hall, MB; Bess, JJ. Residential segregation and racial cancer disparities: a systematic review. J. Racial Ethn. Health Disparities 2017, 4, 1195–1205. [Google Scholar] [CrossRef]
- Darden, JT; Rahbar, M; Jezierski, L; Li, M; Velie, E. The measurement of neighborhood socioeconomic characteristics and black and white residential segregation in metropolitan Detroit: implications for the study of social disparities in health. Ann. Assoc. Am. Geogr. 2010, 100, 137–158. [Google Scholar] [CrossRef]
- White, K.; Borrell, L.N. Racial/ethnic residential segregation: framing the context of health risk and health disparities. Health Place 2011, 17, 438–448. [Google Scholar] [CrossRef]
- Lutfi, K; Trepka, MJ; Fennie, KP; Ibanez, G; Gladwin, H. Racial residential segregation and risky sexual behavior among non-Hispanic blacks, 2006–2010. Soc. Sci. Med. 2015, 140, 95–103. [Google Scholar] [CrossRef] [PubMed]
- Thorpe, RJ; Kennedy-Hendricks, A; Griffith, DM; Bruce, MA; Coa, K; Bell, CN; Young, J; Bowie, JV; LaVeist, T A. Race, social and environmental conditions, and health behaviors in men. Fam. Community Health 2015, 38(4), 297–306. [Google Scholar] [CrossRef]
- Kitto, ME; Green, JG. Mapping the indoor radon potential in New York at the township level. Atmos. Environ. 2008, 42, 8007–8014. [Google Scholar] [CrossRef]
- Kropat, G; Bochud, F; Jaboyedoff, M; Laedermann, JP; Murith, C; Palacios, M.; Baechler, S. Major influencing factors of indoor radon concentrations in Switzerland. J. Environ. Radioact. 2014, 129, 7–22. [Google Scholar] [CrossRef]
- Zahnd, WE; Mueller-Luckey, GS; Ratnapradipa, K; Smith, T. Predictors and spatial variation of radon testing in Illinois, 2005–2012. J. Public Health Manag. Pract. 2018, 24, E1–E9. [Google Scholar] [CrossRef]
- Baldwin, G; Frank, E; Fielding, B. US women physicians' residential radon testing practices. Am. J. Prev. Med. 1998, 15, 49–53. [Google Scholar] [CrossRef] [PubMed]
- Hevey, D. Radon risk and remediation: a psychological perspective. Front. Public Health 2017, 5, 63. [Google Scholar] [CrossRef]
- Lantz, PM; Mendez, D; Philbert, MA. Radon, smoking, and lung cancer: the need to refocus radon control policy. Am. J. Public Health 2013, 103, 443–447. [Google Scholar] [CrossRef] [PubMed]
- Stauber, CE; Dai, DJ; Chan, SR; Diem, JE; Weaver, SR; Rothenberg, R. A pilot study to examine exposure to residential radon in under-sampled census tracts of DeKalb County, Georgia, in 2015. Int. J. Environ. Res. Public Health 2017, 14(3), 332. [Google Scholar] [CrossRef] [PubMed]
- Davis, SF; Johnston, JD; Magnusson, BM; Novilla, MLB; Torgersen, BK; Schnell, AJ; Crandall, AA. Predictors of radon testing among Utah residents using a theory-based approach. J. Environ. Health 2018, 80(6), 20–27. Available online: https://www.jstor.org/stable/26329888.
| Correlation coefficient, r (absolute value) | Number of bivariate combinations | Significance of correlation coefficient, r |
|---|---|---|
| >0.281 | 35 | P ≤ 0.01, 71 (73-2) df |
| 0.230-0.281 | 20 | 0.01>P ≤ 0.05, 71 (73-2) df |
| <0.230 | 49 | P > 0.05, 71 (73-2) df |
| Total | 104 |
| Parameter # | Parameter Description | Correlation Coefficient, r | P-value at 71 (73-2) df |
|---|---|---|---|
| 1.0 Demographic & Neighborhood Characteristics | |||
| 19 | Population diversity index | -0.3072 | 0.0092 |
| 22 | Residential segregation index: between Black & White population | -0.4087 | 0.0003 |
| 23 | Median age of the population | 0.3573 | 0.0019 |
| 24 | % Population below 18 years of age | -0.3561 | 0.0020 |
| 25 | % Population 65 years and older | 0.4238 | 0.0002 |
| 29 | Urban population density (per sq. miles) | -0.2537 | 0.0303 |
| 2.0 Housing Characteristics | |||
| 37 | % Occupied housing units | 0.2328 | 0.0475 |
| 39 | %Owner-occupied housing units | 0.2645 | 0.0237 |
| 40 | Median home value ($) | 0.4996 | 0.0001 |
| 43 | %Housing units built 1970 or earlier (older homes) | -0.4205 | 0.0002 |
| 45 | %Housing Units built 1990 or later (newer homes) | 0.3882 | 0.0007 |
| 46 | Average household size of owner-occupied unit | -0.2338 | 0.0474 |
| 47 | Average household size of renter-occupied unit | -0.2461 | 0.0358 |
| 50 | %Single-family homes detached | 0.2559 | 0.0288 |
| 52 | %Single-family homes, total: detached + attached | 0.2645 | 0.0237 |
| 55 | % Units in mobile homes | -0.2360 | 0.0444 |
| 3.0 Population Literacy and Numeracy | |||
| 57 | Lit_P1 (proportion of population with literacy level P1 and below) | -0.4354 | 0.0001 |
| 58 | Lit_P2 (proportion of population with literacy level at P2) | -0.2890 | 0.0132 |
| 59 | Lit_P3 (proportion of population with literacy level P3 and above) | 0.4105 | 0.0003 |
| 60 | Proportion of population with literacy level P2+P3 combined | 0.4365 | 0.0001 |
| 61 | Lit_A (literacy average score indirect estimates) | 0.4085 | 0.0003 |
| 62 | Num_P1 (proportion of population with numeracy level P1 and below) | -0.4316 | 0.0001 |
| 64 | Num_P3 (proportion of population with numeracy level P3 and above) | 0.3981 | 0.0005 |
| 65 | Proportion of population with numeracy level P2+P3 Combined | 0.4335 | 0.0001 |
| 66 | Num_A (numeracy average score indirect estimates) | 0.4074 | 0.0003 |
| 67 | Less_HS (proportion of population with education less than high school) | -0.3665 | 0.0014 |
| 68 | HS (proportion of population with education high school) | -0.2904 | 0.0127 |
| 69 | More_HS (proportion of population with education more than high school) | 0.3581 | 0.0019 |
| 70 | % Having some college education | 0.2331 | 0.0471 |
| 72 | %Having bachelor’s degree in population 25 years and older | 0.2701 | 0.0208 |
| 4.0 Employment and Economy | |||
| 76 | Unemployment (proportion of population with age 16-64 who are unemployed) | -0.2378 | 0.0428 |
| 78 | Occupation: Management (proportion of population age 16 and over who are in the labor force in management, business, science, and arts occupations) | 0.3062 | 0.0084 |
| 79 | Median household income | 0.2546 | 0.0297 |
| 81 | Childcare cost burden (% household Income spent/required for childcare expenses) | -0.3929 | 0.0006 |
| 82 | % Children in poverty | -0.2541 | 0.0301 |
| 84 | Poverty_100 (proportion of population who are below 100 percent of the poverty level) | -0.2625 | 0.0249 |
| 85 | Poverty_150 (proportion of population who are below 150 percent of the poverty level) | -0.2898 | 0.0129 |
| 87 | SNAP (proportion of households who receive Food Stamps/SNAP in the past 12 months) | -0.3884 | 0.0007 |
| 5.0 Social Factors | |||
| 92 | Resilience: % population with 1-2 risk factor | 0.2479 | 0.0345 |
| 96 | % Children in single-parent households | -0.2722 | 0.0198 |
| 97 | Social association rate (#social associations per 10,000 population) | 0.2369 | 0.0436 |
| 6.0 Internet Access | |||
| 94 | %Households with a computer | 0.2311 | 0.0491 |
| 95 | % Households with broadband internet subscription/access | 0.3327 | 0.0040 |
| 7.0 Healthcare, Health, and Well-being | |||
| 100 | Primary Care Physicians (PCP) rate (#PCP per 100,000 population) | 0.3274 | 0.0047 |
| 101 | Primary Care Physicians (PCP) ratio (#people served by one PCP) | -0.3822 | 0.0008 |
| 103 | Life expectancy | 0.3918 | 0.0006 |
| 104 | Food environment index (indicator of access to healthy foods: 0 is the worst, 10 is the best) | 0.3276 | 0.0047 |
| 105 | % Adults with obesity | -0.4751 | 0.0001 |
| 106 | % Population physically inactive | -0.4604 | 0.0001 |
| 107 | % Population with excessive drinking | -0.3573 | 0.0019 |
| 108 | % Adults that reported currently smoking | -0.3453 | 0.0028 |
| 109 | % Adults that reported having fair or poor health | -0.4115 | 0.0003 |
| 110 | Average number of physically unhealthy days per month | -0.3528 | 0.0022 |
| 111 | Average number of mentally unhealthy days per month | -0.2351 | 0.0452 |
| 113 | Age-adjusted lung & bronchus cancer incidence rate cases per 100,000 people | -0.2495 | 0.0332 |
| Population diversity index | Residential Segregation Index† | Median age of the population | % Population below 18 years of age | % Population 65 years and older | Urban population density (per sq. miles) | % Occupied housing units | %Owner-occupied housing Units | Median home value ($) | %Housing units built 1970 or earlier | |
|---|---|---|---|---|---|---|---|---|---|---|
| Population diversity index | 1 | |||||||||
| Residential segregation index† | -0.131 | 1 | ||||||||
| Median age of the population | -0.482** | -0.041 | 1 | |||||||
| % Population below 18 years of age | 0.407** | 0.084 | -0.659** | 1 | ||||||
| % Population 65 years and older | -0.470** | -0.057 | 0.932** | -0.829** | 1 | |||||
| Urban population density (per sq. miles) | 0.540** | -0.099 | -0.628** | 0.392** | -0.593** | 1 | ||||
| % Occupied housing units | 0.365** | -0.041 | -0.729** | 0.729** | -0.810** | 0.450** | 1 | |||
| %Owner-occupied housing Units | -0.265* | -0.014 | 0.312** | 0.052 | 0.162 | -0.312** | -0.154 | 1 | ||
| Median home value ($) | 0.005 | -0.326** | -0.075 | 0.069 | -0.131 | 0.193 | 0.240* | 0.378** | 1 | |
| %Housing units built 1970 or earlier | 0.099 | 0.244* | 0.037 | -0.056 | 0.098 | 0.112 | -0.169 | -0.506** | -0.660** | 1 |
| Correlation coefficient, r (absolute value) | Number of bivariate combinations | Significance of correlation coefficient, r |
|---|---|---|
| >0.281 | 1015 | P ≤ 0.01, 71 (73-2) df |
| 0.230-0.281 | 76 | 0.01>P ≤ 0.05, 71 (73-2) df |
| <0.230 | 394 | P > 0.05, 71 (73-2) df |
|
Total |
1485 |
| Parameter Description | Coefficient | Standard Error | t-value | P>|t| | VIF† | |
|---|---|---|---|---|---|---|
| (Constant) | 32.20 | 2.80 | 11.523 | 0.000 | ||
| Population diversity index | 25.79 | 41.09 | 0.628 | 0.553 | 216.2 | |
| Residential segregation index: between Black & White population | -2.94 | 4.18 | -0.704 | 0.508 | Infinity | |
| Median age of the population | -79.38 | 43.44 | -1.827 | 0.117 | 241.61 | |
| % Population below 18 years of age | 8.70 | 27.00 | 0.322 | 0.758 | 93.35 | |
| % Population 65 years and older | 52.78 | 43.19 | 1.222 | 0.267 | 238.85 | |
| Urban population density (per sq. miles) | 5.14 | 20.73 | 0.248 | 0.812 | 55.02 | |
| % Occupied housing units | -12.81 | 21.16 | -0.605 | 0.567 | 57.34 | |
| %Owner-occupied housing units | -18.29 | 44.96 | -0.407 | 0.698 | 258.88 | |
| Median home value ($) | 56.27 | 27.93 | 2.015 | 0.091 | 99.91 | |
| %Housing units built 1970 or earlier (older homes) | -46.92 | 37.84 | -1.240 | 0.261 | 183.37 | |
| %Housing Units built 1990 or later (newer homes) | -39.59 | 28.68 | -1.381 | 0.217 | 105.3 | |
| Average household size of owner-occupied unit | -20.43 | 16.58 | -1.232 | 0.264 | 35.22 | |
| Average household size of renter-occupied unit | 0.25 | 16.70 | 0.015 | 0.989 | 35.73 | |
| %Single-family homes detached | 0.09 | 168.74 | 0.001 | 1 | 3645.96 | |
| %Single-family homes, total: detached + attached | 87.16 | 149.00 | 0.585 | 0.58 | 2842.87 | |
| % Units in mobile homes | 56.94 | 51.11 | 1.114 | 0.308 | 334.49 | |
| Lit_P1 (proportion of population with literacy level P1 and below) | -559.58 | 1724.10 | -0.325 | 0.757 | 380627.4 | |
| Lit_P2 (proportion of population with literacy level at P2) | -523.25 | 383.96 | -1.363 | 0.222 | Infinity | |
| Lit_P3 (proportion of population with literacy level P3 and above) | 578.58 | 1193.92 | 0.485 | 0.645 | Infinity | |
| Proportion of population with literacy level P2+P3 combined | 528.18 | 1946.45 | 0.271 | 0.795 | Infinity | |
| Lit_A (literacy average score indirect estimates) | -125.48 | 511.39 | -0.245 | 0.814 | 33487 | |
| Num_P1 (proportion of population with numeracy level P1 and below) | 517.85 | 1738.56 | 0.298 | 0.776 | 387039.2 | |
| Num_P3 (proportion of population with numeracy level P3 and above) | -934.98 | 573.56 | -1.630 | 0.154 | 42124.48 | |
| Proportion of population with numeracy level P2+P3 Combined | -421.19 | 2054.09 | -0.205 | 0.844 | 540274.3 | |
| Num_A (numeracy average score indirect estimates) | 221.73 | 824.40 | 0.269 | 0.797 | 87026.01 | |
| Less_HS (proportion of population with education less than high school) | 727.57 | 1258.44 | 0.578 | 0.584 | 202785.8 | |
| HS (proportion of population with education high school) | 575.85 | 1262.06 | 0.456 | 0.664 | 203956.1 | |
| More_HS (proportion of population with education more than high school) | 720.83 | 1896.37 | 0.380 | 0.717 | 460487.4 | |
| % Having some college education | 16.63 | 39.38 | 0.422 | 0.687 | 198.59 | |
| %Having bachelor’s degree in population 25 years and older | 5.10 | 33.38 | 0.153 | 0.884 | 142.68 | |
| Unemployment (proportion of population with age 16-64 who are unemployed) | 4.60 | 8.63 | 0.533 | 0.613 | 9.54 | |
| Occupation: Management (proportion of population age 16 and over who are in the labor force in management, business, science, and arts occupations) | -38.27 | 32.17 | -1.190 | 0.279 | 132.5 | |
| Median household income | -19.64 | 36.12 | -0.544 | 0.606 | 167.08 | |
| Childcare cost burden (% household Income spent/required for childcare expenses) | -2.01 | 23.31 | -0.086 | 0.934 | 69.56 | |
| % Children in poverty | 8.18 | 27.99 | 0.292 | 0.78 | 100.28 | |
| Poverty_100 (proportion of population who are below 100 percent of the poverty level) | -57.86 | 81.43 | -0.711 | 0.504 | 849.12 | |
| Poverty_150 (proportion of population who are below 150 percent of the poverty level) | -25.49 | 33.41 | -0.763 | 0.474 | 142.93 | |
| SNAP (proportion of households who receive Food Stamps/SNAP in the past 12 months) | -39.42 | 37.76 | -1.044 | 0.337 | 182.61 | |
| Resilience: % population with 1-2 risk factor | -12.16 | 14.33 | -0.849 | 0.429 | 26.3 | |
| % Children in single-parent households | -4.04 | 28.74 | -0.141 | 0.893 | 105.76 | |
| Social association rate (#social associations per 10,000 population) | 7.48 | 11.84 | 0.632 | 0.551 | 17.94 | |
| %Households with a computer | -48.30 | 34.87 | -1.385 | 0.215 | 155.69 | |
| % Households with broadband internet subscription/access | 20.13 | 26.44 | 0.761 | 0.475 | 89.48 | |
| Primary Care Physicians (PCP) rate (#PCP per 100,000 population) | 14.17 | 21.78 | 0.650 | 0.539 | 60.75 | |
| Primary Care Physicians (PCP) ratio (#people served by one PCP) | -4.60 | 18.39 | -0.250 | 0.811 | 43.32 | |
| Life expectancy | -38.43 | 26.95 | -1.426 | 0.204 | 93 | |
| Food environment index (indicator of access to healthy foods: 0 is the worst, 10 is the best) | -25.28 | 19.40 | -1.303 | 0.24 | 48.21 | |
| % Adults with obesity | -10.52 | 16.43 | -0.640 | 0.546 | 34.57 | |
| % Population physically inactive | -44.76 | 40.75 | -1.098 | 0.314 | 212.62 | |
| % Population with excessive drinking | 1.40 | 19.20 | 0.073 | 0.944 | 47.22 | |
| % Adults that reported currently smoking | -34.77 | 55.34 | -0.628 | 0.553 | 392.11 | |
| % Adults that reported having fair or poor health | 53.49 | 70.09 | 0.763 | 0.474 | 629.01 | |
| Average number of physically unhealthy days per month | -50.99 | 52.81 | -0.966 | 0.372 | 357.14 | |
| Average number of mentally unhealthy days per month | 22.04 | 20.16 | 1.093 | 0.316 | 52.02 | |
| Age-adjusted lung & bronchus cancer incidence rate cases per 100,000 people | 20.90 | 14.98 | 1.395 | 0.212 | 28.73 | |
| Notes:. | ||||||
| Jarque-Bera (JB) statistic | 0.93 | |||||
| Probability (JB Statistic): | 0.628 | |||||
| R-squared: | 0.945 | |||||
| Adjusted R-squared: | 0.444 | |||||
| F-statistic: | 1.885 | |||||
| Probability (F-statistic): | 0.217 | |||||
| Omnibus Statistic | 1.657 | |||||
| Probability (Omnibus): | 0.437 | |||||
| Durbin-Watson: | 2.111 | |||||
| The smallest eigenvalue | 1.26 × 10⁻²⁹ | |||||
| Kaiser–Meyer–Olkin (KMO) statistic | 0.86 | |||||
| Variable Description | Variable Label | PAF†-1 | PAF-2 | PAF-3 | PAF-4 | Communality |
|---|---|---|---|---|---|---|
| Median home value ($) | Housing Characteristics | 0.923 | 0.049 | -0.141 | 0.192 | 0.894 |
| %Housing units built 1970 or earlier (older homes) | -0.663 | 0.039 | -0.198 | -0.416 | 0.643 | |
| %Housing units built 1990 or later (newer homes) | 0.646 | -0.032 | 0.255 | 0.404 | 0.634 | |
| %single-family homes, total: detached + attached) | 0.650 | 0.147 | 0.535 | 0.386 | 0.782 | |
| % Units in mobile homes | -0.735 | -0.520 | -0.135 | -0.032 | 0.689 | |
| Lit_P1 (literacy Level P1 and below) | Population Literacy and Numeracy | -0.939 | 0.138 | -0.034 | -0.005 | 0.937 |
| Lit_P2 (literacy Level at P2) | -0.880 | -0.398 | 0.114 | 0.008 | 0.884 | |
| Lit_P3 (literacy Level P3 and above) | 0.971 | 0.089 | -0.035 | -0.001 | 0.984 | |
| Literacy level P2+P3 combined | 0.939 | -0.139 | 0.032 | 0.005 | 0.937 | |
| Lit_A (literacy average score indirect estimates) | 0.990 | 0.001 | 0.020 | -0.028 | 0.982 | |
| Num_P1 (numeracy Level P1 and below) | -0.951 | 0.145 | -0.100 | 0.038 | 0.983 | |
| Num_P3 (numeracy Level P3 and above) | 0.990 | 0.091 | -0.032 | -0.021 | 0.971 | |
| Numeracy level P2+P3 combined | 0.952 | -0.150 | 0.099 | -0.027 | 0.985 | |
| Num_A (numeracy average score indirect estimates) | 0.976 | -0.060 | 0.077 | -0.053 | 0.986 | |
| Less_HS (education less than high school) | Institutional Education Attainment | -0.850 | -0.133 | 0.140 | -0.171 | 0.764 |
| HS (education high school) | -0.859 | -0.410 | 0.170 | 0.003 | 0.887 | |
| More_HS (education more than High School) | 0.946 | 0.313 | -0.183 | 0.091 | 0.988 | |
| % Having some college education | 0.878 | 0.321 | -0.034 | 0.034 | 0.808 | |
| %Having bachelor’s degree in population 25 years and older | 0.856 | 0.414 | -0.197 | 0.142 | 0.914 | |
| Occupation: Management (proportion of population age 16 and over who are in the labor force in management, business, science, and arts occupations) | Type of Employment | 0.858 | 0.305 | -0.174 | 0.069 | 0.826 |
| Median household income | Employment, Economy, and Poverty | 0.893 | 0.286 | 0.239 | 0.259 | 0.878 |
| Childcare cost burden (% household Income spent/required for child care expenses) | -0.473 | 0.462 | -0.150 | -0.040 | 0.556 | |
| % Children in poverty | -0.891 | -0.099 | -0.408 | -0.047 | 0.920 | |
| Poverty_100 (proportion of population who are below 100 percent of the poverty level) | -0.823 | 0.025 | -0.328 | -0.209 | 0.824 | |
| Poverty_150 (proportion of population who are below 150 percent of the poverty level) | -0.887 | -0.017 | -0.247 | -0.210 | 0.870 | |
| SNAP (proportion of households who receive Food Stamps/SNAP in the past 12 months) | -0.874 | 0.008 | -0.008 | -0.228 | 0.804 | |
| %Households with a computer | Access to Computer and Internet | 0.840 | 0.349 | 0.275 | -0.099 | 0.787 |
| % Households with broadband internet subscription/access | 0.849 | 0.282 | 0.236 | -0.110 | 0.772 | |
| Primary Care Physicians (PCP) rate (#PCP per 100,000 population) | Access to Healthcare, Health & Well-being, and Lifestyle | 0.484 | 0.244 | -0.333 | -0.034 | 0.425 |
| Life expectancy | 0.857 | 0.186 | -0.142 | 0.311 | 0.845 | |
| Food Environment Index (indicator of access to healthy foods: 0 is the worst, 10 is the best) | 0.717 | -0.143 | 0.109 | 0.101 | 0.586 | |
| % Adults with obesity | -0.798 | 0.185 | 0.054 | 0.146 | 0.736 | |
| %Population physically inactive | -0.975 | 0.012 | 0.021 | -0.014 | 0.954 | |
| % Population with excessive drinking | 0.548 | -0.510 | -0.009 | -0.337 | 0.752 | |
| % Adults that reported currently smoking | -0.944 | -0.336 | 0.060 | -0.180 | 0.959 | |
| % Adults that reported having fair or poor health | -0.981 | 0.035 | -0.063 | -0.007 | 0.976 | |
| Average number of physically unhealthy days per month | -0.968 | -0.189 | -0.016 | -0.161 | 0.940 | |
| Average number of mentally unhealthy days per month | -0.770 | -0.412 | 0.027 | -0.304 | 0.764 | |
| Age-adjusted lung & bronchus cancer incidence rate cases per 100,000 people | -0.571 | -0.340 | 0.343 | -0.456 | 0.774 | |
| % Children in single-parent households | Social Factors | -0.680 | 0.159 | -0.355 | 0.185 | 0.715 |
| Population Diversity Index | Demographic & Neighborhood Characteristics | -0.003 | 0.853 | 0.039 | 0.253 | 0.770 |
| Median age of the population | -0.247 | -0.855 | -0.478 | 0.351 | 0.865 | |
| % Population 65 years and older | -0.317 | -0.857 | -0.666 | 0.274 | 0.964 | |
| Urban population density (per sq. miles) | 0.277 | 0.742 | 0.009 | -0.230 | 0.631 | |
| % Occupied housing units | Housing Characteristics | 0.456 | 0.649 | 0.572 | -0.251 | 0.739 |
| % Population below 18 years of Age | Demographic & Neighborhood Characteristics | 0.264 | 0.685 | 0.783 | -0.067 | 0.797 |
| Average household size of owner-occupied unit | Housing Characteristics | 0.376 | 0.551 | 0.744 | 0.158 | 0.718 |
| Average household size of renter-occupied unit | 0.101 | 0.323 | 0.680 | 0.049 | 0.440 | |
| %single-family homes detached | 0.562 | 0.051 | 0.568 | 0.395 | 0.748 | |
| %Owner-occupied housing units | Housing Characteristics | 0.343 | -0.360 | 0.289 | 0.520 | 0.680 |
| Variance | 28.947 | 5.551 | 3.971 | 2.205 | 40.674 | |
| %Variance | 57.89 | 11.10 | 7.94 | 4.41 | 81.35 | |
| Cronbach’s alpha (standardized) | 0.988 | 0.882 | 0.818 | N/A |
| Coefficients | Standard Error | t-value | P>|t| | VIF§ | Cronbach’s alpha (standardized) | ||
|---|---|---|---|---|---|---|---|
| Constant (b0) | 37.380 | 3.427 | 10.907 | 0.000 | 1.000 | ||
| PAF†-1 | 12.570 | 4.562 | 2.756 | 0.008 | 1.770 | 0.988 | |
| PAF-2 | ─37.726 | 7.480 | ─5.043 | 0.000 | 4.760 | 0.882 | |
| PAF-3 | ─20.454 | 9.494 | ─2.154 | 0.035 | 7.680 | 0.818 | |
| PAF-4 | 6.985 | 6.344 | 1.101 | 0.275 | 3.430 | N/A | |
| Notes:. | |||||||
| R-squared: | 0.362 | ||||||
| Adjusted R-squared: | 0.321 | ||||||
| F-statistic: | 8.925 | ||||||
| Probability (F-statistic): | 8.94 × 10-6 | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




