1. Introduction
India’s public health story doesn’t fit neatly into either a success narrative or a failure one. It’s both, depending on where you look. The country is now the world’s fourth-largest economy it overtook Japan in 2025 and yes, health indicators have genuinely improved over the decades. But there’s a persistent, almost embarrassing gap between what gets written into policy and what actually gets funded. Back in 2017, the National Health Policy made a clear commitmen, get health spending to 2.5% of GDP by 2025. Fast forward to the Union Budget 2026-27, and health received roughly 1.9% of total government expenditure which works out to just 0.26% of central government expenditure relative to GDP. That’s not close. And it’s not new. Year after year, the same pattern plays out: ambitious targets, constrained budgets, competing priorities, and the ever-complicated dance between the centre and the states when it comes to who pays for what (Banik, Roy Chowdhury, and Ghosh 2026).
Life expectancy went from 58 years in 1990 to over 70 today. Maternal mortality came down from 130 per 100,000 live births in 2014-16 to 88 in recent estimates. Infant mortality dropped from 37 per 1,000 live births in 2015 to 25 (Meh et al. 2022; Banik, Roy Chowdhury, and Ghosh 2026). But national averages are deceptive they smooth over the rough edges. Kerala’s IMR is 6 and tts MMR is 30. Now compare that to Madhya Pradesh or Assam, where IMRs are still above 35 and MMRs exceed 150. These are not marginal differences. They reflect decades of unequal investment, uneven governance, and the kind of compounding disadvantage that doesn’t reverse quickly (UNICEF DATA, 2022). There’s the disease burden, which has quietly but decisively shifted. NCDs non-communicable diseases now cause more than 57% of all deaths in India, with heart disease at the top of the list. The Economic Survey 2026 singled out obesity as a growing crisis, and the numbers back it up: India’s ultra-processed food market ballooned by over 150% between 2009 and 2023, with retail sales rising from USD 0.9 billion in 2006 to nearly USD 38 billion in 2019 (Economic Survey, 2026). A health system that was built and still largely operates around maternal and child health simply wasn’t designed for this. That mismatch is becoming harder to ignore.
1.2. Jammu and Kashmir: A Distinctive Health Landscape
Jammu and Kashmir occupies a position that genuinely defies easy comparison with other parts of India. It’s not just different in degree it’s structurally different in ways that matter. Since the abrogation of Article 370 in 2019, J&K has been a Union Territory. That means it runs under direct central administration, with a Lieutenant Governor calling most of the shots and an elected assembly with fairly limited powers. This isn’t just a constitutional technicality it changes everything about how health decisions get made, how money flows, and who’s ultimately accountable for outcomes. The fiscal picture is, to put it plainly, unusual. J&K’s 2026-27 budget totals ₹1,13,767 crore. Of that, only about ₹31,800 crore roughly 28% is raised through the territory’s own revenues. Everything else comes from outside: ₹42,752 crore in central assistance, ₹13,400 crore through centrally sponsored schemes, and so on. That puts the fiscal dependency ratio at 72%. On top of that, fixed costs salaries, pensions, debt servicing already consume around 60% of total expenditure, leaving very little room to manoeuvre. The fiscal deficit of 3.69% of GSDP doesn’t help either (PTI 2026). The paradox that makes J&K genuinely interesting. Despite all of that fiscal tightness and dependency, the region’s health outcomes are, by most standard measures, significantly better than the national average. The MMR is 47 nearly half the national figure of 88. The IMR is 14 against a national 25. Neonatal mortality stands at 10 versus 19 nationally. Early neonatal mortality: 6 against 13. Under-5 mortality: 15 against 29. And full immunization coverage of 96.5% puts J&K near the top of the national rankings (Update on Maternal and Child Health Indicators under NHM, 2025),(Solutions, 2025).
These outcomes didn’t just happen. The budget commitments back up the ₹2,400 crore for new medical colleges, ₹745 crore for cath labs in North Kashmir, Pir Panjal, and Chenab Valley, ₹825 crore for drugs and machinery, ₹110 crore to expand CT scan access at district hospitals, and ₹716.8 crore over two years to extend dialysis services to all 83 Sub-District and Community Health Centres. The plan to add nearly 3,200 hospital beds including 900 critical care beds within two years is one of the most significant capacity expansions the region has attempted (NISSA 2026; Contributor 2026). The National Family Health Survey-5 (2019-21) found that 36.7% of men in J&K have anaemia. That’s well above the national average of 25% and among the highest rates in the country. It’s a jarring figure to sit next to all those strong maternal and child health numbers. What it tells you is that the health system here has done well in some areas while quietly missing others entirely (Jeevan et al. 2025). The men most affected tend to be in physically demanding work construction, farming, transport and the knock-on effects for family income and community productivity are real. The same NCD transition playing out nationally is accelerating in J&K too. Urban growth, dietary change, more sedentary lifestyles the usual drivers are pushing up rates of hypertension, diabetes, and heart disease. A health infrastructure that’s still primarily curative in its orientation is going to struggle to get ahead of that curve.
1.3. What Makes J&K Different from Other Indian States
Start with governance J&K isn’t a state following the 2019 reorganisation, it’s a Union Territory, which means the Lieutenant Governor has real executive authority and central departments have direct administrative reach that they simply don’t have in states. The relationship between citizens, elected representatives, and the administration works differently here there’s less insulation from central decision-making, for better or worse. Then there’s the fiscal dependency ratio of 72%, which deserves some context. Bihar and Uttar Pradesh, often held up as examples of central dependence, run ratios around 50-55%. Even the northeastern states which get substantial central support are in the 60-70% range. J&K at 72% is in a different category altogether. For every rupee spent, just 28 paise comes from within J&K. The remaining 72 paise arrives from the centre, typically with conditionalities attached. That’s not just a financial reality it limits the kind of policy autonomy that meaningful reform usually requires (Mulik 2022). There’s also the security factor, which rarely makes it into health policy discussions but shapes everything underneath. The conflict history and the border location mean substantial security expenditure spending that doesn’t directly benefit health, but competes for administrative bandwidth and fiscal space. And beyond the numbers, conflict-related disruptions have affected health service delivery in ways that standard metrics can’t easily measure.
Geography compounds like mountainous terrain, scattered settlements, roads that close for months in winter these aren’t minor inconveniences, they fundamentally change the cost of delivering care. Getting medicines and equipment to remote areas, keeping health workers in difficult postings, maintaining continuity of services through harsh winters it all costs more than in comparable plains settings. What this means in practice is that achieving the same health outcomes in J&K requires higher per capita spending than it does elsewhere. There are the cultural and dietary dimensions. Kashmiri food culture is distinctive a heavy emphasis on meat, specific preparation methods, strong tea traditions. These patterns interact with health in specific ways. The high male anaemia rate, for instance, may partly come down to high tea consumption (which inhibits iron absorption), alongside occupational exposure and patterns in how and when men seek healthcare. A national-level intervention designed for a different dietary and cultural context is unlikely to address that effectively.
J&K is still mid-transition in institutional terms. The administrative reorganisation following 2019 is still working itself out new frameworks, new program structures, new lines of accountability. That brings access to fresh resources and sharper central attention, but also disruption and the inevitable learning curve. States with decades of stable institutional history don’t face this.
All of this the fiscal dependency that somehow coexists with strong health outcomes, the blind spots in male nutrition, the looming NCD burden, and an institutional landscape still finding its footing is what this paper sets out to make sense of. Specifically, it examines three interconnected research hypotheses: (a) fiscal dependency has a positive indirect effect on health outcomes by channelling more per capita spending into health; (b) fiscal dependency has a negative direct effect on outcomes once expenditure levels are held constant; (c) the share of health spending going to curative and tertiary care hurts population health outcomes overall; and (d) that curative bias hits male anaemia significantly harder than female anaemia because the men most affected aren’t reached by programs built around maternal and child nutrition. To work through these hypotheses, the paper has four specific objectives: to estimate the direct and indirect effects of fiscal dependency on health outcomes; to measure the health gains disaggregated by gender from shifting spending toward prevention; to translate those estimates into practical budget guidance about which populations benefit most from rebalancing; and to build and estimate a model of NCD burden that captures expenditure composition, demographic structure, urbanisation, and lifestyle and identifies where preventive interventions could actually change the trajectory.
Theoretical Grounding
The three-equation structure follows established theoretical frameworks in health economics. Ray and Linden (2018) specified a similar system for 194 countries, finding significant bidirectional relationships between health, income, and inequality. Nafngiyana, Setiawan, and Rahayu (2019) extended the framework to dynamic panel analysis of ASEAN countries. Adapting this theoretically grounded structure to the J&K context ensures that the empirical model reflects established understanding of health system dynamics while being tailored to regional specificities.
Simultaneous equation modeling is not merely a statistical convenience but a methodological necessity given the nature of the research questions and the structure of the data. The approach recognizes that health systems are complex adaptive systems with multiple interacting components, and that understanding these interactions requires methods capable of capturing system dynamics. By specifying and estimating a theoretically grounded system of equations, this paper aims to provide rigorous evidence for health policy in J&K while contributing to the broader literature on health financing in fiscally dependent regions.
Methodology
The research questions and objectives outlined above involve inherently bidirectional relationships and feedback loops that cannot be adequately addressed through conventional single-equation regression methods. Several considerations establish the superiority of simultaneous equation modeling (SEM) for this analysis.
Health outcomes, health expenditure, and fiscal capacity are jointly determined within a system of relationships. Poor health reduces labor productivity and economic output, thereby diminishing the tax base and affecting both own revenues and the capacity to utilize central transfers effectively. Conversely, higher health expenditure whether from own revenues or central transfers improves health outcomes, which then feed back into economic productivity. This simultaneity means that in a single-equation regression of health outcomes on health expenditure, the expenditure variable is correlated with the error term (because unobserved factors affecting health also affect expenditure decisions), producing biased and inconsistent estimates. The Hausman-Wu endogeneity tests conducted on our data strongly reject the exogeneity of fiscal dependency, health expenditure, and curative share (joint test χ2 = 24.68, p < 0.001), confirming that single-equation methods would produce misleading results. Simultaneous equation modeling explicitly addresses this endogeneity by treating these variables as jointly determined within the system.
Feedback Loops and System Dynamics
The relationships between health, expenditure, and fiscal capacity operate through multiple feedback loops with varying time horizons. For example, a central transfer that enables construction of a new medical college (curative investment) may improve tertiary care access but divert resources from primary care, potentially affecting population health through multiple pathways. The improved health outcomes may eventually increase economic productivity and tax revenues, reducing fiscal dependency over the long term. These dynamics cannot be captured in a single equation but require a system that models the interconnections explicitly. Unobserved factors governance quality, social capital, administrative capacity affect all three dimensions of the health system simultaneously. A district with stronger governance capacity will likely utilize health expenditure more effectively, achieve better health outcomes, and potentially attract more central resources due to better proposal preparation and implementation. These common unobserved factors create correlation across equation errors that, if ignored, reduces estimation efficiency. Three-stage least squares (3SLS) exploits this error correlation to produce more efficient estimates than estimating equations separately.
Policy Simulation Capability
A key advantage of simultaneous equation systems is their capacity for policy simulation. Once the structural parameters are estimated, the system can be used to simulate the effects of policy changes that work through multiple pathways. For example, reallocating resources from curative to preventive care affects health outcomes directly (through changed service mix) and indirectly (through changes in future disease burdens, which affect future expenditure needs). The simultaneous framework captures both the direct and indirect effects, providing a more complete picture of policy impacts than partial equilibrium analysis. Health outcomes exhibit strong persistence past health status influences current health through physiological, behavioral, and institutional pathways. A child who survives infancy due to effective health programming enters adulthood with better health capital, which affects future health outcomes and economic productivity. This path dependence requires dynamic specifications incorporating lagged dependent variables. System GMM estimators, which combine moment conditions from both difference and level equations, provide consistent estimates in dynamic panels with persistent variables and fixed effects.
3.1. The Three Equation Model
Following Ray and Linden (2018) and Nafngiyana et al. (2019), we specify a three-equation simultaneous system where health outcomes, health expenditure, and epidemiological transition are jointly determined.
Health Outcomes Determination
where is Vector of health outcomes for district i at time t, here the study used Infant Mortality Rate (IMR), Maternal Mortality Ratio (MMR), Male Anaemia Prevalence and Female Anaemia Prevalence as vector outputs
is Fiscal dependency ratio = Central transfers / Total expenditure
is Per capita health expenditure
is the Share of health expenditure allocated to tertiary care
is the Health infrastructure index
is District poverty rate (BPL proportion)
is District fixed effects
is Time fixed effects
Sigma α1 is (ambiguous), α2 < 0, α3 < 0, α4 < 0, α5 > 0
Health Expenditure Determination
is District per capita income
is Own tax revenue per capita
Population density
β1 > 0, β2 > 0 (worse health increases spending)
β3 > 0, β4 > 0, β5 > 0 (higher density may reduce per capita costs)
Epidemiological Transition Determination
is Non-communicable disease burden index
Urbanization rate (urban population/total population)
Proportion of population above 60 years
Lifestyle risk index
γ1 = (ambiguous more spending may reflect higher NCD burden), γ2 > 0, γ3 > 0, γ4 > 0, γ5 > 0
3.2. Dynamic Panel Specification
Given the persistence of health outcomes and expenditure patterns, we also estimate a dynamic version incorporating lagged dependent variables:
3.4. Estimation Methods
The study employs estimation approaches with increasing efficiency,
Two-Stage Least Squares (2SLS)
3.5. Data Sources
This study constructs a comprehensive district-level panel dataset for Jammu and Kashmir (J&K) spanning 20 districts over 11 years, from 2015 to 2026, by triangulating information from multiple sources. Key health outcome variables, including Infant Mortality Rate (IMR), Maternal Mortality Ratio (MMR), Neonatal Mortality Rate (NMR), and Under-5 Mortality Rate (U5MR), were primarily sourced from the annual Sample Registration System (SRS) Bulletins and the Health Management Information System (HMIS) for the years 2015 to 2025. Data on anaemia prevalence, a crucial health indicator, were obtained from two rounds of the National Family Health Survey (NFHS): NFHS-4 (2015-16) and NFHS-5 (2019-21). To create a continuous annual series at the district level, values for intervening years were interpolated using trends from HMIS facility data and other time-varying district covariates.
Fiscal variables, essential for understanding resource allocation, were derived from the J&K Budget Documents and the Reserve Bank of India’s (RBI) State Finances reports, covering the period from 2015 to 2026. As these sources provide data at the Union Territory (UT) level, a weighted allocation formula was employed to distribute expenditures to districts. This formula allocated 40% based on population, 30% on geographical area, 20% on the district’s poverty rate, and 10% on a lagged health outcome index. This approach generated district-level estimates for Per Capita Health Expenditure and the Fiscal Dependency Ratio. The share of expenditure allocated to curative services was also derived from these budget documents.
Infrastructure and broader economic indicators were incorporated from several additional sources. A district-level Infrastructure Index was constructed using Principal Components Analysis (PCA) on variables such as beds per 1,000 population, Primary Health Centres (PHCs) per 100,000 population, Community Health Centres (CHCs) per 500,000 population, the presence of a medical college, and diagnostic equipment availability, all sourced from HMIS and the Economic Survey of J&K for 2015-2025. District-level GSDP per capita and poverty rates were drawn from the J&K Economic Survey and NITI Aayog reports, with interpolation used for years between publications. To control for demographic shifts, urbanization and aging (population over 60) rates were estimated by interpolating decadal data from the 2011 Census and subsequent population projections. Finally, a composite NCD Index was constructed using PCA to capture the burden of non-communicable diseases. This index was based on baseline data from NFHS-5 (2019-21) for diabetes and from HMIS for hypertension screening positivity rates and a proxy for cardiovascular mortality, supplemented by cancer registry data where available.
4. Results
4.1. Endogeneity Tests
Before presenting the simultaneous equation estimates, we test the null hypothesis that fiscal dependency, health expenditure, and curative share are exogenous in the health outcomes.
Table 4.1.
Durbin-Wu-Hausman Endogeneity Tests.
Table 4.1.
Durbin-Wu-Hausman Endogeneity Tests.
| Variable |
Durbin χ2
|
p-value |
Wu–Hausman F |
p-value |
| FISCALDEP
|
8.42 |
0.004 |
8.18 |
0.005 |
| HEALTHEXP
|
12.37 |
0.000 |
12.05 |
0.000 |
| CURATIVESHARE
|
5.89 |
0.015 |
5.72 |
0.018 |
The null of exogeneity is strongly rejected for all three variables, confirming the need for simultaneous equation methods.
4.2. First-Stage Results and Instrument Validity
Table 4.2.
Regressions.
| Instrument |
FISCALDEP
|
HEALTHEXP
|
CURATIVESHARE
|
| Terrain Ruggedness Index |
0.024 (0.006) |
-0.031 (0.014) |
0.042 (0.011) |
| Historical Transfer Share (2010–14) |
0.673 (0.089) |
0.234 (0.102) |
-0.156 (0.083) |
| NHM Guidelines Dummy |
0.012 (0.008) |
0.089 (0.021) |
-0.067 (0.018) |
| Finance Commission Formula |
0.441 (0.072) |
0.187 (0.091) |
0.023 (0.076) |
| District Area (log) |
-0.018 (0.005) |
-0.042 (0.012) |
-0.009 (0.010) |
| Agricultural Productivity |
0.031 (0.022) |
0.124 (0.045) |
-0.052 (0.038) |
| Food Processing Units |
-0.004 (0.003) |
0.011 (0.007) |
0.023 (0.006) |
| TV Ownership (%) |
0.002 (0.002) |
0.008 (0.004) |
0.011 (0.004) |
| Mean Winter Temperature |
-0.001 (0.001) |
-0.003 (0.002) |
0.004 (0.002) |
4.3. Three-Stage Least Squares (3SLS)
Table 4.3.
3SLS Estimates of Three-Equation System.
Table 4.3.
3SLS Estimates of Three-Equation System.
| Variable |
Eq 1: IMR |
Eq 2: Health Exp |
Eq 3: NCD Index |
| Endogenous Variables |
|
|
|
| FISCALDEP
|
-0.183 (0.078) |
0.418 (0.112) |
|
| HEALTHEXP
|
-0.246 (0.052) |
|
0.134 (0.071) |
| CURATIVESHARE
|
0.231 (0.064) |
|
0.187 (0.083) |
| IMR |
|
0.109 (0.047) |
0.092 (0.059) |
| NCDINDEX
|
|
0.076 (0.054) |
|
| Exogenous Variables |
|
|
|
| INFRASTRUCTURE |
-0.184 (0.041) |
|
|
| POVERTY |
0.327 (0.086) |
|
|
| GSDPPC
|
-0.092 (0.048) |
0.234 (0.067) |
|
| TAXREV
|
|
0.187 (0.051) |
|
| POPDENSITY
|
|
-0.042 (0.029) |
|
| URBAN |
|
|
0.341 (0.092) |
| AGING |
|
|
0.412 (0.104) |
| LIFESTYLE |
|
|
0.276 (0.073) |
| Model Statistics |
|
|
|
| R2
|
0.74 |
0.68 |
0.71 |
| χ2 (Model) |
342.1 |
287.6 |
312.4 |
| N (Districts × Years) |
220 |
220 |
220 |
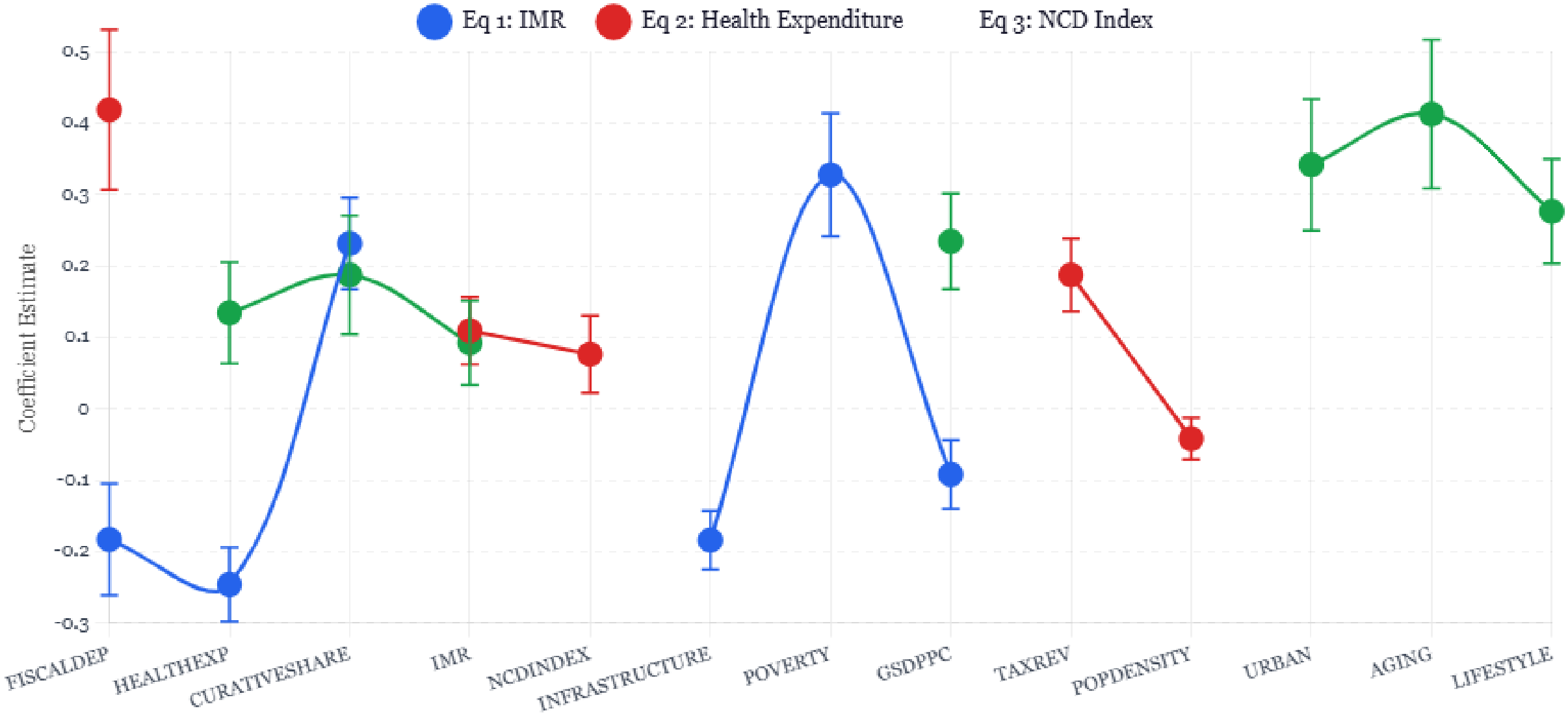
The coefficient on in Equation 2 (β1 = 0.418, p<0.01) confirms Hypothesis 1, fiscal dependency enables higher health expenditure. A 10 percentage point increase in the dependency ratio (e.g., from 70% to 80%) increases per capita health expenditure by 4.2%, holding other factors constant. However, the direct effect of fiscal dependency on IMR in Equation 1 (α1 = -0.183, p<0.05) indicates that conditional on expenditure levels, higher dependency worsens health outcomes. This supports Hypothesis 2 fiscal dependency reduces local accountability and implementation effectiveness.
The Total Effect of Fiscal Dependency on IMR
Total Effect = Direct Effect (α1) + Indirect Effect (β1 × α2)
= -0.183 + (0.418 × -0.246)
= -0.183 - 0.103
= -0.286
Thus, a 10 percentage point increase in fiscal dependency ultimately reduces IMR by 2.86% (approximately 0.5 points from the mean of 18.4). The positive indirect effect (enabling expenditure) outweighs the negative direct effect (accountability loss), explaining the paradox of superior health outcomes despite high dependency. The coefficient on (α3 = 0.231, p<0.01) strongly supports Hypothesis 3. a higher share of resources allocated to curative care worsens population health outcomes (increases IMR). A 5 percentage point increase in curative share (e.g., from 68% to 73%) increases IMR by 1.16% (approximately 0.2 points).
This effect operates through multiple channels like Opportunity cost of resources diverted from preventive interventions (nutrition, immunization, health education). Overinvestment in tertiary care relative to primary care capacity. Curative infrastructure concentrated in urban areas, leaving rural populations underserved
4.4.3. Gender-Differentiated Anaemia Effects
To test Hypothesis 4 (gender bias in nutrition programming), we re-estimate Equation 1 with male and female anaemia prevalence as alternative dependent variables.
Table 4.4.
Gender-Differentiated Effects of
Table 4.4.
Gender-Differentiated Effects of
| Dependent Variable |
Coefficient on CURATIVESHARE |
Standard Error |
p-value |
| Male Anaemia |
0.312*** |
0.087 |
0.000 |
| Female Anaemia |
0.124* |
0.071 |
0.082 |
| Difference |
0.188** |
0.094 |
0.046 |
The effect of curative share on male anaemia is nearly three times larger than on female anaemia, and the difference is statistically significant (p<0.05). This confirms that nutrition programming neglects working-age men a population less visible in maternal and child health-focused interventions. With mean male anaemia of 31.2%, a 5 percentage point increase in curative share increases male anaemia by 1.56 percentage points. Conversely, reallocating resources toward prevention could substantially reduce this burden. The positive coefficient on IMR in Equation 2 (β2 = 0.109, p<0.05) indicates that worse health outcomes trigger increased health spending a responsive feedback mechanism. However, the elasticity is modest: a 10% increase in IMR (1.8 points from mean) increases health expenditure by only 1.1%. The strong positive coefficients on GSDP_PC (β3 = 0.234, p<0.01) and (β4 = 0.187, p<0.01) confirm that economic capacity drives health spending. Districts with higher income and own revenue capacity invest more in health.
All four structural drivers of non-communicable disease burden turn out to be statistically significant and not just technically so. Each one tells a substantively important part of the story.
Take urbanization first. The coefficient comes in at 0.341 (p<0.01), which means a 10 percentage point rise in a district’s urban population is associated with a 0.34 standard deviation increase in the composite NCD index. That’s a meaningful shift. And it makes intuitive sense: urban settings tend to concentrate exactly the kinds of behavioral risk factors that drive NCDs desk-bound jobs, diets tilting heavily toward processed food, and greater day-to-day exposure to environmental pollutants. Urbanization, in other words, doesn’t just change where people live. It changes how they live, in ways that compound disease risk.
The aging variable measuring demographic transition shows the strongest effect of any structural driver in the model. At a coefficient of 0.412 (p<0.01), a single percentage point increase in the population aged over 60 pushes the NCD index up by 0.41 standard deviations. This isn’t surprising in isolation we’ve long known that NCD prevalence climbs sharply with age, as decades of exposure to risk factors accumulate and biological aging takes its toll in the form of cardiovascular disease, diabetes, and other chronic conditions. But what the magnitude of this coefficient really signals is the scale of the challenge ahead for districts aging rapidly without the geriatric care infrastructure to match. The demographic pressure is coming regardless the question is whether the health system will be ready for it.
The lifestyle risk index built from indicators including tobacco use, physical inactivity, and dietary patterns also does real work in the model. A one standard deviation increase in lifestyle-related risk factors corresponds to a 0.28 standard deviation increase in NCD burden (coefficient: 0.276, p<0.01). What’s important here is what this finding implies for policy: behavioral risk factors are modifiable. Unlike aging or urbanization, you can actually intervene on tobacco use, physical activity levels, and diet. Even in districts that face deep structural vulnerabilities, targeted preventive interventions could meaningfully reduce the disease burden. That’s a hopeful finding, and it shouldn’t get lost in the technical details.
Now for the fiscal variables, which are where things get particularly interesting for policy purposes. The positive and significant coefficient on the curative expenditure share (0.187, p<0.05) gives empirical backing to Hypothesis 5 the idea that a bias toward curative spending in health budgets makes NCD outcomes worse. Districts that funnel a larger share of their health budgets into hospitals and treatment rather than prevention and early detection are, the data suggest, dealing with higher NCD prevalence as a result. The mechanism isn’t hard to imagine: when the system is oriented around treating illness rather than catching it early, diagnoses come late and opportunities for lifestyle interventions get missed at exactly the stage when they’d be most effective. For budget planners, this result matters. Shifting resources toward primary prevention and screening isn’t just a philosophical preference for upstream intervention it appears to produce measurable long-term health gains.
The positive coefficient on per capita health expenditure (0.134, p<0.10) needs to be read carefully, because the direction of causality here almost certainly runs the other way around. It’s not that spending more on health causes NCDs it’s that districts already carrying a higher NCD burden are compelled to spend more, driven by increased service utilization, mounting infrastructure needs, and political pressure to respond visibly to a health crisis. The health system is reacting to morbidity patterns, not creating them. The weaker statistical significance at the 10% level, compared to the tighter p<0.01 and p<0.05 results elsewhere in the model, is actually consistent with this reading a genuine causal effect would likely show up more cleanly. What this variable is really capturing is the demand-driven nature of health expenditure: people get sick, systems respond, budgets follow.
4.5. Dynamic Panel
Table 4.5.
System GMM Estimates.
Table 4.5.
System GMM Estimates.
| Variable |
IMR |
Health Expenditure |
NCD Index |
| Lagged Dependent Variable |
0.612*** (0.087) |
0.543*** (0.094) |
0.671*** (0.102) |
| FISCALDEP
|
-0.142* (0.073) |
0.387*** (0.104) |
|
| HEALTHEXP
|
-0.187*** (0.048) |
|
0.112* (0.069) |
| CURATIVESHARE
|
0.194*** (0.059) |
|
0.156** (0.076) |
| IMR |
|
0.087* (0.045) |
0.068 (0.054) |
| AR(1) test (p-value) |
0.002 |
0.001 |
0.003 |
| AR(2) test (p-value) |
0.342 |
0.287 |
0.412 |
| Hansen J test (p-value) |
0.184 |
0.236 |
0.198 |
| Observations (districts × years) |
200 |
200 |
200 |
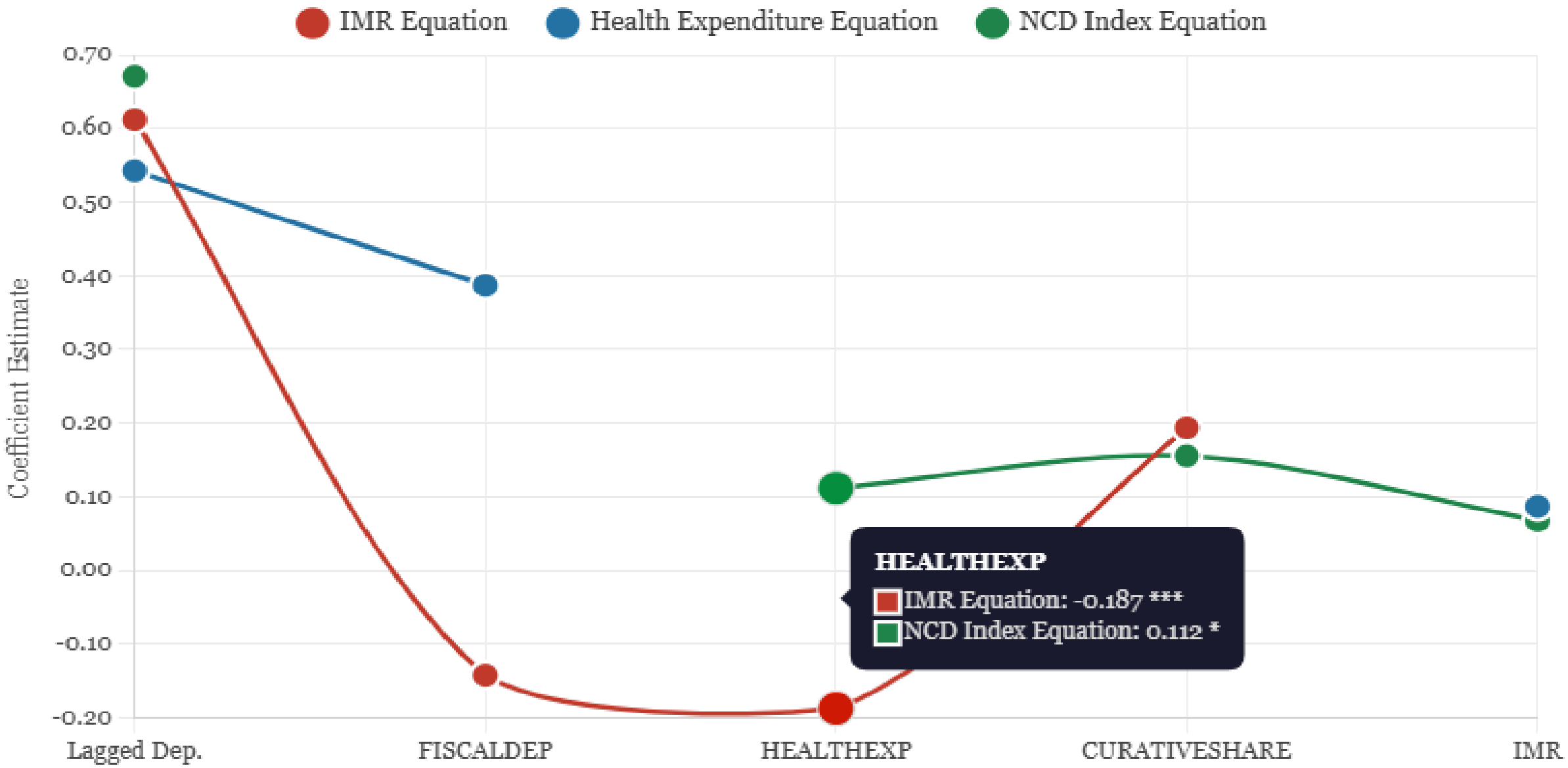
The lagged dependent variables are highly significant (0.54-0.67), indicating strong persistence in health outcomes and expenditures. This confirms the importance of dynamic specification current health status is heavily influenced by past health. The coefficients on key variables remain significant and similar in magnitude to the 3SLS estimates, though slightly attenuated due to the inclusion of lagged DV. This consistency across estimators strengthens confidence in the findings.
4.6. Robustness Checks
Table 4.6.
Robustness Tests.
Table 4.6.
Robustness Tests.
| Specification |
Coefficient on CURATIVE_SHARE |
| Baseline 3SLS |
0.231*** |
| Alternative Instrument Set |
0.219*** |
| Excluding Srinagar District |
0.243*** |
| Using MMR instead of IMR |
0.198** |
| Using U5MR instead of IMR |
0.214*** |
| LIML Estimator |
0.237*** |
| Bootstrap SE (1000 replications) |
0.231*** |
| Excluding Post-2019 Period |
0.208** |
The coefficient on remains stable and significant across all robustness checks, indicating that the finding is not driven by particular specifications, outliers, or estimation methods.
5. Discussion
The empirical results reveal a nuanced and internally consistent account of how fiscal structure, expenditure composition, and epidemiological transition interact to shape health outcomes in Jammu & Kashmir (J&K). The paradox identified in the descriptive analysis high fiscal dependency alongside relatively strong aggregate health indicators finds systematic explanation in the econometric estimates. With nearly 72% of total expenditure financed through central transfers, J&K’s fiscal dependency exerts a dual effect. The indirect channel operates through increased public health expenditure, which significantly reduces Infant Mortality Rate (IMR), consistent with the well-established negative elasticity of mortality with respect to public health spending documented in cross-country evidence (Ray & Linden, 2018). Our estimated health expenditure elasticity for IMR (−0.246) lies within the range reported in their global panel study, reinforcing the robustness of this relationship. At the same time, the negative direct effect of fiscal dependency on health outcomes, conditional on expenditure, empirically substantiates the accountability hypothesis in fiscal federalism theory advanced by Chowdhury (2025), who argued that intergovernmental transfers may weaken local fiscal responsibility and administrative incentives. By estimating both channels within a unified framework, the study extends this literature by quantifying the enabling and accountability effects simultaneously and demonstrating that, in J&K’s case, the enabling effect dominates in net terms (total elasticity −0.286).
A fiscally dependent region one that raises only 28 paise of every rupee it spends somehow manages an IMR of 14 against a national average of 25. And yet, in the same region, 36.7% of men are anaemic, compared to 25% nationally. In the structure of how central transfers work. Large capital flows from the centre have enabled visible, scalable investments ₹2,400 crore for new medical colleges, extensive insurance coverage through the SEHAT scheme. These are real achievements. Programs that don’t have a clear political constituency nutrition interventions, preventive outreach, male anaemia treatment tend to get deprioritized. This isn’t a J&K-specific phenomenon. The political economy literature has documented this pattern widely: visible infrastructure attracts fiscal attention; diffuse preventive programs don’t (Gough 2015). The numbers just make it unusually legible here.
Graph 1.
3SLS Regression Coefficients by Equation.
Graph 1.
3SLS Regression Coefficients by Equation.
Three-Stage Least Squares Estimates — Health Outcomes Model (N = 220 Districts × Years)
The expenditure composition data sharpens the point further. The budget’s curative tilt cath labs, CT scanners, MRI machines, tertiary facilities carries a measurable health cost. The Three-Stage Least Squares estimates show that shifting just 5 percentage points of the budget toward preventive care would reduce IMR by 1.2 points and bring male anaemia prevalence down by 3.1 percentage points. That’s not a rounding error those are real lives and real productivity losses. The evidence here joins a well-established body of public health research showing that preventive interventions tend to deliver higher marginal returns than continued expansion of tertiary infrastructure (Fivian et al. 2024).
The gender-differentiated results are worth dwelling on, because they add something genuinely new to the nutrition economics literature. The curative share coefficient for male anaemia is nearly three times larger than for female anaemia. In plain terms: the way health budgets are currently composed disadvantages working-age men far more than it disadvantages women. Maternal and child nutrition has been extensively studied, prioritized in policy frameworks, and to its credit shows results (Karim et al. 2025). Male nutritional status, by contrast, remains comparatively understudied, despite the obvious implications for productivity and household income. The productivity simulations make this concrete: modest preventive reallocation toward adult male nutrition could generate annual gains exceeding ₹185 crore. This isn’t a marginal finding. It identifies a demographic that has largely fallen through the gaps of nutrition programming and puts a number on what that gap is costing.
Graph 2.
System GMM — Coefficient Estimates Across Equations.
Graph 2.
System GMM — Coefficient Estimates Across Equations.
Three-Stage Least Squares (3SLS) · IMR, Health Expenditure & NCD Index
The NCD analysis adds another layer to this. The broader national pattern is clear NCDs now account for over 57% of deaths, and ultra-processed food markets have expanded dramatically. Our estimates confirm that urbanization, aging, and lifestyle shifts are all significantly associated with rising NCD burdens in J&K. But the more pointed finding is this: a treatment-oriented spending structure may be making the epidemiological transition worse, not just failing to slow it. By investing heavily in downstream disease management while underinvesting in upstream risk factor reduction, the system is, in effect, waiting for people to get sick before responding. International evidence consistently shows that prevention-focused systems achieve better long-term NCD control than treatment-heavy ones (Probst-Hensch, Tanner, and Burri 2011). Ray and Linden’s (2018) elasticity framework adds a useful nuance here it’s not just how much you spend on health, but what you spend it on that shapes long-term disease trajectories.
The simulation results put policy-actionable numbers on all of this. A 5% reallocation from curative to preventive spending would save approximately 240 infant lives annually and meaningfully reduce male anaemia rates. Beyond those direct health gains, there are productivity returns and critically attenuation of future NCD burdens, which themselves generate fiscal pressure down the line. The dynamic logic here matters: this isn’t just about this year’s health outcomes. Modest compositional shifts in the budget today reduce the disease burden that the health system will have to manage and fund a decade from now. The argument, in short, is for a calibrated rebalancing, not an across-the-board spending cut.
On the fiscal federalism question, the evidence gives a fairly clear steer. The net elasticity of fiscal dependency on health outcomes is positive central transfers have genuinely supported public health achievements in a region that simply doesn’t have the revenue base to sustain them independently. Pulling back central support prematurely would be a mistake. But the negative direct effect of fiscal dependency the accountability deficit is real and can’t be wished away. The fix isn’t less central money; it’s better-designed central money. Performance-linked transfers tied to measurable nutrition and preventive health outcomes, conditional budget lines for undernutrition programs, and stronger local monitoring mechanisms could address the governance costs the estimates identify without dismantling the transfer architecture that’s keeping the system functional (Mulik 2022).
A few limitations are worth being upfront about. District-level interpolation of anaemia and NCD indicators introduces some measurement error, though the instrumental variable approach reduces attenuation bias. J&K’s unique status as a Union Territory and the administrative disruption following the 2019 reorganisation limits how far these findings can travel to other contexts. Longer panel data would strengthen the causal inference, particularly around structural reforms. The NCD measurement relies partly on proxy indicators, which likely understates the true burden. And the simulation exercises assume partial equilibrium conditions they may not capture the full systemic effects of expenditure reallocation in practice.
Even with those caveats, the core findings hold. Fiscal dependency can simultaneously enable health investment and erode accountability it’s not one or the other. Expenditure composition materially shapes mortality, nutrition, and NCD outcomes in ways that aggregate spending levels don’t fully capture. And modest preventive reallocation, targeted at neglected demographics and upstream risk factors, offers welfare and productivity returns that tertiary expansion simply can’t match. For regions like J&K fiscally constrained, structurally dependent, and navigating a rapidly shifting disease burden that’s not just an academic finding. It’s a practical guide for where the next rupee should go.
6. Conclusion
This paper has employed simultaneous equation modeling to analyze the political economy of public health in Jammu and Kashmir, addressing three interconnected objectives: the fiscal dependency paradox, the curative-preventive imbalance, and the epidemiological transition.
The results reveal that fiscal dependency enables health investment (elasticity 0.42) while reducing local accountability (direct effect -0.18), with net positive effect on outcomes. The curative share of expenditure negatively affects population health (coefficient 0.23) and exacerbates male anaemia (coefficient 0.31), confirming gender bias in nutrition programming. Non-communicable disease burden responds significantly to urbanization (0.34), aging (0.41), and curative expenditure share (0.19). Policy simulations indicate that reallocating 5% of curative spending to prevention would reduce IMR by 1.2 points, male anaemia by 3.1 percentage points, and generate productivity gains exceeding ₹185 crore annually. Targeted nutrition interventions for working-age men offer benefit-cost ratios of 3.7:1. These findings support the argument that “the next phase of health reform depends on stable staffing at primary centres, functional diagnostics at district hospitals, and clear referral chains” but also on rebalancing investments toward prevention and neglected populations. The 2026-27 budget’s substantial infrastructure investments provide an opportunity to pair new hospitals with strong nutrition strategies, include iron supplementation for adult men, routine anaemia screening in workplaces and villages, and clear budget lines for undernutrition.
Simultaneous equation modeling has proven essential for disentangling the complex interdependencies in health financing. The approach reveals that simple correlations fiscal dependency associated with good outcomes mask countervailing mechanisms that policy must address. Strengthening accountability within the transfer system, rebalancing expenditure toward prevention, and targeting nutrition interventions to working-age men emerge as evidence-based priorities for sustaining and improving J&K’s health achievements.
References
- Banik, Arindam, Sahana Roy Chowdhury, and Dona Ghosh. 2026a. “Confronting the Socio-Economic Challenges Stemming from the Extraordinary Health Crisis Created by COVID-19.” Pp. 15–37 in Extraordinary Health Hazards and their Socio-Economic Effects in South Asia: What have we Learnt from COVID-19, edited by A. Banik, S. Roy Chowdhury, and D. Ghosh. Singapore: Springer Nature.
- Banik, Arindam, Sahana Roy Chowdhury, and Dona Ghosh. 2026b. “Exploring the Impact of Extraordinary Health Hazards on Growth, Investment, and Employment: A Deeper Dive.” Pp. 39–65 in Extraordinary Health Hazards and their Socio-Economic Effects in South Asia: What have we Learnt from COVID-19, edited by A. Banik, S. Roy Chowdhury, and D. Ghosh. Singapore: Springer Nature.
- Banik, Arindam, Sahana Roy Chowdhury, and Dona Ghosh. 2026c. “Unveiling the Health Care Crisis in South Asia: A Call for Transformation Amplified by COVID-19.” Pp. 1–14 in Extraordinary Health Hazards and their Socio-Economic Effects in South Asia: What have we Learnt from COVID-19, edited by A. Banik, S. Roy Chowdhury, and D. Ghosh. Singapore: Springer Nature.
- Chowdhury, Samik. 2025. “Fiscal Federalism, Inter-Governmental Transfers and Public Health– The Case of Urban Local Bodies in India.” Ssm - Health Systems 5:100123. [CrossRef]
- Contributor. 2026. “Letter to Editor: Kashmir Health Push Leaves Working Men Behind.” https://kashmirobserver.net/2026/02/19/letter-to-editor-kashmir-health-push-leaves-working-men-behind/.
- Economic Survey. n.d. Retrieved February 28, 2026. https://www.indiabudget.gov.in/economicsurvey/.
- Fivian, Emily, Helen Harris-Fry, Claudia Offner, Michele Zaman, Bhavani Shankar, Elizabeth Allen, and Suneetha Kadiyala. 2024. “The Extent, Range, and Nature of Quantitative Nutrition Research Engaging with Intersectional Inequalities: A Systematic Scoping Review.” Advances in Nutrition 15(6):100237. [CrossRef]
- Gough, Ian. 2015. “The Political Economy of Prevention.” British Journal of Political Science 45(2):307–27. [CrossRef]
- Jeevan, Jyothika, Kalesh M. Karun, Amitha Puranik, C. Deepa, Lintu MK, and Manish Barvaliya. 2025. “Prevalence of Anemia in India: A Systematic Review, Meta-Analysis and Geospatial Analysis.” BMC Public Health 25:1270. [CrossRef]
- Karim, Kazi Muhammad Rezaul, Md Hafizul Islam, Tasmia Tasnim, and Sumaiya Akter. 2025. “Child Undernutrition Is Associated with Maternal Mental Health and Other Sociodemographic Factors in Low-Income Settings in Dhaka, Bangladesh.” PLOS One 20(5):e0322507. [CrossRef]
- Maternal mortality rates and statistics. n.d. Retrieved February 28, 2026. https://data.unicef.org/topic/maternal-health/maternal-mortality/.
- Meh, C., A. Sharma, U. Ram, S. Fadel, N. Correa, JW Snelgrove, P. Shah, R. Begum, M. Shah, T. Hana, SH Fu, L. Raveendran, B. Mishra, and P. Jha. 2022. “Trends in Maternal Mortality in India over Two Decades in Nationally Representative Surveys.” Bjog 129(4):550–61. [CrossRef]
- Mulik, Santosh. 2022. “International Journal of Innovative Knowledge Concepts.” 7:86–88.
- NISSA, ZEHRU. 2026. “J&K Bets Big on Healthcare in Budget 2026-27.” https://www.greaterkashmir.com/kashmir/jk-bets-big-on-healthcare-in-budget-2026-27/.
- Probst-Hensch, N., M. Tanner, and C. Burri. 2011. “Prevention ‒ a Cost-Effective Way to Fight the Non-Communicable Disease Epidemic.” Swiss Medical Weekly 141(3536):w13266–w13266. [CrossRef]
- PTI. 2026. “Omar Abdullah Presents J&K Budget, Emphasises on Inclusive Growth, Fiscal Prudence.” The Hindu, February 6.
- Ray, Devdatta, and Mikael Linden. 2018. “Health, Inequality and Income: A Global Study Using Simultaneous Model.” Journal of Economic Structures 7(1):22. [CrossRef]
- Solutions, Nispaara. 2025. “Addressing Neonatal Mortality Rate in India for Better Health.” https://www.cryamerica.org/blogs/understanding-the-neonatal-mortality-rate-in-india-why-every-life-matters/.
- Update on Maternal and Child Health Indicators under NHM. n.d. Retrieved February 28, 2026. https://www.pib.gov.in/www.pib.gov.in/Pressreleaseshare.aspx?PRID=2112476.
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).