Submitted:
02 March 2026
Posted:
03 March 2026
You are already at the latest version
Abstract

Keywords:
1. Introduction
2. Methodology
2.1. Study Design and Data Source
2.2. Study Population & Eligibility Criteria
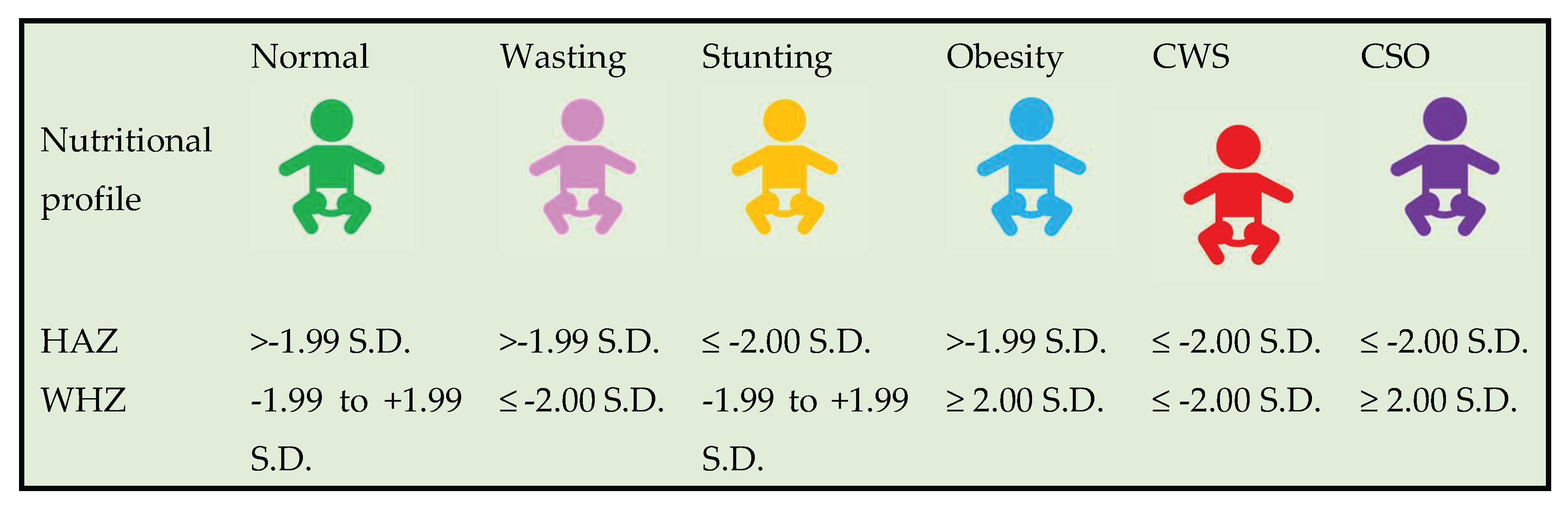
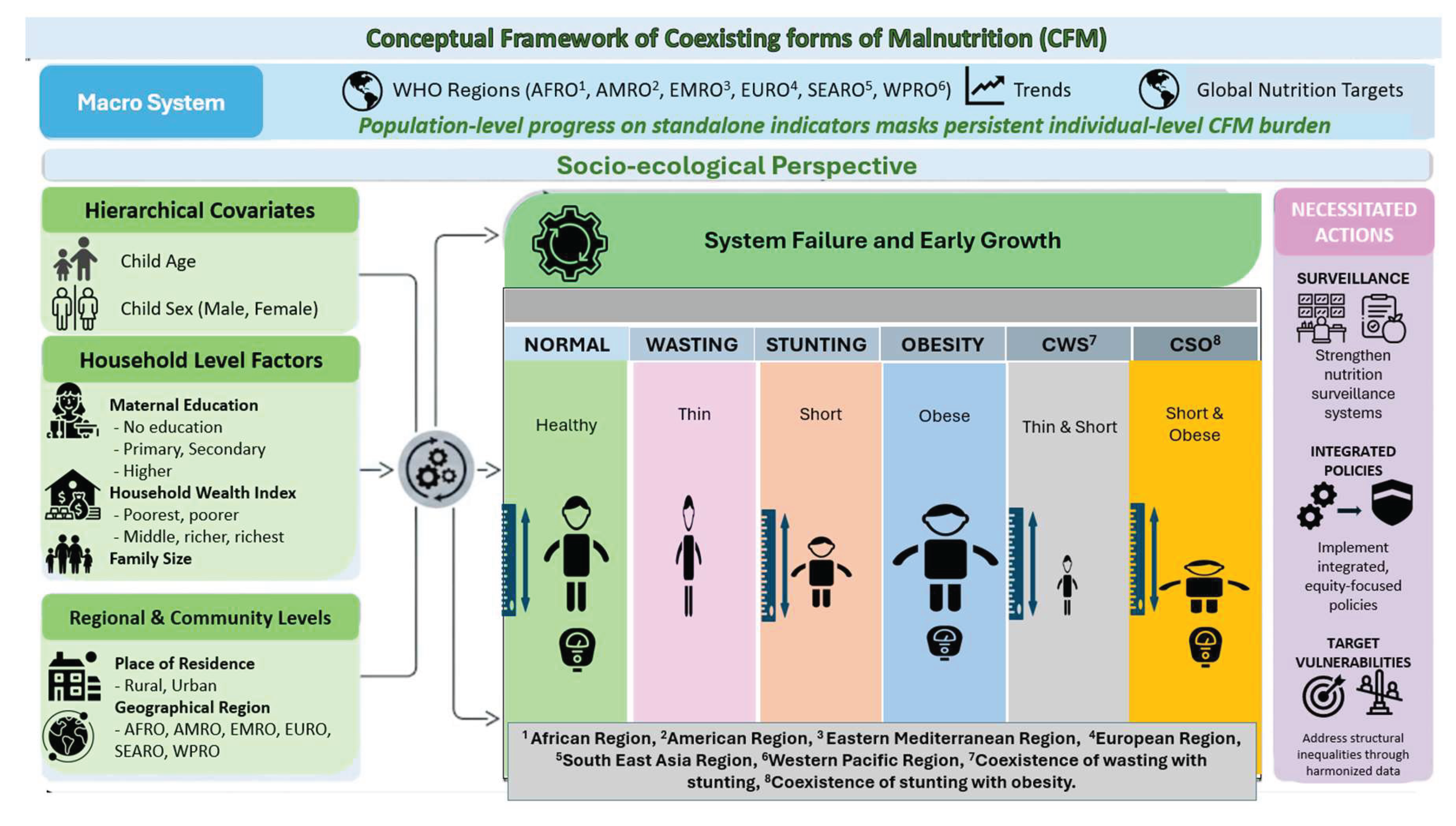
2.3. Conceptual Framework
2.4. Study Outcomes
2.5. Study Covariates
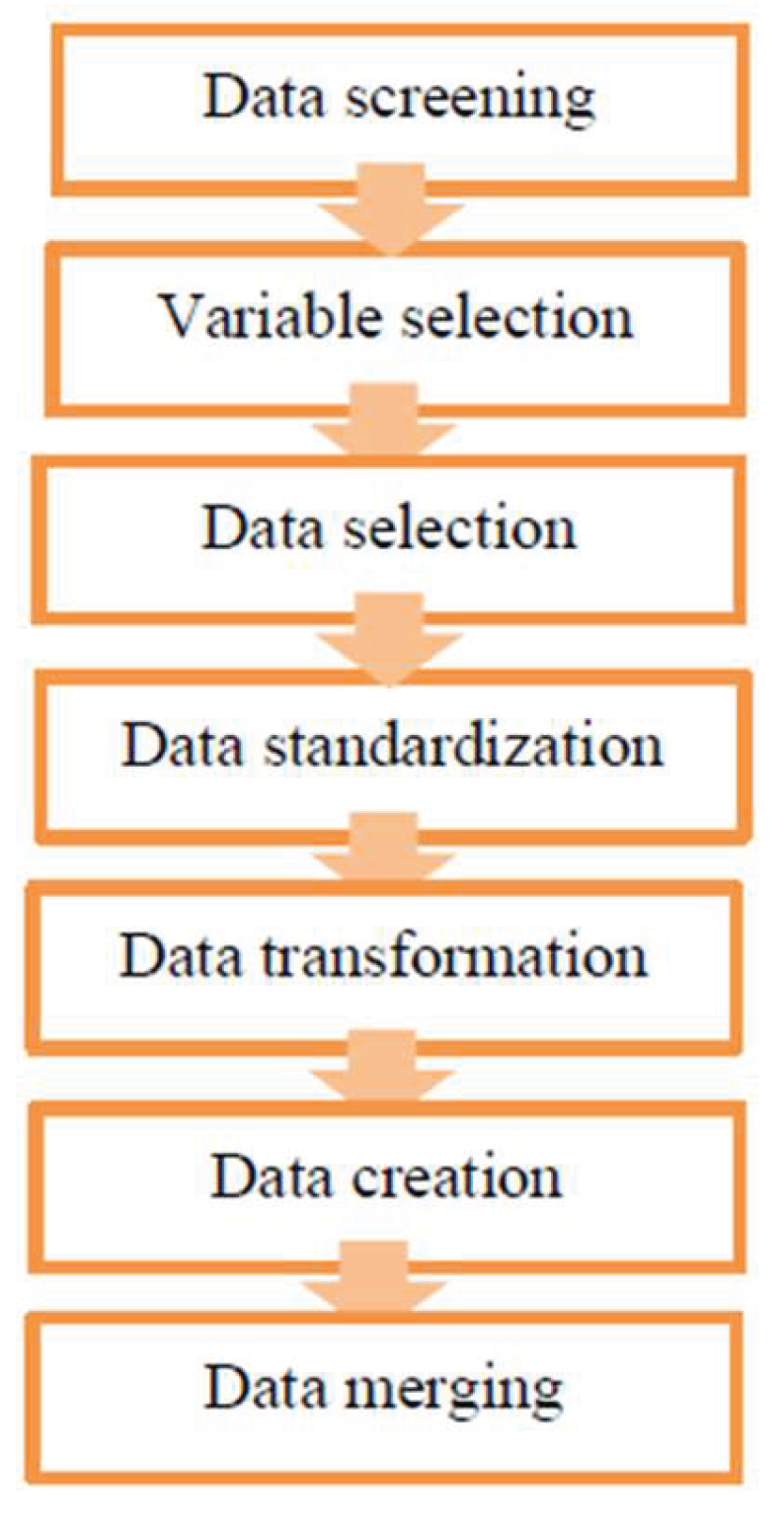
2.6. Data Handling and Management
2.7. Statistical Analysis
2.8. Ethical Considerations
3. Results
3.1. Scenario-Based Projections of GNTs to 2030 Among Children Under Five Across LMICs
3.2. Baseline, Current and Scenario-Based Projections of Various Forms of Malnutrition Including CFM Among Children Under Five Across LMICs
3.3. Determinants of Standalone and Coexisting Forms of Malnutrition Among Children Under Five Across LMICs
4. Discussion
4.2. Strengths and Limitation
4.3. Policy Implications
4.5. Future Directions
4.6. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
List of Abbreviations
| AFRO | African Region |
| AMRO/PAHO | Region of the Americas / Pan American Health Organization |
| ARR | Annual Rate of Change |
| CFM | Coexisting Forms of Malnutrition |
| COVID-19 | Coronavirus Disease 2019 |
| CSO | Coexistence of Stunting with Obesity |
| CSW / CWS | Coexistence of Stunting with Wasting / Coexistence of Wasting with Stunting |
| DHS | Demographic and Health Surveys |
| DRC | Democratic Republic of Congo |
| EMRO | Eastern Mediterranean Region |
| EURO | European Region |
| GBD | Global Burden of Disease |
| GLM/ GzLM | Generalised Linear Model |
| GNR | Global Nutritional Report |
| GNT | Global Nutrition Target |
| HAZ | Height-for-Age Z-score |
| JME | Joint Malnutrition Estimates |
| LICs | Low-Income Countries |
| LMICs | Low- and Middle-Income Countries |
| MDGs | Millennium Development Goals |
| MICS | Multiple Indicator Cluster Surveys |
| OR | Odds Ratio |
| PDHS | Pakistan Demographic and Health Surveys |
| SDGs | Sustainable Development Goals |
| SEARO | South-East Asia Region |
| SFM | Standalone Forms of Malnutrition |
| UHC | Universal Health Coverage |
| UICs | Upper Income Countries |
| UNICEF | United Nations Children's Fund |
| USAID | United States Agency for International Development |
| VIF | Variance Inflation Factor |
| WAZ | Weight-for-Age Z-score |
| WASH | Water, Sanitation and Hygiene |
| WHO | World Health Organization |
| WHZ | Weight-for-Height Z-score |
| WPRO | Western Pacific Region |
References
- Madewell, ZJ; Keita, AM; Das, PM; Mehta, A; Akelo, V; Oluoch, OB; et al. Contribution of malnutrition to infant and child deaths in Sub-Saharan Africa and South Asia. BMJ Glob Health 2024, 9(12). [Google Scholar] [CrossRef]
- Malnutrition [Internet] [Internet]. World Health Organization. 2024. Available online: https://www.who.int/news-room/fact-sheets/detail/malnutrition.
- Levels and Trends in Child Malnutrition: Key Findings of the 2023 [Internet]; World Health Organization, 2023; Available online: https://www.who.int/publications/i/item/9789240073.
- Khaliq, A; Godil, MS; Taseen, S; Usmani, IA; Chowdhury, TS. Prevalence, Trends, and Determinants of Double Burden of Malnutrition Among the Mother-Child Dyads of Pakistan. Int J Pediatr. 2025, 2025, 8816802. [Google Scholar] [CrossRef]
- Silva, NJ; Paixao, ES; Brachowicz, N; Barreix, G; Landin-Basterra, E; Rubio, FA; et al. Early life exposure to economic shocks and association with childhood malnutrition: a pooled analysis of 230 nationwide surveys from 68 low-income and middle-income countries. Lancet Glob Health 2025, 13(8), e1367–e77. [Google Scholar] [CrossRef]
- Landin Basterra, E; Gentilini, U; Cavalcanti, DM; da Silva, AF; de Oliveira Ferreira de Sales, L; Silva, NJ; Rasella, D. Impact of social protection on child malnutrition and mortality across 46 LMICs: a longitudinal study over two decades with insights from the COVID-19 pandemic. EClinicalMedicine 2025, 87, 103414. [Google Scholar] [CrossRef]
- Escher, NA; Andrade, GC; Ghosh-Jerath, S; Millett, C; Seferidi, P. The effect of nutrition-specific and nutrition-sensitive interventions on the double burden of malnutrition in low-income and middle-income countries: a systematic review. Lancet Glob Health 2024, 12(3), e419–e32. [Google Scholar] [CrossRef]
- de Hoop, T; Molotsky, A; Walcott, R; Gaitan-Rossi, P; Hernandez-Cordero, S; Laar, A; et al. The role of nutrition-sensitive interventions in improving nutritional outcomes: findings from a systematic review and meta-analysis. Int J Equity Health 2025, 24(1), 325. [Google Scholar] [CrossRef]
- Oruamabo, RS. Child malnutrition and the Millennium Development Goals: much haste but less speed? Arch Dis Child. 2015, 100 Suppl, S19–22. [Google Scholar] [CrossRef]
- Minna Sabbahi, Jiewen Li, Claire Davis, Downs SM. The Role of the Sustainable Development Goals to Reduce the Global Burden of Malnutrition. Advances in Food Security and Sustainability 2018, 3, 277–333.
- GNT, C. Global, regional, and national progress towards the 2030 GNTs and forecasts to 2050: a systematic analysis for the Global Burden of Disease Study 2021. Lancet 2025, 404(10471), 2543–83. [Google Scholar]
- Local Burden of Disease Child Growth Failure C. Mapping child growth failure across low- and middle-income countries. Nature 2020, 577(7789), 231–4. [CrossRef]
- GNTs 2030 to improve maternal, infant and young child nutrition. [Internet]. 2023. Available online: https://www.who.int/publications/m/item/global-nutrition-targets-2030.
- Description of The DHS Program. Rockville (MD): The DHS Program [Internet]. The DHS Program. Available online: https://dhsprogram.com/data/Guide-to-DHS-Statistics/Description_of_The_Demographic_and_Health_Surveys_Program.htm.
- DHS Recode Manual. Rockville (MD): The DHS Program [Internet]. Available online: https://dhsprogram.com/publications/publication-dhsg4-dhs-questionnaires-and-manuals.cfm.
- MICS — Multiple Indicator Cluster Surveys. [Internet]. 2025. Available online: https://mics.unicef.org/](https://mics.unicef.org/.
- WHO regional offices and regions. [Internet]. World Health Organization. Available online: https://www.who.int/about/who-we-are/regional-offices.
- World Bank country and lending groups (for income classification). [Internet]. Available online: https://datahelpdesk.worldbank.org/knowledgebase/articles/906519-world-bank-country-and-lending-groups.
- Khaliq, A; Ashar, B; Rehman, HA; Junaid, M; Rizwan, Y; Aijaz, N; et al. Global, regional and national estimates of coexisting forms of malnutrition among the neonates, infants and young children - A secondary data analysis of Demographic & Health Surveys (DHS) from 2006 to 2024. F1000Res 2025, 14, 1414. [Google Scholar]
- Stunting in a Nutshell [Internet]. World Health Organization, 2015. Available online: https://www.who.int/news/item/19-11-2015-stunting-in-a-nutshell.
- Daley, SF; Balasundaram, P. Obesity in Pediatric Patients; StatPearls: Treasure Island (FL), 2025. [Google Scholar]
- Khaliq, A; Wraith, D; Nambiar, S; Miller, Y. A review of the prevalence, trends, and determinants of coexisting forms of malnutrition in neonates, infants, and children. BMC Public Health 2022, 22(1), 879. [Google Scholar] [CrossRef]
- Khaliq, A. Determinants and distribution of coexisting forms of malnutrition among neonates, infants and children of Pakistan Queensland University of Technology; 2023. [Google Scholar]
- Headey, D; Heidkamp, R; Osendarp, S; Ruel, M; Scott, N; Black, R; et al. Impacts of COVID-19 on childhood malnutrition and nutrition-related mortality. Lancet 2020, 396(10250), 519–21. [Google Scholar] [CrossRef]
- Roberton, T; Carter, ED; Chou, VB; Stegmuller, AR; Jackson, BD; Tam, Y; et al. Early estimates of the indirect effects of the COVID-19 pandemic on maternal and child mortality in low-income and middle-income countries: a modelling study. Lancet Glob Health 2020, 8(7), e901–e8. [Google Scholar] [CrossRef]
- The Extension of the 2025 Maternal, Infant and Young Child Nutrition Targets to 2030 [Internet]. WHO/UNICEF. 2019. Available online: https://data.unicef.org/resources/who-unicef-discussion-paper-nutrition-targets/.
- Improving Resilience to Weather Shocks and Climate Change [Internet]. 2024. Available online: https://hdl.handle.net/10986/42793.
- Global Report on Food Crises (GRFC) 2025 [Internet]. FSIN and Global Network Against Food Crises. 2025. Available online: https://www.wfp.org/publications/global-report-food-crises-grfc.
- Gillespie, S; Haddad, L; Mannar, V; Menon, P; Nisbett, N; Maternal; Child Nutrition Study, G. The politics of reducing malnutrition: building commitment and accelerating progress. Lancet 2013, 382(9891), 552–69. [Google Scholar] [CrossRef]
- UNICEF Conceptual Framework on Maternal and Child Nutrition [Internet]. 2021. Available online: https://www.unicef.org/documents/conceptual-framework-nutrition.
- Global action plan on child wasting: a framework for action to accelerate progress in preventing and managing child wasting and the achievement of the Sustainable Development Goals [Internet]. World Health Organization, 2020. Available online: https://www.who.int/publications/m/item/global-action-plan-on-child-wasting-a-framework-for-action.
- Swinburn, BA; Kraak, VI; Allender, S; Atkins, VJ; Baker, PI; Bogard, JR; et al. The Global Syndemic of Obesity, Undernutrition, and Climate Change: The Lancet Commission report. Lancet 2019, 393(10173), 791–846. [Google Scholar] [CrossRef]
- Jamison, DT; Summers, LH; Alleyne, G; Arrow, KJ; Berkley, S; Binagwaho, A; et al. Global health 2035: a world converging within a generation. Lancet 2013, 382(9908), 1898–955. [Google Scholar] [CrossRef]
- The state of global nutrition [Internet]. 2021. Available online: https://globalnutritionreport.org/reports/2021-global-nutrition-report/.
- Hawkes, C; Ruel, MT; Salm, L; Sinclair, B; Branca, F. Double-duty actions: seizing programme and policy opportunities to address malnutrition in all its forms. Lancet 2020, 395(10218), 142–55. [Google Scholar] [CrossRef]
- Popkin, BM; Corvalan, C; Grummer-Strawn, LM. Dynamics of the double burden of malnutrition and the changing nutrition reality. Lancet 2020, 395(10217), 65–74. [Google Scholar] [CrossRef]
- Monteiro, CA; Moubarac, JC; Cannon, G; Ng, SW; Popkin, B. Ultra-processed products are becoming dominant in the global food system. Obes Rev. 2013, 14 2 Suppl, 21–8. [Google Scholar] [CrossRef]
- Black, RE; Victora, CG; Walker, SP; Bhutta, ZA; Christian, P; de Onis, M; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382(9890), 427–51. [Google Scholar] [CrossRef]
- de Pee, S; Bloem, MW. Current and potential role of specially formulated foods and food supplements for preventing malnutrition among 6- to 23-month-old children and for treating moderate malnutrition among 6- to 59-month-old children. Food Nutr Bull. 2009, 30((3) Suppl, S434–63. [Google Scholar] [CrossRef]
- Akseer, N; Bhatti, Z; Rizvi, A; Salehi, AS; Mashal, T; Bhutta, ZA. Coverage and inequalities in maternal and child health interventions in Afghanistan. BMC Public Health 2016, 16 Suppl 2(Suppl 2), 797. [Google Scholar] [CrossRef]
- Musaiger, AO. Overweight and obesity in eastern mediterranean region: prevalence and possible causes. J Obes. 2011, 2011, 407237. [Google Scholar] [CrossRef]
- Spears, D; Ghosh, A; Cumming, O. Open defecation and childhood stunting in India: an ecological analysis of new data from 112 districts. PLoS One 2013, 8(9), e73784. [Google Scholar] [CrossRef]
- Collaborators GBDD. Health effects of dietary risks in 195 countries, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2019, 393(10184), 1958–72. [CrossRef]
- Jomaa, L; Naja, F; Cheaib, R; Hwalla, N. Household food insecurity is associated with a higher burden of obesity and risk of dietary inadequacies among mothers in Beirut, Lebanon. BMC Public Health 2017, 17(1), 567. [Google Scholar] [CrossRef]
- Derek Headey, DS; You, Liangzhi; Guo, Zhe. Remoteness, urbanization, and child nutrition in sub-Saharan Africa. Agricultural Economics 2018, 49(6), 765–75. [Google Scholar] [CrossRef]
- Victora, CG; de Onis, M; Hallal, PC; Blossner, M; Shrimpton, R. Worldwide timing of growth faltering: revisiting implications for interventions. Pediatrics 2010, 125(3), e473-80. [Google Scholar] [CrossRef]
- Dassie, GA; Chala Fantaye, T; Charkos, TG; Sento Erba, M; Balcha Tolosa, F. Factors influencing concurrent wasting, stunting, and underweight among children under five who suffered from severe acute malnutrition in low- and middle-income countries: a systematic review. Front Nutr. 2024, 11, 1452963. [Google Scholar] [CrossRef]
- Rezaeizadeh, G; Mansournia, MA; Keshtkar, A; Farahani, Z; Zarepour, F; Sharafkhah, M; et al. Maternal education and its influence on child growth and nutritional status during the first two years of life: a systematic review and meta-analysis. EClinicalMedicine 2024, 71, 102574. [Google Scholar] [PubMed]
- Katoch, OR. Determinants of malnutrition among children: A systematic review. Nutrition 2022, 96, 111565. [Google Scholar] [CrossRef] [PubMed]
- Birhanu, F; Yitbarek, K; Bobo, FT; Atlantis, E; Woldie, M. Undernutrition in children under five associated with wealth-related inequality in 24 low- and middle-income countries from 2017 to 2022. Sci Rep. 2024, 14(1), 3326. [Google Scholar] [PubMed]
- Caleyachetty, R; Kumar, NS; Bekele, H; Manaseki-Holland, S. Socioeconomic and urban-rural inequalities in the population-level double burden of child malnutrition in the East and Southern African Region. PLOS Glob Public Health 2023, 3(4), e0000397. [Google Scholar] [CrossRef]
- Popkin, BM; Ng, SW. The nutrition transition to a stage of high obesity and noncommunicable disease prevalence dominated by ultra-processed foods is not inevitable. Obes Rev. 2022, 23(1), e13366. [Google Scholar] [CrossRef]
- Prentice, AM; Ward, KA; Goldberg, GR; Jarjou, LM; Moore, SE; Fulford, AJ; Prentice, A. Critical windows for nutritional interventions against stunting. Am J Clin Nutr. 2013, 97(5), 911–8. [Google Scholar] [CrossRef]
- Harvey, CA; Rakotobe, ZL; Rao, NS; Dave, R; Razafimahatratra, H; Rabarijohn, RH; et al. Extreme vulnerability of smallholder farmers to agricultural risks and climate change in Madagascar. Philos Trans R Soc Lond B Biol Sci. 2014, 369(1639), 20130089. [Google Scholar]

| Survey period | Stunting | Wasting | Obesity | ||||
|---|---|---|---|---|---|---|---|
| Prevalence | Status | Prevalence | Status | Prevalence | Status | ||
| African Region (AFRO) | |||||||
| Benin | 2012 | 44.6 | ↓ | 26.1 | ↓ | 9 | ↓ |
| 2018 | 32.7 | 5.3 | 3.8 | ||||
| 2030 | 17.6 | 0.2 | 0.7 | ||||
| Burundi | 2010 | 55.7 | ↑ | 5.3 | ↓ | 5.4 | ↑ |
| 2016 | 55.2 | 3.4 | 5.4 | ||||
| 2030 | 54.1 | 1.2 | 5.4 | ||||
| Burkina Faso | 2014 | 35.2 | ↓ | 12.9 | ↓ | 6.4 | ↓ |
| 2021 | 22.4 | 9.3 | 3.8 | ||||
| 2030 | 13.3 | 6.1 | 1.9 | ||||
| Cameron | 2011 | 32.7 | ↓ | 7.1 | ↑ | 6.6 | ↑ |
| 2022 | 29.2 | 7.9 | 8.3 | ||||
| 2030 | 27.8 | 8.5 | 9.8 | ||||
| Chad | 2010 | 40.1 | ↓ | 9.8 | ↓ | 6.3 | ↑ |
| 2019 | 31.9 | 12.4 | 7.7 | ||||
| 2030 | 25.9 | 16.4 | 9.8 | ||||
| Comoros | 2012 | 28.6 | ↓ | 15.4 | ↓ | 6.8 | ↓ |
| 2022 | 16.9 | 4 | 0.8 | ||||
| 2030 | 12.9 | 1.4 | 0.1 | ||||
| Congo | 2012 | 31.1 | ↓ | 7.8 | ↓ | 4.3 | ↓ |
| 2015 | 21 | 6 | 2.2 | ||||
| 2030 | 4.7 | 1.6 | 0.1 | ||||
| Cote de Ivore | 2012 | 44.9 | ↓ | 9 | ↑ | 6.3 | ↑ |
| 2021 | 37.5 | 10.2 | 5.8 | ||||
| 2030 | 30.5 | 11.6 | 5.3 | ||||
|
DRC |
2010 | 27.1 | ↓ | 11.7 | ↓ | 4.6 | ↓ |
| 2018 | 19.7 | 5.6 | 3.3 | ||||
| 2030 | 12.4 | 1.9 | 2 | ||||
|
Eswatini |
2010 | 28.4 | ↓ | 11.1 | ↓ | 4.9 | ↓ |
| 2022 | 19.9 | 5.7 | 3.8 | ||||
| 2030 | 14.6 | 3.7 | 3.2 | ||||
| Ethiopia | 2011 | 32.2 | ↓ | 10.2 | ↑ | 5.3 | ↓ |
| 2016 | 32 | 11.2 | 4.8 | ||||
| 2030 | 31.5 | 14.6 | 3.6 | ||||
|
Gambia |
2013 | 26.7 | ↓ | 3.7 | ↓ | 2.1 | ↓ |
| 2020 | 26.9 | 3.1 | 1.8 | ||||
| 2030 | 27.4 | 2.4 | 1.4 | ||||
|
Ghana |
2014 | 34.8 | ↓ | 9.6 | ↓ | 5.3 | ↓ |
| 2022 | 18.4 | 7.4 | 4.4 | ||||
| 2030 | 10.6 | 5.7 | 3.7 | ||||
| Guinea | 2012 | 40.5 | ↓ | 7.7 | ↓ | 5.8 | ↑ |
| 2018 | 38.4 | 4.4 | 5.9 | ||||
| 2030 | 34.9 | 1.4 | 6.1 | ||||
|
Guinea-Bissau |
2014 | 32.1 | ↑ | 7.7 | ↓ | 4.1 | ↑ |
| 2019 | 33.1 | 5.8 | 5 | ||||
| 2030 | 35.7 | 3.1 | 7.7 | ||||
|
Kenya |
2014 | 48.9 | ↓ | 8 | ↑ | 8.1 | ↓ |
| 2022 | 39.6 | 6.4 | 4.6 | ||||
| 2030 | 33.5 | 5.1 | 2.6 | ||||
| Lesotho | 2014 | 47.2 | ↓ | 9 | ↓ | 5.1 | ↓ |
| 2024 | 36.1 | 5.3 | 4.1 | ||||
| 2030 | 30.9 | 3.9 | 3.6 | ||||
|
Liberia |
2013 | 38.7 | ↓ | 11 | ↓ | 5.5 | ↓ |
| 2020 | 27.9 | 9 | 4.6 | ||||
| 2030 | 17.5 | 6.8 | 3.6 | ||||
|
Madagascar |
2009 | 27 | ↓ | 9.3 | ↑ | 4.1 | ↑ |
| 2021 | 25.8 | 10.5 | 4.3 | ||||
| 2030 | 25 | 11.5 | 4.5 | ||||
| Malawi | 2010 | 40.3 | ↓ | 9.4 | ↓ | 5.6 | ↓ |
| 2016 | 33.9 | 4.5 | 4.2 | ||||
| 2030 | 29.2 | 0.8 | 2.1 | ||||
| Mali | 2013 | 43.2 | ↓ | 16.9 | ↓ | 8.1 | ↓ |
| 2018 | 37.2 | 5.6 | 5.1 | ||||
| 2030 | 35 | 0.4 | 1.7 | ||||
| Mauritania | 2011 | 41 | ↑ | 5.4 | ↓ | 2.7 | ↓ |
| 2015 | 43.2 | 4.3 | 2.8 | ||||
| 2030 | 49.4 | 1.8 | 3.2 | ||||
| Mozambique | 2011 | 28.1 | ↓ | 6.9 | ↑ | 3.8 | ↓ |
| 2023 | 25.6 | 6.1 | 2 | ||||
| 2030 | 24.9 | 5.7 | 1.4 | ||||
| Nigeria | 2013 | 44.5 | ↓ | 6.3 | ↓ | 5.4 | ↓ |
| 2018 | 34.7 | 4 | 4.8 | ||||
| 2030 | 21.9 | 1.3 | 3.6 | ||||
| Rwanda | 2013 | 17 | ↓ | 2.9 | ↑ | 1.2 | ↓ |
| 2020 | 13.2 | 3.5 | 0.7 | ||||
| 2030 | 9.42 | 4.6 | 0.3 | ||||
|
Sao Tome & Principe |
2014 | 21.5 | ↓ | 8.9 | ↑ | 4.2 | ↑ |
| 2019 | 20.5 | 9.5 | 4.2 | ||||
| 2030 | 19 | 11.1 | 4.2 | ||||
| Senegal | 2011 | 35.2 | ↓ | 14.8 | ↓ | 7.1 | ↓ |
| 2023 | 31.6 | 6.8 | 5.4 | ||||
| 2030 | 30.3 | 4.3 | 4.6 | ||||
| Sierra Leone | 2013 | 30.2 | ↓ | 0.5 | ↑ | 0.3 | ↑ |
| 2019 | 20.2 | 1.4 | 0.4 | ||||
| 2030 | 11.38 | 4.5 | 0.7 | ||||
| Togo | 2010 | 33.7 | ↓ | 2.6 | ↑ | 3 | ↓ |
| 2017 | 24.6 | 3.8 | 2 | ||||
| 2030 | 17.34 | 5.7 | 0.9 | ||||
| Uganda | 2011 | 33.5 | ↓ | 6.6 | ↓ | 4.8 | ↓ |
| 2019 | 29.5 | 5.2 | 4.1 | ||||
| 2030 | 25.3 | 3.8 | 3.3 | ||||
| Zambia | 2013 | 40.4 | ↓ | 9.1 | ↓ | 4.6 | ↓ |
| 2018 | 35.5 | 7 | 4.2 | ||||
| 2030 | 29 | 4.4 | 3.4 | ||||
| Zimbabwe | 2011 | 32.6 | ↑ | 6.2 | ↑ | 4.6 | ↑ |
| 2015 | 36.6 | 6.7 | 5.2 | ||||
| 2030 | 56.6 | 8.8 | 8.2 | ||||
| American Region (AMRO) | |||||||
| Haiti | 2012 | 23.7 | ↓ | 6.2 | ↓ | 4.2 | ↓ |
| 2017 | 22.9 | 5.4 | 3.7 | ||||
| 2030 | 21.3 | 3.77 | 2.7 | ||||
| Honduras | 2012 | 27 | ↓ | 3.1 | ↓ | 5.4 | ↓ |
| 2019 | 19.8 | 1.3 | 0.5 | ||||
| 2030 | 12.9 | 0.5 | 0.1 | ||||
| Eastern Mediterranean Region (EMRO) | |||||||
|
Egypt |
2008 |
29.4 |
↓ |
17.7 |
↑ |
9 |
↓ |
| 2014 | 21 | 17.2 | 7.3 | ||||
| 2030 | 9.3 | 30.5 | 4.2 | ||||
| Jordan | 2012 | 8.8 | ↓ | 3 | ↑ | 4.3 | ↑ |
| 2023 | 9.3 | 4.6 | 7 | ||||
| 2030 | 10.66 | 6.6 | 9.5 | ||||
| Pakistan | 2012 | 45.2 | ↓ | 11.1 | ↓ | 6.3 | ↓ |
| 2017 | 38.5 | 6.9 | 4.2 | ||||
| 2030 | 30.9 | 3.6 | 1.5 | ||||
| Palestine | 2010 | 11 | ↓ | 4.4 | ↓ | 4.2 | ↑ |
| 2020 | 8.8 | 3 | 8.2 | ||||
| 2030 | 7.23 | 2.4 | 16.1 | ||||
| Sudan | 2010 | 35.8 | ↑ | 9.9 | ↓ | 6.3 | ↑ |
| 2014 | 39.8 | 8.7 | 6.7 | ||||
| 2030 | 61.3 | 5.2 | 8.6 | ||||
| Tunisia | 2011 | 10.5 | ↑ | 2.3 | ↑ | 0.2 | ↑ |
| 2023 | 12.6 | 2.9 | 0.2 | ||||
| 2030 | 14 | 3.3 | 0.2 | ||||
| Yemen | 2013 | 46.8 | ↑ | 12.1 | ↓ | 7.7 | ↑ |
| 2023 | 48.8 | 9.5 | 8.9 | ||||
| 2030 | 51.4 | 8.7 | 9.8 | ||||
| European Region (EURO) | |||||||
| Kyrgyzstan | 2014 | 13.2 | ↓ | 2 | ↑ | 0.2 | ↓ |
| 2018 | 10.8 | 2 | 0 | ||||
| 2030 | 6.2 | 2 | 0 | ||||
|
Tajikistan |
2012 | 26.2 | ↓ | 12.9 | ↓ | 4.3 | ↓ |
| 2017 | 19.6 | 8.6 | 3.4 | ||||
| 2030 | 9.4 | 3 | 1.8 | ||||
| Southeast Asian Region (SEARO) | |||||||
|
Bangladesh |
2011 |
41.5 |
↓ |
10.2 |
↑ |
8.6 |
↓ |
| 2022 | 24.5 | 9.5 | 5.2 | ||||
| 2030 | 16.7 | 9.1 | 3.6 | ||||
| India | 2015 | 39.4 | ↓ | 16.2 | ↑ | 8 | ↓ |
| 2021 | 36.8 | 16.7 | 6.8 | ||||
| 2030 | 34.7 | 18.4 | 5.3 | ||||
| Nepal | 2011 | 42.9 | ↓ | 7.8 | ↓ | 5.6 | ↓ |
| 2022 | 28.4 | 5.8 | 4.5 | ||||
| 2030 | 21 | 4.7 | 3.8 | ||||
|
Timor-Leste |
2010 | 57.9 | ↓ | 16.3 | ↑ | 8.9 | ↑ |
| 2016 | 47.4 | 20.4 | 10.1 | ||||
| 2030 | 32.2 | 35.2 | 13.6 | ||||
| Western Pacific Region (WPRO) | |||||||
| Laos | 2012 | 46.2 | ↓ | 3.6 | ↑ | 3 | ↑ |
| 2017 | 33.3 | 7.4 | 3.1 | ||||
| 2030 | 19.5 | 48.6 | 3.4 | ||||
| Survey period | Malnutrition | Stunting | Wasting | Obesity | CSO | CWS | |
|---|---|---|---|---|---|---|---|
| Prevalence | Prevalence | Prevalence | Prevalence | Prevalence | Prevalence | ||
| Benin | 2012 | 62.7 | 27.6 | 13.3 | 4.8 | 4.2 | 12.8 |
| 2018 | 38.5 | 29.4 | 4.6 | 1.2 | 2.6 | 0.7 | |
| 2030 | 35.4 | 33.4 | 0.6 | 0.4 | 1 | 0 | |
| Burundi | 2010 | 59.9 | 49.2 | 3.3 | 0.9 | 4.5 | 2 |
| 2016 | 58.6 | 49.8 | 2.6 | 0.8 | 4.6 | 0.8 | |
| 2030 | 58.3 | 51.0 | 1.8 | 0.6 | 4.8 | 0.1 | |
| Burkina Faso | 2014 | 47.8 | 28.5 | 11.5 | 1.1 | 5.3 | 1.4 |
| 2021 | 31.7 | 18.6 | 8.5 | 0.8 | 3 | 0.8 | |
| 2030 | 19.6 | 11.5 | 5.8 | 0.5 | 1.4 | 0.4 | |
| Cameron | 2011 | 41.1 | 27.4 | 4.5 | 3.9 | 2.7 | 2.6 |
| 2022 | 39.6 | 23.4 | 3.7 | 6.7 | 1.6 | 4.2 | |
| 2030 | 41 | 20.8 | 3.2 | 10 | 1.1 | 5.9 | |
| Chad | 2010 | 49.9 | 33.8 | 9.8 | 0 | 6.3 | 0 |
| 2019 | 44.3 | 24.2 | 12.4 | 0 | 7.7 | 0 | |
| 2030 | 33.5 | 16.1 | 7.6 | 0 | 9.8 | 0 | |
| Comoros | 2012 | 43.6 | 21.4 | 10.8 | 4.2 | 2.6 | 4.6 |
| 2022 | 20.9 | 16.1 | 4 | 0.0 | 0.8 | 0 | |
| 2030 | 14.5 | 12.6 | 1.6 | 0 | 0.3 | 0 | |
| Congo | 2012 | 39.1 | 27 | 6.4 | 1.6 | 2.7 | 1.4 |
| 2015 | 27 | 18.8 | 6 | 0 | 2.2 | 0 | |
| 2030 | 9.3 | 3.9 | 4.6 | 0 | 0.8 | 0 | |
| Cote de Ivore | 2012 | 53.9 | 38.6 | 8.1 | 0.9 | S | 0.9 |
| 2021 | 47.9 | 31.9 | 9.2 | 1.2 | 4.6 | 1 | |
| 2030 | 43.2 | 25.5 | 11.1 | 1.6 | 3.9 | 1.1 | |
| DRC |
2010 | 38.2 | 21.9 | 10 | 1.1 | 3.5 | 1.7 |
| 2018 | 26.5 | 17.6 | 5.3 | 1.5 | 1.8 | 0.3 | |
| 2030 | 17.2 | 11.8 | 2.4 | 2.4 | 0.6 | 0 | |
| Eswatini |
2010 | 39.8 | 23.8 | 8.8 | 2.6 | 2.3 | 2.3 |
| 2022 | 26.7 | 17.2 | 5.3 | 1.5 | 2.3 | 0.4 | |
| 2030 | 18.9 | 12.2 | 3.3 | 1 | 2.3 | 0.1 | |
| Ethiopia | 2011 | 42.6 | 27.1 | 8.5 | 1.9 | 3.4 | 1.7 |
| 2016 | 42.1 | 26.1 | 7.9 | 2.2 | 2.6 | 3.3 | |
| 2030 | 55 | 23.5 | 6.7 | 3.3 | 1.2 | 20.3 | |
| Gambia |
2013 | 30.4 | 24.6 | 3.7 | 0 | 2.1 | 0 |
| 2020 | 30 | 25.1 | 3.1 | 0 | 1.8 | 0 | |
| 2030 | 29.9 | 26.0 | 2.5 | 0 | 1.4 | 0 | |
| Ghana |
2014 | 44.2 | 29.3 | 6.9 | 2.5 | 2.8 | 2.7 |
| 2022 | 27.3 | 15.5 | 6.8 | 2.1 | 2.3 | 0.6 | |
| 2030 | 19 | 8.6 | 6.7 | 1.7 | 1.9 | 0.1 | |
| Guinea | 2012 | 49 | 35.5 | 4.4 | 4.1 | 1.7 | 3.3 |
| 2018 | 44.5 | 34.2 | 1.9 | 4.2 | 1.7 | 2.5 | |
| 2030 | 40 | 31.8 | 0.7 | 4.4 | 1.7 | 1.4 | |
| Guinea-Bissau |
2014 | 40 | 28.2 | 6.3 | 1.6 | 2.5 | 1.4 |
| 2019 | 39.8 | 29 | 4.1 | 2.6 | 2.4 | 1.7 | |
| 2030 | 46 | 30.9 | 2.9 | 7.4 | 2.2 | 2.6 | |
| Kenya |
2014 | 53.9 | 37.8 | 3.9 | 1.1 | 7 | 4.1 |
| 2022 | 45.9 | 34.9 | 5.4 | 0.9 | 3.7 | 1 | |
| 2030 | 41.7 | 31.4 | 7.5 | 0.7 | 1.9 | 0.2 | |
| Lesotho | 2014 | 54 | 39.9 | 3.9 | 2.9 | 2.2 | 5.1 |
| 2024 | 41.8 | 32.4 | 3.3 | 2.4 | 1.7 | 2 | |
| 2030 | 35.9 | 28.4 | 2.9 | 2.1 | 1.4 | 1.1 | |
| Liberia |
2013 | 49.1 | 32.6 | 9.6 | 0.8 | 4.7 | 1.4 |
| 2020 | 36.7 | 23.1 | 7.8 | 1 | 3.6 | 1.2 | |
| 2030 | 25 | 14.2 | 6.1 | 1.4 | 2.4 | 0.9 | |
| Madagascar |
2009 | 36.3 | 22.9 | 9.3 | 0 | 4.1 | 0 |
| 2021 | 36.3 | 21.5 | 10.5 | 0 | 4.3 | 0 | |
| 2030 | 37.1 | 20.5 | 12.1 | 0 | 4.5 | 0 | |
| Malawi | 2010 | 48.6 | 33.6 | 4.9 | 3.4 | 2.2 | 4.5 |
| 2016 | 39.2 | 30.5 | 3.1 | 2.2 | 2 | 1.4 | |
| 2030 | 31.8 | 27.5 | 1.9 | 0.7 | 1.6 | 0.1 | |
| Mali | 2013 | 57.4 | 32.4 | 11 | 3.2 | 4.9 | 5.9 |
| 2018 | 43.2 | 32.5 | 4.8 | 1.2 | 3.9 | 0.8 | |
| 2030 | 36.8 | 32.8 | 1.7 | 0.1 | 2.2 | 0 | |
| Mauritania | 2011 | 46.4 | 38.3 | 5.4 | 0 | 2.7 | 0 |
| 2015 | 47.5 | 40.4 | 4.3 | 0 | 2.8 | 0 | |
| 2030 | 55.4 | 49.3 | 2.9 | 0 | 3.2 | 0 | |
| Mozambique | 2011 | 35.4 | 24.7 | 5.4 | 1.9 | 1.9 | 1.5 |
| 2023 | 31.7 | 23.6 | 6.1 | 0 | 2 | 0.0 | |
| 2030 | 31.5 | 22.9 | 6.6 | 0 | 2 | 0 | |
| Nigeria | 2013 | 50.6 | 38.9 | 2.7 | 3.4 | 2 | 3.6 |
| 2018 | 40.4 | 31.6 | 2 | 3.7 | 1.1 | 2.0 | |
| 2030 | 27.7 | 21.2 | 1.3 | 4.5 | 0.2 | 0.5 | |
| Rwanda | 2013 | 19.9 | 15.8 | 2.9 | 0 | 1.2 | 0 |
| 2020 | 16.7 | 12.5 | 3.5 | 0 | 0.7 | 0 | |
| 2030 | 14.02 | 9.1 | 4.6 | 0 | 0.32 | 0 | |
| Sao Tome & Principe | 2014 | 31.2 | 18.1 | 8.6 | 1.1 | 3.1 | 0.3 |
| 2019 | 30.6 | 16.9 | 9.3 | 0.8 | 3.4 | 0.2 | |
| 2030 | 30.4 | 14.8 | 11.0 | 0.4 | 4.1 | 0.1 | |
| Senegal | 2011 | 49 | 27.1 | 9.6 | 4.2 | 2.9 | 5.2 |
| 2023 | 38.9 | 26.7 | 4.7 | 2.6 | 2.8 | 2.1 | |
| 2030 | 34.8 | 26.4 | 2.6 | 1.9 | 2.7 | 1.2 | |
| Sierra Leone | 2013 | 30.7 | 29.9 | 0.5 | 0 | 0.3 | 0 |
| 2019 | 21.6 | 19.8 | 1.4 | 0 | 0.4 | 0 | |
| 2030 | 15.88 | 10.8 | 4.5 | 0 | 0.58 | 0 | |
| Togo | 2010 | 36.3 | 30.7 | 2.6 | 0 | 3 | 0 |
| 2017 | 28.4 | 22.6 | 3.8 | 0 | 2 | 0 | |
| 2030 | 23.04 | 16.4 | 5.7 | 0 | 0.94 | 0 | |
| Uganda | 2011 | 40.5 | 29.1 | 4.8 | 2.2 | 2.6 | 1.8 |
| 2019 | 36 | 26.7 | 3.9 | 2.6 | 1.5 | 1.3 | |
| 2030 | 31.5 | 23.8 | 3 | 3.2 | 0.7 | 0.8 | |
| Zambia | 2013 | 48.7 | 35 | 5.8 | 2.5 | 2.1 | 3.3 |
| 2018 | 42.5 | 31.3 | 4.4 | 2.6 | 1.6 | 2.6 | |
| 2030 | 34.8 | 26.8 | 3 | 2.8 | 0.8 | 1.4 | |
| Zimbabwe | 2011 | 39.6 | 28.8 | 3.8 | 3.2 | 1.4 | 2.4 |
| 2015 | 44.8 | 32.9 | 4.3 | 3.9 | 1.3 | 2.4 | |
| 2030 | 68.3 | 50.3 | 6.4 | 8.2 | 1.0 | 2.4 | |
| Haiti | 2012 | 30.9 | 20.5 | 4.9 | 2.3 | 1.9 | 1.3 |
| 2017 | 29.4 | 20.3 | 4.2 | 2.3 | 1.4 | 1.2 | |
| 2030 | 26.4 | 19.7 | 2.8 | 2.3 | 0.63 | 0.97 | |
| Honduras | 2012 | 33.5 | 25.0 | 2.3 | 4.2 | 1.2 | 0.8 |
| 2019 | 21.1 | 19.3 | 1.3 | 0 | 0.5 | 0 | |
| 2030 | 13.4 | 12.8 | 0.5 | 0 | 0.1 | 0 | |
| Egypt | 2008 | 45 | 18.3 | 7.5 | 8.1 | 0.9 | 10.2 |
| 2014 | 38.1 | 13.6 | 10.8 | 6.3 | 1 | 6.4 | |
| 2030 | 41.2 | 6.2 | 28.7 | 3.2 | 1.3 | 1.8 | |
| Jordan | 2012 | 15 | 7.7 | 2.1 | 4.1 | 0.2 | 0.9 |
| 2023 | 18.5 | 6.9 | 2.3 | 6.9 | 0.1 | 2.3 | |
| 2030 | 22.66 | 6.4 | 2.4 | 9.6 | 0.06 | 4.2 | |
| Pakistan | 2012 | 52.8 | 35.4 | 5.9 | 1.7 | 4.6 | 5.2 |
| 2017 | 44.9 | 33.8 | 5.1 | 1.3 | 2.9 | 1.8 | |
| 2030 | 35 | 29.9 | 3.5 | 0.6 | 0.9 | 0.1 | |
| Palestine | 2010 | 17.8 | 9.2 | 2.9 | 3.9 | 0.3 | 1.5 |
| 2020 | 18.3 | 7.1 | 1.4 | 8.1 | 0.1 | 1.6 | |
| 2030 | 25.53 | 5.5 | 0.7 | 17.6 | 0.03 | 1.7 | |
| Sudan | 2010 | 45.7 | 29.5 | 9.9 | 0 | 6.3 | 0 |
| 2014 | 48.5 | 33.1 | 8.7 | 0 | 6.7 | 0 | |
| 2030 | 66.5 | 52.7 | 5.2 | 0 | 8.6 | 0 | |
| Tunisia | 2011 | 12.8 | 10.3 | 2.3 | 0 | 0.2 | 0 |
| 2023 | 15.5 | 12.4 | 2.9 | 0 | 0.2 | 0 | |
| 2030 | 17.3 | 13.8 | 3.3 | 0 | 0.2 | 0 | |
| Yemen | 2013 | 58.2 | 38.4 | 10.7 | 0.7 | 7 | 1.4 |
| 2023 | 58.3 | 39.9 | 9.5 | 0 | 8.9 | 0 | |
| 2030 | 60.1 | 40.9 | 8.7 | 0 | 10.5 | 0 | |
| Kyrgyzstan | 2014 | 15.2 | 13 | 2 | 0 | 0.2 | 0 |
| 2018 | 12.8 | 10.8 | 2 | 0 | 0 | 0 | |
| 2030 | 8.2 | 6.2 | 2 | 0 | 0 | 0 | |
| Tajikistan |
2012 | 38.6 | 21.4 | 10.0 | 2.4 | 1.9 | 2.9 |
| 2017 | 28.7 | 16.7 | 6.9 | 2.2 | 1.2 | 1.7 | |
| 2030 | 13.7 | 8.7 | 2.6 | 1.7 | 0.3 | 0.4 | |
| Bangladesh | 2011 | 51.9 | 33.1 | 9.5 | 0.9 | 7.7 | 0.7 |
| 2022 | 34.7 | 20.0 | 9.1 | 1.1 | 4.1 | 0.4 | |
| 2030 | 26.9 | 13.9 | 8.9 | 1.3 | 2.6 | 0.2 | |
| India | 2015 | 55 | 30.8 | 14.7 | 0.9 | 7.1 | 1.5 |
| 2021 | 52.5 | 29 | 14.4 | 1.3 | 5.5 | 2.3 | |
| 2030 | 50.8 | 26.5 | 13.9 | 2.2 | 3.7 | 4.5 | |
| Nepal | 2011 | 50.7 | 37.3 | 7.2 | 0.6 | 5.0 | 0.6 |
| 2022 | 35 | 24.7 | 5.6 | 1 | 3.5 | 0.2 | |
| 2030 | 27 | 18.2 | 4.6 | 1.4 | 2.7 | 0.1 | |
| Timor-Leste |
2010 | 71.7 | 46.5 | 12.9 | 0.9 | 8 | 3.4 |
| 2016 | 65.6 | 35.1 | 16.8 | 1.4 | 8.7 | 3.6 | |
| 2030 | 67.6 | 18.1 | 31.2 | 4.2 | 10.1 | 4.0 | |
| Laos | 2012 | 49.8 | 43.2 | 3.4 | 0.2 | 2.8 | 0.2 |
| 2017 | 40.7 | 30.2 | 6.9 | 0.5 | 2.6 | 0.5 | |
| 2030 | 68.1 | 11.9 | 43.1 | 5.5 | 2.1 | 5.5 |
| Variables | Stunting | Wasting | Obesity | CWS | CSO |
| Individual factors | |||||
| Age of child (in year) | 1.15 (1.14 to 1.15) * | 0.86 (0.86 to 0.87) * | 0.84 (0.83 to 0.85) * | 1.03 (1.02 to 1.03) * | 0.83 (0.82 to 0.84) * |
| Child sex: Female (reference) Male |
Ref 1.14 (1.13 to 1.15) * |
Ref 1.10 (1.08 to 1.11) * |
Ref 1.13 (1.09 to 1.16) * |
Ref 1.46 (1.43 to 1.48) * |
Ref 1.12 (1.08 to 1.15) * |
| Household factors | |||||
| Education: None Primary Secondary Higher (reference) |
2.19 (2.14 to 2.23) * 1.99 (1.94 to 2.03) * 1.41 (1.39 to 1.44) * Ref |
1.54 (1.50 to 1.59) * 1.19 (1.15 to 1.22) * 1.10 (1.07 to 1.12) * Ref |
0.79 (0.74 to 0.84) * 0.74 (0.69 to 0.78) * 0.71 (0.68 to 0.75) * Ref |
2.94 (2.79 to 3.09) * 2.21 (2.10 to 2.33) * 1.51 (1.44 to 1.59) * Ref |
1.41 (1.33 to 1.50) * 1.03 (0.96 to 1.09) 0.89 (0.84 to 0.94) * Ref |
| Wealth index Poorest Poorer Middle Richer Richest (reference) |
2.00 (1.96 to 2.04) * 1.73 (1.71 to 1.77) * 1.51 (1.48 to 1.54) * 1.27 (1.25 to 1.30) * Ref |
1.48 (1.26 to 1.73) * 1.24 (1.05 to 1.47) * 1.30 (1.10 to 1.54) * 1.20 (1.01 to 1.42) * Ref |
0.62 (0.59 to 0.69) * 0.68 (0.64 to 0.72) * 0.79 (0.75 to 0.83) * 0.82 (0.78 to 0.86) * Ref |
2.59 (2.48 to 2.70) * 1.95 (1.87 to 2.04) * 1.58 (1.51 to 1.65) * 1.29 (1.23 to 1.34) * Ref |
0.73 (0.44 to 1.21) 0.64 (0.37 to 1.11) 0.59 (0.33 to 1.05) 0.69 (0.40 to 1.18) Ref |
| Regional & Community factors | |||||
| Place of residence Rural Urban (reference) |
1.19 (1.17 to 1.21) * Ref |
1.04 (1.02 to 1.06) * Ref |
0.99 (0.95 to 1.03) Ref |
1.14 (1.11 to 1.17) * Ref |
1.13 (1.08 to 1.17) * Ref |
| Geographical regions AFRO AMRO EMRO EURO SEARO WPRO (reference) |
0.85 (0.83 to 0.87) * 0.52 (0.50 to 0.54) * 0.83 (0.81 to 0.86) * 0.49 (0.47 to 0.51) * 1.30 (1.27 to 1.34) * Ref |
1.24 (1.08 to 1.40) * 0.59 (0.46 to 0.75) * 1.73 (1.50 to 1.98) * 1.65 (1.39 to 1.97) * 3.65 (3.21 to 4.15) * Ref |
4.82 (3.99 to 5.84) * 6.00 (4.95 to 7.45) * 6.65 (5.49 to 8.06) * 3.00 (2.39 to 3.78) * 4.56 (3.76 to 5.51) * Ref |
1.05 (0.98 to 1.13) 0.32 (0.28 to 0.36) * 1.64 (1.51 to 1.76) * 0.36 (0.30 to 0.43) * 3.27 (3.05 to 3.51) * Ref |
2.70 (1.89 to 3.86) * 0.49 (0.24 to 1.04) 5.13 (3.58 to 7.36) * 3.90 (2.58 to 5.92) * 5.10 (3.59 to 7.28) * Ref |
| Temporal factor | |||||
| Year | 0.97 (0.97 to 0.98) * | 0.98 (0.98 to 0.98) * | 0.98 (0.97 to 0.98) * | 0.97 (0.97 to 0.97) * | 0.94 (0.94 to 0.94) * |
| Variables | Stunting | Wasting | Obesity | CWS | CSO |
| Individual factors | |||||
| Year * Age of child (in year) | 0.99 (0.99 to 0.99) * | 1.01 (1.01 to 1.01) * | 1.00 (0.99 to 1.00) | 0.99 (0.99 to 0.99) * | 0.98 (0.97 to 0.98) * |
| Child sex * Year Female (reference) Male |
Ref 0.99 (0.99 to 1.01) |
Ref 1.01 (0.99 to 1.01) |
Ref 1.00 (0.99 to 1.01) |
Ref 0.99 (0.99 to 1.00) |
Ref 1.01 (1.00 to 1.02) * |
| Household factors | |||||
| Education * Year None Primary Secondary Higher (reference) |
0.99 (0.99 to 1.00) 0.99 (0.98 to 0.99) * 0.99 (0.98 to 0.99) * Ref |
0.99 (0.98 to 0.99) * 0.99 (0.98 to 0.99) * 1.00 (0.99 to 1.01) Ref |
0.92 (0.90 to 0.93) * 0.99 (0.97 to 1.00) 1.00 (0.99 to 1.01) Ref |
0.95 (0.93 to 0.96) * 0.93 (0.92 to 0.95) * 0.98 (0.96 to 0.99) * Ref |
0.92 (0.91 to 0.94) * 0.98 (0.96 to 0.99) * 1.02 (1.01 to 1.04) * Ref |
| Wealth index * Year Poorest Poorer Middle Richer Richest (reference) |
0.98 (0.97 to 0.98) * 0.98 (0.97 to 0.98) * 0.98 (0.97 to 0.99) * 0.97 (0.96 to 0.97) * Ref |
1.01 (1.00 to 1.02) * 1.01 (0.99 to 1.01) 1.00 (0.99 to 1.01) * 1.00 (0.99 to 1.01) Ref |
0.98 (0.97 to 0.99) * 0.99 (0.98 to 1.01) 1.00 (0.99 to 1.01) 0.99 (0.98 to 1.00) Ref |
1.01 (0.99 to 1.05) 0.99 (0.99 to 1.00) 0.99 (0.99 to 1.00) 0.99 (0.99 to 1.00) Ref |
1.02 (1.01 to 1.04) * 1.01 (1.00 to 1.03) * 1.02 (1.00 to 1.03) * 1.00 (0.98 to 1.02) Ref |
| Regional & Community factors | |||||
| Place of residence * Year Rural Urban (reference) |
0.99 (0.99 to 1.00) Ref |
0.99 (0.99 to 1.00) Ref |
0.99 (0.99 to 1.00) Ref |
1.88 (1.88 to 1.89) * Ref |
1.01 (0.99 to 1.01) Ref |
| Geographical regions * Year AFRO AMRO EMRO EURO SEARO WPRO (reference) |
0.98 (0.97 to 0.99) * 1.02 (1.01 to 1.03) * 1.07 (1.06 to 1.08) * 0.97 (0.96 to 0.99) * 1.00 (0.99 to 1.01) Ref |
0.95 (0.94 to 0.97) * 0.97 (0.95 to 0.99) * 1.01 (0.99 to 1.02) 0.89 (0.88 to 0.92) * 0.99 (0.98 to 1.01) Ref |
1.10 (1.08 to 1.11) * 1.00 (0.98 to 1.02) * 1.07 (1.06 to 1.09) * 1.06 (1.03 to 1.10) * 1.13 (1.11 to 1.14) * Ref |
0.98 (0.96 to 0.98) * 1.02 (1.00 to 1.05) * 1.08 (1.06 to 1.09) * 0.99 (0.96 to 1.02) 0.98 (0.96 to 0.99) * Ref |
0.72 (0.67 to 0.76) * 0.69 (0.64 to 0.75) * 0.71 (0.66 to 0.76) * 0.64 (0.59 to 0.71) * 0.86 (0.81 to 0.92) * Ref |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





