1. Introduction
Feeding and Eating Disorders (FEDs) are complex mental health conditions characterized by clinically significant disturbances in eating behaviours and in the psychological and biological mechanisms regulating food intake [
1]. Their classification is defined within the International Classification of Diseases of the World Health Organization [
2]. FEDs represent a major and growing public health concern worldwide due to their increasing prevalence, early onset, chronic trajectories, and profound psychosocial impact [
3,
4,
5,
6].
Contemporary clinical literature emphasizes the need for integrated and multidisciplinary treatment models that extend beyond symptom reduction and support long-term recovery, social inclusion, and improvements in quality of life [
7,
8,
9]. In line with these recommendations, several institutions and research centers have developed guidelines for the nutritional and psychosocial rehabilitation of patients with eating disorders [
10,
11,
12,
13]. Within this framework, recovery is increasingly conceptualized as a multidimensional and dynamic process influenced not only by clinical interventions but also by environmental, relational, and lifestyle factors.
In recent years, nature-based interventions have gained recognition as complementary therapeutic approaches for a wide range of mental health conditions [
14]. A substantial body of international research demonstrates that exposure to green environments is associated with reduced stress levels, improved emotional regulation, enhanced social interaction, and overall psychological well-being [
15,
16,
17]. Activities such as horticulture and gardening have shown promising outcomes in supporting individuals with mental health conditions and other vulnerable groups by fostering responsibility, embodied engagement, and social connectedness [
18].
Within this broader context, socially oriented agricultural practices—commonly referred to as social farming—have emerged as innovative and multifunctional models combining food production with therapeutic, educational, and social inclusion objectives. These initiatives create environments in which agricultural activities generate health benefits, promote learning processes, and strengthen community engagement [
19,
20,
21,
22,
23,
24]. Social farming projects typically involve collaboration among farmers, healthcare and social services, third-sector organizations, and public institutions, thereby offering structured pathways for individuals experiencing social exclusion or health-related vulnerabilities. Their therapeutic relevance has also been documented in specific clinical contexts; for example, Curzio et al. [
25] highlighted the role of horticultural practices in mitigating pathological traits such as excessive control and impatience among individuals with FEDs.
Among the different forms of social farming and urban agriculture, community gardens represent a distinct subset characterized by their collective and participatory nature. Particularly in densely urbanized contexts, they play a crucial role in delivering ecosystem services while providing inclusive spaces for citizens and vulnerable groups [
22,
26,
27,
28].
Despite the diversity of organizational models, community gardens share a common collective dimension [
27,
29]. They can be understood as forms of urban agriculture in which open and shared spaces are collectively managed by groups of gardeners [
30], and as deliberately designed nature-based solutions capable of achieving multiple environmental and social objectives in urban settings [
31]. These spaces promote active participation by non-profit organizations, citizen groups, schools, and public institutions [
26], while also enabling individuals with disabilities and other forms of vulnerability to participate [
32]. By fostering social ties, mutual support, and a sense of belonging [
30,
33], community gardens contribute not only to individual well-being but also to broader community resilience.
Parallel to the growing recognition of nature-based therapies, the spatial dimension of healthcare accessibility has become a central concern within health geography and spatial planning research. Geographic Information Systems (GIS) and spatial Decision Support Systems (DSS) are widely used to analyze the distribution of services, evaluate accessibility patterns, and support evidence-based planning [
15,
34,
35]. Spatial accessibility models and location–allocation approaches have contributed significantly to improving the organization of healthcare systems and promoting the equitable distribution of services [
36,
37]. Furthermore, GIS-based multi-criteria decision analysis has proven effective in addressing complex demand–supply interactions within spatial planning processes [
38,
39], and GIS-based DSS are increasingly employed to match health needs with territorially distributed resources in support of informed decision making [
15].
Despite the expanding literature on nature-based therapeutic interventions and the increasing integration of spatial tools in healthcare planning, these research trajectories have largely developed in parallel. Clinical and psychosocial studies emphasize the importance of integrated and recovery-oriented care models for individuals with FEDs, while environmental and planning research highlights the positive effects of agricultural spaces and green infrastructure on mental health, social cohesion, and health equity [
40,
41,
42,
43]. However, limited attention has been devoted to the spatial organization of these therapeutic opportunities and to the systematic matching of patients’ differentiated needs with available socio-agricultural resources.
Few studies adopt a spatially explicit, decision-support perspective capable of connecting health demand with territorially distributed therapeutic environments. To date, no research has proposed a GIS-based model specifically designed to identify and match agricultural and green therapeutic settings with the diverse needs of individuals undergoing treatment for eating disorders.
To address this gap, the present study develops and tests a GIS-based DSS aimed at matching the specific therapeutic needs of individuals with FEDs to the spatial distribution and characteristics of social-agricultural and green environments. The DSS is designed to connect care associations supporting individuals with eating disorders with educational and social farms and community gardens, thereby strengthening the link between food production environments and psychosocial well-being.
The research is guided by the following questions:
(i)How can a GIS-based DSS support the identification of therapeutic agricultural and green environments tailored to the needs of individuals with eating disorders?
(ii)What spatial and organizational mismatches exist between the demand expressed by users of a FED care centre and the available territorial supply?
(iii)What are the implications of these mismatches for sustainable urban and regional planning aimed at promoting health equity and social inclusion?
2. Materials and Methods
2.1. Methodological Framework
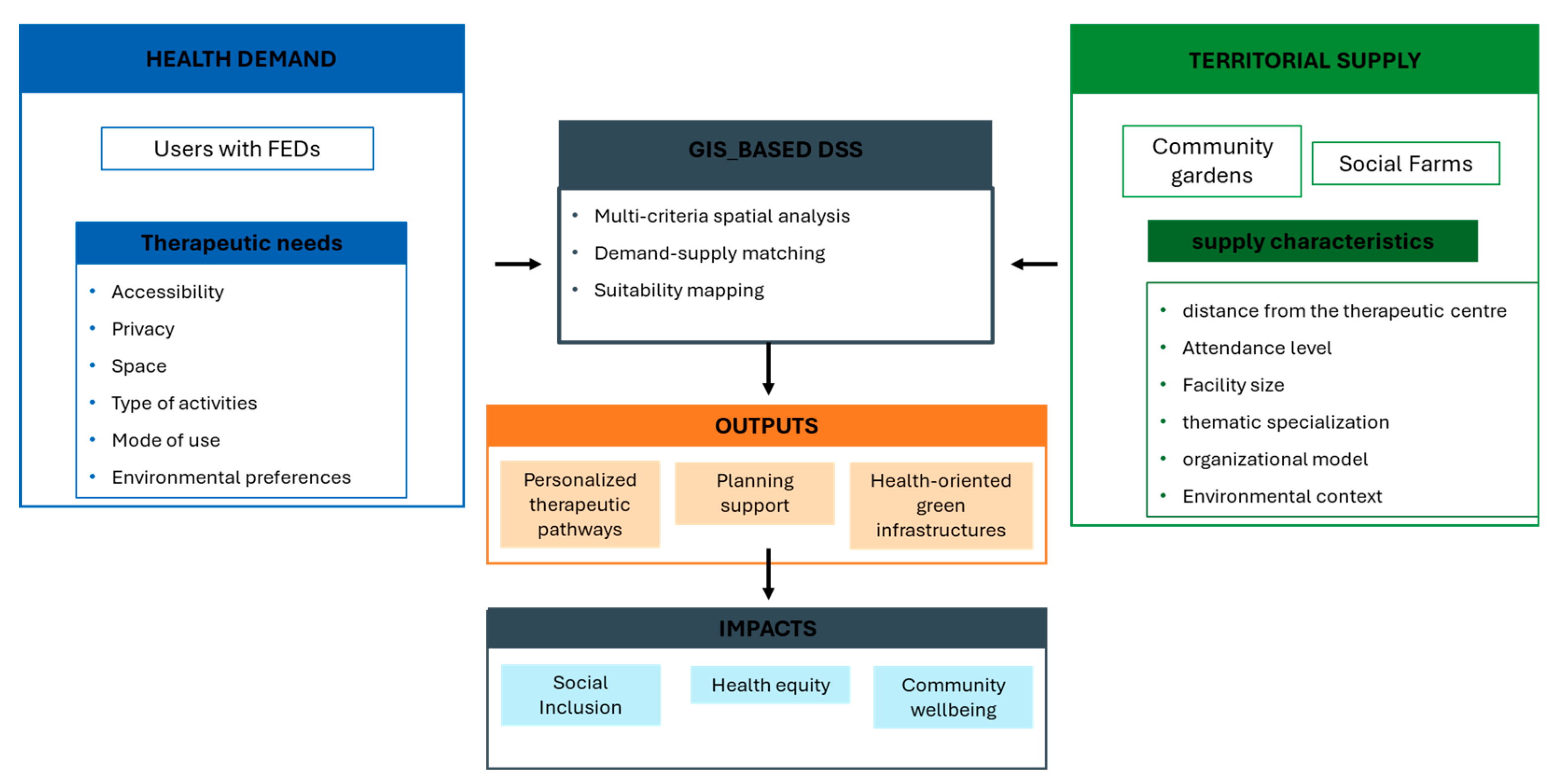
Figure 1 illustrates the methodological framework adopted in this study. The research develops a GIS-based DSS designed to spatially match the demand for therapeutic agricultural experiences expressed by users of a FED treatment center with the territorial supply of social farms and community gardens.
The methodological workflow consists of three main phases: (1) identification and characterization of therapeutic demand; (2) mapping and analysis of socio-agricultural supply; (3) implementation of a GIS-based multi-criteria matching process.
This structured approach enables a systematic comparison of user preferences and spatial attributes of available facilities.
2.1. Study Area and Case Study
The demand side was analyzed through the case study called “Il Pellicano”, which is an association located in the historic center of Perugia (Umbria, Italy). Established in 1997, the association is dedicated to the treatment and psychosocial support of individuals with Feeding and Eating Disorders (FEDs) and currently assists an average of 175 patients per year. The main objectives of the center include reducing compulsive behaviors associated with FEDs and providing practical strategies for their long-term management. Il Pellicano operates as a “help-home”, defined as a welcoming, non-medicalized environment grounded in mutual self-help principles [
44]. Therapeutic activities include assisted meals, food familiarization training, and a variety of creative workshops such as painting, sewing, and theatre. The center also maintains a small garden used for self-production and for the cultivation of fruit and vegetables. Beyond clinical support, the association promotes the development of a strong social network aimed at preventing isolation and identifying both behavioral and structural risk factors affecting patients [
24]. Most users are young people, with female adolescents representing approximately 33.3% of the total patient population. In addition to healthcare professionals (21%), the association actively involves patients’ families (25%) and volunteer citizens (20.7%) in its programs and initiatives [
44]. Il Pellicano is currently exploring strategies to reconnect patients with food production environments and has recently collaborated in the design of a local community garden [
45]. This orientation provided the basis for investigating the spatial integration of socio-agricultural resources into therapeutic pathways.
The supply of agricultural environments suitable for food-production experiences was assessed by mapping social farms and community gardens located within the municipality of Perugia and neighboring municipalities. The Umbria Region hosts 164 registered social farms, of which 58 are located within the selected municipalities (Perugia, Assisi, Corciano, Deruta, Gubbio, Magione, Marsciano, Panicale, Piegaro, Torgiano, Umbertide, and Valfabbrica). In addition, the city of Perugia includes six community gardens. The primary data source for identifying social farms was the official Umbria regional portal [
46].
2.2. Data Collection: Demand and Supply Assessment
Data collection involved the administration of two structured questionnaires designed to capture both therapeutic demand and territorial supply.
The first questionnaire targeted users of Il Pellicano. The instrument consisted of 21 questions designed to identify preferences for agricultural environments and green spaces. It explored perceived needs regarding accessibility, privacy, facility size, environmental context, thematic activities, and organizational models of access. The objective was to translate subjective therapeutic preferences into structured variables suitable for spatial analysis. The questionnaire was administered in paper format by healthcare professionals working at the association.
The second questionnaire was addressed to managers or owners of the identified supply facilities, including the 58 social farms located in the selected municipalities, the six community gardens in Perugia, and the garden managed by Il Pellicano. This instrument included 16 questions designed to capture the main characteristics of each facility, such as the type and frequency of users, the thematic focus of activities, the duration and structure of programs, spatial size, organizational model, environmental setting, and attendance levels. The questionnaire was conducted through telephone interviews.
Participation in both surveys was voluntary.
2.3. Development of the GIS-Based Decision Support System
The DSS was developed using QGIS version 3.40.6. All facilities identified on the supply side, together with the therapeutic center representing the demand origin, were georeferenced and incorporated into a spatial database. Questionnaire responses were encoded and stored as attribute data associated with each mapped location.
The core of the DSS consists of a multi-criteria spatial matching process designed to compare individual therapeutic preferences with the characteristics of available facilities. The variables used in the analysis include thematic areas of activity, environmental context, organizational model of service provision, attendance level, facility size, and spatial accessibility. Thematic areas were grouped into categories such as nature and biodiversity, agriculture, environmental measures, animal-related activities, and food education. Environmental context refers to whether a facility is in an open and visible setting or in a quiet and secluded environment. Organizational models distinguish between facilities that are freely accessible, accessible by booking, structured through scheduled time slots, or adaptable according to specific needs. Attendance level reflects the degree of public presence, while facility size was classified into four ranges based on surface area.
Accessibility was assessed through network analysis using the “Shortest Path (Point to Layer)” tool available in QGIS. This tool calculates the minimum travel distance along the road network derived from OpenStreetMap data between the therapeutic center and each supply facility. By relying on network distance rather than straight-line (Euclidean) distance, the analysis provides a more realistic estimation of spatial accessibility.
The matching process was implemented through SQL-based queries within the GIS environment. Each individual demand profile was cross-referenced with the full set of supply attributes. A facility was considered suitable when all selected preferences expressed by a user corresponded to the characteristics available at that location. In this way, the DSS identifies fully compatible sites capable of supporting personalized therapeutic pathways.
Finally, the system was exported to a shared Google My Maps platform to allow interactive consultation by healthcare professionals and, where appropriate, patients. The platform enables users to visualize the spatial distribution of facilities, access descriptive information and images, and support the collaborative design of tailored therapeutic experiences.
3. Results
3.1. Demand Analysis
Of the 175 patients supported annually by the association, 24 agreed to participate in the study, representing approximately 13.7% of the total population. Although the sample is limited in size, it provides an exploratory insight into the variability of therapeutic preferences within a real-world clinical context. Given the modest number of respondents, percentages should be interpreted cautiously and understood as indicative tendencies rather than statistically generalizable findings.
The age distribution shows a predominance of young adults, with 50% of respondents aged 18–25 and 25% aged 26–35. This reflects the demographic profile typically associated with FED prevalence and suggests that the preferences identified may be particularly representative of younger users engaged in recovery pathways.
Table 1 shows results of therapeutic demand and highlights a differentiated structure in which certain spatial and organizational characteristics emerge as clearly preferred, while others appear to play a secondary role, as indicated by the high proportion of indifferent responses in some attributes.
One of the most notable findings concerns accessibility. The high proportion of indifferent responses (75%) indicates that distance from the therapeutic centre is not perceived as a primary constraint. This suggests that experiential and qualitative attributes of agricultural environments may outweigh spatial proximity in shaping therapeutic choices. However, given the limited sample size, this result should not be interpreted as evidence that accessibility is universally irrelevant; rather, it indicates that within this subgroup, other dimensions appear more salient.
Privacy preferences reveal internal heterogeneity. While 33.33% of respondents expressed a preference for moderate privacy and 12.5% for high privacy, a non-negligible share (25%) reported low privacy needs, suggesting comfort with socially active environments. The coexistence of these divergent orientations highlights the multidimensional nature of recovery trajectories in FED contexts. The 29.17% rate of indifference further reinforces the variability of therapeutic expectations and suggests that personalization is crucial.
Spatial preferences are more clearly structured. The concentration of responses toward very large facilities (33.33%) and medium-sized spaces (29.17%) suggests that participants may associate larger environments with greater therapeutic opportunity, diversity of activities, and perceived freedom. The marginal demand for small facilities (4.17%) may reflect concerns about limited experiential variety or social exposure. Nevertheless, because each percentage point corresponds to a small number of individuals, these interpretations remain exploratory.
Thematic preferences show a strong convergence toward agriculture and nature and biodiversity (33% each), which together account for two-thirds of expressed demand. This concentration suggests that direct engagement with ecological and productive processes may play a central symbolic and experiential role in therapeutic imagination. The complete absence of interest in animal-related activities is noteworthy but should be interpreted cautiously, as it may reflect sample-specific preferences rather than a broader trend.
Organizational flexibility emerges as a potentially critical factor. Half of respondents prefer facilities that are always open and freely accessible, indicating a desire for autonomy and self-directed engagement. Given the psychological characteristics often associated with FEDs, including ambivalence toward externally imposed structures, this preference may reflect a broader need for perceived control within recovery pathways. However, the 33.33% indifference rate suggests that for a substantial subset of users, organizational format is secondary to environmental and thematic qualities.
Environmental context preferences are relatively balanced, with a slight predominance of quiet and secluded settings (37.5%). This may indicate the therapeutic relevance of protected environments that reduce social exposure. At the same time, nearly one-third of respondents preferred open and visible settings or declared indifference, again pointing to heterogeneous recovery needs.
Overall, the demand analysis reveals variability rather than uniformity. The findings underscore the importance of a decision-support approach that accommodates differentiated profiles rather than assuming standardized therapeutic environments.
3.2. Supply Analysis
78% of contacted facilities agreed to participate, ensuring relatively robust coverage of the territorial supply. However, non-response rates for certain variables (approximately 20% in some categories) introduce partial uncertainty into the interpretation of supply characteristics.
Table 2 shows that the territorial supply is characterized by low accessibility, with almost three-quarters of the facilities located more than 1 kilometer from the therapeutic center.
The spatial distribution of facilities confirms a structural distance between therapeutic demand and agricultural resources, with 73.85% of locations situated more than 1 km from the therapeutic center. While this may not represent a decisive constraint according to the demand analysis, it potentially introduces logistical barriers, particularly for users with limited mobility or economic resources.
Privacy conditions represent a clearer mismatch. The predominance of high-attendance environments (66.15%) and the absence of low-attendance facilities indicate that the territorial system is primarily configured as socially intensive. Given that a proportion of users expressed a preference for higher privacy, this structural imbalance may partially explain the limited number of full matches identified by the DSS.
The supply system is strongly oriented toward very large facilities (58.46%), which aligns with the expressed demand for extensive environments. This structural compatibility in spatial capacity represents one of the strongest points of convergence between demand and supply.
From a thematic perspective, the universal availability of agriculture and nature-related activities suggests high potential alignment with user preferences. However, the relatively low availability of environmental measures (8%) and moderate provision of food education (45%) may limit options for users seeking diversified thematic experiences.
Organizationally, the predominance of highly adaptable models (47.69%) suggests latent flexibility within the system. However, the low percentage of freely accessible facilities (9.23%) contrasts with the strong demand for autonomous access, potentially generating friction in practical implementation.
Environmental configuration shows a predominance of open and exposed settings (50.77%), while secluded environments account for only 23.08%. This imbalance may affect users expressing stronger privacy needs.
Importantly, 89% of facilities declared willingness to develop programs specifically dedicated to individuals with FEDs. Although only one facility has already implemented such an initiative, this high level of declared readiness indicates substantial potential for future demand–supply alignment through targeted planning interventions.
3.3. Demand–Supply Matching
The GIS-based matching process identified full correspondence between demand and supply for 37% of users. Given the strict criterion adopted (requiring simultaneous satisfaction of all selected preferences) this percentage should be interpreted as conservative. Even minor divergences in a single variable result in exclusion from the “full match” category.
From a methodological standpoint, the 37% full-match rate does not imply that the remaining 63% of users lack viable options. Rather, it indicates that no facility satisfies the entire combination of expressed criteria. Partial matches may still provide therapeutically meaningful opportunities, especially if certain variables (e.g., thematic focus) carry greater subjective weight than others (e.g., organizational model).
The limited sample size further constrains the generalizability of the 37% figure. Because each individual profile substantially affects aggregate results, small changes in expressed preferences could significantly alter the matching percentage. Therefore, findings should be interpreted as a proof of concept demonstrating the feasibility of a spatially explicit decision-support approach rather than as a definitive assessment of territorial adequacy.
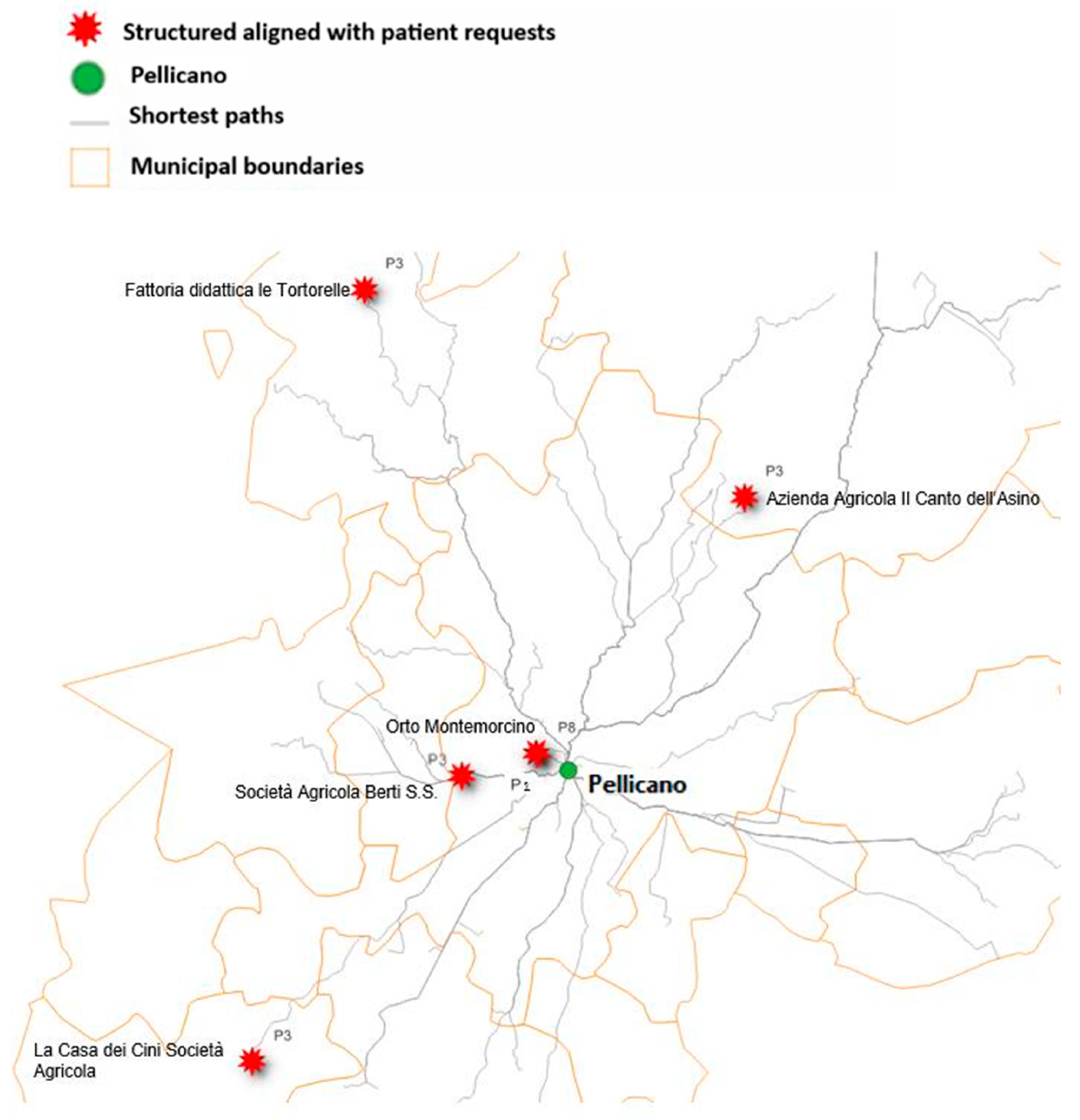
Figure 2 shows an example of results for three patients (P1, P3, P8) who found social farms that responded to their needs. Patient P1 and patient P8 found only one correspondence (The community garden called “Orto di Montemorcino”). Patient P1 has asked for a food production site proposing an activity linked to “agriculture” and “environmental measures”, with a large availability of space (between two and five hectares), moderate attendance, and situated in a quiet, secluded context. Patient P8 asked for the same characteristics as P1, except for the thematic interests, which he selected as “nature and biodiversity” and “food education”.
Patient P3 identified four social farms that meet his needs. He expressed a preference for a food production site larger than 5 hectares, characterized by high attendance, located in a quiet, secluded setting, and organized with differentiated access for user categories. The preferred thematic areas are “nature and biodiversity” and “agriculture”.
The case examples (P1, P3, P8) illustrate how differentiated preference structures yield varying numbers of compatible sites, ranging from 1 to 4 matches. This variability confirms the importance of individualized spatial assessment.
Figure 2 shows the results of interrogating the DSS in the QGIS environment, where the patient can enter their query, and the map highlights only the facilities that meet their needs.
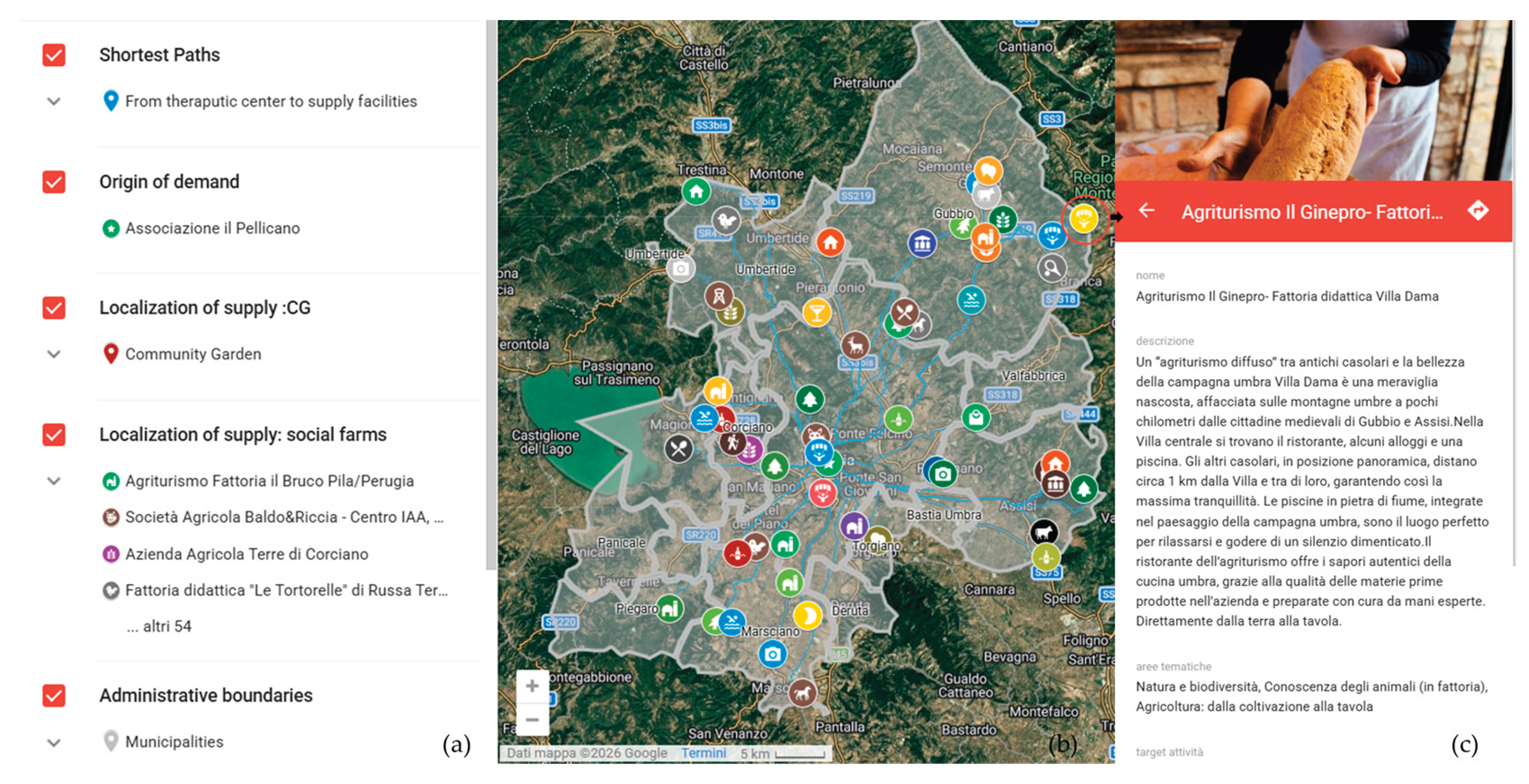
Instead,
Figure 3 shows how the DSS appears to patients in the MyMpas environment. Patients can select each facility to view photos, a brief description, and its main characteristics. This map can be accessed directly in Google Maps mobile app, allowing users to locate each site at any time.
Overall, the results highlight three key analytical insights: the heterogeneity of therapeutic preferences among individuals with FEDs; the structural characteristics and current limitations of territorial supply; the utility of GIS-based multi-criteria matching in revealing both compatibility and gaps within health–environment systems.
4. Discussion
4.1. The Challenge of Identifying Tailored Solutions for Personalized Therapeutic Pathways
The multi-criteria spatial analysis, based on accessibility, privacy needs, spatial capacity, thematic preferences, organizational models, and environmental conditions, enabled the identification of fully compatible facilities for 37% of participating patients. This percentage should be interpreted cautiously, as the matching procedure required simultaneous satisfaction of all selected criteria. Even minor discrepancies in a single variable resulted in exclusion from the “full match” category. Therefore, the 37% value reflects a conservative estimate of alignment between therapeutic demand and territorial supply.
The comparison between demand (
Table 1) and supply (
Table 2) highlights that the most significant mismatches concern the organizational model, attendance level (privacy conditions), and spatial capacity.
From an organizational standpoint, 50% of respondents preferred facilities that were freely accessible, without booking or time-scheduling requirements. This need for autonomy may reflect the importance of self-directed engagement within recovery pathways. Although community gardens generally satisfy this criterion, they are often perceived as either too small or too close to the therapeutic center. Conversely, social farms more frequently adopt structured access systems. This organizational asymmetry suggests that adapting management models—by leaving certain areas freely accessible while scheduling structured activities—could significantly improve alignment without requiring major spatial redesign.
Privacy conditions represent another structural imbalance. While patient preferences are heterogeneous (12.5% high need for privacy, 33.33% medium, and 25% low), the supply is predominantly characterized by high-attendance environments (66.15%), with a near absence of low-attendance facilities. This imbalance limits the availability of protected and socially less exposed spaces for individuals who perceive calm and reduced visibility as therapeutically relevant. The literature on restorative environments emphasizes the importance of settings that reduce social pressure and cognitive overload [
47], supporting the need for more differentiated privacy configurations.
Regarding spatial capacity, although very large areas are widely available (58.46%), there is a relative shortage of medium (4.62%), and large (12.31%) facilities compared to patient demand (45.84% combined preference for 1–5 ha spaces). This polarization between very large rural farms and small urban gardens leaves an intermediate spatial scale underrepresented. From a planning perspective, this suggests that diversifying spatial typologies, rather than simply quantitative expansion, may be necessary to better respond to therapeutic demand.
Environmental context also contributes to mismatches. While 37.5% of patients prefer quiet, secluded environments and 29.17% prefer open, visible spaces, the supply is predominantly open, exposed spaces (over 50%). Landscape design interventions—such as vegetative buffers or spatial zoning—could help reconcile these differences by creating differentiated microenvironments within the same facility.
Interestingly, although 73.85% of supply resources are located more than one kilometer from the therapeutic center, accessibility does not appear to constitute a decisive barrier. A large majority of respondents (75%) declared indifference to walking distance. This finding contrasts with traditional accessibility models commonly used in spatial planning [
48], in which proximity is often considered a primary determinant of service utilization. Qualitative feedback indicates that some patients prefer more distant environments to create symbolic separation from the clinical setting, while others are willing to travel by car. This suggests that psychological distance may, in specific contexts, be as relevant as physical proximity.
From a thematic perspective, the limited availability of activities related to environmental measures (8% of supply) contrasts with patient interest in sustainability, energy saving, water management, and ecological footprint awareness (17% of demand). Expanding educational components on environmental sustainability could therefore enhance the attractiveness and therapeutic relevance of social farms, particularly considering the growing recognition of nature-based solutions for promoting well-being [
49,
50].
These findings contribute to the broader debate on integrating green infrastructure into health-oriented spatial planning. Urban green infrastructure is increasingly recognized as a determinant of health equity and access to restorative environments [
41]. Studies conducted across different socio-spatial contexts, including Hyderabad, India [
51], demonstrate the role of green spaces in supporting vulnerable populations. Although eating disorders are not explicitly addressed in those studies, individuals with FEDs can reasonably be included among groups benefiting from supportive environmental conditions. Furthermore, exposure to green environments has been consistently associated with improved mental health outcomes and reduced stress levels [
47], reinforcing the rationale for integrating socio-agricultural spaces into therapeutic pathways.
The developed DSS enables continuous updating of the supply layer, allowing the incorporation of newly designed facilities or modified organizational models over time. Horticultural therapy has already demonstrated promising effects in reducing psychological and physiological stress in adolescents with anorexia nervosa [
25], supporting the clinical plausibility of structured agricultural engagement. More broadly, health outcomes depend not only on medical interventions but also on access to environments that promote psychophysical well-being [
52]. In this sense, spatial planning becomes a complementary component of recovery-oriented healthcare.
Two main limitations should be acknowledged. First, the selection and weighting of matching criteria were defined by the researchers, without patient participation in validating the DSS interface. Future research should adopt co-design approaches that allow users to refine criteria and contribute to variable weighting, thereby increasing therapeutic relevance. Second, the limited number of respondents (n = 24) restricts the statistical generalizability of the findings. The study should therefore be interpreted as an exploratory methodological contribution rather than a representative epidemiological assessment. Expanding participation through gradual engagement processes could strengthen both empirical robustness and practical usability.
4.2. Innovation and Lessons for Landscape Planners and Public Administrators
This study provides three main contributions to the existing literature. First, it bridges eating disorder recovery research and nature-based therapeutic approaches by introducing a spatially explicit analytical framework. The integration of nature-based solutions into health-oriented spatial planning is increasingly recognized as a strategic priority for promoting mental well-being and reducing health inequalities [
53,
54]. Within this perspective, social agriculture and community gardens can be interpreted as components of green infrastructure delivering ecosystem services for public health [
55].
Second, the study develops an operational GIS-based decision-support model that enables systematic matching between individualized health-related needs and territorially distributed resources. The use of GIS-based spatial multi-criteria analysis represents a consolidated approach in healthcare planning and accessibility assessment [
56], but its application to personalized therapeutic pathways for individuals with FEDs represents an innovative methodological extension.
Third, the research contributes planning-oriented evidence to the debate on health equity and community well-being. Previous studies have applied GIS-based approaches to balance demand and supply of spatial resources such as urban forests [
35], public transport systems [
57], and water resources [
58]. However, few have focused on tailored responses for vulnerable communities [
59]. By identifying mismatches between therapeutic demand and territorial provision, this study underscores the need to diversify spatial typologies, accessibility models, and organizational structures of green and agricultural spaces.
The proposed DSS is conceptually transferable to other territorial contexts and to different categories of vulnerable users. Its methodological framework—based on spatial matching between expressed needs and socio-environmental characteristics—can be adapted to various geographical scales and institutional settings. In this sense, the model represents a scalable decision-support approach rather than a context-specific tool.
From a policy perspective, integrating healthcare systems, social farming networks, and green infrastructure planning emerges as a key strategy for promoting health equity and social inclusion. The DSS can support public administrations in identifying priority intervention areas, optimizing resource allocation, and designing place-based therapeutic networks. In this framework, spatial planning becomes an active component of public health policy, contributing to the creation of inclusive, restorative, and health-supportive environments for vulnerable groups.