1. Introduction
Sutureless intrascleral intraocular lens fixation using the double-needle technique, commonly known as the Yamane technique (Yamane SFIOL), was first introduced by Yamane et al. in 2014 [
1] and subsequently refined with flanged haptics in 2017 [
2]. The technique enables secure scleral fixation of a three-piece IOL without sutures, thereby reducing manipulation and suture-related complications.
Yamane SFIOL is indicated for aphakia and dislocation or subluxation of the crystalline lens or posterior chamber IOL in eyes with inadequate capsular or zonular support due to trauma, complicated cataract surgery, pseudoexfoliation, or prior vitreoretinal procedures. Several modifications of the original technique have been proposed, addressing IOL design, haptic configuration, and vitreous management to improve stability and refractive predictability.
Comparative studies of alternative secondary IOL fixation strategies, including Gore-Tex–sutured scleral fixation and Z-suture techniques [
3,
4] , as well as a recent systematic review and meta-analysis [
5], report visual and refractive outcomes comparable to those achieved with the Yamane technique. These findings position Yamane SFIOL as a competitive sutureless option that avoids suture-related complications while maintaining stable functional results.
Although several studies have reported favorable anatomical and visual outcomes following Yamane SFIOL implantation, most series primarily focus on surgical feasibility, refractive stability, and complication profiles rather than on clinically relevant predictors of postoperative visual acuity [
5,
6,
7,
8]. In addition, available studies often include heterogeneous surgical approaches, limited follow-up, or trauma-specific cohorts, which may reduce the broader applicability of the prognostic conclusions [
5,
8]. Therefore, data on long-term functional outcomes and independent predictors of postoperative BCVA in consecutive real-world cohorts remain limited.The present study was designed to evaluate long-term visual outcomes after Yamane SFIOL implantation and to identify independent clinical predictors of postoperative BCVA in a single-surgeon consecutive series with extended follow-up.
The aim of this study was to evaluate visual outcomes, expressed as best-corrected visual acuity (BCVA), after sutureless scleral-fixated intraocular lens implantation using the Yamane technique and to identify clinical predictors of postoperative BCVA.
2. Materials and Method
Study design: this single-center, single-surgeon study included consecutive eyes undergoing Yamane SFIOL for aphakia or lens/posterior chamber intraocular lens (PC IOL) ectopia, with at least 1 year of postoperative follow-up available. Procedures were performed at the Clinic for Eye Diseases, University Clinical Center of Serbia, Belgrade, between January 2020 and December 2024; no Yamane SFIOL procedures were performed in 2021 due to COVID-related restrictions. The study adhered to the Declaration of Helsinki, was approved by the institutional review board Medical faculty, University of Belgrade (approval No. 25/VI-5) and by Ethics Committee of the Clinical Center of Serbia (approval No. 1600/56), and written informed consent was obtained from all patients.
Patients and outcome: All patients underwent a comprehensive ophthalmologic examination. BCVA was measured using a Snellen chart at a distance of 6 meters and recorded in decimal notation. Eyes were eligible if Yamane SFIOL was indicated for aphakia or lens/PC IOL dislocation in the setting of insufficient capsular/zonular support and if ≥1-year follow-up was available. Exclusion criteria included significant keratopathy, corneal scarring, prior corneal transplantation, active uveitis, acute ocular infection, or uncontrolled intraocular pressure (except urgent cases requiring prompt surgery).
Surgical procedure: Yamane SFIOL implantation was performed in accordance with the previously published technique (2). Anterior or pars plana vitrectomy was undertaken, when indicated, with a 23-gauge Stellaris PC platform (Bausch & Lomb) under either peribulbar or sub-Tenon’s anesthesia. Dislocated crystalline lenses were removed via endophacoemulsification or vitrectomy probe while mature lenses were removed through a 6.0-mm sclerocorneal incision. Dislocated IOLs were explanted through a 3.0-mm limbal incision after optic bisection with endothelial protection. A three-piece MA60AC IOL (Alcon) was implanted using the flanged double-needle technique; angled sclerotomies were created 2 mm posterior to the limbus at 3 and 9 o’clock, haptics were externalized through 30-gauge thin wall needles, flanged with high-temperature cautery, and secured in scleral tunnels. Beginning in 2022, all Yamane SFIOL procedures were performed with a Yamane stabilizer.
Statistical analysis: Depending on the type of variables and the normality of the distribution, results were presented as frequency (percent), median (range) and mean ± standard deviation. Statistical hypotheses were tested using Wilcoxon test. Examination of the relations of the dependent variable in repeated measurements with possible predictors was done using generalized linear mixed-effects modeling approach using lme4 package for the R. Independent variables that were significant in univariable models (p<0.1) were used as the independent variables in the multivariable model. All p-values less than 0.05 were considered significant. Statistical data analysis was performed using IBM SPSS Statistics 31 (IBM Corporation, Armonk, NY, USA) and R-4.5.0 software (The R Foundation for Statistical Computing, Vienna, Austria)
3. Results
Eighty-seven eyes of 85 patients were included. Mean age was 68.2 ± 11.4 years (range, 35–88); 70.6% of patients were male. Eye laterality was evenly distributed. Surgeries were performed between 2020 and 2024, most frequently in 2023 (37.9%) and 2024 (40.2%). Baseline characteristics and univariable associations with postoperative BCVA are summarized in
Table 1.
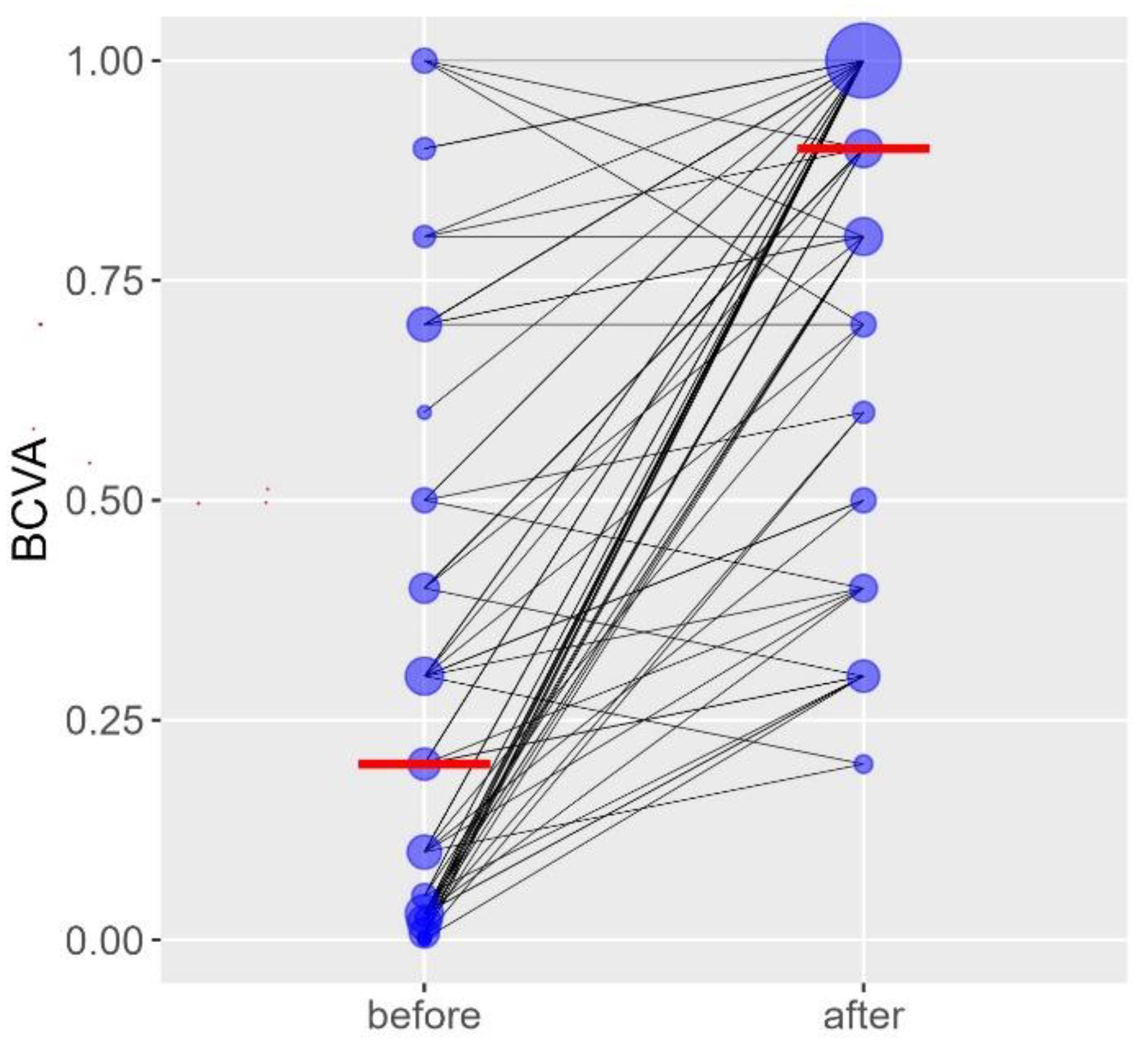
As illustrated in
Figure 1, median BCVA, expressed in Snellen decimal notation, improved significantly from 0.2 (range, 0.001-1.0) preoperatively to 0.9 (range, 0.20-1.0) postoperatively (p < 0.001). The paired distribution demonstrates a consistent postoperative gain across individual eyes, with the majority showing a marked shift toward higher visual acuity values after surgery.
Median follow-up was 26.5 months (range, 12–68.8). Preoperative spherical equivalent was 5.25 D vs. postoperative 0.02 D (p<0,001). The median IOL power was 21.5 D (range 16.5 – 26.5 D) and showed no statistically significant association with postoperative best-corrected visual acuity (B=0.005, p=0.675).
Importantly, the primary indication for the Yamane technique, whether aphakia (in 57,5% cases) or lens/IOL ectopia (in 42.5% cases), did not influence postoperative visual outcomes, underscoring the procedure’s comparable functional efficacy across different clinical indications. Similarly, postoperative visual outcomes did not differ according to the primary indication for the Yamane technique (B = - 0.015, p=0.752). Among 37 cases with ectopia, lens subluxation was observed in 9 (10.3%), IOL subluxation in 15 (17.2%), lens luxation in 5 (5.7%), and IOL luxation in 8 (9.2%) cases. Ectopia of the IOL or natural lens was observed in 20 cases (54.1%) with blunt ocular trauma and in 14 cases (37.8%) with pseudoexfoliation. These two factors represent clear causes and/or predisposing conditions for lens/IOL dislocation, including 5 cases (13.5%) presenting with both factors. In the remaining cases, no definitive cause could be identified. By contrast, in aphakic eyes, the underlying causes could be clearly identified. Blunt ocular trauma was present in 20 cases (40%), open-globe injury in 5 (10%), intraoperative IOL implantation failure during phacoemulsification in 21 (42%), and postoperative aphakia in 4 cases (8%).
Preoperative ocular comorbidity showed no significant association with postoperative best-corrected visual acuity, either with respect to its presence (B = −0.074, p = 0.182) or the number of preoperative ocular comorbidity (B= −0.028, p = 0.281). Among preoperative ocular findings, as detailed in
Table 2, blunt ocular trauma, pseudoexfoliation syndrome, capsular glaucoma, and macular edema showed a significant association with postoperative BCVA, whereas the remaining preoperative ocular conditions were not significantly associated with visual outcome.
In only 15 cases (17.2%), the Yamane procedure was performed as a standalone surgery , and this did not significantly affect postoperative BCVA (B = 0.022, p = 0.072). Additional surgical procedures were commonly performed alongside the Yamane technique, most frequently vitrectomy-related interventions and pupilloplasty. However, none of the additional procedures demonstrated a statistically significant association with postoperative best-corrected visual acuity. Silicone oil evacuation showed a trend toward poorer visual outcomes, although this did not reach statistical significance. The intraoperative use of a Yamane stabilizer, applied in 76 (87.4%) cases, did not show a significant association with postoperative BCVA (B=0.086, p=0.211). Detailed data are summarized in
Table 3.
Ocular trauma represented the predominant underlying cause leading to sutureless intrascleral IOL fixation, with blunt mechanisms being far more common than open-globe injuries. While open-globe trauma invariably resulted in aphakia with no significant influence on postoperative BCVA (B=0.085, p=0.393), blunt trauma produced a heterogeneous spectrum of lens status, including both aphakia and lens/IOL ectopia. Blunt ocular trauma was a significant predictor of postoperative BCVA in univariable analysis (
Table 3) but demonstrated only a borderline association in the multivariable model (Table 5).
Variables included in the multivariable model were selected based on clinical relevance and univariable screening (p < 0.10), prioritizing preoperative ocular status and potential confounders while avoiding collinearity. Capsular glaucoma was excluded due to strong collinearity with pseudoexfoliation syndrome and the limited number of cases, which could compromise model stability. In the reduced multivariable model, age, macular edema, and silicone oil removal remained significant predictors of postoperative BCVA, whereas blunt ocular trauma showed a borderline association, and pseudoexfoliation was not independently significant. Detailed results are presented in
Table 4.
4. Discussion
Our findings are consistent with contemporary evidence demonstrating that sutureless intrascleral intraocular lens fixation using the Yamane technique provides significant and durable improvement in visual acuity. Similar to large comparative and long-term series, we observed reliable and consistent postoperative BCVA as well as proved versatile outcome across different indications [
2,
6,
7].
The magnitude and stability of visual improvement in our cohort align with the seminal description of the flanged thin wall double-needle technique by Yamane et al. [
2] and with subsequent reports across heterogeneous clinical settings, including aphakia, lens/IOL dislocation, and IOL exchange. Importantly, our analysis extends prior work by demonstrating that postoperative visual outcomes are driven primarily by patient-related and retinal factors rather than by the indication for fixation itself.
Ocular trauma was a frequent underlying etiology in our cohort. In agreement with trauma-focused series [
8] , in this study, blunt trauma was associated with better visual outcomes in univariable analysis; however, this association weakened after multivariable adjustment, suggesting that concomitant retinal pathology, rather than the traumatic mechanism per se, determines postoperative vision. Open-globe injury, although uniformly resulting in aphakia, did not adversely affect postoperative BCVA, further emphasizing the dominant role of retinal status in visual prognosis.
Recent investigations addressing technical nuances of the Yamane technique, including IOL design and intraoperative variations [
9,
10,
11,
12,
13], consistently demonstrate preserved anatomical stability and refractive accuracy. In line with these reports, we found no significant influence of adjunctive procedures or IOL power on postoperative BCVA. Similarly, vitreous management strategy, anterior vitrectomy versus pars plana vitrectomy, did not affect visual outcomes, corroborating recent comparative analyses [
14,
15].
Among preoperative factors, age and macular edema emerged as independent negative predictors of postoperative BCVA. Silicone oil removal was also associated with worse outcomes, likely reflecting underlying vitreoretinal complexity rather than the procedure itself, as previously noted in trauma and vitreoretinal series [
8].
Several limitations should be considered. The single-center setting may limit the generalizability of the findings. The wide spectrum of underlying ocular pathology, particularly in trauma-related eyes, may have affected visual outcomes despite multivariable adjustment. In addition, the small number of eyes with certain conditions, such as macular edema or a history of silicone oil removal, may have reduced statistical power. Finally, BCVA was measured using Snellen notation rather than logMAR, which may be less sensitive to subtle changes in visual acuity.
In contrast to prior reports that primarily describe anatomical and refractive outcomes, our study emphasizes clinically relevant predictors of functional visual recovery and demonstrates that postoperative BCVA is driven mainly by retinal status and patient age rather than by surgical indication or technical variables. These findings provide practical prognostic insight for preoperative counseling and case selection in eyes undergoing Yamane SFIOL fixation.
5. Conclusions
The strengths of this study include the consecutive case design, a relatively long and uniform follow-up period, and the use of a single-surgeon approach, which reduces procedural variability and facilitates clearer interpretation of clinical predictors. The comprehensive assessment of preoperative ocular status and adjunctive intraoperative procedures, considered as potential predictors of postoperative visual outcome, further strengthens the analysis.
Overall, these findings support the Yamane technique as a reliable, consistent, and versatile method for secondary intraocular lens fixation across a wide range of indications. Postoperative visual outcomes appear to be driven mainly by patient age and preexisting retinal pathology rather than by the indication for fixation, traumatic etiology, or the need for additional surgical procedures. These observations are clinically relevant for preoperative counseling and for setting realistic expectations, particularly in older patients and in eyes with macular disease or a history of complex vitreoretinal surgery.
Author Contributions
For research articles with several authors, a short paragraph specifying their individual contributions must be provided. The following statements should be used “Conceptualization, GD and MS.; methodology, GD and MS.; software, ZB.; validation, ZB.; formal analysis, ZB.; investigation, GD and MB.; resources, GD and VS.; data curation, GD and JJ; writing—original draft preparation, GD and JJ.; writing—review and editing, GD and MS.; visualization, VS and MB.; supervision, MS.; project administration, GD and VS.; funding acquisition, GD. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki, and approved by the Ethics Committee of Faculty of Medicine, University of Belgrade (No. 25/VI-5), as well as the Ethics Committee of University Clinical Center of Serbia (No. 1600/56).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study. Written informed consent has been obtained from the patient(s) to publish this paper.:
Data Availability Statement
The datasets generated and/or analyzed during the current study are not publicly available due to privacy and ethical restrictions involving participant confidentiality, but are available from the corresponding author on reasonable request.
Acknowledgments
The authors thank Dr Sanja Erić for her assistance in processing the collected data. During the preparation of this manuscript, the authors used of AI-based language tools (ChatGPT) to assist with improving the clarity and readability of the manuscript. The authors have reviewed and edited the output and take full responsibility for the content of this publication.
Conflicts of Interest
The authors declare no conflicts of interest.
Abbreviations
The following abbreviations are used in this manuscript:
| BCVA |
Best Corrected Visual Acuity |
| Yamane SFIOL |
Sutureless intrascleral intraocular lens fixation using the Yamane technique |
| IOL |
Intraocular lens |
| D |
diopter |
| ICCE |
intracapsular cataract extraction |
References
- Yamane, S; Inoue, M; Arakawa, A; Kadonosono, K. Sutureless 27-gauge needle-guided intrascleral intraocular lens implantation with lamellar scleral dissection. Ophthalmology 2014, 121(1), 61–6. [Google Scholar] [CrossRef] [PubMed]
- Yamane, S; Sato, S; Maruyama-Inoue, M; Kadonosono, K. Flanged Intrascleral Intraocular Lens Fixation with Double-Needle Technique. Ophthalmology 2017, 124(8), 1136–42. [Google Scholar] [CrossRef] [PubMed]
- Drummond, SC; Feist, JE; Crosson, JN; Haider, AA; Fuerst, JS; Hughes, DA; et al. Scleral Fixated Secondary IOLs: An Outcomes Comparison Between the Yamane and Gore-Tex-Sutured Techniques. Ophthalmic Surg Lasers Imaging Retina 2024, 55(7), 384–90. [Google Scholar] [CrossRef] [PubMed]
- Simsek, M; Besek, NK; Kirgiz, A; Ahmet, S; Atik, BK; Tellioğlu, A. Comparison of refractive outcomes in patients following scleral fixated intraocular lens implantation with Yamane and Z-suture techniques. Eur J Ophthalmol. 2025, 35(2), 537–43. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C; Palka, C; Zhu, D; Lai, D; Winokur, J; Shwani, T; et al. Clinical Outcomes in Scleral Fixation Secondary Intraocular Lens with Yamane versus Suture Techniques: A Systematic Review and Meta-Analysis. J Clin Med. 2024, 13(11). [Google Scholar] [CrossRef] [PubMed]
- Guerin, PL; Guerin, GM; Pastore, MR; Gouigoux, S; Tognetto, D. Long-term functional outcome between Yamane technique and retropupillary iris-claw technique in a large study cohort. J Cataract Refract Surg. 2024, 50(6), 605–10. [Google Scholar] [CrossRef] [PubMed]
- Sahin Vural, G; Guven, YZ; Karahan, E; Zengin, MO. Long term outcomes of Yamane technique in various indications. Eur J Ophthalmol. 2023, 33(6), 2210–6. [Google Scholar] [CrossRef] [PubMed]
- Nowomiejska, K; Haszcz, D; Onyszkiewicz, M; Choragiewicz, T; Czarnek-Chudzik, A; Szpringer-Wabicz, A; et al. Double-Needle Yamane Technique Using Flanged Haptics in Ocular Trauma-A Retrospective Survey of Visual Outcomes and Safety. J Clin Med. 2021, 10(12), 26052. [Google Scholar] [CrossRef] [PubMed]
- Icoz, M; Erkan, E. Comparison of Two Different Intraocular Lenses Used in the Modified Yamane Technique. J Cataract Refract Surg. 2025. [Google Scholar] [CrossRef] [PubMed]
- Aydin, FO; Aksoy, BK; Ceylan, A; Akbaş, YB; Karapapak, M; Yildiz, BK; et al. Comparison of two different intraocular lenses used in the modified Yamane technique. Indian J Ophthalmol. 2025, 73(3), 416–21. [Google Scholar] [CrossRef] [PubMed]
- Kelkar, A; Kelkar, J; Kothari, A; Mehta, H; Chitale, S; Fogla, R; et al. Comparison of Two Modified Sutureless Techniques of Scleral Fixation of Intraocular Lens. Ophthalmic Surg Lasers Imaging Retina 2018, 49(10), e129–e34. [Google Scholar] [CrossRef] [PubMed]
- Aljindan, M; Hamdi, A; Alali, NM; Hashem, F; HB, AL. Safety, efficacy, and clinical outcomes of transconjunctival intrascleral fixation of an intraocular lens. BMC Ophthalmol. 2024, 24(1), 380. [Google Scholar] [CrossRef] [PubMed]
- Ucar, F; Cetinkaya, S. Flattened flanged intrascleral intraocular lens fixation technique. Int Ophthalmol. 2020, 40(6), 1455–60. [Google Scholar] [CrossRef] [PubMed]
- Atilgan, CU; Tekin, K; Aydugan, MT; Kosekahya, P; Kosekahya, A; Citirik, M. Intraocular lens position outcomes in modified Yamane's technique: The comparison of anterior vitrectomy versus pars plana vitrectomy. Indian J Ophthalmol. 2025, 73 (Suppl 3), S466–s71. [Google Scholar] [CrossRef] [PubMed]
- Tang, Y; Yao, S; Chu, Y; Han, Q. Vitreous management in Yamane's technique for crystalline lens dislocation: anterior vitrectomy or PPV? BMC Ophthalmol. 2023, 23(1), 466. [Google Scholar] [CrossRef] [PubMed]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).