Submitted:
12 February 2026
Posted:
12 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
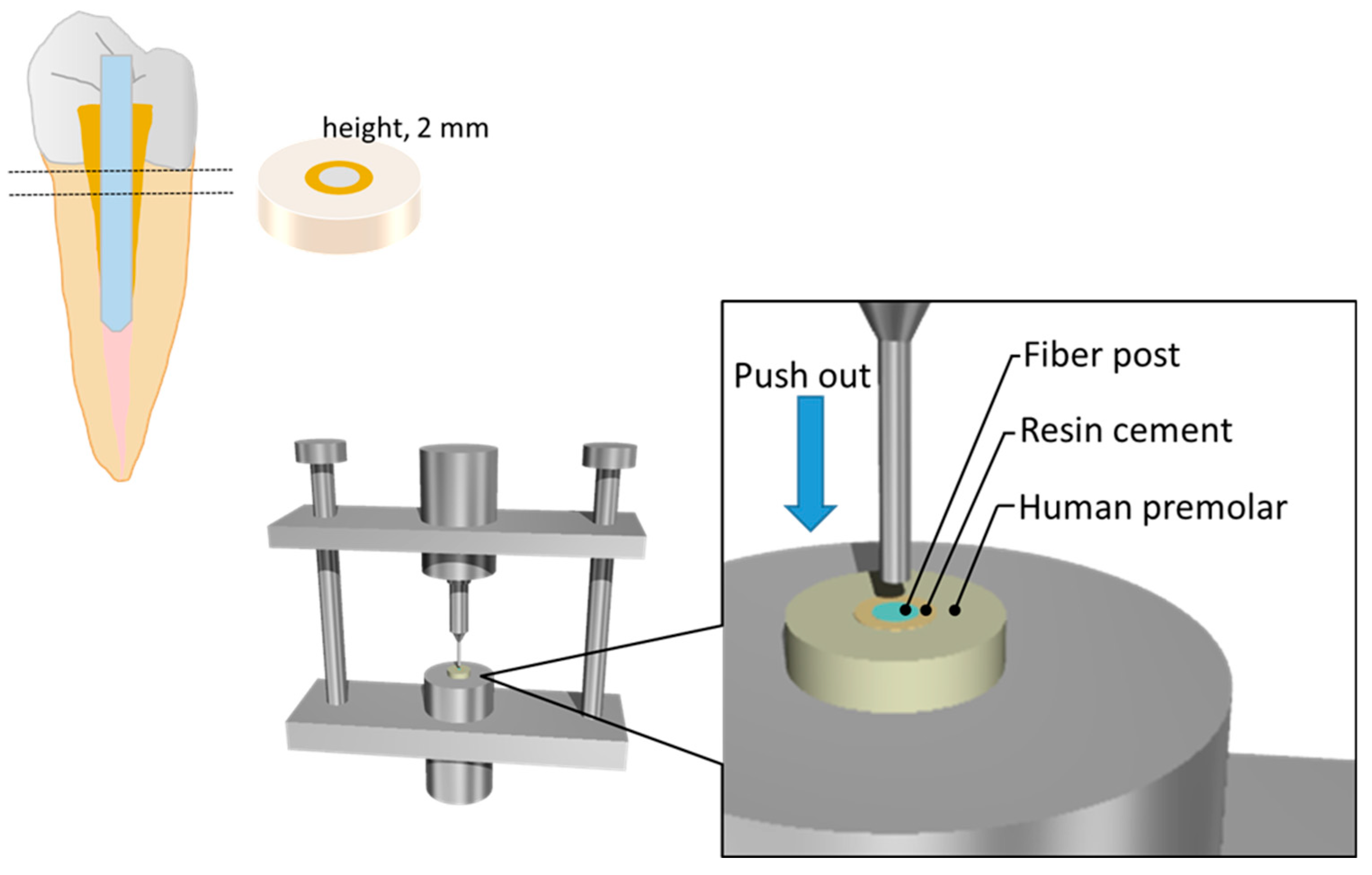
2.1. Push-out Test
2.2. Pull-out Test
2.3. Shear Bond Strength of Resin Cement to Root Dentin
2.4. Flexural Strength and Flexural Modulus of Elasticity of Resin Cement
2.5. Scanning Electron Microscope (SEM) Observations
2.6. Statistical Analysis
3. Results
3.1. Push-out Test
3.2. Pull-Out Test for Pretreatment with Manufacturers’ Recommended Agents
3.3. Pull-Out Test for Pretreatment with Tokuyama Universal Bond II
3.4. Statistical Comparisons between Two Pretreatment Agents
3.5. Shear Bond Strength to Root Dentin
3.6. Flexural Strength
3.7. Flexural Modulus of Elasticity
3.8. SEM Observations
3.9. Correlations
4. Discussion
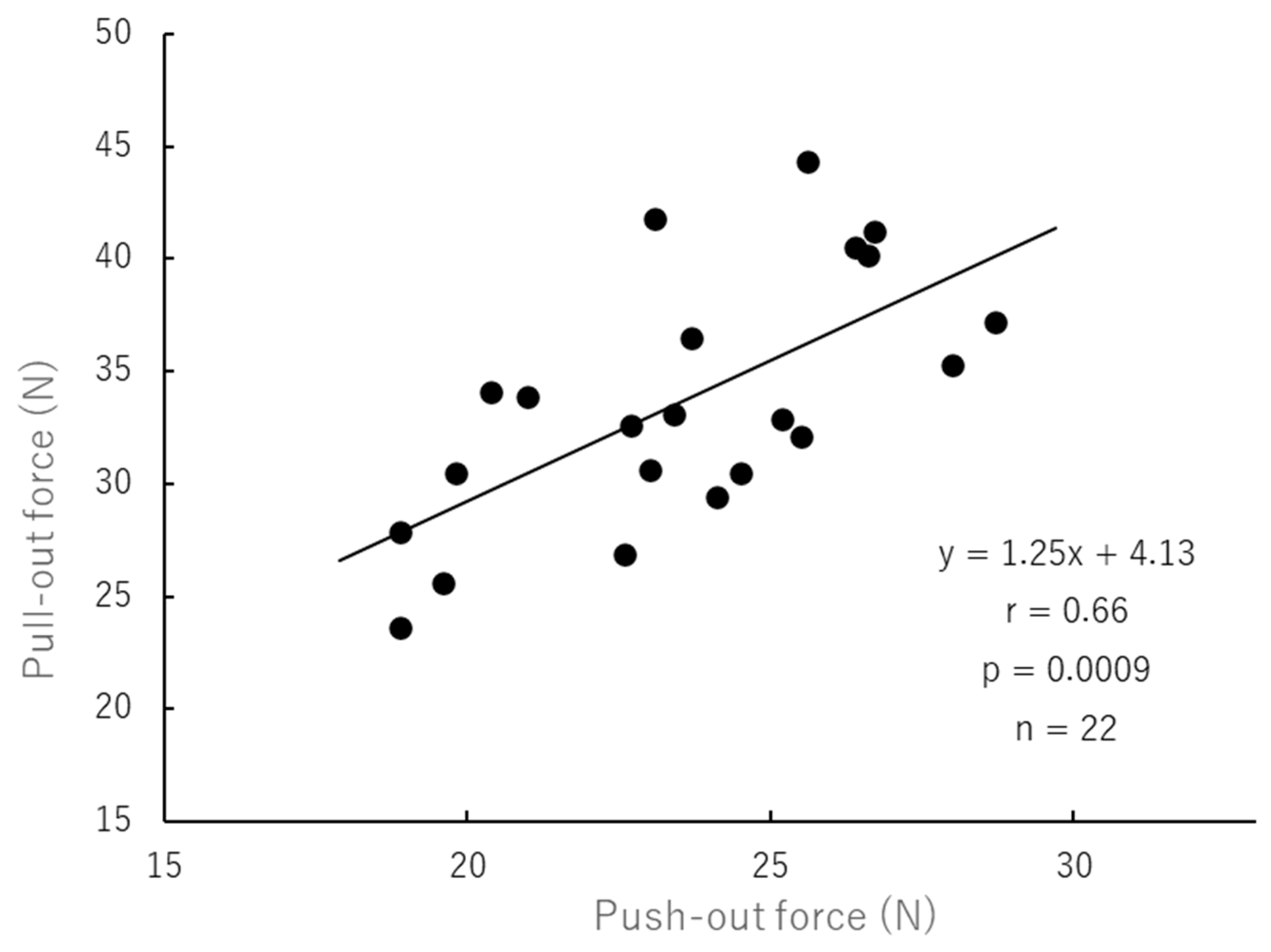
4.1. Correlation Between Push-out Force and Pull-out Force (Table 11 and Figure 3)
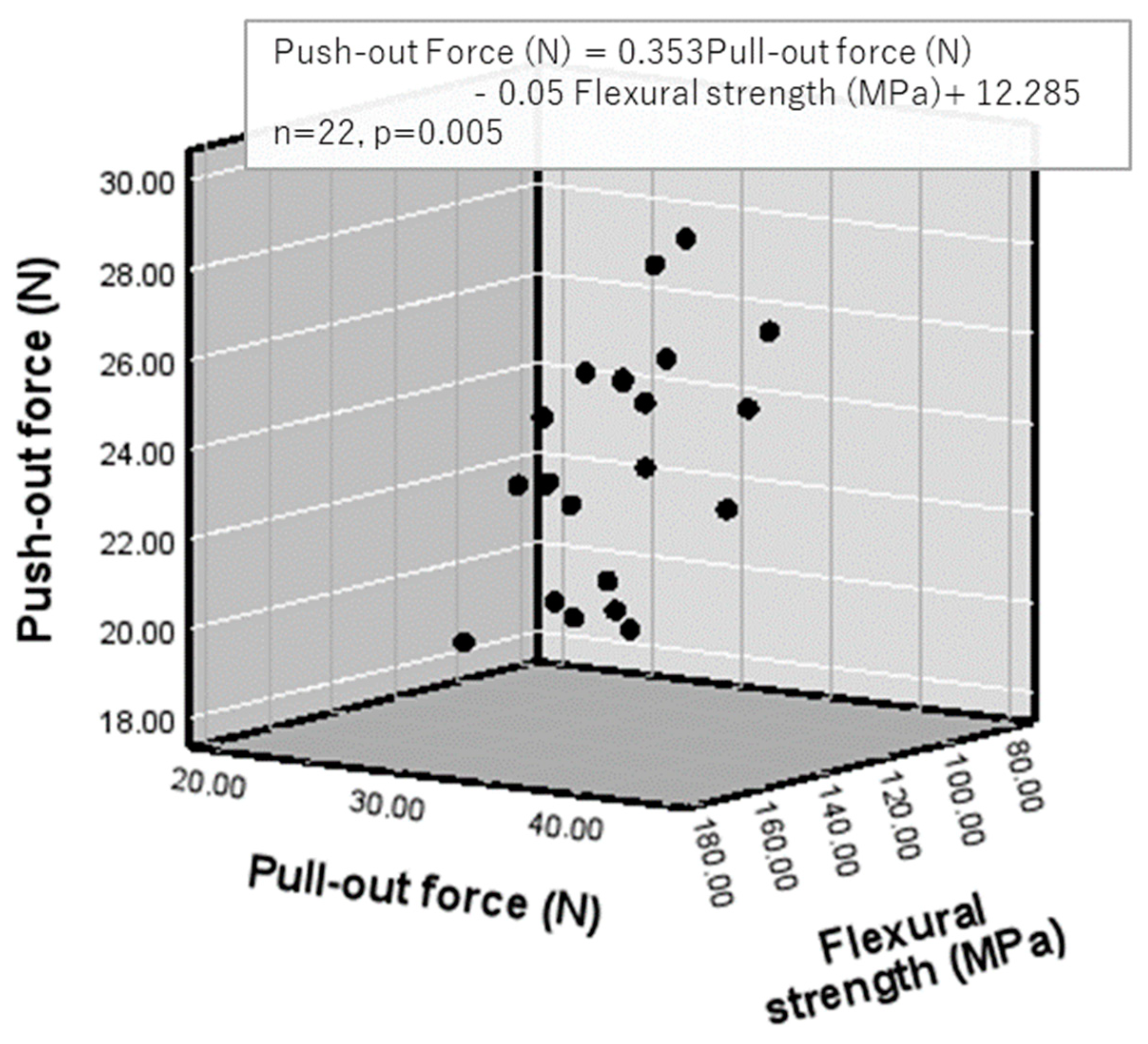
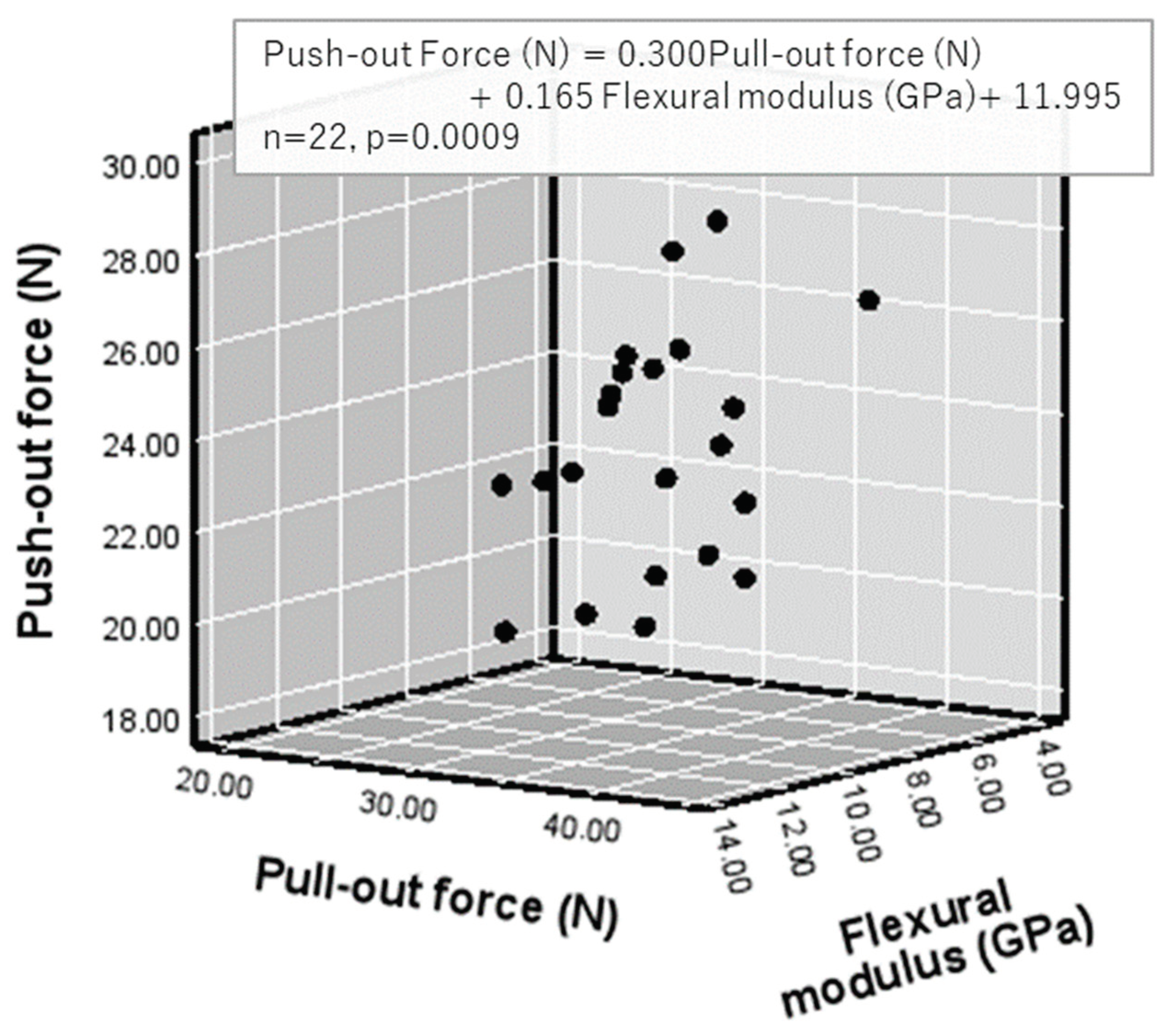
4.2. Correlation Between Push-out Force and Flexural Modulus of Elasticity or Flexural Strength (Table 11 and Figure 4)
4.3. Correlation Between Push-out Force and Shear Bond Strength (Table 11)
4.4. Correlations among Push-out Force, Pull-out Force, and Flexural Strength or Flexural Modulus of Elasticity (Figure 4 and Figure 5)
4.5. Versatility of Universal Adhesives
4.6. Applicability of Tokuyama Universal Bond II as General-Purpose Universal Adhesive
4.7. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Dental Materials, Properties and Manipulation, 9th ed.; Powers, J.M., Wataha, J.C., Eds.; Mosby Elsevier: St. Louis, MI, USA, 2008; p. pp. 203−204. [Google Scholar]
- Sidoli, G.E.; King, P.A.; Setchell, D.J. An in vitro evaluation of a carbon fiber based post and core system. J. Prosthet. Dent. 1997, 78, 5−9. [Google Scholar] [CrossRef]
- Combe, E.C.; Shaglouf, A.-M.S.; Watts, D.C.; Wilson, N.H.F. Mechanical properties of direct core build-up materials. Dent. Mater. 1999, 15, 158−165. [Google Scholar] [CrossRef]
- Pest, L.B.; Cavalli, G.; Bertani, P.; Gagliani, M. Adhesive post-endodontic restorations with fiber posts: push-out tests and SEM observations. Dent. Mater. 2002, 18, 596−602. [Google Scholar]
- Gutierrez, M.F.; Sutil, E.; Malaquias, P.; de Paris Matos, P.; de Souza, L.M.; Reis, A.; Perdigao, J.; Loguercio, A.D. Effect of self-curing activators and curing protocols on adhesive properties of universal adhesives bonded to dual-cured composites. Dent. Mater. 2017, 33, 775−787. [Google Scholar] [CrossRef]
- Phillips’ Science of Dental Materials, 13th ed.; Shen, C., Rawls, H.R., Esquivel-Upshaw, J.F., Eds.; Mosby Elsevier: St. Louis, MI, USA, 2022; p. pp. 202−232. [Google Scholar]
- Seefeld, F.; Wenz, H.J.; Ludwig, K.; Kern, M. Resistance to fracture and structural characteristics of different fiber reinforced post systems. Dent. Mater. 2007, 23, 265−271. [Google Scholar] [CrossRef] [PubMed]
- Yenisey, M.; Kulunk, S. Effect of chemical surface treatments of quartz and glass fiber posts on the retention of a composite resin. J. Prosthet. Dent. 2008, 99, 38−45. [Google Scholar] [CrossRef]
- Torres-Sanchez, C.; Montoya-Salazar, V.; Cordoba, P.; Velez, C.; Guzman-Duran, A.; Gutierrez-Perez, J.L.; Torres-Lagares, D. Fracture resistance of endodontically treated teeth restored with glass fiber reinforced posts and cast gold post and cores cemented with three cement. J. Prosthet. Dent. 2013, 110, 127−133. [Google Scholar] [CrossRef] [PubMed]
- Tsujimoto, A.; Barkmeier, W.W.; Takamizawa, T.; Wilwerding, T.M.; Latta, M.A.; Miyazaki, M. Interfacial characteristics and bond durability of universal adhesive to various substrates. Oper. Dent. 2017, 42, e59–e70. [Google Scholar] [CrossRef] [PubMed]
- Ona, M.; Wakabayashi, N.; Yamazaki, T.; Takaichi, A.; Igarashi, Y. The influence of elastic modulus mismatch between tooth and post and core restorations on root fracture. Int. Endod. J. 2013, 46, 47−52. [Google Scholar] [CrossRef]
- ThanNaing, S.; Abdou, A.; Sayed, M.; Sumi, Y.; Tagami, J.; Hiraishi, N. Dentin anti-demineralization potential of surface reaction-type pre-reacted glass-ionomer filler containing self-adhesive resin cement. Clin. Oral Investig. 2022, 26, 1333–1342. [Google Scholar] [CrossRef]
- Tian, T.; Tsoi, J.K.-H.; Matinlinna, J.P.; Burrow, M.F. Aspects of bonding between resin luting cements and glass ceramic materials. Dent. Mater. 2014, 30, e147−e162. [Google Scholar] [CrossRef] [PubMed]
- Hooshmand, T.; van Noort, R.; Keshvad, A. Storage effect of a pre-activated silane on the resin to ceramic bond. Dent. Mater. 2004, 20, 635−642. [Google Scholar] [CrossRef]
- Tian, T.; Tsoi, J.K.-H.; Matinlinna, J.P.; Burrow, M.F. Aspects of bonding between resin luting cements and glass ceramic materials. Dent. Mater. 2014, 30, e147−e162. [Google Scholar] [CrossRef] [PubMed]
- Yoshihara, K.; Nagaoka, N.; Sonoda, A.; Maruo, Y.; Makita, Y.; Okihara, T.; Irie, M.; Yoshida, Y.; Van Meerbeek, B. Effectiveness and stability of silane coupling agent incorporated in “universal” adhesives. Dent. Mater. 2016, 32, 1218−1225. [Google Scholar] [CrossRef]
- Gutierrez, M.F.; Sutil, E.; Malaquias, P.; de Paris Matos, P.; de Souza, L.M.; Reis, A.; Perdigao, J.; Loguercio, A.D. Effect of self-curing activators and curing protocols on adhesive properties of universal adhesives bonded to dual-cured composites. Dent. Mater. 2017, 33, 775−787. [Google Scholar] [CrossRef]
- Dyer, S.; Walton, T.R.; Pegoraro, A.A. E-glass and S-glass fiber reinforced posts: physical properties and clinical performance. J. Prosthet. Dent. 2004, 92, 447−453. [Google Scholar]
- Luhrs, A.-K.; Pongprueksa, P.; De Munck, J.; Geurtsen, W.; Van Meerbeek, B. Curing mode affects bond strength of adhesively luted composite CAD/CAM restorations to dentin. Dent. Mater. 2014, 30, 281−291. [Google Scholar] [CrossRef]
- Madrigal, E.L.; Tichy, A.; Hosaka, K.; Ikeda, M.; Nakajima, M.; Tagami, J. The effect of curing mode of dual-cure cements on bonding performance of universal adhesives to enamel, dentin and various restorative materials. Dent. Mater. J. 2021, 40, 446−454. [Google Scholar] [CrossRef]
- Irie, M.; Maruo, Y.; Nishigawa, G.; Yoshihara, K.; Matsumoto, T. Flexural strength of resin core build-up materials: Correlation to root dentin shear bond strength and pull-out force. Polym. 2020, 12, 2947. [Google Scholar] [CrossRef] [PubMed]
- Irie, M.; Okada, M.; Maruo, Y.; Nishigawa, G.; Matsumoto, T. Shear bond strength of resin luting materials to lithium disilicate ceramic: Correlation between flexural strength and modulus of elasticity. Polym. 2023, 15, 1128. [Google Scholar] [CrossRef]
- Irie, M.; Okada, M.; Maruo, Y.; Nishigawa, G.; Matsumoto, T. Long-term bonding performance of one-bottle vs. two-bottle bonding agents to lithium disilicate ceramics. Polym. 2024, 16, 2266. [Google Scholar] [CrossRef] [PubMed]
- Available online: ://tokuyama-dental.eu/en/shop/bonding-agents-adhesives/15312-universal-bond-ii.

| Product | Composition | Manufacturer | Batch No. |
| RelyX Universal Resin Cement | Surface treated glass powder filler, Phosphate ester monomer, TEGDMA, DiurethaneDimethacrylate, Silica filler, Initiator, Titanium Dioxide | Solventum, Seefeld, Germany | 11531204 |
| Clearfil DC Core Automix ONE | Bis-GMA, TEGDMA, Hydrophilic aliphatic dimethacrylate, Hydrophobic aromatic dimethacrylate, Silanated barium glass filler, Silanated colloidal silica, Colloidal silica, dl-Camphor Quinone, Aluminum oxide filler, Initiators, Accelerators, Pigments. Filler content: 74 wt.%, 52 vol.%. | Kuraray Noritake Dental, Tainai, Niigata, Japan | 8L06384 |
| ESTECORE | Bis-GMA, TEGDMA, Bis-MPEPP, Silica-Zirconia Filler, Camphorquinone, Peroxide, Radial amplifier, Others, Filler content: 75 wt.% | Tokuyama Dental, Tokyo, Japan | U295 |
| ESTECEM II Plus | Paste A: Bis-GMA, TEGDMA, Bis-MPEPP, Silica-Zirconia Filler Paste B: Bis-GMA, TEGDMA, Bis-MPEPP, Silica-Zirconia Filler, Camphorquinone, Peroxide, Filler content: 74 wt.%. |
Tokuyama Dental, Tokyo, Japan |
A09719 |
| UniFil Core EM | UDMA, Dimethacrylate, Fluoroaluminosilicate glass, Iron oxide, Dibenzoyl peroxide, Butylated hydroxytoluene, Filler content: 75 wt.% | GC, Hasunuma, Itabashi, Tokyo, Japan | 2302201 |
| MultiCore Flow | Ytterbium trifluoride, Bis-GMA, UDMA, TEGDMA, Dibenzoyl peroxide, Filler content: 70 wt. %, 46 vol. %, The particle size ranges from 0.04 to 25 µm. | Ivoclar Vivadent AG, Schaan, Liechtenstein | ZO7ZCY |
| BeaitiLink SA | Paste A: Zirconium silicate filler, Bis-GMA, Phosphonic acid monomer, Carboxylic acid monomer, Polymerization initiator, Others Paste B: Glass powder filler (S-PRG filler), UDMA, Polymerization initiator, Pigments, Others Filler content: approximately 60 wt.% |
Shofu, Kyoto, Japan |
122303 |
| NX3 | Barium Aluminoborosilicate glass, Ytterbium trifluoride, Fumed Silica, TEGDMA, UDMA, EBPADMA, Initiator, Stabilizer, Filler content: 67.5 wt.%, 43.3 vol.% | Kerr, Orange CA, USA |
A172592 |
| Core-X flow | Urethane Dimethacrylate, Di- & Tri-functional Methacrylates, Barium Boron, Fluoroaluminosilicate Glass, Camphorquinone (CQ) Photoinitiator, Photoaccelerators, Silicon Dioxide, Benzoyl Peroxid | DENTSPLY Caulk, Milford | DE 19963 |
| SI-300381 | Paste A: Fluoroboroaluminosilicate glass, Bis-GMA, TEGDMA, Polymerization initiator, Pigments, Others Paste B: Fluoroboroaluminosilicate glass, Bis-GMA, TEGDMA, Polymerization initiator, Others |
Shofu, Kyoto, Japan | 250517D |
| i-TFC system Post Resin | Dimethacrylates, Silica, Barium glass filler, Photoinitiators, Stabilizer, Others Filler content: 67 wt.% | SUN MEDICAL, Moriyama, Japan | MX13 |
| Adhesive | Batch No. | Composition | Manufacturer | Surface treatment |
| Scotchbond Universal Plus Adhesive | 8846013 | Brominated dimethacrylate, HEMA, Silane Treated Silica, Vitrabond Copolymer, MDP, Initiators, MPTES,Ethanol, Water | 3M, Seefeld, Germany | Scotchbond Universal Plus Adhesive (20 s) – air (5 s) |
| CLEAFIL Universal Bond Quick 2 | AH0023 | 3-Methacryloxypropyl trimethoxysilane, MDP, Ethanol |
Kuraray Noritake Dental, Tainai, Niigata, Japan | CLEAFIL CERAMIC PRIMER PLUS (1-2 s) – air (5 s) |
| G-Cem One Multi Primer | 2104221 | Vinyl silane, Phosphate ester monomer, Thiophosphate ester monomer, Methacrylic ester, Ethanol |
GC, Hasunuma, Itabashi, Tokyo, Japan | G-Cem One Multi Primer (10 s) – air (5 s) |
| Tokuyama Universal Bond II (A+B) | Bond A: 0011 Bond B: 0510 |
Liquid A: Phosphoric acid monomer (New 3D-SR monomer), MTU-6, HEMA, Bis-GMA, TEGDMA, Acetone, Others. Liquid B: γ-MPTES, Borate, Peroxide, Acetone, Ethanol, Water, Others |
Tokuyama Dental, Tokyo, Japan | Tokuyama Universal Bond II Mix (Liquid A + Liquid B, 1-2 s) – air (5 s) |
| Monobond Plus | ZO1LG8 | Phosphoric acid monomer, Silane methacylate, Ethanol | Ivoclar Vivadent AG, Schaan, Liechtenstein | Monobond Plus (60 s) – air |
| BeautiBond Xtreme | 042347 | Acetone, Water, Bis-GMA, TEGDMA, Phosphoric ester monomer, Silane coupling agent, Initiator, Others | Shofu, Kyoto, Japan | BeautiBond Xtreme (20 s) – air |
| OptiBond eXTRa Universal | Primer: 8199022 Adhesive: 8181793 |
HEMA, dimethacrylate monomers, tri-functional methacrylate monomer, Ethanol, Photo-initiator, Bariumaluminosilicate filler, Silica, Sodium hexafluorosilicate | Kerr, Orange CA, USA | OptiBond eXTRa Adhesive (15 s) – air (5 s) – LED light (5 s) |
| Prime&Bond universal | DE 19963 | Phosphoric acid modified acrylate resin, Multifunctional acrylate,, Bifunctional acrylate, Acidic acrylate, Isopropanol, Water, Initiator, Stabilizer | DENTSPLY Caulk, Milford |
Endodontic post cementation 1. Apply mixture of Prime&Bond universal & Dentsply Self cure Activator post surface 2. Leave it undisturbed for 10 sec. and dry naturally Post Cementation Core-X flow into the post space and immediately insert the post into the post space. Light-cure from every aspect using a light-curing unit to fix the post: Halogen for 20 sec. |
| SI-303062 | Primer A: 250317 Primer B: 250314 |
Primer A: Acetone, Distilled water, Bis-GMA, Carboxylic acid monomer, TEGDMA, Phosphonic acid monomer, others Primer B: Distilled water, Acetone, initiator |
Shofu, Kyoto, Japan |
Preparation of the post Apply SHOFU Porcelain Primer to the post in one layer with a disposable brush. Leave it undisturbed for 10 sec. and dry naturally Pretreatment of post space Primer A and Primer B in equal amounts and apply the mixture onto the entire adhesive surface of the post space. Leave undisturbed for 10 sec. Air dry with gentle air for 3 sec and then dry with stronger air to dry the surface sufficiently. Light-cure with a light-curing unit: Halogen for 10 sec. Post Cementation Fill SI-300381 Paste into the post space and immediately insert the post into the post space. Light-cure from every aspect using a light-curing unit to fix the post: Halogen for 20 sec. |
| i-TFC Luminous Bond II | Bond: FW1, Catalyst blush: ES1 |
Bond: Methacrylic acid esters (4-META, others), Acetone, water, others Catalyst blush: Aromatic amines, aromatic sulfinates |
SUN MEDICAL, Moriyama, Japan | Mix (Bond + Catalyst prush, 5 sec) – air (10 sec) – LED light (20 sec) |
| Product (Diameter) | Composition | Manufacturer | Batch No. |
| RelyX FiberPost (1.6 mm) | Glass fibers, Composite resin matrix | Solventum, Seefeld, Germany | 306831603 |
| Tokuyama FR Post (1.6 mm) | Glass fibers, Colpolymer Bis-GMA resin | Tokuyama Dental, Tokyo, Japan | 1604251 |
| GC Fiber Post (1.6 mm) | Glass fibers,Metacrylate | GC, Tokyo, Japan | 1609021 |
| Clearfil AD Fiber Post (1.6 mm) | Glass fibers, Colpolymer Bis-GMA and Methacrylic acid monomer | Kuraray Noritake Dental, Tainai, Niigata, Japan | 7U0001 |
| BeautiCore FiberPost (1.6 mm) | Glass fiber, Copolymer of Bis-GMA and Methacrylic ester monomer | Shofu, Kyoro, Japan | 41601 |
| i-TFC Luminous Fiber II (1.6 mm) | Glass components: Borosilicate glass, barium oxide, and others Resin component: Dimethacrylate and diacrylate copolymer, others |
SUN MEDICAL, Moriyama, Japan | EL1S |
| Core build-up systems: Resin cement / Pretreating agent / Fiber-post | Time | t-Test * | |
| Base (1-day) | TC 20k | ||
| RelyX Universal Resin Cement / Scotchbond Universal Plus Adhesive / RelyX Fiber Post |
19.8 (4.2, 0) ab# | 19.6 (3.1, 0) e | NS |
| Clearfil DC Core Automix ONE / Clearfil Universalbond Quick 2 + Clearfil Porcelain Bond Activator / Cleafil AD Fiber Post | 24.5 (5.3, 0) abc | 23.0 (4.3, 0) efgh | NS |
| UniFil Core EM / G-Premio BOND + G-Premio BOND DCA / GC Fiber Post | 23.4 (4.6, 1) abc | 20.4 (2.4, 0) ef | NS |
| ESTECEM II / Tokuyama Universal Bond II (A+B) / Tokuyama FR Post |
26.7 (3.6, 0) c | 23.1 (3.9, 0) efgh | NS |
| ESTECORE Hand Type / Tokuyama Universal Bond II (A+B) / Tokuyama FR Post |
26.4 (2.9, 0) c | 25.6 (3.2, 0) efg | NS |
| MultiCore Flow / Monobond Plus / BeautiCore Fiber | 23.7 (5.0, 0) abc | 18.9 (2.7, 0) e | S |
| NX3 / OptiBond XTR + Porcelain Primer (Shofu) / BeautiCore Fiber | 26.6 (4.9, 0) c | 18.9 (3.2, 0) e | S |
| BeautiLink SA Automix + BeautiBond Xtreme, BeautiCore FiberPost | 25.2 (3.6, 0) bc | 24.1 (3.1, 0) efgh | NS |
| SI-303062 (A + B) / SI-300381 / Post pretreated by BeautiBond Xtreme / BeautiCore FiberPost | 28.7 (2.7, 0) d | 28.0 (2.6, 0) h | NS |
| core-X flow / Prime&Bond universal + Self cure Activator / FluoroPost | 25.5 (4.9,0) bc | 22.6 (4.7, 0) efgh | NS |
| i-TFC system Post Resin / i-TFC Luminous Bond II / i-TFC Luminous Fiber II | 21.0 (4.2, 0) abc | 22.7 (4.2, 0) efgh | NS |
| Materials / Fiber post (each manufacturer's recommended pretreatment agent) | Time | t-Test * | ||
| Base (1-day) | TC 20k | |||
| RelyX Universal Resin Cement / RelyX Fiber Post (Scotchbond Universal Plus Adhesive) | 30.5 (2.7, 0) abcde | 25.6 (3.1, 0) jk | S | |
| Clearfil DC Core Automix ONE / Clearfil AD Fiber Post (Clearfil Universalbond Quick 2) | 30.5 (3.5, 0) abcde | 30.6 (4.7, 0) jklno | NS | |
| UniFil Core EM / GC Fiber Post (G-Premio BOND + G-Premio BOND DCA) | 33.1 (5.0, 0) cdef | 34.1 (5.0, 0) mnopq | NS | |
| ESTECEM II / Tokuyama FR Post (Tokuyama Universal Bond II) | 41.2 (3.4, 0) hi | 41.8 (2.5, 0) s | NS | |
| ESTECORE Hand Type / Tokuyama FR Post (Tokuyama Universal Bond II) | 40.5 (3.7, 0) hi | 44.3 (3.3, 0) s | NS | |
| MultiCore Flow / BeautiCore Fiber (Monobond Plus) | 36.5 (1.5, 0) ghi | 23.6 (2.7, 0) j | S | |
| NX3 / BeautiCore Fiber (OptiBond XTR + Porcelain Primer) | 40.2 (4.5, 0) ghi | 27.9 (4.6, 0) jklmn | S | |
| BeautiLink SA Automix / BeautiCore FiberPost (BeautiBond Xtreme) | 32.9 (2.3, 0) bcdef | 29.4 (3.9, 0) jklm | NS | |
| SI-303062 / BeautiCore FiberPost (BeautiBond Xtreme) | 37.2 (3.5, 0) fghi | 35.3 (3.3, 0) nopqr | NS | |
| core-X flow / FluoroPost (Prime&Bond universal + Self cure Activator) | 32.1 (4.1, 0) bcdef | 26.9 (3.4, 0) jkl | NS | |
| i-TFC system Post Resin / i-TFC Luminous Fiber II (i-TFC Luminous Bond II) | 33.9 (4.0, 0) cdef | 32.6 (5.0, 0) lmnop | NS | |
| Materials / Fiber post (pretreated by Tokuyama Universal Bond II) | Time | t-Test * | ||
| Base (1-day) | TC 20k | |||
| RelyX Universal Resin Cement / RelyX Fiber Post | 34.2 (4.5, 0) abcd | 38.2 (4.7, 0) lmnopq | NS | |
| Clearfil DC Core Automix ONE / Clearfil AD Fiber Post | 34.7 (4.5, 0) abcde | 35.5 (3.0, 0) jklmno | NS | |
| UniFil Core EM / GC Fiber Post | 38.0 (4.0, 0) bcdefgh | 32.7 (2.8, 0) jkl | S | |
| ESTECEM II / Tokuyama FR Post | 41.2 (3.4, 0) fghi | 41.8 (2.5, 0) pqr | NS | |
| ESTECORE Hand Type / Tokuyama FR Post | 40.5 (3.7, 0) efghi | 44.3 (3.3, 0) r | NS | |
| MultiCore Flow / BeautiCore FiberPost | 42.5 (1.2, 0) hi | 36.9 (5.5, 0) klmnopq | S | |
| NX3 / BeautiCore FiberPost | 39.0 (2.6, 0) defghi | 32.3 (1.7, 0) jkl | S | |
| BeautiLink SA Automix / BeautiCore FiberPost | 35.8 (4.1, 0) abcdefg | 32.0 (3.1, 0) jk | NS | |
| SI-303062 / BeautiCore FiberPost | 38.0 (4.0, 1) bcdefgh | 35.0 (3.7, 0) jklmno | NS | |
| core-X flow / FluoroPost | 35.7 (2.9, 0) abcdef | 32.8 (4.4, 0) jkl | NS | |
| i-TFC system Post Resin / i-TFC Luminous Fiber II | 33.2 (3.8, 0) abcd | 30.1 (5.8, 0) j | NS | |
| RelyX Universal Resin Cement | Clearfil DC Core Automix ONE | UniFil Core EM | ESTECEM II | |||||||
| Base | TC 20k | Base | TC 20k | Base | TC 20k | Base | TC 20k | |||
| NS | S | NS | NS | NS | NS | NS | NS | |||
| ESTECORE Hand Type | MultiCore Flow | NX3 | BeautiLink SA Automix | |||||||
| Base | TC 20k | Base | TC 20k | Base | TC 20k | Base | TC 20k | |||
| NS | NS | NS | S | NS | S | NS | NS | |||
| SI-303062 | core-X flow | i-TFC system Post Resin | ||||||||
| Base | TC 20k | Base | TC 20k | Base | TC 20k | |||||
| NS | NS | NS | S | NS | NS | |||||
| Materials / Pretreating agent | Time | t-Test * | |
| Base (1-day) | TC 20k | ||
| RelyX Universal Resin Cement / Scotchbond Universal Plus Adhesive | 22.3 (3.9, 0) cd | 19.2 (3.4, 0) fghi | NS |
| Clearfil DC Core Automix ONE / Clearfil Universalbond Quick 2 | 23.7 (3.7, 0) de | 22.8 (2.9, 0) hij | NS |
| UniFil Core EM / G-Premio BOND + G-Premio BOND DCA | 18.0 (4.1, 0) abc | 19.0 (3.3, 0) fghi | NS |
| ESTECEM II / Tokuyama Universal Bond II | 22.0 (2.4, 0) bcd | 20.3 (2.0, 0) fghi | NS |
| ESTECORE Hand Type / Tokuyama Universal Bond II | 22.5 (3.5, 0) cd | 21.6 (2.2, 0) fghi | NS |
| MultiCore Flow / Monobond Plus | 21.2 (2.8, 0) abcd | 21.5 (3.3, 0) fghi | NS |
| NX3 / OptiBond XTR | 22.5 (3.0, 0) cd | 16.8 (2.3, 0) fg | S |
| BeautiLink SA Automix / BeautiBond Xtreme | 28.0 (4.3, 0) e | 19.9 (2.4, 0) fghi | S |
| SI-303062 / BeautiBond Xtreme | 21.0 (2.6, 0) abcd | 18.6 (1.9, 0) fghi | NS |
| core-X flow / Prime&Bond universal + Self cure Activator | 20.7 (4.2, 0) abcd | 18.1 (2.4, 0) fgh | NS |
| i-TFC system Post Resin / i-TFC Luminous Bond II | 17.8 (2.9, 0) abc | 16.4 (3.3, 0) f | NS |
| Materials | Time | t-Test * | |
| Base (1-day) | TC 20k | ||
| RelyX Universal Resin Cement | 117.5 (7.0) c | 108.8 (8.8) kl | NS |
| Clearfil DC Core Automix ONE | 140.6 (9.6) efgh | 140.9 (8.6) pqr | NS |
| UniFil Core EM | 153.6 (11.4) i | 151.2 (12.1) rs | NS |
| ESTECEM II | 162.1 (11.7) i | 146.4 (10.1) qr | S |
| ESTECORE Hand Type | 172.2 (10.2) i | 153.9 (13.3) rs | S |
| MultiCore Flow | 142.1 (9.1) fgh | 126.3 (8.2) mno | S |
| NX3 | 123.7 (9.8) cd | 97.9 (8.7) k | S |
| BeautiLink SA Automix | 128.9 (5.3) cdef | 101.7 (9.3) k | S |
| SI-303062 | 133.3 (6.4) defg | 132.2 (5.8) mnopq | NS |
| core-X flow | 136.0 (9.7) defg | 128.0 (10.6) mnop | NS |
| i-TFC system Post Resin | 139.4 (6.4) efgh | 143.6 (9.0) pqr | S |
| Materials | Time | t-Test * | |
| Base (1-day) | TC 20k | ||
| RelyX Universal Resin Cement | 4.27 (0.41) a | 4.24 (0.28) i | NS |
| Clearfil DC Core Automix ONE | 8.43 (0.55) cde | 10.57 (1.10) nop | S |
| UniFil Core EM | 11.12 (0.92) fg | 11.26 (0.52) pq | NS |
| ESTECEM II | 12.42 (1.79) g | 10.72 (0.67) op | S |
| ESTECORE Hand Type | 13.80 (1.35) h | 12.52 (0.59) r | NS |
| MultiCore Flow | 8.44 (0.47) cde | 7.77 (0.81) kl | NS |
| NX3 | 5.97 (0.49) b | 5.90 (0.46) j | NS |
| BeautiLink SA Automix | 8.49 (0.95) cde | 7.91 (0.86) kl | NS |
| SI-303062 | 8.97 (0.77) de | 9.27 (0.96) mn | NS |
| core-X flow | 8.86 (0.82) de | 9.75 (0.77) mno | NS |
| i-TFC system Post Resin | 7.35 (0.52) c | 7.92 (0.35) kl | NS |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




