Submitted:
04 February 2026
Posted:
05 February 2026
You are already at the latest version
Abstract
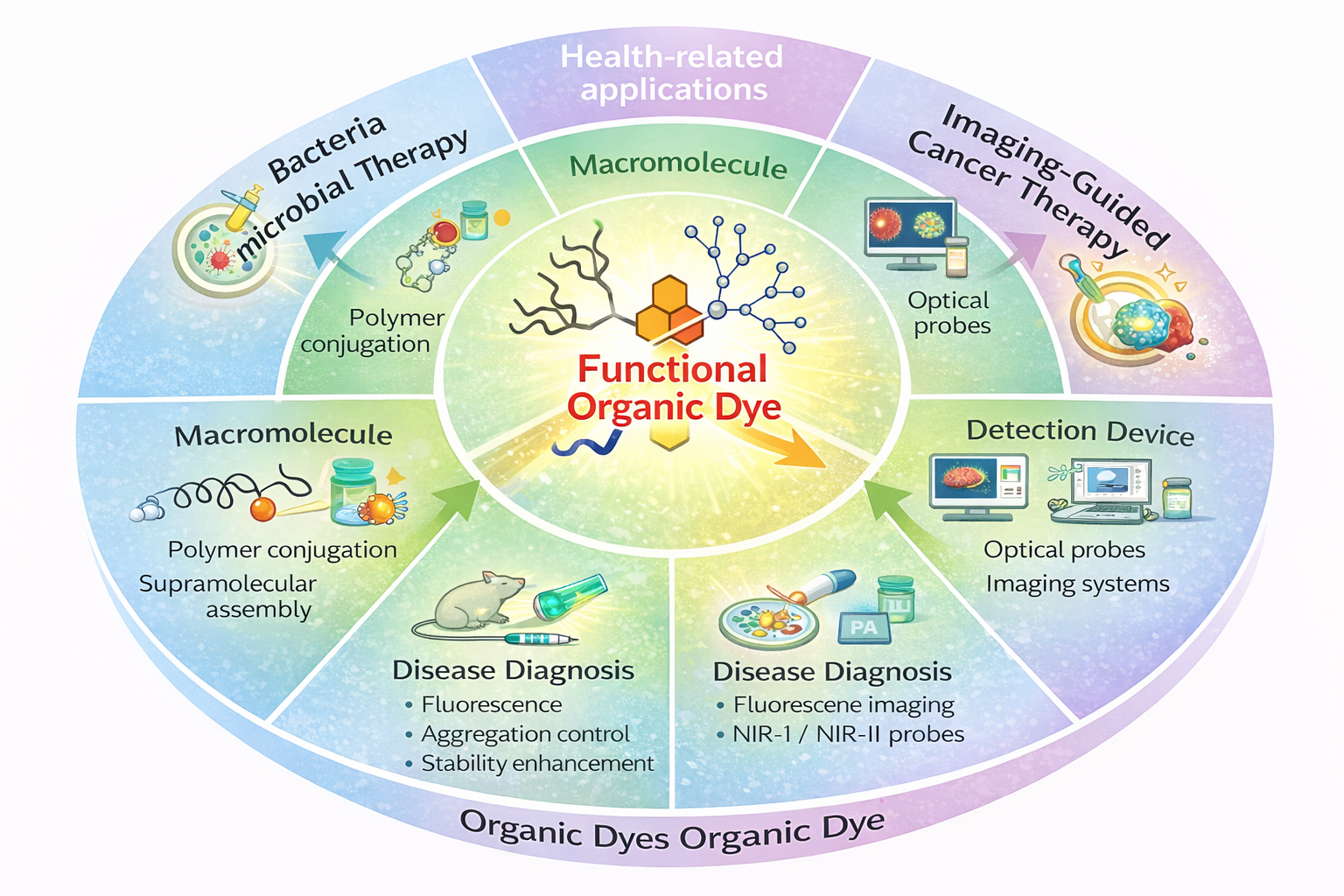
Keywords:
1. Introduction
2. Design Strategy
3. Healthcare Applications
3.1. Antimicrobial and Antibacterial Applications
3.2. Disease Diagnosis
3.2.1. In Vitro Diagnosis
3.2.2. In Vivo Diagnosis
4. Photoacoustic Imaging Applications
5. SERS Based Imaging
6. Cardiovascular Imaging
7. Light Based Therapy
7.1. Dyes for Photothermal Therapy Applications
7.2. Organic Dyes for Photodynamic Therapy (PDT)
8. Dyes for Intraoperative Surgery Guidance and Therapy
9. Summary and Outlook
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Baldini, F.; Dholakia, K.; French, P.; Guntinas-Lichius, O.; Kohler, A.; Mäntele, W.; Marcu, L.; Sroka, R.; Umapathy, S.; Popp, J. Shining a Light on the Future of Biophotonics. J. Biophotonics 2025, 18, e202500148. [CrossRef]
- Banstola, A.; Lin, Z.-T.; Li, Y.; Wu, M.X. PhotoChem Interplays: Lighting the Way for Drug Delivery and Diagnosis. Adv. Drug Deliv. Rev. 2025, 219, 115549. [CrossRef]
- Datta, R.; Heaster, T.M.; Sharick, J.T.; Gillette, A.A.; Skala, M.C. Fluorescence Lifetime Imaging Microscopy: Fundamentals and Advances in Instrumentation, Analysis, and Applications. J. Biomed. Opt. 2020, 25, 1. [CrossRef]
- Choi, W.; Park, B.; Choi, S.; Oh, D.; Kim, J.; Kim, C. Recent Advances in Contrast-Enhanced Photoacoustic Imaging: Overcoming the Physical and Practical Challenges. Chem. Rev. 2023, 123, 7379–7419. [CrossRef]
- Pan, W.; Rafiq, M.; Haider, W.; Guo, Y.; Wang, H.; Xu, M.; Yu, B.; Cong, H.; Shen, Y. Recent Advances in NIR-II Fluorescence/Photoacoustic Dual-Modality Imaging Probes. Coord. Chem. Rev. 2024, 514, 215907. [CrossRef]
- Cuadrado, C.F.; Lagos, K.J.; Stringasci, M.D.; Bagnato, V.S.; Romero, M.P. Clinical and Pre-Clinical Advances in the PDT/PTT Strategy for Diagnosis and Treatment of Cancer. Photodiagnosis Photodyn Ther. 2024, 50, 104387. [CrossRef]
- Omidian, H.; Dey Chowdhury, S. Advances in Photothermal and Photodynamic Nanotheranostics for Precision Cancer Treatment. J. Nanotheranostics 2024, 5, 228–252. [CrossRef]
- Cai, Y.; Chai, T.; Nguyen, W.; Liu, J.; Xiao, E.; Ran, X.; Ran, Y.; Du, D.; Chen, W.; Chen, X. Phototherapy in Cancer Treatment: Strategies and Challenges. Sig. Transduct. Target. Ther. 2025, 10, 115. [CrossRef]
- Huis In ‘T Veld, R.V.; Heuts, J.; Ma, S.; Cruz, L.J.; Ossendorp, F.A.; Jager, M.J. Current Challenges and Opportunities of Photodynamic Therapy against Cancer. Pharmaceutics 2023, 15, 330. [CrossRef]
- Stenspil, S.G.; Laursen, B.W. Photophysics of Fluorescent Nanoparticles Based on Organic Dyes – Challenges and Design Principles. Chem. Sci. 2024, 15, 8625–8638. [CrossRef]
- Ostroverkhova, O. Organic Optoelectronic Materials: Mechanisms and Applications. Chem. Rev. 2016, 116, 13279–13412. [CrossRef]
- Bouachrine, M.; Ayachi, S. Organic Electronics: Pioneering the Future of Sustainable and Flexible Technology. RSC Adv. 2025, 15, 45177–45195. [CrossRef]
- Cheng, W.; Chen, H.; Liu, C.; Ji, C.; Ma, G.; Yin, M. Functional Organic Dyes for Health-related Applications. VIEW 2020, 1, 20200055. [CrossRef]
- Kumar, P.P.P.; Saxena, S.; Joshi, R. BODIPY Dyes: A New Frontier in Cellular Imaging and Theragnostic Applications. Colorants 2025, 4, 13. [CrossRef]
- Kumar, P.P.P. The Role of Perylene Diimide Dyes as Cellular Imaging Agents and for Enhancing Phototherapy Outcomes. Colorants 2025, 4, 22. [CrossRef]
- Jiang, Z.; Ding, Y.; Lovell, J.F.; Zhang, Y. Design and Application of Organic Contrast Agents for Molecular Imaging in the Second near Infrared (NIR-II) Window. Photoacoustics 2022, 28, 100426. [CrossRef]
- Zhao, M.; Chen, X. Recent Advances in NIR-II Materials for Biomedical Applications. Acc. Mater. Res. 2024, 5, 600–613. [CrossRef]
- Han, S.; Lee, D.; Kim, S.; Kim, H.-H.; Jeong, S.; Kim, J. Contrast Agents for Photoacoustic Imaging: A Review Focusing on the Wavelength Range. Biosensors 2022, 12, 594. [CrossRef]
- Li, C.; Liu, C.; Fan, Y.; Ma, X.; Zhan, Y.; Lu, X.; Sun, Y. Recent Development of Near-Infrared Photoacoustic Probes Based on Small-Molecule Organic Dye. RSC Chem. Biol. 2021, 2, 743–758. [CrossRef]
- Liu, H.; Wang, M.; Ji, F.; Jiang, Y.; Yang, M. Mini Review of Photoacoustic Clinical Imaging: A Noninvasive Tool for Disease Diagnosis and Treatment Evaluation. J. Biomed. Opt. 2024, 29. [CrossRef]
- Goloviznina, K.; Lepre, L.F.; Sabelle, S.; Pádua, A.A.H.; Costa Gomes, M. Enhancement of the Solubility of Organic Dyes in Aqueous Ionic Solvents Doped with Surfactants. Journal of Molecular Liquids 2022, 357, 118958. [CrossRef]
- Kim, J.Y.; Hwang, T.G.; Woo, S.W.; Lee, J.M.; Namgoong, J.W.; Yuk, S.B.; Chung, S.; Kim, J.P. Simple Modification of Basic Dyes with Bulky & Symmetric WCAs for Improving Their Solubilities in Organic Solvents without Color Change. Sci Rep 2017, 7, 46178. [CrossRef]
- Svechkarev, D.; Mohs, A.M. Organic Fluorescent Dye-Based Nanomaterials: Advances in the Rational Design for Imaging and Sensing Applications. Curr. Med. chem. 2019, 26, 4042–4064. [CrossRef]
- Arunkumar, E.; Forbes, C.C.; Smith, B.D. Improving the Properties of Organic Dyes by Molecular Encapsulation. Eur. J. Org. Chem. 2005, 2005, 4051–4059. [CrossRef]
- Li, Y.; Cai, Z.; Liu, S.; Zhang, H.; Wong, S.T.H.; Lam, J.W.Y.; Kwok, R.T.K.; Qian, J.; Tang, B.Z. Design of AIEgens for Near-Infrared IIb Imaging through Structural Modulation at Molecular and Morphological Levels. Nat. Commun. 2020, 11, 1255. [CrossRef]
- Cappello, D.; Buguis, F.L.; Gilroy, J.B. Tuning the Properties of Donor–Acceptor and Acceptor–Donor–Acceptor Boron Difluoride Hydrazones via Extended π-Conjugation. ACS Omega 2022, 7, 32727–32739. [CrossRef]
- Ramezani, P.; De Smedt, S.C.; Sauvage, F. Supramolecular Dye Nanoassemblies for Advanced Diagnostics and Therapies. Bioeng. Transl. Med. 2024, 9, e10652. [CrossRef]
- Zhang, Y.; Yang, Z.; Zheng, X.; Yang, L.; Song, N.; Zhang, L.; Chen, L.; Xie, Z. Heavy Atom Substituted Near-Infrared BODIPY Nanoparticles for Photodynamic Therapy. Dyes and Pigments 2020, 178, 108348. [CrossRef]
- Kumar, P.P.P.; Yadav, P.; Shanavas, A.; Neelakandan, P.P. Aggregation Enhances Luminescence and Photosensitization Properties of a Hexaiodo-BODIPY. Mater. Chem. Front. 2020, 4, 965–972. [CrossRef]
- Fang, L.; Chen, Z.; Dai, J.; Pan, Y.; Tu, Y.; Meng, Q.; Diao, Y.; Yang, S.; Guo, W.; Li, L.; et al. Recent Advances in Strategies to Enhance Photodynamic and Photothermal Therapy Performance of Single-Component Organic Phototherapeutic Agents. Adv. Sci. 2025, 12, 2409157. [CrossRef]
- Shan, G.; Weissleder, R.; Hilderbrand, S.A. Upconverting Organic Dye Doped Core-Shell Nano-Composites for Dual-Modality NIR Imaging and Photo-Thermal Therapy. Theranostics 2013, 3, 267–274. [CrossRef]
- Reisch, A.; Runser, A.; Arntz, Y.; Mély, Y.; Klymchenko, A.S. Charge-Controlled Nanoprecipitation as a Modular Approach to Ultrasmall Polymer Nanocarriers: Making Bright and Stable Nanoparticles. ACS Nano 2015, 9, 5104–5116. [CrossRef]
- Sun, X.; Xiang, T.; Xie, L.; Ren, Q.; Chang, J.; Jiang, W.; Jin, Z.; Yang, X.; Ren, W.; Yu, Y. Recent Advances in Fluorescent Nanomaterials Designed for Biomarker Detection and Imaging. Materials Today Bio 2025, 32, 101763. [CrossRef]
- Nath, P.; Mahtaba, K.R.; Ray, A. Fluorescence-Based Portable Assays for Detection of Biological and Chemical Analytes. Sensors 2023, 23, 5053. [CrossRef]
- Spagnolo, A.M. Bacterial Infections: Surveillance, Prevention and Control. Pathogens 2024, 13, 181. [CrossRef]
- Tang, X.; Qi, Q.; Li, B.; Zhu, Z.; Lu, J.; Liu, L. Recent Advances on Fluorescent Sensors for Detection of Pathogenic Bacteria. Chemosensors 2025, 13, 182. [CrossRef]
- Salam, Md.A.; Al-Amin, Md.Y.; Pawar, J.S.; Akhter, N.; Lucy, I.B. Conventional Methods and Future Trends in Antimicrobial Susceptibility Testing. Saudi J. Biol. Sci. 2023, 30, 103582. [CrossRef]
- Boehle, K.E.; Gilliand, J.; Wheeldon, C.R.; Holder, A.; Adkins, J.A.; Geiss, B.J.; Ryan, E.P.; Henry, C.S. Utilizing Paper-Based Devices for Antimicrobial-Resistant Bacteria Detection. Angew. Chem. Int. Ed. 2017, 56, 6886–6890. [CrossRef]
- Chen, S.; Chen, Q.; Li, Q.; An, J.; Sun, P.; Ma, J.; Gao, H. Biodegradable Synthetic Antimicrobial with Aggregation-Induced Emissive Luminogens for Temporal Antibacterial Activity and Facile Bacteria Detection. Chem. Mater. 2018, 30, 1782–1790. [CrossRef]
- Wang, W.; Wu, F.; Zhang, Q.; Zhou, N.; Zhang, M.; Zheng, T.; Li, Y.; Tang, B.Z. Aggregation-Induced Emission Nanoparticles for Single Near-Infrared Light-Triggered Photodynamic and Photothermal Antibacterial Therapy. ACS Nano 2022, 16, 7961–7970. [CrossRef]
- Yang, Y.; He, P.; Wang, Y.; Bai, H.; Wang, S.; Xu, J.; Zhang, X. Supramolecular Radical Anions Triggered by Bacteria In Situ for Selective Photothermal Therapy. Angew. Chem. Int. Ed. 2017, 56, 16239–16242. [CrossRef]
- Bodaghi, A.; Fattahi, N.; Ramazani, A. Biomarkers: Promising and Valuable Tools towards Diagnosis, Prognosis and Treatment of Covid-19 and Other Diseases. Heliyon 2023, 9, e13323. [CrossRef]
- Das, S.; Dey, M.K.; Devireddy, R.; Gartia, M.R. Biomarkers in Cancer Detection, Diagnosis, and Prognosis. Sensors 2023, 24, 37. [CrossRef]
- Asci Erkocyigit, B.; Ozufuklar, O.; Yardim, A.; Guler Celik, E.; Timur, S. Biomarker Detection in Early Diagnosis of Cancer: Recent Achievements in Point-of-Care Devices Based on Paper Microfluidics. Biosensors 2023, 13, 387. [CrossRef]
- Wang, Y.; Pei, H.; Jia, Y.; Liu, J.; Li, Z.; Ai, K.; Lu, Z.; Lu, L. Synergistic Tailoring of Electrostatic and Hydrophobic Interactions for Rapid and Specific Recognition of Lysophosphatidic Acid, an Early-Stage Ovarian Cancer Biomarker. J. Am. Chem. Soc. 2017, 139, 11616–11621. [CrossRef]
- Joh, D.Y.; Hucknall, A.M.; Wei, Q.; Mason, K.A.; Lund, M.L.; Fontes, C.M.; Hill, R.T.; Blair, R.; Zimmers, Z.; Achar, R.K.; et al. Inkjet-Printed Point-of-Care Immunoassay on a Nanoscale Polymer Brush Enables Subpicomolar Detection of Analytes in Blood. Proc. Natl. Acad. Sci. U.S.A. 2017, 114. [CrossRef]
- Yang, S.K.; Shi, X.; Park, S.; Doganay, S.; Ha, T.; Zimmerman, S.C. Monovalent, Clickable, Uncharged, Water-Soluble Perylenediimide-Cored Dendrimers for Target-Specific Fluorescent Biolabeling. J. Am. Chem. Soc. 2011, 133, 9964–9967. [CrossRef]
- Zhou, J.; Zhang, J.; Lai, Y.; Zhou, Z.; Zhao, Y.; Wang, H.; Wang, Z. Guanidinium-Dendronized Perylene Bisimides as Stable, Water-Soluble Fluorophores for Live-Cell Imaging. New J. Chem. 2013, 37, 2983. [CrossRef]
- Kaur, P.; Singh, K. Recent Advances in the Application of BODIPY in Bioimaging and Chemosensing. J. Mater. Chem. C 2019, 7, 11361–11405. [CrossRef]
- Collot, M.; Boutant, E.; Lehmann, M.; Klymchenko, A.S. BODIPY with Tuned Amphiphilicity as a Fluorogenic Plasma Membrane Probe. Bioconjugate Chem. 2019, 30, 192–199. [CrossRef]
- Polita, A.; Stancikaitė, M.; Žvirblis, R.; Maleckaitė, K.; Dodonova-Vaitkūnienė, J.; Tumkevičius, S.; Shivabalan, A.P.; Valinčius, G. Designing a Green-Emitting Viscosity-Sensitive 4,4-Difluoro-4-Bora-3a,4a-Diaza- s -Indacene (BODIPY) Probe for Plasma Membrane Viscosity Imaging. RSC Adv. 2023, 13, 19257–19264. [CrossRef]
- Li, A.; Wang, F.; Li, Y.; Peng, X.; Liu, Y.; Zhu, L.; He, P.; Yu, T.; Chen, D.; Duan, M.; et al. Fluorination of Aza-BODIPY for Cancer Cell Plasma Membrane-Targeted Imaging and Therapy. ACS Appl. Mater. Interfaces 2025, acsami.4c17943. [CrossRef]
- Xiong, T.; Chen, Y.; Peng, Q.; Li, M.; Lu, S.; Chen, X.; Fan, J.; Wang, L.; Peng, X. Pyrazolone-Protein Interaction Enables Long-Term Retention Staining and Facile Artificial Biorecognition on Cell Membranes. J. Am. Chem. Soc. 2024, 146, 24158–24166. [CrossRef]
- Ni, Y.; Zeng, L.; Kang, N.; Huang, K.; Wang, L.; Zeng, Z.; Chang, Y.; Wu, J. Meso -Ester and Carboxylic Acid Substituted BODIPYs with Far-Red and Near-Infrared Emission for Bioimaging Applications. Chemistry A European J 2014, 20, 2301–2310. [CrossRef]
- Jiang, X.-D.; Gao, R.; Yue, Y.; Sun, G.-T.; Zhao, W. A NIR BODIPY Dye Bearing 3,4,4a-Trihydroxanthene Moieties. Org. Biomol. Chem. 2012, 10, 6861. [CrossRef]
- Kand, D.; Liu, P.; Navarro, M.X.; Fischer, L.J.; Rousso-Noori, L.; Friedmann-Morvinski, D.; Winter, A.H.; Miller, E.W.; Weinstain, R. Water-Soluble BODIPY Photocages with Tunable Cellular Localization. J. Am. Chem. Soc. 2020, 142, 4970–4974. [CrossRef]
- Zhang, X.; Wu, Y.; Chen, L.; Song, J.; Yang, H. Optical and Photoacoustic Imaging In Vivo : Opportunities and Challenges. Chem. biomed. Imaging 2023, 1, 99–109. [CrossRef]
- Chu, B.; Chen, Z.; Shi, H.; Wu, X.; Wang, H.; Dong, F.; He, Y. Fluorescence, Ultrasonic and Photoacoustic Imaging for Analysis and Diagnosis of Diseases. Chem. Commun. 2023, 59, 2399–2412. [CrossRef]
- Asanuma, D.; Sakabe, M.; Kamiya, M.; Yamamoto, K.; Hiratake, J.; Ogawa, M.; Kosaka, N.; Choyke, P.L.; Nagano, T.; Kobayashi, H.; et al. Sensitive β-Galactosidase-Targeting Fluorescence Probe for Visualizing Small Peritoneal Metastatic Tumours in Vivo. Nat. Commun. 2015, 6, 6463. [CrossRef]
- Hu, D.; Zha, M.; Zheng, H.; Gao, D.; Sheng, Z. Recent Advances in Indocyanine Green-Based Probes for Second Near-Infrared Fluorescence Imaging and Therapy. Research 2025, 8, 0583. [CrossRef]
- Gao, Y.; Zhu, L.; Du, Z.; Xiong, J.; Ma, R.; Aili, M.; Alifu, N.; Dong, B. Recent Advances in Near-Infrared Cyanine Dye-Based Fluorescent Nanoprobes for Tumor Imaging and Therapy. Int. J. Nanotheranostics 2025, Volume 20, 13911–13937. [CrossRef]
- Sun, M.; Müllen, K.; Yin, M. Water-Soluble Perylenediimides: Design Concepts and Biological Applications. Chem. Soc. Rev. 2016, 45, 1513–1528. [CrossRef]
- Zong, L.; Zhang, H.; Li, Y.; Gong, Y.; Li, D.; Wang, J.; Wang, Z.; Xie, Y.; Han, M.; Peng, Q.; et al. Tunable Aggregation-Induced Emission Nanoparticles by Varying Isolation Groups in Perylene Diimide Derivatives and Application in Three-Photon Fluorescence Bioimaging. ACS Nano 2018, 12, 9532–9540. [CrossRef]
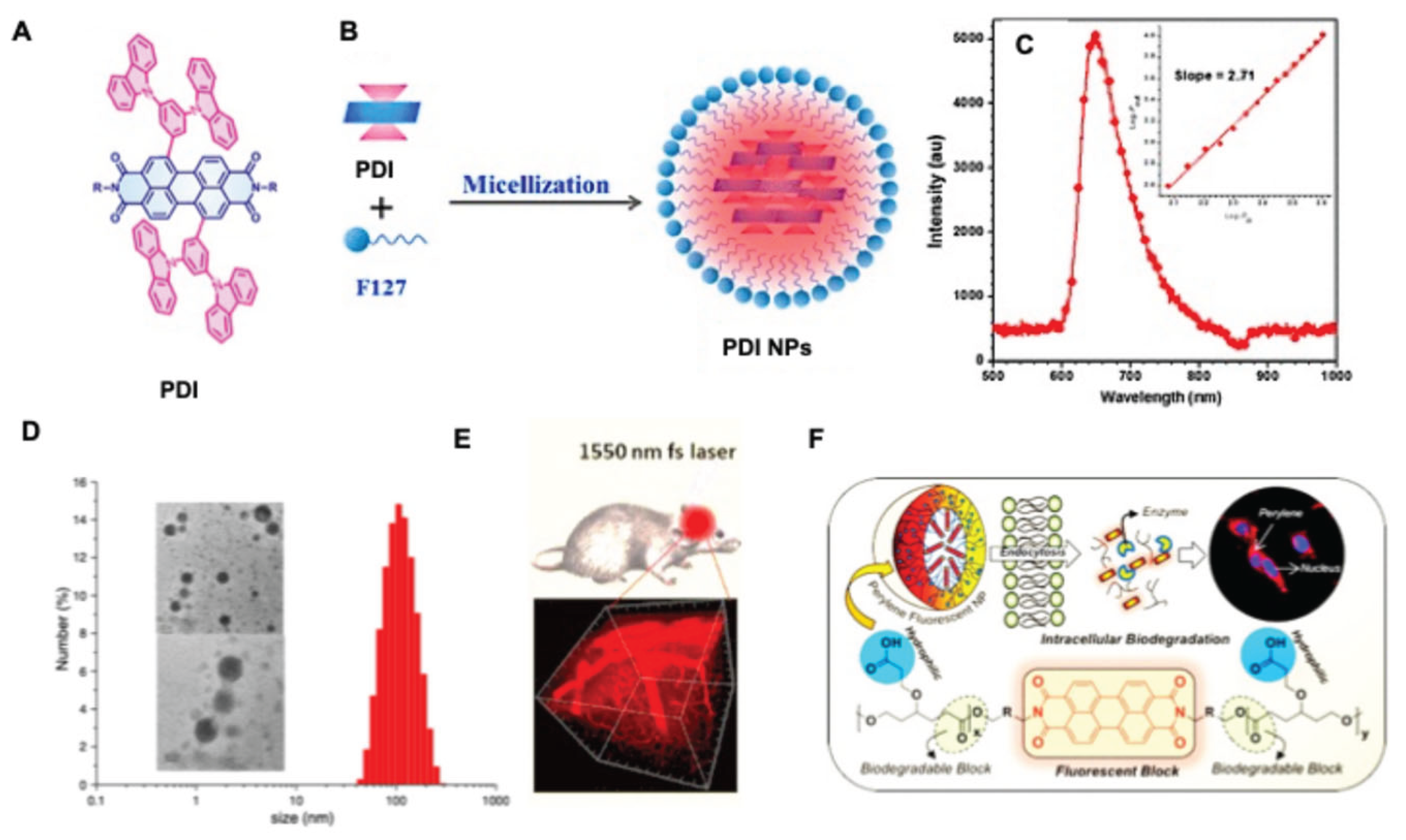
- Kulkarni, B.; Malhotra, M.; Jayakannan, M. Perylene-Tagged Polycaprolactone Block Copolymers and Their Enzyme-Biodegradable Fluorescent Nanoassemblies for Intracellular Bio-Imaging in Cancer Cells. ACS Appl. Polym. Mater. 2019, 1, 3375–3388. [CrossRef]
- Li, Z.; Lin, T.-P.; Liu, S.; Huang, C.-W.; Hudnall, T.W.; Gabbaï, F.P.; Conti, P.S. Rapid Aqueous [18F]-Labeling of a Bodipy Dye for Positron Emission Tomography/Fluorescence Dual Modality Imaging. Chem. Commun. 2011, 47, 9324. [CrossRef]
- Chansaenpak, K.; Wang, H.; Wang, M.; Giglio, B.; Ma, X.; Yuan, H.; Hu, S.; Wu, Z.; Li, Z. Synthesis and Evaluation of [18 F]-Ammonium BODIPY Dyes as Potential Positron Emission Tomography Agents for Myocardial Perfusion Imaging. Chem. Eur. J. 2016, 22, 12122–12129. [CrossRef]
- Liu, S.; Lin, T.-P.; Li, D.; Leamer, L.; Shan, H.; Li, Z.; Gabbaï, F.P.; Conti, P.S. Lewis Acid-Assisted Isotopic18 F-19 F Exchange in BODIPY Dyes: Facile Generation of Positron Emission Tomography/Fluorescence Dual Modality Agents for Tumor Imaging. Theranostics 2013, 3, 181–189. [CrossRef]
- Liu, S.; Li, D.; Zhang, Z.; Surya Prakash, G.K.; Conti, P.S.; Li, Z. Efficient Synthesis of Fluorescent-PET Probes Based on [18F]BODIPY Dye. Chem. Commun. 2014, 50, 7371. [CrossRef]
- Leiloglou, M.; Kedrzycki, M.S.; Chalau, V.; Chiarini, N.; Thiruchelvam, P.T.R.; Hadjiminas, D.J.; Hogben, K.R.; Rashid, F.; Ramakrishnan, R.; Darzi, A.W.; et al. Indocyanine Green Fluorescence Image Processing Techniques for Breast Cancer Macroscopic Demarcation. Sci. Rep. 2022, 12, 8607. [CrossRef]
- Chen, Y.; Liu, W.; Li, B.; Gao, X.; Zhou, K.; Zhang, M.; Yang, G.; Cui, M. Synthesis, Preclinical Evaluation, and First-in-Human Assessment of ICG-PSMA-D5: A PSMA-Targeted Probe for Fluorescence-Guided Surgery of Prostate Cancer. J. Med. Chem. 2025, 68, 3858–3872. [CrossRef]
- Sheng, Z.; Hu, D.; Zheng, M.; Zhao, P.; Liu, H.; Gao, D.; Gong, P.; Gao, G.; Zhang, P.; Ma, Y.; et al. Smart Human Serum Albumin-Indocyanine Green Nanoparticles Generated by Programmed Assembly for Dual-Modal Imaging-Guided Cancer Synergistic Phototherapy. ACS Nano 2014, 8, 12310–12322. [CrossRef]
- Deng, G.; Zhu, T.; Zhou, L.; Zhang, J.; Li, S.; Sun, Z.; Lai, J.; Meng, X.; Li, W.; Zhang, P.; et al. Bovine Serum Albumin-Loaded Nano-Selenium/ICG Nanoparticles for Highly Effective Chemo-Photothermal Combination Therapy. RSC Adv. 2017, 7, 30717–30724. [CrossRef]
- Beard, P. Biomedical Photoacoustic Imaging. Interface Focus. 2011, 1, 602–631. [CrossRef]
- Jung, D.; Park, S.; Lee, C.; Kim, H. Recent Progress on Near-Infrared Photoacoustic Imaging: Imaging Modality and Organic Semiconducting Agents. Polymers 2019, 11, 1693. [CrossRef]
- Kim, C.; Song, K.H.; Gao, F.; Wang, L.V. Sentinel Lymph Nodes and Lymphatic Vessels: Noninvasive Dual-Modality in Vivo Mapping by Using Indocyanine Green in Rats—Volumetric Spectroscopic Photoacoustic Imaging and Planar Fluorescence Imaging. Radiology 2010, 255, 442–450. [CrossRef]
- Sano, K.; Ohashi, M.; Kanazaki, K.; Makino, A.; Ding, N.; Deguchi, J.; Kanada, Y.; Ono, M.; Saji, H. Indocyanine Green-Labeled Polysarcosine for in Vivo Photoacoustic Tumor Imaging. Bioconjugate Chem. 2017, 28, 1024–1030. [CrossRef]
- Capozza, M.; Blasi, F.; Valbusa, G.; Oliva, P.; Cabella, C.; Buonsanti, F.; Cordaro, A.; Pizzuto, L.; Maiocchi, A.; Poggi, L. Photoacoustic Imaging of Integrin-Overexpressing Tumors Using a Novel ICG-Based Contrast Agent in Mice. Photoacoustics 2018, 11, 36–45. [CrossRef]
- Zhu, K.; Zhang, X.; Wu, Y.; Song, J. Ratiometric Optical and Photoacoustic Imaging In Vivo in the Second Near-Infrared Window. Acc. Chem. Res. 2023, 56, 3223–3234. [CrossRef]
- Wang, S.; Yu, G.; Ma, Y.; Yang, Z.; Liu, Y.; Wang, J.; Chen, X. Ratiometric Photoacoustic Nanoprobe for Bioimaging of Cu2+. ACS Appl. Mater. Interfaces 2019, 11, 1917–1923. [CrossRef]
- Li, X.; Tang, Y.; Li, J.; Hu, X.; Yin, C.; Yang, Z.; Wang, Q.; Wu, Z.; Lu, X.; Wang, W.; et al. A Small-Molecule Probe for Ratiometric Photoacoustic Imaging of Hydrogen Sulfide in Living Mice. Chem. Commun. 2019, 55, 5934–5937. [CrossRef]
- Rong, X.; Xia, X.; Wang, R.; Su, Z.; Liu, T.; Zhang, Z.; Long, S.; Du, J.; Fan, J.; Sun, W.; et al. Near-Infrared and Highly Photostable Squaraine-Based Nanoparticles for Photoacoustic Imaging Guided Photothermal Therapy. Dyes and Pigments 2023, 211, 111055. [CrossRef]
- An, F.-F.; Deng, Z.-J.; Ye, J.; Zhang, J.-F.; Yang, Y.-L.; Li, C.-H.; Zheng, C.-J.; Zhang, X.-H. Aggregation-Induced Near-Infrared Absorption of Squaraine Dye in an Albumin Nanocomplex for Photoacoustic Tomography in Vivo. ACS Appl. Mater. Interfaces 2014, 6, 17985–17992. [CrossRef]
- Merkes, J.M.; Lammers, T.; Kancherla, R.; Rueping, M.; Kiessling, F.; Banala, S. Tuning Optical Properties of BODIPY Dyes by Pyrrole Conjugation for Photoacoustic Imaging. Advanced Optical Materials 2020, 8, 1902115. [CrossRef]
- Xiang, P.; Shen, Y.; Shen, J.; Feng, Z.; Sun, M.; Zhang, Q.; Li, S.; Li, D.; Zhang, G.; Wu, Z.; et al. Functional Terpyridyl Iron Complexes for in Vivo Photoacoustic Imaging. Inorg. Chem. Front. 2020, 7, 2753–2758. [CrossRef]
- Chitgupi, U.; Lovell, J.F. Naphthalocyanines as Contrast Agents for Photoacoustic and Multimodal Imaging. Biomed. Eng. Lett. 2018, 8, 215–221. [CrossRef]
- Duffy, M.J.; Planas, O.; Faust, A.; Vogl, T.; Hermann, S.; Schäfers, M.; Nonell, S.; Strassert, C.A. Towards Optimized Naphthalocyanines as Sonochromes for Photoacoustic Imaging in Vivo. Photoacoustics 2018, 9, 49–61. [CrossRef]
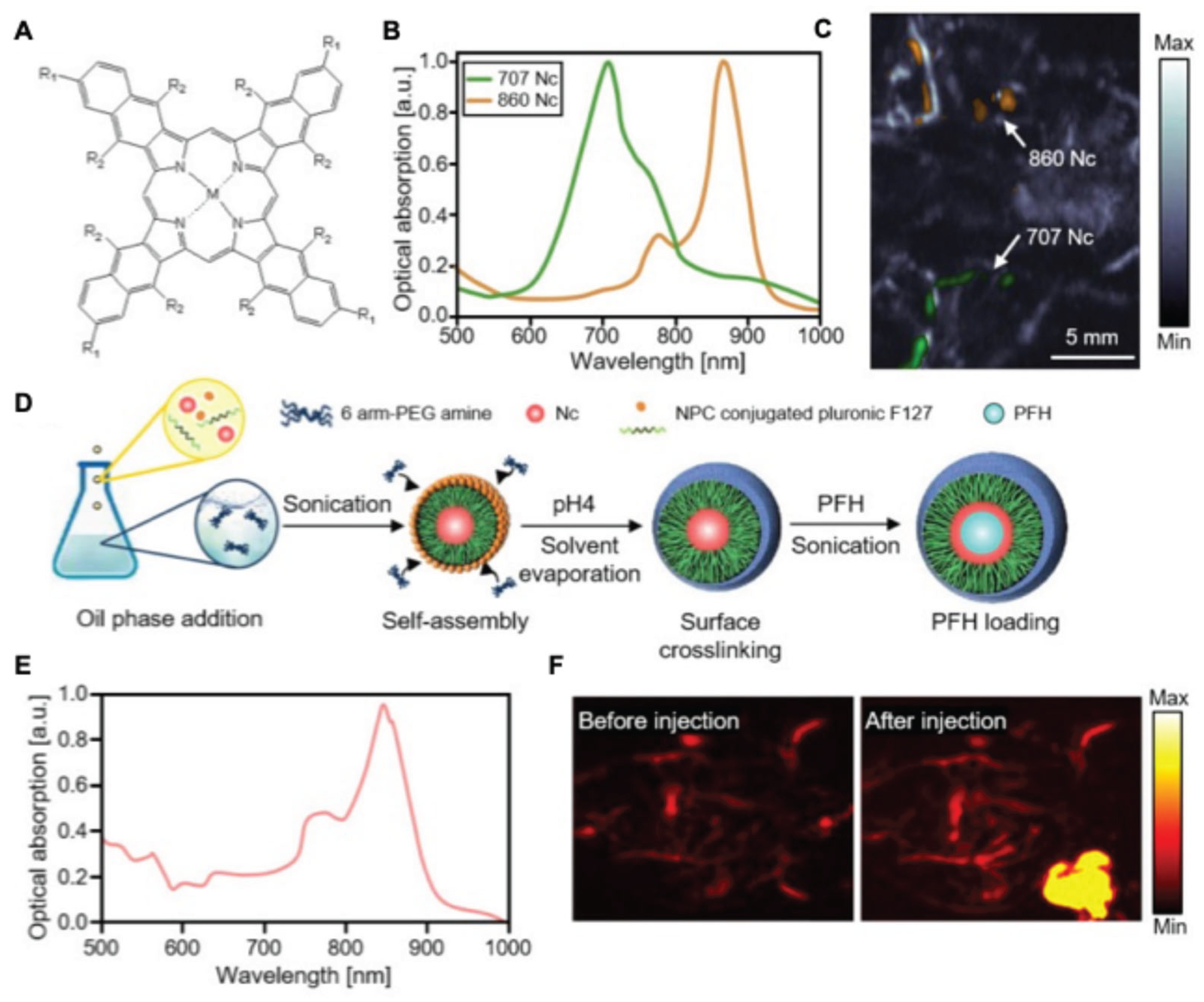
- Zhang, Y.; Jeon, M.; Rich, L.J.; Hong, H.; Geng, J.; Zhang, Y.; Shi, S.; Barnhart, T.E.; Alexandridis, P.; Huizinga, J.D.; et al. Non-Invasive Multimodal Functional Imaging of the Intestine with Frozen Micellar Naphthalocyanines. Nature Nanotech. 2014, 9, 631–638. [CrossRef]
- Lee, C.; Kim, J.; Zhang, Y.; Jeon, M.; Liu, C.; Song, L.; Lovell, J.F.; Kim, C. Dual-Color Photoacoustic Lymph Node Imaging Using Nanoformulated Naphthalocyanines. Biomaterials 2015, 73, 142–148. [CrossRef]
- Zhang, Y.; Hong, H.; Sun, B.; Carter, K.; Qin, Y.; Wei, W.; Wang, D.; Jeon, M.; Geng, J.; Nickles, R.J.; et al. Surfactant-Stripped Naphthalocyanines for Multimodal Tumor Theranostics with Upconversion Guidance Cream. Nanoscale 2017, 9, 3391–3398. [CrossRef]
- Choi, H.; Choi, W.; Kim, J.; Kong, W.H.; Kim, K.S.; Kim, C.; Hahn, S.K. Multifunctional Nanodroplets Encapsulating Naphthalocyanine and Perfluorohexane for Bimodal Image-Guided Therapy. Biomacromolecules 2019, 20, 3767–3777. [CrossRef]
- Fan, Q.; Cheng, K.; Yang, Z.; Zhang, R.; Yang, M.; Hu, X.; Ma, X.; Bu, L.; Lu, X.; Xiong, X.; et al. Perylene-Diimide-Based Nanoparticles as Highly Efficient Photoacoustic Agents for Deep Brain Tumor Imaging in Living Mice. Adv. Mater. 2015, 27, 843–847. [CrossRef]
- Yang, Y.; Fryer, C.; Sharkey, J.; Thomas, A.; Wais, U.; Jackson, A.W.; Wilm, B.; Murray, P.; Zhang, H. Perylene Diimide Nanoprobes for In Vivo Tracking of Mesenchymal Stromal Cells Using Photoacoustic Imaging. ACS Appl. Mater. Interfaces 2020, 12, 27930–27939. [CrossRef]
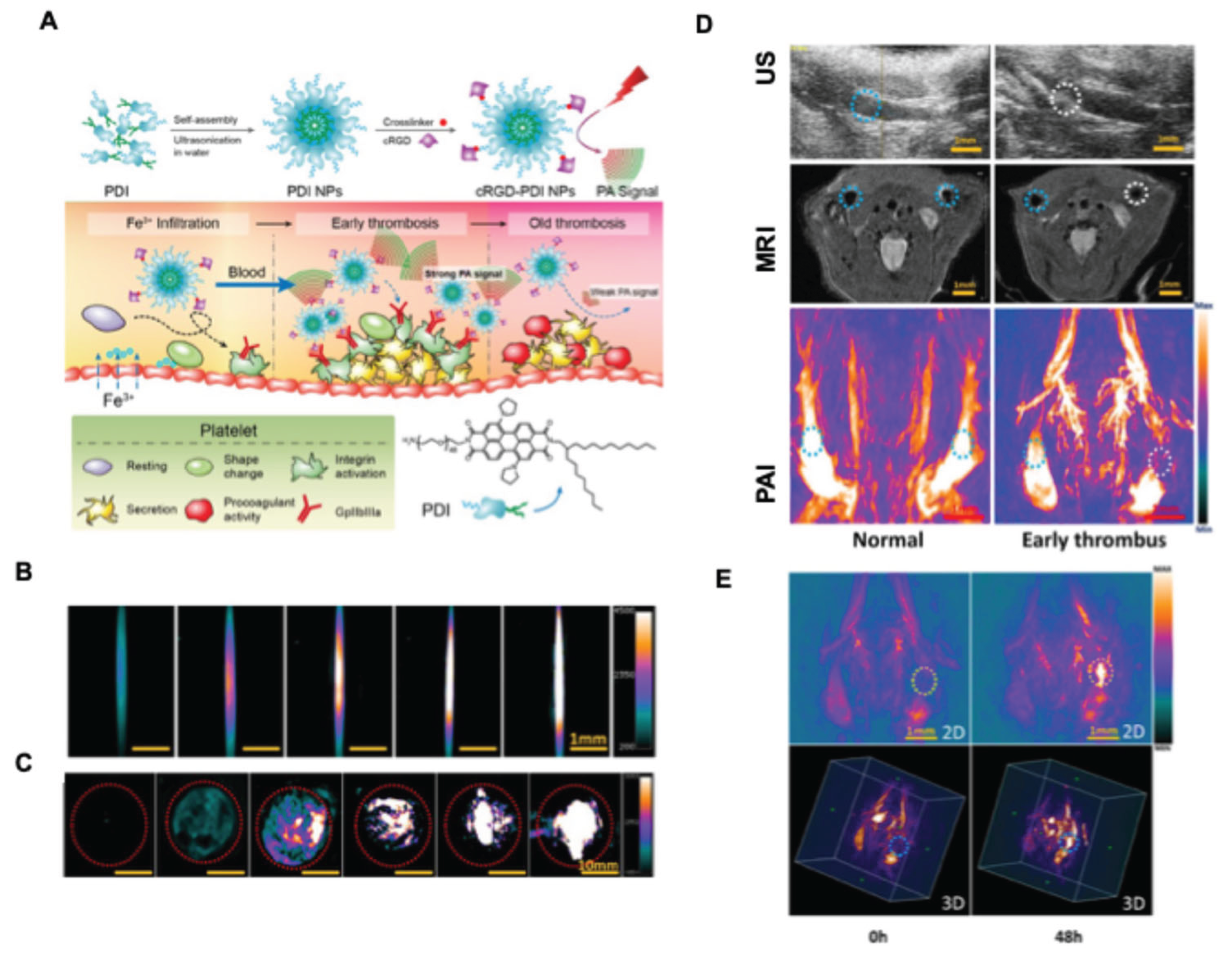
- Cui, C.; Yang, Z.; Hu, X.; Wu, J.; Shou, K.; Ma, H.; Jian, C.; Zhao, Y.; Qi, B.; Hu, X.; et al. Organic Semiconducting Nanoparticles as Efficient Photoacoustic Agents for Lightening Early Thrombus and Monitoring Thrombolysis in Living Mice. ACS Nano 2017, 11, 3298–3310. [CrossRef]
- Jokerst, J.V.; Gambhir, S.S. Molecular Imaging with Theranostic Nanoparticles. Acc. Chem. Res. 2011, 44, 1050–1060. [CrossRef]
- Wang, Y.; Yan, B.; Chen, L. SERS Tags: Novel Optical Nanoprobes for Bioanalysis. Chem. Rev. 2013, 113, 1391–1428. [CrossRef]
- Pimenta, S.; Correia, J.H. Biomedical Applications of Raman Spectroscopy: A Review. Photochem 2025, 5, 29. [CrossRef]
- Kumar, P.P.P.; Kaushal, S.; Lim, D.-K. Recent Advances in Nano/Microfabricated Substrate Platforms and Artificial Intelligence for Practical Surface-Enhanced Raman Scattering-Based Bioanalysis. Trends Anal. Chem. 2023, 168, 117341. [CrossRef]
- Wu, M.C.; Wei, J.H.; Fan, R.Y.; Sim, E.Z.; Yong, K.; Gong, T.; Kong, K.V. Self-Assembled BODIPY@Au Core-Shell Structures for Durable Neuroprotective Phototherapy. ChemBioChem. 2025, 26, e202400562. [CrossRef]
- Adarsh, N.; Ramya, A.N.; Maiti, K.K.; Ramaiah, D. Unveiling NIR Aza-Boron-Dipyrromethene (BODIPY) Dyes as Raman Probes: Surface-Enhanced Raman Scattering (SERS)-Guided Selective Detection and Imaging of Human Cancer Cells. Chemistry A European J 2017, 23, 14286–14291. [CrossRef]
- Klapper, M.; Ehmke, M.; Palgunow, D.; Böhme, M.; Matthäus, C.; Bergner, G.; Dietzek, B.; Popp, J.; Döring, F. Fluorescence-Based Fixative and Vital Staining of Lipid Droplets in Caenorhabditis Elegans Reveal Fat Stores Using Microscopy and Flow Cytometry Approaches. Journal of Lipid Research 2011, 52, 1281–1293. [CrossRef]
- Lim, D.-K.; Kumar, P.P.P. Recent Advances in SERS-Based Bioanalytical Applications: Live Cell Imaging. Nanophotonics 2024, 13, 1521–1534. [CrossRef]
- Kneipp, J.; Kneipp, H.; Rice, W.L.; Kneipp, K. Optical Probes for Biological Applications Based on Surface-Enhanced Raman Scattering from Indocyanine Green on Gold Nanoparticles. Anal. Chem. 2005, 77, 2381–2385. [CrossRef]
- Garnaik, U.; Chandra, A.; Goel, V.; Gulyás, B.; Padmanabhan, P.; Agarwal, S. Development of SERS Active Nanoprobe for Selective Adsorption and Detection of Alzheimer’s Disease Biomarkers Based on Molecular Docking. Int. J Nanomedicine. 2024, Volume 19, 8271–8284. [CrossRef]
- Kneipp, J.; Kneipp, H.; Rajadurai, A.; Redmond, R.W.; Kneipp, K. Optical Probing and Imaging of Live Cells Using SERS Labels. J. Raman Spectroscopy 2009, 40, 1–5. [CrossRef]
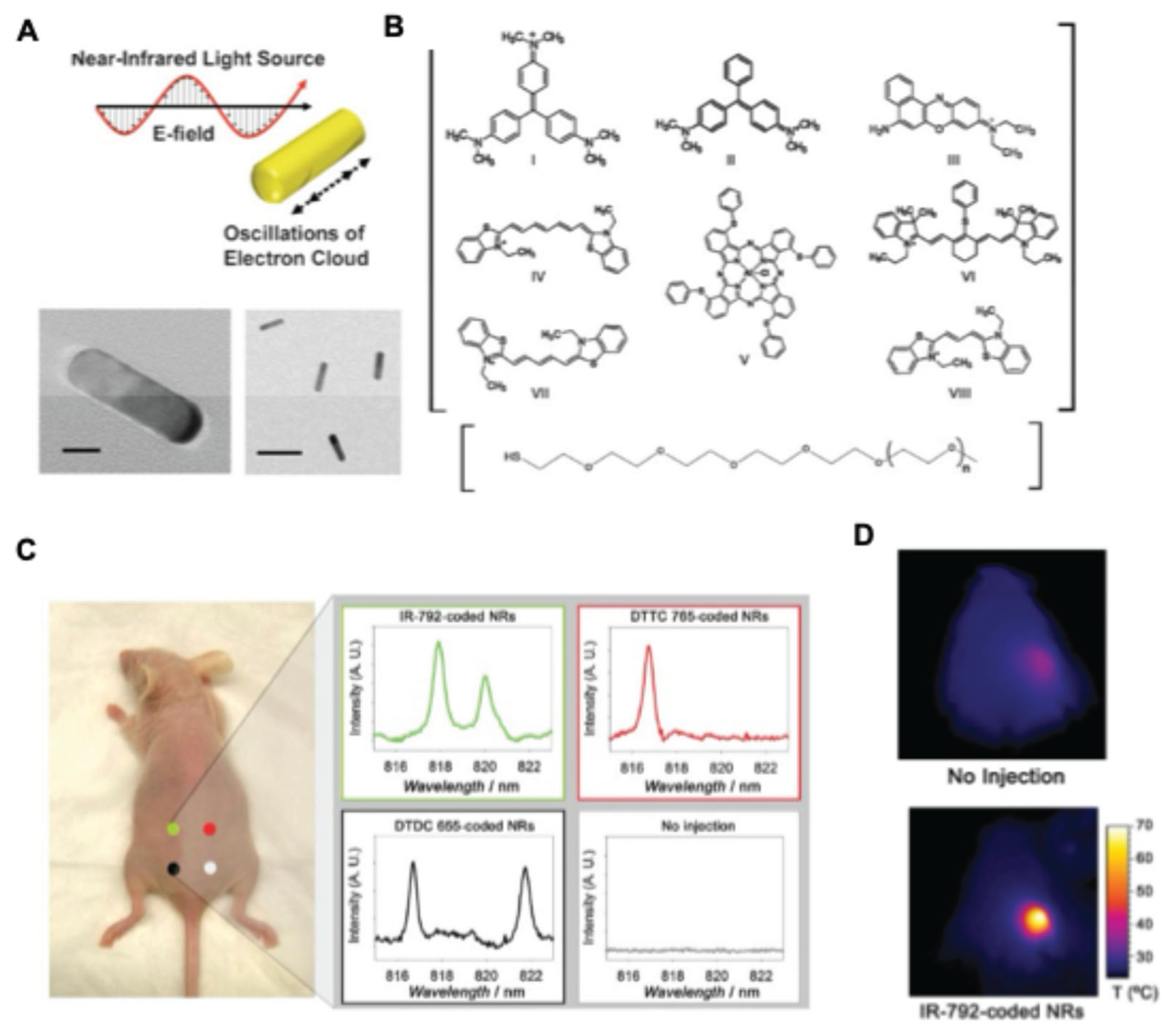
- Von Maltzahn, G.; Centrone, A.; Park, J.; Ramanathan, R.; Sailor, M.J.; Hatton, T.A.; Bhatia, S.N. SERS-Coded Gold Nanorods as a Multifunctional Platform for Densely Multiplexed Near-Infrared Imaging and Photothermal Heating. Adv. Mater. 2009, 21, 3175–3180. [CrossRef]
- Wang, X.; Chen, L.; Wei, J.; Zheng, H.; Zhou, N.; Xu, X.; Deng, X.; Liu, T.; Zou, Y. The Immune System in Cardiovascular Diseases: From Basic Mechanisms to Therapeutic Implications. Sig Transduct Target Ther. 2025, 10, 166. [CrossRef]
- Li, B.; Zhao, M.; Feng, L.; Dou, C.; Ding, S.; Zhou, G.; Lu, L.; Zhang, H.; Chen, F.; Li, X.; et al. Organic NIR-II Molecule with Long Blood Half-Life for in Vivo Dynamic Vascular Imaging. Nat. Commun. 2020, 11, 3102. [CrossRef]
- Sun, C.; Li, B.; Zhao, M.; Wang, S.; Lei, Z.; Lu, L.; Zhang, H.; Feng, L.; Dou, C.; Yin, D.; et al. J -Aggregates of Cyanine Dye for NIR-II in Vivo Dynamic Vascular Imaging beyond 1500 Nm. J. Am. Chem. Soc. 2019, 141, 19221–19225. [CrossRef]
- Narita, Y.; Shimizu, K.; Ikemoto, K.; Uchino, R.; Kosugi, M.; Maess, M.B.; Magata, Y.; Oku, N.; Ogawa, M. Macrophage-Targeted, Enzyme-Triggered Fluorescence Switch-on System for Detection of Embolism-Vulnerable Atherosclerotic Plaques. Journal of Controlled Release 2019, 302, 105–115. [CrossRef]
- Park, S.-J.; Kim, B.; Choi, S.; Balasubramaniam, S.; Lee, S.-C.; Lee, J.Y.; Kim, H.S.; Kim, J.-Y.; Kim, J.-J.; Lee, Y.-A.; et al. Imaging Inflammation Using an Activated Macrophage Probe with Slc18b1 as the Activation-Selective Gating Target. Nat. Commun. 2019, 10, 1111. [CrossRef]
- Li, L.; Chen, Y.; Chen, W.; Tan, Y.; Chen, H.; Yin, J. Photodynamic Therapy Based on Organic Small Molecular Fluorescent Dyes. Chinese Chemical Letters 2019, 30, 1689–1703. [CrossRef]
- Ain, N.U.; Rehman, Z.; Ibrahim, T.K.; Kebaili, I.; Boukhris, I.; Al-Buriahi, M.S. Organic Dyes-Based Photothermal Ablation of Cancer Cells: A Review. Dyes and Pigments 2025, 237, 112687. [CrossRef]
- Kejík, Z.; Hajduch, J.; Abramenko, N.; Vellieux, F.; Veselá, K.; Fialová, J.L.; Petrláková, K.; Kučnirová, K.; Kaplánek, R.; Tatar, A.; et al. Cyanine Dyes in the Mitochondria-Targeting Photodynamic and Photothermal Therapy. Commun. Chem. 2024, 7, 180. [CrossRef]
- Mok, H.; Jeong, H.; Kim, S.-J.; Chung, B.H. Indocyanine Green Encapsulated Nanogels for Hyaluronidase Activatable and Selective near Infrared Imaging of Tumors and Lymph Nodes. Chem. Commun. 2012, 48, 8628. [CrossRef]
- Peng, C.-L.; Shih, Y.-H.; Lee, P.-C.; Hsieh, T.M.-H.; Luo, T.-Y.; Shieh, M.-J. Multimodal Image-Guided Photothermal Therapy Mediated by188 Re-Labeled Micelles Containing a Cyanine-Type Photosensitizer. ACS Nano 2011, 5, 5594–5607. [CrossRef]
- Hassan, M.; Su, Y.T.; Iqbal, S.Z.; Nawaz, R.; Wang, Y.; Jiang, W. Symmetrically Fluorinated D-π-A Structured Cyanine Dye for Highly Efficient NIR-II Imaging-Guided Cancer Phototheranostics. Small 2024, 20, 2401905. [CrossRef]
- Han, H.S.; Choi, K.Y. Advances in Nanomaterial-Mediated Photothermal Cancer Therapies: Toward Clinical Applications. Biomedicines 2021, 9, 305. [CrossRef]
- Bartusik-Aebisher, D.; Rogóż, K.; Henrykowska, G.; Aebisher, D. Advances in Near-Infrared BODIPY Photosensitizers: Design Strategies and Applications in Photodynamic and Photothermal Therapy. Pharmaceuticals 2025, 19, 53. [CrossRef]
- Kim, G.; Luo, Y.; Shin, M.; Bouffard, J.; Bae, J.; Kim, Y. Making the Brightest Ones Dim: Maximizing the Photothermal Conversion Efficiency of BODIPY-Based Photothermal Agents. Adv Healthcare Materials 2024, 13, 2400885. [CrossRef]
- Liu, Y.; Song, N.; Chen, L.; Liu, S.; Xie, Z. Synthesis of a Near-Infrared BODIPY Dye for Bioimaging and Photothermal Therapy. Chemistry An Asian Journal 2018, 13, 989–995. [CrossRef]
- Pewklang, T.; Saiyasombat, W.; Chueakwon, P.; Ouengwanarat, B.; Chansaenpak, K.; Kampaengsri, S.; Lai, R.; Kamkaew, A. Revolutionary Pyrazole-based Aza-BODIPY: Harnessing Photothermal Power Against Cancer Cells and Bacteria. ChemBioChem 2024, 25, e202300653. [CrossRef]
- Yang, Z.; Tian, R.; Wu, J.; Fan, Q.; Yung, B.C.; Niu, G.; Jacobson, O.; Wang, Z.; Liu, G.; Yu, G.; et al. Impact of Semiconducting Perylene Diimide Nanoparticle Size on Lymph Node Mapping and Cancer Imaging. ACS Nano 2017, 11, 4247–4255. [CrossRef]
- Yang, Z.; Fan, W.; Zou, J.; Tang, W.; Li, L.; He, L.; Shen, Z.; Wang, Z.; Jacobson, O.; Aronova, M.A.; et al. Precision Cancer Theranostic Platform by In Situ Polymerization in Perylene Diimide-Hybridized Hollow Mesoporous Organosilica Nanoparticles. J. Am. Chem. Soc. 2019, 141, 14687–14698. [CrossRef]
- Yuan, A.; Wu, J.; Tang, X.; Zhao, L.; Xu, F.; Hu, Y. Application of Near-Infrared Dyes for Tumor Imaging, Photothermal, and Photodynamic Therapies. Journal of Pharmaceutical Sciences 2013, 102, 6–28. [CrossRef]
- Ciubini, B.; Visentin, S.; Serpe, L.; Canaparo, R.; Fin, A.; Barbero, N. Design and Synthesis of Symmetrical Pentamethine Cyanine Dyes as NIR Photosensitizers for PDT. Dyes and Pigments 2019, 160, 806–813. [CrossRef]
- Jiao, L.; Song, F.; Cui, J.; Peng, X. A Near-Infrared Heptamethine Aminocyanine Dye with a Long-Lived Excited Triplet State for Photodynamic Therapy. Chem. Commun. 2018, 54, 9198–9201. [CrossRef]
- Kim, B.; Sui, B.; Yue, X.; Tang, S.; Tichy, M.G.; Belfield, K.D. In Vitro Photodynamic Studies of a BODIPY-Based Photosensitizer. Eur J Org Chem 2017, 2017, 25–28. [CrossRef]
- Jung, H.S.; Han, J.; Shi, H.; Koo, S.; Singh, H.; Kim, H.-J.; Sessler, J.L.; Lee, J.Y.; Kim, J.-H.; Kim, J.S. Overcoming the Limits of Hypoxia in Photodynamic Therapy: A Carbonic Anhydrase IX-Targeted Approach. J. Am. Chem. Soc. 2017, 139, 7595–7602. [CrossRef]
- Kumar, P.P.P.; Yadav, P.; Shanavas, A.; Thurakkal, S.; Joseph, J.; Neelakandan, P.P. A Three-Component Supramolecular Nanocomposite as a Heavy-Atom-Free Photosensitizer. Chem. Commun. 2019, 55, 5623–5626. [CrossRef]
- Rahman, A.; Praveen Kumar, P.P.; Yadav, P.; Goswami, T.; Shanavas, A.; Ghosh, H.N.; Neelakandan, P.P. Gold–BODIPY Nanoparticles with Luminescence and Photosensitization Properties for Photodynamic Therapy and Cell Imaging. ACS Appl. Nano Mater. 2022, 5, 6532–6542. [CrossRef]
- Kumar, P.P.P. A Multimode Detection Platform for Biothiols Using BODIPY Dye-Conjugated Gold Nanoparticles. Colorants 2024, 3, 214–228. [CrossRef]
- Praveen Kumar, P.P.; Kaur, N.; Shanavas, A.; Neelakandan, P.P. Nanomolar Detection of Biothiols via Turn-ON Fluorescent Indicator Displacement. Analyst 2020, 145, 851–857. [CrossRef]
- Chornovolenko, K.; Koczorowski, T. Phthalocyanines Conjugated with Small Biologically Active Compounds for the Advanced Photodynamic Therapy: A Review. Molecules 2025, 30, 3297. [CrossRef]
- Wang, H.; Wang, S.; Liu, Z.; Dong, C.; Yang, J.; Gong, X.; Chang, J. Upconverting Crystal/Dextran-g-DOPE with High Fluorescence Stability for Simultaneous Photodynamic Therapy and Cell Imaging. Nanotechnology 2014, 25, 155103. [CrossRef]
- Avşar, G.; Sari, F.A.; Yuzer, A.C.; Soylu, H.M.; Er, O.; Ince, M.; Lambrecht, F.Y. Intracellular Uptake and Fluorescence Imaging Potential in Tumor Cell of Zinc Phthalocyanine. International Journal of Pharmaceutics 2016, 505, 369–375. [CrossRef]
- Zhao, Z.; Chan, P.-S.; Li, H.; Wong, K.-L.; Wong, R.N.S.; Mak, N.-K.; Zhang, J.; Tam, H.-L.; Wong, W.-Y.; Kwong, D.W.J.; et al. Highly Selective Mitochondria-Targeting Amphiphilic Silicon(IV) Phthalocyanines with Axially Ligated Rhodamine B for Photodynamic Therapy. Inorg. Chem. 2012, 51, 812–821. [CrossRef]
- Li, K.; Qiu, L.; Liu, Q.; Lv, G.; Zhao, X.; Wang, S.; Lin, J. Conjugate of Biotin with Silicon(IV) Phthalocyanine for Tumor-Targeting Photodynamic Therapy. Journal of Photochemistry and Photobiology B: Biology 2017, 174, 243–250. [CrossRef]
- Zheng, B.-Y.; Yang, X.-Q.; Zhao, Y.; Zheng, Q.-F.; Ke, M.-R.; Lin, T.; Chen, R.-X.; Ho, K.K.K.; Kumar, N.; Huang, J.-D. Synthesis and Photodynamic Activities of Integrin-Targeting Silicon(IV) Phthalocyanine-cRGD Conjugates. European Journal of Medicinal Chemistry 2018, 155, 24–33. [CrossRef]
- Hill, J.E.; Linder, M.K.; Davies, K.S.; Sawada, G.A.; Morgan, J.; Ohulchanskyy, T.Y.; Detty, M.R. Selenorhodamine Photosensitizers for Photodynamic Therapy of P-Glycoprotein-Expressing Cancer Cells. J. Med. Chem. 2014, 57, 8622–8634. [CrossRef]
- Caldas, M.; Artiga, Á.; Marin, R.; Ming, L.; Jaque, D.; Silva, L.P.D.; Reis, R.L.; Correlo, V.M. Enhanced Cell Uptake of Rhodamine B for Photodynamic Therapy under Hypoxic Conditions Using Sepia Melanin Nanoparticles. ACS Appl. Nano Mater. 2025, 8, 16328–16339. [CrossRef]
- Piao, W.; Hanaoka, K.; Fujisawa, T.; Takeuchi, S.; Komatsu, T.; Ueno, T.; Terai, T.; Tahara, T.; Nagano, T.; Urano, Y. Development of an Azo-Based Photosensitizer Activated under Mild Hypoxia for Photodynamic Therapy. J. Am. Chem. Soc. 2017, 139, 13713–13719. [CrossRef]
- Chiba, M.; Ichikawa, Y.; Kamiya, M.; Komatsu, T.; Ueno, T.; Hanaoka, K.; Nagano, T.; Lange, N.; Urano, Y. An Activatable Photosensitizer Targeted to γ-Glutamyltranspeptidase. Angew Chem Int Ed 2017, 56, 10418–10422. [CrossRef]
- Wang, Z.; Liu, X.; Ma, Y.; Zheng, J.; Xu, K.; Chang, Y.; Ye, Z.; Ling, Y.; Wang, L. Novel Type I/II Carbazole/Benzindole Photosensitizers Achieve Chemo-Photodynamic Synergistic Therapy for Suppressing Solid Tumors and Drug-Resistant Bacterial Infections. Molecules 2025, 30, 2560. [CrossRef]
- Zhang, C.-J.; Hu, Q.; Feng, G.; Zhang, R.; Yuan, Y.; Lu, X.; Liu, B. Image-Guided Combination Chemotherapy and Photodynamic Therapy Using a Mitochondria-Targeted Molecular Probe with Aggregation-Induced Emission Characteristics. Chem. Sci. 2015, 6, 4580–4586. [CrossRef]
- Yuan, Y.; Zhang, C.-J.; Xu, S.; Liu, B. A Self-Reporting AIE Probe with a Built-in Singlet Oxygen Sensor for Targeted Photodynamic Ablation of Cancer Cells. Chem. Sci. 2016, 7, 1862–1866. [CrossRef]
- Wang, D.; Su, H.; Kwok, R.T.K.; Hu, X.; Zou, H.; Luo, Q.; Lee, M.M.S.; Xu, W.; Lam, J.W.Y.; Tang, B.Z. Rational Design of a Water-Soluble NIR AIEgen, and Its Application in Ultrafast Wash-Free Cellular Imaging and Photodynamic Cancer Cell Ablation. Chem. Sci. 2018, 9, 3685–3693. [CrossRef]
- Zou, J.; Lu, H.; Zhao, X.; Li, W.; Guan, Y.; Zheng, Y.; Zhang, L.; Gao, H. A Multi-Functional Fluorescent Probe with Aggregation-Induced Emission Characteristics: Mitochondrial Imaging, Photodynamic Therapy and Visualizing Therapeutic Process in Zebrafish Model. Dyes and Pigments 2018, 151, 45–53. [CrossRef]
- Hu, W.; Xie, M.; Zhao, H.; Tang, Y.; Yao, S.; He, T.; Ye, C.; Wang, Q.; Lu, X.; Huang, W.; et al. Nitric Oxide Activatable Photosensitizer Accompanying Extremely Elevated Two-Photon Absorption for Efficient Fluorescence Imaging and Photodynamic Therapy. Chem. Sci. 2018, 9, 999–1005. [CrossRef]
- Zheng, Z.; Zhang, T.; Liu, H.; Chen, Y.; Kwok, R.T.K.; Ma, C.; Zhang, P.; Sung, H.H.Y.; Williams, I.D.; Lam, J.W.Y.; et al. Bright Near-Infrared Aggregation-Induced Emission Luminogens with Strong Two-Photon Absorption, Excellent Organelle Specificity, and Efficient Photodynamic Therapy Potential. ACS Nano 2018, 12, 8145–8159. [CrossRef]
- Liu, Y.; Hu, X.; Wang, L.; Liu, X.; Bing, T.; Tan, W.; Shangguan, D. Quinacridone Derivative as a New Photosensitizer: Photodynamic Effects in Cells and in Vivo. Dyes and Pigments 2017, 145, 168–173. [CrossRef]
- Li, M.; Xia, J.; Tian, R.; Wang, J.; Fan, J.; Du, J.; Long, S.; Song, X.; Foley, J.W.; Peng, X. Near-Infrared Light-Initiated Molecular Superoxide Radical Generator: Rejuvenating Photodynamic Therapy against Hypoxic Tumors. J. Am. Chem. Soc. 2018, 140, 14851–14859. [CrossRef]
- Wang, R.; Hua, S.; Xing, Y.; Wang, R.; Wang, H.; Jiang, T.; Yu, F. Organic Dye-Based Photosensitizers for Fluorescence Imaging-Guided Cancer Phototheranostics. Coordination Chemistry Reviews 2024, 513, 215866. [CrossRef]
- Rainu, S.K.; Ramachandran, R.G.; Parameswaran, S.; Krishnakumar, S.; Singh, N. Advancements in Intraoperative Near-Infrared Fluorescence Imaging for Accurate Tumor Resection: A Promising Technique for Improved Surgical Outcomes and Patient Survival. ACS Biomater. Sci. Eng. 2023, 9, 5504–5526. [CrossRef]
- Li, S.; Cheng, D.; He, L.; Yuan, L. Recent Progresses in NIR-I/II Fluorescence Imaging for Surgical Navigation. Front. Bioeng. Biotechnol. 2021, 9, 768698. [CrossRef]
- Li, H.; Yao, Q.; Sun, W.; Shao, K.; Lu, Y.; Chung, J.; Kim, D.; Fan, J.; Long, S.; Du, J.; et al. Aminopeptidase N Activatable Fluorescent Probe for Tracking Metastatic Cancer and Image-Guided Surgery via in Situ Spraying. J. Am. Chem. Soc. 2020, 142, 6381–6389. [CrossRef]
- Hu, Z.; Fang, C.; Li, B.; Zhang, Z.; Cao, C.; Cai, M.; Su, S.; Sun, X.; Shi, X.; Li, C.; et al. First-in-Human Liver-Tumour Surgery Guided by Multispectral Fluorescence Imaging in the Visible and near-Infrared-I/II Windows. Nat. Biomed. Eng. 2019, 4, 259–271. [CrossRef]
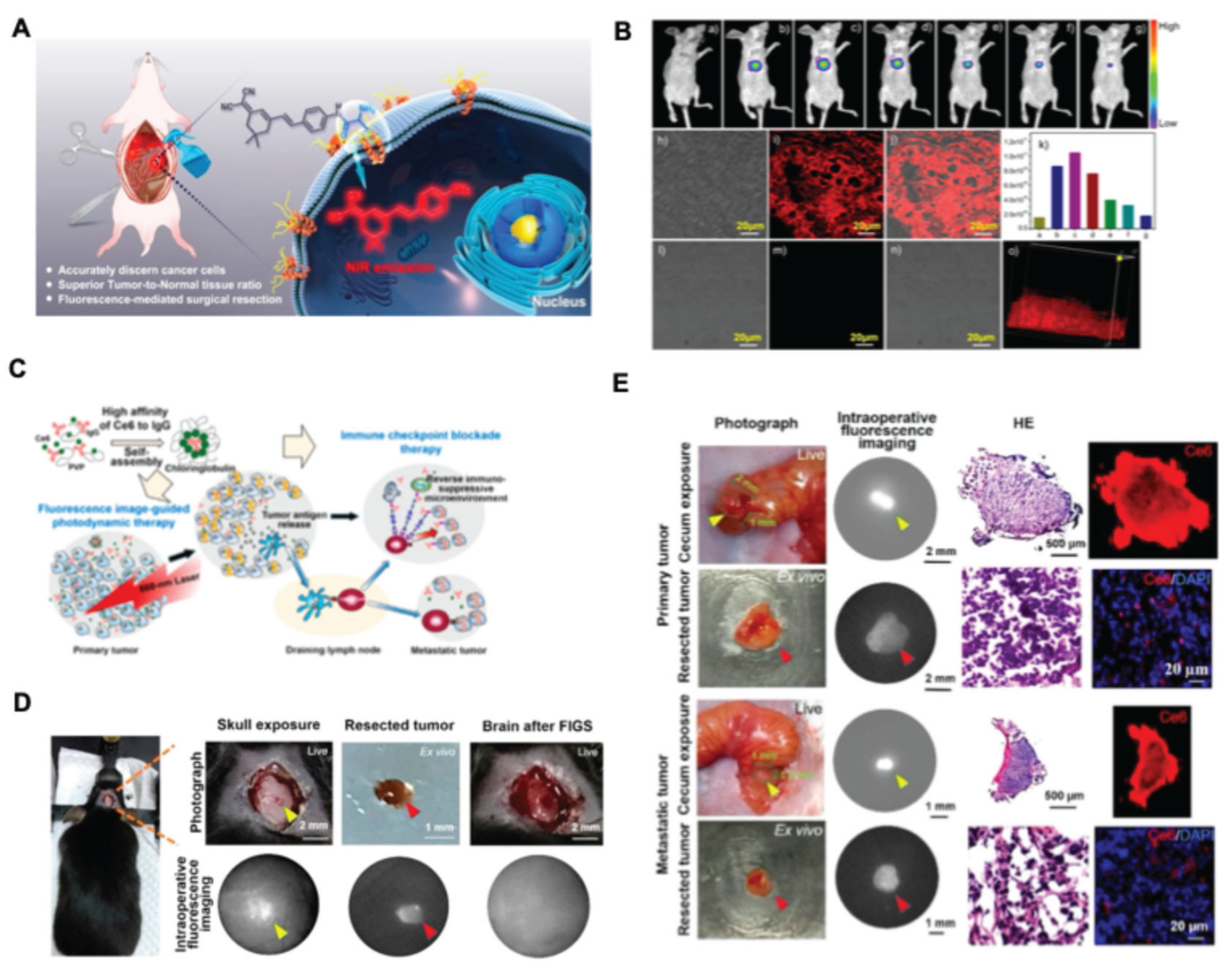
- Xu, J.; Yu, S.; Wang, X.; Qian, Y.; Wu, W.; Zhang, S.; Zheng, B.; Wei, G.; Gao, S.; Cao, Z.; et al. High Affinity of Chlorin E6 to Immunoglobulin G for Intraoperative Fluorescence Image-Guided Cancer Photodynamic and Checkpoint Blockade Therapy. ACS Nano 2019, 13, 10242–10260. [CrossRef]
- Lee, M.H.; Kim, J.Y.; Han, J.H.; Bhuniya, S.; Sessler, J.L.; Kang, C.; Kim, J.S. Direct Fluorescence Monitoring of the Delivery and Cellular Uptake of a Cancer-Targeted RGD Peptide-Appended Naphthalimide Theragnostic Prodrug. J. Am. Chem. Soc. 2012, 134, 12668–12674. [CrossRef]
- Xu, Z.; He, B.; Shen, J.; Yang, W.; Yin, M. Fluorescent Water-Soluble Perylenediimide-Cored Cationic Dendrimers: Synthesis, Optical Properties, and Cell Uptake. Chem. Commun. 2013, 49, 3646. [CrossRef]
- Cheng, W.; Cheng, H.; Wan, S.; Zhang, X.; Yin, M. Dual-Stimulus-Responsive Fluorescent Supramolecular Prodrug for Antitumor Drug Delivery. Chem. Mater. 2017, 29, 4218–4226. [CrossRef]
- Cai, Y.; Ji, C.; Zhang, S.; Su, Z.; Yin, M. Synthesis of Water-Soluble Dye-Cored Poly(Amidoamine) Dendrimers for Long-Term Live Cell Imaging. Sci. China Mater. 2018, 61, 1475–1483. [CrossRef]
- Maiti, S.; Park, N.; Han, J.H.; Jeon, H.M.; Lee, J.H.; Bhuniya, S.; Kang, C.; Kim, J.S. Gemcitabine–Coumarin–Biotin Conjugates: A Target Specific Theranostic Anticancer Prodrug. J. Am. Chem. Soc. 2013, 135, 4567–4572. [CrossRef]
- Bhuniya, S.; Maiti, S.; Kim, E.; Lee, H.; Sessler, J.L.; Hong, K.S.; Kim, J.S. An Activatable Theranostic for Targeted Cancer Therapy and Imaging. Angew. Chem. Int. Ed. 2014, 53, 4469–4474. [CrossRef]
- Yang, Z.; Lee, J.H.; Jeon, H.M.; Han, J.H.; Park, N.; He, Y.; Lee, H.; Hong, K.S.; Kang, C.; Kim, J.S. Folate-Based Near-Infrared Fluorescent Theranostic Gemcitabine Delivery. J. Am. Chem. Soc. 2013, 135, 11657–11662. [CrossRef]
- Xu, Z.; Guo, K.; Yu, J.; Sun, H.; Tang, J.; Shen, J.; Müllen, K.; Yang, W.; Yin, M. A Unique Perylene-Based DNA Intercalator: Localization in Cell Nuclei and Inhibition of Cancer Cells and Tumors. Small 2014, 10, 4087–4092. [CrossRef]
- Xu, Z.; Cheng, W.; Guo, K.; Yu, J.; Shen, J.; Tang, J.; Yang, W.; Yin, M. Molecular Size, Shape, and Electric Charges: Essential for Perylene Bisimide-Based DNA Intercalator to Localize in Cell Nuclei and Inhibit Cancer Cell Growth. ACS Appl. Mater. Interfaces 2015, 7, 9784–9791. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




