Submitted:
04 February 2026
Posted:
05 February 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and Methods
Study Design and Setting
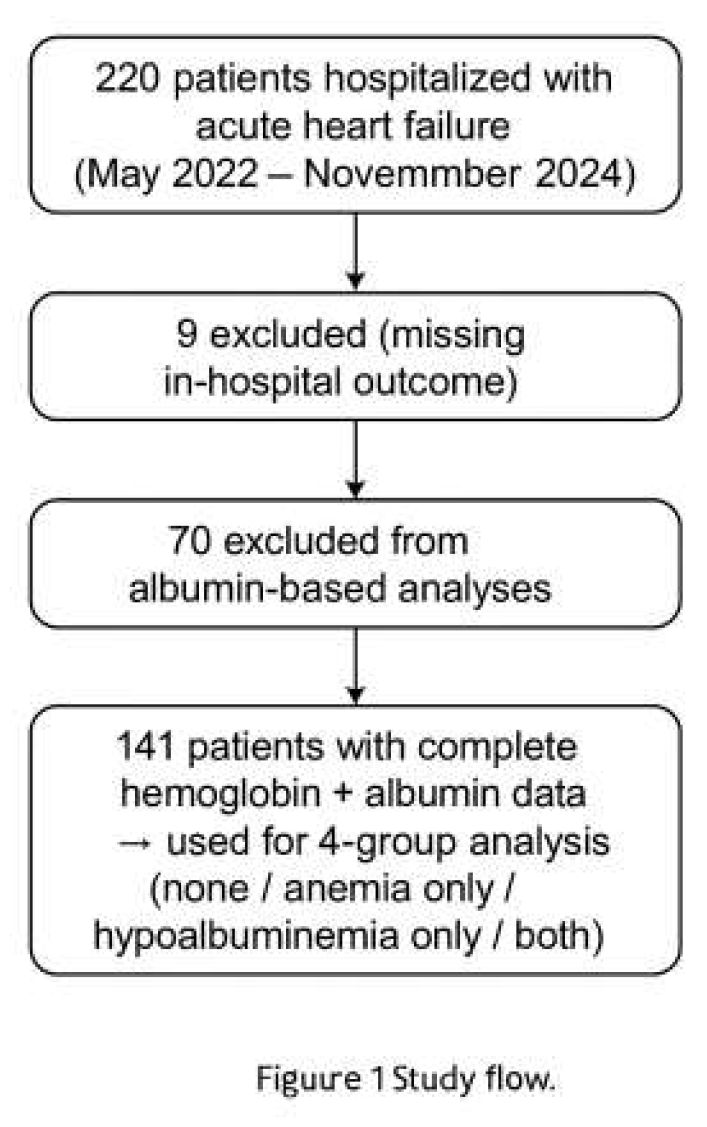
Study Population
- in-hospital outcome data were unavailable (n = 9),
- they presented with severe concomitant infections,
- they had acute coronary syndromes requiring immediate revascularization,
- they had active malignancy at the time of admission.
Clinical and Laboratory Data Collection
Definitions
- no anemia and no hypoalbuminemia,
- anemia only,
- hypoalbuminemia only,
- both anemia and hypoalbuminemia.
Statistical Analysis
Results
Baseline Characteristics
Prognostic Value of Hemoglobin and Albumin
Prognostic Value of LDH, NLR, and the CALLY Index
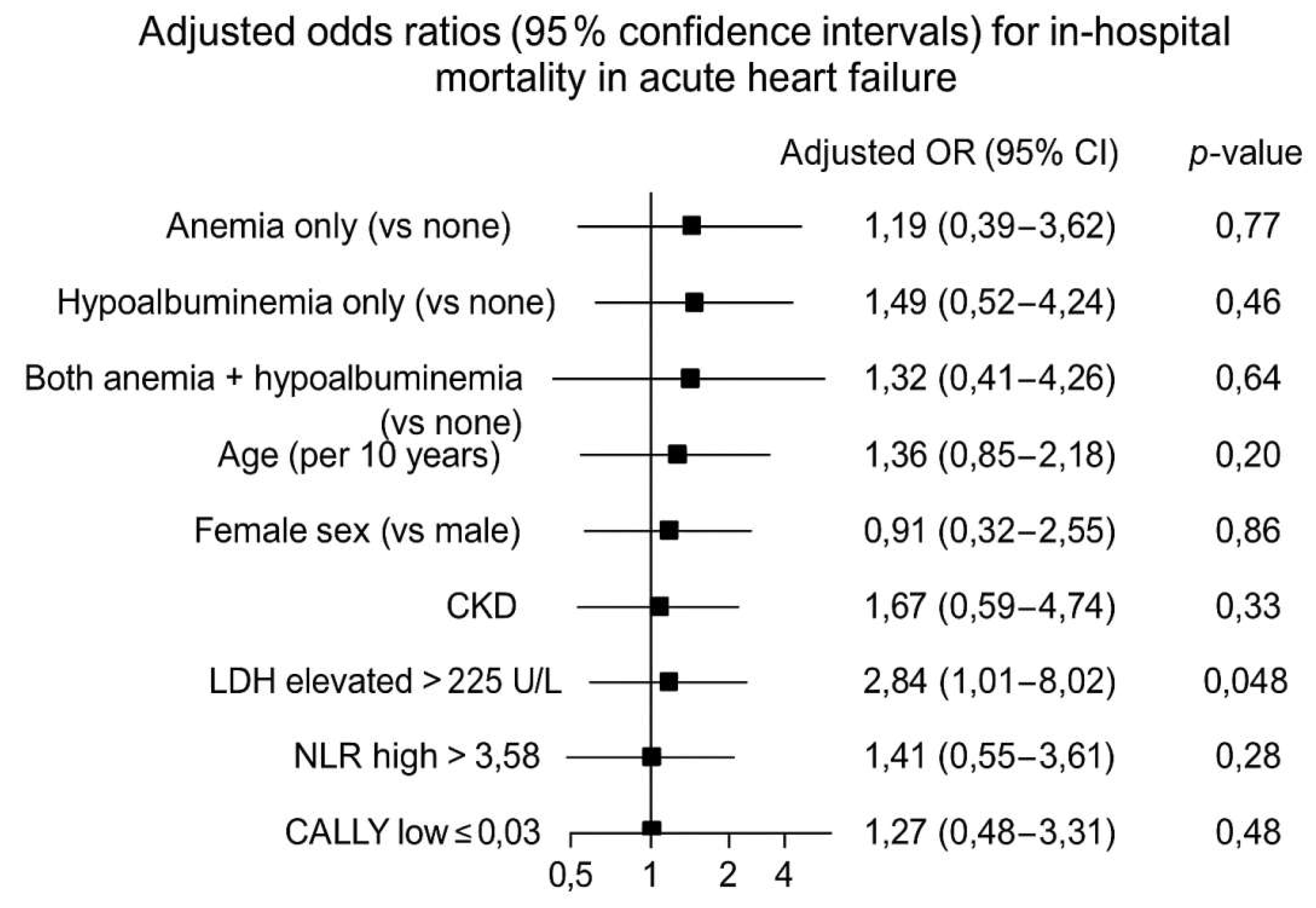
Multivariable Model Performance
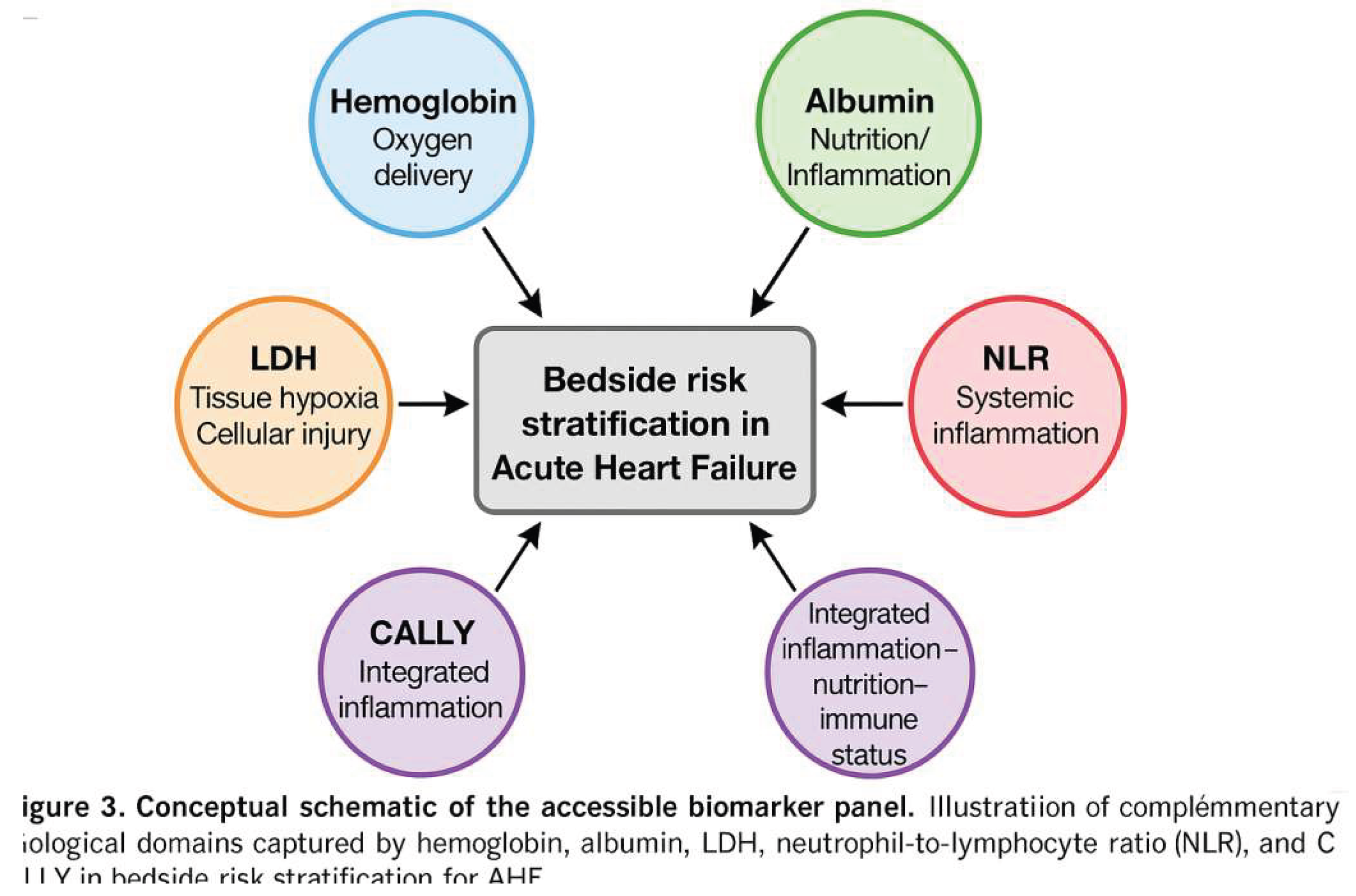
Discussion
Limitations
Conclusion
Highlights
- Lactate dehydrogenase (LDH) was independently associated with in-hospital mortality in acute heart failure.
- Anemia and hypoalbuminemia were associated with crude mortality but did not retain independent prognostic significance.
- Low-cost and routinely available biomarkers may support practical risk stratification across the acute–chronic heart failure spectrum.
- This real-world cohort reflects clinical challenges in resource-limited settings where BNP and NT-proBNP testing is unavailable.
- LDH may provide clinically relevant prognostic information with potential implications for chronic heart failure care.
Declaration of Generative AI and AI-assisted Technologies in the Writing Process
Institutional Review Board Statement
Data Availability Statement
References
- Ponikowski, P; Voors, AA; Anker, SD; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021, 42(36), 3599–3726. [Google Scholar]
- McDonagh, TA; Metra, M; Adamo, M; et al. The 2021 ESC Heart Failure Guidelines: key updates and clinical implications. Eur Heart J. 2022, 43(4), 221–228. [Google Scholar]
- Savarese, G; Lund, LH. Global public health burden of heart failure. Nat Rev Cardiol. 2017, 14(10), 639–649. [Google Scholar] [CrossRef] [PubMed]
- Dokainish, H; Teo, K; Zhu, J; et al. Heart failure in Africa, Asia, the Middle East and South America: The INTER-CHF study. Lancet Glob Health 2017, 5(8), e742–e750. [Google Scholar] [CrossRef] [PubMed]
- Tang, WHW; Yeo, PSD; Hart, R; et al. Anemia in acute decompensated heart failure: prevalence and prognostic significance. Clin Cardiol. 2009, 32(7), E35–E39. [Google Scholar]
- Groenveld, HF; Januzzi, JL, Jr.; Damman, K; et al. Anemia and mortality in heart failure: a systematic review and meta-analysis. J Am Coll Cardiol. 2008, 52(10), 818–827. [Google Scholar] [CrossRef]
- Arques, S; Ambrosi, P; Gelisse, R; et al. Hypoalbuminemia in elderly patients with acute decompensated heart failure. J Am Geriatr Soc. 2003, 51(8), 1229–1230. [Google Scholar]
- Horwich, TB; Kalantar-Zadeh, K; MacLellan, WR; Fonarow, GC. Albumin levels predict survival in patients with advanced heart failure. J Am Coll Cardiol. 2008, 52(11), 1216–1222. [Google Scholar]
- Arques, S; Ambrosi, P. Human serum albumin in the clinical syndrome of heart failure. J Card Fail. 2011, 17(6), 451–458. [Google Scholar] [CrossRef]
- Semba, RD; Nicklett, EJ; Ferrucci, L. Does hypoalbuminemia affect mortality in older persons? Results from the InCHIANTI study. J Gerontol A Biol Sci Med Sci. 2010, 65(8), 795–801. [Google Scholar]
- Liu, M; Chan, CP; Yan, BP; et al. Albumin and mortality in heart failure: a meta-analysis. Eur J Heart Fail. 2012, 14(4), 386–392. [Google Scholar]
- Arques, S; Roux, E; Ambrosi, P. Hypoalbuminemia in heart failure: pathophysiologic mechanisms and clinical significance. Heart Fail Rev. 2019, 24(1), 1–10. [Google Scholar]
- Yancy, CW; Jessup, M; Bozkurt, B; et al. 2017 ACC/AHA/HFSA heart failure focused update. J Am Coll Cardiol. 2017, 70(6), 776–803. [Google Scholar] [CrossRef] [PubMed]
- Zazula, AD; Precoma-Neto, D; Gomes, AM; et al. The neutrophil-to-lymphocyte ratio as an inflammatory marker in acute coronary syndromes. Clin Chim Acta 2008, 395(1–2), 65–70. [Google Scholar]
- Uthamalingam, S; Patvardhan, EA; Subramanian, S; et al. Utility of the neutrophil-to-lymphocyte ratio in predicting long-term outcomes in acute decompensated heart failure. Am J Cardiol. 2011, 107(3), 433–438. [Google Scholar] [CrossRef]
- Bhat, T; Teli, S; Rijal, J; et al. Neutrophil to lymphocyte ratio and cardiovascular diseases: a review. Expert Rev Cardiovasc Ther. 2013, 11(1), 55–59. [Google Scholar] [CrossRef]
- Durmus, E; Kivrak, T; Gerin, F; et al. The relationship between NLR and heart failure subtypes. Eur Rev Med Pharmacol Sci. 2015, 19(21), 4331–4338. [Google Scholar]
- Forget, P; Khalifa, C; Defour, JP; et al. What is the normal value of the neutrophil-to-lymphocyte ratio? BMC Res Notes 2017, 10(1), 12. [Google Scholar] [CrossRef]
- de Jager, CPC; Wever, PC; Gemen, EFA; et al. The neutrophil–lymphocyte ratio in patients with community-acquired pneumonia. Eur J Clin Microbiol Infect Dis. 2010, 29(12), 1501–1507. [Google Scholar] [CrossRef]
- Núñez, J; Miñana, G; Bodi, V; et al. Low lymphocyte count and cardiovascular diseases. Int J Cardiol. 2011, 146(2), 264–270. [Google Scholar]
- Kinoshita, A; Onoda, H; Imai, N; et al. The CRP/albumin ratio as a novel prognostic marker in hepatocellular carcinoma. J Clin Oncol. 2015, 33 (15_suppl), 4105. [Google Scholar]
- Suzuki, K; Imai, N; et al. Prognostic significance of the CALLY index in cancer and cardiovascular disease. Nutrients 2021, 13(7), 2401. [Google Scholar]
- Chen, L; Wu, C; Gao, R; et al. Serum lactate dehydrogenase and outcomes in acute heart failure. Eur J Heart Fail. 2020, 22(5), 898–906. [Google Scholar]
- Liu, T; Li, G; Li, L; et al. Lactate dehydrogenase as a biomarker for mortality in critical illness: a meta-analysis. Crit Care 2021, 25(1), 171. [Google Scholar]
- Niimi, N; Ikeda, Y; Shimizu, M; et al. Association of LDH with in-hospital mortality in acute heart failure: multicenter cohort. Heart Vessels 2023, 38(3), 522–531. [Google Scholar]
- Lu, J; Wang, X; et al. Elevated serum LDH levels and poor prognosis in acute decompensated heart failure. ESC Heart Fail. 2022, 9(1), 356–366. [Google Scholar]
- Shah, KS; Xu, H; Matsouaka, RA; et al. HF with preserved, borderline, and reduced EF: 5-year outcomes. J Am Coll Cardiol. 2017, 70(20), 2476–2486. [Google Scholar] [CrossRef]
- Bhatla, A; Maisel, A. Biomarkers in acute heart failure. Heart Fail Clin. 2019, 15(3), 323–334. [Google Scholar]
- Dhingra, A; Givertz, MM. Interpretation and use of natriuretic peptides. J Am Coll Cardiol. 2019, 73(9), 1184–1201. [Google Scholar]
- Yilmaz, S; Altay, H; Özkan, A; et al. Predictors of mortality in patients hospitalized for AHF. ESC Heart Fail. 2023, 10(2), 1259–1269. [Google Scholar]
- Yao, Y; Zhao, M; et al. Elevated LDH predicts short-term mortality in AHF. Front Cardiovasc Med. 2021, 8, 714485. [Google Scholar]
- Wu, Y; Chen, J; et al. Prognostic significance of LDH in cardiovascular diseases: systematic review. BMC Cardiovasc Disord. 2022, 22, 307. [Google Scholar]
- Mentz, RJ; Greene, SJ; DeVore, AD; et al. Biomarkers in heart failure: implications and challenges. Heart Fail Rev. 2017, 22(6), 725–734. [Google Scholar]
- van der Meer, P; Gaggin, HK; Dec, GW. ACC/AHA/ESC/HFSA recommendations on biomarkers in HF. J Am Coll Cardiol. 2021, 78(5), 494–504. [Google Scholar]
- Harjola, VP; Mullens, W; Banaszewski, M; et al. Organ congestion in HF: assessment and implications. Eur J Heart Fail. 2016, 18(7), 760–771. [Google Scholar]
- Ferreira, JP; Metra, M; Mordi, IR; et al. Heart failure in low-resource settings. ESC Heart Fail. 2020, 7(6), 4213–4224. [Google Scholar]
- Fudim, M; O'Connor, CM; Ahmad, T. Biomarker-guided therapy in HF. Curr Heart Fail Rep. 2018, 15(6), 429–436. [Google Scholar]
- Felker, GM; Mentz, RJ; Teerlink, JR; et al. Serial biomarker measurement in AHF: RELAX-AHF insights. Eur J Heart Fail. 2016, 18(12), 1420–1428. [Google Scholar]
- Ahmad, T; Fiuzat, M; Felker, GM; O'Connor, CM. Novel biomarkers in chronic HF. Nat Rev Cardiol. 2012, 9(6), 347–359. [Google Scholar] [CrossRef]
- Wang, L; Li, Y; et al. Temporal trends in biomarker changes in HF. Front Cardiovasc Med. 2023, 10, 1164325. [Google Scholar]
- Mueller, C; McDonagh, T; et al. Biomarker-based strategies in AHF management. Eur Heart J. 2023, 44(5), 412–427. [Google Scholar]
| Variable | Overall cohort (n = 220) |
| Age, years | 59.5 ± 14.7 |
| Male sex, n (%) | 138 (62.7) |
| Diabetes mellitus, n (%) | 129 (58.6) |
| Hypertension, n (%) | 118 (53.6) |
| Chronic kidney disease, n (%) | 29 (13.2) |
| Ischemic heart disease, n (%) | 11 (5.0) |
| Hemoglobin, g/dL | 11.7 (IQR 10.0–13.3) |
| Serum albumin, g/dL | 3.0 (IQR 2.4–3.8) |
| Lactate dehydrogenase, U/L | 54.5 (IQR 20.0–123.0) |
| C-reactive protein, mg/L | 45.0 (IQR 17.0–99.0) |
| Neutrophil-to-lymphocyte ratio | 3.6 (IQR 2.3–6.9) |
| Hemoglobin–Albumin subgroup | n | In-hospital mortality, n (%) |
| No anemia / No hypoalbuminemia | 38 | 2 (5.3) |
| Anemia only | 32 | 6 (18.8) |
| Hypoalbuminemia only | 34 | 8 (23.5) |
| Anemia + Hypoalbuminemia | 37 | 5 (14.8) |
| Total | 141 | 21 (14.9) |
| Variable | Adjusted OR | 95% Confidence Interval | P value |
| Age (per year increase) | 1.03 | 0.99–1.07 | 0.11 |
| Male sex | 1.21 | 0.48–3.05 | 0.68 |
| Chronic kidney disease | 1.89 | 0.72–4.96 | 0.20 |
| Anemia | 1.42 | 0.54–3.71 | 0.47 |
| Hypoalbuminemia | 1.67 | 0.63–4.45 | 0.30 |
| Lactate dehydrogenase | 2.84 | 1.01–8.02 | 0.048 |
| Neutrophil-to-lymphocyte ratio >3.58 | 1.96 | 0.91–4.24 | 0.09 |
| CALLY index ≤0.03 | 1.88 | 0.85–4.13 | 0.11 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




