Submitted:
22 January 2026
Posted:
26 January 2026
You are already at the latest version
Abstract
Keywords:
Background
Methods
Study Design
Search Strategy
Eligibility Criteria
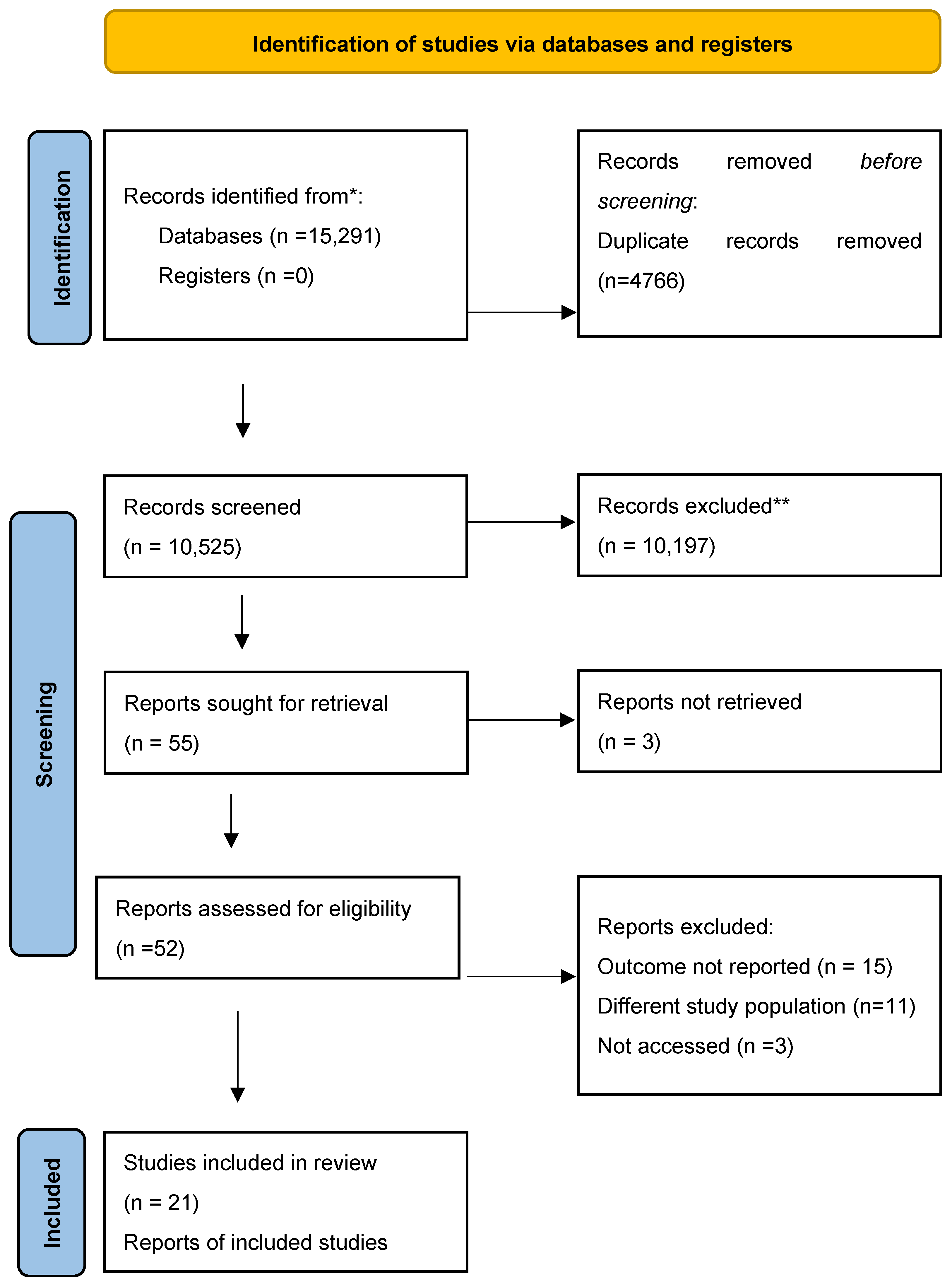
Study Selection
Data Extraction and Quality Assessment
Statistical Analysis
Results
Characteristics of Included Studies
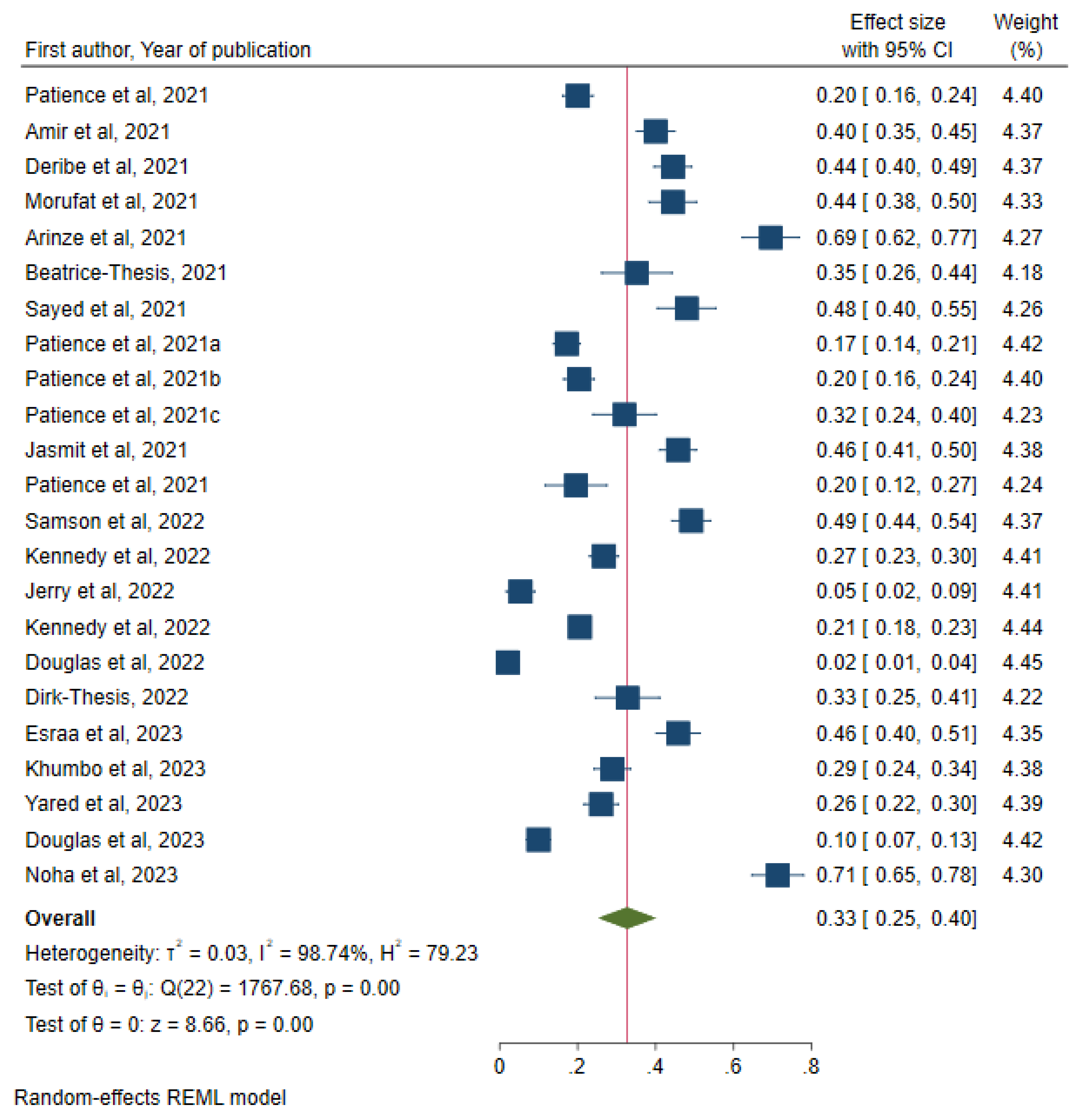
Pooled Prevalence
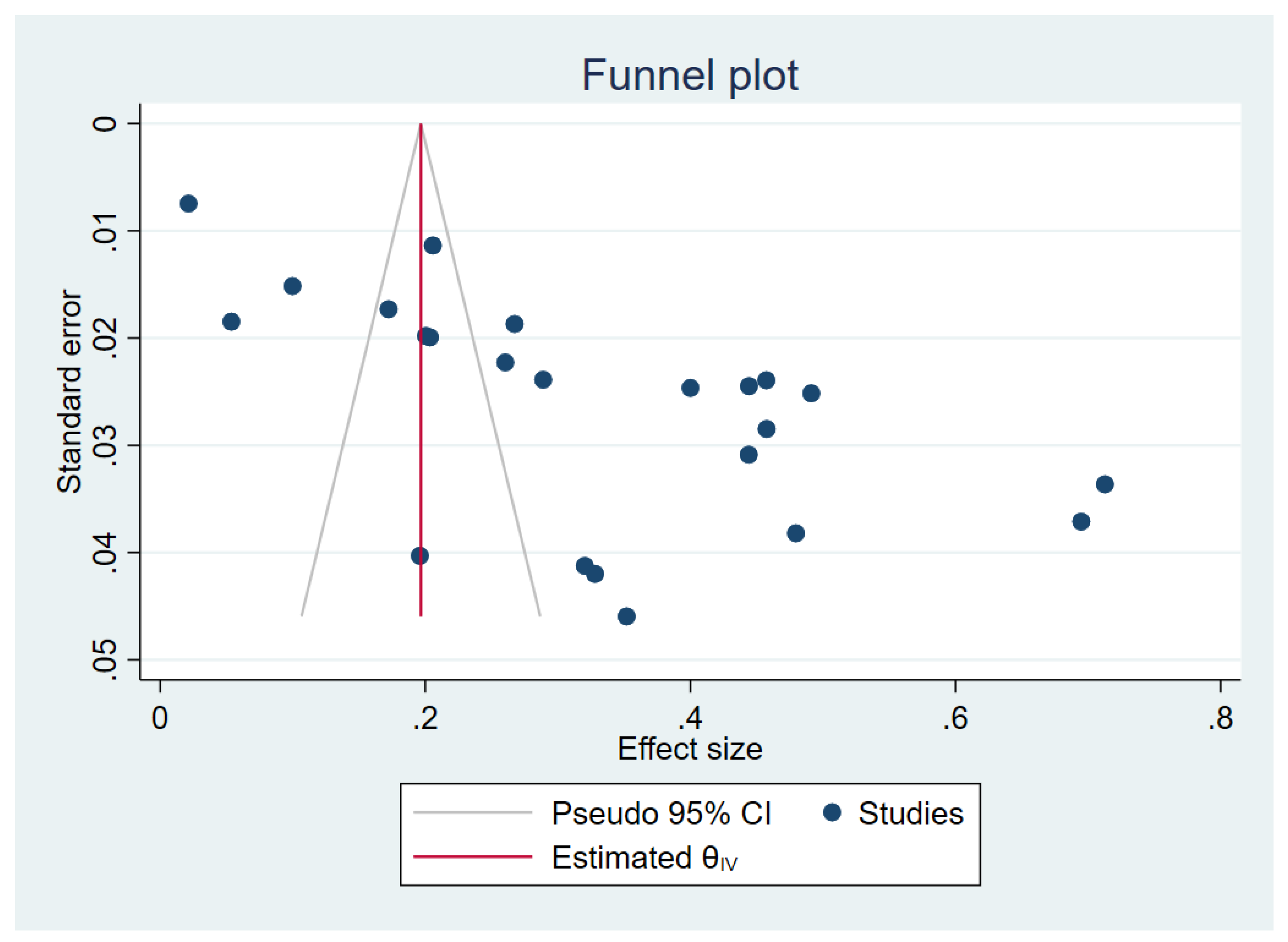
Publication Bias
Subgroup Analysis
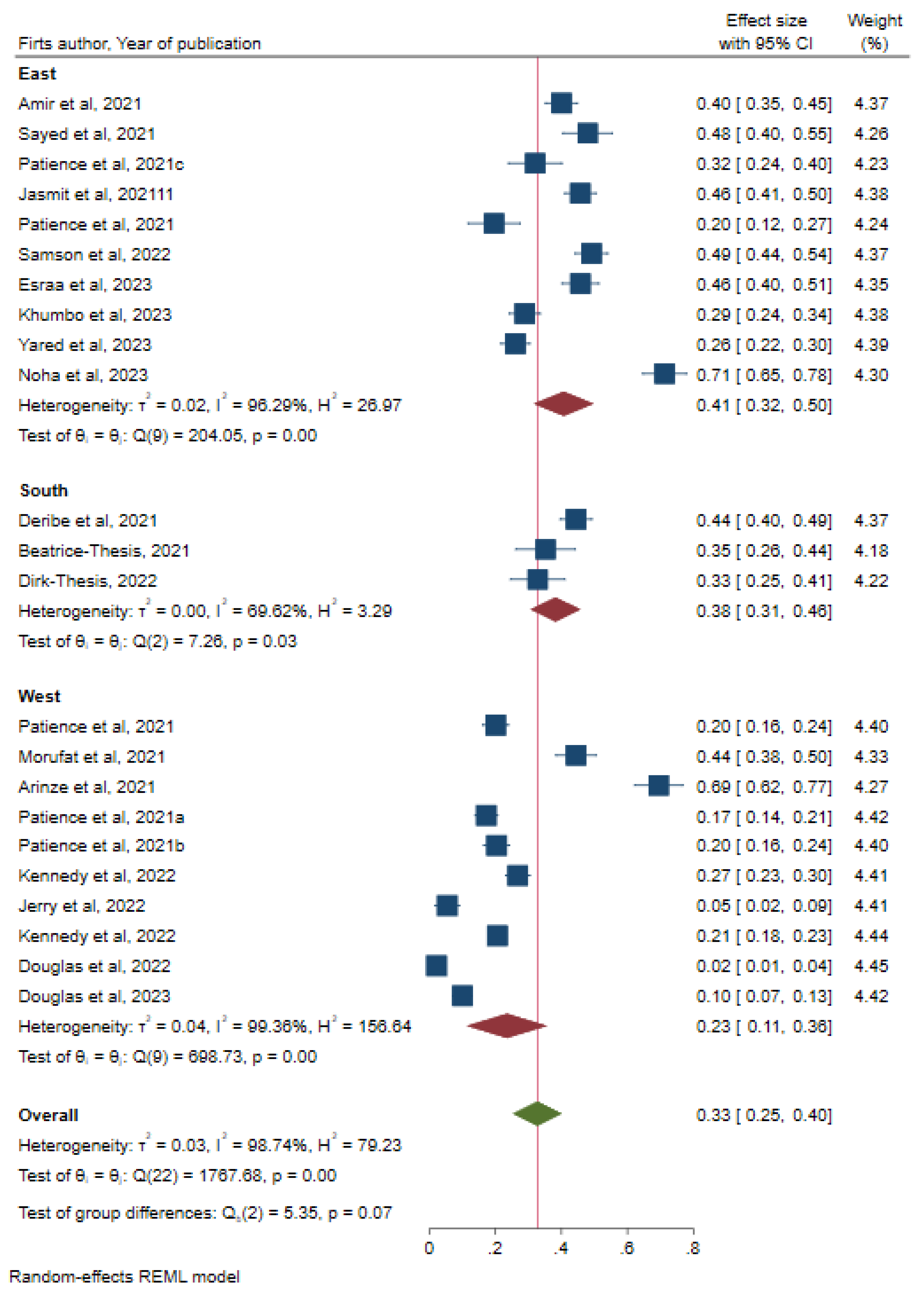
Subgroup Analysis by Region
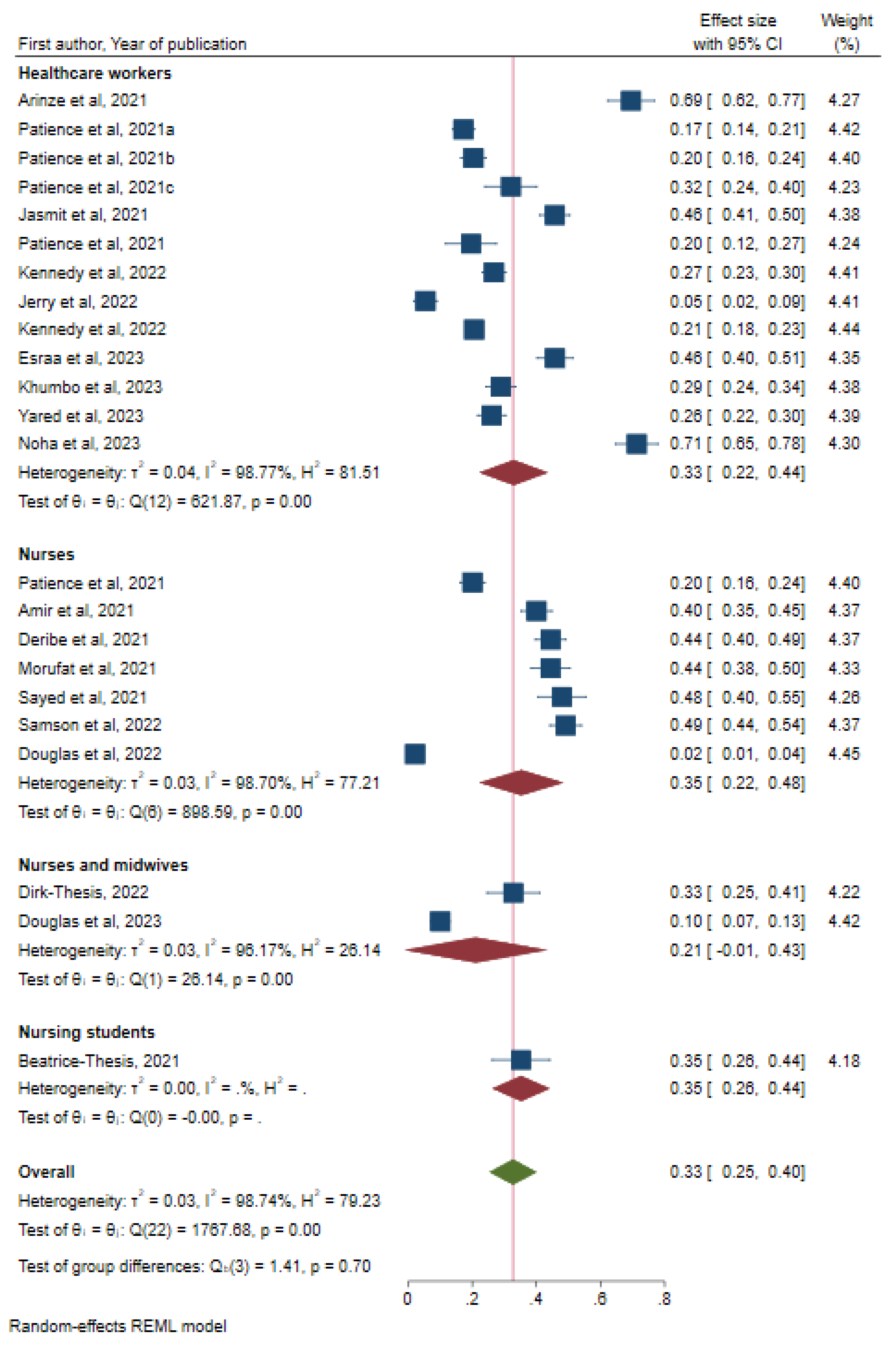
Subgroup Analysis by Study Participants
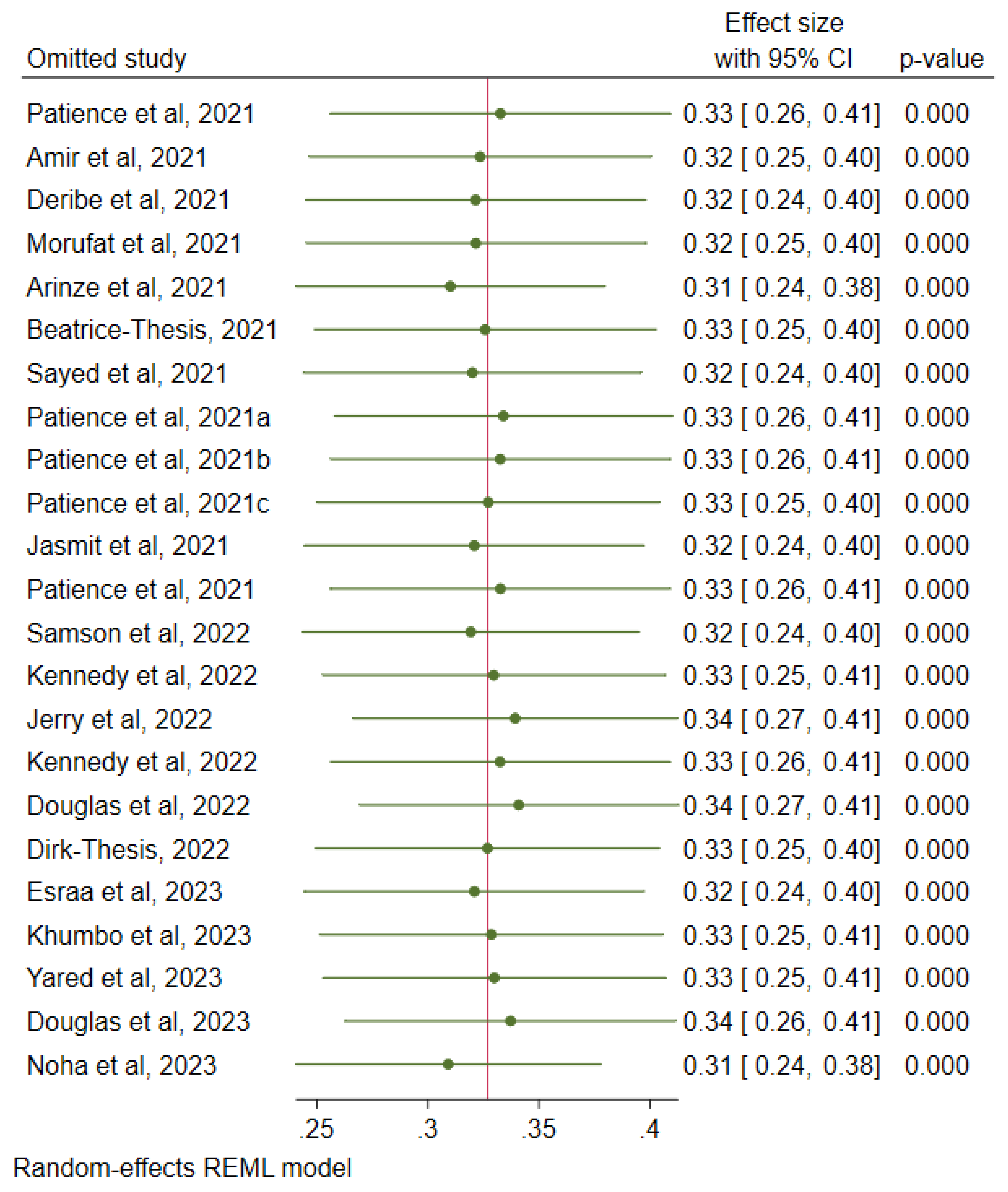
Sensitivity Analysis
Predictors of Burnout
Discussion
Implications and Recommendations
Strengths and Limitations of the Study
Conclusion
Supplementary Materials
Ethical Approval
References
- Afulani, P. A., Gyamerah, A. O., Nutor, J. J., Laar, A., Aborigo, R. A., Malechi, H., Sterling, M., & Awoonor-Williams, J. K. (2021). Inadequate preparedness for response to COVID-19 is associated with stress and burnout among healthcare workers in Ghana. PLOS ONE, 16(4), e0250294. [CrossRef]
- Afulani, P. A., Nutor, J. J., Agbadi, P., Gyamerah, A. O., Musana, J., Aborigo, R. A., Odiase, O., Getahun, M., Ongeri, L., Malechi, H., Madadi, M. O., Arhinful, B., Kelly, A. M., & Awoonor-Williams, J. K. (2021). Job satisfaction among healthcare workers in Ghana and Kenya during the COVID-19 pandemic: Role of perceived preparedness, stress, and burnout. PLOS Global Public Health, 1(10), e0000022. [CrossRef]
- Afulani, P. A., Ongeri, L., Kinyua, J., Temmerman, M., Mendes, W. B., & Weiss, S. J. (2021). Psychological and physiological stress and burnout among maternity providers in a rural county in Kenya: Individual and situational predictors. BMC Public Health, 21(1), 453. [CrossRef]
- Alabi, M. A., Ishola, A. G., Onibokun, A. C., & Lasebikan, V. O. (2021). Burnout and quality of life among nurses working in selected mental health institutions in South West Nigeria. African Health Sciences, 21(3), 1428–1439. [CrossRef]
- Alfadul, E. S. A., Idrees Abdalmotalib, M. M., Alrawa, S. S. K., Osman, R. O. A., Hassan, H. M. A., Albasheir, A. T., Hasabo, E. A., Mohamed, S. O. O., & Shaaban, K. M. A. (2023). Burnout and its associated factors among healthcare workers in COVID-19 isolation centres in Khartoum, Sudan: A cross-sectional study. PloS One, 18(7), e0288638. [CrossRef]
- Ali, S. K., Shah, J., & Talib, Z. (2021). COVID-19 and mental well-being of nurses in a tertiary facility in Kenya. PloS One, 16(7), e0254074. [CrossRef]
- Amir, K., & Okalo, P. (2022). Frontline nurses’ compassion fatigue and associated predictive factors during the second wave of COVID-19 in Kampala, Uganda. Nursing Open.
- Aziato, L., Ani-Amponsah, M., Iddrisu, M., & Ohene, L. A. (2021). The Impact of Covid-19 on the African Workforce Through the Lenses of Nurses and Midwives. Gendered Perspectives on Covid-19 Recovery in Africa: Towards Sustainable Development, 111–129.
- Busch, I. M., Moretti, F., Mazzi, M., Wu, A. W., & Rimondini, M. (2021). What we have learned from two decades of epidemics and pandemics: A systematic review and meta-analysis of the psychological burden of frontline healthcare workers. Psychotherapy and Psychosomatics, 90(3), 178–190.
- Chandra, V. (2012). Work–life balance: Eastern and western perspectives. The International Journal of Human Resource Management, 23(5), 1040–1056.
- Chersich, M. F., Gray, G., Fairlie, L., Eichbaum, Q., Mayhew, S., Allwood, B., English, R., Scorgie, F., Luchters, S., & Simpson, G. (2020). COVID-19 in Africa: Care and protection for frontline healthcare workers. Globalization and Health, 16, 1–6.
- De Pablo, G. S., Vaquerizo-Serrano, J., Catalan, A., Arango, C., Moreno, C., Ferre, F., Shin, J. Il, Sullivan, S., Brondino, N., & Solmi, M. (2020). Impact of coronavirus syndromes on physical and mental health of health care workers: Systematic review and meta-analysis. Journal of Affective Disorders, 275, 48–57.
- Dechasa, D. B., Worku, T., Baraki, N., Merga, B. T., & Asfaw, H. (2021). Burnout and associated factors among nurses working in public hospitals of Harari region and Dire Dawa administration, eastern Ethiopia. A cross sectional study. PloS One, 16(10), e0258224. [CrossRef]
- Dubale, B. W., Friedman, L. E., Chemali, Z., Denninger, J. W., Mehta, D. H., Alem, A., Fricchione, G. L., Dossett, M. L., & Gelaye, B. (2019). Systematic review of burnout among healthcare providers in sub-Saharan Africa. BMC Public Health, 19(1), 1–20.
- El Dabbah, N. A., & Elhadi, Y. A. M. (2023). High levels of burnout among health professionals treating COVID-19 patients in two Nile basin countries with limited resources. Scientific Reports, 13(1), 6455. [CrossRef]
- Elbarazi, I., Loney, T., Yousef, S., & Elias, A. (2017). Prevalence of and factors associated with burnout among health care professionals in Arab countries: A systematic review. BMC Health Services Research, 17, 1–10.
- Galanis, P., Vraka, I., Fragkou, D., Bilali, A., & Kaitelidou, D. (2021). Nurses’ burnout and associated risk factors during the COVID-19 pandemic: A systematic review and meta-analysis. Journal of Advanced Nursing, 77(8), 3286–3302.
- Gelaw, Y. M., Hanoch, K., & Adini, B. (2023). Burnout and resilience at work among health professionals serving in tertiary hospitals, in Ethiopia. Frontiers in Public Health, 11, 1118450. [CrossRef]
- Ghahramani, S., Lankarani, K. B., Yousefi, M., Heydari, K., Shahabi, S., & Azmand, S. (2021). A systematic review and meta-analysis of burnout among healthcare workers during COVID-19. Frontiers in Psychiatry, 12.
- Higgins, J. P. T., Thompson, S. G., Deeks, J. J., & Altman, D. G. (2003). Measuring inconsistency in meta-analyses. BMJ : British Medical Journal, 327(7414), 557–560.
- Hur, G., Cinar, N., & Suzan, O. K. (2022). Impact of COVID-19 pandemic on nurses’ burnout and related factors: A rapid systematic review. Archives of Psychiatric Nursing, 41, 248–263.
- Jun, J., Ojemeni, M. M., Kalamani, R., Tong, J., & Crecelius, M. L. (2021). Relationship between nurse burnout, patient and organizational outcomes: Systematic review. International Journal of Nursing Studies, 119, 103933.
- Kabunga, A., & Okalo, P. (2021a). Frontline Nurses’ Post-Traumatic Stress Disorder and Associated Predictive Factors During the Second Wave of COVID-19 in Central, Uganda. Neuropsychiatric Disease and Treatment, 3627–3633.
- Kabunga, A., & Okalo, P. (2021b). Prevalence and predictors of burnout among nurses during COVID-19: A cross-sectional study in hospitals in central Uganda. BMJ Open, 11(9), e054284.
- Konlan, K. D., Asampong, E., Dako-Gyeke, P., & Glozah, F. N. (2022a). Burnout and allostatic load among health workers engaged in human resourced-constrained hospitals in Accra, Ghana. BMC Health Services Research, 22(1), 1163. [CrossRef]
- Konlan, K. D., Asampong, E., Dako-Gyeke, P., & Glozah, F. N. (2022b). Burnout syndrome among healthcare workers during COVID-19 Pandemic in Accra, Ghana. PloS One, 17(6), e0268404. [CrossRef]
- Koontalay, A., Suksatan, W., Prabsangob, K., & Sadang, J. M. (2021). Healthcare workers’ burdens during the COVID-19 pandemic: A qualitative systematic review. Journal of Multidisciplinary Healthcare, 3015–3025.
- Lourens, D. C. (2022). The prevalence of burnout in nurses working in private healthcare facilities in Mbombela/Nelspruit during the COVID-19 pandemic [Stellenbosch : Stellenbosch University]. http://hdl.handle.net/10019.1/126116.
- MacGregor, H., Leach, M., Desclaux, A., Grant, C., Martineau, F., Parker, M., Sams, K., & Sow, K. (2023). COVID-19 in sub-Saharan Africa: Pandemic preparedness and response. In How to Live through a Pandemic (pp. 40–63). Routledge.
- Morgan, R. L., Whaley, P., Thayer, K. A., & Schünemann, H. J. (2018). Identifying the PECO: A framework for formulating good questions to explore the association of environmental and other exposures with health outcomes. Environment International, 121(Pt 1), 1027–1031. [CrossRef]
- Munn, Z., Moola, S., Lisy, K., Riitano, D., & Tufanaru, C. (2017). Systematic reviews of prevalence and incidence. Joanna Briggs Institute Reviewer’s Manual. Adelaide, South Australia: The Joanna Briggs Institute, 5–1.
- Nutor, J. J., Aborigo, R. A., Okiring, J., Kuwolamo, I., Dorzie, J. B. K., Getahun, M., Mendes, W. B., & Afulani, P. A. (2022). Individual and situational predictors of psychological and physiological stress and burnout among maternity providers in Northern Ghana. PloS One, 17(12), e0278457. [CrossRef]
- Nwosu, A. D. G., Ossai, E., Onwuasoigwe, O., Ezeigweneme, M., & Okpamen, J. (2021). Burnout and presenteeism among healthcare workers in Nigeria: Implications for patient care, occupational health and workforce productivity. Journal of Public Health Research, 10(1), 1900. [CrossRef]
- Opoku, D. A., Ayisi-Boateng, N. K., Mohammed, A., Sulemana, A., Gyamfi, A. O., Owusu, D. K., Yeboah, D., Spangenberg, K., Ofosu, H. M., & Edusei, A. K. (2023). Determinants of burnout among nurses and midwives at a tertiary hospital in Ghana: A cross-sectional study. Nursing Open, 10(2), 869–878. [CrossRef]
- Opoku, D. A., Ayisi-Boateng, N. K., Osarfo, J., Sulemana, A., Mohammed, A., Spangenberg, K., Awini, A. B., & Edusei, A. K. (2022). Attrition of Nursing Professionals in Ghana: An Effect of Burnout on Intention to Quit. Nursing Research and Practice, 2022, e3100344. [CrossRef]
- Ouzzani, M., Hammady, H., Fedorowicz, Z., & Elmagarmid, A. (2016). Rayyan—A web and mobile app for systematic reviews. Systematic Reviews, 5(1), 210. [CrossRef]
- Owuor, R. A., Mutungi, K., Anyango, R., & Mwita, C. C. (2020). Prevalence of burnout among nurses in sub-Saharan Africa: A systematic review. JBI Evidence Synthesis, 18(6), 1189–1207.
- Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffmann, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., Chou, R., Glanville, J., Grimshaw, J. M., Hróbjartsson, A., Lalu, M. M., Li, T., Loder, E. W., Mayo-Wilson, E., McDonald, S., … Moher, D. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ, n71. [CrossRef]
- Phiri, K., Songo, J., Whitehead, H., Chikuse, E., Moucheraud, C., Dovel, K., Phiri, S., Hoffman, R. M., & Oosterhout, J. J. van. (2023). Burnout and depression: A cross sectional study among health care workers providing HIV care during the COVID-19 pandemic in Malawi. PLOS Global Public Health, 3(9), e0001887. [CrossRef]
- Potgieter, B. (2021). Stress, burnout, and compassion fatigue of undergraduate nursing students at a public university during the COVID-19 pandemic. http://scholar.ufs.ac.za/xmlui/handle/11660/11784.
- Pradas-Hernández, L., Ariza, T., Gómez-Urquiza, J. L., Albendín-García, L., De la Fuente, E. I., & Cañadas-De la Fuente, G. A. (2018). Prevalence of burnout in paediatric nurses: A systematic review and meta-analysis. PloS One, 13(4), e0195039.
- Rizzo, A., Yıldırım, M., Öztekin, G. G., Carlo, A. De, Nucera, G., Szarpak, Ł., Zaffina, S., & Chirico, F. (2023). Nurse burnout before and during the COVID-19 pandemic: A systematic comparative review. Frontiers in Public Health, 11, 1225431.
- Shah, J., Monroe-Wise, A., Talib, Z., Nabiswa, A., Said, M., Abeid, A., Ali Mohamed, M., Mohamed, S., & Ali, S. K. (2021). Mental health disorders among healthcare workers during the COVID-19 pandemic: A cross-sectional survey from three major hospitals in Kenya. BMJ Open, 11(6), e050316. [CrossRef]
- Stemmer, R., Bassi, E., Ezra, S., Harvey, C., Jojo, N., Meyer, G., Özsaban, A., Paterson, C., Shifaza, F., & Turner, M. B. (2022). A systematic review: Unfinished nursing care and the impact on the nurse outcomes of job satisfaction, burnout, intention-to-leave and turnover. Journal of Advanced Nursing, 78(8), 2290–2303.
- Sterne, J. A. C., Sutton, A. J., Ioannidis, J. P. A., Terrin, N., Jones, D. R., Lau, J., Carpenter, J., Rücker, G., Harbord, R. M., Schmid, C. H., Tetzlaff, J., Deeks, J. J., Peters, J., Macaskill, P., Schwarzer, G., Duval, S., Altman, D. G., Moher, D., & Higgins, J. P. T. (2011). Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ, 343, d4002. [CrossRef]
- Udho, S., & Kabunga, A. (2022). Burnout and Associated Factors among Hospital-Based Nurses in Northern Uganda: A Cross-Sectional Survey. BioMed Research International, 2022, e8231564. [CrossRef]
| Predictor | No. of studies | OR (95% CI) | I2 (%) | P value |
|---|---|---|---|---|
| Male | 23 | 1.20(1.19-1.21) | 99.40 | <0.001 |
| Married | 23 | 1.46(1.45-1.47) | 99.40 | <0.001 |
| High workload | 11 | 1.26(1.25-1.27) | 99.5 | <0.001 |
| Night shift | 4 | 1.23(1.22-1.24) | 99.7 | <0.001 |
| Use of PPE | 2 | 1.38(1.34-1.42) | 99.1 | <0.001 |
| Low working experience | 14 | 1.30(1.28-1.31) | 98.1 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




