Submitted:
21 January 2026
Posted:
22 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Study Design
2.3. Experimental Procedures and Measures
2.3.1. Fatigue Resistance/ Strength Endurance - Gait Analysis
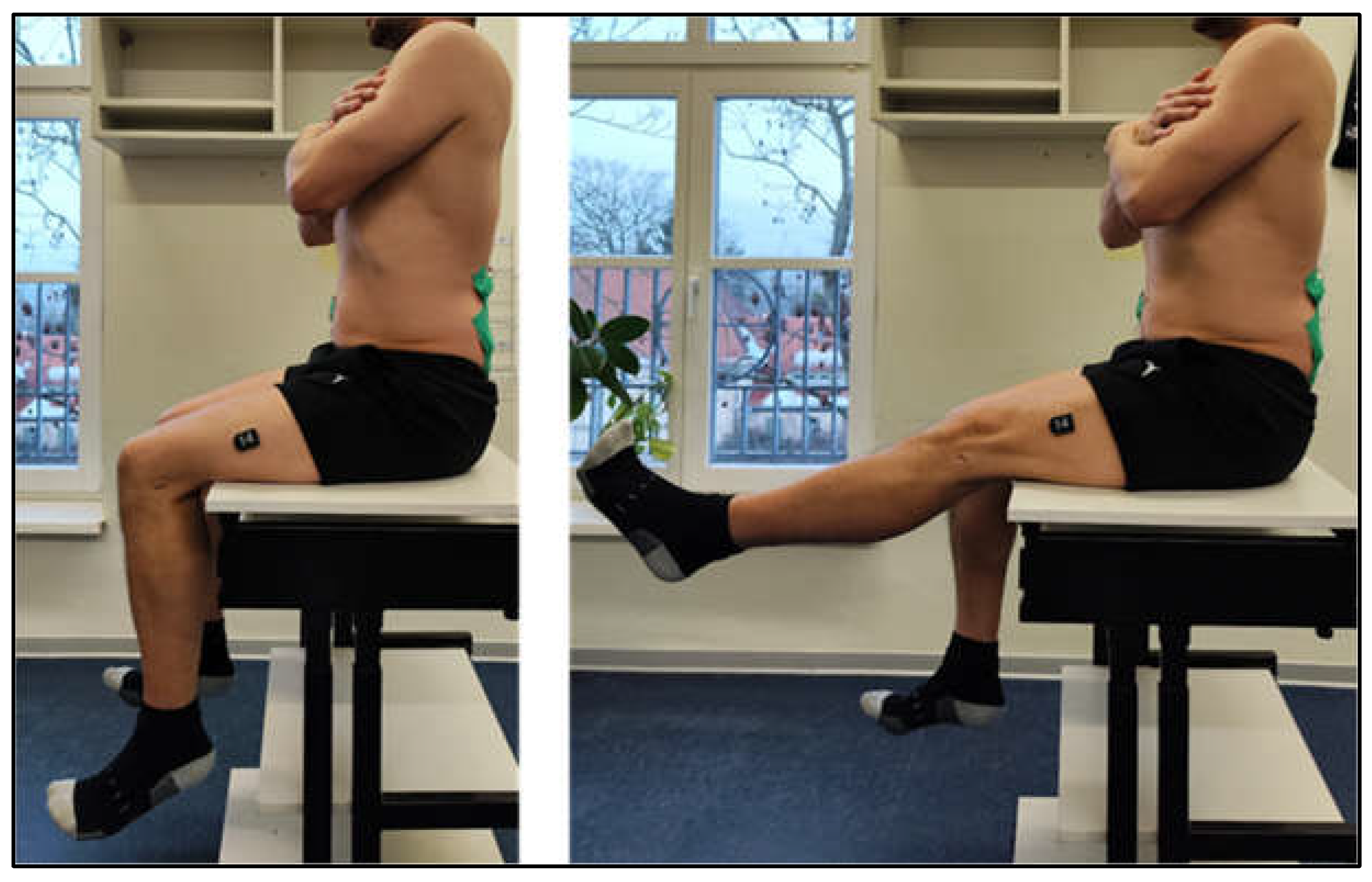
2.3.2. Neuromuscular Control and Range of Motion (ROM)
2.3.3. Lumbopelvic Stability
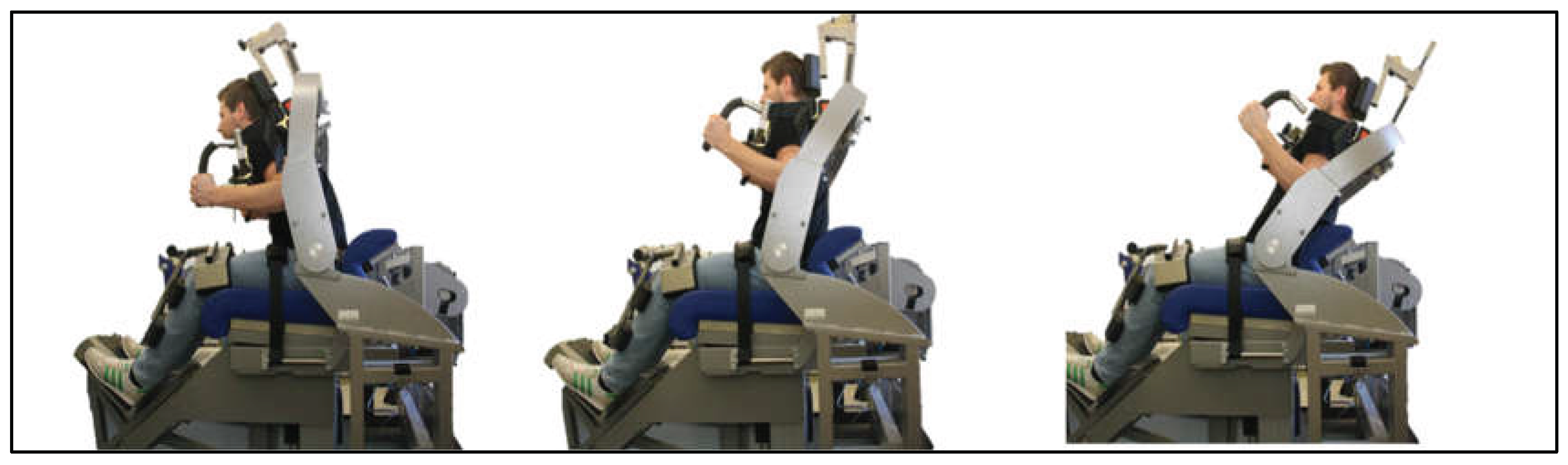
2.3.4. Global Trunk Musculature
2.4. Data Acquisition and Statistical Analysis
2.4.1. EMG and IMU System „Cometa”
2.4.2. CoP Measuring System
2.5. Ethic
3. Results
3.1. Fatigue Resistance/ Strength Endurance - Gait Analysis
3.2. Neuromuscular Control
3.3. Mobility/Bending
3.4. Lumbopelbß0ibe Mobility/Bending
| measurement | term | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|---|
| L_Multifidii | minENV | 0.033 | 0.6 | 1.8 | 0.43 | -0.83 |
| R_Int_Oblique | meanRAW | 0.053 | 0.43 | -0.00018 | 0.0004 | 0.000721 |
| L_ThoracicEs | meanRAW | 0.050 | 0.41 | -0.00049 | 3.94E-05 | 0.000743 |
3.5. Core Strength
4. Discussion
4.1. Functional Assessment
4.1.1. Fatigue Resistance/Strength Endurance - Gait Analysis
4.1.2. Neuromuscular Control
4.1.3. Mobility Bending
4.1.4. Lumbar-Pelvic Stability
4.1.5. Core Strength
4.2. Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
Appendix A.1 Search Strings
| Identification | ||
| Database | Search Query | Hits |
| PubMed | ((((“Low Back Pain” OR “LBP”) AND (“functional movement screen*” OR “functional assessment” OR “assessment instruments” OR assessment* OR FMS OR “EMG” OR “NRS”)) AND (diagn* OR prevent* OR control)) NOT (therapy OR reha* OR fractur* OR pregnancy OR imag* OR prevalence OR EEG OR effect* OR stress OR question* OR biomark* OR inflam*)) | n = 296 |
| CINAHL | n = 40 | |
| Screening | ||
| Results reviewed for duplicates | n = 312 | |
| Excluded after title abstract screening | n = 213 | |
| full texts checked for suitability | n = 99 | |
| full texts checked for suitability | n = 99 | |
| excluded | reason | case number |
| No access to full text/no full text (too old) | n = 29 | |
| Population | different search terms (no LBP) | n = 35 |
| Intervention | different intervention | n = 12 |
| Outcome | different outcome | n = 13 |
| Studies included in Rewiev | n = 10 |
References
- Duhautois, R; Erhel, C; Guergoat-Larivière, M; Mofakhami, M. More and Better Jobs, But Not for Everyone: Effects of Innovation in French Firms. ILR Rev. 2022, 75, 90–116. [Google Scholar]
- Rose, SJ. The Growth of the Office Economy: Underrecognized Sector in High-Income Economies. Crit Sociol. 2021, 47, 795–805. [Google Scholar] [CrossRef]
- Parry, S; Straker, L. The contribution of office work to sedentary behaviour associated risk. BMC Public Health 2013, 13, 296. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, ML; de, Luca K; Haile, LM; Steinmetz, JD; Culbreth, GT; Cross, M; et al. Global, regional, and national burden of low back pain, 1990–2020, its attributable risk factors, and projections to 2050: a systematic analysis of the Global Burden of Disease Study 2021. Lancet Rheumatol. 2023, 5, e316–e329. [Google Scholar] [CrossRef] [PubMed]
- Violante, FS; Mattioli, S; Bonfiglioli, R. Low-back pain. In Handbook of Clinical Neurology [Internet]; Elsevier, 2015; pp. 397–410. Available online: https://www.sciencedirect.com/science/chapter/handbook/abs/pii/B9780444626271000202?via%3Dihub (accessed on 14 January 2026).
- Hoy, D; March, L; Brooks, P; Blyth, F; Woolf, A; Bain, C; et al. The global burden of low back pain: estimates from the Global Burden of Disease 2010 study. Ann Rheum Dis. 2014, 73, 968–974. [Google Scholar] [CrossRef]
- Schmidt, CO; Raspe, H; Pfingsten, M; Hasenbring, M; Basler, HD; Eich, W; et al. Back Pain in the German Adult Population: Prevalence, Severity, and Sociodemographic Correlates in a Multiregional Survey. Spine 2007, 32, 2005–2011. [Google Scholar] [CrossRef]
- Brinjikji, W; Luetmer, PH; Comstock, B; Bresnahan, BW; Chen, LE; Deyo, RA; et al. Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. AJNR Am J Neuroradiol. 2015, 36, 811–816. [Google Scholar] [CrossRef]
- Webster, BS; Bauer, AZ; Choi, Y; Cifuentes, M; Pransky, GS. Iatrogenic consequences of early magnetic resonance imaging in acute, work-related, disabling low back pain. Spine 2013, 38, 1939–1946. [Google Scholar] [CrossRef]
- Chou, R; Qaseem, A; Owens, DK; Shekelle, P; Clinical Guidelines Committee of the American College of Physicians. Diagnostic imaging for low back pain: advice for high-value health care from the American College of Physicians. Ann Intern Med. 2011, 154, 181–189. [Google Scholar] [CrossRef]
- Hall, AM; Aubrey-Bassler, K; Thorne, B; Maher, CG. Do not routinely offer imaging for uncomplicated low back pain. BMJ. 2021, 372, n291. [Google Scholar] [CrossRef]
- Downie, A; Hancock, M; Jenkins, H; Buchbinder, R; Harris, I; Underwood, M; et al. How common is imaging for low back pain in primary and emergency care? Systematic review and meta-analysis of over 4 million imaging requests across 21 years. Br J Sports Med. 2020, 54, 642–651. [Google Scholar] [CrossRef]
- Jenkins, HJ; Downie, AS; Maher, CG; Moloney, NA; Magnussen, JS; Hancock, MJ. Imaging for low back pain: is clinical use consistent with guidelines? A systematic review and meta-analysis. Spine J Off J North Am Spine Soc. 2018, 18, 2266–2277. [Google Scholar] [CrossRef] [PubMed]
- Sánchez-Zuriaga, D; López-Pascual, J; Garrido-Jaén, D; de Moya, MFP; Prat-Pastor, J. Reliability and validity of a new objective tool for low back pain functional assessment. Spine 2011, 36, 1279–1288. [Google Scholar] [CrossRef] [PubMed]
- Rosenberg, N. Objective Measurement of Musculoskeletal Pain: A Comprehensive Review. Diagnostics 2025, 15, 1581. [Google Scholar] [CrossRef] [PubMed]
- Chu, Y; Zhao, X; Han, J; Su, Y. Physiological Signal-Based Method for Measurement of Pain Intensity. Front Neurosci [Internet]. 26 May 2017, 11. Available online: https://www.frontiersin.org/journals/neuroscience/articles/10.3389/fnins.2017.00279/full (accessed on 14 January 2026).
- Wang, X; Jia, R; Li, J; Zhu, Y; Liu, H; Wang, W; et al. Research Progress on the Mechanism of Lumbarmultifidus Injury and Degeneration. Oxid Med Cell Longev. 2021, 2021, 6629037. [Google Scholar] [CrossRef]
- Abd-Elsayed, A; Kurt, E; Kollenburg, L; Hasoon, J; Wahezi, SE; Storlie, NR. Lumbar Multifidus Dysfunction and Chronic Low Back Pain: Overview, Therapies, and an Update on the Evidence. Pain Pract Off J World Inst Pain. 2025, 25, e70044. [Google Scholar] [CrossRef]
- Foster, NE; Anema, JR; Cherkin, D; Chou, R; Cohen, SP; Gross, DP; et al. Prevention and treatment of low back pain: evidence, challenges, and promising directions. The Lancet 2018, 391, 2368–2383. [Google Scholar] [CrossRef]
- da Silva, RA; Vieira, ER; Cabrera, M; Altimari, LR; Aguiar, AF; Nowotny, AH; et al. Back muscle fatigue of younger and older adults with and without chronic low back pain using two protocols: A case-control study. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol. 2015, 25, 928–936. [Google Scholar]
- Abdelaty, EM; Shendy, S; Lotfy, O; Hassan, KA. The difference in multifidus muscle morphology and motor control in non-specific low back pain with clinical lumbar instability and healthy subjects: A case-control study. Physiother Res Int J Res Clin Phys Ther. 2024, 29, e2047. [Google Scholar] [CrossRef]
- Jung, SH; Hwang, UJ; Ahn, SH; Kim, HA; Kim, JH; Kwon, OY. Lumbopelvic motor control function between patients with chronic low back pain and healthy controls: a useful distinguishing tool: The STROBE study. Medicine (Baltimore) 2020, 99, e19621. [Google Scholar]
- Behennah, J; Conway, R; Fisher, J; Osborne, N; Steele, J. The relationship between balance performance, lumbar extension strength, trunk extension endurance, and pain in participants with chronic low back pain, and those without. Clin Biomech. 2018, 53, 22–30. [Google Scholar]
- van Dieën, JH; Reeves, NP; Kawchuk, G; van Dillen, LR; Hodges, PW. Motor Control Changes in Low Back Pain: Divergence in Presentations and Mechanisms. J Orthop Sports Phys Ther. 2019, 42, 11. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, PB; Caneiro, JP; O’Keeffe, M; Smith, A; Dankaerts, W; Fersum, K; et al. Cognitive Functional Therapy: An Integrated Behavioral Approach for the Targeted Management of Disabling Low Back Pain. Phys Ther. 2018, 98, 408–423. [Google Scholar] [CrossRef] [PubMed]
- Shakourisalim, M; Martinez, KB; Golabchi, A; Tavakoli, M; Rouhani, H. Estimation of lower back muscle force in a lifting task using wearable IMUs. J Biomech. 2024, 167, 112077. [Google Scholar] [CrossRef]
- O’Sullivan, P; Caneiro, JP; O’Keeffe, M; O’Sullivan, K. Unraveling the Complexity of Low Back Pain. J Orthop Sports Phys Ther. 2016, 46, 932–937. [Google Scholar] [CrossRef]
- Kumar, R; Marla, K; Sporn, K; Paladugu, P; Khanna, A; Gowda, C; et al. Emerging Diagnostic Approaches for Musculoskeletal Disorders: Advances in Imaging, Biomarkers, and Clinical Assessment. Diagnostics [Internet]. 27 June 2025, 15. Available online: https://www.mdpi.com/2075-4418/15/13/1648 (accessed on 14 January 2026).
- Klasen, BW; Hallner, D; Schaub, C; Willburger, R; Hasenbring, M. Validation and reliability of the German version of the Chronic Pain Grade questionnaire in primary care back pain patients. Psycho-Soc Med. 2004, 1, Doc07. [Google Scholar]
- Ekstrom, RA; Osborn, RW; Hauer, PL. Surface electromyographic analysis of the low back muscles during rehabilitation exercises. J Orthop Sports Phys Ther. 2008, 38, 736–745. [Google Scholar]
- Hermens, HJ; Freriks, B; Disselhorst-Klug, C; Rau, G. Development of recommendations for SEMG sensors and sensor placement procedures. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol. 2000, 10, 361–374. [Google Scholar]
- Phothirook, P; Amatachaya, S; Peungsuwan, P; Phothirook, P; Amatachaya, S; Peungsuwan, P. Muscle Activity and Co-Activation of Gait Cycle during Walking in Water and on Land in People with Spastic Cerebral Palsy. Int J Environ Res Public Health [Internet]. 19 Jan 2023, 20. Available online: https://www.mdpi.com/1660-4601/20/3/1854 (accessed on 19 January 2026).
- Koltermann, JJ; Gerber, M. Quantification of the Dependence of the Measurement Error on the Quantization of the A/D Converter for Center of Pressure Measurements. Biomechanics 2022, 2, 309–318. [Google Scholar] [CrossRef]
- Clark, RA; Bryant, AL; Pua, Y; McCrory, P; Bennell, K; Hunt, M. Validity and reliability of the Nintendo Wii Balance Board for assessment of standing balance. Gait Posture 2010, 31, 307–310. [Google Scholar] [CrossRef]
- Koltermann, JJ; Beck, H; Beck, M; Beck, H; Beck, M. Investigation of the Correlation between Factors Influencing the Spectrum of Center of Pressure Measurements Using Dynamic Controlled Models of the Upright Stand and Subject Measurements. Appl Sci [Internet]. 28 May 2020, 10. Available online: https://www.mdpi.com/2076-3417/10/11/3741 (accessed on 14 January 2026).
- Koltermann, JJ; Gerber, M; Beck, H; Beck, M. Validation of Different Filters for Center of Pressure Measurements by a Cross-Section Study. Technologies [Internet]. 2019, 7. Available online: https://www.mdpi.com/2227-7080/7/4/68 (accessed on 14 January 2026).
- Kongsted, A; Kent, P; Quicke, JG; Skou, ST; Hill, JC. Risk-stratified and stepped models of care for back pain and osteoarthritis: are we heading towards a common model? Pain Rep. 2020, 5, e843. [Google Scholar] [CrossRef] [PubMed]
- Tagliaferri, SD; Miller, CT; Owen, PJ; Mitchell, UH; Brisby, H; Fitzgibbon, B; et al. Domains of Chronic Low Back Pain and Assessing Treatment Effectiveness: A Clinical Perspective. Pain Pract Off J World Inst Pain. 2020, 20, 211–225. [Google Scholar]
- Xu, X; Sekiguchi, Y; Honda, K; Izumi, SI. Motion analysis of 3D multi-segmental spine during gait in symptom remission people with low back pain: a pilot study. BMC Musculoskelet Disord. 2025, 26, 269. [Google Scholar] [CrossRef]
- Smith, JA; Kulig, K. Altered Multifidus Recruitment During Walking in Young Asymptomatic Individuals With a History of Low Back Pain. J Orthop Sports Phys Ther. 2016, 46, 365–374. [Google Scholar] [CrossRef] [PubMed]
- Al-Eisa, E; Egan, D; Deluzio, K; Wassersug, R. Effects of pelvic asymmetry and low back pain on trunk kinematics during sitting: a comparison with standing. Spine 2006, 31, E135–E143. [Google Scholar] [CrossRef]
- Yu, Q; Huang, H; Zhang, Z; Hu, X; Li, W; Li, L; et al. The association between pelvic asymmetry and non-specific chronic low back pain as assessed by the global postural system. BMC Musculoskelet Disord. 2020, 21, 596. [Google Scholar]
- Bryndal, A; Nawos-Wysocki, W; Grochulska, A; Łosiński, K; Glowinski, S. Effects of gait speed on paraspinal muscle activation: an sEMG analysis of the multifidus and erector spinae. PeerJ. 2025, 13, e19244. [Google Scholar] [CrossRef]
- Danneels, LA; Coorevits, PL; Cools, AM; Vanderstraeten, GG; Cambier, DC; Witvrouw, EE; et al. Differences in electromyographic activity in the multifidus muscle and the iliocostalis lumborum between healthy subjects and patients with sub-acute and chronic low back pain. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2002, 11, 13–19. [Google Scholar]
- Zhang, S; Xu, Y; Han, X; Wu, W; Tang, Y; Wang, C. Functional and Morphological Changes in the Deep Lumbar Multifidus Using Electromyography and Ultrasound. Sci Rep. 2018, 8, 6539. [Google Scholar]
- Wattananon, P; Ibrahim, AA; Rujirek, N; Kongoun, S; Klahan, K; Richards, J. Motor unit behavior of lumbar multifidus during a forward trunk bending task performed under different speeds and loads in asymptomatic participants. Sci Rep. 2025, 15, 44822. [Google Scholar] [CrossRef]
- Ruhe, A; Fejer, R; Walker, B. Center of pressure excursion as a measure of balance performance in patients with non-specific low back pain compared to healthy controls: a systematic review of the literature. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2011, 20, 358–368. [Google Scholar]
- Koltermann, JJ; Floessel, P; Hammerschmidt, F; Disch, AC; Koltermann, JJ; Floessel, P; et al. A Statistical and AI Analysis of the Frequency Spectrum in the Measurement of the Center of Pressure Track in the Seated Position in Healthy Subjects and Subjects with Low Back Pain. Sensors [Internet]. 9 May 2024, 24. Available online: https://www.mdpi.com/1424-8220/24/10/3011 (accessed on 14 January 2026).
- Hodges, PW; Richardson, CA. Inefficient muscular stabilization of the lumbar spine associated with low back pain. A motor control evaluation of transversus abdominis. Spine 1996, 21, 2640–2650. [Google Scholar] [PubMed]
- van Dieën, JH; Cholewicki, J; Radebold, A. Trunk muscle recruitment patterns in patients with low back pain enhance the stability of the lumbar spine. Spine 2003, 28, 834–841. [Google Scholar] [CrossRef] [PubMed]
- Naqvi, Waqar M; Vaidya, Laukik; Kumar, Kiran. Impact of low back pain on fear of movement and functional activities. Int J Res Pharm Sci. 2020, 11, 4830–4835. [Google Scholar] [CrossRef]
- Zhou, T; Salman, D; McGregor, AlisonH. Recent clinical practice guidelines for the management of low back pain: a global comparison. BMC Musculoskelet Disord. 2024, 25, 344. [Google Scholar] [CrossRef]
- Paoletti, M; Belli, A; Palma, L; Paniccia, M; Tombolini, F; Ruggiero, A; et al. Data acquired by wearable sensors for the evaluation of the flexion-relaxation phenomenon. Data Brief. 2020, 31, 105957. [Google Scholar] [CrossRef]
- Hodges, PW; Danneels, L. Changes in Structure and Function of the Back Muscles in Low Back Pain: Different Time Points, Observations, and Mechanisms. J Orthop Sports Phys Ther. 2019, 49, 464–476. [Google Scholar] [CrossRef]
- Bednar, DA; Bednar, ED. Internal lumbar disc derangement with instability catch from monosegmental discopathy. The forgotten mechanical and kinetic surgical back pain syndrome. Clin Neurol Neurosurg. 2022, 212, 107033. [Google Scholar]
- Sheeran, L; Al-Amri, M; Sparkes, V; Davies, JL; Sheeran, L; Al-Amri, M; et al. Assessment of Spinal and Pelvic Kinematics Using Inertial Measurement Units in Clinical Subgroups of Persistent Non-Specific Low Back Pain. Sensors [Internet]. 26 Mar 2024, 24. Available online: https://www.mdpi.com/1424-8220/24/7/2127 (accessed on 15 January 2026).
- Sorensen, CJ; Johnson, MB; Norton, BJ; Callaghan, JP; Van Dillen, LR. Asymmetry of lumbopelvic movement patterns during active hip abduction is a risk factor for low back pain development during standing. Hum Mov Sci. 2016, 50, 38–46. [Google Scholar] [CrossRef]
- Faur, C; Patrascu, JM; Haragus, H; Anglitoiu, B. Correlation between multifidus fatty atrophy and lumbar disc degeneration in low back pain. BMC Musculoskelet Disord. 2019, 20, 414. [Google Scholar] [CrossRef]
- Lee, JH; Hoshino, Y; Nakamura, K; Kariya, Y; Saita, K; Ito, K. Trunk muscle weakness as a risk factor for low back pain. A 5-year prospective study. Spine 1999, 24, 54–57. [Google Scholar] [CrossRef]
- Dvir, Z; Keating, JL. Trunk Extension Effort in Patients with Chronic Low Back Dysfunction. Spine 2003, 28, 685. [Google Scholar] [CrossRef]
- Reyes-Ferrada, W; Chirosa-Rios, L; Rodriguez-Perea, A; Jerez-Mayorga, D; Chirosa-Rios, I. Isokinetic Trunk Strength in Acute Low Back Pain Patients Compared to Healthy Subjects: A Systematic Review. Int J Environ Res Public Health 2021, 18, 2576. [Google Scholar] [CrossRef]
- O’Keeffe, M; Ferreira, GE; Harris, IA; Darlow, B; Buchbinder, R; Traeger, AC; et al. Effect of diagnostic labelling on management intentions for non-specific low back pain: A randomized scenario-based experiment. Eur J Pain Lond Engl. 2022, 26, 1532–1545. [Google Scholar] [CrossRef]
- Wirth, B; Schweinhardt, P. Personalized assessment and management of non-specific low back pain. Eur J Pain. 2024, 28, 181–198. [Google Scholar] [CrossRef]
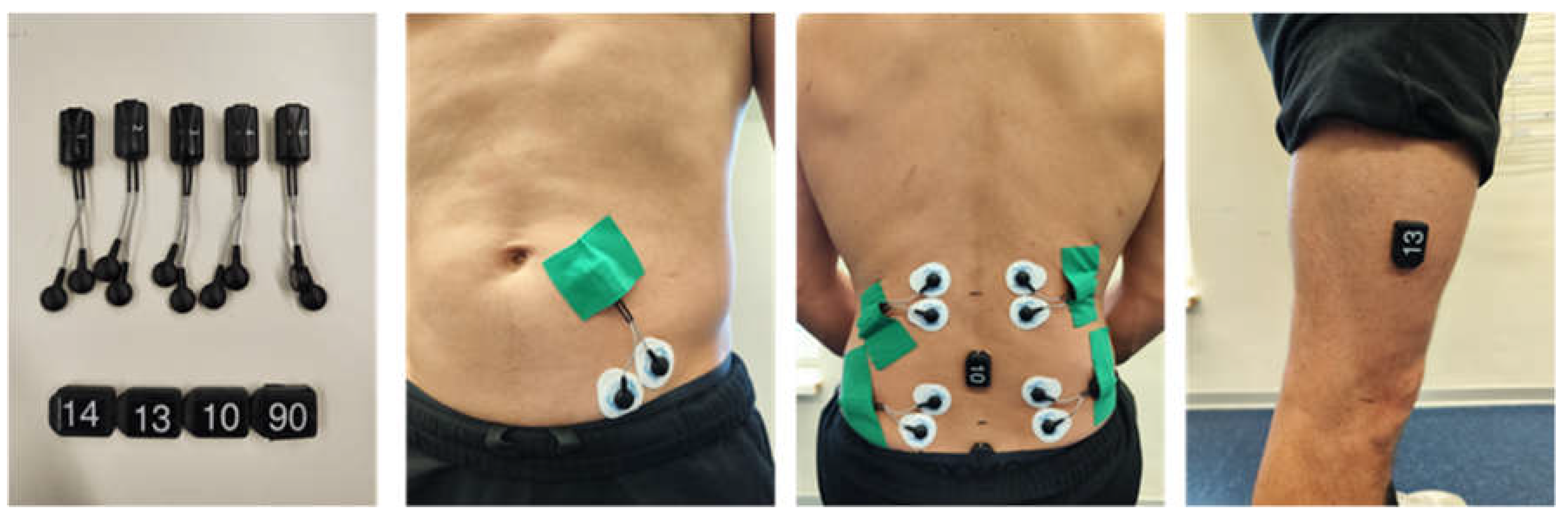
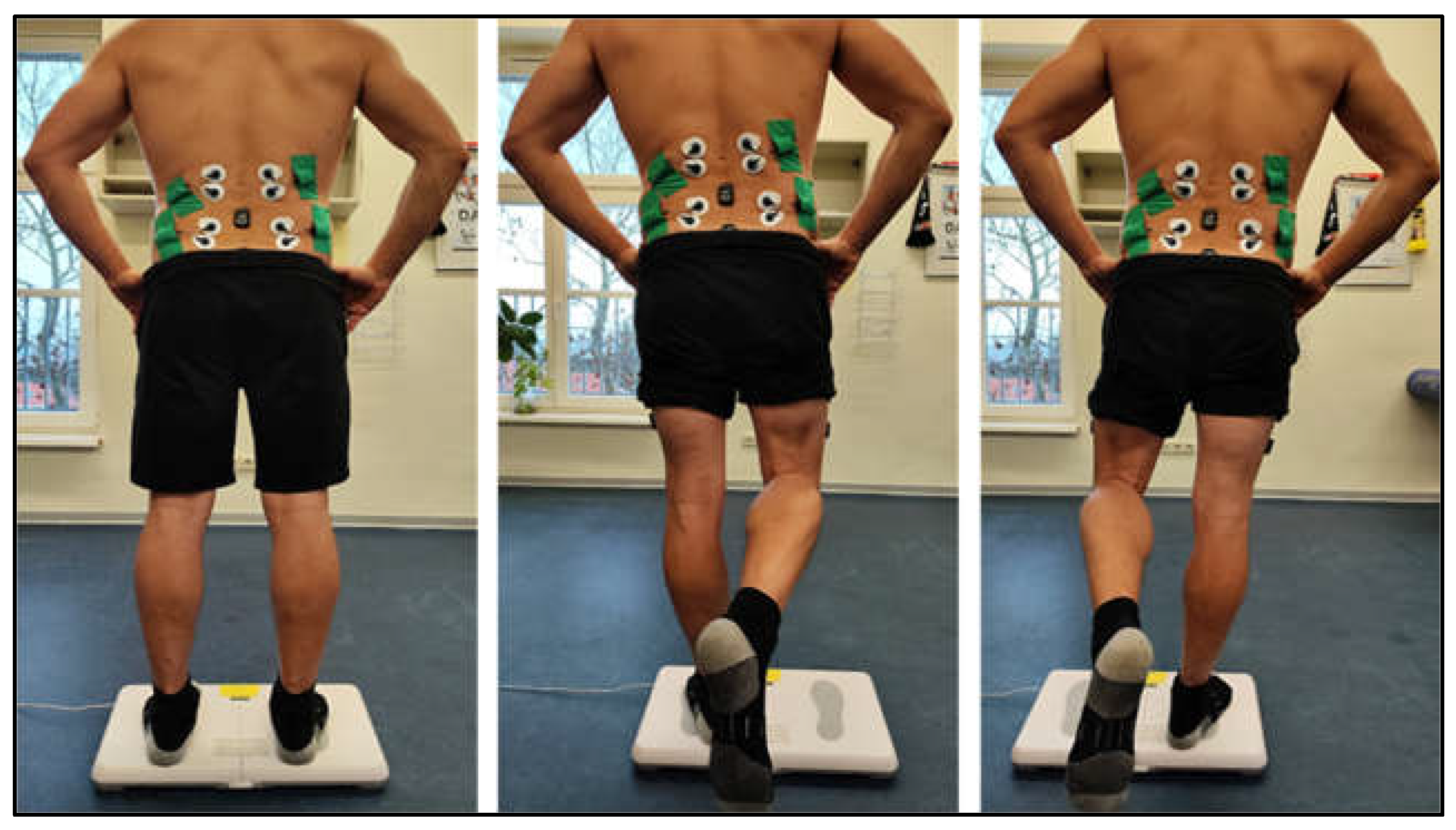
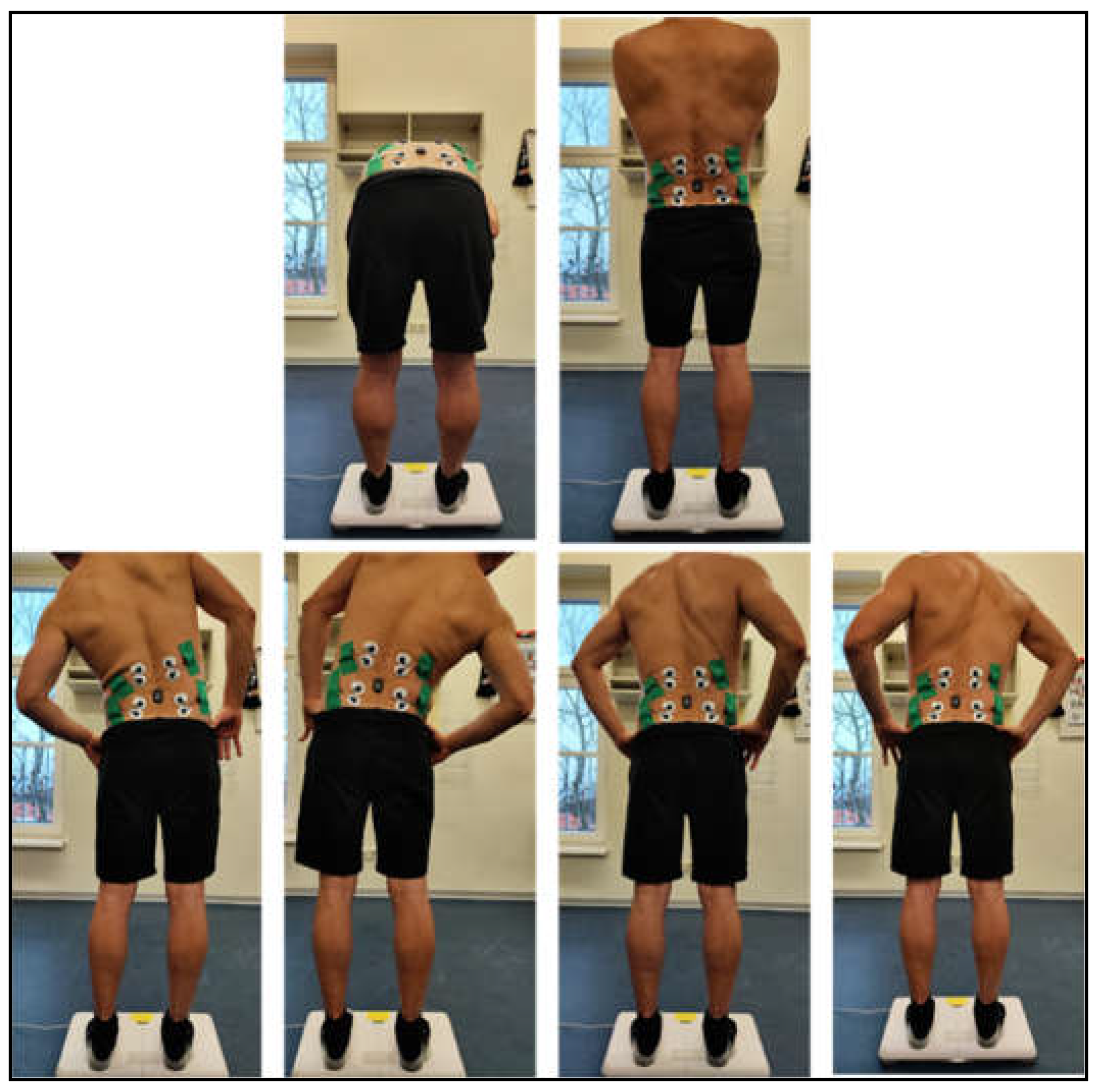
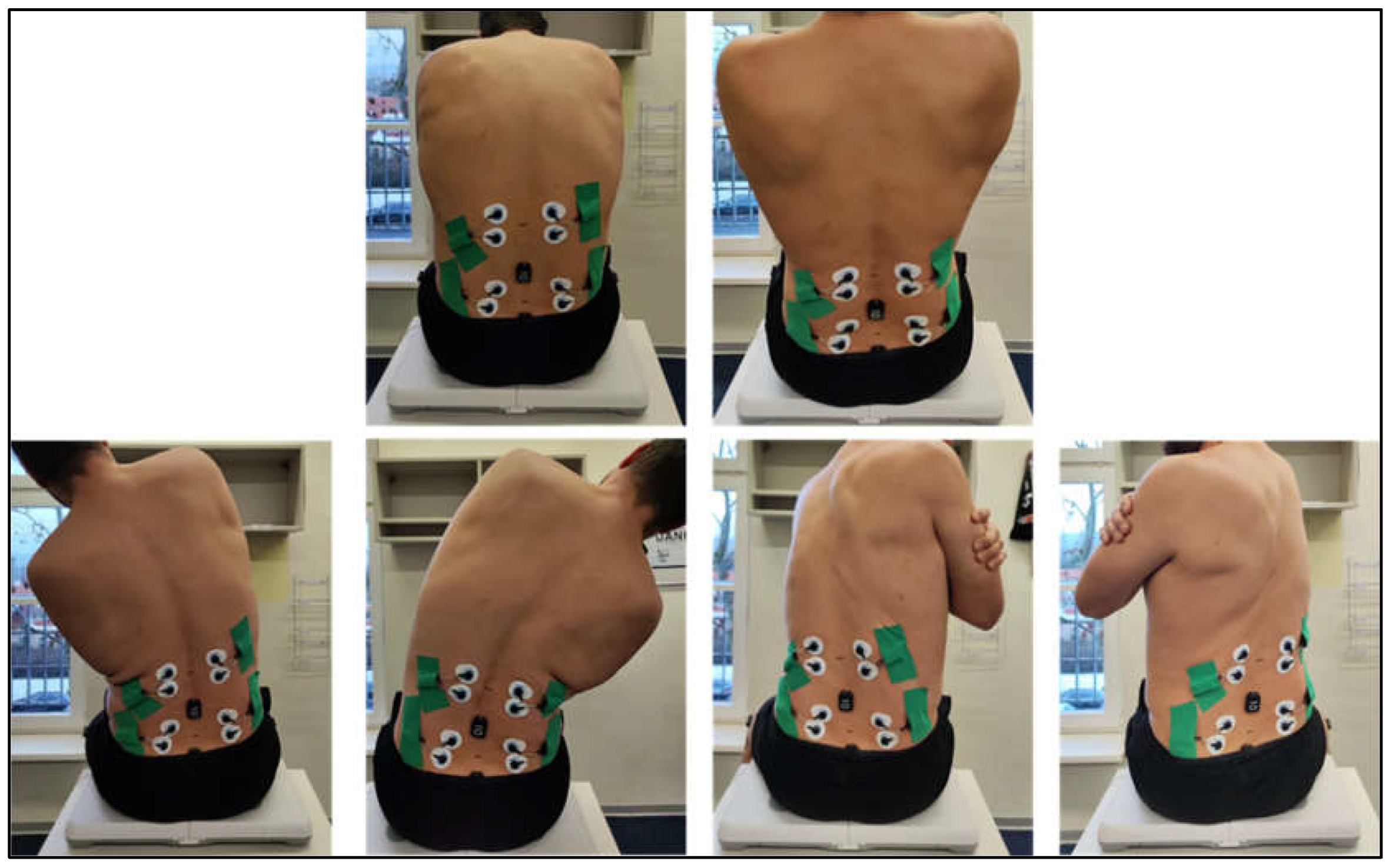
| Group | Male [n] | Height [cm] | Weight [kg] | Age [years] |
|---|---|---|---|---|
| no Pain | 2 | 1760(2.8) | 82.5(13.4) | 34.0(7.1) |
| Low-intensity pain | 6 | 181.3 (5.9) | 89.6(19.8) | 40.1(8.3) |
| High-intensity pain | 5 | 182.8(7.8) | 87.0(13.2) | 40.2(7.2) |
| Group | Female [n] | Height [cm] | Weight [kg] | Age [years] |
| no Pain | 7 | 170.5(5.2) | 66.9(8.0) | 44.7(11.1) |
| Low-intensity pain | 8 | 169.6(6.8) | 69.2(11.6) | 46.8(16.1) |
| High-intensity pain | 10 | 167.4 (4.1) | 70.06(13.2) | 45.7(10.4) |
| Functional Level | Assessment | Technical Equipment |
|---|---|---|
| fatigue resistance/ Strength Endurance |
100m Gait test; | EMG and IMU |
| Mobility and neuromuscular control (CoP) | 60 s bipedal and monopedal (left and right) stance with eyes open; Spinal ROM tests while standing and sitting, every movement twice: flexion/extension, lateral bending and rotation; 60 s upright sitting with eyes open |
CoP- force plate EMG and IMU |
| Lumbo-pelvine Stability | modified slump test | EMG and IMU |
| global trunk musculature | 5x 6 s isometric trunk strength measurements in the sagittal plane in different flexion angular positions of the hip: 90°, 80°, 105° and 120° | IsoMed 2000- Ferstl GmbH |
| Position | Measurement | p.value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|---|
| Pelvis_Acc_X | max_slopeR | 0.043 | 0.558 | 0.02 | 0.02 | 0.035 |
| R_Multifidii | max_slopeL | 0.049 | 0.488 | 0.02 | 0.03 | 0.03 |
| Pelvis_Acc_X | max_steigungR | 0.043 | 0.558 | 0.02 | 0.02 | 0.035 |
| Left_Thigh_Acc_Z | varL | 0.042 | 0.562 | 0.03 | 0.04 | 0.063 |
| Left_Thigh_Acc_Z | max_slopeR | 0.012 | 0.759 | 0.01 | 0.02 | 0.028 |
| Left_Thigh_Acc_Z | max_steigungR | 0.012 | 0.759 | 0.01 | 0.02 | 0.02 |
| L_Multifidii | meanR | 0.05 | 0.505 | 0.0009 | 0.0007 | 0.0005 |
| R_Multifidii | aucR | 0.046 | 0.509 | 0.07 | 0.07 | 0.05 |
| Measurement | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|
| FreqBandEnergy_L | 0.023 | 0.661 | 2.54E+14 | 2.7E+14 | 3.98E+14 |
| AreaTrembling | 0.033 | 0.599 | 1.53E+14 | 4.46E+14 | 4.2E+14 |
| SwayArea_Ellipse | 0.024 | 0.654 | 1.99E+14 | 4.3E+14 | 4.61E+14 |
| MeanFreq_X | 0.048 | 0.505 | 2.30E+14 | 3.34E+14 | 3.82E+14 |
| Power_Y | 0.031 | 0.608 | 1.99E+14 | 2.3E+14 | 2.67E+14 |
| Power_X | 0.027 | 0.634 | 3.6E+14 | 2.94E+14 | 1.72E+14 |
| DistanceTrembling | 0.05 | 0.523 | 5.0E+14 | 4.58E+14 | 3.87E+14 |
| FreqBandEnergy_H | 0.019 | 0.691 | 3.06E+14 | 3.89E+14 | 5.72E+14 |
| VelocityTrembling | 0.04 | 0.57 | 3.88E+14 | 3.07E+14 | 1.65E+14 |
| DominantFreq_Y | 0.049 | 0.497 | 152587890.6 | 3.33E+08 | 6.1E+08 |
| Position | measurement | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|---|
| R_Int_Oblique | minENV | 0.033 | 0.60 | -7.48 | -0.05 | 0.54 |
| L_Multifidii | minENV | 0.001 | 0.93 | 2.12 | 0.81 | -0.47 |
| R_ThoracicEs | minRAW | 0.055 | 0.47 | -81.22 | -102.67 | -166.51 |
| R_ThoracicEs | maxRAW | 0.052 | 0.48 | 76.29 | 109.66 | 181.36 |
| L_ThoracicEs | minRAW | 0.047 | 0.53 | -96.84 | -83.80 | -163.481 |
| R_Multifidii | minENV | 0.012 | 0.75 | -2.07 | -0.45 | 1.60 |
| measurement | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|
| LWS_Acc_X_max | 0.024 | 0.658 | 1.185 | 0.92 | 0.84 |
| LWS_Acc_X_range | 0.03 | 0.623 | 1.18 | 0.94 | 0.85 |
| LWS_roll_max | 0.019 | 0.69 | 78.44 | 68.40 | 60.99 |
| LWS_roll_range | 0.023 | 0.665 | 81.93 | 65.67 | 58.26 |
| Pelvis_Acc_X_max | 0.03 | 0.62 | 0.940 | 0.68 | 0.64 |
| Pelvis_Acc_X_range | 0.03 | 0.623 | 0.93 | 0.68 | 0.64 |
| Pelvis_roll_max | 0.028 | 0.632 | 58.19 | 47.66 | 42.95 |
| R_Multifidii_env_min | 0.049 | 0.512 | 3.14 | 3.20 | 6.66 |
| L_Multifidii_env_min | 0.034 | 0.598 | 2.79 | 3.38 | 7.99 |
| LWS_Acc_X_area | 0.037 | 0.582 | 3.02 | 2.34 | 1.92 |
| lws_pelvis_pitch_min | 0.003 | 0.905 | 4.47 | 0.43 | 0.06 |
| measurement | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|
| LWS_Acc_X_area | 0.012 | 0.753 | 4.03 | 2.66 | 2.37 |
| lws_pelvis_pitch_min | 0.009 | 0.798 | 6.5 | 1.99 | 0.09 |
| R_ThoracicEs_env_mean | 0.035 | 0.594 | 13.46 | 18.02 | 23.08 |
| R_ThoracicEs_env_RMS | 0.039 | 0.576 | 15.51 | 21.55 | 26.43 |
| L_Multifidii_DutyCycle | 0.042 | 0.563 | 0.71 | 0.77 | 0.88 |
| LWS_Acc_X_area | 0.005 | 0.845 | 3.90 | 2.82 | 2.24 |
| LWS_Acc_Y_min | 0.029 | 0.626 | -0.12 | -0.06 | -0.041 |
| lws_pelvis_pitch_area | 0.021 | 0.681 | 216.87 | 123.89 | 125.03 |
| LWS_pitch_area | 0.031 | 0.613 | 426.20 | 342.91 | 286.77 |
| LWS_roll_range | 0.031 | 0.617 | 102.96 | 65.04 | 62.29 |
| Pelvis_Acc_X_area | 0.017 | 0.711 | 2.91 | 2.18 | 1.68 |
| pelvis_thigh_roll_area | 0.018 | 0.705 | 175.35 | 125.86 | 117.24 |
| R_Multifidii_env_min | 0.016 | 0.719 | 2.33 | 2.48 | 6.02 |
| R_ThoracicEs_raw_mean | 0.036 | 0.587 | 0.00 | 0.007 | 0.016 |
| Measurement | p value | power | Mean no Pain | Mean Low intensity pain | Mean High-intensity pain |
|---|---|---|---|---|---|
| Nm/ kg | Nm/ kg | Nm/ kg | |||
| flex_max_0 | 0.033 | 0.607 | 1.28 | 1.31 | 1.67 |
| flex_max_10 | 0.702 | 0.067 | 1.24 | 1.22 | 1.58 |
| ext_max_0 | 0.029 | 0.634 | 3.01 | 2.68 | 2.62 |
| ext_max_15 | 0.016 | 0.724 | 3.19 | 2.78 | 2.73 |
| ext_max_30 | 0.879 | 0.053 | 3.13 | 2.71 | 2.82 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




