Submitted:
15 January 2026
Posted:
16 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Sample
2.2. Procedure
2.3. Measures
2.3.1. Self-Perceptions of Memory Deficits
2.3.2. Attitudes Towards Aging
2.3.3. Aging Stereotypes
2.3.4. Subjective Age
| Source | Variable name | Description | Interpretation of highest score |
|---|---|---|---|
| Perceptions of memory complaints | |||
| Illness Perception Questionnaire-Memory (IPQ-M) (Hurt et al, 2010) | Identity | Number of physical symptoms related to memory problems |
More symptoms related to memory problems |
| Timeline acute/chronic |
Expected duration of their memory problems | Memory problems will persist for a long time | |
| Timeline stability/decline |
Perceived progression of memory | Memory problems will worsen over time | |
| Personal control (Helplessness) |
Perceived ability to prevent/improve memory problems |
Stronger perceived control over memory problems. | |
| Personal control (Blame) |
Guilt about not doing enough to prevent memory problems | Stronger feeling of guilt | |
| Consequences | Negative impact of memory problems on one's life | Memory problems have a negative impact on life. | |
| Treatment control | Memory problems can be managed with medical care | Medical treatment can help manage memory | |
| Emotional representation |
Negative emotional response to memory problems |
Stronger negative emotional reactions to memory problems. | |
| Illness coherence | Perceived understanding of one’s memory problems | Greater insight regarding memory problems | |
| Social comparison | Comparison of one's memory with that of same-aged peers | Stronger perceptions of having a worse memory than same-aged peers | |
| Attitudes towards aging | |||
| Aging opinion survey (Kafer et al, 1980) | Personal anxiety | Anxiety and negative emotions about one’s own aging | Greater anxiety toward aging |
| Aging Perceptions Questionnaire (Barker et al, 2007) | Consequences positives |
Beneficial aspect of aging | More positive attitudes toward aging |
| Control positive | Positive aspects depend on their own actions | More positive attitudes toward aging | |
| Fear of Alzheimer's Disease Scale (French et al, 2012) | Fear of developing Alzheimer's disease (AD) | Concerns related to the possibility of developing Alzheimer’s disease | Stronger general fear of developing the disease |
| Stereotypes of older adults | |||
| Attitudes towards older people (Tuckman and Lorge, 1953) | Mental deterioration | Negative stereotypical beliefs about age-related cognitive decline | Stronger endorsement of negative stereotypes about cognitive aging |
| Subjective age | |||
| Self-perceptions of aging (Kotter-Grühn & Hess, 2012) | Felt age | Age the person feels | A negative score indicates feeling younger than their chronological age, a positive score indicates feeling older |
| Desired age | Age the person wishes to have | ||
| Apparent age | Age the person believes others attribute to them | ||
| Patient group (hospital) n = 129 |
Control group (laboratory) n = 84 |
p-value | η2 p | |||
|---|---|---|---|---|---|---|
| Mean (± SD) | Cronbach’s α | Mean (± SD) | Cronbach’s α | |||
| Self-perceptions of memory deficits | ||||||
| Identity | 8.04 (±4.37) | - | 6.79 (±4.54) | - | .048 | 0.02 |
| Timeline acute/chronic (Time_a/c) | 3.55 (±0.93) | 0.78 | 3.70 (±0.94) | 0.71 | .250 | 0.01 |
| Timeline stability/decline (Time_s/d) | 3.79 (±0.93) | 0.88 | 3.79 (±0.94) | 0.84 | .990 | 0.00 |
| Personal control (Blame) | 3.29 (±0.91) | 0.78 | 3.66 (±0.94) | 0.73 | .005 | 0.04 |
| Consequences (Conseq) | 2.85 (±0.89) | 0.58 | 2.08 (±0.90) | 0.72 | <.001 | 0.15 |
| Emotional representation (Emo_Rep) | 3.31 (±1.15) | 0.86 | 2.45 (±1.15) | 0.83 | <.001 | 0.12 |
| Illness coherence (Ill_Coh) | 2.68 (±1.03) | 0.59 | 3.51 (±1.04) | 0.72 | <.001 | 0.13 |
| Social comparison (Soc_Comp) | 2.99 (±0.92) | 0.76 | 2.42 (±0.93) | 0.77 | <.001 | 0.08 |
| Attitudes toward aging | ||||||
| Personal anxiety towards aging (Anxiety) | 2.89 (±0.75) | 0.73 | 2.71 (±0.75) | 0.57 | .091 | 0.01 |
| Consequences positive (Conseq_pos) | 3.63 (±0.85) | 0.68 | 3.57 (±0.86) | 0.76 | .641 | 0.00 |
| Control positive (Ctrl_pos) | 4.33 (±0.66) | 0.78 | 4.41 (±0.66) | 0.66 | .406 | 0.00 |
| General fear (Gen_Fear) | 2.86 (±0.97) | 0.65 | 2.48 (±0.99) | 0.66 | .008 | 0.04 |
| Stereotypes of older adults | ||||||
| Mental deterioration (Men_Det) | 2.44 (±0.58) | 0.84 | 2.44 (±0.59) | 0.84 | .994 | 0.00 |
| Subjective age | ||||||
| Felt age | 63.10 (±8.23) | - | 61.20 (±8.44) | - | .116 | 0.01 |
| Discrepancy score for Felt age (Felt_a) | -8.98 (±11.81) | - | -11.68 (±12.10) | - | .114 | 0.01 |
| Desired age | 47.60 (±14.54) | - | 45.40 (±14.39) | - | .288 | 0.00 |
| Discrepancy score for Desired age (Des_a) | -30.80 (±20.67) | - | -34.00 (±20.35) | - | .277 | 0.00 |
| Apparent age | 62.00 (±4.99) | - | 62.10 (±4.87) | - | .846 | 0.00 |
| Discrepancy score for Apparent age (App_a) | -10.06 (±7.16) | - | -9.76 (±6.97) | - | .766 | 0.00 |
2.4. Statistical Analysis
2.5. Data Preparation
3. Results
3.1. Descriptive Statistics
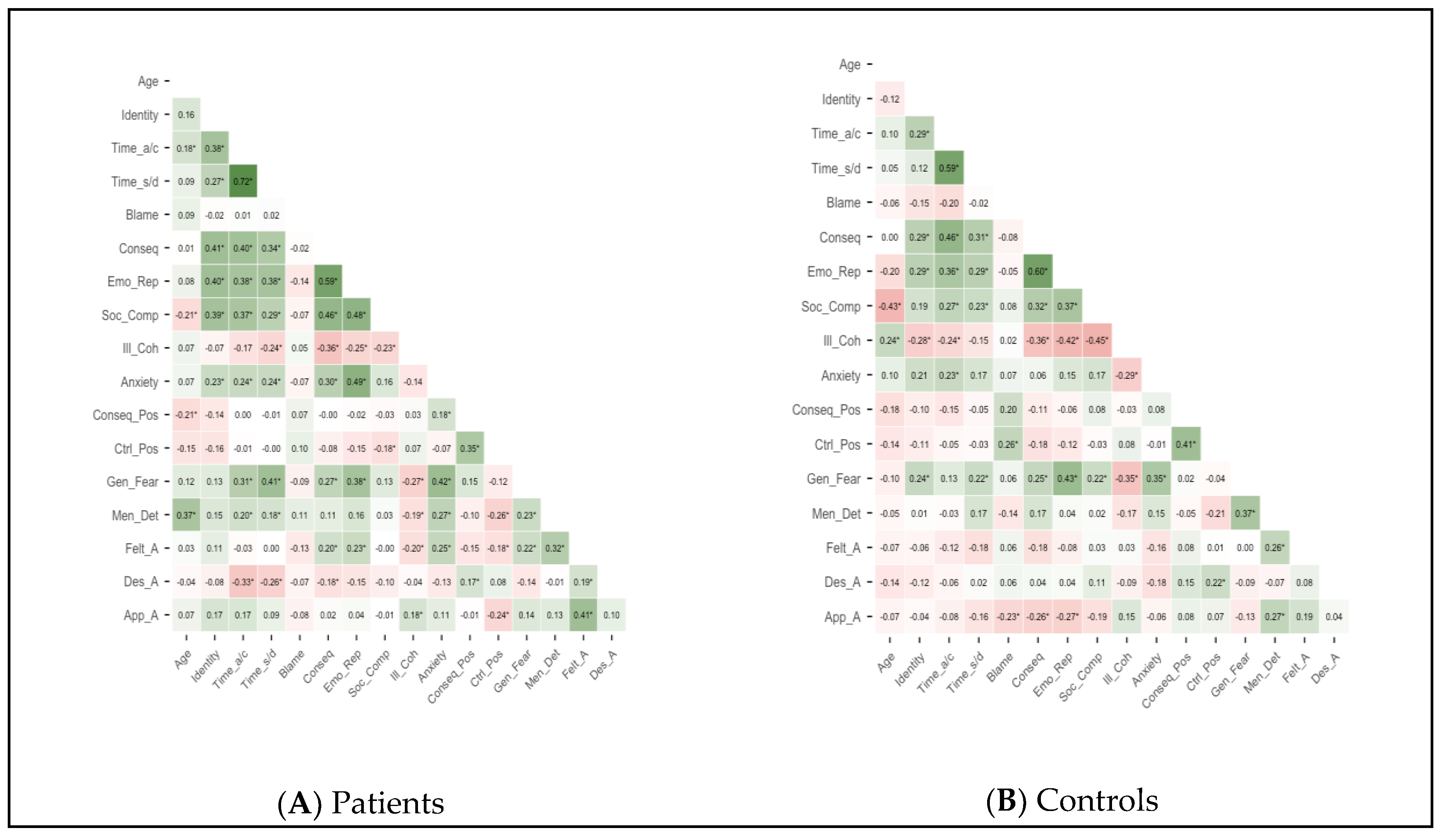
3.2. Correlation Matrix
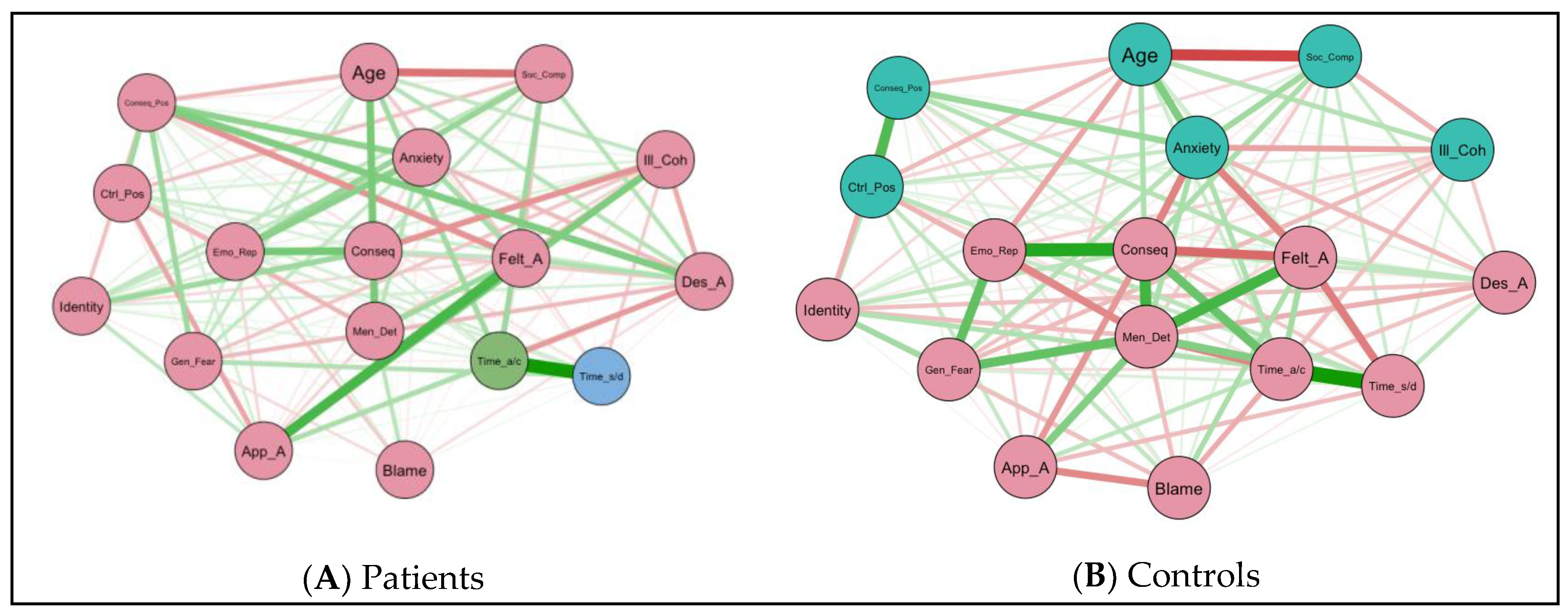
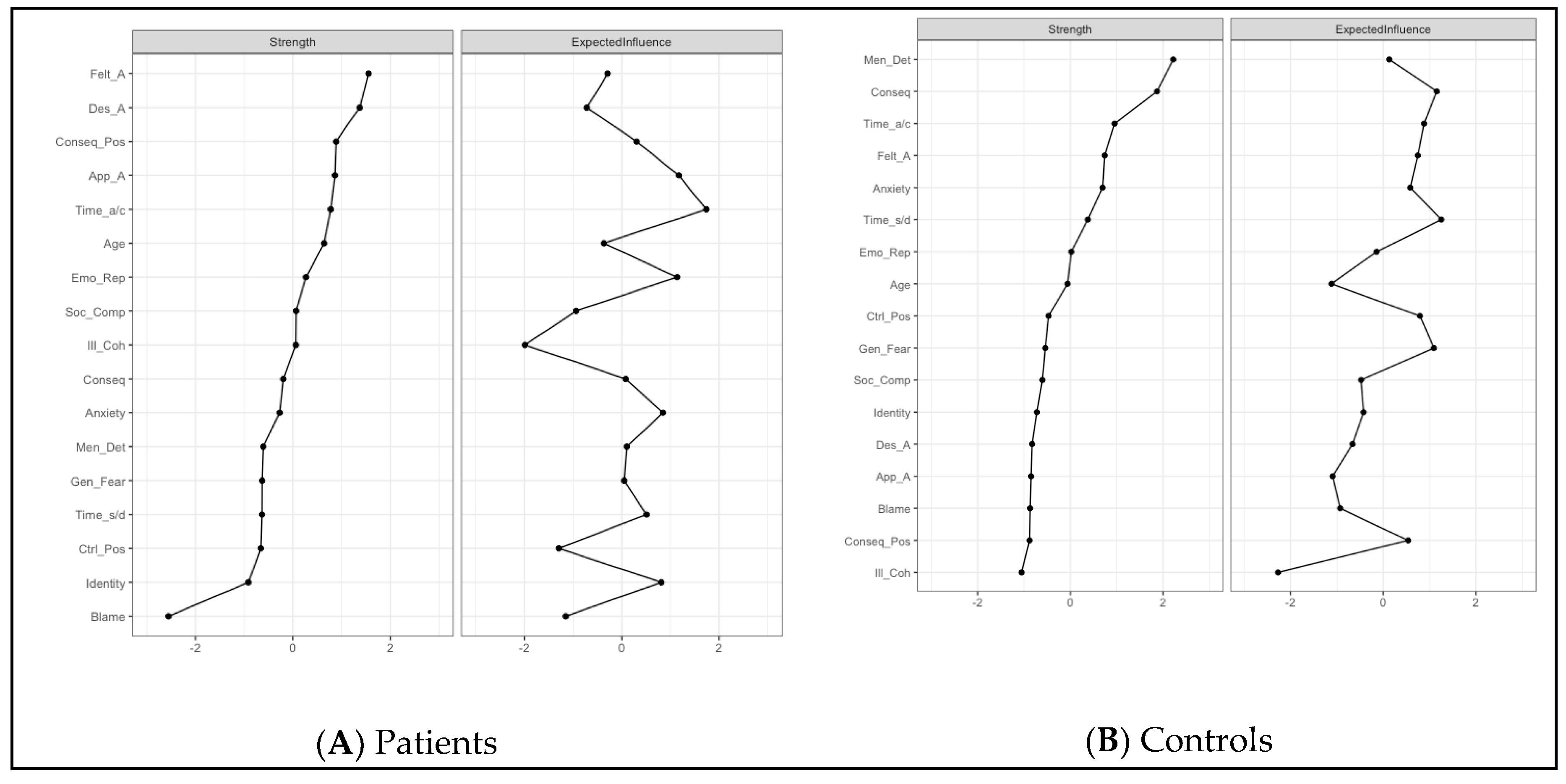
3.3. Network Analysis
4. Discussion
4.1. Chronicity Beliefs and Subjective Age as Influencers of Emotional Distress in Patients
4.2. Internalizing Aging Stereotypes in the Control Sample
4.3. Illness Coherence as a Regulator of Emotional Distress Across Groups
4.4. Community Structure of Representational Networks
4.5. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| MMSE | Mini Mental State Examination |
| QCC | Questionnaire of Cognitive Complaints |
| GDS | Geriatric Depression Scale |
| IADL | Instrumental Activities of Daily Living |
| NINCDS-ADRDA | National Institute of Neurological and Communicative Diseases and Stroke/Alzheimer's Disease and Related Disorders Association |
| SPC | Socio-professional category |
| MG-CFA | Multi-Group Confirmatory Factor Analysis |
| IPQ-M | Illness Perceptions Questionnaire - Memory |
| AOS | Aging Opinion Survey |
| APQ | Aging Perceptions Questionnaire |
| FADS | Fear of Alzheimer’s Disease Scale |
| GGM | Gaussian Graphical Models |
| CS-coefficients | Correlation Stability Coefficients |
| MCAR | Missing Completely at Random |
| MICE | Multiple Imputation by Chained Equations |
| Time_a/c | Timeline acute/chronic |
| Time_s/d | Timeline stability/decline |
| Blame | Personal control (Blame) |
| Conseq | Consequences |
| Emo_Rep | Emotional representation |
| Ill_Coh | Illness coherence |
| Soc_Comp | Social comparison |
| Anxiety | Personal anxiety towards aging |
| Conseq_Pos | Consequences positive |
| Ctrl_Pos | Control positive |
| Gen_Fear | General fear; |
| Men_Det | Mental deterioration |
| Felt_A | Felt age |
| Des_A | Desired age |
| App_A | Apparent age |
| Age | Chronological age |
| EI | Expected Influence |
References
- Deary, I. J., Corley, J., Gow, A. J., Harris, S. E., Houlihan, L. M., Marioni, R. E., Penke, L., Rafnsson, S. B., & Starr, J. M. Age-associated cognitive decline. British Medical Bulletin, 2009, 92(1), 135–152. [CrossRef]
- Corley, J., Conte, F., Harris, S. E., Taylor, A. M., Redmond, P., Russ, T. C., Deary, I. J., & Cox, S. R. Predictors of longitudinal cognitive ageing from age 70 to 82 including APOE e4 status, early-life and lifestyle factors: The Lothian Birth Cohort 1936. Molecular Psychiatry, 2023, 28(3), 1256–1271. [CrossRef]
- Ekström, I., Josefsson, M., Bäckman, L., & Laukka, E. J. Predictors of cognitive aging profiles over 15 years: A longitudinal population-based study. Psychology and Aging, 2024, 39(5), 467–483. [CrossRef]
- Ten Kate, M., Dicks, E., Visser, P. J., Van Der Flier, W. M., Teunissen, C. E., Barkhof, F., Scheltens, P., Tijms, B. M., & Alzheimer’s Disease Neuroimaging Initiative. Atrophy subtypes in prodromal Alzheimer’s disease are associated with cognitive decline. Brain, 2018, 141(12), 3443–3456. [CrossRef]
- Hurt, C. S., Burns, A., Brown, R. G., & Barrowclough, C. Perceptions of subjective memory complaint in older adults: The Illness Perception Questionnaire – Memory (IPQ-M). International Psychogeriatrics, 2010, 22(5), 750–760. [CrossRef]
- Shinan-Altman, S., & Werner, P. Illness representations of dementia: A scoping review. Clinical Interventions in Aging, 2019, Volume 14, 179–193. [CrossRef]
- Cosentino, S., Devanand, D., & Gurland, B. A Link between Subjective Perceptions of Memory and Physical Function: Implications for Subjective Cognitive Decline. Journal of Alzheimer’s Disease, 2018, 61(4), 1387–1398. [CrossRef]
- García-García, L., Fernandes-Pires, J. A., Márquez-González, M., Pedroso-Chaparro, M. D. S., Benito-Rincón, C., Pérez-Cardona, L. M., & Losada-Baltar, A. Self-perceptions of Aging and Distress in Middle-aged and Older Adults. The Role of Perceived Control and Pleasant Activities. The Spanish Journal of Psychology, 2025, 28, e8. [CrossRef]
- Levy, B. Stereotype Embodiment: A Psychosocial Approach to Aging. Current Directions in Psychological Science, 2009, 18(6), 332–336. [CrossRef]
- Barber, S. J. The applied implications of age-based stereotype threat for older adults. Journal of Applied Research in Memory and Cognition, 2020, 9(3), 274–285. [CrossRef]
- Fernández-Ballesteros, R., Bustillos, A., & Huici, C. Positive Perception of Aging and Performance in a Memory Task: Compensating for Stereotype Threat? Experimental Aging Research, 2015, 41(4), 410–425. [CrossRef]
- Kotter-Grühn, D., & Hess, T. M. The Impact of Age Stereotypes on Self-perceptions of Aging Across the Adult Lifespan. The Journals of Gerontology: Series B, 2012, 67(5), 563–571. [CrossRef]
- Wettstein, M., Wahl, H.-W., Drewelies, J., Wurm, S., Huxhold, O., Ram, N., & Gerstorf, D Younger Than Ever? Subjective Age Is Becoming Younger and Remains More Stable in Middle-Age and Older Adults Today. Psychological Science, 2023, 34(6), 647–656. [CrossRef]
- Hagger, M. S., & Orbell, S. The common-sense model of illness self-regulation: A conceptual review and proposed extended model. Health Psychology Review, 2022, 16(3), 347–377. [CrossRef]
- Petrie, K. J., Jago, L. A., & Devcich, D. A. The role of illness perceptions in patients with medical conditions: Current Opinion in Psychiatry, 2007, 20(2), 163–167. [CrossRef]
- Lin, F., Gleason, C. E., & Heidrich, S. M. Illness Representations in Older Adults with Mild Cognitive Impairment. Research in Gerontological Nursing, 2012, 5(3), 195–206. [CrossRef]
- Perry-Young, L., Owen, G., Kelly, S., & Owens, C. How people come to recognise a problem and seek medical help for a person showing early signs of dementia: A systematic review and meta-ethnography. Dementia, 2018, 17(1), 34–60. [CrossRef]
- Tyrrell, M., Religa, D., Fossum, B., Hedman, R., Skovdahl, K., & Hillerås, P. Embarking on a memory assessment voice of older persons living with memory impairment. Dementia, 2021, 20(2), 717–733. [CrossRef]
- Visser, L. N. C., Fruijtier, A., Kunneman, M., Bouwman, F. H., Schoonenboom, N., Staekenborg, S. S., Wind, H. A., Hempenius, L., De Beer, M. H., Roks, G., Boelaarts, L., Kleijer, M., Smets, E. M. A., & Van Der Flier, W. M. Motivations of patients and their care partners for visiting a memory clinic. A qualitative study. Patient Education and Counseling, 2023, 111, 107693. [CrossRef]
- Jiao, Y.-C., Chang, J., Liu, C., Zhou, S.-Y., Ji, Y., & Meng, Y. Factors influencing the help-seeking behavior in patients with mild cognitive impairment: A qualitative study. BMC Health Services Research, 2023, 23(1), 1345. [CrossRef]
- Régner, I., & Huguet, P. Age-based stereotype threat effects: From the laboratory to the clinical setting. Cortex, 2025, 183, 261–273. [CrossRef]
- Barber, S. J., Mather, M., & Gatz, M. How Stereotype Threat Affects Healthy Older Adults’ Performance on Clinical Assessments of Cognitive Decline: The Key Role of Regulatory Fit. The Journals of Gerontology Series B: Psychological Sciences and Social Sciences, 2015, 70(6), 891–900. [CrossRef]
- Haslam, C., Morton, T. A., Haslam, S. A., Varnes, L., Graham, R., & Gamaz, L “When the age is in, the wit is out”: Age-related self-categorization and deficit expectations reduce performance on clinical tests used in dementia assessment. Psychology and Aging, 2012, 27(3), 778–784. [CrossRef]
- Mazerolle, M., Régner, I., Barber, S. J., Paccalin, M., Miazola, A. C., Huguet, P., & Rigalleau, F. Negative Aging Stereotypes Impair Performance on Brief Cognitive Tests Used to Screen for Predementia. The journals of gerontology. Series B, Psychological sciences and social sciences, 2017, 72(6), 932–936. [CrossRef]
- Mazerolle, M., Régner, I., Rigalleau, F., & Huguet, P. Stereotype Threat Alters the Subjective Experience of Memory. Experimental psychology, 2015, 62(6), 395–402. [CrossRef]
- Leventhal, H., Meyer, D., & Nerenz, D. The Common Sense Model of Illness Representations. Medical Psychology, 1980, 2, 7–30.
- Hagger, M. S., & Orbell, S. A Meta-Analytic Review of the Common-Sense Model of Illness Representations. Psychology & Health, 2003, 18(2), 141–184. [CrossRef]
- Hill, N. L., Do, J., Bratlee-Whitaker, E., Turner, J. R., Sillner, A., Fishman, C., & Mogle, J. Views of Aging and Subjective Cognition in Middle-Aged and Older Adults: A Systematic Review. Gerontology, 2024, 71(1), 49–70. [CrossRef]
- Barker, M., O’Hanlon, A., McGee, H. M., Hickey, A., & Conroy, R. M. Cross-sectional validation of the Aging Perceptions Questionnaire: A multidimensional instrument for assessing self-perceptions of aging. BMC Geriatrics, 2007, 7(1), 9. [CrossRef]
- Westerhof, G. J., Nehrkorn-Bailey, A. M., Tseng, H.-Y., Brothers, A., Siebert, J. S., Wurm, S., Wahl, H.-W., & Diehl, M. Longitudinal effects of subjective aging on health and longevity: An updated meta-analysis. Psychology and Aging, 2023, 38(3), 147–166. [CrossRef]
- Klusmann, V., Sproesser, G., Wolff, J. K., & Renner, B. Positive Self-perceptions of Aging Promote Healthy Eating Behavior Across the Life Span via Social-Cognitive Processes. The Journals of Gerontology: Series B, 2019, 019, 74(5), 735–744. [CrossRef]
- French, S. L., Floyd, M., Wilkins, S., & Osato, S. The Fear of Alzheimer’s Disease Scale: A new measure designed to assess anticipatory dementia in older adults. International Journal of Geriatric Psychiatry, 2012, 27(5), 521–528. [CrossRef]
- Westerhof, G. J., Miche, M., Brothers, A. F., Barrett, A. E., Diehl, M., Montepare, J. M., Wahl, H.-W., & Wurm, S. The influence of subjective aging on health and longevity: A meta-analysis of longitudinal data. Psychology and Aging, 2014, 29(4), 793–802. [CrossRef]
- Klaiber, P., & Pauly, T. Daily Fluctuations in Subjective Age among Older Adults: Links with Stressors, Positive Events, and Emotional Reactions. Gerontology, 2025, 71(3), 239–251. [CrossRef]
- Aftab, A., Lam, J. A., Thomas, M. L., Daly, R., Lee, E. E., & Jeste, D. V. Subjective age and its relationships with physical, mental, and cognitive functioning: A cross-sectional study of 1,004 community-dwelling adults across the lifespan. Journal of Psychiatric Research, 2022, 152, 160–166. [CrossRef]
- Nelson, A. P., & O’Connor, M. G. Mild Cognitive Impairment: A Neuropsychological Perspective. CNS Spectrums, 2008, 13(1), 56–64. [CrossRef]
- Delrieu, J., Ceccaldi, M., Epelbaum, S., Gabelle, A., Krolak-Salmon, P., Paquet, C., & Vellas, B. La maladie d’Alzheimer au stade prodromal : comment pouvons-nous la diagnostiquer et la prendre en charge ? Devons-nous le faire ?. Année Gérontologique, 2018, 32(2).
- Delage, É., Rouleau, I., Akzam-Ouellette, M.-A., Rahayel, S., Filiatrault, M., & Joubert, S. Patterns of cortical thickness in MCI patients with and without semantic impairment. Brain and Cognition, 2025, 184, 106258. [CrossRef]
- Epskamp, S., Rhemtulla, M., & Borsboom, D. Generalized Network Psychometrics: Combining Network and Latent Variable Models. Psychometrika, 2017, 82(4), 904–927. [CrossRef]
- Hevey, D. Network analysis: A brief overview and tutorial. Health Psychology and Behavioral Medicine, 2018, 6(1), 301–328. [CrossRef]
- Folstein, M. F., Folstein, S. E., & McHugh, P. R. “Mini-mental state.” Journal of Psychiatric Research, 1975, 12(3), 189–198. [CrossRef]
- Thomas-Antérion, C., Ribas, C., Honoré-Masson,S., Berne, G., Rule, JH., Laurent, B. Le questionnaire de plainte cognitive (QPC) : un outil de recherche de plainte suspecte d’évoquer une maladie d’Alzheimer. Année Gérontologique, 2003, 17, 56-65.
- Yesavage, J. A., Brink, T. L., Rose, T. L., Lum, O., Huang, V., Adey, M., & Leirer, V. O. Development and validation of a geriatric depression screening scale: A preliminary report. Journal of Psychiatric Research, 1982, 17(1), 37–49. [CrossRef]
- Dubois B, Touchon J, Portet F, Ousset PJ, Vellas B, Michel B. « Les cinq mots » épreuve simple et sensible pour le diagnostic de la maladie d’Alzheimer. Presse médicale 2002; 31:1696–9.
- Lawton, M. P., & Brody, E. M. Assessment of older people: self-maintaining and instrumental activities of daily living. The Gerontologist, 1969, 9(3), 179–186.
- Sawilowsky, S. S. New Effect Size Rules of Thumb. Journal of Modern Applied Statistical Methods, 2009, 8(2), 597–599. [CrossRef]
- Gauthier, K., Morand, A., Dutheil, F., Alescio-Lautier, B., Boucraut, J., Clarys, D., Eustache, F., Girard, N., Guedj, E., Mazerolle, M., Paccalin, M., De La Sayette, V., Zaréa, A., Huguet, P., Michel, B. F., Desgranges, B., AGING consortium, & Régner, I. Ageing stereotypes and prodromal Alzheimer’s disease (AGING): Study protocol for an ongoing randomised clinical study. BMJ Open, 2019, 9(10), e032265. [CrossRef]
- Besozzi, A. Etude des perceptions des troubles mnésiques au cours de la démarche diagnostique en consultation `` mémoire ’ ’. Université de Lorraine, France, 2017.
- Kafer, R. A., Rakowskl, W., Lachman, M., & Hickey, T. Aging Opinion Survey: A Report on Instrument Development. The International Journal of Aging and Human Development, 1980, 11(4), 319–333. [CrossRef]
- Tuckman, J., & Lorce, I. Attitudes towards old people. The Journal of Social Psychology, 1953, 37, 249-260.
- Epskamp, S., Borsboom, D., & Fried, E. I. Estimating psychological networks and their accuracy: A tutorial paper. Behavior Research Methods, 2018, 50(1), 195–212. [CrossRef]
- Constantin, M. A., Schuurman, N. K., & Vermunt, J. K. A general Monte Carlo method for sample size analysis in the context of network models. Psychological Methods, 2023. [CrossRef]
- Jones, P. J., Ma, R., & McNally, R. J. Bridge Centrality: A Network Approach to Understanding Comorbidity. Multivariate Behavioral Research, 2021, 56(2), 353–367. [CrossRef]
- Costantini, G., Epskamp, S., Borsboom, D., Perugini, M., Mõttus, R., Waldorp, L. J., & Cramer, A. O. J. State of the aRt personality research: A tutorial on network analysis of personality data in R. Journal of Research in Personality, 2015, 54, 13–29. [CrossRef]
- Pons, P., & Latapy, M. Computing communities in large networks using random walks. Journal of Graph Algorithms and Applications, 2006, 10(2), 191-218.
- Tavakol, M., & Dennick, R. Making sense of Cronbach’s alpha. International Journal of Medical Education, 2011, 2, 53–55. [CrossRef]
- Jamshidian, M., & Jalal, S. Tests of Homoscedasticity, Normality, and Missing Completely at Random for Incomplete Multivariate Data. Psychometrika, 2010, 75(4), 649–674. [CrossRef]
- Bunn, F., Goodman, C., Sworn, K., Rait, G., Brayne, C., Robinson, L., McNeilly, E., & Iliffe, S. Psychosocial Factors That Shape Patient and Carer Experiences of Dementia Diagnosis and Treatment: A Systematic Review of Qualitative Studies. PLoS Medicine, 2012, 9(10), e1001331. [CrossRef]
- Marquet, M., Boutaayamou, M., Schwartz, C., Locquet, M., Bruyère, O., Croisier, J.-L., & Adam, S. Does negative information about aging influence older adults’ physical performance and subjective age? Archives of Gerontology and Geriatrics, 2018, 78, 181–189. [CrossRef]
- Weiss, D., & Lang, F. R. “They” are old but “I” feel younger: Age-group dissociation as a self-protective strategy in old age. Psychology and Aging, 2012, 27(1), 153–163. [CrossRef]
- Ruth, N., Tsigeman, E., Likhanov, M., Kovas, Y., & Müllensiefen, D. Personality and engagement with music: Results from network modeling in three adolescent samples. Psychology of Music, 2023, 51(4), 1223–1242. [CrossRef]
- Likhanov, M., Fillon, A., Demolliens, M., ROBERT, A., Darnon, C., Huguet, P., & Regner, I. Network analysis of anxiety-related traits in male and female vocational students: Identifying potential targets for educational interventions. PsyArXiv, 2025. [CrossRef]
- Hu, L., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal, 6(1), 1–55. [CrossRef]
- Chen, F. F. (2007). Sensitivity of Goodness of Fit Indexes to Lack of Measurement Invariance. Structural Equation Modeling: A Multidisciplinary Journal, 14(3), 464–504. [CrossRef]
- André, S., Maulana, R., Helms-Lorenz, M., Telli, S., Chun, S., Fernández-García, C.-M., De Jager, T., Irnidayanti, Y., Inda-Caro, M., Lee, O., Safrina, R., Coetzee, T., & Jeon, M. (2020). Student Perceptions in Measuring Teaching Behavior Across Six Countries: A Multi-Group Confirmatory Factor Analysis Approach to Measurement Invariance. Frontiers in Psychology, 11, 273. [CrossRef]
- Marsh, H. W., Hau, K.-T., & Wen, Z. (2004). In Search of Golden Rules: Comment on Hypothesis-Testing Approaches to Setting Cutoff Values for Fit Indexes and Dangers in Overgeneralizing Hu and Bentler’s (1999) Findings. Structural Equation Modeling: A Multidisciplinary Journal, 11(3), 320–341. [CrossRef]
- Steenkamp, J. E. M., & Baumgartner, H. (1998). Assessing Measurement Invariance in Cross-National Consumer Research. Journal of Consumer Research, 25(1), 78–107. [CrossRef]
| Patient group (hospital) n = 130 |
Control group (laboratory) n = 84 |
p-value | Cohen’s d | |
|---|---|---|---|---|
| Gender ratio (M/F) | 44 / 86 | 26 / 58 | .7711 | -- |
| Age (years) (±SD) | 70.96 (±8.74) | 66.44 (±8.09) | < .0012 | 0.53 |
| [Age range] | [50–87] | [50–89] | - | -- |
| SPC ratio (low/med/ high) | 44 / 49 / 37 | 21 / 30 / 33 | .2021 | -- |
| Education years (±SD) | 12.27 (±3.38) | 14.44 (±2.86) | < .0012 | 0.68 |
| MMSE scores (±SD) | 27.45 (±1.74) | 28.14 (±1.61) | .0042 | 0.41 |
| QCC scores (±SD) | 5.10 (±1.33) | 3.16 (±1.57) | < .0012 | 1.36 |
| GDS scores (±SD) | 6.19 (±2.71) | 5.65 (±3.26) | .1912 | 0.18 |
| 5-word test (±SD) | 9.95 (±0.26) | 10.00 (±0.00) | .0582 | 0.27 |
| IADL scores (±SD) | 0.00 (±0.00) | 0.00 (±0.00) | - | -- |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




