Submitted:
13 January 2026
Posted:
14 January 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Maternal Microbiome and Neonatal Health
Vaginal Microbiome and Pregnancy Health
Preterm Birth and Miscarriage
Gestational Diabetes Mellitus (GDM)
Chorioamnionitis and Premature Rupture of Membranes (PROM)
Placental Microbiome
Breast-Milk Microbiome
Neonatal Microbiome and Early-Life Outcomes
Neurodevelopmental Outcomes
Allergic and Atopic Diseases
Malnutrition
Gut Microbiome and Sepsis Risk in Neonates
Culture Negative Sepsis and Microbial Shifts
Urinary Tract Infections (UTI)
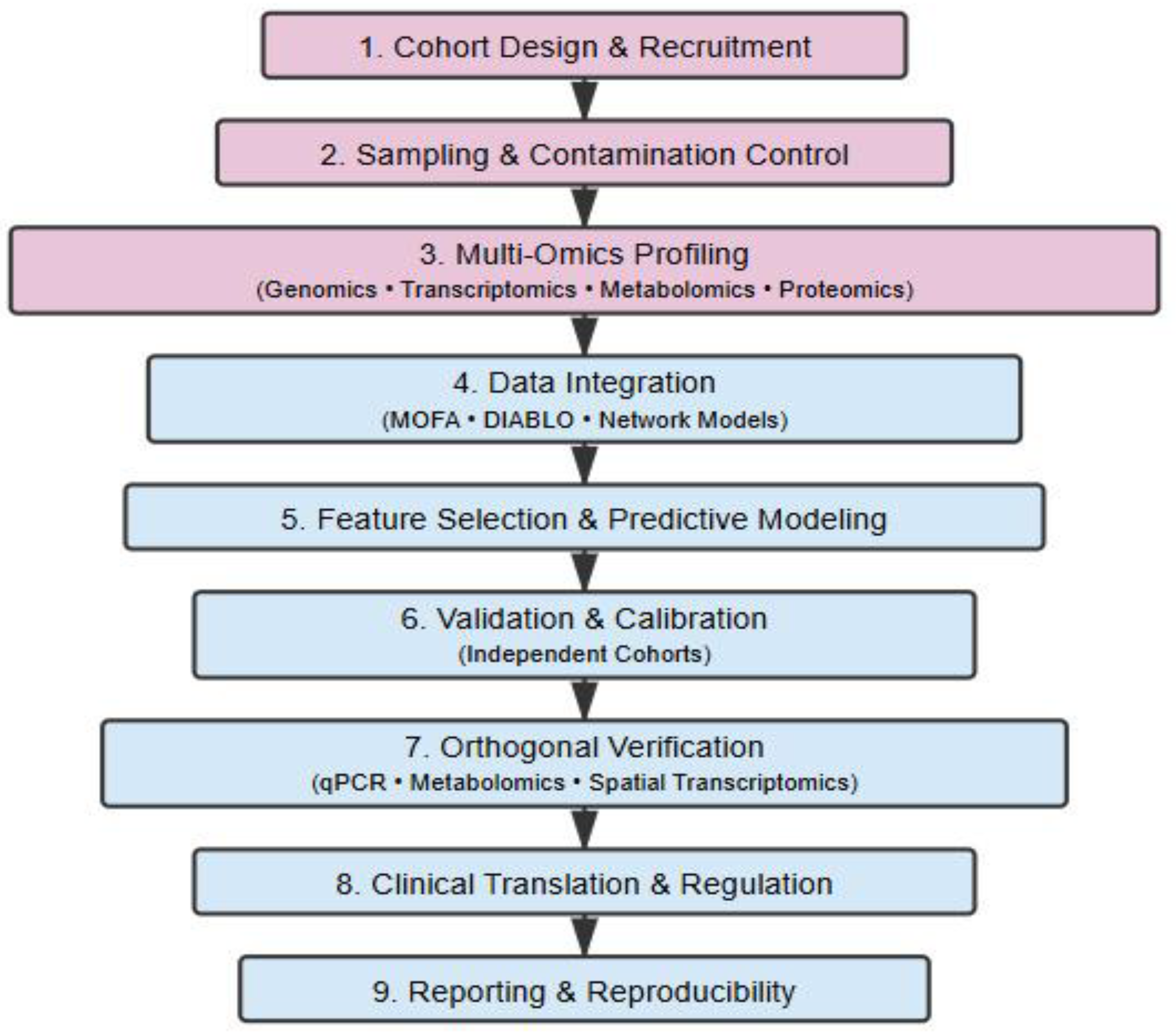
Integration of Omics for Precision Medicine
Diagnostic Pathway
Clinical Applications and Challenges
Challenges in Clinical Translation
Conclusions
Author Contributions
Funding
References
- Azad, M.B.; Konya, T.; Persaud, R.R.; Guttman, D.S.; Chari, R.S.; Field, C.J.; Sears, M.R.; Mandhane, P.J.; Turvey, S.E.; Subbarao, P.; Becker, A.B.; Scott, J.A.; Kozyrskyj, A.L. Impact of maternal intrapartum antibiotics, method of birth and breastfeeding on gut microbiota during the first year of life: a prospective cohort study. BJOG 2016, 123, 983–993. [Google Scholar] [CrossRef] [PubMed]
- Davis, E.C.; Castagna, V.P.; Sela, DA..; Hillard, M.A.; Lindberg, S.; Mantis, N.J.; Seppo, A.E.; Järvinen, K.M. Gut microbiome and breast-feeding: implications for early immune development. J Allergy Clin Immunol 2022, 150, 523–534. [Google Scholar] [CrossRef] [PubMed]
- Dominguez-Bello, M.G.; Costello, E.K.; Contreras, M.; Magris, M.; Hidalgo, G.; Fierer, N.; Knight, R. Delivery mode shapes the acquisition and structure of the initial microbiota across multiple body habitats in newborns. Proc Natl Acad Sci USA 2010, 107, 11971–11975. [Google Scholar] [CrossRef] [PubMed]
- Shao, Y.; Forster, S.C.; Tsaliki, E.; Vervier, K.; Strang, A.; Simpson, N.; Kumar, N.; Stares, M.D.; Rodger, A.; Brocklehurst, P.; Field, N.; Lawley, T.D. Stunted microbiota and opportunistic pathogen colonization in caesarean-section birth. Nature 2019, 574, 117–121. [Google Scholar] [CrossRef]
- Brooks, B.; Firek, B.A.; Miller, C.S.; Sharon, I.; Thomas, B.C.; Baker, R.; Morowitz, M.J.; Banfield, J.F. Microbes in the neonatal intensive care unit resemble those found in the gut of premature infants. Microbiome 2 2014, 1. [Google Scholar] [CrossRef]
- Aagaard, K.; Ma, J.; Antony, K. M.; Ganu, R.; Petrosino, J.; Versalovic, J. The Placenta Harbors a Unique Microbiome. HHS Public Access 2016, 6(237), 1–22. [Google Scholar] [CrossRef]
- Abdelaziz, E. H.; Ismail, R.; Mabrouk, M. S.; Amin, E. Multi-omics data integration and analysis pipeline for precision medicine: Systematic review. Computational Biology and Chemistry 2024, 113, 108254. [Google Scholar] [CrossRef]
- Acharya, D.; Mukhopadhyay, A. A comprehensive review of machine learning techniques for multi-omics data integration: Challenges and applications in precision oncology. Briefings in Functional Genomics 2024, 23(5), 549–560. [Google Scholar] [CrossRef]
- Acuña, I.; Cerdó, T.; Ruiz, A.; Torres-espínola, F. J.; López-moreno, A.; Aguilera, M.; Suárez, A.; Campoy, C. Infant gut microbiota associated with fine motor skills. Nutrients 2021, 13(5), 1–13. [Google Scholar] [CrossRef]
- Ahmed, U.; Fatima, F.; Farooq, H. A.; Ahmed, U.; Fatima, F.; Farooq, H. A. Maternal and child health DYSBIOSIS AS A GLOBAL HEALTH CHALLENGE 2025, 93(8), 1–8.
- Barrientos, G.; Ronchi, F.; Conrad, M. L. Nutrition during pregnancy: Influence on the gut microbiome and fetal development. American Journal of Reproductive Immunology 2024, 91(1), e13802. [Google Scholar] [CrossRef] [PubMed]
- Biagi, E.; Aceti, A.; Quercia, S.; Beghetti, I.; Rampelli, S.; Turroni, S.; Soverini, M.; Zambrini, A. V.; Faldella, G.; Candela, M.; Corvaglia, L.; Brigidi, P. Microbial Community Dynamics in Mother’s Milk and Infants Mouth and Gut in Moderately Preterm Infants 2018, 9(October), 1–10. [CrossRef]
- Blanton, L. V.; Charbonneau, M. R.; Salih, T.; Barratt, M. J.; Venkatesh, S.; Ilkaveya, O.; Subramanian, S.; Manary, M. J.; Trehan, I.; Jorgensen, J. M.; Fan, Y.; Henrissat, B.; Leyn, S. A.; Rodionov, D. A.; Osterman, A. L. Kenneth M. Maleta Christopher B. Newgard3, 4, 5, 6, Per Ashorn11, 16, Kathryn G. Dewey10, and Jeffrey Gordon1, 2, & 1Center Gut bacteria that rescue growth impairments transmitted by immature microbiota from undernourished children. HHS Public Access 2016, 351(6275), 1–18. [Google Scholar] [CrossRef]
- Boix-Amorós, A.; Collado, M. C.; Mira, A. Relationship between milk microbiota, bacterial load, macronutrients, and human cells during lactation. Frontiers in Microbiology 2016, 7(APR), 1–9. [Google Scholar] [CrossRef]
- Cavanagh, M.; Amabebe, E.; Kulkarni, N. S.; Papageorgiou, M. D.; Walker, H.; Wyles, M. D.; Anumba, D. O. Vaginal host immune-microbiome-metabolite interactions associated with spontaneous preterm birth in a predominantly white cohort. Npj Biofilms and Microbiomes 2025, 11(1), 1–23. [Google Scholar] [CrossRef]
- Chen, J. diao; Ke, C. W.; Deng, X.; Jiang, S.; Liang, W.; Ke, B. X.; Li, B.; Tan, H.; Liu, M. Brucellosis in Guangdong Province, people’s republic of China, 2005-2010. Emerging Infectious Diseases 2013, 19(5), 817–818. [Google Scholar] [CrossRef]
- Das, P.; Babaei, P.; Nielsen, J. Metagenomic analysis of microbe-mediated vitamin metabolism in the human gut microbiome. BMC Genomics 2019, 20(1), 208. [Google Scholar] [CrossRef]
- D’Auria, E.; Peroni, D. G.; Sartorio, M. U. A.; Verduci, E.; Zuccotti, G. V.; Venter, C. The Role of Diet Diversity and Diet Indices on Allergy Outcomes. Frontiers in Pediatrics 2020, 8(September), 1–14. [Google Scholar] [CrossRef]
- de Goffau, M. C.; Lager, S.; Sovio, U.; Gaccioli, F.; Cook, E.; Peacock, S. J.; Parkhill, J.; Charnock-Jones, D. S.; Smith, G. C. S. Author Correction: Human placenta has no microbiome but can contain potential pathogens (Nature, (2019), 572, 7769, (329-334), 10.1038/s41586-019-1451-5). Nature 2019, 574(7778), E15. [Google Scholar] [CrossRef]
- Deianova, N.; de Boer, N. K.; Aoulad Ahajan, H.; Verbeek, C.; Aarnoudse-Moens, C. S. H.; Leemhuis, A. G.; van Weissenbruch, M. M.; van Kaam, A. H.; Vijbrief, D. C.; Hulzebos, C. V.; Giezen, A.; Cossey, V.; de Boode, W. P.; de Jonge, W. J.; Benninga, M. A.; Niemarkt, H. J.; de Meij, T. G. J. Duration of Neonatal Antibiotic Exposure in Preterm Infants in Association with Health and Developmental Outcomes in Early Childhood. Antibiotics 2023, 12(6). [Google Scholar] [CrossRef]
- Dombrowska-Pali, A.; Wiktorczyk-Kapischke, N.; Chrustek, A.; Olszewska-Słonina, D.; Gospodarek-Komkowska, E.; Socha, M. W. Human Milk Microbiome-A Review of Scientific Reports. Nutrients 2024, 16(10), 1–36. [Google Scholar] [CrossRef]
- Doyle, R. M.; Harris, K.; Kamiza, S.; Harjunmaa, U.; Ashorn, U.; Nkhoma, M.; Dewey, K. G.; Maleta, K.; Ashorn, P.; Klein, N. Bacterial communities found in placental tissues are associated with severe chorioamnionitis and adverse birth outcomes; 2017; pp. 1–23. [Google Scholar]
- Duranti, S.; Lugli, G. A.; Mancabelli, L.; Armanini, F.; Turroni, F.; James, K.; Ferretti, P.; Gorfer, V.; Ferrario, C.; Milani, C.; Mangifesta, M.; Anzalone, R.; Zolfo, M.; Viappiani, A.; Pasolli, E.; Bariletti, I.; Canto, R.; Clementi, R.; Cologna, M.; Ventura, M. Maternal inheritance of bifidobacterial communities and bifidophages in infants through vertical transmission; 2017; pp. 1–13. [Google Scholar] [CrossRef]
- Enache, R.-M.; Roşu, O. A.; Profir, M.; Pavelescu, L. A.; Creţoiu, S. M.; Gaspar, B. S. Correlations Between Gut Microbiota Composition, Medical Nutrition Therapy, and Insulin Resistance in Pregnancy—A Narrative Review. International Journal of Molecular Sciences 2025, 26(3), 1372. [Google Scholar] [CrossRef]
- Erny, D.; De Angelis, A. L. H.; Jaitin, D.; Wieghofer, P.; Staszewski, O.; David, E.; Keren-Shaul, H.; Mahlakoiv, T.; Jakobshagen, K.; Buch, T.; Schwierzeck, V.; Utermöhlen, O.; Chun, E.; Garrett, W. S.; Mccoy, K. D.; Diefenbach, A.; Staeheli, P.; Stecher, B.; Amit, I.; Prinz, M. Host microbiota constantly control maturation and function of microglia in the CNS. Nature Neuroscience 2015, 18(7), 965–977. [Google Scholar] [CrossRef]
- Farhat, S.; Hemmatabadi, M.; Ejtahed, H. S.; Shirzad, N.; Larijani, B. Microbiome alterations in women with gestational diabetes mellitus and their offspring: A systematic review. Frontiers in Endocrinology 2022, 13(December), 1–14. [Google Scholar] [CrossRef] [PubMed]
- FDA. Laboratory Developed Tests (LDTs). Blueprint for Breakthroughs—Charting the Course for Precision Medicine 2018. [Google Scholar]
- Fox, R.; Kitt, J.; Leeson, P.; Aye, C. Y. L.; Lewandowski, A. J. Preeclampsia: Risk Factors, Diagnosis, Management, and the Cardiovascular Impact on the Offspring. Journal of Clinical Medicine 2020, 8(10), 1–22. [Google Scholar] [CrossRef] [PubMed]
- Gehrig, J. L.; Venkatesh, S.; Chang, H.; Hibberd, M. C.; Kung, V. L.; Cheng, J.; Chen, R. Y.; Subramanian, S.; Cowardin, C. A.; Meier, M. F.; Donnell, D. O.; Talcott, M.; Spears, L. D.; Semenkovich, C. F.; Henrissat, B.; Giannone, R. J.; Hettich, R. L.; Ilkayeva, O.; Muehlbauer, M.; Gordon, J. I. Effects of microbiota-directed foods in gnotobiotic animals and undernourished children 2019, 139. [CrossRef]
- Gerede, A.; Nikolettos, K.; Vavoulidis, E.; Margioula-Siarkou, C.; Petousis, S.; Giourga, M.; Fotinopoulos, P.; Salagianni, M.; Stavros, S.; Dinas, K.; Nikolettos, N.; Domali, E. Vaginal Microbiome and Pregnancy Complications: A Review. Journal of Clinical Medicine 2024, 13(13). [Google Scholar] [CrossRef]
- Gudnadottir, U.; Debelius, J. W.; Du, J.; Hugerth, L. W.; Danielsson, H.; Schuppe-Koistinen, I.; Fransson, E.; Brusselaers, N. The vaginal microbiome and the risk of preterm birth: A systematic review and network meta-analysis. Scientific Reports 2022, 12(1), 1–8. [Google Scholar] [CrossRef]
- Gupta, A.; Chan, S. Y.; Toh, R.; Low, J. M.; Ming, I.; Liu, Z.; Lim, S. L.; Lee, L. Y.; Swarup, S. Gestational diabetes - related gut microbiome dysbiosis is not influenced by different Asian ethnicities and dietary interventions: A pilot study. Scientific Reports 2024, 1–14. [Google Scholar] [CrossRef]
- Hanna, M.; Huang, S.; Ross, M.; Reyes, A.; Perera, D.; Surathu, A.; Javornik Cregeen, S.; Hagan, J.; Pammi, M. Microbiome Signatures and Inflammatory Biomarkers in Culture-Negative Neonatal Sepsis. Applied Microbiology 2025, 5(3), 57. [Google Scholar] [CrossRef]
- Heida, F. H.; Kooi, E. M. W.; Wagner, J.; Nguyen, T.; Hulscher, J. B. F.; Van Zoonen, A. G. J. F.; Bos, A. F.; Harmsen, H. J. M.; De Goffau, M. C. Weight shapes the intestinal microbiome in preterm infants: Results of a prospective observational study; 2021; pp. 1–12. [Google Scholar]
- Hermansson, H.; Kumar, H.; Collado, M. C.; Salminen, S.; Isolauri, E.; Rautava, S. Breast milk microbiota is shaped by mode of delivery and intrapartum antibiotic exposure. Frontiers in Nutrition 2019, 6. [Google Scholar] [CrossRef] [PubMed]
- Hoskinson, C.; Dai, D. L. Y.; Del Bel, K. L.; Becker, A. B.; Moraes, T. J.; Mandhane, P. J.; Finlay, B. B.; Simons, E.; Kozyrskyj, A. L.; Azad, M. B.; Subbarao, P.; Petersen, C.; Turvey, S. E. Delayed gut microbiota maturation in the first year of life is a hallmark of pediatric allergic disease. Nature Communications 2023, 14(1), 4785. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.; Liang, X.; Bao, H.; Ma, G.; Tang, X.; Luo, H.; Xiao, X. Multi-omics analysis reveals the associations between altered gut microbiota, metabolites, and cytokines during pregnancy. mSystems 2024, 9(3), 1–16. [Google Scholar] [CrossRef]
- Iqbal, F.; Siva, N.; Shenoy, P. A.; Lewis, L. E. S.; Purkayastha, J.; Eshwara, V. K. Gut Pathogen Colonization: A Risk Factor to Bloodstream Infections in Preterm Neonates Admitted in the Neonatal Intensive Care Unit-A Prospective Cohort Study. Neonatology 2025, 122(2), 151–160. [Google Scholar] [CrossRef]
- Jarmusch, A. K.; Vrbanac, A.; Momper, J. D.; Ma, J. D.; Alhaja, M.; Liyanage, M.; Knight, R.; Dorrestein, P. C.; Tsunoda, S. M. Enhanced Characterization of Drug Metabolism and the Influence of the Intestinal Microbiome: A Pharmacokinetic, Microbiome, and Untargeted Metabolomics Study. Clinical and Translational Science 2020, 13(5), 972–984. [Google Scholar] [CrossRef]
- Kamath, S.; Hammad Altaq, H.; Abdo, T. Management of Sepsis and Septic Shock: What Have We Learned in the Last Two Decades? Microorganisms 2023, 11(9). [Google Scholar] [CrossRef]
- Kelly, M. S.; Dahl, E. M.; Jeries, L. M.; Sysoeva, T. A.; Karstens, L. Characterization of pediatric urinary microbiome at species-level resolution indicates variation due to sex, age, and urologic history. Journal of Pediatric Urology 2024, 20(5), 884–893. [Google Scholar] [CrossRef]
- Klingenberg, C.; Kornelisse, R. F.; Buonocore, G.; Maier, R. F.; Stocker, M. Culture-Negative Early-Onset Neonatal Sepsis—At the Crossroad Between Efficient Sepsis Care and Antimicrobial Stewardship. Frontiers in Pediatrics 2018, 6, 285. [Google Scholar] [CrossRef]
- Koren, O.; Goodrich, J. K.; Cullender, T. C.; Spor, A.; Laitinen, K.; Bäckhed, H. K.; Gonzalez, A.; Werner, J. J.; Angenent, L. T.; Knight, R.; Bäckhed, F.; Isolauri, E.; Salminen, S.; Ley, R. E. During pregnancy 2013, 150(3), 470–480. [CrossRef]
- Kumar, H.; du Toit, E.; Kulkarni, A.; Aakko, J.; Linderborg, K. M.; Zhang, Y.; Nicol, M. P.; Isolauri, E.; Yang, B.; Collado, M. C.; Salminen, S. Distinct patterns in human milk microbiota and fatty acid profiles across specific geographic locations. Frontiers in Microbiology 2016, 7(OCT). [Google Scholar] [CrossRef] [PubMed]
- Kuperman, A.; Zimmerman, A.; Hamadia, S.; Ziv, O.; Gurevich, V.; Fichtman, B.; Gavert, N.; Straussman, R.; Rechnitzer, H.; Barzilay, M.; Shvalb, S.; Bornstein, J.; Ben-Shachar, I.; Yagel, S.; Haviv, I.; Koren, O. Deep microbial analysis of multiple placentas shows no evidence for a placental microbiome. BJOG 2019, 170. [Google Scholar] [CrossRef]
- Lackey, K. A.; Williams, J. E.; Meehan, C. L.; Zachek, J. A.; Benda, E. D.; Price, W. J.; Foster, J. A.; Sellen, D. W.; Kamau-Mbuthia, E. W.; Kamundia, E. W.; Mbugua, S.; Moore, S. E.; Prentice, A. M.; D. G., K; Kvist, L. J.; Otoo, G. E.; García-Carral, C.; Jiménez, E.; Ruiz, L.; McGuire, M. K. What’s normal? Microbiomes in human milk and infant feces are related to each other but vary geographically: The inspire study. Frontiers in Nutrition 2019, 6(April). [Google Scholar] [CrossRef] [PubMed]
- Lebon, A.; Labout, J. A. M.; Verbrugh, H. A.; Jaddoe, V. W. V.; Hofman, A.; van Wamel, W. J. B.; van Belkum, A.; Moll, H. A. Role of Staphylococcus aureus Nasal Colonization in Atopic Dermatitis in Infants. Arch Pediatr Adolesc Med 2009, 163(4), 745–749. [Google Scholar] [CrossRef] [PubMed]
- Levanova, L. A.; Markovskaya, A. A.; Otdushkina, Y. L.; Zakharova, Yu. V. Gut microbiota and urinary tract infections in children. Fundamental and Clinical Medicine 2021, 6(2), 24–30. [Google Scholar] [CrossRef]
- Lu, J.; Zhang, W.; He, Y.; Jiang, M.; Liu, Z.; Zhang, J.; Zheng, L.; Zhou, B.; Luo, J.; He, C.; Shan, Y.; Zhang, R.; Fan, K. L.; Fang, B.; Wan, C. Multi-omics decodes host-specific and environmental microbiome interactions in sepsis. Frontiers in Microbiology 2025, 16. [Google Scholar] [CrossRef]
- Ma, S.; Wang, Y.; Ji, X.; Dong, S.; Wang, S.; Zhang, S.; Deng, F.; Chen, J.; Lin, B.; Khan, B. A.; Liu, W.; Hou, K. Relationship between gut microbiota and the pathogenesis of gestational diabetes mellitus: A systematic review; 2024; Volume May, pp. 1–11. [Google Scholar] [CrossRef]
- Mora-Janiszewska, O.; Bialic, K.; Faryniak, A.; Darmochwał-Kolarz, D. A Review of Modulation of Gut Microbiota to Mitigate Gestational Diabetes: Implications for Maternal and Child Health. MSM 2025, 31(e948897), 1–21. [Google Scholar] [CrossRef]
- Morrow, A. L.; Lagomarcino, A. J.; Schibler, K. R.; Taft, D. H.; Yu, Z.; Wang, B.; Altaye, M.; Wagner, M.; Gevers, D.; Ward, D. V.; Kennedy, M. A.; Huttenhower, C.; Newburg, D. S. Early microbial and metabolomic signatures predict later onset of necrotizing enterocolitis in preterm infants. Microbiome 2013, 1(1), 1–16. [Google Scholar] [CrossRef]
- Nakshine, V. S.; Jogdand, S. D. A Comprehensive Review of Gestational Diabetes Mellitus: Impacts on Maternal Health, Fetal Development, Childhood Outcomes, and Long-Term Treatment Strategies. Cureus 2023, 15(10). [Google Scholar] [CrossRef]
- Neu, J.; Stewart, C. J. Neonatal microbiome in the multiomics era: Development and its impact on long-term health. Pediatric Research 2025, 1–9. [Google Scholar] [CrossRef]
- Ni, D.; Tan, J.; Macia, L.; Nanan, R. Breastfeeding is associated with enhanced intestinal gluconeogenesis in infants. BMC Medicine 2024, 22(1), 106. [Google Scholar] [CrossRef] [PubMed]
- Pannaraj, P. S.; Li, F.; Cerini, C.; Bender, J. M.; Yang, S.; Rollie, A.; Adisetiyo, H.; Zabih, S.; Lincez, P. J.; Bittinger, K.; Bailey, A.; Bushman, F. D.; Sleasman, J. W.; Aldrovandi, G. M. Association Between Breast Milk Bacterial Communities and Establishment and Development of the Infant Gut Microbiome 2019, 90095(7), 647–654. [CrossRef]
- Panzer, J. J.; Romero, R.; Greenberg, J. M.; Winters, A. D.; Galaz, J.; Gomez-Lopez, N.; Theis, K. R. Is there a placental microbiota? A critical review and re-analysis of published placental microbiota datasets. BMC Microbiology 2023, 23(1), 1–20. [Google Scholar] [CrossRef] [PubMed]
- Parrish, A.; Boudaud, M.; Grant, E. T.; Willieme, S.; Neumann, M.; Wolter, M.; Craig, S. Z.; De Sciscio, A.; Cosma, A.; Hunewald, O.; Ollert, M.; Desai, M. S. Akkermansia muciniphila exacerbates food allergy in fibre-deprived mice. Nature Microbiology 2023, 8(10), 1863–1879. [Google Scholar] [CrossRef]
- Pokharel, P.; Dhakal, S.; Dozois, C. M. The Diversity of Escherichia coli Pathotypes and Vaccination Strategies against This Versatile Bacterial Pathogen. Microorganisms 2023, 11(2). [Google Scholar] [CrossRef]
- Reasoner, S. A.; Flores, V.; Van Horn, G.; Morales, G.; Peard, L. M.; Abelson, B.; Manuel, C.; Lee, J.; Baker, B.; Williams, T.; Schmitz, J. E.; Clayton, D. B.; Hadjifrangiskou, M. Survey of the infant male urobiome and genomic analysis of Actinotignum spp. Npj Biofilms and Microbiomes 2023, 9(1). [Google Scholar] [CrossRef]
- Reyman, M.; van Houten, M. A.; Watson, R. L.; Chu, M. L. J. N.; Arp, K.; de Waal, W. J.; Schiering, I.; Plötz, F. B.; Willems, R. J. L.; van Schaik, W.; Sanders, E. A. M.; Bogaert, D. Effects of early-life antibiotics on the developing infant gut microbiome and resistome: A randomized trial. Nature Communications 2022, 13(1), 1–12. [Google Scholar] [CrossRef]
- Richards, A. L.; Muehlbauer, A. L.; Alazizi, A.; Burns, M. B.; Findley, A.; Messina, F.; Gould, T. J.; Cascardo, C.; Pique-Regi, R.; Blekhman, R.; Luca, F. Gut Microbiota Has a Widespread and Modifiable Effect on Host Gene Regulation. mSystems 2019, 4(5). [Google Scholar] [CrossRef]
- Singh, P.; Elhaj, D. A. I.; Ibrahim, I.; Abdullahi, H.; Al Khodor, S. Maternal microbiota and gestational diabetes: Impact on infant health. Journal of Translational Medicine 2023, 21(1), 1–16. [Google Scholar] [CrossRef]
- Srivastava, A.; Shete, O.; Gulia, A.; Aggarwal, S.; Ghosh, T. S.; Ahuja, V.; Anand, S. Role of Gut and Urinary Microbiome in Children with Urinary Tract Infections: A Systematic Review. Diagnostics 2025, 15(1), 1–12. [Google Scholar] [CrossRef]
- Srivastava, V.; Kumar, R. Yeast-Based Screening of Anti-Viral Molecules; 2024; pp. 1–15. [Google Scholar]
- Su, M.; Wang, Y.; Yuan, Q.; Tang, D.; Lu, Y.; Wu, X.; Xiong, W.; Li, Y.; Liu, T.; Zeng, S.; Wei, S. The impact of gestational diabetes mellitus on maternal-fetal pregnancy outcomes and fetal growth: A multicenter longitudinal cohort study. Frontiers in Pediatrics 2025, 13(May), 1–7. [Google Scholar] [CrossRef]
- Subramanian, S.; Huq, S.; Yatsunenko, T.; Haque, R.; Alam, M. A.; Benezra, A.; Destefano, J.; Meier, M. F.; Muegge, B. D.; Barratt, M. J.; Vanarendonk, L. G.; Zhang, Q.; Province, A.; Petri, W. A.; Ahmed, T.; Gordon, J. I. Persistent Gut Microbiota Immaturity in Malnourished Bangladeshi Children. HHS Public Access 2014, 510(7505), 417–421. [Google Scholar] [CrossRef] [PubMed]
- Sweeney, E. L.; Kallapur, S. G.; Gisslen, T.; Lambers, D. S.; Chougnet, C. A.; Stephenson, S.; Jobe, A. H.; Knox, C. L. Placental Infection With Ureaplasma species Is Associated With Histologic Chorioamnionitis and Adverse Outcomes in Moderately Preterm and Late-Preterm Infants. 213 2016. [Google Scholar] [CrossRef]
- Tian, Z.; Zhang, X.; Yao, G.; Jin, J.; Zhang, T.; Sun, C.; Wang, Z.; Zhang, Q. Intestinal flora and pregnancy complications: Current insights and future prospects. iMeta 2024, 3(2), 1–39. [Google Scholar] [CrossRef] [PubMed]
- Tun, H. M.; Peng, Y.; Chen, B.; Konya, T. B.; Morales-Lizcano, N. P.; Chari, R.; Field, C. J.; Guttman, D. S.; Becker, A. B.; Mandhane, P. J.; Moraes, T. J.; Sears, M. R.; Turvey, S. E.; Subbarao, P.; Simons, E.; Scott, J. A.; Kozyrskyj, A. L. Ethnicity Associations With Food Sensitization Are Mediated by Gut Microbiota Development in the First Year of Life. Gastroenterology 2021, 161(1), 94–106. [Google Scholar] [CrossRef]
- Turjeman, S.; Collado, M. C.; Koren, O. ScienceDirect The gut microbiome in pregnancy and pregnancy complications. Current Opinion in Endocrine and Metabolic Research 2021, 18, 133–138. [Google Scholar] [CrossRef]
- Uchil, R. R.; Kohli, Gur. sinGh; KateKhaye, V. M.; SwaMi, onKaR c. Strategies to Combat Antimicrobial Resistance. Journal of Clinical and Diagnostic Research 2014, 8(7), 8–11. [Google Scholar] [CrossRef]
- Vonaesch, P.; Morien, E.; Andrianonimiadana, L.; Sanke, H.; Mbecko, J. R.; Huus, K. E.; Naharimanananirina, T.; Gondje, B. P.; Nigatoloum, S. N.; Vondo, S. S.; Kaleb Kandou, J. E.; Randremanana, R.; Rakotondrainipiana, M.; Mazel, F.; Djorie, S. G.; Gody, J. C.; Finlay, B. B.; Rubbo, P. A.; Parfrey, L. W.; Sansonetti, P. J. Stunted childhood growth is associated with decompartmentalization of the gastrointestinal tract and overgrowth of oropharyngeal taxa. Proceedings of the National Academy of Sciences of the United States of America 2018, 115(36), E8489–E8498. [Google Scholar] [CrossRef]
- Yao, W.; Wen, R.; Huang, Z.; Huang, X.; Chen, K.; Hu, Y.; Li, Q.; Zhu, W.; Ou, D.; Bai, H. Gut microbiota composition in early pregnancy as a diagnostic tool for gestational diabetes mellitus. Microbiology Spectrum 2025, 13(8), 1–14. [Google Scholar] [CrossRef]
| Condition | Microbiome Site | Pathogenic Taxa (↑) | Protective / Depleted Taxa (↓) | Proposed Biomarker / Mechanism |
|---|---|---|---|---|
| Preterm Birth (PTB) | Vaginal | Lactobacillus iners, Gardnerella, Atopobium, Prevotella | L. crispatus | Dysbiosis → inflammation → premature labor |
| Miscarriage | Vaginal | Gardnerella, Prevotella, Atopobium | Lactobacillus spp. | Loss of protective flora → immune activation |
| Gestational Diabetes (GDM) | Gut | Escherichia–Shigella, Klebsiella | Bifidobacterium, Faecalibacterium | Carbohydrate metabolism shift → insulin resistance |
| Preeclampsia | Gut/Placenta | Clostridium, Desulfovibrio | Bacteroides, Lactobacillus | Endotoxin-driven endothelial dysfunction |
| Neonatal Sepsis | Gut | Escherichia/Shigella, Streptococcus, Enterococcus | Akkermansia, Bacteroides | Pathogenic overgrowth → bloodstream infection |
| Allergy/Atopy | Neonatal Gut | Staphylococcus aureus, Enterobacteriaceae | Bifidobacterium breve, B. longum | Reduced SCFA → Th2 bias |
| Malnutrition / Stunting | Neonatal Gut | Enterobacteriaceae | Faecalibacterium, Roseburia | Inflammation & immature microbiota |
| NEC Risk | Breast Milk / Neonatal Gut | Low Bifidobacterium, high Staphylococcus | High Bifidobacterium | Predictive milk ratio for NEC |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




