Submitted:
09 January 2026
Posted:
12 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Design of the Review and Conceptual Framework Development
2.2. Literature Search Strategy and Scope
2.3. Analytical Framework and Criteria for Synthesis
2.4. Development of the Regulatory Control State (RCS) Construct
2.5. Ethical Considerations and Scope of Application
3. Results: Conceptual Framework of the MAC/MAB–RCS Model
3.1. Identification of a Core Regulatory Dimension in Addiction
3.2. Regulatory Control State (RCS) as a Functional Clinical Construct
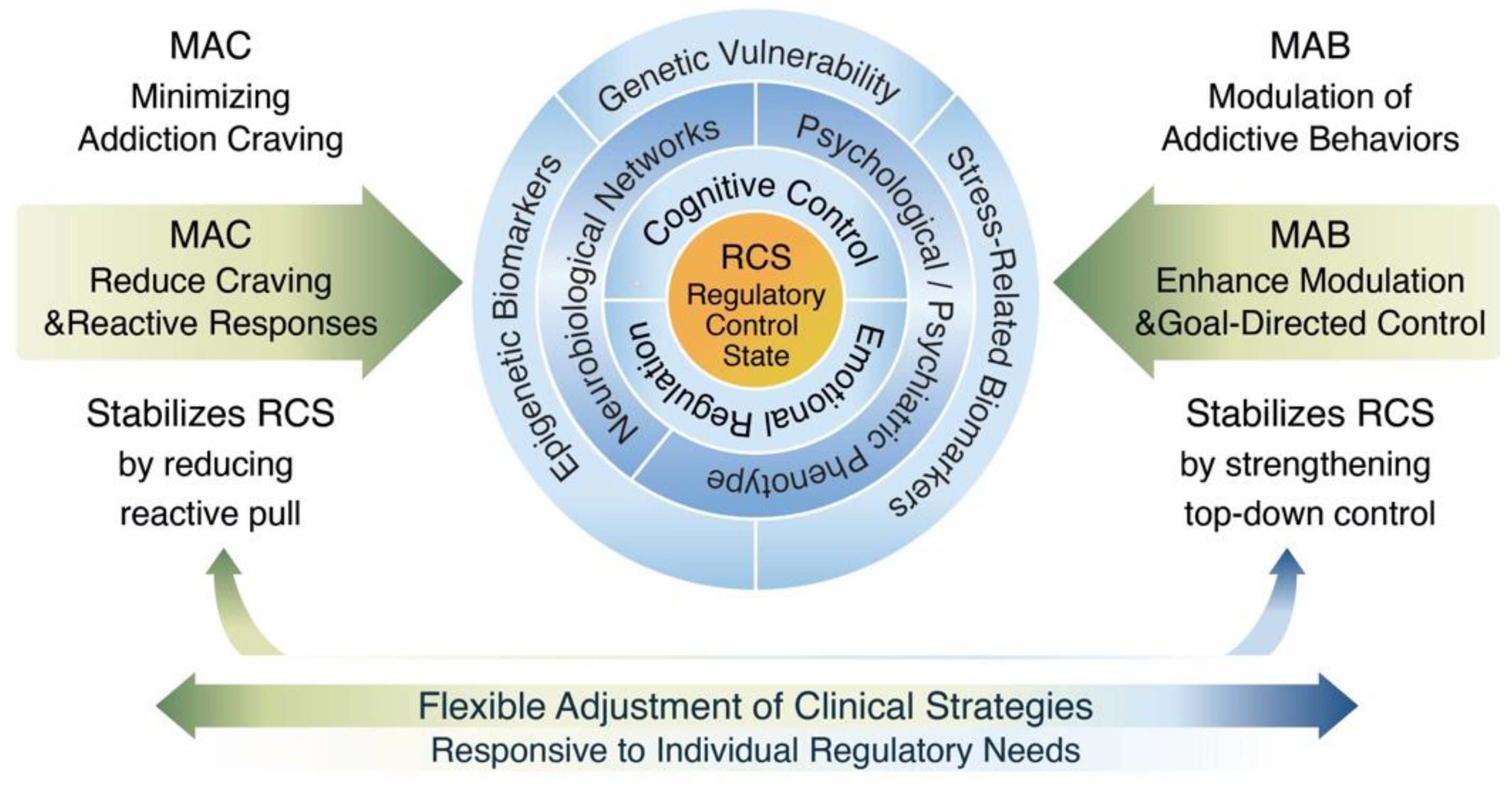
3.3. Structure of the MAC/MAB–RCS Model
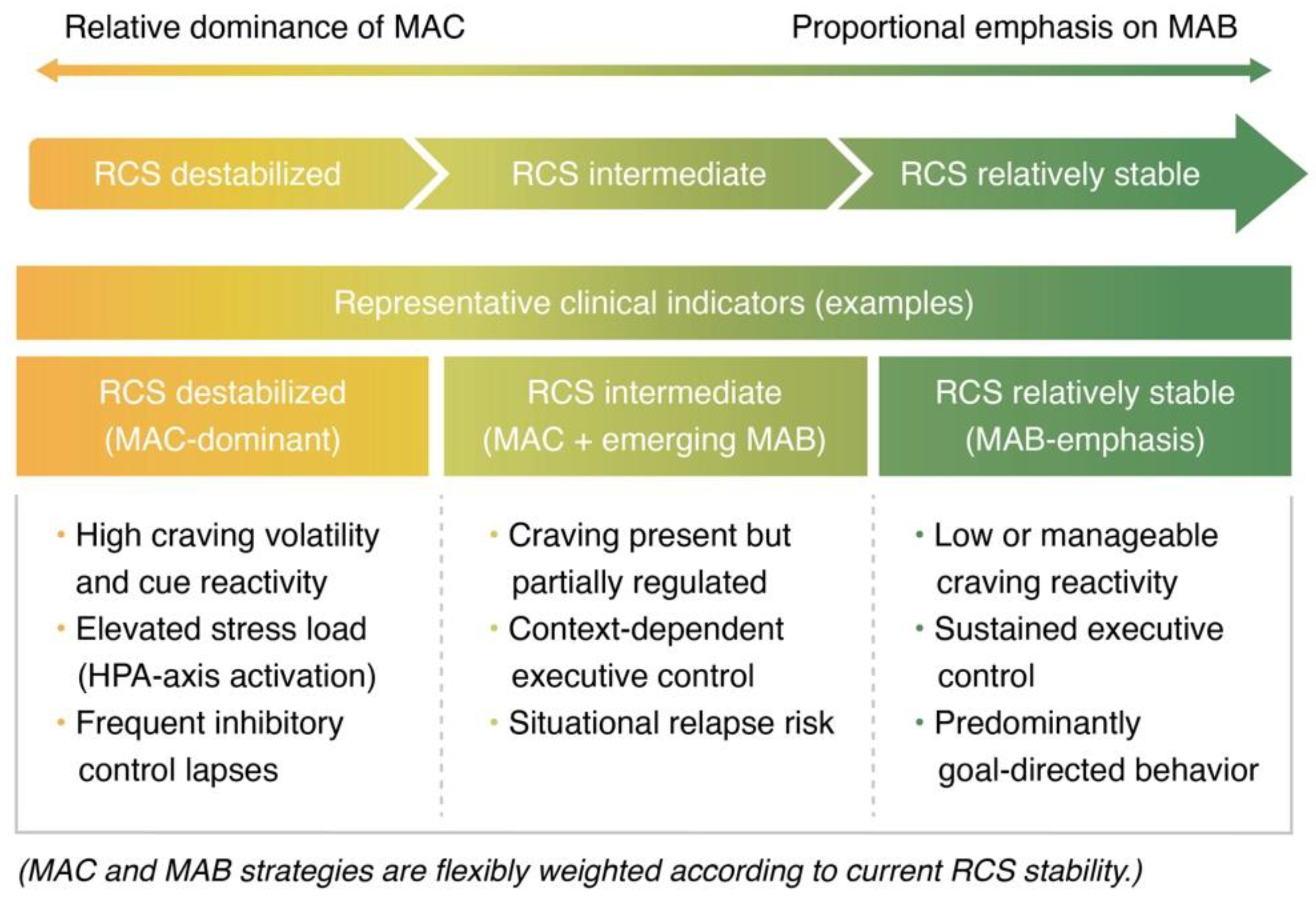
3.4. Dynamic Interpretation of Risk Within the MAC/MAB–RCS Framework
3.5. Positioning the Model Within Precision Psychiatry
4. Multidomain Structure of the MAC/MAB–RCS Framework
4.1. Rationale for a Multidomain Approach
4.2. Genetic Domain: Regulatory Vulnerability Stratification
4.3. Epigenetic and Stress-Related Biomarkers Domain
4.4. Psychological Phenotype Domain: Clinical Expression of RCS
4.5. Neurobiological Network Domain
4.6. Integration Across Domains: From Data to Clinical Interpretation
5. Discussion
5.1. Bridging Neurobiological Knowledge and Clinical Decision-Making in Addiction Psychiatry
5.2. Regulatory Control State as a Functional Clinical Construct
5.3. Clinical Implications: From Reactive Treatment to Risk Trajectory Management
5.4. System-Level Implications and Compatibility with Stepped Care Models
5.5. Limitations and Responsible Interpretation of the Framework
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Blithikioti, C.; Fried, E.I.; Albanese, E.; Field, M.; Cristea, I.A. Reevaluating the brain disease model of addiction. Lancet Psychiatry 2025, 12, 469–474. [Google Scholar] [CrossRef]
- Ferrer-Pérez, C.; Montagud-Romero, S.; Blanco-Gandía, M.C. Neurobiological theories of addiction: A comprehensive review. Psychoactives 2024, 3, 35–47. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; Text Revision (DSM-5-TR); APA Publishing: Washington, DC, USA, 2022. [Google Scholar]
- World Health Organization. International Classification of Diseases, 11th Revision (ICD-11); WHO: Geneva, Switzerland, 2022. [Google Scholar]
- Volkow, N.D.; Blanco, C. Substance use disorders: A comprehensive update of classification, epidemiology, neurobiology, clinical aspects, treatment and prevention. World Psychiatry 2023, 22, 203–229. [Google Scholar] [CrossRef]
- Karvelis, P.; Paulus, M.P.; Diaconescu, A.O. Individual differences in computational psychiatry: A review of current challenges. Neurosci. Biobehav. Rev. 2023, 152, 105137. [Google Scholar] [CrossRef] [PubMed]
- Lim, T.V.; Ersche, K.D. Theory-driven computational models of drug addiction. Addiction Neuroscience 2023, 5, 100066. [Google Scholar] [CrossRef]
- González-Roz, A.; Castaño, Y.; Krotter, A.; Salazar-Cedillo, A.; Gervilla, E. Emotional dysregulation in relation to substance use and addictive behaviors: Findings from five separate meta-analyses. Int. J. Clin. Health Psychol. 2024, 24, 100502. [Google Scholar] [CrossRef]
- Tabugan, D.C.; Bredicean, A.C.; Anghel, T.; Dumache, R.; Muresan, C.; Corsaro, L.; Hogea, L. Novel insights into addiction management: A meta-analysis on intervention for relapse prevention. Medicina 2025, 61, 619. [Google Scholar] [CrossRef] [PubMed]
- Drossel, G.; Brucar, L.R.; Rawls, E.; Hendrickson, T.J.; Zilverstand, A. Subtypes in addiction and their neurobehavioral profiles across three functional domains. Psychiatry 2023, 13, 127. [Google Scholar] [CrossRef] [PubMed]
- Hand, L.J.; Paterson, L.M.; Lingford-Hughes, A.R. Re-evaluating our focus in addiction: Emotional dysregulation is a critical driver of relapse to drug use. Transl. Psychiatry 2024, 14, 467. [Google Scholar] [CrossRef]
- Zhang, X.; Zhang, H.; Shao, Y.; Li, Y.; Zhang, F.; Zhang, H. Common neural patterns of substance use disorder: A seed-based resting-state functional connectivity meta-analysis. Psychiatry 2025, 15, 190. [Google Scholar] [CrossRef]
- Lin, E.R.H.; Potenza, M.N.; Leeman, R.F.; Yip, S.W.; Grilo, C.M. The limbic system in co-occurring substance use and anxiety disorders: Shared neurobiology and transdiagnostic dimensional frameworks. Brain Sci. 2024, 14, 1285. [Google Scholar] [CrossRef]
- Hofmann, W. Going beyond the individual level in self-control research. Nat. Rev. Psychol. 2024, 3, 56–66. [Google Scholar] [CrossRef]
- Rolls, E.T. Emotion, motivation, reasoning, and how their brain systems are related. Brain Sci. 2025, 15, 507. [Google Scholar] [CrossRef]
- Sinha, R. Stress and substance use disorders: Risk, relapse, and neuroadaptive disruptions. J. Clin. Investig. 2024, 134, e172883. [Google Scholar] [CrossRef] [PubMed]
- Baillet, E.; Auriacombe, M.; Romao, C.; Garnier, H.; Gauld, C.; Vacher, C.; Swendsen, J.; Fatseas, M.; Serre, F. Craving changes in first 14 days of addiction treatment: An outcome predictor of 5-year substance use status. Transl. Psychiatry 2024, 14, 497. [Google Scholar] [CrossRef]
- Zaiser, J.; Hoffmann, S.; Zimmermann, S.; Gessner, T.; Deck, M.; Bekier, N.K.; Abel, M.; Radler, P.; Langejürgen, J.; Lenz, B.; et al. Individual stress reactivity predicts alcohol craving and alcohol consumption in alcohol use disorder in experimental and real-life settings. Psychiatry 2025, 15, 226. [Google Scholar] [CrossRef]
- Ulisse, K.; Albitar, J.; Aromin, J.T.; Berry, J. Emerging interventions in behavioral addictions: Psychedelic and neuromodulation strategies targeting executive control and regulation networks. Brain Sci. 2025, 15, 980. [Google Scholar] [CrossRef] [PubMed]
- Witkiewitz, K.; Tucker, J.A. Whole person recovery from substance use disorder: A call for research examining a dynamic behavioral ecological model of contexts supportive of recovery. Addict. Res. Theory 2024, 32, 1–12. [Google Scholar] [CrossRef]
- Del Palacio-Gonzalez, A.; Thylstrup, B.; Rømer Thomsen, K. Psychological factors predicting patients’ risk of relapse after enrollment in drug use treatment: A systematic review. J. Subst. Use Addict. Treat. 2024, 161, 209354. [Google Scholar] [CrossRef] [PubMed]
- Guerrin, C.G.J.; Tesselaar, D.R.M.; Booij, J.; Schellekens, A.F.A.; Homberg, J.R. Precision medicine in substance use disorders: Integrating behavioral, environmental, and biological insights. Neurosci. Biobehav. Rev. 2025, 176, 106311. [Google Scholar] [CrossRef]
- Kendler, K.S.; Ohlsson, H.; Sundquist, J.; Sundquist, K. The number of episodes of major psychiatric and substance use disorders as an index of genetic risk and genetic heterogeneity. Mol. Psychiatry 2025, 30, 968–975. [Google Scholar] [CrossRef]
- Nikolova, Y.S.; Ruocco, A.C.; Felsky, D.; Lange, S.; Prevot, T.D.; Vieira, E.; Voineskos, D.; Wardell, J.D.; Blumberger, D.M.; Clifford, K.; et al. Cognitive dysfunction in the addictions (CDiA): Protocol for a neuron-to-neighbourhood collaborative research program. Front. Psychiatry 2025, 16, 1455968. [Google Scholar] [CrossRef]
- Borrego-Ruiz, A.; Borrego, J.J. Addiction susceptibility: Genetic factors, personality traits, and epigenetic interactions with the gut microbiome. Genes 2025, 16, 1447. [Google Scholar] [CrossRef]
- Gerring, Z.F.; Thorp, J.G.; Treur, J.L.; Verweij, K.J.H.; Derks, E.M. The genetic landscape of substance use disorders: Insights from genome-wide studies. Mol. Psychiatry 2024, 29, 1234–1248. [Google Scholar] [CrossRef]
- Margolis, M.P.; Tang, M.; Gagliardi, M.; Wen, C.; Wu, Y.; Wray, N.R.; Ziller, M.J.; Gandal, M.J. From variants to mechanisms: Neurogenomics in the post-GWAS era. Neuron 2025, 113, 3509–3530. [Google Scholar] [CrossRef]
- Hayes, R.M.; Mason, C.E.; Miller, J.J. The clinical use of epigenetics in psychiatry: A narrative review of epigenetic mechanisms, key candidate genes, and precision psychiatry. Front. Psychiatry 2025, 16, 1671122. [Google Scholar] [CrossRef]
- Liu, S.X.; Harris, A.C.; Gewirtz, J.C. How life events may confer vulnerability to addiction: The role of epigenetics. Front. Mol. Neurosci. 2024, 17, 1462769. [Google Scholar] [CrossRef]
- Oka, T.; Sasaki, A.; Kobayashi, N. A transdiagnostic dimensional approach to behavioral dysregulation: Examining self-reported reward and punishment sensitivity across psychopathology. J. Affect. Disord. 2025, 387, 119493. [Google Scholar] [CrossRef] [PubMed]
- Zhong, G.; Chen, T.; Zhong, N.; Rezapour, T.; Haghparast, A.; Jiang, H.; Su, H.; Yuan, T.; Robbins, T.W.; Du, J.; et al. Transdiagnostic neuromodulation of impulsivity: Current status and future trajectories. Transl. Psychiatry 2025, 15, 209. [Google Scholar] [CrossRef] [PubMed]
- Peng, Z.; Jia, Q.; Mao, J.; Luo, X.; Huang, A.; Zheng, H.; Jiang, S.; Ma, Q.; Ma, C.; Yi, Q. Neurotransmitters crosstalk and regulation in the reward circuit of subjects with behavioral addiction. Front. Psychiatry 2024, 15, 1439727. [Google Scholar] [CrossRef] [PubMed]
- Regier, P.S.; Hager, N.M.; Gawrysiak, M.; Ehmann, S.; Ayaz, H.; Childress, A.R.; Fan, Y. Differential large-scale network functional connectivity in cocaine-use disorder associates with drug-use outcomes. Sci. Rep. 2025, 15, 9636. [Google Scholar] [CrossRef]
- Li, X.; Kass, G.; Wiers, C.E.; Shi, Z. The brain salience network at the intersection of pain and substance use disorders: Insights from functional neuroimaging research. Curr. Addict. Rep. 2024, 11, 797–808. [Google Scholar] [CrossRef]
- Kurtin, D.L.; Prabhu, A.M.; Hassan, Q.; Groen, A.; Amer, M.J.; Lingford-Hughes, A.; Paterson, L.M. Differences in fMRI-based connectivity during abstinence or interventions between heroin-dependent individuals and healthy controls. Neurosci. Biobehav. Rev. 2025, 172, 106116. [Google Scholar] [CrossRef] [PubMed]
- Huang, K.; Shu, N. AI-powered integration of multimodal neuroimaging for precision psychiatry: Methods, challenges, and clinical opportunities. Cell Rep. Med. 2025, 6, 102132. [Google Scholar] [CrossRef] [PubMed]
- Kas, M.J.H.; Penninx, B.W.J.H.; Knudsen, G.M.; Cuthbert, B.; Falkai, P.; Sachs, G.S.; Ressler, K.J.; Bałkowiec-Iskra, E.; Butlen-Ducuing, F.; Leboyer, M.; et al. Precision psychiatry roadmap: Towards a biology-informed framework for mental disorders. Mol. Psychiatry 2025, 30, 3846–3855. [Google Scholar] [CrossRef] [PubMed]
- Kwako, L.E.; Momenan, R.; Litten, R.Z.; Koob, G.F.; Goldman, D. Addictions Neuroclinical Assessment: A Neuroscience-Based Framework for Addictive Disorders. Biol. Psychiatry 2016, 80, 179–189. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



