Submitted:
24 December 2025
Posted:
25 December 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
1.1. The ME/CFS Enigma
1.2. The ACE Connection
1.3. Preliminary Pharmacological Observations
1.4. Scope and Structure
2. Neurobiological Foundations
2.1. The Locus Coeruleus: Anatomy and Function
2.2. The CRF-LC Stress Axis
2.3. ACEs: Programming the Stress System
2.4. Transgenerational Epigenetic Transmission: The ‘ACE-Negative’ Paradox
2.5. LC Vulnerability to Chronic Stress
2.6. The Glymphatic Connection
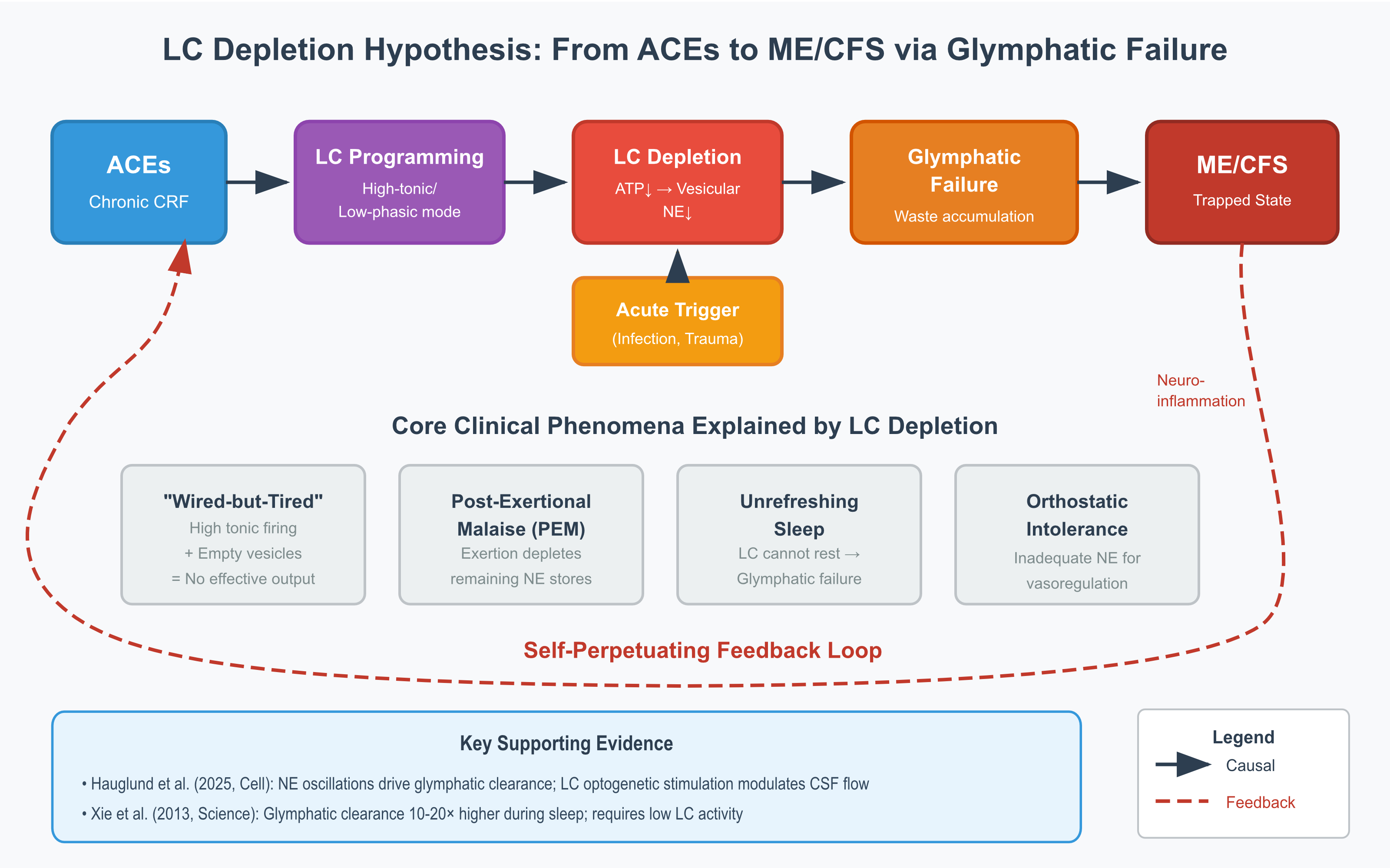
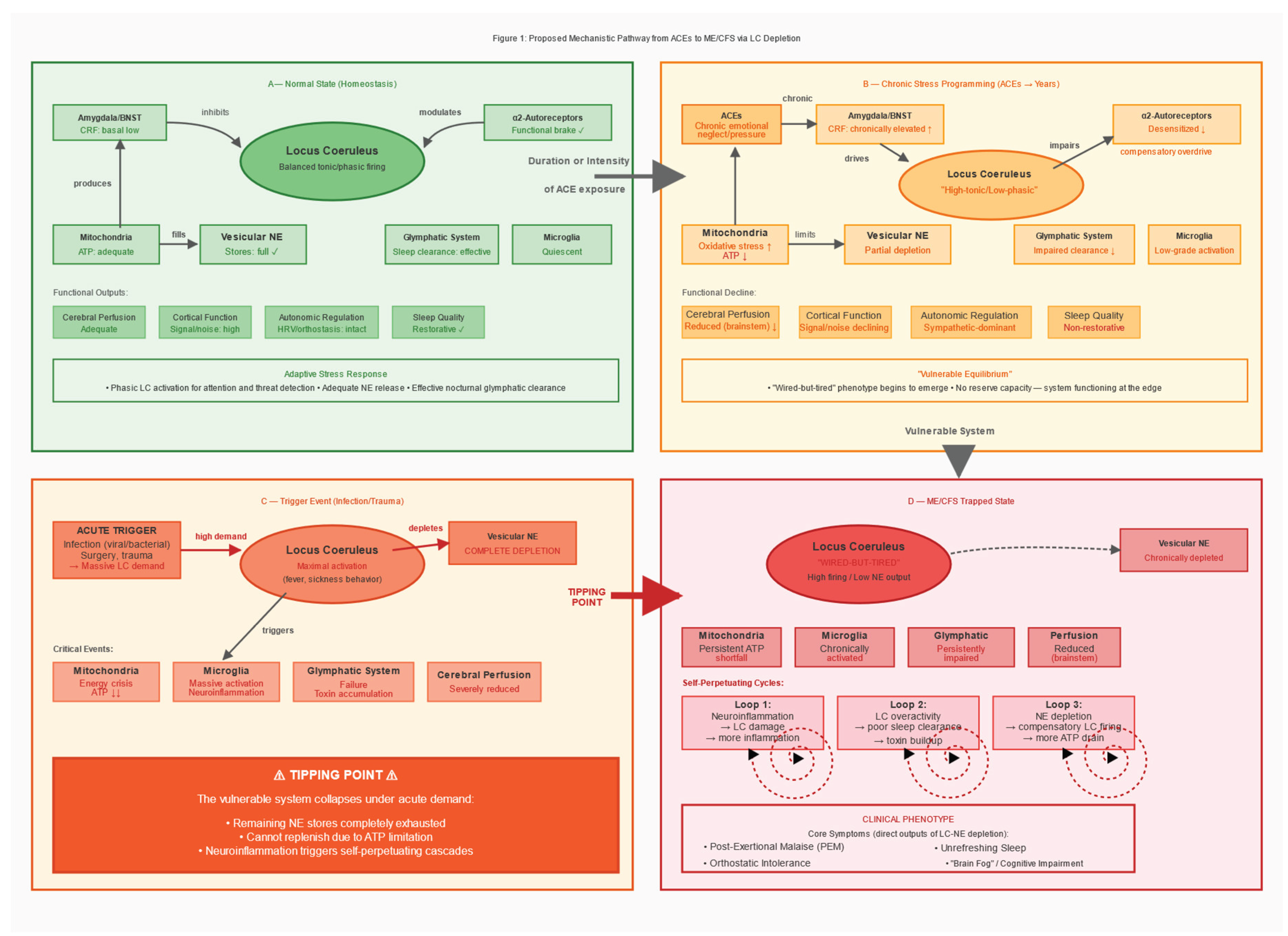
3. The Proposed Mechanism
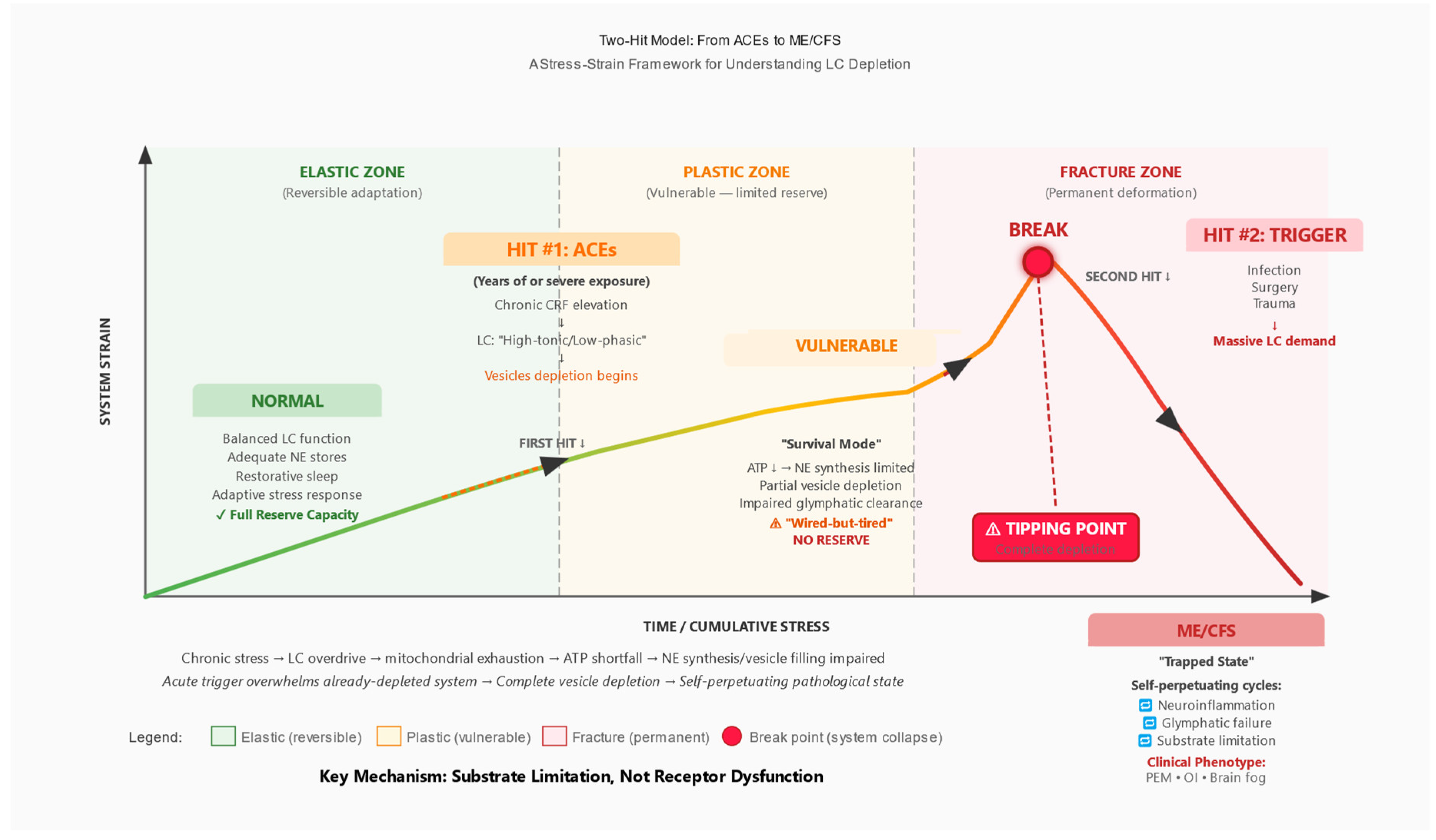
3.1. Multi-Stage Model
3.2. Differentiation from Existing Two-Hit Models
4. Clinical Phenomena Through the LC Depletion Lens
4.1. The ‘Wired-but-Tired’ Paradox
4.2. Post-Exertional Malaise
4.3. Orthostatic Intolerance
4.4. Unrefreshing Sleep
5. Supporting Evidence and Alternative Explanations
5.1. Evidence Supporting the Hypothesis
5.2. Alternative and Complementary Mechanisms
5.3. Limitations and Uncertainties
6. Testable Predictions and Research Agenda
6.1. Neuromelanin-Sensitive MRI of the LC
6.2. NET-PET Imaging
6.3. CSF Metabolite Profiling
6.4. Physiological Measures (HRV, Pupillometry)
6.5. Pharmacological Differentiation (N-of-1 Trials)
6.6. Transcutaneous Auricular Vagus Nerve Stimulation (taVNS): A Therapeutic Window to the LC-NE System
6.6.1. Pupillary Responses as LC Activity Proxy
6.6.2. Orthostatic Intolerance: Direct Evidence from POTS
6.6.3. Cognitive Function and Brain Fog
6.6.4. Stimulation Laterality: Unilateral vs. Bilateral
6.6.5. Proposed Study Design for ME/CFS
6.7. Prospective ACE-ME/CFS Cohort
7. Potential Disconfirming Evidence
8. Discussion
8.1. Strengths
8.2. Weaknesses
8.3. Implications if Hypothesis Is Correct
9. Conclusion
Funding
Ethics
Acknowledgments
Data Availability
Conflicts of Interest
Abbreviations
References
- Amann, Rupert P. 2008. “The Cycle of the Seminiferous Epithelium in Humans: A Need to Revisit?” Journal of Andrology 29 (5): 469-487. [CrossRef]
- Aston-Jones, Gary, and Jonathan D. Cohen. 2005. “An Integrative Theory of Locus Coeru-leus-Norepinephrine Function: Adaptive Gain and Optimal Performance.” Annual Review of Neuroscience 28: 403-450.
- Badran, Bashar W., Lowell T. Dowdle, Oliver J. Mithoefer, Nathan T. LaBate, Jeff Coatsworth, Jared C. Brown, William H. DeVries, Chris W. Austelle, Lisa M. McTea-gue, and Mark S. George. 2018. “Neurophysiologic Effects of Transcutaneous Auricular Vagus Nerve Stimulation (taVNS) via Electrical Stimulation of the Tragus: A Concur-rent taVNS/fMRI Study and Review.” Brain Stimulation 11 (3): 492-500. [CrossRef]
- Baig, Sheharyar S., Marharyta Kamarova, Ali Ali, Li Su, Jesse Dawson, Jessica N. Red-grave, and Arshad Majid. 2022. “Transcutaneous Vagus Nerve Stimulation (tVNS) in Stroke: The Evidence, Challenges and Future Directions.” Autonomic Neuroscience 237: 102909. [CrossRef]
- Bangasser, Debra A., and Rita J. Valentino. 2020. “The Locus Coeruleus-Norepinephrine System in Stress and Arousal: Unraveling Historical, Current, and Future Perspectives.” Frontiers in Psychiatry 11: 601519.
- Baumeister, David, Rabia Akhtar, Simona Ciufolini, Carmine M. Pariante, and Valeria Mondelli. 2016. “Childhood Trauma and Adulthood Inflammation: A Meta-Analysis.” Molecular Psychiatry 21 (5): 642-649.
- Betts, Matthew J., Evgeniya Kirilina, Maria C.G. Otaduy, et al. 2019. “Locus Coeruleus Imaging as a Biomarker for Noradrenergic Dysfunction in Neurodegenerative Diseases.” Brain 142 (9): 2558-2571.
- Blockmans, Daniel, Peter Persoons, Boudewijn Van Houdenhove, and Hugo Bobbaers. 2006. “Does Methylphenidate Reduce the Symptoms of Chronic Fatigue Syndrome?” The American Journal of Medicine 119 (12): 1047-1053.
- Borges, Uirassu, Leonie Knops, Sylvain Laborde, Stefanie Klatt, and Markus Raab. 2020. “Transcutaneous Vagus Nerve Stimulation May Enhance Only Specific Aspects of the Core Executive Functions. A Randomized Crossover Trial.” Frontiers in Neuro-science 14: 523. [CrossRef]
- Bremner, J. Douglas, Matthew T. Wittbrodt, and Nil Z. Gurel. 2024. “Transcutaneous Auri-cular Vagus Nerve Stimulation for Treating Emotional Dysregulation and Inflammation in Common Neuropsychiatric Disorders.” Brain Sciences 16 (1): 8. [CrossRef]
- Bunea, Ioana M., Aurora Szentagotai-Tatar, and Andrei C. Miu. 2017. “Early-Life Adversi-ty and Cortisol Response to Social Stress: A Meta-Analysis.” Translational Psychiatry 7 (12): 1274.
- Burger, Andreas M., Mathijs D’Agostini, Bart Verkuil, and Ilse Van Diest. 2020. “Moving Beyond Belief: A Narrative Review of Potential Biomarkers for Transcutaneous Vagus Ner-ve Stimulation.” Psychophysiology 57 (6): e13571. [CrossRef]
- Burkusis, Michal, Vladislav Plaks, Adi Michael, et al. 2015. “Environment and the Develo-ping Embryo.” In Principles of Developmental Genetics, 2nd ed., 143-154. Academic Press.
- D’Agostini, Mathijs, Cristina Ottaviani, Steven Verbeke, et al. 2022. “Transcutaneous Auri-cular Vagus Nerve Stimulation Cannot Modulate the P3b Event-Related Potential in Healthy Volunteers.” Clinical Neurophysiology 135: 22-29. [CrossRef]
- Da Silva, Joao P., et al. 2025. “Delineating Clinical Phenotypes and HPA-Axis Dysfunction in ME/CFS.” Presented at IACFS/ME 2025 Conference [conference abstract--not peer-reviewed].
- Dias, Brian G., and Kerry J. Ressler. 2014. “Parental Olfactory Experience Influences Beha-vior and Neural Structure in Subsequent Generations.” Nature Neuroscience 17 (1): 89-96. [CrossRef]
- Diedrich, André, Vasile Urechie, Dana Shiffer, Stefano Rigo, Maura Minonzio, Beatri-ce Cairo, Emily C. Smith, Luis E. Okamoto, Franca Barbic, Alessandro Bisoglio, Al-berto Porta, Italo Biaggioni, and Raffaello Furlan. 2021. “Transdermal Auricular Vagus Stimulation for the Treatment of Postural Tachycardia Syndrome.” Autonomic Neuro-science 236: 102886. [CrossRef]
- Edwards, Robert H. 2007. “The Neurotransmitter Cycle and Quantal Size.” Neuron 55 (6): 835-849.
- Eiden, Lee E., and Eberhard Weihe. 2011. “VMAT2: A Dynamic Regulator of Brain Mono-aminergic Neuronal Function Interacting with Drugs of Abuse.” Annals of the New York Academy of Sciences 1216: 86-98.
- Fang, Jiliang, Natalia Egorova, Peijing Rong, Jian Liu, Yue Hong, Yufeng Fan, Xian Wang, Hong Wang, Yazhuo Yu, Yuanpin Ma, Cong Xu, Shaoyuan Li, Jiping Zhao, Ming Luo, Bing Zhu, and Jian Kong. 2017. “Early Cortical Biomarkers of Longitudinal Transcutaneous Vagus Nerve Stimulation Treatment Success in Depression.” Neu-roImage: Clinical 14: 105-111. [CrossRef]
- Farmer, Adam D., Andreas Strzelczyk, Martina Finisguerra, et al. 2021. “International Con-sensus Based Review and Recommendations for Minimum Reporting Standards in Research on Transcutaneous Vagus Nerve Stimulation (Version 2020).” Frontiers in Human Neuro-science 14: 568051. [CrossRef]
- Felitti, Vincent J., Robert F. Anda, Dale Nordenberg, et al. 1998. “Relationship of Childhood Abuse and Household Dysfunction to Many of the Leading Causes of Death in Adults.” American Journal of Preventive Medicine 14 (4): 245-258.
- Frangos, Eleni, Jens Ellrich, and Barry R. Komisaruk. 2015. “Non-Invasive Access to the Vagus Nerve Central Projections via Electrical Stimulation of the External Ear: fMRI Evi-dence in Humans.” Brain Stimulation 8 (3): 624-636. [CrossRef]
- Goldstein, David S., and Dejene Aregawi. 2025. “Low Brain Norepinephrine in ME/CFS.” Presented at IACFS/ME 2025 Conference [conference abstract--not peer-reviewed].
- Hauglund, Natalie L., Mie Andersen, Kamilla Tokarska, et al. 2025. “Norepinephrine-Mediated Slow Vasomotion Drives Glymphatic Clearance During Sleep.” Cell 188 (3): 606-622. [CrossRef]
- Hendrix, Jolien, et al. 2025. “Sympathetic Dysfunction in ME/CFS: A Meta-Analysis.” Presented at IACFS/ME 2025 Conference [conference abstract--not peer-reviewed].
- Jacobs, Heidi I. L., Joost M. Riphagen, Carinne M. Razat, Sebastian Wiese, and Ale-xander T. Sack. 2015. “Transcutaneous Vagus Nerve Stimulation Boosts Associative Memory in Older Individuals.” Neurobiology of Aging 36 (5): 1860-1867. [CrossRef]
- Joshi, Siddhartha, Yin Li, Rishi M. Kalwani, and Joshua I. Gold. 2016. “Relationships Between Pupil Diameter and Neuronal Activity in the Locus Coeruleus, Colliculi, and Cin-gulate Cortex.” Neuron 89 (1): 221-234.
- Joshi, Siddhartha, and Joshua I. Gold. 2020. “Pupil Size as a Window on Neural Sub-strates of Cognition.” Trends in Cognitive Sciences 24 (6): 466-480. [CrossRef]
- Kempke, Stefan, Patrick Luyten, Steven Claes, et al. 2013. “Self-Critical Perfectionism and Fatigue and Pain in Chronic Fatigue Syndrome.” Psychological Medicine 43 (5): 995-1002.
- Keute, Marius, Mustafa Demirezen, Arnd Graf, Notger G. Mueller, and Tino Zaehle. 2019. “No Modulation of Pupil Size and Event-Related Pupil Response by Transcuta-neous Auricular Vagus Nerve Stimulation (taVNS).” Scientific Reports 9: 11452. [CrossRef]
- Komaroff, Anthony L., and W. Ian Lipkin. 2021. “Insights from Myalgic Encephalomyeli-tis/Chronic Fatigue Syndrome May Help Unravel the Pathogenesis of Postacute COVID-19 Syndrome.” Trends in Molecular Medicine 27 (9): 895-906.
- Ludwig, Mareike, Celine Wienke, Matthew J. Betts, Tino Zaehle, and Dorothea Hammerer. 2021. “Current Challenges in Reliably Targeting the Noradrenergic Locus Coeruleus Using Transcutaneous Auricular Vagus Nerve Stimulation (taVNS).” Autonomic Neuroscience 236: 102900. [CrossRef]
- Ludwig, Mareike, Celine Wienke, Matthew J. Betts, Tino Zaehle, and Dorothea Häm-merer. 2024. “Current and Future Directions in Transcutaneous Vagus Nerve Stimula-tion: Research, Application, and Effects on the Locus Coeruleus-Norepinephrine Sys-tem.” Neuroscience & Biobehavioral Reviews 159: 105607. [CrossRef]
- Lumey, L. H., Aryeh D. Stein, and Ezra Susser. 2011. “Prenatal Famine and Adult Health.” Annual Review of Public Health 32: 237-262. [CrossRef]
- McGowan, Patrick O., Aya Sasaki, Ana C. D’Alessio, et al. 2009. “Epigenetic Regulation of the Glucocorticoid Receptor in Human Brain Associates with Childhood Abuse.” Nature Neuroscience 12 (3): 342-348.
- Murphy, Peter R., Redmond G. O’Connell, Michael O’Sullivan, Ian H. Robertson, and Joshua H. Balsters. 2014. “Pupil Diameter Covaries with BOLD Activity in Human Locus Coeru-leus.” Human Brain Mapping 35 (8): 4140-4154.
- Nakatomi, Yasuhito, Kei Mizuno, Akira Ishii, et al. 2014. “Neuroinflammation in Patients with Chronic Fatigue Syndrome/Myalgic Encephalomyelitis: An [11C-(R)]PK11195 PET Study.” Journal of Nuclear Medicine 55 (6): 945-950.
- Naviaux, Robert K., Jane C. Naviaux, Kefeng Li, et al. 2016. “Metabolic Features of Chronic Fatigue Syndrome.” Proceedings of the National Academy of Sciences USA 113 (37): E5472-E5480.
- Nedergaard, Maiken. 2013. “Garbage Truck of the Brain.” Science 340 (6140): 1529-1530.
- Nelson, Maximilian J., Joel S. Bahl, Jonathan D. Buckley, Ross L. Thomson, and Kade Davi-son. 2019. “Evidence of Altered Cardiac Autonomic Regulation in ME/CFS: A Systematic Review and Meta-Analysis.” Medicine 98 (43): e17600.
- Painter, Rebecca C., Clive Osmond, Peter Gluckman, et al. 2008. “Transgenerational Effects of Prenatal Exposure to the Dutch Famine on Neonatal Adiposity and Health in Later Life.” BJOG 115 (10): 1243-1249. [CrossRef]
- Perroud, Nader, Ariane Paoloni-Giacobino, Paco Prada, et al. 2011. “Increased Methylation of Glucocorticoid Receptor Gene (NR3C1) in Adults with a History of Childhood Maltreat-ment.” Translational Psychiatry 1 (12): e59.
- Pietrzak, Robert H., Jean-Dominique Gallezot, Yiyun S. Ding, et al. 2013. “Association of PTSD with Reduced In Vivo Norepinephrine Transporter Availability in the Locus Coeru-leus.” JAMA Psychiatry 70 (11): 1199-1205.
- Priovoulos, Nikos, Heidi I. L. Jacobs, Dimo Ivanov, Kamil Uludag, Frans R. J. Verhey, and Benedikt A. Poser. 2018. “High-Resolution In Vivo Imaging of Human Locus Coeruleus by Magnetization Transfer MRI at 3T and 7T.” NeuroImage 168: 427-436.
- Redgrave, Jessica N., Lyndsey Moore, Tobi Oyekunle, Mubarak Ebrahim, Konstanti-nos Falidas, Nicola Snowdon, Ali Ali, and Arshad Majid. 2018. “Transcutaneous Auri-cular Vagus Nerve Stimulation with Concurrent Upper Limb Repetitive Task Practice for Poststroke Motor Recovery: A Pilot Study.” Journal of Stroke and Cerebrovascular Diseases 27 (7): 1998-2005. [CrossRef]
- Reik, Wolf, Wendy Dean, and Jorn Walter. 2001. “Epigenetic Reprogramming in Mammali-an Development.” Science 293 (5532): 1089-1093. [CrossRef]
- Ridgewell, Christopher, Keith J. Heaton, Andrea Hildebrandt, Jeremy Couse, David Leber, and William H. Neumeier. 2021. “The Effects of Transcutaneous Auricular Va-gal Nerve Stimulation on Cognition in Healthy Individuals: A Meta-Analysis.” Neu-ropsychology 35 (4): 352-365. [CrossRef]
- Rodgers, Ali B., Christopher P. Morgan, Stefanie L. Bronson, et al. 2013. “Paternal Stress Exposure Alters Sperm MicroRNA Content and Reprograms Offspring HPA Stress Axis Regulation.” Journal of Neuroscience 33 (21): 9003-9012. [CrossRef]
- Sara, Susan J. 2009. “The Locus Coeruleus and Noradrenergic Modulation of Cogniti-on.” Nature Reviews Neuroscience 10 (3): 211-223. [CrossRef]
- Sasaki, Hiroyuki, and Yasuhisa Matsui. 2008. “Epigenetic Events in Mammalian Germ-Cell Development: Reprogramming and Beyond.” Nature Reviews Genetics 9 (2): 129-140. [CrossRef]
- Schwarz, Lindsay A., and Liqun Luo. 2015. “Organization of the Locus Coeruleus-Norepinephrine System.” Current Biology 25 (21): R1051-R1056.
- Shiffer, Dana, Stefano Rigo, Maura Minonzio, Deniz Timothy Yarsuvat, Eleonora To-baldini, Ludovico Furlan, Nicola Montano, Beatrice Cairo, Alberto Porta, Antonio Roberto Zamunér, Stefanos Bonovas, Vasile Urechie, Italo Biaggioni, André Diedrich, and Raffaello Furlan. 2025. “Short and Long Term Effects of a Two-Week Transcutane-ous Vagus Nerve Stimulation in Hyperadrenergic Postural Orthostatic Tachycardia Syndrome: A Proof-of-Concept Trial.” European Journal of Internal Medicine. [CrossRef]
- Shungu, Dikoma C., Natalie Weiduschat, James W. Murrough, et al. 2012. “Increased Ventricular Lactate in Chronic Fatigue Syndrome. III. Relationships to Cortical Glutathione and Clinical Symptoms.” NMR in Biomedicine 25 (9): 1073-1087.
- Skora, Lidia, Anna Marzecová, and Gerhard Jocham. 2024. “Tonic and Phasic Transcu-taneous Auricular Vagus Nerve Stimulation (taVNS) Both Evoke Rapid and Transient Pupil Dilation.” Brain Stimulation 17 (2): 233-244. [CrossRef]
- Stavrakis, Stavros, James A. Stoner, M. Beth Humphrey, Lynsie Morris, Andrea Fili-berti, John C. Reynolds, Khaled Elkholey, Imran Javed, Nik Twidale, Pavel Riha, Savita Varahan, Benjamin J. Scherlag, Warren M. Jackman, Tarun W. Dasari, and Sunny S. Po. 2020. “TREAT AF (Transcutaneous Electrical Vagus Nerve Stimulation to Suppress Atrial Fibrillation): A Randomized Clinical Trial.” JACC: Clinical Electro-physiology 6 (3): 282-291. [CrossRef]
- Stavrakis, Stavros, Praloy Chakraborty, Kassem Farhat, Seabrook Whyte, Lynsie Mor-ris, Zain Ul Abideen Asad, Brittany Karfonta, Juvaria Anjum, H. Greg Matlock, Xue Cai, and Xichun Yu. 2024. “Noninvasive Vagus Nerve Stimulation in Postural Ta-chycardia Syndrome: A Randomized Clinical Trial.” JACC: Clinical Electrophysiology 10 (2): 346-355. [CrossRef]
- Valentino, Rita J., and Elisabeth Van Bockstaele. 2008. “Convergent Regulation of Locus Coeruleus Activity as an Adaptive Response to Stress.” European Journal of Pharmacology 583 (2-3): 194-203.
- van Campen, C. Linda M. C., Peter C. Rowe, and Frans C. Visser. 2020. “Cerebral Blood Flow Is Reduced in Severe ME/CFS Patients During Mild Orthostatic Stress Testing.” Healthcare 8 (2): 169.
- Van Houdenhove, Boudewijn, Etienne Neerinckx, Romain Lysens, et al. 2001. “Victimizati-on in Chronic Fatigue Syndrome and Fibromyalgia in Tertiary Care.” Psychosomatics 42 (1): 21-28.
- Ventura-Bort, Carlos, Iria Garcia de Gurtubay, Pablo Bermejo, et al. 2023. “Immediate Effects and Duration of a Short and Single Application of Transcutaneous Auricular Vagus Nerve Stimulation on P300 Event Related Potential.” Frontiers in Neuroscience 17: 1096865. [CrossRef]
- Villani, Valentina, Manos Tsakiris, and Ruben T. Azevedo. 2022. “Transcutaneous Vagus Nerve Stimulation Modulates Pupil Size and Interoceptive Attention.” Psycho-physiology 59 (4): e13983. [CrossRef]
- Warren, Christopher M., Kim D. Tona, Lucia Ber, Ruud L. van den Brink, Loes van Nieuwenhoven, Eco J. C. de Geus, and Sander Nieuwenhuis. 2019. “The Neuromodu-latory and Hormonal Effects of Transcutaneous Vagus Nerve Stimulation as Evidenced by Salivary Alpha Amylase, Salivary Cortisol, Pupil Diameter, and the P3 Event-Related Potential.” Brain Stimulation 12 (3): 635-642. [CrossRef]
- Wienke, Celine, Marcus Grueschow, Aiden Haghikia, and Tino Zaehle. 2023. “Phasic, Event-Related Transcutaneous Auricular Vagus Nerve Stimulation Modifies Behavio-ral, Pupillary, and Low-Frequency Oscillatory Power Responses.” Journal of Neuro-science 43 (36): 6306-6319. [CrossRef]
- Wirth, Klaus, and Carmen Scheibenbogen. 2020. “A Unifying Hypothesis of the Pathophy-siology of ME/CFS: Insights from Autoantibodies Against Beta2-Adrenergic Receptors.” Autoimmunity Reviews 19 (6): 102527.
- Xie, Lulu, Hongyi Kang, Qiwu Xu, et al. 2013. “Sleep Drives Metabolite Clearance from the Adult Brain.” Science 342 (6156): 373-377. [CrossRef]
- Yakunina, Natalia, Sam Soo Kim, and Eui-Cheol Nam. 2017. “Optimization of Transcuta-neous Vagus Nerve Stimulation Using Functional MRI.” Neuromodulation: Technology at the Neural Interface 20 (3): 290-300. [CrossRef]
- Yehuda, Rachel, Nikolaos P. Daskalakis, Linda M. Bierer, et al. 2016. “Holocaust Exposure Induced Intergenerational Effects on FKBP5 Methylation.” Biological Psychiatry 80 (5): 372-380. [CrossRef]
- Yehuda, Rachel, and Amy Lehrner. 2018. “Intergenerational Transmission of Trauma Effects: Putative Role of Epigenetic Mechanisms.” World Psychiatry 17 (3): 243-257. [CrossRef]
- Young, Joel L. 2013. “Use of Lisdexamfetamine Dimesylate in Treatment of Executive Functioning Deficits and Chronic Fatigue Syndrome: A Double-Blind, Placebo-Controlled Study.” Psychiatry Research 207 (1-2): 127-133.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



