Submitted:
17 December 2025
Posted:
19 December 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
1.1. The ME/CFS Enigma
1.2. The ACE Connection
1.3. Preliminary Pharmacological Observations
1.4. Scope and Structure
2. Neurobiological Foundations
2.1. The Locus Coeruleus: Anatomy and Function
2.2. The CRF-LC Stress Axis
2.3. ACEs: Programming the Stress System
2.4. LC Vulnerability to Chronic Stress
2.5. The Glymphatic Connection
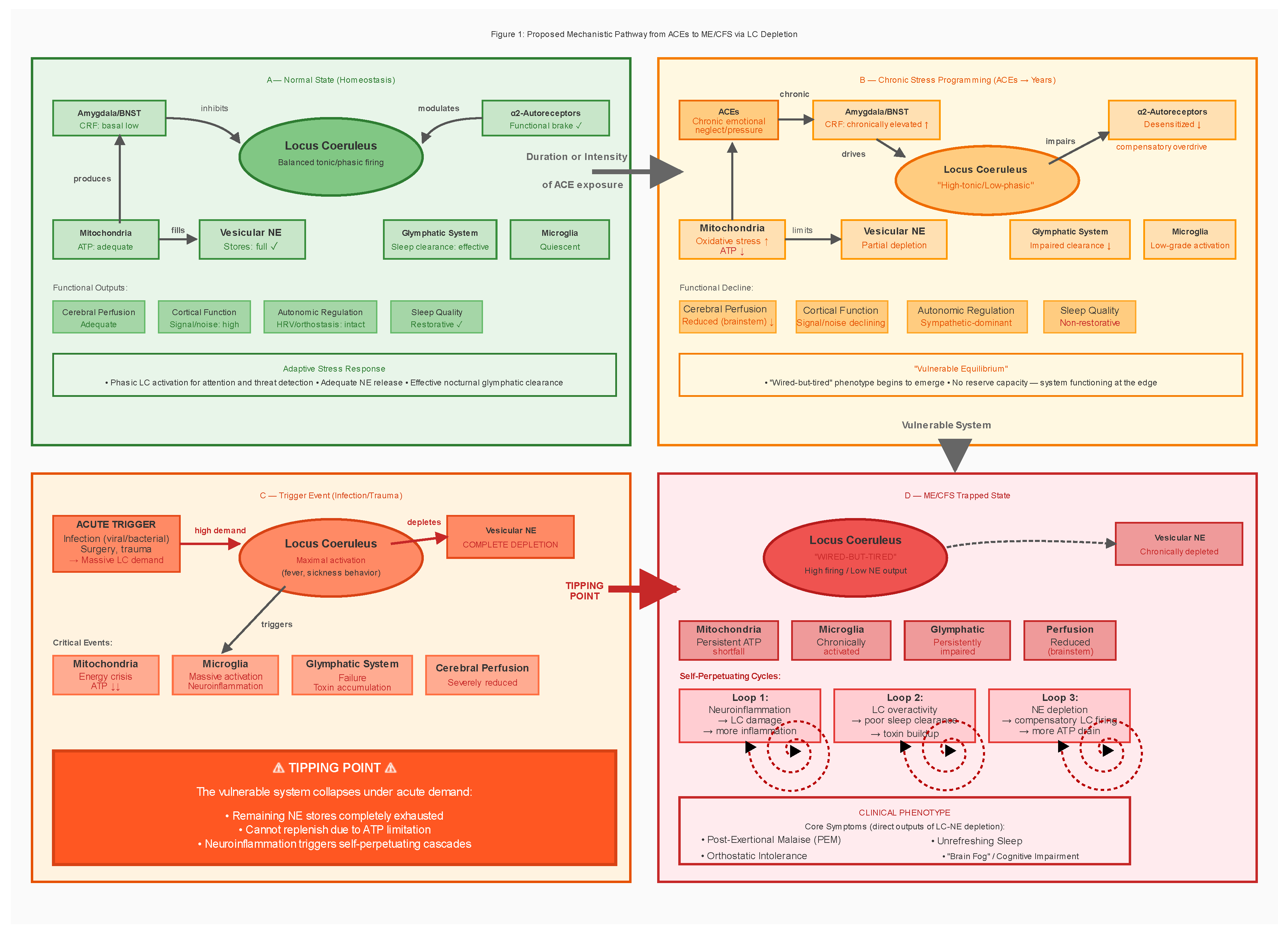
3. The Proposed Mechanism
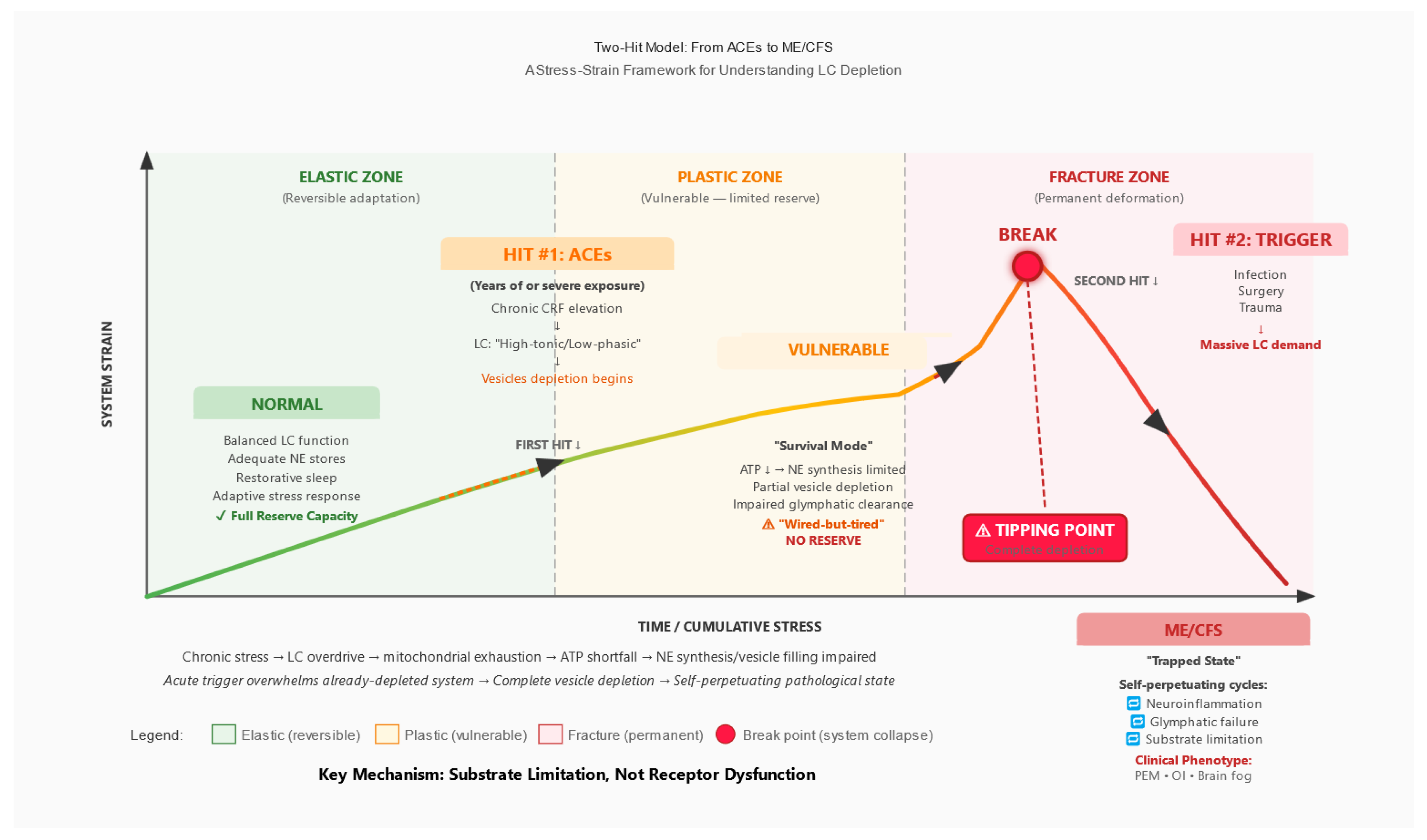
3.1. Multi-Stage Model
3.2. Differentiation from Existing Two-Hit Models
4. Clinical Phenomena Through the LC Depletion Lens
4.1. The ‘Wired-but-Tired’ Paradox
4.2. Post-Exertional Malaise
4.3. Orthostatic Intolerance
4.4. Unrefreshing Sleep
5. Supporting Evidence and Alternative Explanations
5.1. Evidence Supporting the Hypothesis
5.2. Alternative and Complementary Mechanisms
5.3. Limitations and Uncertainties
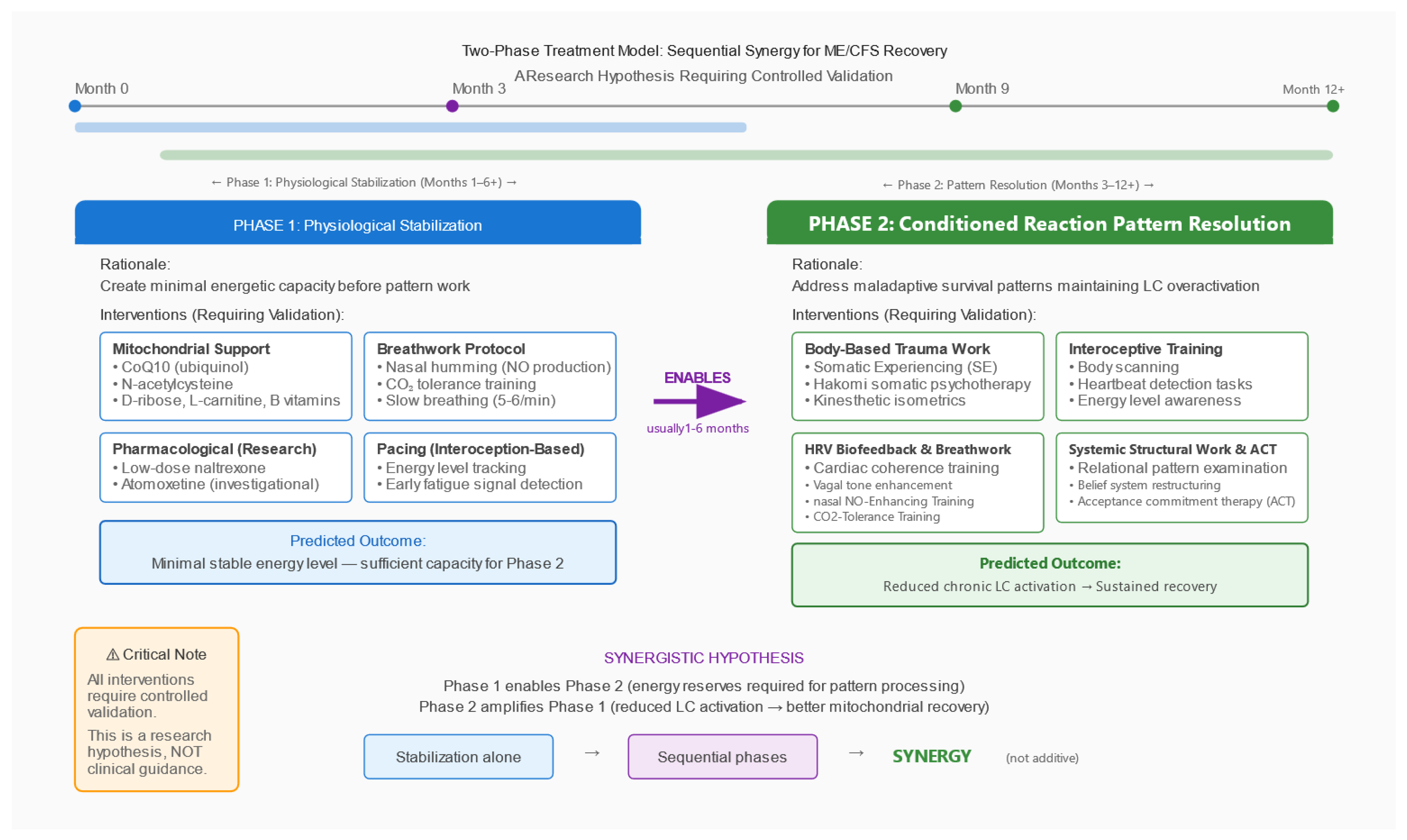
6. Testable Predictions and Research Agenda
6.1. Neuromelanin-Sensitive MRI of the LC
6.2. NET-PET Imaging
6.3. CSF Metabolite Profiling
6.4. Physiological Measures (HRV, Pupillometry)
6.5. Pharmacological Differentiation (N-of-1 Trials)
6.6. Prospective ACE-ME/CFS Cohort
7. Potential Disconfirming Evidence
8. Discussion
8.1. Strengths
8.2. Weaknesses
8.3. Implications if Hypothesis Is Correct
9. Conclusions
Funding
Conflicts of Interest
Acknowledgments
Data Availability
Ethics
Abbreviations
References
- Aston-Jones, G. and Cohen, J.D. (2005) ‘An integrative theory of locus coeruleus-norepinephrine function: adaptive gain and optimal performance’, Annual Review of Neuroscience, 28, pp. 403–450.
- Bangasser, D.A. and Valentino, R.J. (2020) ‘The locus coeruleus-norepinephrine system in stress and arousal: unraveling historical, current, and future perspectives’, Frontiers in Psychiatry, 11, p. 601519.
- Baumeister, D., Akhtar, R., Ciufolini, S., Pariante, C.M. and Mondelli, V. (2016) ‘Childhood trauma and adulthood inflammation: a meta-analysis’, Molecular Psychiatry, 21(5), pp. 642–649.
- Betts, M.J., Kirilina, E., Otaduy, M.C.G., et al. (2019) ‘Locus coeruleus imaging as a biomarker for noradrenergic dysfunction in neurodegenerative diseases’, Brain, 142(9), pp. 2558–2571. 9.
- Blockmans, D., Persoons, P., Van Houdenhove, B. and Bobbaers, H. (2006) ‘Does methylphenidate reduce the symptoms of chronic fatigue syndrome?’, The American Journal of Medicine, 119(12), pp. 1047–1053.
- Bunea, I.M., Szentágotai-Tătar, A. and Miu, A.C. (2017) ‘Early-life adversity and cortisol response to social stress: a meta-analysis’, Translational Psychiatry, 7(12), p. 1274.
- Da Silva, J.P. et al. (2025) ‘Delineating clinical phenotypes and HPA-axis dysfunction in ME/CFS’, presented at IACFS/ME 2025 Conference [conference abstract—not peer-reviewed].
- Edwards, R.H. (2007) ‘The neurotransmitter cycle and quantal size’, Neuron, 55(6), pp. 835–849.
- Eiden, L.E. and Weihe, E. (2011) ‘VMAT2: a dynamic regulator of brain monoaminergic neuronal function interacting with drugs of abuse’, Annals of the New York Academy of Sciences, 1216, pp. 86–98.
- Felitti, V.J., Anda, R.F., Nordenberg, D., et al. (1998) ‘Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults’, American Journal of Preventive Medicine, 14(4), pp. 245–258.
- Goldstein, D.S. and Aregawi, D. (2025) ‘Low brain norepinephrine in ME/CFS’, presented at IACFS/ME 2025 Conference [conference abstract—not peer-reviewed].
- Hauglund, N.L., Andersen, M., Tokarska, K., et al. (2025) ‘Norepinephrine-mediated slow vasomotion drives glymphatic clearance during sleep’, Cell, 188(3), pp. 606–622. [CrossRef]
- Hendrix, J. et al. (2025) ‘Sympathetic dysfunction in ME/CFS: a meta-analysis’, presented at IACFS/ME 2025 Conference [conference abstract—not peer-reviewed].
- Joshi, S., Li, Y., Kalwani, R.M. and Gold, J.I. (2016) ‘Relationships between pupil diameter and neuronal activity in the locus coeruleus, colliculi, and cingulate cortex’, Neuron, 89(1), pp. 221–234.
- Kempke, S., Luyten, P., Claes, S., et al. (2013) ‘Self-critical perfectionism and fatigue and pain in chronic fatigue syndrome’, Psychological Medicine, 43(5), pp. 995–1002.
- Komaroff, A.L. and Lipkin, W.I. (2021) ‘Insights from myalgic encephalomyelitis/chronic fatigue syndrome may help unravel the pathogenesis of postacute COVID-19 syndrome’, Trends in Molecular Medicine, 27(9), pp. 895–906.
- McGowan, P.O., Sasaki, A., D’Alessio, A.C., et al. (2009) ‘Epigenetic regulation of the glucocorticoid receptor in human brain associates with childhood abuse’, Nature Neuroscience, 12(3), pp. 342–348.
- Murphy, P.R., O’Connell, R.G., O’Sullivan, M., Robertson, I.H. and Balsters, J.H. (2014) ‘Pupil diameter covaries with BOLD activity in human locus coeruleus’, Human Brain Mapping, 35(8), pp. 4140–4154.
- Nakatomi, Y., Mizuno, K., Ishii, A., et al. (2014) ‘Neuroinflammation in patients with chronic fatigue syndrome/myalgic encephalomyelitis: an [11C-(R)]PK11195 PET study’, Journal of Nuclear Medicine, 55(6), pp. 945–950.
- Naviaux, R.K., Naviaux, J.C., Li, K., et al. (2016) ‘Metabolic features of chronic fatigue syndrome’, Proceedings of the National Academy of Sciences USA, 113(37), pp. E5472–E5480.
- Nedergaard, M. (2013) ‘Garbage truck of the brain’, Science, 340(6140), pp. 1529–1530.
- Nelson, M.J., Bahl, J.S., Buckley, J.D., Thomson, R.L. and Davison, K. (2019) ‘Evidence of altered cardiac autonomic regulation in ME/CFS: a systematic review and meta-analysis’, Medicine, 98(43), p. e17600.
- Perroud, N., Paoloni-Giacobino, A., Prada, P., et al. (2011) ‘Increased methylation of glucocorticoid receptor gene (NR3C1) in adults with a history of childhood maltreatment’, Translational Psychiatry, 1(12), p. e59.
- Pietrzak, R.H., Gallezot, J.D., Ding, Y.S., et al. (2013) ‘Association of PTSD with reduced in vivo norepinephrine transporter availability in the locus coeruleus’, JAMA Psychiatry, 70(11), pp. 1199–1205.
- Priovoulos, N., Jacobs, H.I.L., Ivanov, D., Uludağ, K., Verhey, F.R.J. and Poser, B.A. (2018) ‘High-resolution in vivo imaging of human locus coeruleus by magnetization transfer MRI at 3T and 7T’, NeuroImage, 168, pp. 427–436.
- Schwarz, L.A. and Luo, L. (2015) ‘Organization of the locus coeruleus-norepinephrine system’, Current Biology, 25(21), pp. R1051–R1056.
- Shungu, D.C., Weiduschat, N., Murrough, J.W., et al. (2012) ‘Increased ventricular lactate in chronic fatigue syndrome. III. Relationships to cortical glutathione and clinical symptoms’, NMR in Biomedicine, 25(9), pp. 1073–1087.
- Valentino, R.J. and Van Bockstaele, E. (2008) ‘Convergent regulation of locus coeruleus activity as an adaptive response to stress’, European Journal of Pharmacology, 583(2–3), pp. 194–203.
- van Campen, C.L.M.C., Rowe, P.C. and Visser, F.C. (2020) ‘Cerebral blood flow is reduced in severe ME/CFS patients during mild orthostatic stress testing’, Healthcare, 8(2), p. 169.
- Van Houdenhove, B., Neerinckx, E., Lysens, R., et al. (2001) ‘Victimization in chronic fatigue syndrome and fibromyalgia in tertiary care’, Psychosomatics, 42(1), pp. 21–28.
- Wirth, K. and Scheibenbogen, C. (2020) ‘A unifying hypothesis of the pathophysiology of ME/CFS: insights from autoantibodies against β2-adrenergic receptors’, Autoimmunity Reviews, 19(6), p. 102527.
- Xie, L., Kang, H., Xu, Q., et al. (2013) ‘Sleep drives metabolite clearance from the adult brain’, Science, 342(6156), pp. 373–377. [CrossRef]
- Young, J.L. (2013) ‘Use of lisdexamfetamine dimesylate in treatment of executive functioning deficits and chronic fatigue syndrome: a double-blind, placebo-controlled study’, Psychiatry Research, 207(1–2), pp. 127–133.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



