Submitted:
12 December 2025
Posted:
15 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design, Setting and Duration
2.2. Study Population and Eligibility Criteria
2.3. Sampling Technique
2.4. Sample Size Calculation
2.5. Data Collection Tool
2.5.1. Quantitative Tool
2.5.2. Qualitative Tool
2.6. Data Collection Procedure
2.7. Data Analysis
2.7.1. Quantitative Data Analysis
2.7.2. Qualitative Data Analysis
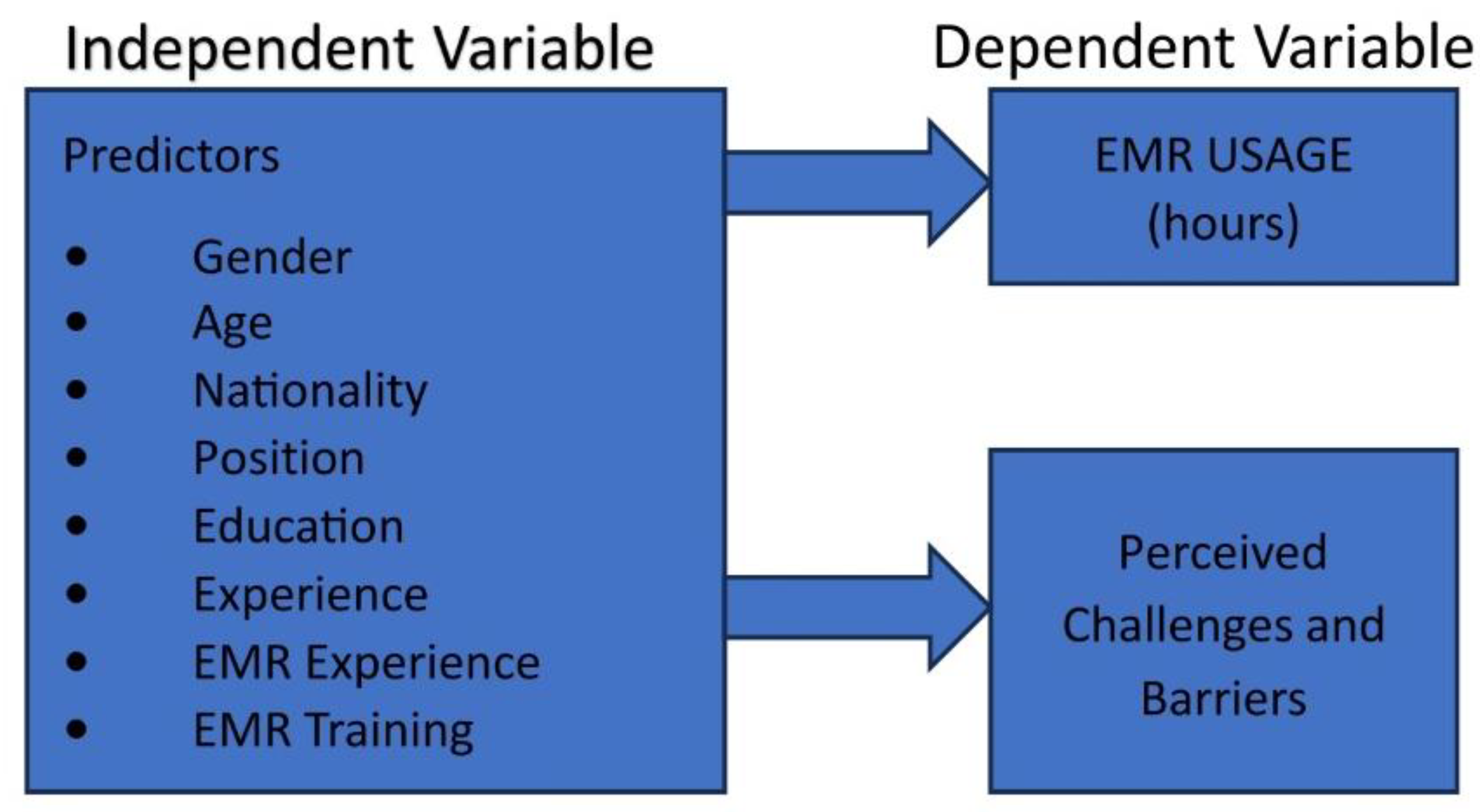
2.8. Conceptual Framework
2.9. Ethical Consideration
3. Results
3.1. Quantitative Data Results
3.2. Qualitative Data Results
3.2.1. Demographic Profile
3.2.2. Hours of EMR Use
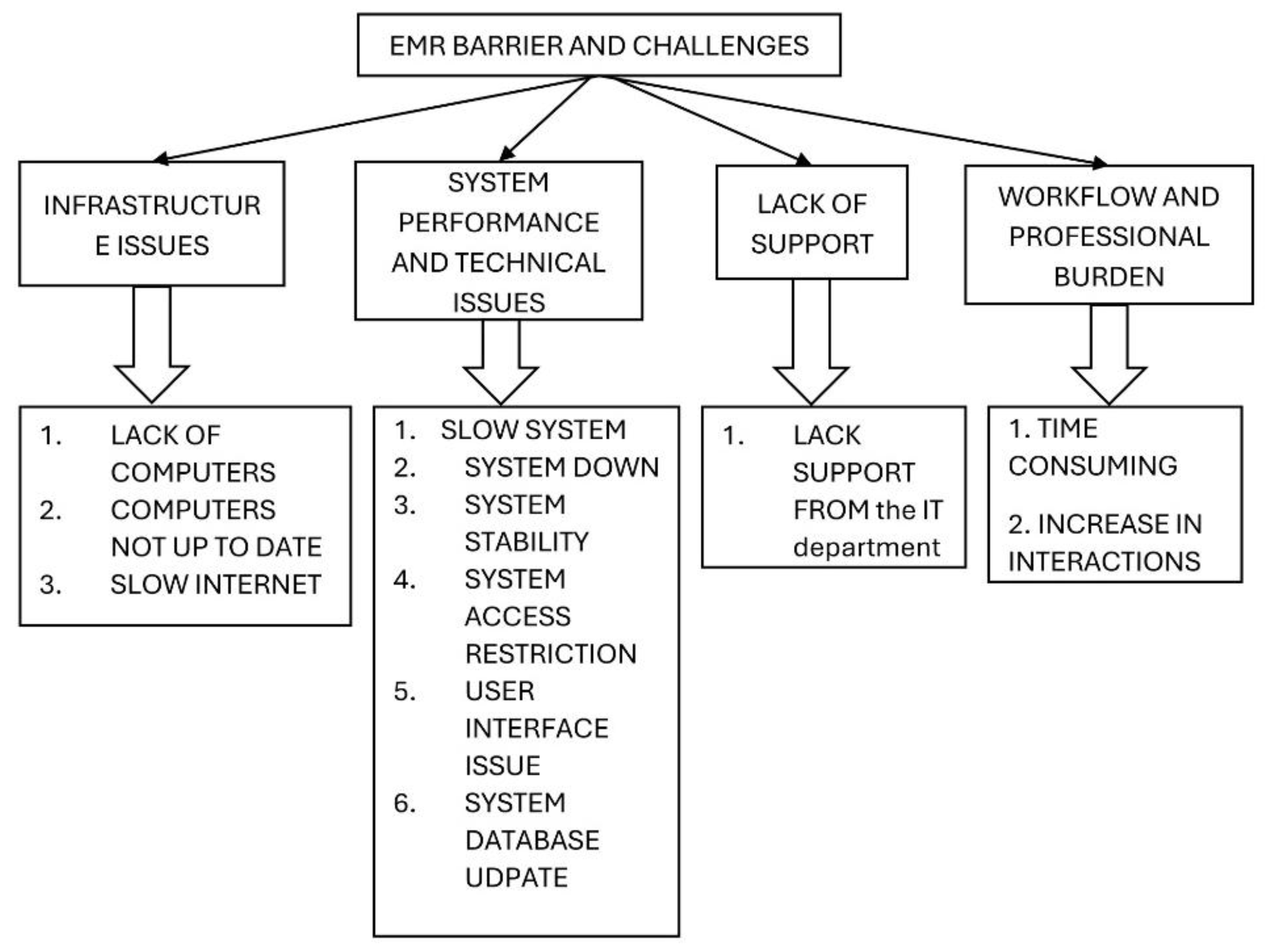
3.2.3. Challenges and Barriers Related to EMRs
3.2.3.1. Infrastructure Issues
3.2.3.3. Lack of Support
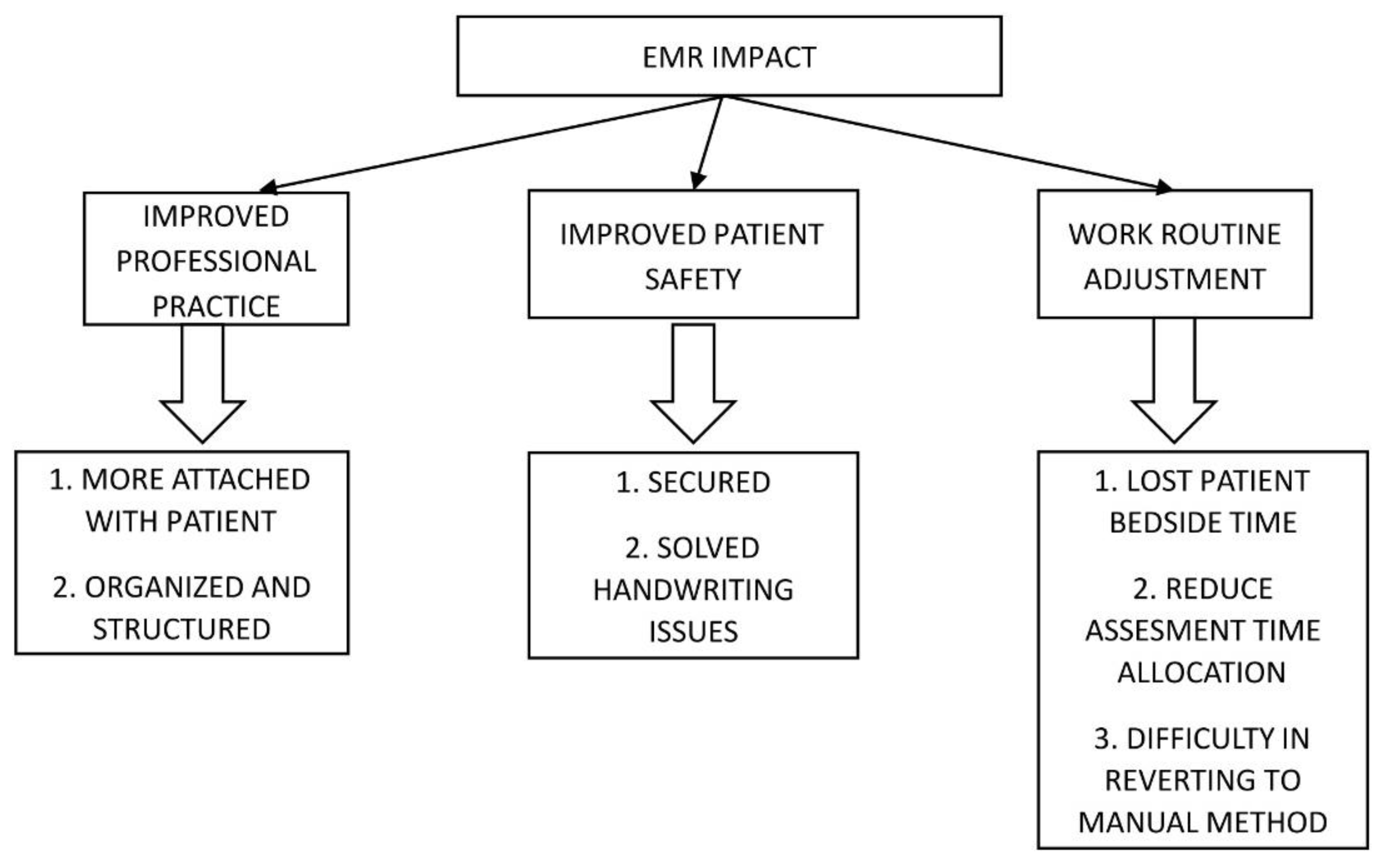
3.2.4. Impact of EMR Usage
3.2.4.1. Improved Professional Practice
3.2.4.2. Improved Patient Safety
3.2.4.3. Work Routine Adjustment
4. Discussion
4.1. Mean EMR Use Hours for Physicians and Nurses
4.2. Difference Between EMR Use Between Physicians and Nurses
4.3. Predictors of Extended EMR Use
4.4. Challenges and Barriers Related to EMR
4.5. Study Limitations, Strengths, and Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Menachemi, N.; Collum, T.H. Benefits and drawbacks of electronic health record systems. Risk Manag Healthc Policy 2011, 4, 47–55. [Google Scholar] [CrossRef] [PubMed]
- Jabali, K.; Jarrar, M.t. Electronic Health Records Functionalities in Saudi Arabia: Obstacles and Major Challenges. Global Journal of Health Science 2018, 10, 50–50. [Google Scholar] [CrossRef]
- Akwaowo, C.D.; Sabi, H.M.; Ekpenyong, N.; Isiguzo, C.M.; Andem, N.F.; Maduka, O.; Dan, E.; Umoh, E.; Ekpin, V.; Uzoka, F.M. Adoption of electronic medical records in developing countries-A multi-state study of the Nigerian healthcare system. Front Digit Health 2022, 4, 1017231. [Google Scholar] [CrossRef] [PubMed]
- Alotaibi, Y.K.; Federico, F. The impact of health information technology on patient safety. Saudi Med J 2017, 38, 1173–1180. [Google Scholar] [CrossRef]
- De Benedictis, A.; Lettieri, E.; Gastaldi, L.; Masella, C.; Urgu, A.; Tartaglini, D. Electronic Medical Records implementation in hospital: An empirical investigation of individual and organizational determinants. PLoS One 2020, 15, e0234108. [Google Scholar] [CrossRef]
- Abdullah Alharbi, R. Adoption of electronic health records in Saudi Arabia hospitals: Knowledge and usage. Journal of King Saud University - Science 2023, 35, 102470. [Google Scholar] [CrossRef]
- National E-Health Strategy. Available online: https://www.moh.gov.sa/en/Ministry/nehs/Pages/Ehealth.aspx (accessed on November 25).
- Babbott, S.; Manwell, L.B.; Brown, R.; Montague, E.; Williams, E.; Schwartz, M.; Hess, E.; Linzer, M. Electronic medical records and physician stress in primary care: results from the MEMO Study. J Am Med Inform Assoc 2014, 21, e100-106. [Google Scholar] [CrossRef]
- Murad, M.H.; Vaa Stelling, B.E.; West, C.P.; Hasan, B.; Simha, S.; Saadi, S.; Firwana, M.; Viola, K.E.; Prokop, L.J.; Nayfeh, T.; et al. Measuring Documentation Burden in Healthcare. J Gen Intern Med 2024, 39, 2837–2848. [Google Scholar] [CrossRef]
- Harris, D.A.; Haskell, J.; Cooper, E.; Crouse, N.; Gardner, R. Estimating the association between burnout and electronic health record-related stress among advanced practice registered nurses. Appl Nurs Res 2018, 43, 36–41. [Google Scholar] [CrossRef]
- Ehrenfeld, J.M.; Wanderer, J.P. Technology as friend or foe? Do electronic health records increase burnout? Curr Opin Anaesthesiol 2018, 31, 357–360. [Google Scholar] [CrossRef]
- Alhur, A. Overcoming Electronic Medical Records Adoption Challenges in Saudi Arabia. Cureus 2024, 16, e53827. [Google Scholar] [CrossRef] [PubMed]
- Khalifa, M. Barriers to Health Information Systems and Electronic Medical Records Implementation. A Field Study of Saudi Arabian Hospitals. Procedia Computer Science 2013, 21, 335–342. [Google Scholar] [CrossRef]
- Ilker, E.; Sulaiman Abubakar, M.; Rukayya Sunusi, A. Comparison of Convenience Sampling and Purposive Sampling. American Journal of Theoretical and Applied Statistics 2015, 5, 1–4. [Google Scholar] [CrossRef]
- Sample size to detect a significant difference between two proportions. Available online: https://epitools.ausvet.com.au/twoproportions (accessed on 20 November).
- What specialty spends the most time on paperwork and administration? Available online: https://www.beckersphysicianleadership.com/physician-workforce/what-specialty-spends-the-most-time-on-paperwork-and-administration (accessed on November 25).
- AlOtaib, Y.; AlSaedi, M. Physicians’ Perceptions and Attitudes toward Use of Electronic Medical Record Systems in Riyadh. World Family Medicine Journal /Middle East Journal of Family Medicine 2022, 20. [Google Scholar] [CrossRef]
- Alessa, T. Clinicians' Attitudes Toward Electronic Health Records in Saudi Arabia. Cureus 2024, 16, e56281. [Google Scholar] [CrossRef]
- Asiri, S. Factors Influencing Electronic Health Record Workflow Integration Among Nurses in Saudi Arabia: Cross-Sectional Study. SAGE Open Nurs 2024, 10, 23779608241260547. [Google Scholar] [CrossRef]
- Al Otaybi, H.F.; Al-Raddadi, R.M.; Bakhamees, F.H. Performance, Barriers, and Satisfaction of Healthcare Workers Toward Electronic Medical Records in Saudi Arabia: A National Multicenter Study. Cureus 2022, 14, e21899. [Google Scholar] [CrossRef]
- Neuendorf, K.A. Content analysis and thematic analysis. In Advanced research methods for applied psychology; Routledge, 2018; pp. 211–223. [Google Scholar]
- Davis, F.D. Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS quarterly 1989, 319–340. [Google Scholar] [CrossRef]
- Rotenstein, L.S.; Holmgren, A.J.; Downing, N.L.; Bates, D.W. Differences in Total and After-hours Electronic Health Record Time Across Ambulatory Specialties. JAMA Intern Med 2021, 181, 863–865. [Google Scholar] [CrossRef]
- Rotenstein, L.S.; Holmgren, A.J.; Healey, M.J.; Horn, D.M.; Ting, D.Y.; Lipsitz, S.; Salmasian, H.; Gitomer, R.; Bates, D.W. Association Between Electronic Health Record Time and Quality of Care Metrics in Primary Care. JAMA Netw Open 2022, 5, e2237086. [Google Scholar] [CrossRef]
- Overhage, J.M.; McCallie, D., Jr. Physician Time Spent Using the Electronic Health Record During Outpatient Encounters: A Descriptive Study. Ann Intern Med 2020, 172, 169–174. [Google Scholar] [CrossRef]
- Holmgren, A.J.; Lindeman, B.; Ford, E.W. Resident Physician Experience and Duration of Electronic Health Record Use. Appl Clin Inform 2021, 12, 721–728. [Google Scholar] [CrossRef] [PubMed]
- Bakhoum, N.; Gerhart, C.; Schremp, E.; Jeffrey, A.D.; Anders, S.; France, D.; Ward, M.J. A Time and Motion Analysis of Nursing Workload and Electronic Health Record Use in the Emergency Department. J Emerg Nurs 2021, 47, 733–741. [Google Scholar] [CrossRef] [PubMed]
- Seto, R.; Inoue, T.; Tsumura, H. Clinical documentation improvement for outpatients by implementing electronic medical records. Stud Health Technol Inform 2014, 201, 102–107. [Google Scholar] [PubMed]
- Alkasasbeh, A.; Jarrah, S.; Alhusamiah, B.; Tarawneh, F. Factors Influencing the Utilization and Adoption of Electronic Health Records among Nurses in Jordanian Hospitals. Jordan Journal of Nursing Research 2025, 4, 1–13. [Google Scholar] [CrossRef]
- Goldstein, I.H.; Hribar, M.R.; Reznick, L.G.; Chiang, M.F. Analysis of Total Time Requirements of Electronic Health Record Use by Ophthalmologists Using Secondary EHR Data. AMIA Annu Symp Proc 2018, 2018, 490–497. [Google Scholar]
- Wang, J.K.; Ouyang, D.; Hom, J.; Chi, J.; Chen, J.H. Characterizing electronic health record usage patterns of inpatient medicine residents using event log data. PLoS One 2019, 14, e0205379. [Google Scholar] [CrossRef]
- Tamli, N.; Sain, M. Exploring Innovative Strategies For Patient-Centered Care In The Nursing Profession. A Bi-annual South Asian Journal of Research & Innovation 2023, 10, 19–30. [Google Scholar] [CrossRef]
- Forde-Johnston, C.; Butcher, D.; Aveyard, H. An integrative review exploring the impact of Electronic Health Records (EHR) on the quality of nurse-patient interactions and communication. J Adv Nurs 2023, 79, 48–67. [Google Scholar] [CrossRef]
- Camilleri, N.; Henks, N.; Seo, K.; Kim, J.H. EMR usage and nurse documentation burden in a medical intensive care unit. In Proceedings of the International Conference on Human-Computer Interaction, 2022; pp. 165–173. [Google Scholar]
- AlQahtani, M.; AlShaibani, W.; AlAmri, E.; Edward, D.; Khandekar, R. Electronic Health Record-Related Stress Among Nurses: Determinants and Solutions. Telemed J E Health 2021, 27, 544–550. [Google Scholar] [CrossRef]
- Gaffney, A.; Woolhandler, S.; Cai, C.; Bor, D.; Himmelstein, J.; McCormick, D.; Himmelstein, D.U. Medical Documentation Burden Among US Office-Based Physicians in 2019: A National Study. JAMA Intern Med 2022, 182, 564–566. [Google Scholar] [CrossRef] [PubMed]
- Rotenstein, L.S.; Fong, A.S.; Jeffery, M.M.; Sinsky, C.A.; Goldstein, R.; Williams, B.; Melnick, E.R. Gender Differences in Time Spent on Documentation and the Electronic Health Record in a Large Ambulatory Network. JAMA Netw Open 2022, 5, e223935. [Google Scholar] [CrossRef] [PubMed]
- Asaad Nasser Izzuldeen Qasimi, S.A.S.A.M.M.M.T.M.H.A.B.M.H. Privacy Issues Hindering Implementation and Use of Electronic Health Records in the Middle East. Journal of International Crisis and Risk Communication Research 2025, 1274–1278. [Google Scholar] [CrossRef]
- Aldosari, B.; Al-Mansour, S.; Aldosari, H.; Alanazi, A. Assessment of factors influencing nurses acceptance of electronic medical record in a Saudi Arabia hospital. Informatics in Medicine Unlocked 2017, 10. [Google Scholar] [CrossRef]
- Yehualashet, D.E.; Seboka, B.T.; Tesfa, G.A.; Demeke, A.D.; Amede, E.S. Barriers to the Adoption of Electronic Medical Record System in Ethiopia: A Systematic Review. J Multidiscip Healthc 2021, 14, 2597–2603. [Google Scholar] [CrossRef]
- Samadbeik, M.; Fatehi, F.; Braunstein, M.; Barry, B.; Saremian, M.; Kalhor, F.; Edirippulige, S. Education and Training on Electronic Medical Records (EMRs) for health care professionals and students: A Scoping Review. Int J Med Inform 2020, 142, 104238. [Google Scholar] [CrossRef]
- Hamdan AB, M.R.; Mahmud, A. Challenges in the use Electronic Medical Records in Middle Eastern Countries: A Narrative Review. Malaysian Journal of Medicine and Health Sciences 2023, 19, 334–340. [Google Scholar] [CrossRef]
- Rule, A.; Chiang, M.F.; Hribar, M.R. Using electronic health record audit logs to study clinical activity: a systematic review of aims, measures, and methods. J Am Med Inform Assoc 2020, 27, 480–490. [Google Scholar] [CrossRef]
- Arndt, B.G.; Beasley, J.W.; Watkinson, M.D.; Temte, J.L.; Tuan, W.J.; Sinsky, C.A.; Gilchrist, V.J. Tethered to the EHR: Primary Care Physician Workload Assessment Using EHR Event Log Data and Time-Motion Observations. Ann Fam Med 2017, 15, 419–426. [Google Scholar] [CrossRef]
- del Mar Rodriguez, T.L.M.; O'Hara, K.; McKanna, T.M.D.; Decker, S. Implementing a New EMR. How Should We Train the Staff? Journal of PeriAnesthesia Nursing 2021, 36, e18–e19. [Google Scholar] [CrossRef]
- Bekele, T.A.; Gezie, L.D.; Willems, H.; Metzger, J.; Abere, B.; Seyoum, B.; Abraham, L.; Wendrad, N.; Meressa, S.; Desta, B.; et al. Barriers and facilitators of the electronic medical record adoption among healthcare providers in Addis Ababa, Ethiopia. Digit Health 2024, 10, 20552076241301946. [Google Scholar] [CrossRef] [PubMed]
- Sugiarto, P.; Purnami, C.; Jati, S. Supporting and Inhibiting Factors in Implementing Electronic Medical Records (EMR) Policy in Indonesia. BIO Web of Conferences 2024, 133, 00038. [Google Scholar] [CrossRef]
- Feryansyah, A.; Suprapto, S.; Wardani, R. Analysis of the Implementation of Electronic Medical Records in Community Health Centers. Indonesian Journal of Global Health Research 2025, 7, 919–930. [Google Scholar] [CrossRef]
- Gutiérrez, O.; Romero, G.; Pérez, L.; Salazar, A.; Charris, M.; Wightman, P. HealthyBlock: Blockchain-Based IT Architecture for Electronic Medical Records Resilient to Connectivity Failures. International Journal of Environmental Research and Public Health 2020, 17, 7132. [Google Scholar] [CrossRef]
- Avula, R. Addressing Barriers in Data Collection, Transmission, and Security to Optimize Data Availability in Healthcare Systems for Improved Clinical Decision-Making and Analytics. Applied Research in Artificial Intelligence and Cloud Computing 2021, 4, 78–93. [Google Scholar]
- Kessy, E.C.; Kibusi, S.M.; Ntwenya, J.E. Electronic medical record systems data use in decision-making and associated factors among health managers at public primary health facilities, Dodoma region: a cross-sectional analytical study. Front Digit Health 2023, 5, 1259268. [Google Scholar] [CrossRef]
- El Mahalli, A. Adoption and Barriers to Adoption of Electronic Health Records by Nurses in Three Governmental Hospitals in Eastern Province, Saudi Arabia. Perspect Health Inf Manag 2015, 12, 1f. [Google Scholar]
- Kiri, V.A.; Ojule, A.C. Electronic medical record systems: A pathway to sustainable public health insurance schemes in sub-Saharan Africa. Nigerian Postgraduate Medical Journal 2020, 27, 1–7. [Google Scholar] [CrossRef]
- Larsen, E.; Rao, A.; Sasangohar, F. Understanding the scope of downtime threats: A scoping review of downtime-focused literature and news media. Health Informatics Journal 2020, 26, 146045822091853. [Google Scholar] [CrossRef]
- Chen, J.; Li, Z.; Ma, W.; Tang, Y.; Liu, C.; Ma, S.; Xu, M.; Zhang, Q. Enhancing the timeliness of EMR documentation in resident doctors: the role of PDCA cycle management. BMC Medical Education 2024, 24, 1367. [Google Scholar] [CrossRef]
- Dutta, B.; Hwang, H.G. The adoption of electronic medical record by physicians: A PRISMA-compliant systematic review. Medicine (Baltimore) 2020, 99, e19290. [Google Scholar] [CrossRef] [PubMed]
- Mattingly, N.S. EVALUATION OF USER INTERFACE DESIGN IN ELECTRONIC MEDICAL RECORDS SOFTWARE FOR DIRECT PRIMARY CARE CLINICS; California State Polytechnic University: Pomona, 2022. [Google Scholar]
- Afzal, F.; Ahmad, A.; Ali, Q.; Joshi, S.; Mehra, S. Fulfilling the need of hour: Systematic review of challenges associated with electronic medical record (EMR) implementation-SBEA model. Vidyabharati International Interdisciplinary Research Journal 2021, 13, 649–662. [Google Scholar]
- Albagmi, S. The effectiveness of EMR implementation regarding reducing documentation errors and waiting time for patients in outpatient clinics: a systematic review. F1000Res 2021, 10, 514. [Google Scholar] [CrossRef] [PubMed]
- Li, E.; Clarke, J.; Ashrafian, H.; Darzi, A.; Neves, A.L. The impact of electronic health record interoperability on safety and quality of care in high-income countries: systematic review. Journal of medical Internet research 2022, 24, e38144. [Google Scholar] [CrossRef]
- Flynn, L. The benefits and challenges of multisite studies: lessons learned. AACN Adv Crit Care 2009, 20, 388–391. [Google Scholar] [CrossRef]
- Sedgwick, P. Multistage sampling. Bmj 2015, 351, h4155. [Google Scholar] [CrossRef]
- Anvari, F.; Efendić, E.; Olsen, J.; Arslan, R.C.; Elson, M.; Schneider, I.K. Bias in self-reports: An initial elevation phenomenon. Social Psychological and Personality Science 2023, 14, 727–737. [Google Scholar] [CrossRef]
- Taris, T.W.; Kessler, S.R.; Kelloway, E.K. Strategies addressing the limitations of cross-sectional designs in occupational health psychology: What they are good for (and what not). 2021, 35, 1–5. [Google Scholar] [CrossRef]
- De la Croix, A.; Barrett, A.; Stenfors, T. How todo research interviews in different ways. The clínical teacher 2018, 15, 451–456. [Google Scholar] [CrossRef]
- Redd, T.K.; Doberne, J.W.; Lattin, D.; Yackel, T.R.; Eriksson, C.O.; Mohan, V.; Gold, J.A.; Ash, J.S.; Chiang, M.F. Variability in Electronic Health Record Usage and Perceptions among Specialty vs. Primary Care Physicians. AMIA Annu Symp Proc 2015, 2015, 2053–2062. [Google Scholar]
|
Total participants (n=503) |
Physicians (n=162) |
Nurses (n=341) |
|||||
| Gender | Number | % | Number | % | Number | % | |
| Male | 165 | 32.8 | 93 | 57.4 | 72 | 21.1 | |
| Female | 338 | 67.2 | 69 | 42.6 | 269 | 78.9 | |
| Age (years) | |||||||
| Below 30 | 82 | 16.3 | 40 | 24.7 | 42 | 12.3 | |
| 30 to below 40 | 226 | 44.9 | 59 | 36.4 | 167 | 49 | |
| 40 to below 50 | 122 | 24.3 | 48 | 29.6 | 74 | 21.7 | |
| 50 and above | 73 | 14.5 | 15 | 9.3 | 58 | 17 | |
| Nationality | |||||||
| Saudi | 191 | 38 | 117 | 72.2 | 74 | 21.7 | |
| Non-Saudi | 312 | 62 | 45 | 27.8 | 267 | 78.3 | |
| Position of physicians | |||||||
| Intern | 4 | 0.8 | 4 | 2.5 | - | - | |
| Resident | 69 | 13.7 | 69 | 42.6 | - | - | |
| Fellow | 10 | 2 | 10 | 6.2 | - | - | |
| Specialist | 36 | 7.2 | 36 | 22.2 | - | - | |
| Consultant | 38 | 7.6 | 38 | 23.5 | - | - | |
| General Practitioner | 5 | 1 | 5 | 3.1 | - | - | |
| Primary specialty for physicians | |||||||
| Anaesthesia | 7 | 1.4 | 7 | 4.3 | - | - | |
| Cardiology | 4 | 0.8 | 4 | 2.5 | - | - | |
| Emergency medicine | 5 | 1 | 5 | 3.1 | - | - | |
| Family medicine | 21 | 4.2 | 21 | 13 | - | - | |
| General practitioner | 5 | 1 | 5 | 3.1 | - | - | |
| Intensivist | 4 | 0.8 | 4 | 2.5 | - | - | |
| Internal medicine | 20 | 4 | 20 | 12.3 | - | - | |
| Neurosurgery | 8 | 1.6 | 8 | 4.9 | - | - | |
| OB/Gynaecology | 13 | 2.6 | 13 | 8 | - | - | |
| Ophthalmology | 3 | 0.6 | 3 | 1.9 | - | - | |
| Orthopaedic | 11 | 2.2 | 11 | 6.8 | - | - | |
| Paediatric | 44 | 8.7 | 44 | 27.2 | - | - | |
| Surgery | 17 | 3.4 | 17 | 10.5 | - | - | |
| Position of nurses | |||||||
| Clinical nurse specialist | 82 | 16.3 | - | - | 82 | 24 | |
|
Front line (Direct patient care provider) |
209 | 41.6 | - | - | 209 | 61.3 | |
| Nurse manager/supervisor | 50 | 9.9 | - | - | 50 | 14.7 | |
| Work setting for nurses | |||||||
| Hospital (inpatient) | 159 | 31.6 | - | - | 159 | 46.6 | |
| Hospital (outpatient) | 43 | 8.5 | - | - | 43 | 12.6 | |
| Emergency room (ER) | 35 | 7 | - | - | 35 | 10.3 | |
| Intensive Care Unit (ICU) | 98 | 19.5 | - | - | 98 | 28.7 | |
| Transitional Care Unit (TCU) | 1 | 0.2 | - | - | 1 | 0.3 | |
| Surgical/Operating Room | 29 | 5.8 | - | - | 29 | 8.5 | |
| Primary Healthcare centre | 14 | 2.8 | - | - | 14 | 4.1 | |
| Nursing admin | 9 | 1.8 | - | - | 9 | 2.6 | |
| Burn unit | 1 | 0.2 | - | - | 1 | 0.3 | |
| Neonatal Intensive Care Unit (NICU) | 1 | 0.2 | - | - | 1 | 0.3 | |
| Burn Care Unit (BCU) | 1 | 0.2 | - | - | 1 | 0.3 | |
| Highest level of education certificate in profession | |||||||
| Diploma | 46 | 9.1 | 3 | 1.9 | 43 | 12.6 | |
| Bachelor’s degree | 327 | 65 | 73 | 45.1 | 254 | 74.5 | |
| Master’s degree | 83 | 16.5 | 43 | 26.5 | 40 | 11.7 | |
| Doctorate (PhD or equivalent) | 47 | 9.3 | 43 | 26.5 | 4 | 1.2 | |
| Years of experience in healthcare | |||||||
| Less than 1 year | 16 | 3.2 | 5 | 3.1 | 11 | 3.2 | |
| 1 to less than 5 years | 86 | 17.1 | 53 | 32.7 | 33 | 9.7 | |
| 5 to less than 10 years | 109 | 21.7 | 34 | 21 | 75 | 22 | |
| 10 to less than 20 years | 181 | 36 | 35 | 21.6 | 146 | 42.8 | |
| 20 years and above | 111 | 22.1 | 35 | 21.6 | 76 | 22.3 | |
| Years of experience in healthcare setting utilizing EMR | |||||||
| Less than 1 year | 30 | 6 | 11 | 6.8 | 19 | 5.6 | |
| 1 to less than 5 years | 200 | 39.8 | 80 | 49.4 | 120 | 35.2 | |
| 5 to less than 10 years | 142 | 28.2 | 34 | 21 | 108 | 31.7 | |
| 10 to less than 20 years | 107 | 21.3 | 32 | 19.8 | 75 | 22 | |
| 20 years and above | 24 | 4.8 | 5 | 3.1 | 19 | 5.6 | |
| Region of work | |||||||
| Riyadh | 252 | 50.1 | 101 | 62.3 | 151 | 44.3 | |
| Makkah | 132 | 26.2 | 31 | 19.1 | 101 | 29.6 | |
| Dammam | 119 | 23.7 | 30 | 18.5 | 89 | 26.1 | |
| Question | Total Participant | Physicians | Nurses | |||
| On average, how many hours per Shift/day do you spend using the EMR system? | Number | % | Number | % | Number | % |
| Less than 1 hour | 17 | 3.4 | 4 | 2.5 | 13 | 3.8 |
| 1 - 2 hours | 49 | 9.7 | 23 | 14.2 | 26 | 7.6 |
| 3 - 4 hours | 125 | 24.9 | 61 | 37.7 | 64 | 18.8 |
| 5 – 6 hours | 98 | 19.5 | 43 | 26.5 | 55 | 16.1 |
| More than 6 hours | 214 | 42.5 | 31 | 19.1 | 183 | 53.7 |
| What specific tasks do you use the EMR system for? | ||||||
| Reviewing test results | 372 | 74 | 142 | 87.7 | 230 | 67.4 |
| Documenting patient histories | 348 | 69.2 | 140 | 86.4 | 208 | 61 |
| Patient admission | 319 | 63.4 | 105 | 64.8 | 214 | 62.8 |
| Updating progress notes | 305 | 60.6 | 144 | 88.9 | 161 | 47.2 |
| Nursing notes | 305 | 60.6 | 7 | 4.3 | 298 | 87.4 |
| Nursing initial assessment | 288 | 57.3 | 8 | 4.9 | 280 | 82.1 |
| Discharge process | 285 | 56.7 | 100 | 61.7 | 185 | 54.3 |
| Writing reports | 272 | 54.1 | 114 | 70.4 | 158 | 46.3 |
| Updating treatment plans | 244 | 48.5 | 130 | 80.2 | 114 | 33.4 |
| Communication with other healthcare providers “Request/consultation” | 231 | 45.9 | 118 | 72.8 | 113 | 33.1 |
| Nursing care plan | 228 | 45.3 | 4 | 2.5 | 224 | 65.7 |
| Entering diagnostic data | 203 | 40.4 | 120 | 74.1 | 83 | 24.3 |
| Prescribing medications | 197 | 39.2 | 144 | 88.9 | 53 | 15.5 |
| Other | 19 | 3.8 | 3 | 1.9 | 16 | 4.7 |
| Have you received formal training in using the EMR system? | ||||||
| No | 65 | 12.9 | 34 | 21 | 31 | 9.1 |
| Yes | 438 | 87.1 | 128 | 79 | 310 | 90.9 |
| How many hours of EMR training have you received? | ||||||
| Zero | 65 | 12.9 | 30 | 18.5 | 35 | 10.3 |
| Less than 5 hours | 246 | 48.9 | 88 | 54.3 | 158 | 46.3 |
| 5 - 10 hours | 126 | 25 | 33 | 20.4 | 93 | 27.3 |
| More than 10 hours | 66 | 13.1 | 11 | 6.8 | 55 | 16.1 |
| What are the primary challenges you face when using the EMR system? | ||||||
| Lack of adequate training | 141 | 28 | 73 | 45.1 | 68 | 19.9 |
| Slow system performance | 239 | 47.5 | 64 | 39.5 | 175 | 51.3 |
| System crashes or errors | 169 | 33.6 | 66 | 40.7 | 103 | 30.2 |
| Difficulty navigating the system | 122 | 24.3 | 61 | 37.7 | 61 | 17.9 |
| Time-consuming data entry | 258 | 51.3 | 110 | 67.9 | 148 | 43.4 |
| Lack of user-friendly interface | 123 | 24.5 | 51 | 31.5 | 72 | 21.1 |
| Disrupts workflow | 143 | 28.4 | 54 | 33.3 | 89 | 26.1 |
| Difficulty in communication with other healthcare providers via the EMR | 110 | 21.9 | 44 | 27.2 | 66 | 19.4 |
| Lack of adequate technical support | 157 | 31.2 | 54 | 33.3 | 103 | 30.2 |
| Other | 16 | 3.2 | 5 | 3.1 | 11 | 3.2 |
| ALL | Nurse | Physician | |||||
| Time Category (hour) | Approx. Midpoint (hours /day) | Number | Total hours/day | Number | Total hours/day | Number | Total hours/day |
| <1 | 0.5 | 17 | 8.5 | 13 | 6.5 | 4 | 2 |
| 1–2 | 1.5 | 49 | 73.5 | 26 | 39 | 23 | 34.5 |
| 3–4 | 3.5 | 125 | 437.5 | 64 | 224 | 61 | 213.5 |
| 5–6 | 5.5 | 98 | 539 | 55 | 302 | 43 | 236.5 |
| >6 | 7 | 214 | 1498 | 183 | 1281 | 31 | 217 |
| Position | Work Hours per Day | Work days per Week | Total Work Hours per month | Mean of EMR usage hours per day | Total of EMR usage hours per month | % of EMR usage per month out of the total monthly working hours | P-value |
| Nurses | 12 | 4 | 208 | 5.43 ± 2.03 | 86.80 | 41.73 | 0.001 * |
| Physicians | 12 | 4 | 208 | 4.34 ± 1.87 | 69.44 | 33.38 |
| Odds Ratio | 95 % CI | P-value | |||
| Lower | Upper | ||||
| Gender | Male | Reference Group | |||
| Female | 3.08 | 2.17 | 4.36 | 0.001* | |
| Age | Below 30 | Reference Group | |||
| 30-40 | 1.94 | 0.89 | 2.78 | 0.005* | |
| 40-50 | 1.81 | 1.09 | 3.04 | 0.022* | |
| 50 above | 1.57 | 1.23 | 3.07 | 0.118 | |
| Nationality | Saudi | Reference Group | |||
| Non-Saudi | 2.92 | 2.09 | 1.41 | 0.001* | |
| Position | Physician | Reference Group | |||
| Nurse | 2.98 | 2.12 | 4.20 | 0.001* | |
| Education | Diploma | Reference Group | |||
| Bachelor | 0.69 | 0.39 | 1.27 | 0.241 | |
| Master | 0.50 | 0.25 | 0.99 | 0.047* | |
| Doctorate | 0.28 | 0.14 | 0.61 | 0.001* | |
| Experience | < 1 year | Reference Group | |||
| 1-5 year | 2.66 | 0.99 | 7.19 | 0.053 | |
| 5-10 year | 5.05 | 1.88 | 13.55 | 0.001* | |
| 10-20 year | 5.23 | 1.99 | 13.76 | 0.001* | |
| 20+ year | 4.15 | 1.55 | 11.15 | 0.005* | |
| EMR Experience | < 1 year | Reference Group | |||
| 1-5 year | 1.32 | 0.66 | 2.69 | 0.429 | |
| 5-10 year | 2.13 | 1.03 | 4.41 | 0.041* | |
| 10-20 year | 2.08 | 0.99 | 4.41 | 0.055 | |
| 20+ year | 2.30 | 0.85 | 6.26 | 0.101 | |
| EMR Training | 0 | Reference Group | |||
| < 5 hours | 1.00 | 0.62 | 1.65 | 0.978 | |
| 5-10 hours | 1.55 | 0.92 | 2.76 | 0.095 | |
| 10+ hours | 2.33 | 1.22 | 4.47 | 0.010* | |
| Region | Riyadh | Reference Group | |||
| Makkah | 1.54 | 1.05 | 2.26 | 0.026* | |
| Dammam | 1.08 | 0.72 | 1.64 | 0.690 | |
|
Number (%) |
Number (%) |
Number (%) |
Number (%) |
Number (%) |
Mean ± SD | Mean ± SD | Mean ± SD | ||
| 1. I received adequate training in using EMR | 53 (10.5) | 54 (10.7) | 146 (29) | 174 (34.6) | 76 (15.1) | 3.33 ± 1.17 | 3.04 ± 1.21 | 3.47 ± 1.13 | < 0.001* |
| 2. I always receive immediate support when facing technical issues with the EMR system | 49 (9.7) | 72 (14.3) | 175(34.8) | 152 (30.2) | 55 (10.9) | 3.18 ± 1.11 | 3.01 ± 1.15 | 3.26 ± 1.09 | 0.018* |
| 3. In my opinion, EMR documentation has significantly increased the quality of patient care | 35 (7) | 19 (3.8) | 137(27.2) | 185 (36.8) | 127(25.2) | 3.70 ± 1.1 | 3.91 ± 1.01 | 3.6 ± 1.13 | 0.003* |
| 4. EMR documentation affects my ability to interact with patients directly | 42 (8.3) | 108(21.5) | 157(31.2) | 137 (27.2) | 59 (11.7) | 2.87 ± 1.13 | 2.77 ± 1.23 | 2.92 ± 1.08 | 0.158 |
| 5. Performing tasks on the EMR takes more time compared to direct patient care | 42 (8.3) | 85 (16.9) | 159(31.6) | 131 (26) | 86 (17.1) | 2.73 ± 1.17 | 2.48 ± 1.22 | 2.85 ± 1.13 | 0.001* |
| 6. Utilizing the EMR system for performing tasks has enhanced my job satisfaction | 32 (6.4) | 44 (8.7) | 177(35.2) | 181 (36) | 69 (13.7) | 3.42 ± 1.04 | 3.44 ± 1.05 | 3.41 ± 1.04 | 0.780 |
| 7. I believe that my age affects my ability in using the EMR system | 156 (31) | 152(30.2) | 112(22.3) | 62 (12.3) | 21 (4.2) | 3.72 ± 1.15 | 3.62 ± 1.26 | 3.76 ± 1.1 | 0.186 |
| 8. I believe that my years of experience affect my ability in using the EMR system | 100(19.9) | 156 (31) | 103(20.5) | 98 (19.5) | 46 (9.1) | 3.33 ± 1.25 | 3.09 ± 1.29 | 3.44 ± 1.22 | 0.003* |
| 9. My working position (title) influences the time spent on EMR system (e.g., junior, senior, intern) | 80 (15.9) | 137(27.2) | 125(24.9) | 112 (22.3) | 49 (9.7) | 3.17 ± 1.22 | 2.69 ± 1.3 | 3.4 ± 1.11 | 0.001* |
| 10. My health care setting affects the time spent on EMR system | 52 (10.3) | 100(19.9) | 169(33.6) | 133 (26.4) | 49 (9.7) | 2.95 ± 1.13 | 2.61 ± 1.05 | 3.11 ± 1.13 | 0.001* |
| 11. The time spent using EMR system has a positive impact on my job satisfaction | 36 (7.2) | 70 (13.9) | 166 (33) | 168 (33.4) | 63 (12.5) | 3.30 ± 1.08 | 3.3 ± 1.13 | 3.3 ± 1.06 | 0.933 |
| * Significant p value | |||||||||
| Likert scale with 5 points ; where is 1 strongly disagree, 2 disagree ,3 neutral ,4 agree and 5 strongly agree | |||||||||
| Predictor | β | t | P value |
| Gender | 0.008 | 0.174 | 0.862 |
| Age | 0.054 | 0.788 | 0.431 |
| Nationality | 0.075 | 1.259 | 0.209 |
| Position | 0.163 | 2.877 | 0.004* |
| Education level | 0.038 | 0.744 | 0.457 |
| Years in healthcare | 0.012 | 0.146 | 0.884 |
| EMR experience | –0.033 | –0.621 | 0.535 |
| Work region | –0.110 | –2.401 | 0.017* |
| Hours of EMR training | 0.173 | 3.826 | <0.001* |
|
R² = 0.118, F=7.298, p < 0.001 * Significant p value |
|||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




