Submitted:
04 December 2025
Posted:
04 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Participants
Exclusion Criteria Included
- Atypical disease characteristics
- Previous participation in LSVT BIG
- Use of a duodopa pump or Deep Brain Stimulation
- Cognitive impairment or dementia affecting comprehension or ability to follow program instructions (Mini-Mental State Examination score ≤24) [37]
- Cardiovascular conditions limiting engagement in high-amplitude exercise
2.3. Measurement Outcomes
2.3.1. Balance Assessments
2.3.2. Gait Assessments
2.4. Equipment Required
2.5. Assessors
2.6. Intervention
- Maximal Daily Exercises: Seven multidirectional, high-amplitude full-body exercises performed repetitively, with two in a seated position and five standing.
- Functional Component Tasks: Five functional activities, including a standard sit-to-stand task and four individualized exercises tailored to each patient’s daily life and goals, based on clinical evaluation.
- Hierarchy Tasks: One to three complex, multilevel tasks progressively increased in difficulty over the four-week program, customized to each patient’s real-life goals and interests.
- BIG Walking: Gait training emphasizing increased step length, arm swing, posture, and walking speed.
- Carryover Assignment: Activities assigned to patients to integrate BIG movements into real-world conditions.
- Homework: Daily independent practice of “Maximal Daily Exercises,” “Functional Component Tasks,” and “Hierarchy Tasks” outside supervised sessions.
2.7. Experimental Procedure
2.8. Data Analysis
3. Results
3.1. Patient Characteristics
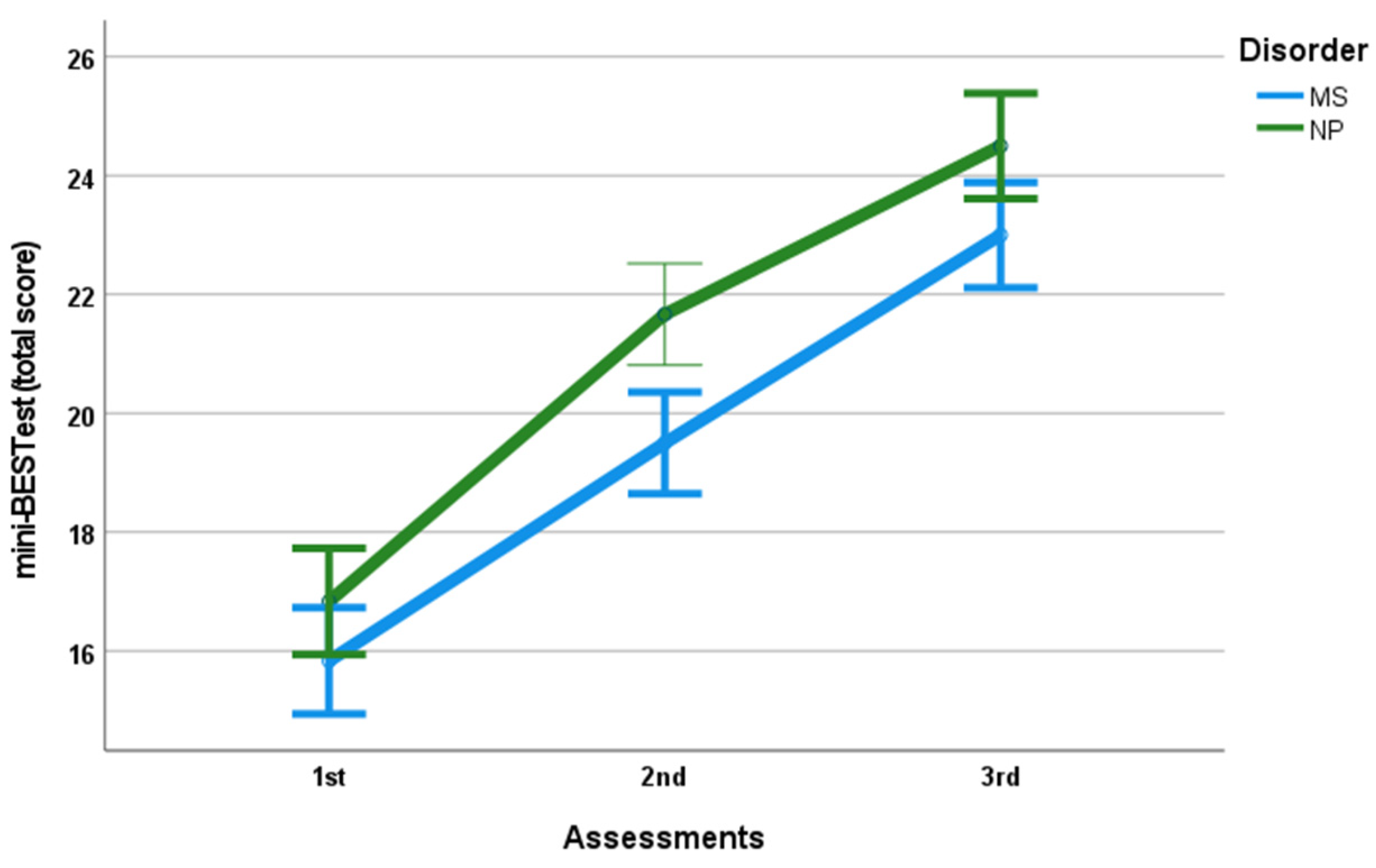
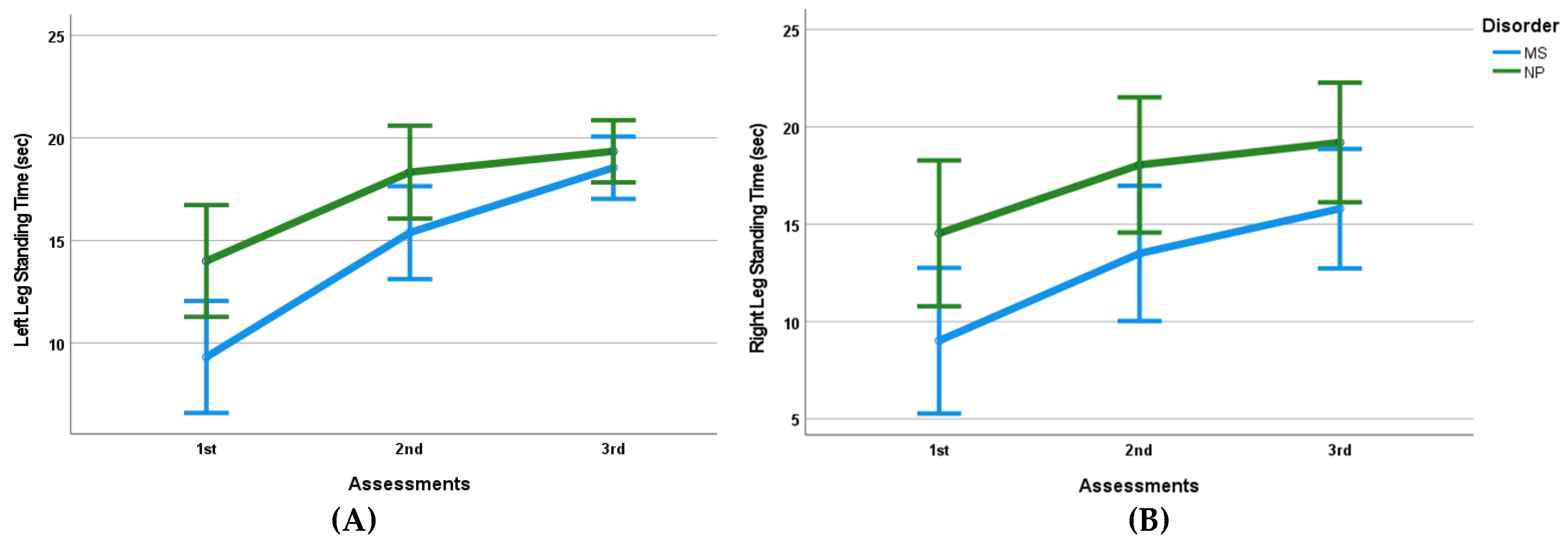
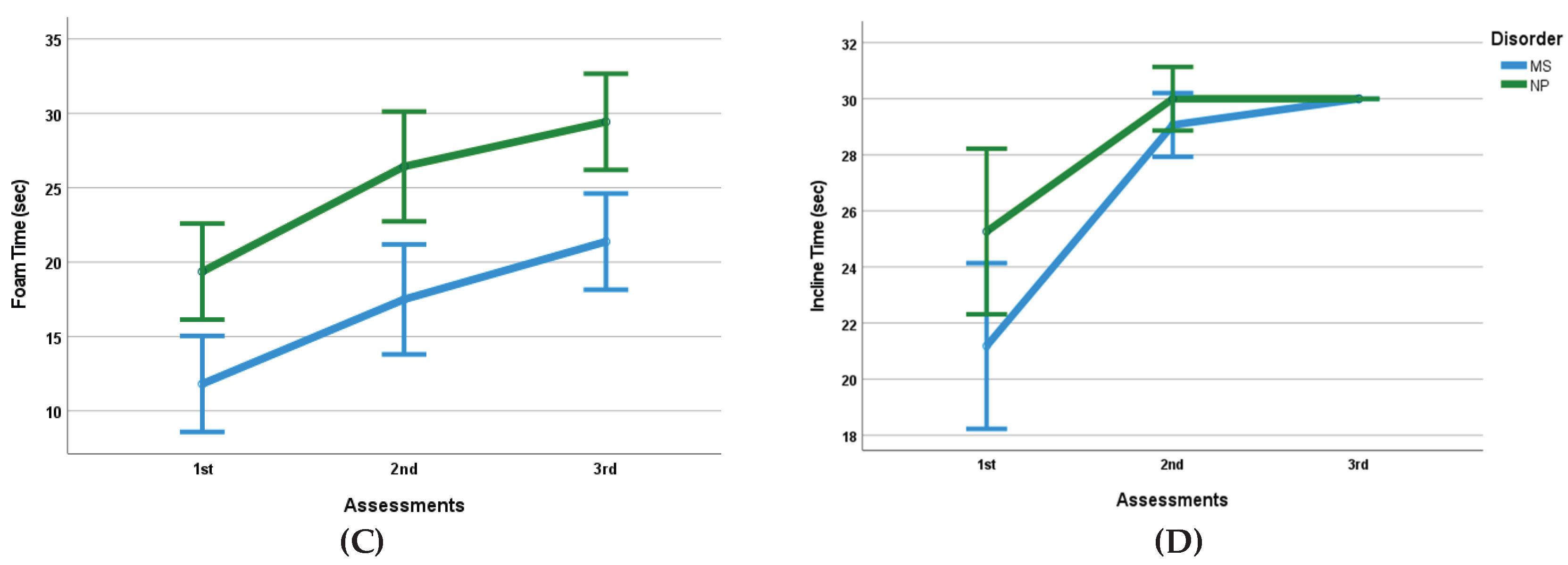
3.2. Balance
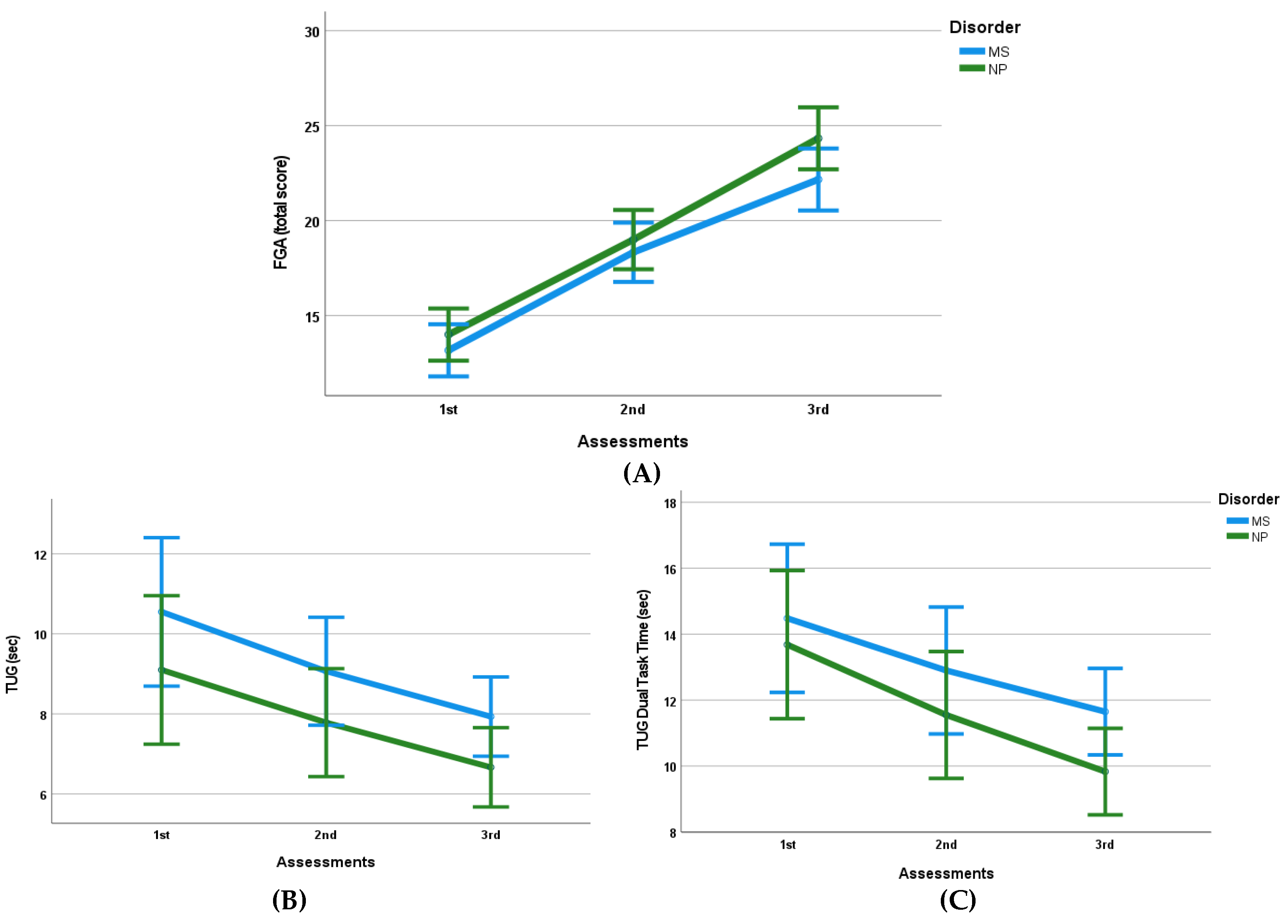
3.3. Gait Assessment
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Pu, T.; Huang, M.; Kong, X.; Wang, M.; Chen, X.; Feng, X.; Wie, C.; Wenig, X.; Xu, F. Lee Silverman Voice Treatment to improve speech in Parkinson’s disease: A systemic review and meta-analysis. Parkinson’s Dis. 2021, 2021, e3366870. [CrossRef]
- Bryans, L.A.; Palmer, A.D.; Anderson, S.; Schindler, J.; Graville, D.J. The Impact of Lee Silverman Voice Treatment (LSVT LOUD®) on Voice, Communication, and Participation: Findings from a Prospective, Longitudinal Study. J Commun Disord. 2020, 89, 106031. [CrossRef]
- Ebersbach, G.; Ebersbach, A.; Edler, D.; Kaufhold, O.; Kusch, M.; Kupsch, A.; Wissel, J. Comparing exercise in Parkinson’s disease-the Berlin BIG Study. Mov. Dis. 2010, 25(12), 1902-1908. [CrossRef]
- Fox, C.; Ebersbach, G.; Ramig, L.; Sapir, S. LSVT LOUD and LSVT BIG: Behavioral Treatment Programs for Speech and Body Movement in Parkinson Disease. Parkinson’s Dis. 2012, 2012, 1-12. [CrossRef]
- Farley, B.G.; Fox, C.M.; Ramig, L.O. McFarland, DH. Intensive Amplitude-specific Therapeutic Approaches for Parkinsonʼs Disease. Top. Geriatr. Rehabil. 2008, 24(2), 99-114. [CrossRef]
- Peterka, M.; Odorfer, T.; Schwab, M.; Volkmann, J.; Zeller, D. LSVT-BIG therapy in Parkinson’s disease: physiological evidence for proprioceptive recalibration. BMC Neurol. 2020, 20(1), 276. [CrossRef]
- Konczak, J.; Krawczewski, K.; Tuite, P.; Maschke, M. The perception of passive motion in Parkinson’s disease. J. Neurol. 2007, 254(5), 655-663. [CrossRef]
- Conte, A.; Khan, N.; Defazio, G.; Rothwell, J.C.; Berardelli, A. Pathophysiology of somatosensory abnormalities in Parkinson disease. Nat. Rev. Neuro. 2013, 9(12), 687-697. [CrossRef]
- Matsuno, A.; Matsushima, A.; Saito, M.; Sakurai, K.; Kobayashi, K.; Yoshiki, S. Quantitative assessment of the gait improvement effect of LSVT BIG® using a wearable sensor in patients with Parkinson’s disease. Heliyon. 2023, 9(6), e16952-e16952. [CrossRef]
- Janssens, J.; Malfroid, K.; Nyffeler, T.; Bohlhalter, S.; Vanbellingen, T. Application of LSVT BIG Intervention to Address Gait, Balance, Bed Mobility, and Dexterity in People with Parkinson Disease: A Case Series. Phys. Ther. 2014, 94(7), 1014-1023. [CrossRef]
- Clarkin, C. LSVT®BIG Exercise-Induced Neuroplasticity in People with Parkinson’s Disease: An Assessment of Physiological and Behavioral Outcomes. Open Access Dissertations. University of Rhode Island, ProQuest Number: 27741888, 2020. [CrossRef]
- Flood, M.W.; O’Callaghan, B.P.F.; Diamond, P.; Liegey, J.; Hughes, G.; Lowery, M.M. Quantitative clinical assessment of motor function during and following LSVT-BIG® therapy. J Neuroeng Rehabil. 2020, 17(1), 92. [CrossRef]
- Doucet, B. M.; Blanchard, M.; Franc, I. Effects of LSVT BIG® on Bradykinesia During Activities of Daily Living. OTJR: Occupational Therapy Journal of Research. 2025, 0(0) 15394492251367275. [CrossRef]
- Sadaghiani, Z.; Tahan, N.; Ganjeh, S.; Baghban, A.A.; Khoshdel, A.; Shoeibi, A. Evaluating the Impact of Adding Lee Silverman Voice Treatment BIG into Routine Physiotherapy on Both Motor and Nonmotor Functions in Individuals with Parkinson’s Disease. Dubai Medical Journal, 2025, 8(1), 12–22. [CrossRef]
- McDonnell, M.N.; Rischbieth, B.; Schammer, T.T.; Seaforth, C.; Shaw, A.J.; Phillips, A.C. Lee Silverman Voice Treatment (LSVT)-BIG to improve motor function in people with Parkinson’s disease: a systematic review and meta-analysis. Clin. Rehabil. 2017, 32(5), 607-618. [CrossRef]
- Kim, D.Y.; Oh, H.M.; Bok, S.K.; Chang, W.H.; Choi, Y.; Chun, M.H.; Han, S.J.; Han, T.R.; Jee, S.; Jung, S.H.; Jung, H.Y.; Jung, T.D.; Kim, M.W.; Kim, E.J.; Kim, H.S.; Kim, Y.H.; Kim, Y.; Kim, D.Y.; Kim, D.Y.; Kim, D.K.; Ko, S.H.; Ko, M.H.; Lee, J.K.; Lee, J.; Lee, S.J.; Lee, S.G.; Lim, S.H.; Oh, B.M.; … Yang, S.N.; Yoo S.D.; Yoo, W.K. KSNR Clinical Consensus Statements: Rehabilitation of Patients with Parkinson’s Disease. Brain Neurorehabil. 2020, 13(2), e17. [CrossRef]
- Kantarci, O.; Wingerchuk, D. Epidemiology and natural history of multiple sclerosis: new insights. Cur. Opin. Neurol. 2006, 19(3), 248-254. [CrossRef]
- Amatya, B.; Khan, F.; Galea, M. Rehabilitation for people with multiple sclerosis: an overview of Cochrane Reviews. Cochrane Database Syst Rev. 2019, 14, 1(1), CD012732. [CrossRef]
- Kelleher, K.J.; Spence, W.; Solomonidis, S.; Apatsidis, D. The characterisation of gait patterns of people with multiple sclerosis. Disabil. Rehabil. 2010, 32(15), 1242-1250. [CrossRef]
- Beer, S.; Khan, F.; Kesselring, J. Rehabilitation interventions in multiple sclerosis: an overview. J. Neurol. 2012, 259(9), 1994-2008. [CrossRef]
- Barin, L.; Salmen, A.; Disanto, G.; Babačić, H.; Calabrese, P.; Chan, A.; Kamm, C.P.; Kesselring, J.; Kuhle, J.; Gobbi, C.; Pot, C.; Puhan, M.A.; von Wyl, V.; Swiss Multiple Sclerosis Registry (SMSR). The disease burden of Multiple Sclerosis from the individual and population perspective: Which symptoms matter most? Mult Scler Relat Disord. 2018, 25, 12-121. [CrossRef]
- Hamilton, F.; Rochester, L.; Paul, L.; Rafferty, D.; O’Leary, C.; Evans, J. Walking and talking: an investigation of cognitive—motor dual tasking in multiple sclerosis. Mult. Scler. J. 2009, 15(10), 1215-1227. [CrossRef]
- White, L.J.; McCoy, S.C.; Castellano, V.; Gutierrez, G.; Stevens, J.E.; Walter, G.A.; Vandenborne, K. Resistance training improves strength and functional capacity in persons with multiple sclerosis. Mult. Scler. J. 2004, 10(6), 668-674. [CrossRef]
- Sandoval, AEG. Exercise in Multiple Sclerosis. Phys Med Rehabil Clin N Am 2013, 24(4), 605-618. [CrossRef]
- Feltham, M.G.; Collett, J.; Izadi, H.; Wade, D.T.; Morris, M.G.; Meaney, A.J.; Howells, K.; Sackley, C.; Dawes, H. Cardiovascular adaptation in people with multiple sclerosis following a twelve week exercise programme suggest deconditioning rather than autonomic dysfunction caused by the disease. Results from a randomized controlled trial. Eur J Phys Rehabil Med. 2013, 49(6), 765-774.
- Halabchi, F.; Alizadeh, Z.; Sahraian, M.A.; Abolhasani, M. Exercise prescription for patients with multiple sclerosis; potential benefits and practical recommendations. BMC Neurol. 2017, 17(1), 185. [CrossRef]
- Duff, W.R.D.; Andrushko, J.W.; Renshaw, D.W.; Chilibeck, P.D.; Farthing, J.P.; Danielson, J.; Evans, C.D.; Impact of Pilates Exercise in Multiple Sclerosis. Int J MS Care. 2018, 20(2), 92-100. [CrossRef]
- Kalron, A.; Rosenblum, U.; Frid, L.; Achiron, A. Pilates exercise training vs. physical therapy for improving walking and balance in people with multiple sclerosis: a randomized controlled trial. Clin. Rehabil. 2016, 31(3), 319-328. [CrossRef]
- Soysal, Tomruk, M.; Zu, M.Z.; Kara, B.; İdiman, E. Effects of Pilates exercises on sensory interaction, postural control and fatigue in patients with multiple sclerosis. Mult Scler Relat Disord. 2016, 7, 70-73. [CrossRef]
- Alphonsus, K.B.; Su, Y.; D’Arcy, C. The effect of exercise, yoga and physiotherapy on the quality of life of people with multiple sclerosis: Systematic review and meta-analysis. Complement Ther Med. 2019, 43, 188-195. [CrossRef]
- Taylor, E.; Taylor-Piliae, R.E. The effects of Tai Chi on physical and psychosocial function among persons with multiple sclerosis: A systematic review. Complement Ther Med. 2017, 31, 100-108. [CrossRef]
- Duan, H.; Jing, Y.; Li, Y.; Lian, Y.; Li, J.; Li, Z. Rehabilitation treatment of multiple sclerosis. Front Immunol. 2023, 14, 1168821. [CrossRef]
- Baldanzi, C.; Crispiatico, V.; Foresti, S.; Groppo, E.; Rovaris, M.; Cattaneo, D.; Vitali, C. Effects of Intensive Voice Treatment (The Lee Silverman Voice Treatment [LSVT LOUD]) in Subjects With Multiple Sclerosis: A Pilot Study. J. Voice. 2022, 36(4), 585.e1-585.e13. [CrossRef]
- Metcalfe, V.; Egan, M.; Sauvé-Schenk, K. LSVT BIG in late stroke rehabilitation: A single-case experimental design study. Can. J. Occup. Ther. 2019, 86, 87–94. [CrossRef]
- Proffitt, R.M.; Henderson, W.; Scholl, S.; Nettleton, M. Lee Silverman Voice Treatment BIG® for a Person With Stroke. Am J Occup Ther. 2018, 72(5), 7205210010p1-7205210010p6. [CrossRef]
- Proffitt, R.; Henderson, W.; Stupps, M.; Binder, L.; Irlmeier, B.; Knapp E. Feasibility of the Lee Silverman voice treatment-BIG intervention in stroke. OTJR Occup. Particip. Health. 2021, 41, 40–46. [CrossRef]
- Fiorenzato, E.; Cauzzo,S.; Weis, L.; Garon, M.; Pistonesi, F.; Cianci, V.; Nasi, L.M.; Vianello, F.; Zecchinelli, L.A.; Pezzoli, G.; Reali, E.; Pozzi, Β.; Isaias, U.I.; Siri, C.; Santangelo, G.; Cuoco, S.; Barone, P.; Antonini, A.; Biundo, R. Optimal MMSE and MoCA cutoffs for cognitive diagnoses in Parkinson's disease: A data-driven decision tree model. J. Neurol. Sci. 2024, 466, 123283. [CrossRef]
- Franchignoni, F.; Horak, F.; Godi, M.; Nardone, A.; Giordano, A. Using psychometric techniques to improve the Balance Evaluation Systems Test: The mini-BESTest. J. Rehabil. Med. 2010, 42, 323–331. [CrossRef]
- Lampropoulou, S.I.; Billis, E.; Gedikoglou, I.A.; Michailidou, C.; Nowicky, A.V.; Skrinou, D.; Michailidi, F.; Chandrinou, D.; Meligkoni, M. Reliability, validity and minimal detectable change of the Mini-BESTest in Greek participants with chronic stroke. Physiother. Theory Pract. 2019, 35, 171–182. [CrossRef]
- Jacobs, J.V.; Horak, F.B.; Tran, V.K.; Nutt, J.G. Multiple balance tests improve the assessment of postural stability in subjects with Parkinson's disease. J Neurol Neurosurg Psychiatry 2006, 77(3), 322-326. [CrossRef]
- Wrisley, D.M.; Marchetti, G.F.; Kuharsky, D.K.; Whitney, S.L. Reliability, internal consistency, and validity of data obtained with the functional gait assessment. Phys Ther. 2004, 84(10), 906-18.
- Lampropoulou, S.; Kellari, A.; Gedikoglou, I.A.; Kozonaki, D.G.; Nika, P.; Sakellari, V. Cross-Cultural Adaptation and Psychometric Characteristics of the Greek Functional Gait Assessment Scale in Healthy Community-Dwelling Older Adults. Appl. Sci., 2024, 14(2), 520. [CrossRef]
- Beauchet, O.; Fantino, B.; Allali, G.; Muir, S.W.; Montero-Odasso, M.; Annweiler, C. Timed Up and Go test and risk of falls in older adults: a systematic review. J Nutr Health Aging 2011 15(10), 933-8. [CrossRef]
- Barry, E. Galvin, R.; Keogh, C.; Horgan, F.; Fahey, T. Is the Timed Up and Go test a useful predictor of risk of falls in community dwelling older adults: a systematic review and meta-analysis. BMC Geriatr. 2014, 14, 14. [CrossRef]
- Kahya, M.; Moon, S.; Ranchet, M.; Vukas, R.R.; Lyons, E.K.; Pahwa, R.; Akinwuntan, A.; Devos H. Brain activity during dual task gait and balance in aging and age-related neurodegenerative conditions: A systematic review. Exp Gerontol. 2019, 128, 110756. [CrossRef]
- Isaacson, S.; O’Brien, A.; Lazaro, J.D.; Ray, A.; Fluet, G. The JFK BIG study: the impact of LSVT BIG® on dual task walking and mobility in persons with Parkinson’s disease. J Phys Ther Sci. 2018, 30(4), 636-641. [CrossRef]
- Fishel, S.C.; Hotchkiss, M.E.; Brown, S.A. The impact of LSVT BIG therapy on postural control for individuals with Parkinson disease: A case series. Physiother Theory Pract. 2020, 36(7), 834-843. [CrossRef]
- Luna, G.; Pardo-Cocuy, .LF.; Garzón, A.; Benítez, A.; Parada-Gereda, H.M. Effectiveness of Lee Silverman Voice Treatment (LSVT®BIG) for improving motor function in patients with Parkinson's disease: a systematic review and meta-analysis of randomised clinical trials. Am J Phys Med Rehabil. 2025, 104(12), 1105-1112. [CrossRef]
- Boissoneault, C.; Datta, S.; Rose, D.K.; Waters, M.J.; Khanna, A.; Daly, J.J. Innovative Long-Dose Neurorehabilitation for Balance and Mobility in Chronic Stroke: A Preliminary Case Series. Brain Sci. 2020, 10(8), 555. [CrossRef]
- Corrini, C.; Gervasoni, E.; Perini, G.; et al. Mobility and balance rehabilitation in multiple sclerosis: A systematic review and dose-response meta-analysis. Mult Scler Relat Disord. 2023, 69, 104424. [CrossRef]
- Zemková, E.; Hamar, D. The Effect of Task-Oriented Sensorimotor Exercise on Visual Feedback Control of Body Position and Body Balance, Hum. Mov. 2010, 11(2): 119-123. [CrossRef]
- Asghari, S.H.; Ilbeigi, S.; Ahmadi, M.M.; Yousefi, M.; Mousavi-Mirzaei, M. Comparative effects of sensory motor and virtual reality interventions to improve gait, balance and quality of life MS patients. Sci Rep. 2025, 15(1). [CrossRef]
- Petzinger, G.M.; Fisher, B.E.; McEwen, S.; Beeler, J.A.; Walsh, J.P.; Jakowec, M.W. Exercise-enhanced neuroplasticity targeting motor and cognitive circuitry in Parkinson’s disease. Lancet Neurol. 2013, 12(7), 716-26. [CrossRef]
- Procházková, M.; Tintera, J.; Špaňhelová, S.; Prokopiusova, T.; Rydlo, J.; Pavlikova, M.; Prochazka, A.; Rasova, K. Brain activity changes following neuroproprioceptive “facilitation, inhibition” physiotherapy in multiple sclerosis: a parallel group randomized comparison of two approaches. Eur J Phys Rehabil Med. 2021, 57(3), 356-365. [CrossRef]
- Tavazzi, E.; Cazzoli, M.; Pirastru, A.; Blasi, V.; Rovaris, M.; Bergsland, N.; Baglio, F. Neuroplasticity and Motor Rehabilitation in Multiple Sclerosis: A Systematic Review on MRI Markers of Functional and Structural Changes. Front Neurosci. 2021, 15, 707675. [CrossRef]
- Straudi, S.; Martinuzzi, C.; Pavarelli, C.; Sabbagh Charabati, A.; Benedetti, M.G.; Foti, C.; Bonato, M.; Zancato, E.; Basaglia, N. A task-oriented circuit training in multiple sclerosis: a feasibility study. BMC Neurol. 2014, 14, 124. [CrossRef]
- Darwish, H.M.; Shalaby, M.N.; Ali, S.A.; Soubhy, Z.H. Effect of Task Oriented Approach on Balance in Ataxic Multiple Sclerosis Patients. Med. J. Cairo Univ. 2019, 87 (7), 4789-4794. [CrossRef]
- Salmani, S., Mousavi, S.H., Navardi, S.; Hosseinzadeh, F.; Pashaeypoor, S. The barriers and facilitators to health-promoting lifestyle behaviors among people with multiple sclerosis during the coronavirus disease 2019 pandemic: a content analysis study. BMC Neurol. 2022, 22 (1), 490. [CrossRef]
- Bombard, Y., Baker, G.R., Orlando, E.; Fancott, C.; Bhatia, P.; Casalino, S.; Onate, K.; Denis J.L.; Pomey M.P. Engaging patients to improve quality of care: a systematic review. Implementation Sci. 2018, 13, 98. [CrossRef]
- Maddocks, M.; Fettes, L.; Takemura, N.; Bayly, J.; Talbot-Rice, H.; Turner, K.; Tiberini, R.; Harding, R.; Murtagh E.M.F.; Siegert, R.J.; Higginson, I.J.; Ashford, S.A.; Turner-Stokes L. Functional goals and outcomes of rehabilitation within palliative care: a multicentre prospective cohort study. BMC Palliat Care. 2025, 24(1), 172. [CrossRef]
- Metcalfe, V.; Egan, M.; Sauvé-Schenk K. LSVT BIG in late stroke rehabilitation: A single-case experimental design study. Can J Occup Ther. 2019, 86(2), 87-94. [CrossRef]
- Bouça-Machado, R.; Rosário, A.; Caldeira, D.; Castro Caldas, A.; Guerreiro, D.; Venturelli, M.; Tinazzi, M.; Schena, F.; Ferreira J. Physical Activity, Exercise, and Physiotherapy in Parkinson's Disease: Defining the Concepts. Mov Disord Clin Pract. 2019, 7(1), 7-15. [CrossRef]
- Li, P.; He, Y.; He, M. The comprehensive impact of exercise interventions on cognitive function and quality of life in alzheimer’s disease patients: a systematic review and meta-analysis. BMC Geriatr. 2025 25, 871. [CrossRef]
- Paltamaa, J.; Sjögren, T.; Peurala, S.; Heinonen, A. Effects of physiotherapy interventions on balance in multiple sclerosis: A systematic review and meta-analysis of randomized controlled trials. J Rehabil Med. 2012, 44(10), 811-23. [CrossRef]
- Snook, E.M.; Motl, R.W. Effect of Exercise Training on Walking Mobility in Multiple Sclerosis: A Meta-Analysis. Neurorehabil. Neural Repair. 2008, 23(2), 108-116. [CrossRef]
- Liu, Y.C.; Yang, Y.R.; Tsai, Y.A.; Wang, R.Y. Cognitive and motor dual task gait training improve dual task gait performance after stroke - A randomized controlled pilot trial. Sci Rep. 2017, 7(1), 4070. [CrossRef]
- Comber, L.; Peterson, E.; O'Malley, N.; Galvin, R.; Finlayson, M.; Coote, S. Development of the Better Balance Program for People with Multiple Sclerosis: A Complex Fall-Prevention Intervention. Int J MS Care. 2021, 23(3), 119-127. [CrossRef]
| Variables |
MS.2 Group Mean (SD) 1 |
PD 3 Group Mean (SD) 1 |
P Value |
| N 4 | 6 | 6 | NA |
| Sex (W: M) 5 | 5W: 1M | 6M | NA |
| Age | 45±8 | 68±3 | NA |
| Mini-BESTest 6 | 15.83±0,98 | 16.83±0.98 | p>0.05 |
| FGA 7 | 13.2±1.6 | 14±1.4 | p>0.05 |
| TUG 8 | 10.5±2.7 | 9.1±0.9 | p>0.05 |
| Variables | MS.2 Group - Mean (SD) 1 | PD 3 Group - Mean (SD) 1 | ||||
| 1st ass/nt 4 | 2nd ass | 3rd ass | 1st ass | 2nd ass | 3rd ass | |
| mini-BESTest (from total score/28) | 15.83 (0.98) | 19.50 (0.84)* | 23.00 (0.89)* | 16.83 (0.98) | 21.67 (1.03)* | 24.50 (1.05)* |
| R leg standing time (sec) | 9.02 (4.68) | 13.50 (5.04)* | 15.80 (4.54)* | 14.53 (3.46) | 18.05 (1.94)* | 19.20 (1.49)* |
| L leg standing time (sec) | 9.32 (3.40) * | 15.38 (3.16)* | 18.55 (2.09)* | 14.00 (2.54) | 18.33 (1.55)* | 19.35 (1.09)* |
| Foam standing time (sec) | 11.82 (4.11) * | 17.50 (5.27) * | 21.38 (4.94) * | 19.37 (2.87) * | 26.43 (2.27) * | 29.43 (0.91) * |
| Incline Standing Time (sec) | 21.18 (2.65) * | 29.07 (1.76)* | 30.00 (0.00)* | 25.27 (3.75)* | 30.00 (0.00) * | 30.00 (0.00) * |
| FGA (from total score/30) | 13.17 (1.60) | 18.33 (2.34)* | 22.17 (2.04)* | 14.00 (1.41) | 19.00 (0.63)* | 24.33 (1.50)* |
| TUG (sec) | 10.55 (2.73) | 9.07 (1.76)* | 7.93 (1.49)* | 9.10 (0.92) | 7.78 (1.14)* | 6.66 (0.37)* |
| Variables | Group | N 1 | Mean Difference ± SD2 | Leven’s Test |
| miniBEST 3 | MS 4 | 6 | 7.17 ± 0.98 | t9.976= -0.859, p>0.05 |
| NP 5 | 6 | 7.67±1.03 | ||
| TUG 6 | MS | 6 | 2.617±1.60 | t7.200= 0.253, p>0.05 |
| NP | 6 | 2.433±0.77 | ||
| TUGdual 7 | MS | 6 | 2.833±2.00 | t9.337= 0.986, p>0.05 |
| NP | 6 | 3.850±1.53 | ||
| FGA 8 | MS | 6 | 9.00±1.26 | t8.805= -1.451, p>0.05 |
| NP | 6 | 10.33±1.86 | ||
| Foam 9 | MS | 6 | 9.577±1.33 | t7.902= -0.451, p>0.05 |
| NP | 6 | 10.067±2.36 | ||
| Incline 10 | MS | 6 | 8.817±2.64 | t8.988= 2.178, p>0.05 |
| NP | 6 | 4.733±3.75 | ||
| RLegStand 11 | MS | 6 | 6.783±3.24 | t9.351= 1.270, p>0.05 |
| NP | 6 | 4.667±2.47 | ||
| LLegStand 12 | MS | 6 | 9.233±2.19 | t9.498= 3.411, p=0.007 |
| NP | 6 | 5.35±1.73 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




