Submitted:
01 December 2025
Posted:
02 December 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Search Strategy
2.3. Eligibility Criteria
- Population: preterm infants (<37 weeks of gestation) with a medical diagnosis of RDS or BPD.
- Intervention: any respiratory physiotherapy technique or modality.
- Study design: randomized controlled trials.
- Publication period: January 2014 to January 2025.
- Language: English or Spanish.
- Preterm infants presenting major comorbidities (e.g., congenital malformations, genetic syndromes, significant cardiovascular abnormalities).
- Studies for which full-text access was not available.
2.4. Study Selection and Data Extraction
2.5. Quality Assessment
2.6. Use of Generative Artificial Intelligence
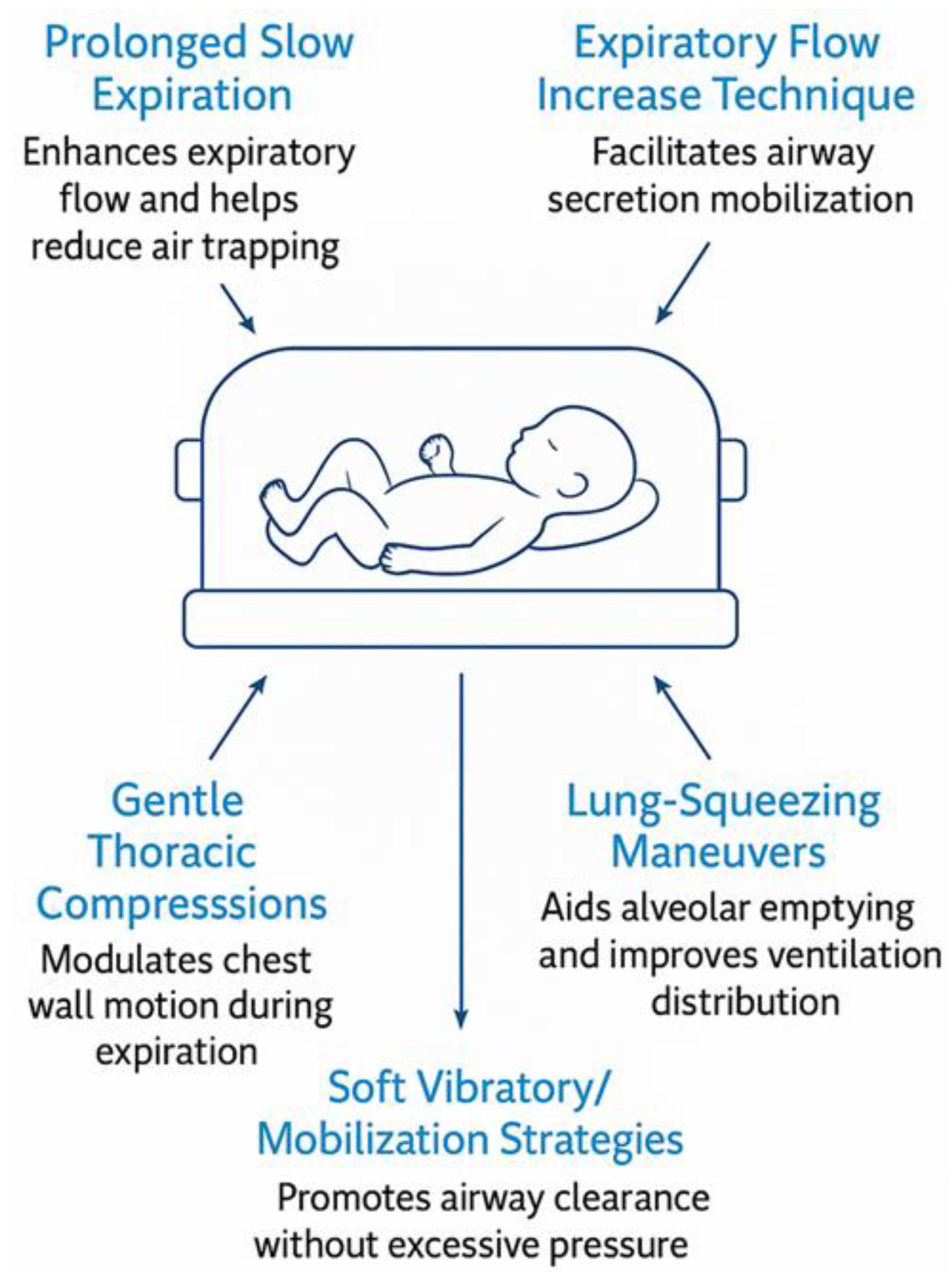
3. Manual Techniques for Enhancing Ventilatory Mechanics and Expiratory Flow
4. Positioning and Postural Management in Respiratory Support
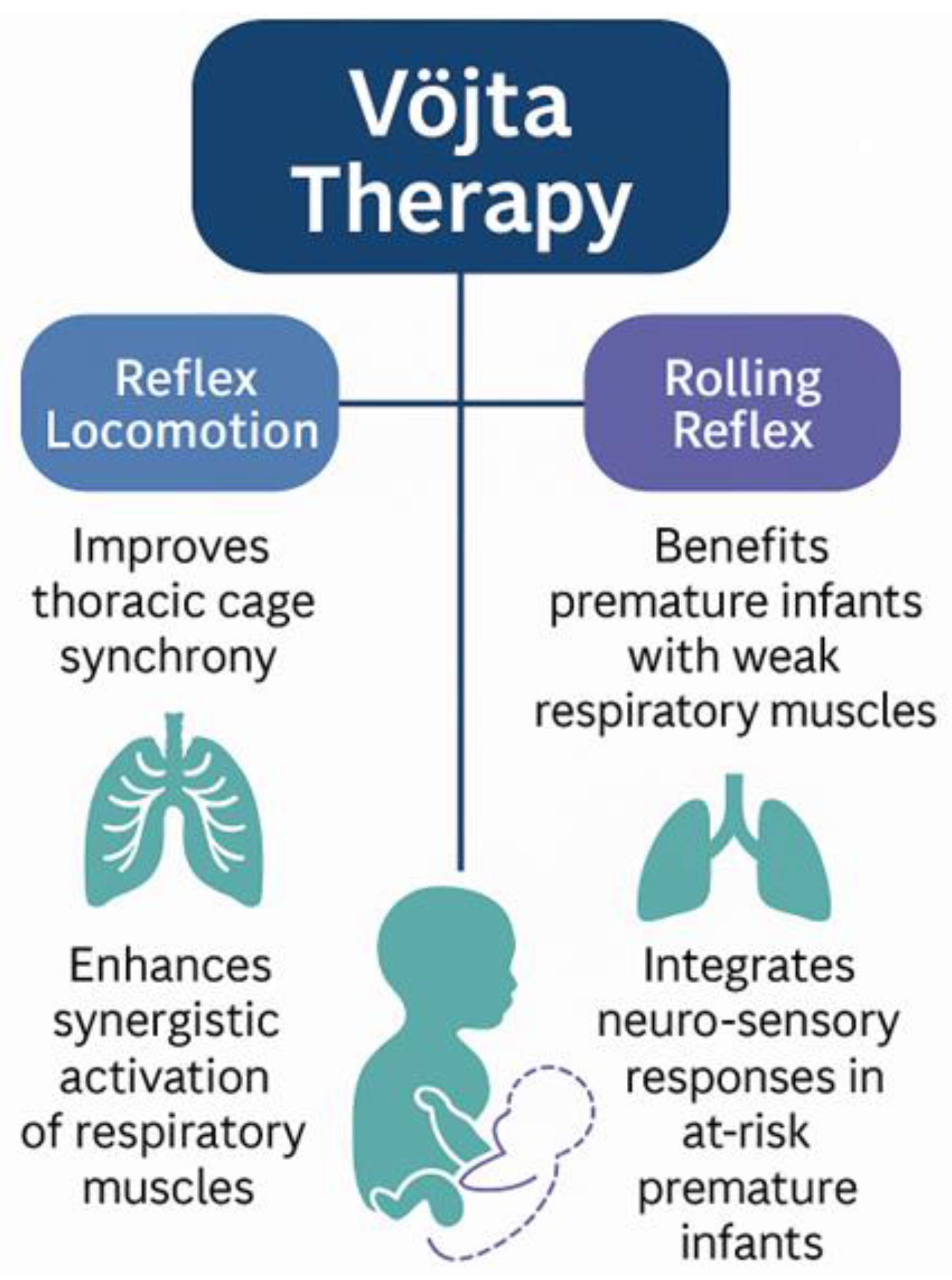
5. Reflex-Based and Neurodevelopmental Approaches
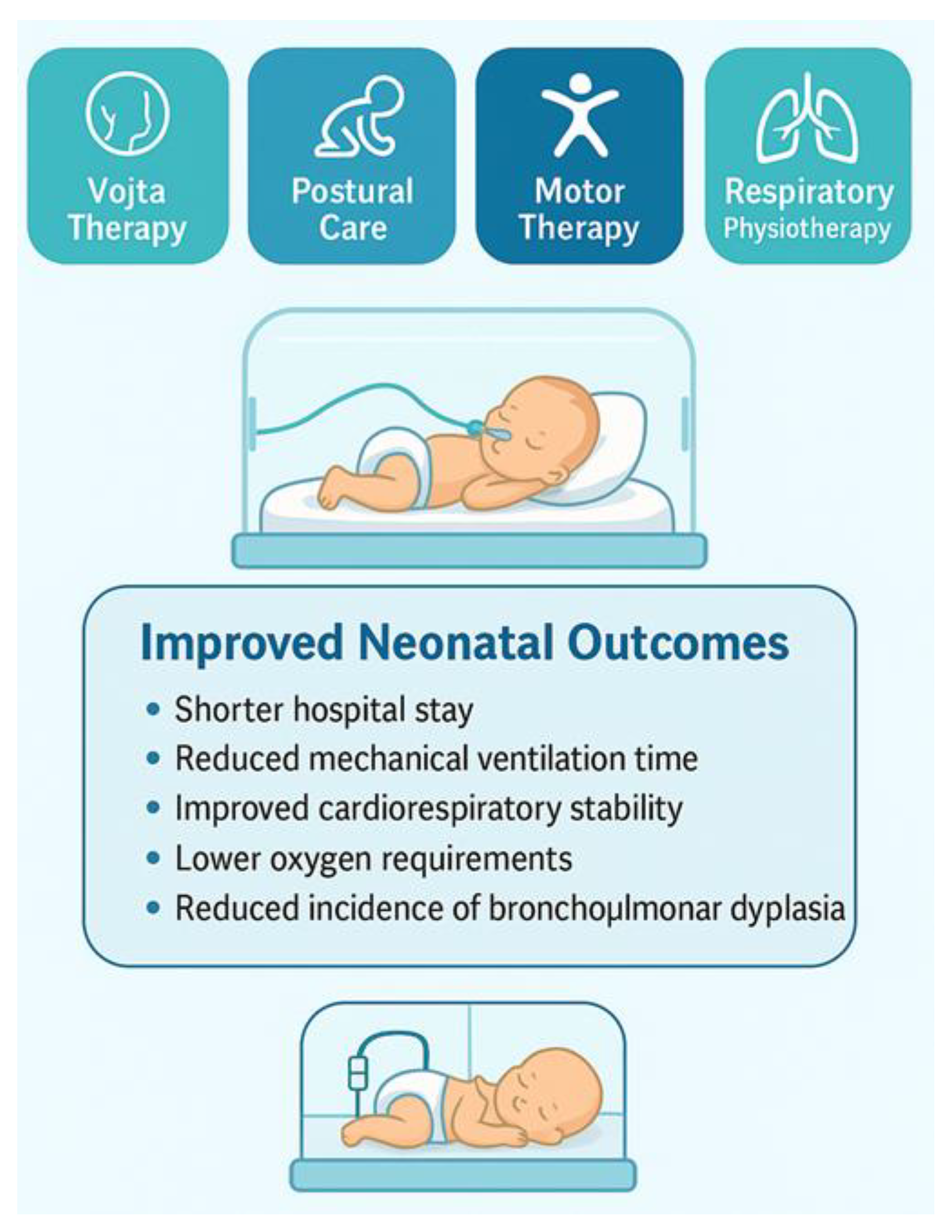
6. Multimodal Rehabilitation Strategies Integrating Respiratory, Postural and Motor Components
7. Synthesis of Evidence Across Respiratory Physiotherapy Modalities
7.1. Immediate Physiological Benefits
- Increases in SpO₂ (14–20, 22)
- Reductions in RR and improved heart rate stability (16–18)
- Better breath sounds and improved auscultatory findings (14, 20)
- Improved respiratory support parameters
- Faster radiological resolution of atelectasis (14, 20)
- Decreased FiO₂ requirements (19, 22)
- Enhanced ventilatory patterns in ventilated preterm infants (15, 17)
7.2. Medium- to Long-Term Clinical Improvements in Multimodal Programs
- Decreased hospitalization duration (13, 21, 23)
- Reduced mechanical ventilation days (13, 23)
- Lower incidence of BPD in one comprehensive intervention trial [21]
7.3. Safety
8. Discussion
8.1. Limitations
8.2. Clinical Implications
9. Conclusions
10. Future Directions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| MDPI | Multidisciplinary Digital Publishing Institute |
| DOAJ | Directory of open access journals |
| TLA | Three letter acronym |
| LD | Linear dichroism |
References
- Ohuma EO, Moller A-B, Bradley E, Chakwera S, Hussain-Alkhateeb L, Lewin A, et al. National, regional, and global estimates of preterm birth in 2020, with trends from 2010: a systematic analysis. Lancet. 2023;402(10409):1261–71. [CrossRef]
- World Health Organization. Newborn mortality: Key facts [Internet]. Geneva: WHO; 2024 [consulted 12 May 2025]. Available from: https://www.who.int/news-room/fact-sheets/detail/newborn-mortality.
- Barreto MGP, Manso MC, Barreto RP, Barreto RP, Vasconcelos LMT, Silva C. Frequency and Risk Factors Associated with Prematurity: A Cohort Study in a Neonatal Intensive Care Unit. J Clin Med. 2024;13:4437.
- Yadav S, Lee B. Neonatal respiratory distress syndrome. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.
- Kalikkot Thekkeveedu R, Guaman MC, Shivanna B. Bronchopulmonary dysplasia: A review of pathogenesis and pathophysiology. Respir Med. 2017;132:170–7. [CrossRef]
- Igual-Blasco A, Piñero-Peñalver J, Fernández-Rego FJ, Torró-Ferrero G, Pérez-López J. Effects of chest physiotherapy in preterm infants with respiratory distress syndrome: a systematic review. Healthcare (Basel). 2023;11(8):1091. [CrossRef]
- Tana M, Bottoni A, Cota F, Papacci P, Di Polito A, Campagnola B, et al. Respiratory physiotherapy versus an individualized postural care program for reducing mechanical ventilation in preterm infants: a randomised controlled trial. Trials. 2021;22(1):1761. [CrossRef]
- Macedo JC de, Olivo CR, Barnabé V, Dias ED, Moraes ÍAP de, Tibério I de FLC, et al. Short-term effects of conventional chest physiotherapy and expiratory flow increase technique on respiratory parameters, heart rate, and pain in mechanically ventilated premature neonates: A randomized controlled trial. Healthcare (Basel). 2024;12(23):2408.
- De Abreu LC, Valenti VE, de Oliveira AG, Leone C, Siqueira AA, Herreiro D, et al. Chest-associated motor physiotherapy improves cardiovascular variables in newborns with respiratory distress syndrome. Int Arch Med. 2011;4(1):37. [CrossRef]
- Gomez-Conesa A, Fernández Rego FJ, Agüera Arenas JJ. Vojta therapy in the reduction of perinatal risk in preterm infants with respiratory distress syndrome and bronchopulmonary dysplasia. Physiotherapy. 2016;102:e199. [CrossRef]
- Chanelière C, Moreux N, Pracros J-P, Bellon G, Reix P. Rib fractures after chest physiotherapy: a report of 2 cases. Arch Pediatr. 2006;13(11):1410–2.
- Nunes A de M, Fernandes ATSF, de Castro Silva AT, Pereira SA. Effects of respiratory physiotherapeutic interventions on pulmonary mechanics, vital parameters and pain in newborns: a systematic review. Can J Respir Ther. 2025;61:145–56.
- Liu Y, Li ZF, Zhong YH, Zhao ZH, Deng WX, Chen LL, et al. Early combined rehabilitation intervention to improve the short-term prognosis of premature infants. BMC Pediatr. 2021;21(1):269. [CrossRef]
- Probst VS, Soares DS, Escobar VC, et al. Effect of bucket hydrotherapy on clinical parameters in infants with bronchopulmonary dysplasia: A pilot randomized clinical trial. Can J Respir Ther. 2025;61. [CrossRef]
- Mendoza JC, Roberts JL, Cook LN. Postural effects on pulmonary function and heart rate of preterm infants with lung disease. J Pediatr. 1991;118(3):445–8. [CrossRef]
- Brunherotti MA, Martinez EZ, Martinez FE. Effect of body position on preterm newborns receiving continuous positive airway pressure. Acta Paediatr. 2014;103(3):e101–5. [CrossRef]
- Hough JL, Johnston L, Brauer SG, Woodgate PG, Pham TMT, Schibler A. Effect of body position on ventilation distribution in preterm infants on continuous positive airway pressure. Pediatr Crit Care Med. 2012;13(4):446–51. [CrossRef]
- Kole J, Metgud D. Effect of lung squeeze technique and reflex rolling on oxygenation in preterm neonates with respiratory problems: A randomized controlled trial. Indian J Health Sci Biomed Res. 2014;7(1):15.
- Thacker NJ, Patel SB, Patel NS. Effect of lung squeezing technique for correcting atelectasis in mechanically ventilated preterm infants with respiratory distress syndrome. Int J Allied Med Sci Clin Res. 2014;2(4):433–8.
- Utario Y, Rustina Y, Waluyanti FT. The quarter prone position increases oxygen saturation in premature infants using continuous positive airway pressure. Compr Child Adolesc Nurs. 2017;40:95–101. [CrossRef]
- Gomez-Conesa A, Fernández Rego FJ, Agüera Arenas JJ. Vojta therapy in the reduction of perinatal risk in preterm infants with respiratory distress syndrome and bronchopulmonary dysplasia. Physiotherapy. 2016;102:e199. [CrossRef]
- Tavares AB, Treichel L, Ling CC, Scopel GG, Lukrafka JL. Fisioterapia respiratória não altera agudamente os parâmetros fisiológicos ou os níveis de dor em prematuros com síndrome do desconforto respiratório internados em unidade de terapia intensiva. Fisioter Pesqui. 2019;26(4):373–9.
- Mehta Y, Shetye J, Nanavati R, Mehta A. Physiological effects of a single chest physiotherapy session in mechanically ventilated and extubated preterm neonates. J Neonatal Perinatal Med. 2016;9(4):371–6. [CrossRef]
- Igual-Blasco A, Piñero-Peñalver J, Fernández-Rego FJ, Torró-Ferrero G, Pérez-López J. Effects of chest physiotherapy in preterm infants with respiratory distress syndrome: a systematic review. Healthcare (Basel). 2023;11(8):1091. [CrossRef]
- Bhandari AP, Nnate DA, Vasanthan L, Konstantinidis M, Thompson J. Positioning for acute respiratory distress in hospitalised infants and children. Cochrane Database Syst Rev. 2022;6(6):CD003645. [CrossRef]
- Ferguson KN, Roberts CT, Manley BJ, Davis PG. Intervenciones para mejorar las tasas de extubación exitosa en bebés prematuros: una revisión sistemática y un metanálisis. JAMA Pediatr. 2017;171(2):165–74.
- De Abreu LC, Valenti VE, de Oliveira AG, Leone C, Siqueira AA, Herreiro D, et al. Chest-associated motor physiotherapy improves cardiovascular variables in newborns with respiratory distress syndrome. Int Arch Med. 2011;4(1):37. [CrossRef]
- Aherrao S, Sharath HV. Effect of thoracic squeezing technique and expiratory flow increase technique on neonates with neonatal respiratory distress syndrome: a case report. Cureus. 2024;16(9):e68702. [CrossRef]
- Ferrara PE, Gatto DM, Codazza S, Zordan P, Stefinlongo G, Di Polito A, et al. PEP mask therapy for the rehabilitation of a pre-term infant with respiratory distress syndrome: a case report. Eur J Phys Rehabil Med. 2023;59(3):436–9. [CrossRef]
- Tavares AB, Treichel L, Ling CC, Scopel GG, Lukrafka JL. Fisioterapia respiratória não altera agudamente os parâmetros fisiológicos ou os níveis de dor em prematuros com síndrome do desconforto respiratório internados em unidade de terapia intensiva. Fisioter Pesqui. 2019;26(4):373–9.
- Hough JL, Johnston L, Brauer SG, Woodgate PG, Pham TMT, Schibler A. Effect of body position on ventilation distribution in preterm infants on continuous positive airway pressure. Pediatr Crit Care Med. 2012;13(4):446–51. [CrossRef]
- Chanelière C, Moreux N, Pracros J-P, Bellon G, Reix P. Rib fractures after chest physiotherapy: a report of 2 cases. Arch Pediatr. 2006;13(11):1410–2.
- Nunes A de M, Fernandes ATSF, de Castro Silva AT, Pereira SA. Effects of respiratory physiotherapeutic interventions on pulmonary mechanics, vital parameters and pain in newborns: a systematic review. Can J Respir Ther. 2025;61:145–56.
| Intervention Characteristics | Specific Measures | Target Effects |
| Comparison of prone vs supine positioning in preterm infants on CPAP. Infants remained in each position for 3 hours before switching to the alternative posture. | Oxygen saturation, respiratory rate, heart rate. Measurements collected immediately post-intervention and at 30–90 minutes. | Prone positioning significantly increased oxygen saturation compared with supine, with no significant changes in RR or HR. Improved oxygenation stability. |
| Assessment of postural effects (supine, prone, lateral positions) on pulmonary function in preterm infants with lung disease. | Pulmonary function tests including lung compliance and tidal volume, plus heart rate. | Prone and lateral positions improved pulmonary mechanics, reduced work of breathing, and enhanced ventilation distribution. |
| Evaluation of body positioning (prone, supine, lateral) in preterm infants receiving CPAP. | Oxygen saturation, respiratory pattern, thoracoabdominal synchrony, ventilation distribution. | Prone and lateral positions improved oxygen saturation and thoracoabdominal synchrony, providing more homogeneous ventilation distribution. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




